Abstract
In order to prevent suicide it is important to understand the factors that put people at increased risk. Many who die by suicide are not employed at the time, often because of mental health problems [1,2]. But among those in the workforce there are occupational groups at high risk of suicide compared with others in the working population [3–7]. Understanding the factors that lie behind these variations in suicide risk according to occupation could lead to more effective suicide prevention in these groups.
Doctors seem to have received a disproportionate amount of attention, possibly reflecting researchers' interest in their own peer group as well as availability of records [4]. Two systematic reviews of suicide among doctors have concluded that suicide rates were indeed higher than for those of the general population, particularly among female doctors [8,9]. Platt and Hawton [5] believed there was also sufficient evidence to conclude that female nurses and farmers are at relatively high risk. Suicide risk in other occupational groups is less clear. Assessment of suicide by occupation in England and Wales using both proportional mortality ratios (PMRs) and standardized mortality ratios (SMRs) showed excess mortality among some broad occupational groups [7]. Health professionals and agricultural workers had high PMRs. Meltzer and colleagues [7] cautioned, as had Kelly and Bunting [3] in an earlier report, that among some professional groups the high proportional mortality ratios (PMRs) for suicide reflected overall low mortality. Boxer and colleagues [4] commented in 1995 on the need for corroborative findings from several studies in view of the likelihood of chance findings when multiple occupations or causes of death are examined. Moreover, there may be real variations internationally.
One of the ways in which occupation might confer risk could be by providing access to and familiarity with a particular method of suicide. Kelly and Bunting [3] noted that in England and Wales, methods of suicide did vary by occupation in line with this theory. This was less evident among women, which they considered was mainly because poisoning accounted for half of all female suicides. Other researchers studying specific occupations have noted the same tendency for an occupational group to use a suicide method to which they have access [10–15]. While there has been debate about the extent to which people will use a different method if the favoured means is not available, it is likely that substitution of means occurs only partially [16]. This would suggest that there is value in increasing knowledge about means of suicide used by those in high risk occupations, in case ways can be found to mitigate some of the risks.
A major review of the epidemiology and prevention of suicide in New Zealand was published recently [17,18]. None of this work, however, examined suicide by occupational group. Three studies examining suicide by occupation have been carried out in New Zealand [19–21]. In a series of analyses examining mortality among men aged 15–64 years for the period 1980–1985, SMRs were calculated by occupational group. Some high risk occupational groups were identified, although small numbers limited the confidence that can be placed on the results for some groups [19]. A major revision to the New Zealand Standard Classification of Occupations (NZSCO) was introduced in 1992 [22], and occupation ceased to be coded by Statistics New Zealand in 1997. Langley and Stephenson [20] were able to identify some high risk occupational groups in New Zealand for the 1991–1996 period, but the new coding system resulted in an inability to determine rates in specific occupational groups and precluded use of a longer time period (because of the changes in the classification of occupations). Gallagher and colleagues [21] investigated suicide by occupational group in New Zealand for the period 2001–2005, but studied only major occupational groups (nine categories), with incomplete data for 2004 and 2005.
We aimed to examine suicide by identified occupational groups in New Zealand over a period of 30 years. We focused on certain groups that we predicted would have high suicide rates if access to and familiarity with particular methods of suicide within those groups put them at risk.
Method
Data were obtained for all suicide deaths (International Classification of Diseases [ICD] codes E950–959), and deaths by injury undetermined whether accidentally or purposefully inflicted (ICD E980–E989), for the years 1973–2004 (ICD 9th and 10th revisions). It was considered appropriate to include deaths with undetermined cause (open verdicts) because of evidence that the majority of these are suicides [3]. Occupational groups of interest were determined by their NZSCO codes [22–25]. The occupational groups of interest were dentists, doctors, farmers (including farm workers), hunters and cullers, military personnel, nurses, pharmacists, police and veterinarians. Mortality data with occupational group recorded were not available for the years 1996 and 1997, so the time period examined was 1973–2004, but excluding 1996 and 1997 (30 years of data). For those deaths where occupation was not coded (for the years 1998–2004) we obtained the free field description of the occupation and coded the data ourselves. Crude mortality rates were calculated based on numbers (including open verdicts) in each occupational group at each quinquennial census, 1976–2001. SMRs were calculated using suicide rates (all methods of suicide combined including open verdicts) in all employed groups as the standard population based on quinquennial census data from 1976 to 2006 as denominator. The SMR is the ratio of number of deaths observed in an occupation, to the number that would be expected if the occupational group of interest (e.g. doctors) had the same age specific mortality rates as the total employed population [26]. An SMR of 1.0 denotes no difference. The age ranges examined were those of the employed population aged 15–64 years, and those aged 15 years and over. Chi-square and, for small numbers, Fisher's exact test p values and 95% confidence intervals (CIs) were calculated. The distribution of the methods of suicide was compared between occupational groups of interest and all occupations not examined here using Chi-square tests, with Fisher's exact test used where there were small expected cell counts. All analyses were performed using SAS 9.1.2 (SAS Institute, Cary, NC) and Stata 10.0 (Statacorp, College Station, TX) and p <0.05 was considered statistically significant. As this was an exploratory study with an a priori interest in some specific occupations, no adjustments were made for multiple comparisons.
