Abstract
This study sought to investigate the distribution of cytokeratin (CK)-immunopositive cells and their relationship to immunocompetent ED1- and OX6-immunopositive cells in rat periodontium by immunohistochemistry and electron microscopy. CK-immunopositive cells were generally distributed along the surface of the tooth root. They could also be found between root dentin and cementum, in the perivascular space, and close to or in the alveolar bone lacunae. ED1-immunopositive cells exhibited a compact shape with small processes and were widely distributed in the periodontium. Few sections demonstrated an intimate relationship between the CK- and ED1-immunopositive cells close to the cementum, in the perivascular space, and close to or in the alveolar bone. Numerous OX6-immunopositive cells with long branching processes were widely distributed in the periodontal ligament, surrounding and holding CK-immunopositive cells in the cell clusters, close to the cementum. Transmission electron microscopy revealed OX6-immunopositive cells that extended their cytoplasmic processes, which contained vesicles and occasionally lysosomes in between the epithelial cells. This study demonstrates the close relationship between the epithelial cells and the immunocompetent cells in a rat periodontium, indicating a functional interrelationship. It is possible that in a non-inflammatory periodontium, the epithelial cells act not independently, but through interaction with immunocompetent cells.
E
Epithelial cells in the PDL are well known to be the main components of cysts and odontogenic tumors in the pathological state (Ten Cate 1972; Hamamoto et al. 1998; Rincon et al. 2006). In the normal PDL, however, ERM have been regarded as a group of epithelial cells with low or no activity. It has recently been reported that ERM express hard-tissue–related proteins such as enamel and bone morphogenetic proteins during cementum repair (Hasegawa et al. 2003). It has also been demonstrated that periodontal nerve endings and ERM have a close relationship (Lambrichts et al. 1993; Kvinnsland et al. 2000; Tadokoro et al. 2002, 2003) and that an interaction between PDL-derived epithelial cells and fibroblasts regulates the expression of alkaline phosphatase, osteocalcin, and bone sialoprotein (Shimonishi et al. 2005, 2008). These reports suggest that ERM function not independently, but through interaction with other cells or in response to extrinsic stimuli.
Many bone marrow–derived, immunocompetent cells are known to be widely present in the PDL even under non-inflammatory, physiological conditions (Kawahara and Takano 1995; Vandevska-Radunovic et al. 1997). The existence of an intercellular relationship between epithelial cells and cells expressing class II molecules (OX6 + cells) has been verified (Tadokoro et al. 2008). The diversity of the ultrastructure of these immunopositive cells indicates possible involvement of several types of immunocompetent cells (Tadokoro et al. 2008).
There are several immunohistochemical markers for the detection of immunocompetent cells. Cells immunoreactive to ED1, a general macrophage marker, are well known to be broadly distributed in the PDL (Kawahara and Takano 1995; Kan et al. 2001; Kaneko et al. 2008). ED1 antigen is localized on the membranes of the phagolysosomal apparatus of nearly all macrophages, and the expression correlates with their phagocytotic capacity (Dijkstra and Damoiseaux 1993; Damoiseaux et al. 1994). However, the relationship between OX6 + and ED1 + cells to epithelial cells in the PDL remains unclear.
Therefore, the aim of the present study was to investigate the total distribution and the relationship of epithelial cells immunoreactive to CK and the cells immunoreactive to ED1 and OX6 antibody in maxillary rat molars, by using double fluorescence immunohistochemistry and confocal laser microscopy, as well as transmission electron microscopy.
Materials and Methods
Animals
Fourteen 6-week-old, male rats (Wistar strain), ∼150 g in weight, were used in this study. The rats were housed in polycarbonate cages in a specific pathogen-free environment. The Institutional Committee for Ethics and Animal Use and Care of Matsumoto Dental University approved all protocols for the animal experiments.
