Abstract
High-altitude pulmonary edema (HAPE) is a potentially life-threatening condition that is rapidly and definitively treated by descent. We report a case of worsening HAPE, presenting more than 18 hours after descent to sea level. The patient was treated with diuretics, calcium channel blockers, and oxygen and improved during a 24-hour observation period. To our knowledge, this is the first reported case of HAPE symptoms increasing after descent from altitude.
Introduction
High-altitude pulmonary edema (HAPE) is a well-documented, life-threatening process that usually occurs in young, healthy individuals who rapidly ascend to altitudes higher than 2500 m and engage in vigorous exercise. Symptoms occur within 24 to 72 hours, beginning with dyspnea, decreased exercise tolerance, and/or chest tightness, and progressing rapidly to pulmonary edema and frank respiratory distress. 1
Field treatment options include oxygen, nifedipine, and inhaled β-agonists, but descent provides the quickest and definitive recovery. Although complete recovery can take days, rapid improvement is usually seen at lower altitudes. 2
The case presented here describes progressive symptoms of pulmonary edema, approximately 18 hours after descent to sea level. To our knowledge, there is no previous description of such a later manifestation of worsening HAPE symptoms.
Case Report
A 25-year old, male, experienced mountaineer with no previous medical history of HAPE presented to our emergency department with complaints of shortness of breath, coughing, and hemoptysis. The day before presentation, he had reached the summit of Mount Rainier (4392 m) from Camp Schurman over Emmons Glacier, and at the top, began to feel more short of breath than expected, coincident with development of a mild headache. He had no change in mental status and no ataxia. Concerned that he was developing mild hypothermia, he rested at the summit to warm up in a sleeping bag and his symptoms slightly improved. During unassisted descent, his headache and dyspnea increased, with one episode of emesis, but he returned to his home in Seattle, Washington (14 m) without further events during approximately 10 hours. He rested but noticed no improvement during the remainder of the day and went to sleep, assuming that he was simply fatigued from the climb.
Awakening approximately 18 hours after descent, the patient had significantly worsened respiratory symptoms. He was short of breath even at rest, with wheezing and a wet cough, and had multiple episodes of pink, frothy sputum. He had no chest pain, fever, extremity edema, headache, or mental status changes. He presented to our emergency department for evaluation.
Before the ascent, the patient was in his usual state of good health and described no antecedent illness. He had no history of elevation-related illness or any risk factors for coronary artery or thromboembolic disease. The patient took no medications; specifically, he was not taking prophylactic acetazolamide, nifedipine, ginkgo, or dexamethasone before or during the ascent. He did not use alcohol, drugs, or tobacco.
Physical examination revealed a fit, seemingly healthy young man in moderate respiratory distress, speaking in 4 to 5 word sentences. His vital signs included: blood pressure 146/92, pulse 108, temperature 36.7°C, respiratory rate 40, and oxygen saturation 88% to 90% on room air. Neck exam showed no jugular venous distension. Lung exam demonstrated bilateral crackles three fourths of the way to the apices. Heart exam was within normal limits, except for tachycardia. Extremities showed no edema. The neurologic exam was within normal limits, with a Glasgow Coma Score of 15.
The patient was immediately placed on continuous electrocardiographic monitoring and oxygen by nasal cannula at 4 L/min−1, raising his oxygen saturations to 96%. An electrocardiogram showed only sinus tachycardia. Chest radiograph revealed significant bilateral pulmonary edema and normal heart size (see the Figure). Complete blood count included a slightly elevated white blood cell count of 10 700 μL−1 and a hematocrit of 51%. Electrolytes, liver enzymes, and creatinine levels were normal. His creatinine kinase level was elevated, at 1196 U/L−1; but his troponin-I level was negative, at 0.02 ng/mL−1. His B-natriuretic peptide level was negative at 45 pg/mL−1. D-dimer assay results were negative.