Results
A total of 940 suicide deaths (including open verdicts) were recorded in the occupations of interest out of a total of 7329 such deaths in all employed persons aged 15–64 years over the full 30 year period. The numbers of men and women employed in each occupation, the numbers of deaths by suicide, and suicide rates are shown in Table 1.
Number employed, number of suicide deaths (including open verdicts), and annual suicide rate by occupation among New Zealanders aged 15–64 years, 1973–2004†
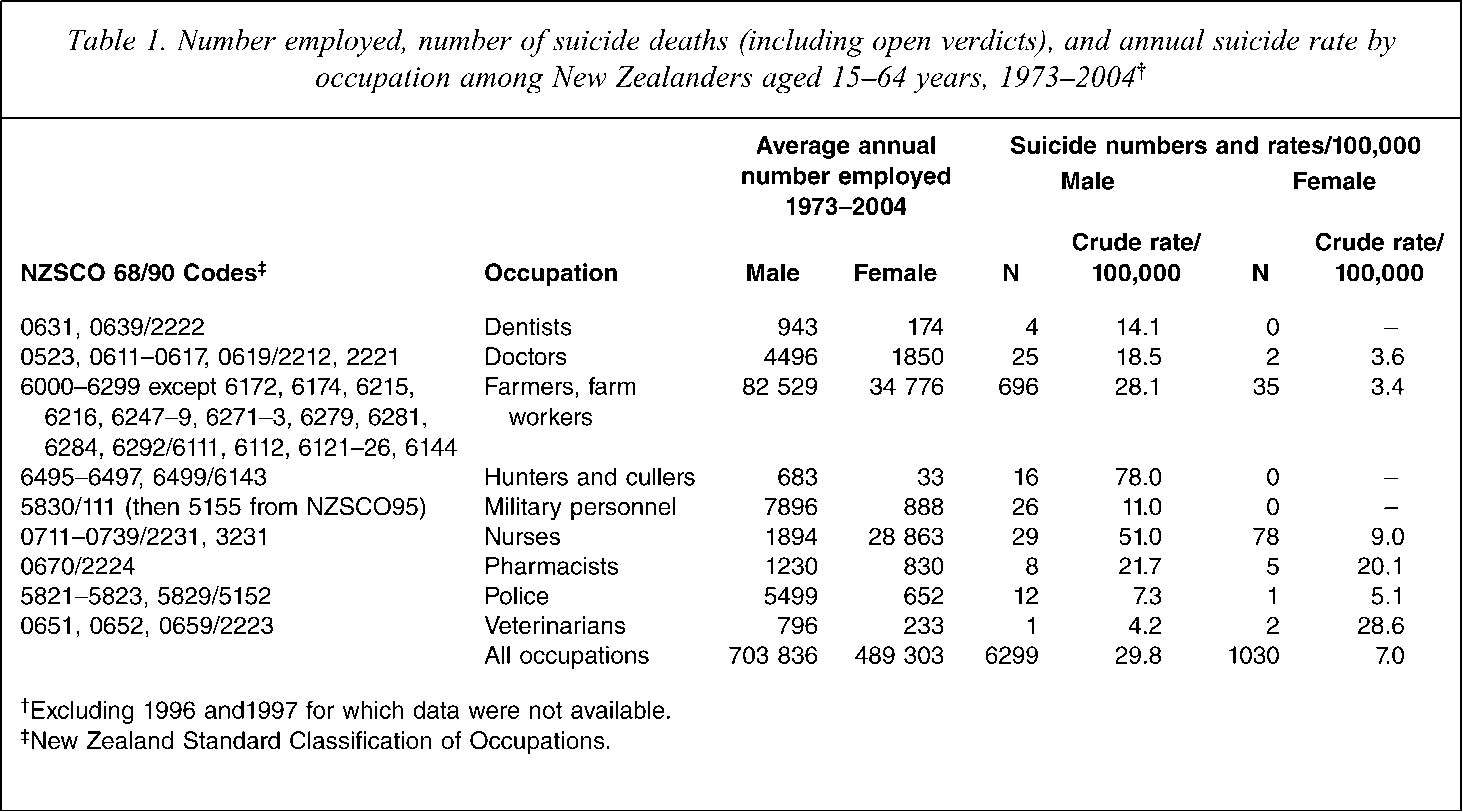
†Excluding 1996 and1997 for which data were not available.
