Abstract
Keywords
Borderline personality disorder (BPD) is one of only two conditions that includes suicide attempts as a criterion for diagnosis in the DSM-IV classification system [1], indicating that suicidal behaviour is a common accompaniment to this disorder. It has also been found, however, that the least prevalent and most changeable criteria for BPD are self-injury and behaviours defending against abandonment [2]. A review suggested that people with BPD improve over the long term, decreasing in suicidality, self-destructiveness and interpersonal maladjustment, if survival is effectively managed during the turbulent years of youth [3]. Nevertheless, a recent review suggested that suicidal behaviour is a common complication, and continues to be a chief concern in the clinical management of BPD [4].
Better treatments for BPD and particularly for the suicidal behaviour and suicide deaths experienced by these patients have been sought for some time. It has been estimated that although 10% will eventually complete suicide, this outcome is not readily predictable, and hospitalization is of unproven value for suicide prevention, possibly producing negative effects [5].
There have been few effective interventions tested in randomized controlled trials (RCTs) to reduce rates of suicide attempt, parasuicide or deliberate self-harm (DSH) in BPD. For outpatients, a day hospital programme with a psychoanalytic treatment component [6] and for female subjects with multiple parasuicidal behaviours, dialectical behaviour therapy (DBT) have been shown to be effective [7]. Both of these therapies have also demonstrated long-term reduction in suicidal behaviour after the cessation of therapy [8–10]. DBT is a team-based treatment combining cognitive, behavioural and mindfulness techniques, delivered in individual therapy, group-based skills training, out-of-hours telephone contact with individual therapist modalities and a therapist consultation group [7].
There have been other trials of DBT with a reduction in suicidal behaviours as the primary outcome, replicated outside of the University of Washington: RCT in the Netherlands [11], a study with inpatients in Germany in a non-controlled design [12], and a three-arm RCT in New York [13]. There have also been adaptations of the duration or ‘dose’ of DBT into a 12 week programme for adolescents [14], 6 months for female veterans [15], 6 months for female subjects with active suicidal ideation [16], 28 weeks skills training for depressed women aged >60 years [17] and 20 weeks for bulimic behaviour [18]. DBT has also been applied in other female BPD populations: drug dependence [19], veterans [15], opioid dependence [20] with bulimic behaviour [18] and in depressed elderly [17].
DBT has been demonstrated to be effective in RCTs for other outcomes including retention in treatment [7,19], fewer inpatient hospital days [7], social and global adjustment [19] and reduction in substance use [19,20]. Nevertheless, there have been some reservations expressed about the limited research base and methodological limitations of the published studies for DBT, especially in the light of the enthusiastic take up of DBT as a treatment [21].
There are no RCTs from Australia addressing suicidal behaviour in BPD, but a non-controlled study of 30 subjects using a self-psychology intervention (Hobson's conversational model) delivered by trainee psychiatrists showed improvement for the year of treatment, which was sustained at follow up 12 months later. Improvements were shown in frequency of use of drugs (both prescribed and illegal), number of visits to medical professionals, number of episodes of violence and self-harm, time away from work, number of hospital admissions, time spent as an inpatient and a score on a self-report index of symptoms [22]. This group was later followed up for a period of 5 years and was compared to a cohort (non-randomized) of waiting list (WL) patients. The primary outcome was improvement in DSM total criteria scores [23]. In a different Australian study, a retrospective examination of two different treatment conditions for BPD patients showed that those who received a special treatment contract had a significantly higher total number of admissions but not more presentations to the emergency department than the standard treatment group [24].
Aims
The purpose of the present study was to compare DBT and the control condition of treatment as usual plus WL for DBT (TAU+WL) for the primary outcomes (differences in proportions and event rates) of any DSH event; general hospital admission for DSH and psychiatric admission for any reason; and mean difference in length of stay for any hospitalization. Secondary outcomes were disability and quality of life measures.
Methods
Setting
The Hunter DBT project was undertaken in Newcastle, Australia at the Centre for Psychotherapy, a clinical outpatient unit of the Hunter New England Mental Health Service. Individual DBT therapists and skills trainers were psychiatrists, social workers, clinical psychologists, psychologists, occupational therapists or nurses by training.
Training
DBT training for therapists was initially undertaken with a self-directed reading programme using the DBT skills manual [25] and other materials suggested by the honorary consultants to the study. An initial introductory programme was conducted and later extended with DBT consultation sessions conducted in Newcastle. Four members of the Hunter DBT treatment team attended a 2 week intensive training in DBT in New Zealand after the project had commenced.
Study design
The Hunter DBT project was an RCT of modified DBT. The intervention condition was based on the comprehensive DBT model, a team-based approach including individual therapy, group-based skills training, telephone access to an individual therapist and therapist supervision groups following the model of treatment developed by Linehan et al. [7]. The main change to the Linehan et al. model was the telephone access to individual therapists. In the present study telephone access was delivered using a group roster of DBT individual therapists (not contact with each participant's individual therapist) between 8:30 a.m. and 10 p.m., and telephone contact with the local psychiatric hospital between 10 p.m. and 8:30 a.m.
The control condition was a 6 month WL for DBT while receiving TAU (TAU+WL). Subjects, both in the initial DBT group and in the TAU+WL group who came to DBT after 6 months were offered 12 months DBT treatment, although the comparison between groups was restricted to the first 6 months of DBT versus TAU+WL. This design was also different to the original Linehan et al. study, which used TAU as the control condition and comparison of groups after 4 months, 8 months and 12 months of DBT therapy.
Randomization
Randomization was carried out by the research staff and participants were allocated by selection of sealed opaque envelopes. Randomization was undertaken after consent to participate and completion of all the baseline measures and eligibility interview.
Treatment procedures
Treatment (DBT) participants were assigned to the next available individual therapist. Treatment subjects were also assigned to the relevant skills training group, meeting weekly with the modules running in the following order: Interpersonal Effectiveness, Emotion Regulation and Distress Tolerance. Each module ran for 8 weeks. Groups had a minimum of four members before commencement and a maximum of eight members. Entry to the skills group occurred only at the commencement of the next skills module.
Participants
The flow of participants through the study is shown in the CONSORT diagram (Figure 1). Of the 112 participants referred for participation in the trial, 16 did not attend the assessment, while 16 were excluded because they did not meet the criteria for BPD and one was of no fixed address (NFA). Of the 79 participants eligible for the programme, three did not complete initial baseline assessments and were therefore excluded from the study, two withdrew consent after assessments and treatment were completed and one died by suicide following the baseline assessment period. Additionally, three completed baseline assessments but due to a technical error some of their demographic and diagnostic data were not recorded and were missing in those analyses.