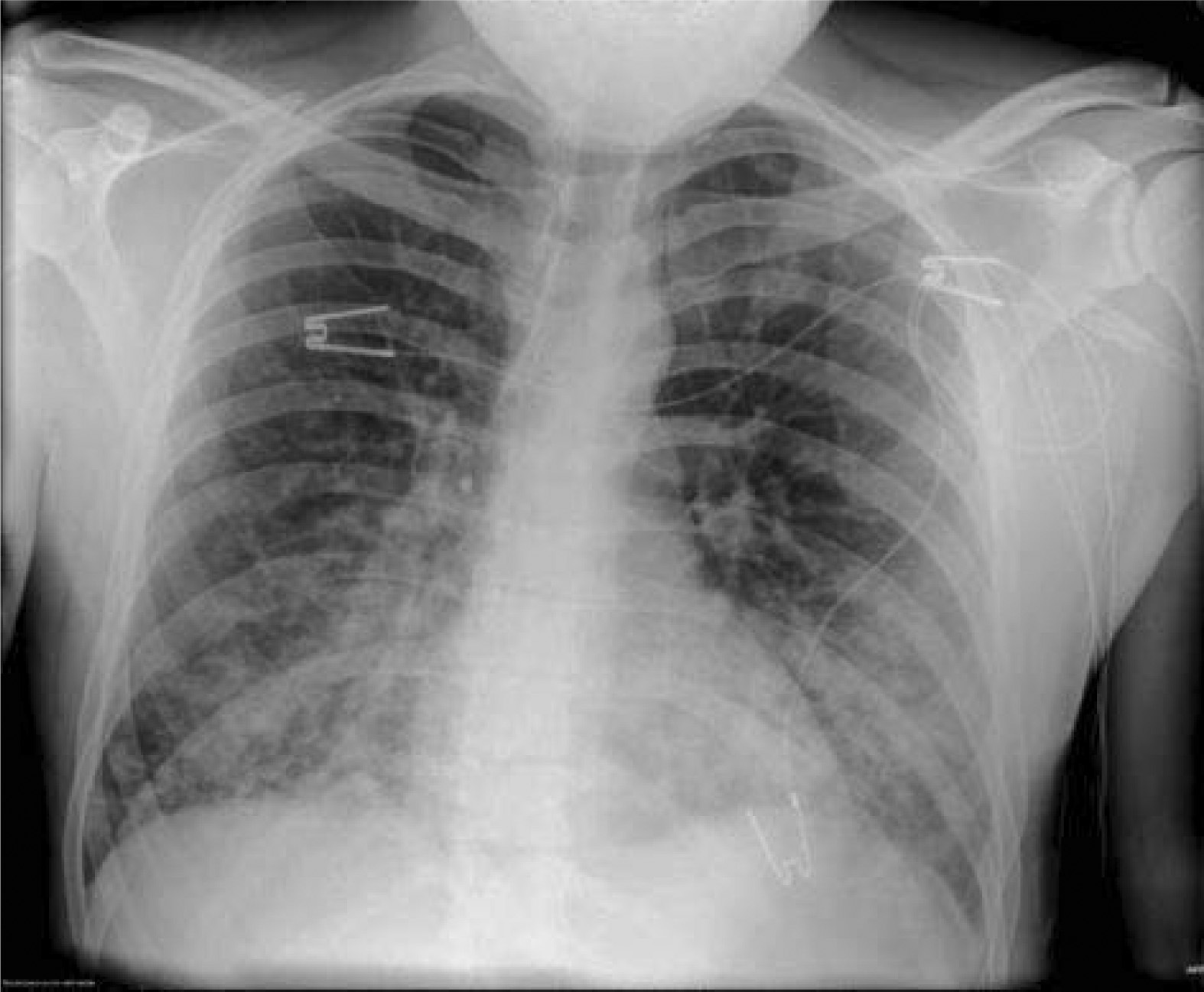
Chest radiograph at presentation.
The patient was treated with 20 mg of furosemide and 2 mg of morphine intravenously with minimal relief or change in his lung examination. A nicardipine drip was started at 5 mg/h−1 with improvement of symptoms. After 2 hours, the patient's lung exam had improved but he continued to saturate in the low 90%s at rest on room air. The nicardipine drip was discontinued and he was admitted to the observation unit for a 24-hour stay on 2 L of oxygen by nasal cannula.
Given the patient's uncommon presentation, an echocardiogram was performed. He had normal left ventricular function with an ejection fraction greater than 65%. There was mild concentric left ventricular hypertrophy consistent with the patient's athleticism. The right ventricle and all valves were normal and there was no pericardial effusion. Pulmonary artery pressures were not measured.
Twenty-four hours after admission the patient felt dramatically improved, was saturating 98% on room air, and had a nearly normal lung exam with only slight crackles bilaterally at the bases.
At follow-up after 2 months, the patient was completely asymptomatic and had had no further episodes; he had climbed once to altitude during that period, reaching 2865 m.
Discussion
HAPE is a form of noncardiogenic pulmonary edema that is caused at least in part by pulmonary hypertension leading to vascular leaking. 3 Many theories have been suggested for the cause of increased pulmonary pressures; although the best evidence supports uneven hypoxic pulmonary vasoconstriction as the primary trigger.4,5 Endothelial dysfunction, 6 inappropriate sympathetic activation, 7 inflammation, 8 and poor alveolar-fluid clearance 9 may also play a role.
HAPE may be more common in men and young people and is exacerbated by extremes of exertion and cold.10,11 Incidence is difficult to determine, although most estimates are 2% to 3% or less, 2 increasing with altitude and rate of ascent.12,13 Other risk factors include previous history of HAPE, 12 and preexisting pulmonary hypertension. 14
Mount Rainier is a high-elevation, frequently summited mountain in the Pacific Northwest that provides a fertile environment for high-altitude illness. Most climbers drive from sea level to begin the climb near 1500 m, reaching Camp Muir (3078 m) or Camp Schurman (2877 m), where they sleep for a few hours. Awakening in the very early hours of the morning, the final ascent brings the climber to 4392 m, often in less than 24 hours from their sea-level origin. Fortunately, few climbers stay at altitude and are back to sea level within 36 hours.
We present here a case of increasing hypoxia and shortness of breath in a patient, 18 hours after descent to sea level, preceded by a rapid ascent without acclimatization. Likely etiologies other than HAPE—asthma, infection, myocardial infarction, or pulmonary embolus 15 —were effectively ruled out with laboratory and radiologic studies; and, although atypical, his clinical course was most consistent with altitude-related illness. In many ways, the patient fits the stereotype for HAPE presentations: a young, fit male developing symptoms during rapid ascent in cold weather. There are no unique aspects to the patient's history or presentation that might suggest why his symptoms persisted for such an abnormally long time after descent. The patient did significantly exert himself (he climbed the final 1500 m in approximately 5 hours, which is well above average, although nowhere near record speed 16 ), which is an important risk factor for HAPE development; but this does not explain why he continued to develop symptoms during hours of rest at sea level after he returned home.
Conservative treatment with oxygen, diuretics, calcium-channel blockers, and observation led to near complete resolution of our patient's pulmonary edema within 2 days of descent. Reasonable periods of monitoring or at least strict and detailed follow up precautions should be considered in HAPE patients who are treated with descent to lower elevations.
Footnotes
Acknowledgment
We thank David Townes, MD, for his thoughts and comments on this manuscript.