‡New Zealand Standard Classification of Occupations.
SMRs for men and women by occupation are shown in Table 2. SMRs were elevated for only three of the nine occupational groups: nurses (both male and female), hunters and cullers (all male), and female pharmacists. Neither doctors nor farmers were at increased risk, and in the case of male doctors the risk was significantly lower than for the total employed population. Risks were also low for female farmers and for men working in the military or police force. Small numbers limited the confidence that could be placed on some of the results, particularly those for dentists and veterinarians. There was no evidence of elevated risk, however, among either of these groups. An analysis of SMRs for all people aged 15 years and over (rather than just 15–64 years) was conducted (data not shown), but the SMRs changed little as a result, except that the SMR for male farmers decreased from 1.0 to 0.8 (CI 0.8 to 0.9), which was significantly below average. Because the three veterinary suicides in the age range 15–64 years and an additional one in a veterinarian aged over 65 years had all occurred in the more recent time period, a separate analysis of veterinarians for the 1998–2004 period for both sexes combined was conducted. The SMR for veterinarians in this period of 1.62 was not significantly high (p = 0.33), with a wide confidence interval reflecting the small number involved.
Number of deaths and standardized mortality ratios (SMRs) for suicide by occupation for New Zealanders aged 15–64 years, 1973–2004†
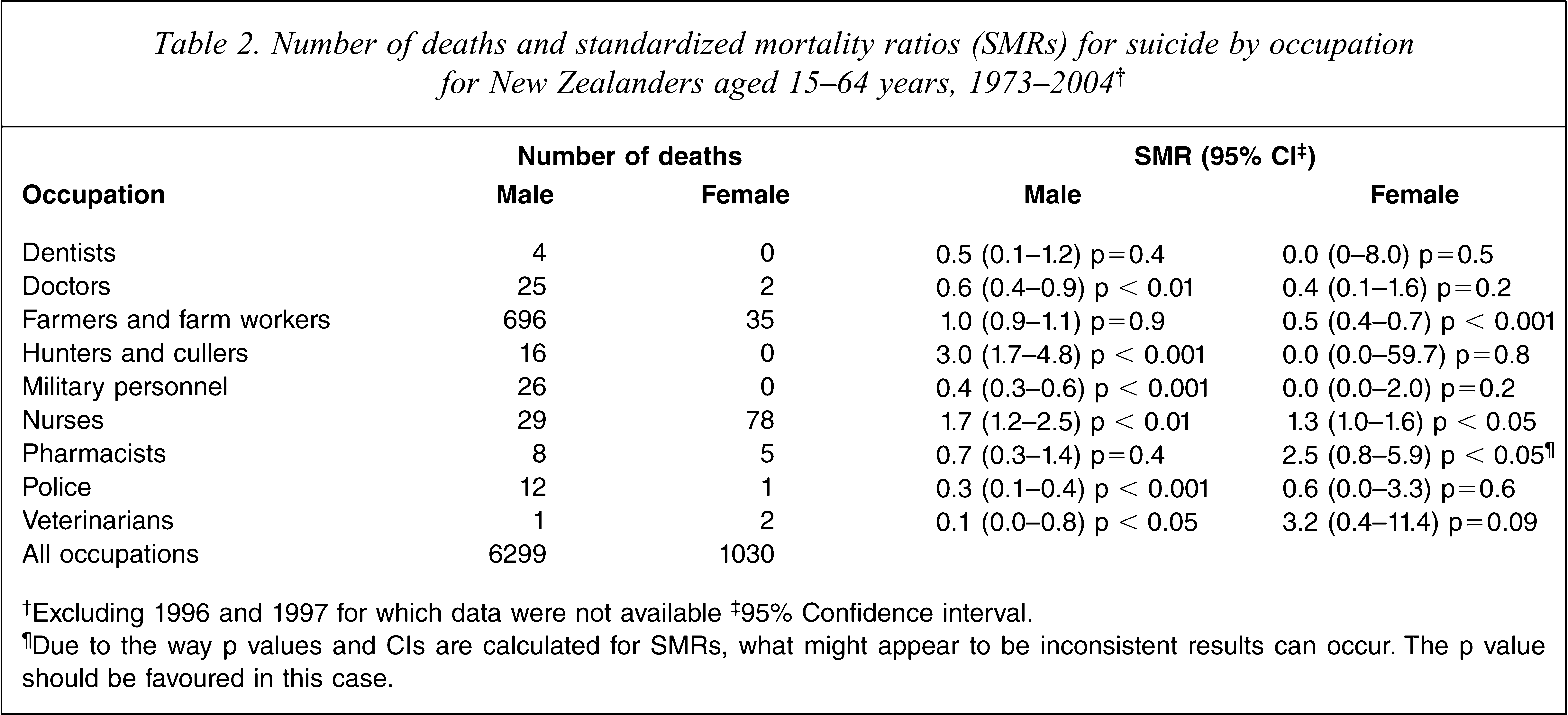
†Excluding 1996 and 1997 for which data were not available ‡95% Confidence interval.