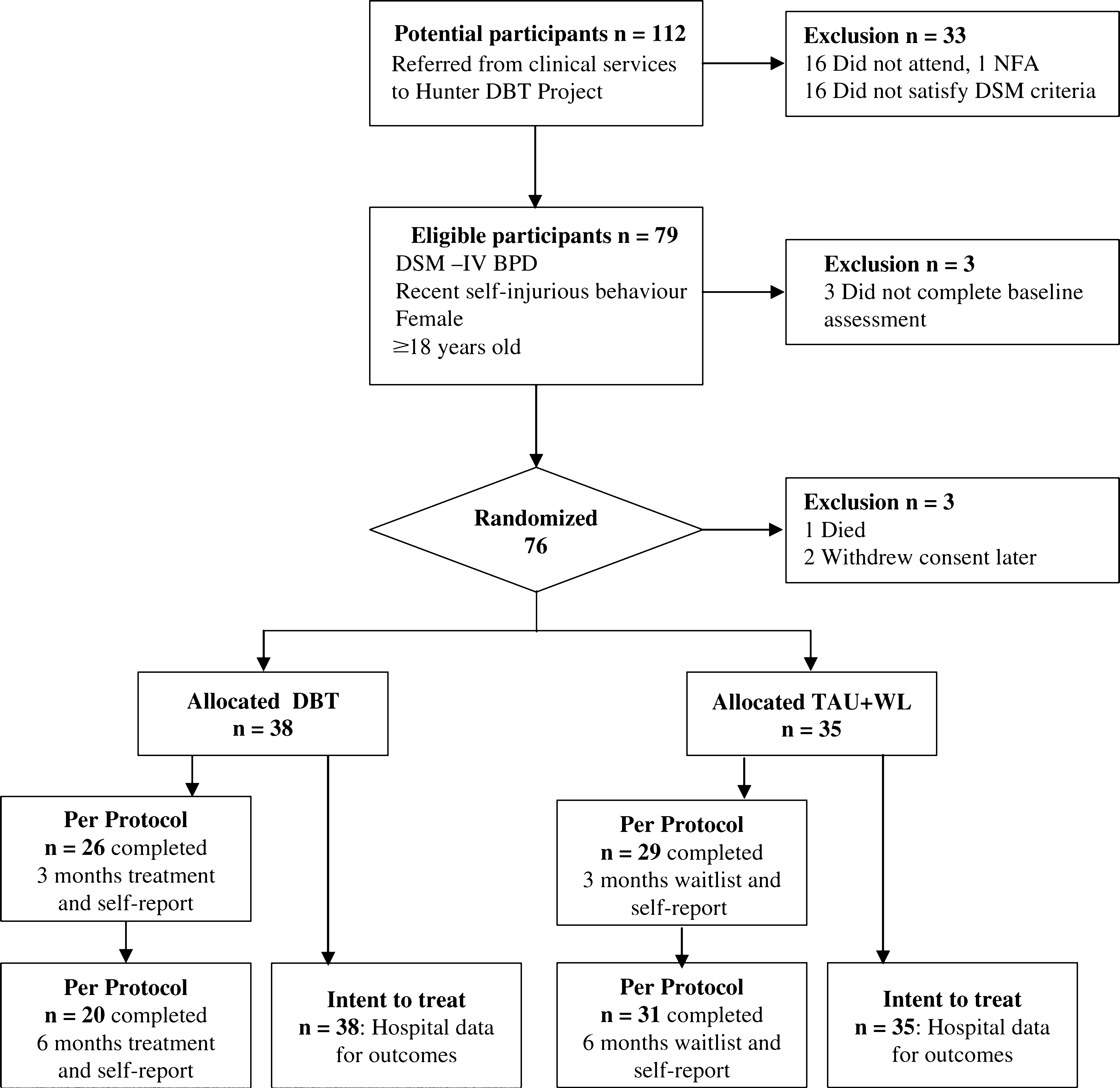
CONSORT Diagram of participant flow. BPD, borderline personality disorder; DBT, dialectical behaviour therapy; NFA, no fixed address; TAU+WL, treatment as usual+ waitlist.
Participants were female, aged 18–65 years, meeting criteria for BPD determined by clinical interview by a psychiatrist using DSM-IV criteria [1] and having a history of multiple episodes of deliberate self-harm, at least three self-reported episodes in the preceding 12 months. The psychiatrist assessor had the option of determining if any potential subjects were unsuitable for inclusion in therapy or unmotivated to participate, although there were no specific criteria for this exclusion. Exclusion criteria were presence of a disabling organic condition, schizophrenia, bipolar affective disorder, psychotic depression, florid antisocial behaviour, or developmental disability. Recruitment commenced in February 2000 and the last participant finished baseline assessment in July 2003.
Participants were referred from treating general practitioners, treating psychiatrists or public mental health services (any units of Hunter Mental Health Services); this process was coordinated by one of the investigators (CW). Referring clinicians were advised of the need for subjects to meet inclusion criteria and the need to maintain current therapy with the subjects until randomization was complete for the DBT group and during the 6 month wait time for the TAU + WL group. Upon commencement of DBT, participants were asked to discontinue psychological therapy of any sort for at least the 12 month duration of DBT.
Assessments and measures
Baseline assessment included parts of the computerized interview used in the Australian National Survey of Mental Health and Wellbeing [26]: demographics; Composite International Diagnostic Interview (CIDI; selected modules): anxiety, depression, bipolar disorders, alcohol abuse and dependence, substance abuse and dependence, International Personality Disorder Examination Questionnaire (IPDEQ) [27]; and the Brief Disability Questionnaire (BDQ) [28]. Other assessment instruments included Lifetime Parasuicide Count–2 [29]; Parasuicide History Interview–3 month period (PHI-2) [30] and the World Health Organization (WHO) Quality of Life–BREF version (WHOQOL-BREF) [31]. Two additional questions were asked at the end of the BDQ: (i) during the last month, how many days in total were you unable to carry out your usual daily activities fully; and (ii) during the last 1 month, how many days in total did you stay in bed all or most of the day because of illness or injury.
Assessments repeated 3 months and 6 months after allocation to DBT or TAU+WL included BDQ, PHI-2 and WHOQOL-BREF.
Outcomes and blindness of raters
Baseline characteristics were determined by research staff before randomization occurred and hence allocation was blind.