Rats were fixed in 4% paraformaldehyde, and the maxillary bone containing the teeth was removed, followed by postfixation in the same fixative overnight. The fixed maxillary bone was decalcified in 5% EDTA with 7% sucrose, and frozen sections were cut sagitally at ∼6–8 μm. Subsequently, the sections were double-immunolabeled with anti-CK (broad wide), and anti-ED1 and OX6 antibodies recognizing epithelial cells and immunocompetent cells, respectively.
Immunohistochemistry
After blocking endogenous peroxidase with methanol, sections were reacted with rabbit polyclonal anti–broad wide CK antibody (Nichirei Biosciences Inc; Tokyo, Japan) as the primary antibody at room temperature for ∼3 hr. After washing with PBS, the sections were reacted with the secondary antibody [Simple Stain Rat MAX-PO (R); Nichirei Biosciences Inc] for 1 hr, followed by washing with PBS. The sections were reacted with DAB or aminoethyl carbazole (AEC) (Nichirei Biosciences Inc) for ∼5 min. After confirming the deposition of reaction products under a light microscope, the sections were washed with PBS to stop the color reaction. Then the sections were divided into two groups and reacted with mouse monoclonal anti-ED1 and OX6 antibodies (at 1:10,000 dilution; Serotec Co., Ltd., Oxford, UK) as the primary antibodies at 4C overnight. After washing with PBS, the sections were reacted with the secondary antibody [Simple Stain Rat MAX-PO (M); Nichirei Biosciences Inc] for 1 hr, followed by washing with PBS. The sections were reacted with Histogreen (AbCys S A; Paris, France) for 5 min. After confirming the deposition of both reaction DAB or AEC and Histogreen products under a light microscope, the sections were stained with or without hematoxylin, overlaid with a coverslip, and photographed. For controls, the primary antibody was replaced by PBS or omitted to confirm its specificity.
In addition, some sections were stained by the fluorescent antibody technique using a fluorescent secondary antibody, as follows.
Immunofluorescence
The secondary antibodies to anti-CK were goat anti-rabbit IgG (1:100 dilution, Alexa Fluor 594; Invitrogen -Life Technologies Corp.; Carlsbad, CA), and to anti-ED1 and −OX6, goat anti-mouse IgG (1:100 dilution, Alex Fluor 488; Invitrogen - Life Technologies Corp.). Sections were reacted with the secondary antibody, washed with PBS, overlaid with a coverslip, and observed under a fluorescence microscope (Olympus BX-50; Tokyo, Japan). For controls, the primary antibody was replaced by PBS or omitted to confirm its specificity, and the remaining staining steps were performed as described above. Following examination of the immunofluorescence reaction, some of the sections were examined with a confocal laser scanning microscope. The confocal optical sectioning was performed with an LSM510 META confocal laser microscopy system (Carl Zeiss; Oberkochen, Germany) coupled to an upright microscope with a Plan Fluor objective (x40). The immunostained sections were covered in mounting medium (Vector Laboratories, Inc.; Burlingame, CA) to prevent evaporation. The confocal images were taken with a 0.7-μm step size. In this study, we focused on the region from 0 μm to 7.0 μm in depth, and picked up serial images in several sections.
Immunoelectron Microscopy
Some frozen sections were immunohistochemically stained with mouse monoclonal anti-OX6 antibody (1:20,000 dilution; Serotec Co., Ltd.). After confirming the DAB reaction, sections were postfixed in 1% osmium tetroxide, dehydrated in a series of alcohol, and embedded in Epon 812. Ultrathin sections, 60–80-nm thick, were cut with a diamond knife on an ultramicrotome (MT-7000; Research and Manufacturing Company, Inc., Tucson, AZ) and then observed under a transmission electron microscope (Hitachi H-7600; Tokyo, Japan) at an accelerated voltage of 80 kV.
