Abstract
The most definitive role of fluorodeoxyglucose (FDG)-PET/computed tomography (CT) at present is surveillance and detecting recurrence in patients who have completed primary therapy but demonstrate a rising serum tumor marker (e.g., CA–125 levels). In this scenario, PET/CT demonstrates high sensitivity and accuracy in detecting lesions that are otherwise challenging, and appears superior (with less interobserver variability) compared with CT alone. Despite the fact that peritoneal deposits may be missed by PET/CT, the overall performance is better than CT alone, FDG-PET does not play a significant additional role in the primary diagnosis of ovarian cancers; however, the role of combined PET/CT modality has recently begun to be re-explored for initial disease staging, particularly because PET/CT can pick up small unsuspected lesions and thereby provide a better disease assessment of the whole body in a single examination, The baseline PET/CT also subserves an important role for future monitoring of therapy response. Therapy monitoring by PET could help to optimize neoadjuvant therapy protocols and to avoid ineffective therapy in nonresponders early in its course, although PET/CT has cost-effectiveness issues that need further evaluation. The prognostic value of FDG-PET/CT has been investigated in the following areas: in the preoperative setting to predict optimal cytoreduction; to assess the value of a positive FDG-PET following primary surgery; and when employed as a replacement for second-look laparotomy following completion of primary surgery and chemotherapy. The data, although promising, are still sparse in all the three domains for a definite recommendation.
Keywords
Ovarian cancer is the sixth most common cancer among women [1,2]. Worldwide there are more than 200,000 new cases of ovarian cancer each year, accounting for around 4% of all cancers diagnosed in women [3]. A woman's risk of developing cancer of the ovaries by the age of 75 years varies between countries, ranging from 0.5 to 1.6%, corresponding to an age-standardized rate of five to 14 cases per year in 100,000 women. In Europe, ovarian cancer is the leading cause of gynecological cancer death; just over a third of women are alive 5 years after diagnosis [4], largely because most women with ovarian cancer present at an advanced stage when surgical cure is usually impossible [5].
The International Federation of Obstetricians and Gynecologists (FIGO) staging is used to describe the spread of the disease (
Management of carcinoma of the ovary involves evaluation and primary staging, followed by primary debulking surgery followed by adjuvant chemotherapy in the early stages, while chemotherapy (neoadjuvant) followed by interval debulking surgery in advanced disease with variations depending on the his to-pathological grade and the general condition of the patient [1].
Preoperative staging is done by imaging followed by surgical staging at laparotomy. Imaging by ultrasonography or computed tomography (CT)/MRI is widely acceptable for carcinoma of the ovary. Over the past few years, especially the past decade, with the advent of functional imaging using PET with 18F-fluorodeoxyglucose (FDG) imaging, diagnostic imaging in oncology has undergone a paradigm shift. With the advent of the routine clinical use of FDG-PET in the early nineties for staging and follow-up of various cancers, we have now arrived at the time of advanced molecular imaging using PET/CT, which combines both functional and anatomical information. Based on the increasing body of literature in the last few years, we now place PET/CT at a certain point in the management of ovarian carcinomas.
Description of the International Federation of Obstetricians and Gynecologists staging of ovarian cancer.
IA. Disease confined to one ovary with no capsular involvement. Peritoneal washings/cytology negative
IB. Disease confined to both ovaries with no capsular involvement. Peritoneal washings/cytology negative
IC. Disease confined to the ovary/ovaries but ovarian capsular involved or cyst rupture
IIA. Extension to uterus or fallopian tubes
IIB. Extension to other pelvic tissues
IIC. As for IIA or IIB but one or both ovaries have ruptured capsule or surface tumor; malignant ascites or positive peritoneal washings
IIIA. Histologically confirmed microscopic seeding of abdominal peritoneal surfaces and negative retroperitoneal lymph nodes
IIIB. Histologically confirmed implants of abdominal peritoneal surfaces less than 2 cm and negative retroperitoneal lymph nodes
IIIC. Histologically confirmed implants of abdominal peritoneal surfaces greater than 2 cm or positive retroperitoneal lymph nodes
IV. Distant metastases (including liver parenchyma/positive pleural fluid cytology)
Data taken from [6].