Outcomes were determined for the intention-to-treat analyses by assessors blinded to allocation, extracting information from psychiatric hospital and general hospital records either by direct examination of the clinical records or by extraction electronically from the Hunter Area Toxicology Service database at Newcastle Mater Hospital [32]. Primary outcomes for the intention-to-treat analyses were the proportion of participants with any hospital admission for DSH and the proportion with any psychiatric hospitalization for any reason; the number of general hospital admissions for DSH and the number of psychiatric hospital admissions for any reason; the length of stay for hospital admissions for DSH and for psychiatric hospital admissions for any reason. General hospital admission for DSH included any episode according to the following definition originally developed for ‘attempted suicide’: ‘any intentional self-injury or the deliberate ingestion of more than the prescribed amount of therapeutic substances, or deliberate ingestion of substances never intended for human consumption’ [33]. Secondary outcomes included any presentation without admission for general hospital-treated DSH and any presentation without admission to a psychiatric hospital for any reason.
For participants who received treatment and completed the self-report instruments at 3 months and 6 months after allocation, per-protocol analyses were conducted. All reasonable attempts were made to maintain blindness to allocation status for these raters, but this could not achieve perfect blindness. Primary outcomes for the per-protocol analyses were undertaken for the proportion of subjects with any episode of DSH (called parasuicide in the rating scales) and the number of DSH events. Secondary outcomes were disability scores and quality of life scores: days out of role in the past month and days spent in bed in the last month; and WHOQOL-BREF scores for all four domains (Physical, Psychological, Social and Environmental). The two items thought to be most relevant to disability for this patient population were chosen a priori for analysis, from the questions following on from the BDQ: days spent in bed and days out of role.
Analyses
Differences in proportions were tested using χ2 test. Event or count data were predominately analysed using either Poisson regression or negative binomial regression when appropriate. Negative binomial regression was used when the distribution showed overdispersion (variance much greater than the mean in Poisson distribution) or the goodness of fit for a Poisson regression showed large χ2 values or the likelihood ratio test of alpha was significantly different from zero. Zero inflated models were used when there was an excess of zero counts in the data and the Vuong test was significant. Results were expressed as incidence rate ratios with 95% confidence intervals (IRR: 95%CI). A post-hoc descriptive graphical analysis of the number of general hospital admissions for DSH and the number of psychiatric admissions for any reason for the period of 12 months (in 6 month blocks) before and after baseline was done to contextualize the pattern of psychiatric hospitalizations and general hospital admission for DSH over a longer time frame than the 6 month comparison of treatment effects.
Analysis of variance (ANOVA) was used for between-group mean differences in age, number of BPD criteria, IPDEQ score and mean number of reported lifetime episodes of self-harm. Mann–Whitney U-test was used for lifetime median number of DSH episodes (due to non-normally distributed data). A repeated-measures analysis of variance (rANOVA) was used for the mean number of DSH events over three 3 month time periods, covering the period of 3 months before baseline until 6 month follow up.
A rANOVA was also used for the secondary outcomes: BDQ days out of role in the past month and days spent in bed in the last month; and WHOQOL-BREF scores for all four domains (Physical, Psychological, Social and Environmental) over the same three time periods. Because these per-protocol analyses are subject to potential attrition bias and hence a threat to internal validity, we also conducted confirmatory linear mixed effect model analyses for any result showing a significant benefit of group (DBT vs TAU+WL) or the interaction of group (DBT vs TAU+WL) × time for the secondary outcomes of disability and quality of life. These confirmatory procedures used intention-to-treat analyses based on randomization status for all subjects who had baseline data available (disability, n = 70; quality of life, n = 73), using fixed effects for group (two levels), time (three levels) and group × time (six levels) predictor variables. Results are reported as F (derived by taking the ratio of the appropriate sums of squares) and p for each significant predictor variable. These analyses were conducted using the MIXED procedure in SPSS version 15 (SPSS, Chicago, IL, USA). All other analyses were conducted using SPSS version 14 or STATA SE version 10 (StataCorp LP, College Station, TX, USA).
Results
Table 1 lists the demographic characteristics and Table 2 the clinical characteristics of the participants at baseline. There were no significant imbalances of any of the a priori selected demographic or clinical variables at baseline.
Demographic characteristics of the sample
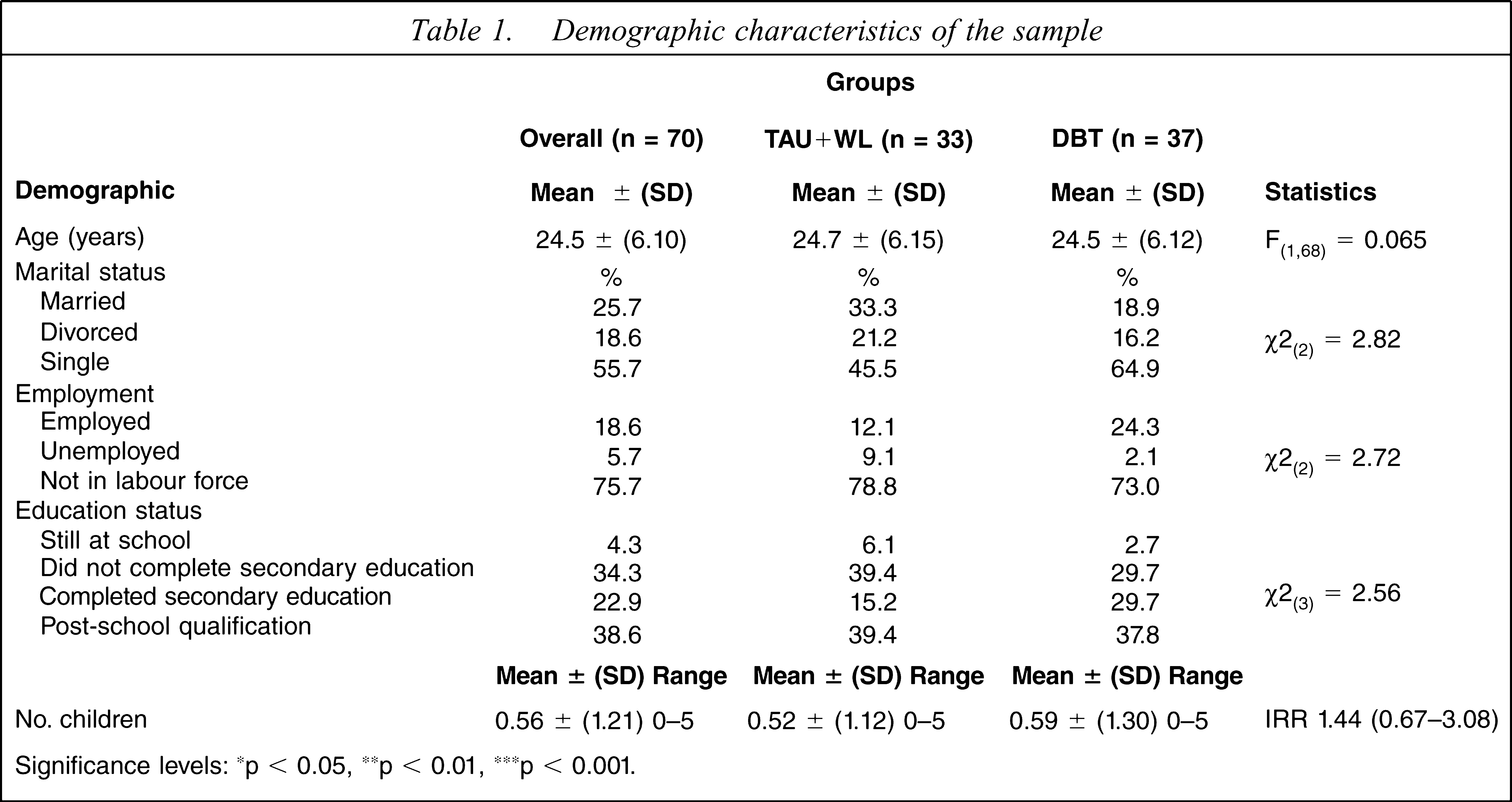
Significance levels: ∗p < 0.05, ∗∗p < 0.01, ∗∗∗p < 0.001.