¶Due to the way p values and CIs are calculated for SMRs, what might appear to be inconsistent results can occur. The p value should be favoured in this case.
Methods of suicide by occupational group are shown in Table 3. Doctors, nurses, pharmacists and veterinarians were more likely to choose poisoning as their method of suicide. For each of these groups the difference in methods used compared with methods used by all other occupations was statistically significant. Farmers and hunters and cullers were more likely to use firearms, but the result for hunters and cullers did not reach statistical significance. Means used by military personnel were significantly different from methods used by those employed in other occupations, but the main method was hanging, and firearm suicides were not overrepresented.
Percentages and numbers of suicides (including open verdicts) by method for specific occupational groups, 1973–2004†
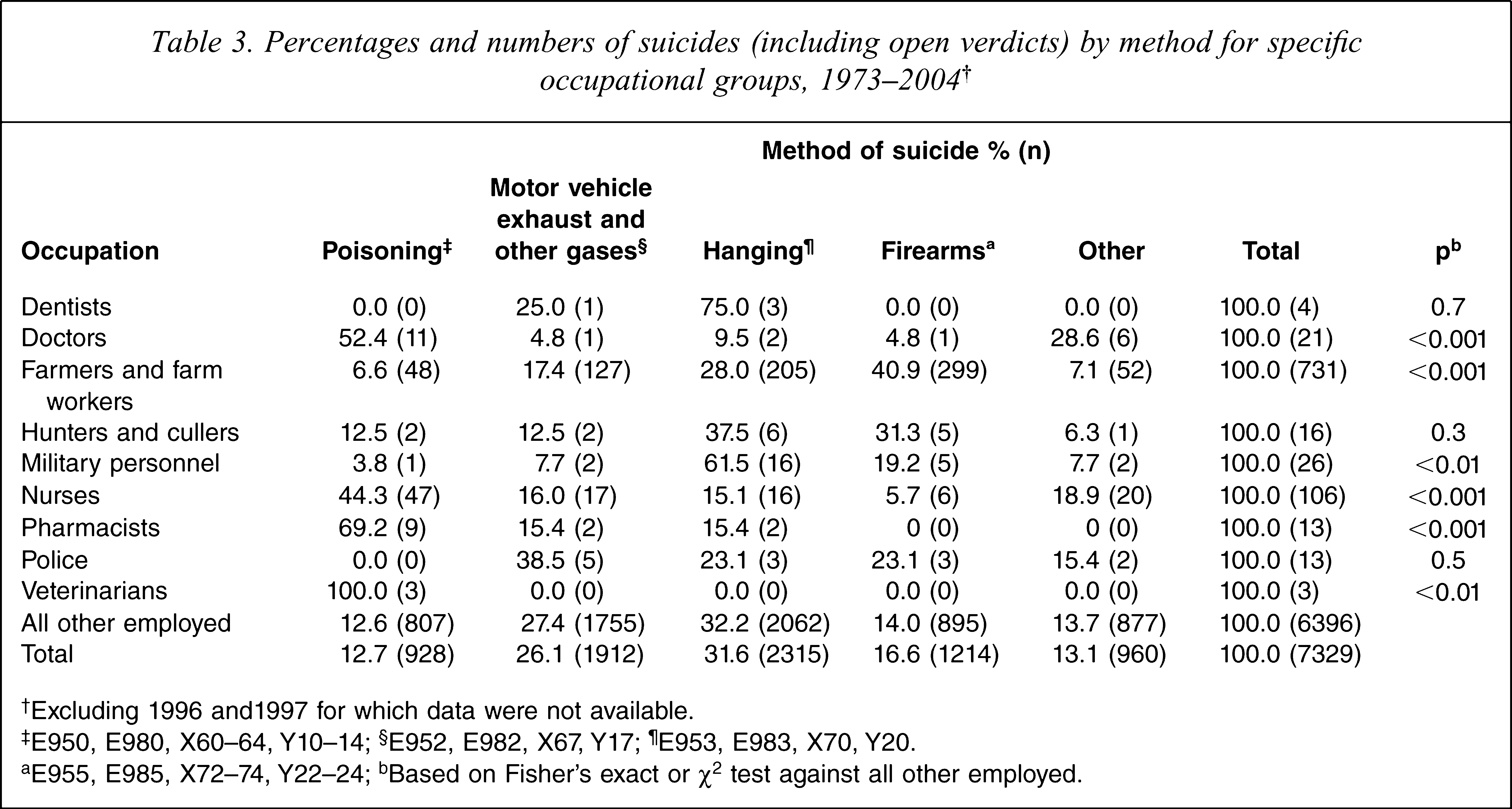
†Excluding 1996 and1997 for which data were not available.
‡E950, E980, X60–64, Y10–14; §E952, E982, X67, Y17; ¶E953, E983, X70, Y20.
aE955, E985, X72–74, Y22–24; bBased on Fisher's exact or χ2 test against all other employed.
Discussion
Few of the occupational groups we investigated had high risks of suicide as assessed by SMRs, and some were at lower risk than the general population. This was despite the fact that eight of the nine groups chosen had presumed access to means of suicide and the remaining occupation, dentistry, involved knowledge that would make acquisition of lethal medication a possibility. Among health-related occupations, nurses (both male and female) and female pharmacists stood out as being at increased risk of suicide. Hunters and cullers had the highest SMRs among the groups studied. In contrast, doctors, farmers and veterinarians were not at high risk. Male doctors in New Zealand were at low risk of suicide. Ease of access to means, however, did appear to have affected the methods chosen, with several health-related occupational groups being more likely to use poisoning than the rest of the employed population. Among those with occupations where firearms were likely to be accessible, there was diversity: farmers were more likely to use firearms but members of the police and armed forces were not.
Strengths of this study include the fact that it is recent, a long time interval was used, very specific occupations of a priori interest were examined, and a summary measure of mortality for each occupation standardized for age was used. The main disadvantage of this measure is that, as the SMR uses data from the census, there is the potential for misclassification bias between numerator and denominator. This is unlikely, however, to apply to the occupations included here except for hunters and cullers. Our main analysis used the working age groups (15–64 years), in which occupation was more likely to be accurately recorded on death certificates and at censuses [27,28]. Even though we included 30 years of data, there were low frequencies of events in some categories. We were unable to include two years of data because the occupations were not available. Another limitation was that because the changes and omissions in occupational coding necessitated coding from free field data, a comprehensive list including all occupations with presumed access to means of suicide was beyond our scope.