Ovarian cancers are usually detected at advanced stages. They tend to recur despite adequate surgery and chemotherapy. Recurrent ovarian malignancies are difficult to detect and even if detected the prognosis is not very favorable in advanced disease with poor 5-year survival rates [4]. Despite these factors, detection of early stage disease, early detection of recurrence following completion of therapy and response to therapy are some of the important situations where PET/CT can play an important role for clinical decision making.
With this background, in this review we aim to discuss the impact of PET/CT in the management of ovarian carcinomas.
Basics of FDG-PET/CT imaging in oncology
PET imaging involves the injection of the tracer 18F-FDG, which is a glucose analog [7]. This is followed by imaging in a PET scanner with or without CT. However, most PET scanners today have an integrated CT component, which is useful for attenuation correction as well as anatomical correlation with coregistration. Organs show FDG uptake, which is dependant on the glucose metabolic status of the cells [7]. Glucose uptake is increased manifolds in malignant cells which forms the basis of increased FDG uptake and functional imaging with FDG-PET [7].
PET/CT in physiological conditions of the ovary
In the ovaries, a baseline FDG uptake and a spectrum of cyclical physiological and benign FDG uptake have to be considered in order to detect or diagnose malignant disease. There are known confounding factors of benign/physiological uptake by the ovaries in the various phases of the menstrual cycle [8–11]; these need to be taken care of when PET /CT scans are performed for the diagnosis of ovarian carcinoma (TABLE 1). On FDG-PET imaging, the ovaries are prominent in the mid-cycle, with focal uptake located in the left or right side superior and posterior to the urinary bladder. Patients with irregular cycles have a low probability of intense uptake in the ovaries and this should be viewed with high suspicion. Corresponding CT correlation should be done in suspicious cases. Characteristic CT appearance is enhancing cyst and no lymphadenopathy.
Physiological uptake patterns of the ovaries on a fluorodeoxyglucose-PET scan.
CT: Computed tomography; FDG: Fluorodeoxyglucose.
It is imperative that FDG-PET/CT scan for evaluation of ovarian/pelvic malignancies is performed in the postmenstrual phase in order to avoid ovarian as well as endometrial activity, which increases in the mid-cycle and menstrual phases, respectively. In postmenopausal women any ovarian uptake should be viewed with high suspicion.
PET/CT in the diagnosis & initial staging of ovarian cancers
Barring a few reports [12–14], it is evident that FDG-PET only has no incremental role with regards to initial diagnosis of suspicious pelvic masses (
Fluorodeoxyglucose-PET in the diagnosis of malignant ovarian lesions.
FDG: Fluorodeoxyglucose; US: Ultrasound.
With the advent of FDG-PET/CT in recent years, the role of PET imaging is being re-explored. PET/CT has been proven to provide incremental information in comparison with CT/MRI only and may play a role in the preoperative staging of carcinoma of the ovary (

PET/computed tomography in initial staging of ovarian cancers.
CT: Computed tomography; TVUS: Transvaginal ultrasound; US: Ultrasound.
Overall, PET/CT has a better lesion detection rate than CT or MRI alone, better efficiency to differentiate benign from malignant lesions – except for borderline lesions - and to pick up other unexpected tumors. Thus, the incremental value of PET/CT has been well proven in initial staging workup although surgery still remains the gold standard.
PET/CT in disease prognostication
PET/CT has been found to be of some incremental value in prognostication and prediction of disease [26–32] after primary treatment, although it does not stand a very strong hold in this area (
Incremental role of PET or PET/computed tomography in prognostication of ovarian cancers.
CT: Computed tomography; LBMI: Large bowel mesenteric implants; SLL: Second-look laparotomy.
PET/CT in detecting disease recurrence of ovarian carcinoma
The highest impact of PET/CT in ovarian cancers is in the detection of recurrence as this is one of the most common malignancies to recur despite adequate therapy (


PET and PET/computed tomography in recurrent ovarian cancers.