Clinical characteristics of the sample
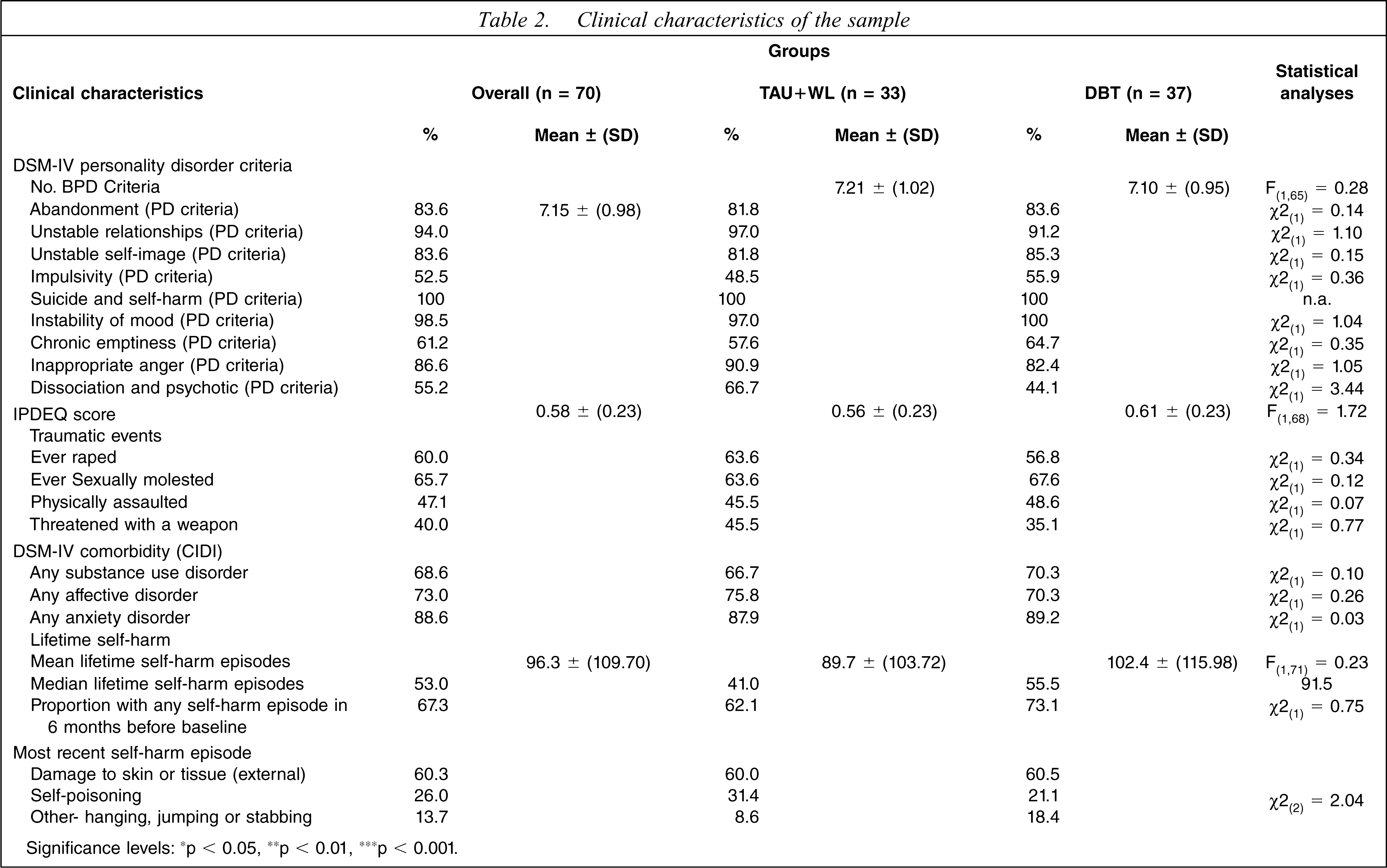
Significance levels: ∗p < 0.05, ∗∗p < 0.01, ∗∗∗p < 0.001.
The participants were young women, usually single, not in the labour force (home duties, pensioner or student), with nearly 40% having some post-schooling qualification. There was considerable exposure to traumatic events of sexual, physical and potentially life-threatening types. The participants showed substantial psychopathology with high rates of BPD criteria, IPDEQ scores and Axis 1 comorbidity. They had a substantial previous history of self-harm events, with external damage to skin (usually by cutting) and self-poisoning being the most common forms.
Table 3 lists the principal outcomes for the intention-to-treat analyses and the per-protocol analyses. For the intention-to-treat analyses, there were no significant differences in proportions for general hospital admission for DSH or for any psychiatric admission. There were no significant differences for the mean number of admissions of either type. Figure 2 also indicates that admissions of both types were rising in the time before the baseline of the study, falling for the 6 months of the study and continuing to fall for the 6 months following the study (when the TAU+WL control group had begun DBT) for both groups.