Our results call into question the importance of access to means as a determinant of occupational suicide risk. Not only was suicide risk not elevated in most of the occupational groups studied, but among male doctors and veterinarians, suicide risk was low. The result for doctors was particularly surprising in view of the fact that doctors have been found to have elevated risks for suicide in many studies, although not universally [9]. In England and Wales, as in New Zealand, the SMR for male doctors was less than that for the general population, although female doctors in England and Wales were at increased risk [7,29]. Hawton and colleagues [29] commented that their use of SMRs rather than PMRs probably explained the difference between their study and earlier ones. In a study of working doctors and dentists in 26 US states, suicide rate ratios were elevated among women doctors but reduced among male doctors and dentists compared with the working population [30]. Langley and Stephenson [20] had not been able to investigate doctors as a specific occupational group in their New Zealand study, but did note that the minor category of ‘health professionals (except nursing)’, which included doctors, had a relatively low suicide rate. A high SMR for suicide among medical graduates of the University of Melbourne was reported in an Australian study, but numbers were small [31]. The SMR for male doctors of 113 was not significantly raised, but that for female doctors (501) was statistically significant despite the low frequency of suicides.
Another surprising result in our study was that New Zealand farmers displayed no elevated suicide risk. As with doctors, some variability in relative risk for farmers has been found internationally [32]. The definition of farmer varies, but usually includes farm workers, as in New Zealand. In Australia, both farm managers and agricultural labourers were noted to have high suicide rates [12]. The Australian farmer codes as used by Page and Fragar [12] included hunters and trappers, a group we assessed separately and found to carry particularly high risks of suicide. This demonstrates how risk may vary among occupations grouped together in occupational coding systems, and may explain some of the international variation. Farming conditions are also likely to vary widely. In Scotland, for example, farmers were more likely to die by suicide in areas where farming was less common [33].
The high risk among hunters and cullers contrasted with the low risk found among members of the police and armed forces despite their handling of firearms. Hunters have constant access to their firearms and use them regularly to kill, whereas police and military access to weapons is strictly controlled, and they are usually used for defensive purposes only. Also likely to be relevant are the pre-enlistment screening, firearm training and regulations, group identity and structured environment in the police and armed forces, with a strong esprit de corps and access to health care [13]. Lower suicide rates than for civilians have been documented in a number of studies of suicide among military personnel [13]. A systematic review of international studies of police suicide found no convincing evidence for elevated risk of suicide [34]. These occupational differences suggest that it is not only access that is important but also the environment in which that access occurs.
The risk of suicide found among New Zealand nurses of both sexes is noteworthy. Langley and Stephenson [20] had noted that ‘nursing associate professionals’ had the highest suicide rate among their list of minor occupational groups, although absolute numbers were small. While some overseas investigators have studied suicide among nurses [35–38], it is ironic that so much more attention has been given to suicide among doctors. In New Zealand, at least, it is nurses, not doctors, who appear to be at increased risk for suicide, particularly male nurses. They are also more likely than the general population to use poisoning. Hawton and colleagues [36] conducted a psychological autopsy study of a series of female nurses in England and Wales who died by suicide. They concluded that the most important strategies for suicide prevention in nurses lay in the prevention, detection, and management of psychiatric disorders. In a Danish case control study of suicide, nurses stood out as a high risk occupational group among those who died by suicide but had never had a psychiatric admission [6]. It was suggested that this could have been due to unidentified psychiatric illness, which raises the question as to whether the perceived stigma of psychiatric illness impinges on help seeking among nurses. In a prospective study of female US nurses, reported stress at home and at work was related to suicide up to 14 years later, with both severe stress and minimal stress levels being associated with higher suicide risk than was light stress [35]. The authors considered that the increased suicide risk with minimal stress might reflect denial or undiagnosed depression. The link with severe stress might suggest a role for health promotion measures designed to reduce work and home stress among nurses.
Suicide prevention is a complex matter. While there are differences among occupations with regard to suicide risk, such risks vary over time and place. Access to means may be less important in some circumstances than in others, perhaps because of the presence of other factors that confer protection. Nevertheless, among the groups we studied with access to lethal means were three groups whose risk of suicide has so far received little attention in New Zealand: nurses, female pharmacists, and hunters and cullers. Those providing medical care for these groups need to be aware of the risk of suicide. In the case of hunters and cullers, their isolated lifestyles may impede access to medical care. Increased social support and attention to any mental health problems could be beneficial, as well as removal of firearms when a person is judged to be suicidal.
Footnotes
Acknowledgements
We thank Glenys Forsyth for assistance with data analysis and Keith Hawton for helpful comments. The required information about mortality was obtained from the Information Directorate of the Ministry of Health.
This study was funded by a grant from the James Hume Fund of the University of Otago. Brian Cox was funded by the Director's Cancer Research Trust.