CT: Computed tomography; FDG: Fluorodeoxyglucose; FIGO: International Federation of Obstetricians and Gynecologists; MIT: Morphologic imaging tests; US: Ultrasound; USG: Ultrasonography.
In fact, this is one definitive clinical indication that has been shown to be cost-effective as well. The use of PET/CT in the group of patients with suspected recurrent disease is cost-effective and can be allowed to redirect the clinical management of patients towards more appropriate therapeutic choices [51].
PET/CT in peritoneal metastases
In patients with metastatic ovarian carcinoma, disease sensitivity of both 18F-FDG-PET and CT for the detection of peritoneal metastases is low; however, with regards to better specificity of FDG-PET, it is preferred for evaluation of residual/recurrent disease with better sensitivity for the retroperitoneal region than the intraperitoneal region (
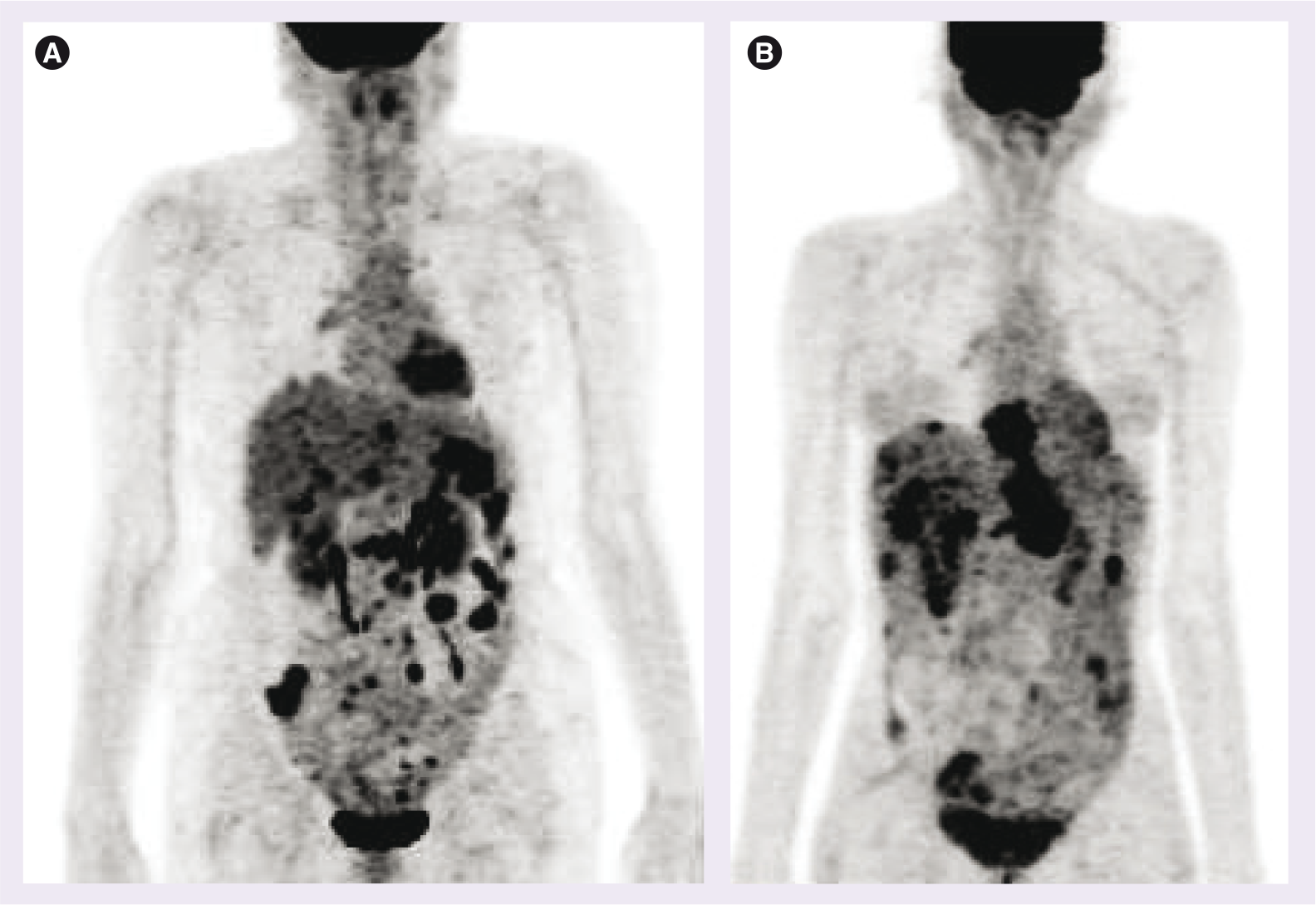
Performance of PET has been found to be a useful tool for the detection of the peritoneal deposits [53–56]. This is due to two factors, in particular: detection of peritoneal carcinomatosis is difficult with CT due to poor sensitivity. Detection with peritoneal biopsy is also fraught with high incidence of sampling errors. Two distinct abnormal scintigraphic patterns of focal and uniform 18F-FDG uptake corresponding to nodular and diffuse peritoneal disease on pathologic examination have been observed for peritoneal carcinomatosis on FDG-PET [57].