Principal outcomes
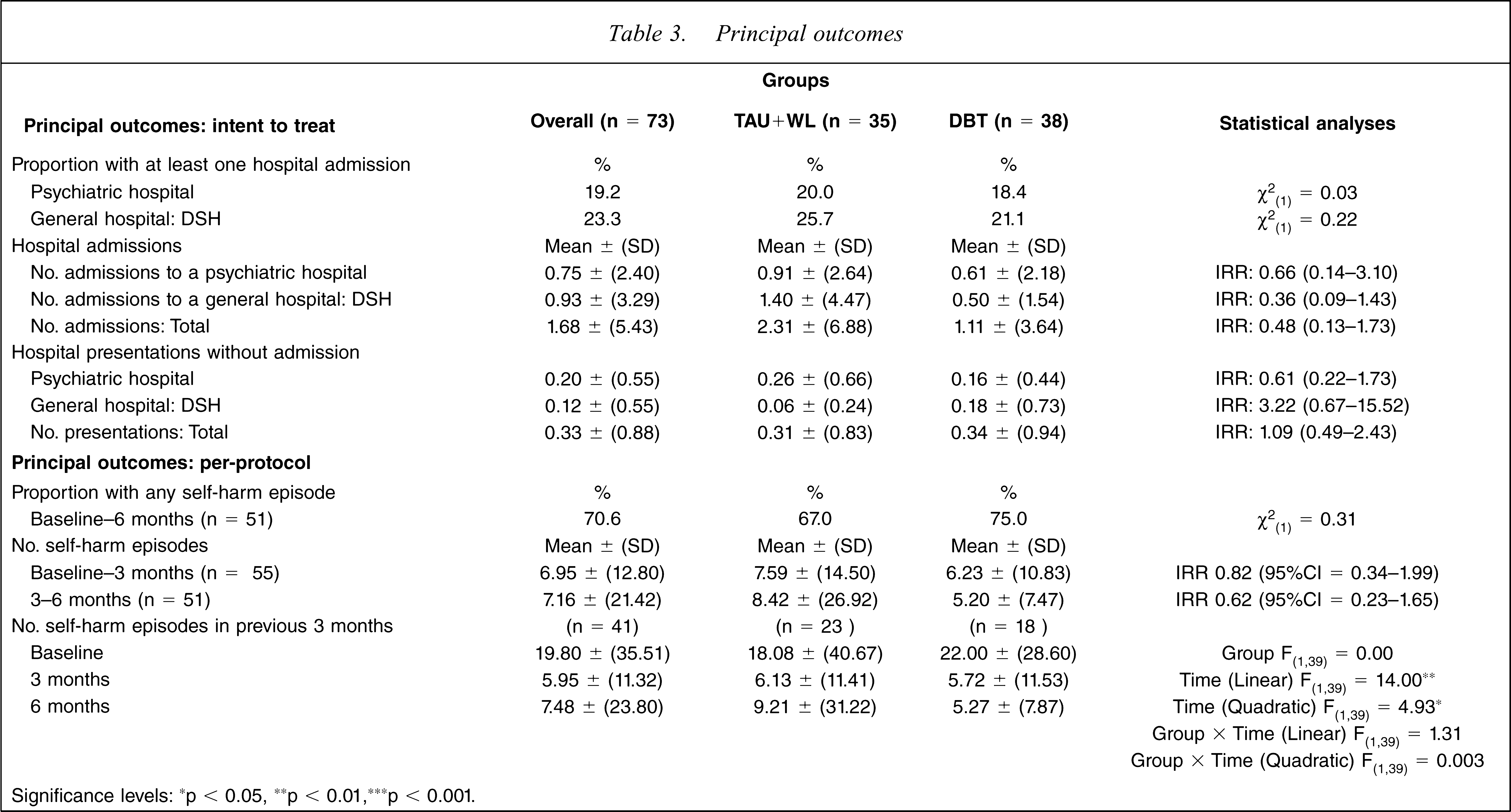
Significance levels: ∗p < 0.05, ∗∗p < 0.01, ∗∗∗p < 0.001.
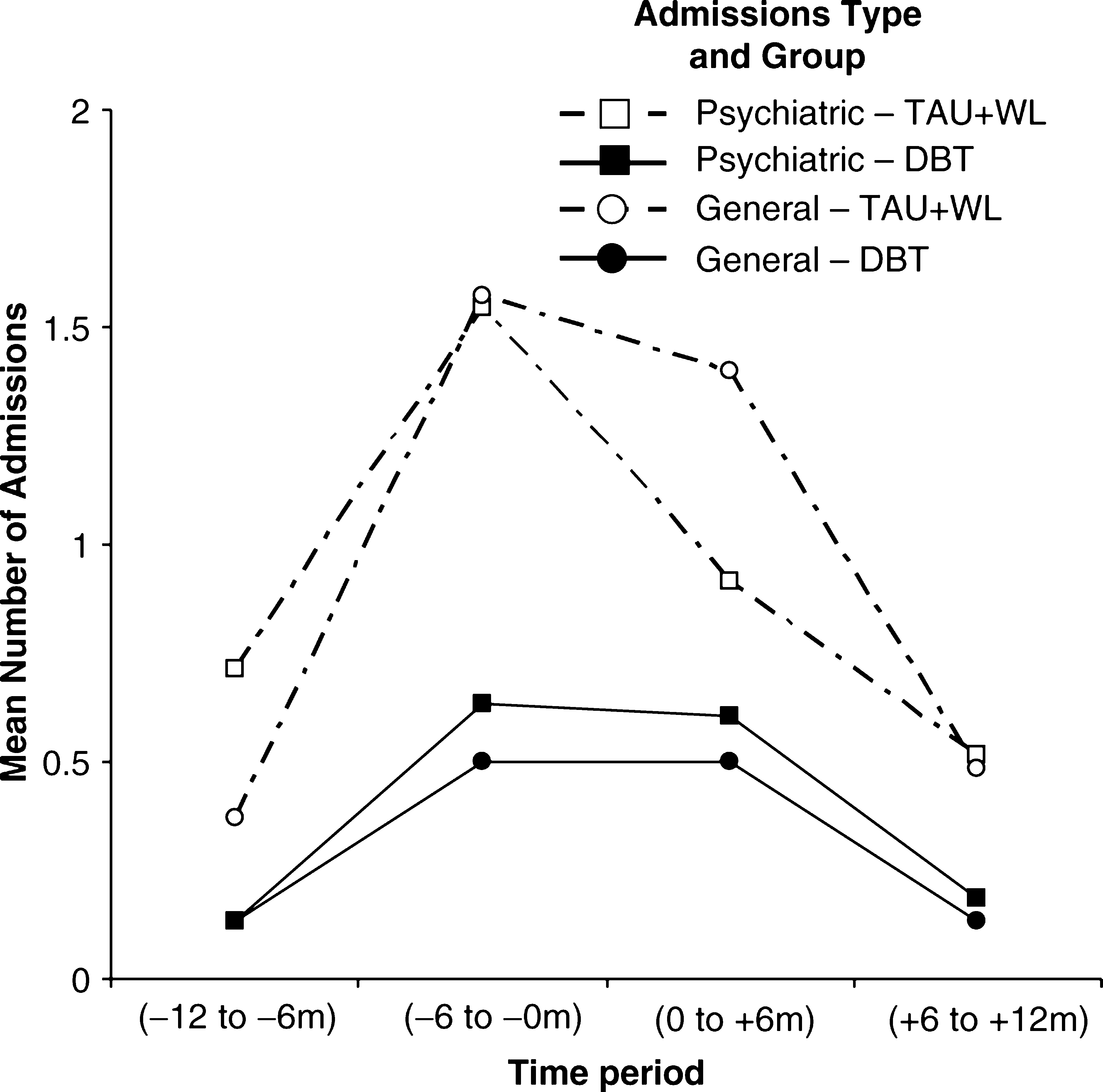
Psychiatric and general hospital admissions during the 12 months before and after study recruitment: (□) psychiatric (treatment as usual waitlist (TAU+ WL)); (▀) psychiatric (Dialectical Behaviour Therapy (DBT); (°) general (TAU+ WL); (•) general (DBT)
The length of stay overall, or the length of stay for those with either type of admission was not significantly different, although the DBT group tended to have shorter lengths of stay. For the 6 months of the study, the mean length of stay overall was as follows: psychiatric hospital for any reason, total = 7.19 ± 27.53 days, control = 9.48 ± 33.63 days, DBT = 5.10 ± 20.62 days (F(1,69) = 0.14); and general hospital for DSH, total = 0.88 ± 2.65 days, control = 1.25 ± 3.54 days, DBT = 0.53 ± 1.38 days (F(1,69)= 0.90). When the analyses were restricted to those who had any hospital admission the mean length of stay was as follows: psychiatric hospital for any reason, total = 37.53 ± 54.5 days, control = 47.43 ± 65.6 days, DBT = 27.64 ± 43.5 days (F(1,10) = 0.69); and general hospital for DSH, total = 3.79 ± 4.47 days, control = 4.88 ± 5.78 days, DBT = 2.56 ± 2.06 days (F(1,13) = 0.17). For the per-protocol analyses, there were no significant differences for the proportion of patients with any DSH episode in 6 months, or for the number of self-harm episodes for the baseline–3 months and 3–6 months periods. There was a significant effect (linear and quadratic) for time in the rANOVA for the number of DSH episodes over the three time periods, but no significant effect for group status.
Table 4 lists the per-protocol results for the secondary outcomes, disability and quality of life. There was no significant effect for group or time in the rANOVA for days spent in bed in the previous month or for days out of role in the previous month. There was a significant beneficial effect for group × time (linear), in favour of DBT for days spent in bed but no significant effect for days out of role. Similarly, for days spent in bed, there was also a significant effect for group (F(1,64.9) = 5.42, p < 0.05) in favour of DBT in the confirmatory mixed-effects analysis.
Secondary outcomes: disability and quality of life
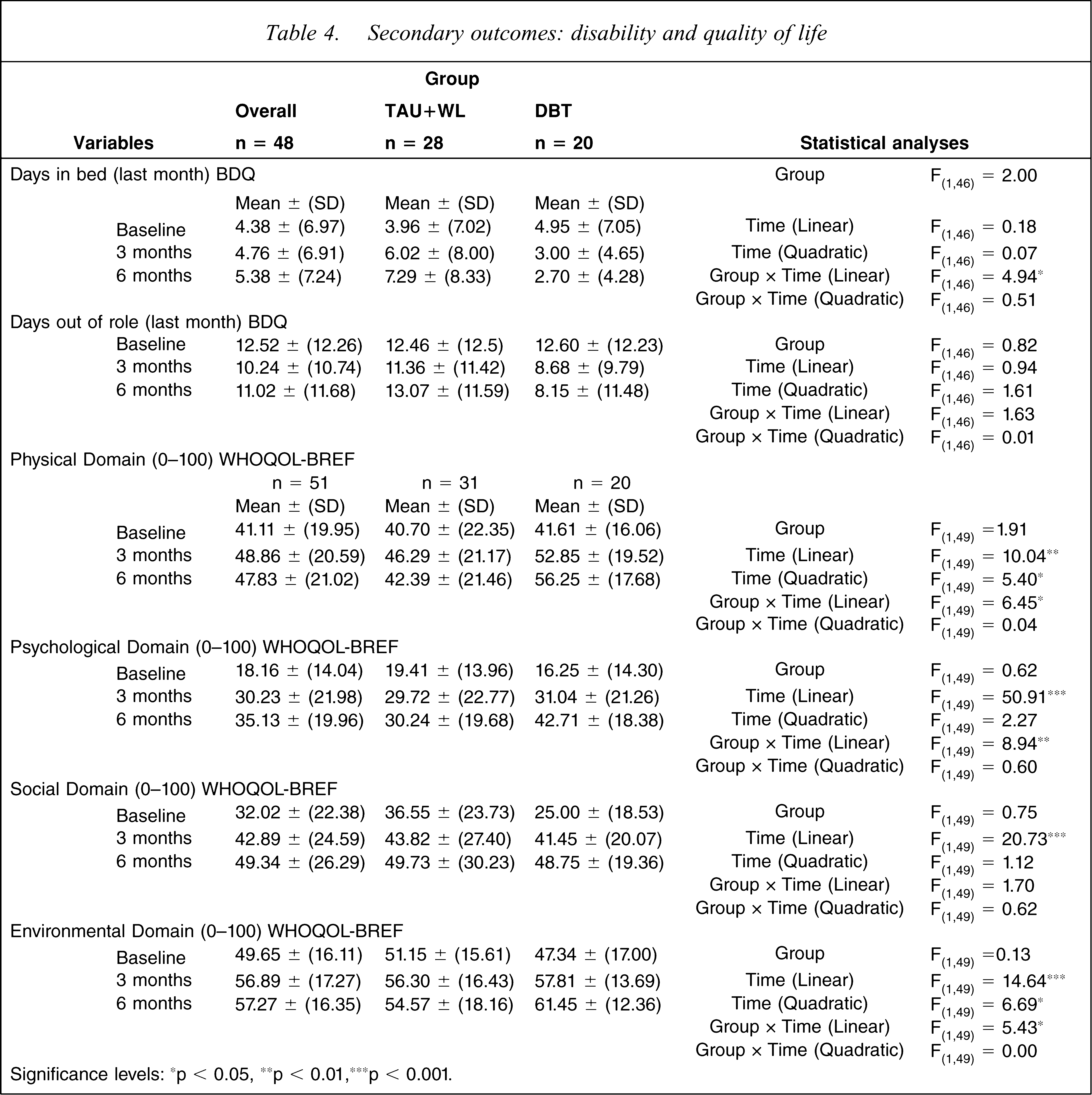
Significance levels: ∗p < 0.05, ∗∗p < 0.01,∗∗∗p < 0.001.
There was a significant beneficial effect for time (linear) and group × time (linear), in favour of DBT, for three of the four domains of quality of life: Physical, Psychological and Environmental. Similarly there was a significant effect for time (F(2,57.2) = 7.56, p < 0.01) and group (F(1,75.6)= 4.58, p < 0.05) for Physical Domain; time (F(2,55.4) = 26.68, p < 0.001) and group × time (F(2,55.4) = 3.28, p < 0.05) for Psychological Domain; but only for time (F(2,56.4) = 8.06, p < 0.01) for Environmental Domain in the confirmatory analyses. There was a significant beneficial effect for time (linear) in the Social Domain but no significant effect for group. Similarly, there was a significant effect only for time (F(2,57.1) = 11.71, p < 0.001) for the Social Domain in the confirmatory analyses.
Discussion
Strengths and weaknesses of the study
This was RCT, using opaque envelope technique, with the main primary outcomes determined by assessors blind to allocation status. These primary outcomes for the intention-to-treat analyses were determined from hospital records and not participant self-report, eliminating the potential for a differential response bias. Participants knew their allocation status but were not told specifically of the outcomes of interest. There were no significant imbalances for the a priori selected demographic or clinical variables at baseline, indicating a successful randomization procedure. The post-hoc pattern of hospitalizations seen in Figure 2, however, suggests a possible imbalance based on general and psychiatric hospitalizations at baseline. Principal analyses were done on an intention-to-treat basis, based on randomization status, with three subjects removed from the TAU+WL group, one because of death soon after randomization and two because of withdrawal of consent after completion of treatment. The statistical techniques used were appropriate to the data analysed [34], in particular the use of either Poisson regression or negative binomial regression when appropriate to analyse event (count) data, which has been only infrequently used before in repetition of DSH studies [35,36]. In the present study the secondary outcomes (disability and quality of life) were determined by participant self-report on various measures and so the losses of participants, particularly from the DBT treatment group in the per-protocol analyses, may limit the internal validity of these secondary outcome results. We also used an alternative analytic model, linear mixed-effect models for repeated measures data, as confirmatory analyses for the secondary outcomes, which strengthens the validity of these results [37].
The current study was powered on the basis of a previously published study [7], which used the repetition of self-reported ‘parasuicide’ as the outcome of interest (DBT 26% vs TAU 60%), which had demonstrated a powerful benefit of 33% absolute risk reduction, 56% relative risk reduction and a number needed to treat of only three (calculated by GC). In the present study two different primary outcomes were used that approximated the self-reported parasuicide outcome in that original study: general hospital admission for DSH, which proved to be relatively infrequent in both the DBT (21%) and TAU+WL (26%) groups; and self-reported DSH, which proved to be relatively frequent in both the DBT (75%) and TAU+WL (67%) groups. We did not have sufficient data from participants to determine whether there was equivalence of treatment hours in the two groups, and so reported benefits in secondary outcomes may be due to differences in therapy hours rather than the specific effects of treatment. The external validity of the study is not known and so generalization from these results to any other populations should be done with caution.
Primary outcomes: DSH and hospitalization
The current study failed to replicate some of the important findings (significant reduction in DSH and reduction in psychiatric hospitalization) from other studies [7,10]. Although there was improvement in both groups over time, there was no significant differential reduction in general hospital-treated DSH, psychiatric hospitalization or self-reported DSH, for either the binary outcome or event rates.
There are several possible explanations as to why DBT was not effective in this study: regression to background (pre-baseline) levels, the Hawthorne effect whereby both groups improved because of the effect of being in a study, the potentially powerful effect of being in a 6 month TAU+WL group for DBT for the control condition, beneficial effects of the TAU condition available in the Hunter region, modifications to standard DBT (including the 6 month duration of DBT, after-hours telephone contact by roster of individual therapists), the possible inferiority of training of DBT therapists to that of those in other studies or inferior adherence to the DBT methods despite adequate training, and methodological differences (e.g. the use of hospital-treated DSH measured by hospital records as a primary outcome or possible differences in the population used in the study).
In the present study the duration for comparison was only 6 months, while the original Linehan et al. study was of 12 months duration [7], and the original Bateman and Fonagy study was of 18 months duration [6], so it could be argued that the current study was too brief in duration of treatment comparisons to demonstrate benefits in terms of DSH or hospitalization for BPD patients. We were aware of this argument during the planning of the current study but believed that a close examination of these previous studies indicated that improvement occurred before 6 months of treatment had elapsed. Linehan et al. examined both number of parasuicidal acts and proportion of subjects with any episode of parasuicide in three time periods: 0–4 months, 4–8 months and 8–12 months, reporting significant differences in favour of DBT for all three time periods for reduction in the number of parasuicidal acts, and for two time periods (0–4 months and 8–12 months) for the proportion of subjects with at least one parasuicidal act in the period. Linehan et al. also examined median psychiatric inpatient days for the same three time periods, reporting significant benefits in favour of DBT only for the 0–4 month and 8–12 month periods, but showing no difference in the proportion with at least one admission in the full 12 month period. [7]. Similarly, Bateman and Fonagy also examined two primary outcomes for three time periods: 0–6 months, 6–12 months and 12–18 months, reporting significantly reduced number of suicide attempts for all three time periods and reduced self-mutilating behaviours for two time periods (6–12 months and 12–18 months) [6]. In the present study, after 6 months the proportions of patients with any episode of DSH were already high in both groups and so a further period of study would have been very unlikely to result in a significant difference being found in favour of DBT or TAU+WL. The mean number of DSH events, however, was non-significantly lower in the DBT group for both the 0–3 month and 3–6 month periods, and so it may have been possible that the 6 month duration of comparison may have been too short to observe an emerging difference in favour of the DBT group. Similarly, hospitalization by proportions and by event rates were also non-significantly in favour of DBT, so the 6 month duration of comparison may have missed emerging differences in favour of DBT.