PET in assessing response to therapy
FDG-PET uptake in the tumor prior to therapy and after neoadjuvant chemotherapy or chemo-radiotherapy in advanced ovarian cancers has been studied [58,59]. Standardized uptake value (SUV)-based assessment of response has been found to be accurate; however, the role of PET in the context of patient management and the cost–effectiveness of this approach needs further evaluation [59,60]. Therapy monitoring by PET could help to optimize neoadjuvant therapy protocols and to avoid ineffective preoperative therapy in nonresponders, but this has to be proven in a larger number of patients and in different neoadjuvant settings such as chemotherapy, radiation therapy, hormone therapy or a combination of these [61]. The results of PET/CT in this situation could also translate into prognostication of the disease. There is relatively less defined course in terms of therapeutic intervention with positive PET/CT results in this clinical setting when compared with other malignancies. This is one of the main reasons why PET/CT is not yet popular in this area [60].
PET in metastatic ovarian cancer & in the setting of rising CA-125 levels
Ovarian cancer can spread locally within the pelvis with subsequent spread within the peritoneal cavity to the rest of the abdomen. Tumor spread can also occur via lymphatics and hematogenously. Lymphadenopathy can be seen in the inguinal, pelvic and para-aortic regions. Hematogenous sites of spread include the liver and lung [62].
Distant metastasis is also seen in the liver, pleura, mediastinum and supraclavicular lymph nodes (

Although we have discussed the role of PET/CT in detecting recurrent/metastatic disease, the area of rising CA-125 levels (tumor markers) with normal anatomical imaging (CT/MRI) deserves special mention (

Overall, better lesion detection in rising tumor markers has been seen with PET/CT than with CT alone [35,40].
Other issues: differentiation of benign versus malignant lesions in ovarian tumor imaging
This is an extension of the initial point discussed under the section, ‘PET/CT in the diagnosis & initial staging of ovarian cancers.‘ Hypermetabolic ovarian lesions, more intense than the physiological hepatic uptake have been considered positive for malignancy in most studies, although in our experience significant overlap can be observed in practice. A cut-off value of SUV greater than or equal to three has been seen to be highly suggestive of malignancy in some studies [62]. SUVs ranging from 3 to 27 have been seen in malignant lesions proven by histopathology [65]. The SUV cut-off-based diagnosis, however, would require more validation. Lesions within SUV of less than two have been considered to be benign by some authorities even if other imaging modalities are positive, for example in borderline ovarian tumors [66]. We believe that more data with PET/CT imaging needs to be accrued in this area for a definitive conclusion.
Conclusion
Theoretically, fusing functional and anatomical information can be of significant benefit for the detection of abdominal lesions such as that in ovarian cancer. Hence, this modality needs to be utilized to its greatest potential in this malignancy. At present, PET/CT does not play a significant additional role in the primary diagnosis of ovarian cancers and holds a position similar to transvaginal ultrasound/CT for this purpose. Primary staging of diagnosed primary ovarian tumors can be better staged using PET/CT before any form of treatment as it adds valuable information regarding the number and extent of lesions. The monitoring of therapy response with PET/CT has cost-effectiveness issues, which need further evaluation. The most definite role of PET/CT is in the surveillance of patients who have received primary therapy with rising CA-125 levels or even normal CA-125 levels with high clinical suspicion. It does perform relatively poorly in peritoneal carcinomatosis, but the overall performance is better than CT alone. PET/CT can pick up unsuspected lesions whether nodal, in the peritoneum or subcapsular liver disease.
Future perspective
The wide application of current generation PET/CT scanners with better resolution in routine clinics will likely increase the role and reliability of this imaging modality in this group of tumors. We speculate the areas in which PET/CT may develop a role in the clinical management of ovarian carcinoma in the future are: as a promising technique in monitoring response to therapy; initial staging of the disease (particularly the metastatic disease burden) with better accuracy that would guide the correct therapeutic strategy; and disease prognostification especially as a replacement of second-look laparotomy following completion of primary therapy.
In these areas, presently this is not used in routine clinics but might change with better results with the application of combined structure-function approach and better quantification techniques. This would, however, be determined by results from more clinical studies, evidence based approach and the availability of newer salvage treatment modalities.
Executive summary
Ovarian cancers being the sixth most common cancer among women with notoriety to being detected at advanced stages and to recur despite adequate treatment, makes them a challenging disease.
Evaluation with primary staging (according to the International Federation of Obstetricians and Gynecologists), followed by chemotherapy and surgery is the usual course of management of these malignancies.
Ovaries show physiologically increased uptake of 18F-fluorodeoxyglucose (FDG) in midcycle of menstruation, which does not happen in patients with irregular cycles or postmenopausal women and thus should be reviewed with suspicion in such patients.
It is thus imperative to image these malignancies in the postmenstrual phase.
The transvaginal ultrasound and computed tomography (CT)/MRI have been the most popular modalities for diagnosis of the primary and initial staging in contrast to FDG-PET only.
With the advent of FDG-PET/CT, it is being observed that fusion imaging does provide incremental information in contrast to only anatomical imaging for initial disease staging as a whole-body modality (especially with regard to metastatic disease burden).
PET/CT has better lesion detection rates and better differentiation of benign from malignant and the probability to pick up unexpected tumors.
Primary aim is to see if PET/CT could replace second-look laparotomy for which Phase III randomized trials are ongoing and results require evaluation.
Ovarian cancers could spread or recur locally within the pelvis whereas metastatic involvement includes peritoneal cavity spread, lymphatic spread to inguinal, pelvic and para-aortic nodes or hematogenous spread to liver and lungs.
PET/CT shows highest impact in this area where it demonstrates higher sensitivity and accuracy in detecting disease involvement in areas like nodal, peritoneal and subcapsular liver disease, which are challenging otherwise with conventional imaging. The assessment of whole-body status is a distinct advantage of this modality in the detection of distant metastasis.
Rising CA-125 with normal anatomical imaging thus forms a definitive indication for FDG-PET/CT imaging. The application results in change in clinical management of over a third of such patients.
Though both PET and CT perform low in this area, PET-CT has been found to be more useful than CT alone and, hence, should be preferred compared with anatomical imaging alone.
FDG-PET/CT shows two distinct patterns of uptake (i.e., focal and uniform uptake for nodular and diffuse peritoneal disease, respectively).
Standardized uptake value based response monitoring has been found to be accurate early in the course of therapy; however, there are cost-effectiveness issues in this area.
Always a challenge in FDG-PET imaging; validation with more studies needs to be continued. Standardized uptake values have been used in most studies and a value of three or more have been suggested to be highly suggestive of malignancy; however, this requires to be critically determined. Combined PET-CT and dual time point imaging may help.
Footnotes
The authors have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants or patents received or pending, or royalties.
No writing assistance was utilized in the production of this manuscript.