In considering other studies, a reduction in parasuicide and suicide attempt has been reported in two studies using DBT at the University of Washington [7,10], while another team at the University of Amsterdam reported reduction in self-mutilation but not suicidal behaviour [11]. One underpowered study from Duke University reported significant decreases in suicidal ideation, but no significant reduction in number of parasuicide acts or number of hospitalizations [15]. Two other small-samplesize studies from the University of Washington on drug-dependent women with BPD [19] and opioid-dependent women, showed no difference in parasuicide [20].
The current study found that the 6 month rate of hospital-treated DSH in the DBT group (21%) was very similar to the 12 month (26%) and 24 month (23%) rates for self-report of parasuicide in the USA [7,10]. The 6 month rate of self-reported DSH in the present study (DBT 75%, TAU+WL 67%), however, was much higher than the equivalent parasuicide rates (DBT 26%, TAU 60% [7] and DBT 21%, expert control 46% [10]). Later studies separated suicidal behaviours into two outcomes, suicide attempts and non-suicidal self-injury [10] or suicidal behaviours and self-mutilation [11], making direct comparison with the current study difficult. The second Linehan et al. study (DBT vs treatment by expert control) showed a significant reduction in suicide attempts in favour of DBT, while both treatments were associated with a reduction in non-suicidal self-injury, meaning no significant difference in non-suicidal self-injury [10]. A 12 month RCT in Amsterdam comparing DBT to TAU found no difference in the frequency of suicidal behaviours (threats, preparation for attempts and attempts) nor the proportion with suicide attempt, but did find a difference in self-mutilating behaviours for the time × treatment condition and a reduction in the proportion with any self-mutilating behaviour in the 6–12 month period [11].
The present study found reductions in psychiatric hospitalization for both groups over time but again no significant benefit in favour of DBT for the binary outcome, the mean event rate or the mean length of stay for those with an admission at the end-point of the trial. In the original DBT trial there was a demonstrated benefit for median days of psychiatric hospitalization after 12 months, but no difference in proportions for any psychiatric admission or for median number of admission per person [7]. In the later DBT trial, using a mixed-effect ANOVA, significantly fewer DBT subjects had any psychiatric admissions after the year 1 (DBT 20% vs expert control 49%) and year 2 (DBT 23% vs expert control 24%) outcomes were combined [10].
In the present study there was one death by suicide in the TAU+WL control group, while in studies from the University of Washington there was one death by suicide in the DBT group [7] and one death in the treatment by expert control group not attributed to suicide but to ‘the cumulative effects of previous suicide attempts’ [10].
Secondary outcomes: disability and quality of life
Life-threatening behaviours and therapy-interfering behaviours are primary targets in DBT (stage 1 target: ‘out of control behaviours’) followed by quality of life-interfering behaviours and increasing behavioural skills, which are also stage 1 targets. Other quality of life and disability issues may also be dealt with at a later stage of therapy (stage 2 target: reducing ‘quiet desperation’). Improvements in disability and quality of life, however, were found in the present study even though there was no differential improvement in DSH and psychiatric hospitalization.
Although there was no significant effect for one measure of overall disability (days out of role), there was a significant benefit for DBT for the more specific disability measure of days spent in bed, an absolute difference of 4 days per month per person, which we consider to be clinically significant. With 81% of participants either not in the labour force or unemployed, it may be difficult to interpret the meaning of the ‘days out of role’ result derived from the BDQ. Nonetheless, with an average of 11 days out of role per month the overall level of disability was high, which was not surprising for this clinical population.
Both groups had substantially lower scores on quality of life measures than the Australian population norms: Physical health domain = 73.5 ± 18.1, Psychological well-being = 70.6 ± 14.0, Social relationships = 71.5 ± 18.2 and Environment domain = 75.1 ± 13.0 [38]. Three of the four quality of life domains, however, showed significant improvement over time for the DBT condition in the present study (group × time interaction), while both groups improved over time for the fourth domain (Social). The magnitude of these improvements in quality of life was substantial and considered to be clinically significant, although the final scores for the Psychological domain still fell short of community population norms by more than one standard deviation, suggesting considerable residual psychological distress or dysfunction.
These improvements in disability and quality of life have only rarely been demonstrated or evaluated in RCTs involving subjects with BPD, again making comparison with the present study difficult. One study of drug-dependent women with BPD showed overall improvement but no differences in social or global adjustment during treatment or at 12 month follow up, with a significantly lower score in the DBT group at 16 month follow up [19]. A later study of opioid-dependent women showed overall improvement but no benefit in social or global adjustment at any time point [20].
Conclusion
For the principal outcomes, the present study found no differences in self-reported DSH, general hospital-treated DSH, psychiatric hospitalization or length of stay in general hospital or psychiatric hospital, although there was considerable improvement in both the DBT and the TAU+WL control groups from baseline levels. Even though the present study did not replicate the benefits of reduction in DSH behaviour and hospital admissions found in other studies [7,10], several secondary outcomes (disability and quality of life) showed clinically significant benefits in favour of DBT, in keeping with the theoretical predictions for DBT. BPD is a common diagnosis in public psychiatric services and the present study suggests that using DBT in a team approach, very similar to the original Linehan et al. treatment model, might produce meaningful improvement in the lives of these patients.
Footnotes
Acknowledgements
Our thanks go to several people for their contributions to the Hunter DBT Project: Dr Chris Hayes, University of Newcastle and Ms Susan Burgoyne as investigators in the initial project development; to Peter Sneesby as Masters of Clinical Psychology student, University of Newcastle, assisting with the initial phases of data collection; to Natalia Carter and Gillian Maddock who helped with data extraction from the clinical records; to Dr Kerrie Clover, University of Newcastle, for assistance with instrument scoring and data cleaning; and to Ben Britton who assisted with linear mixed effect models. Our thanks also go to all the staff who contributed clinical services: individual therapists Danielle Adams, Marianne Ayre, Dr Nick Bendit, Susan Burgoyne, Jennifer Evans, Dr Howard Johnson, Jennifer Koorey, Natalie McCall, Chris McCrory, Jane Taylor and Chris Willcox; and skills trainers Marianne Ayre, Dr Nick Bendit, Linda Bragg, Michael Currie, Annabel Kelly, Michelle Meyer, Ruth Spence and Don Stewart; and also to Dr Neil Port and Dr Howard Johnson, who undertook the baseline clinical interviews. We also appreciated the input from external honorary consultants Dr Marsha Linehan and Dr Kelly Koerner, University of Washington, USA; and several episodes of supplementary training of DBT therapists by Dr Kate Comtois and Dr Kelly Koerner, University of Washington, USA. Finally, without the support and clinical leadership of Dr Howard Johnson, Director of the Centre for Psychotherapy, this study would not have been possible.