(
(
Results
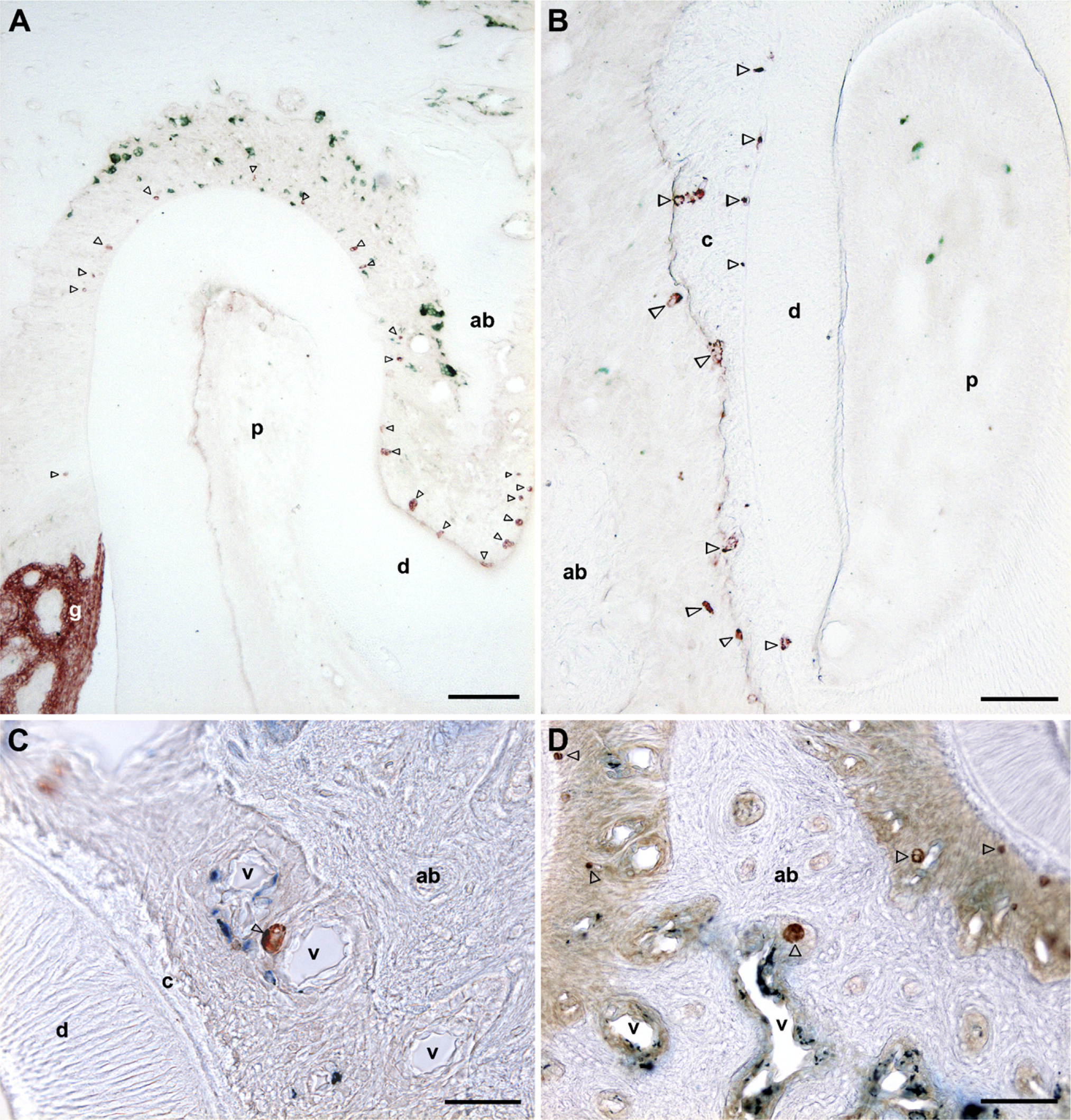
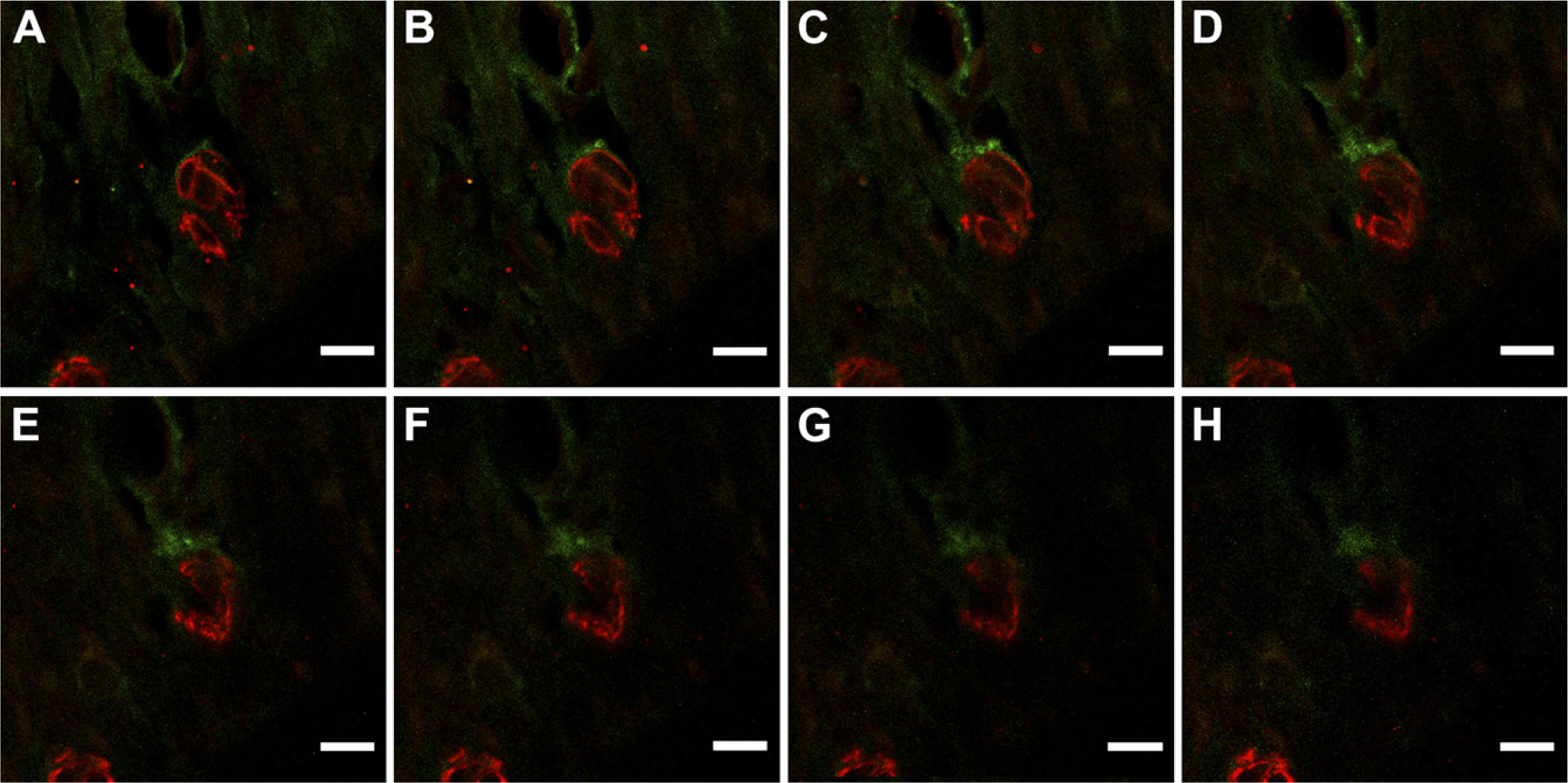
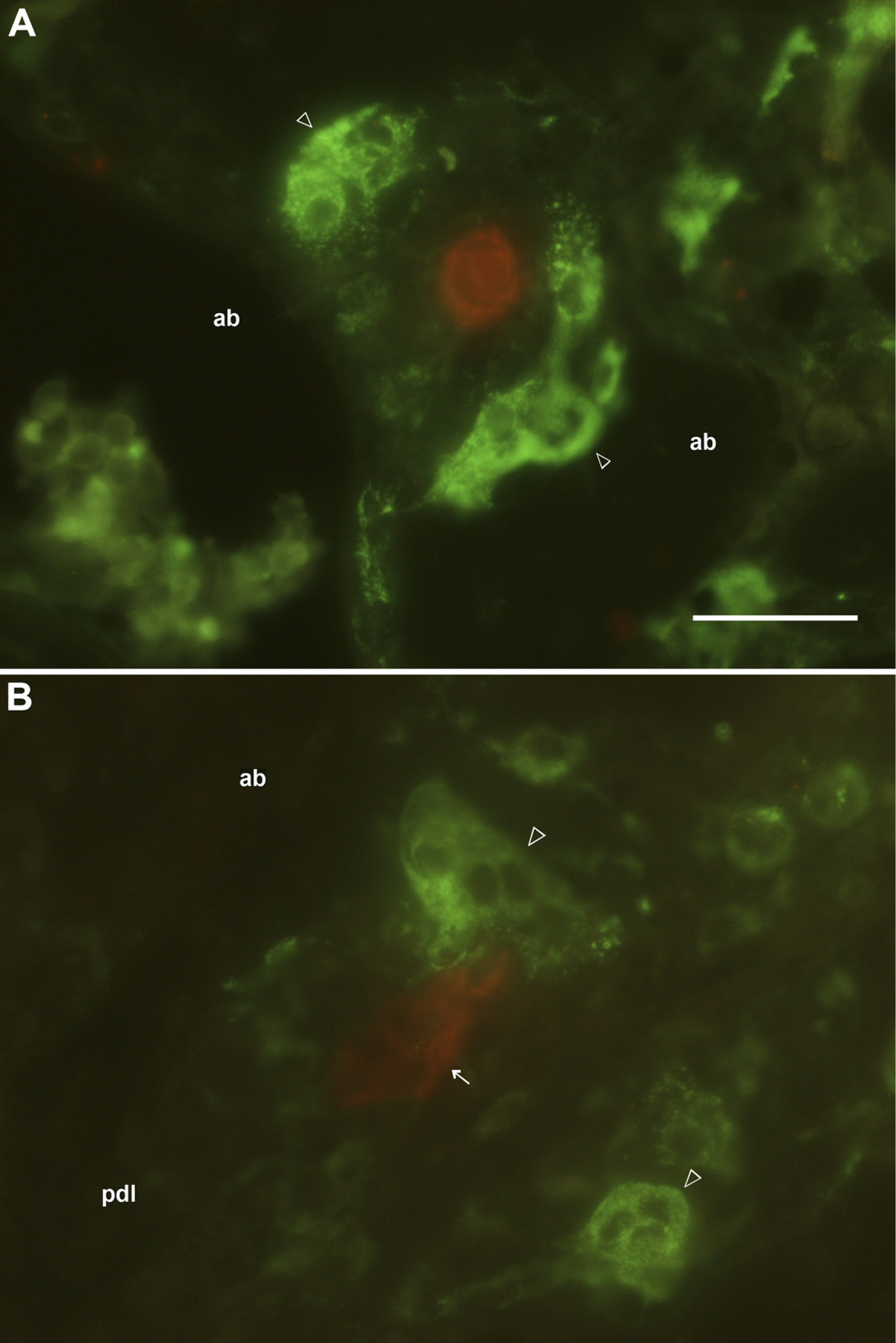
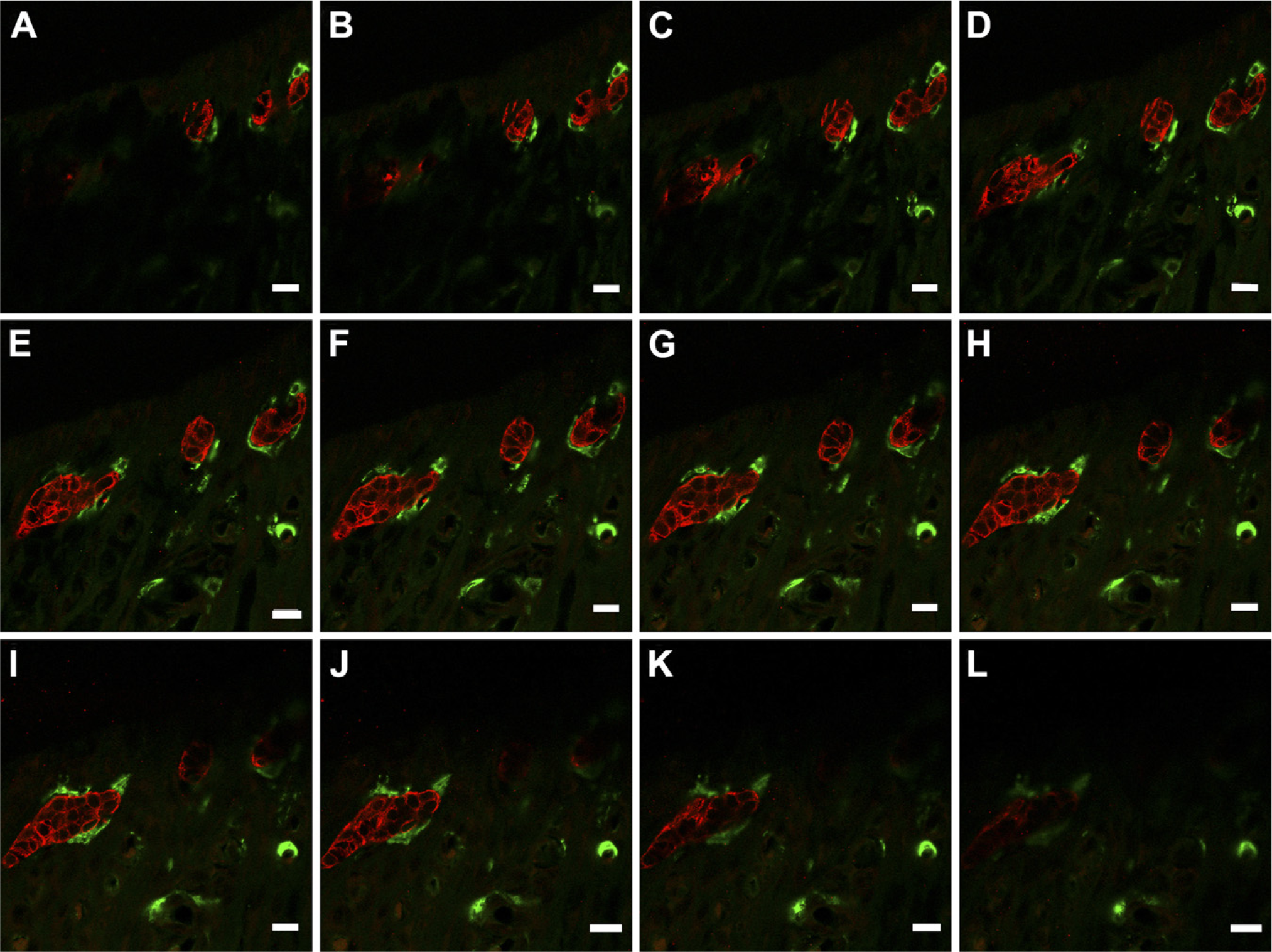
CK-immunopositive cells were usually seen as various-sized aggregates of cells along the root surface of the maxillary molars (Figure 1A). The immnopositive cells were sometimes found near vascular spaces, and close to or in the alveolar bone between the molars, and between the root dentin and cementum (Figures 1B–1D). Double immunostaining with CK and ED1 antibodies showed that CK-immunopositive cells were occasionally close to or in contact with the ED1-immunopositive cells that were compact in shape with fewer processes (Figures 1B and 1C). Confocal scanning laser microscopy of the double immunofluorescence labeling confirmed that the ED1-immunopositive cells were in contact with CK-immunopositive cells (Figures 2A–2H). It was also confirmed that the CK-immunopositive cells close to or in the alveolar bone were often found proximal to or in contact with large ED1-immunopositive cells (Figures 3A and 3B).
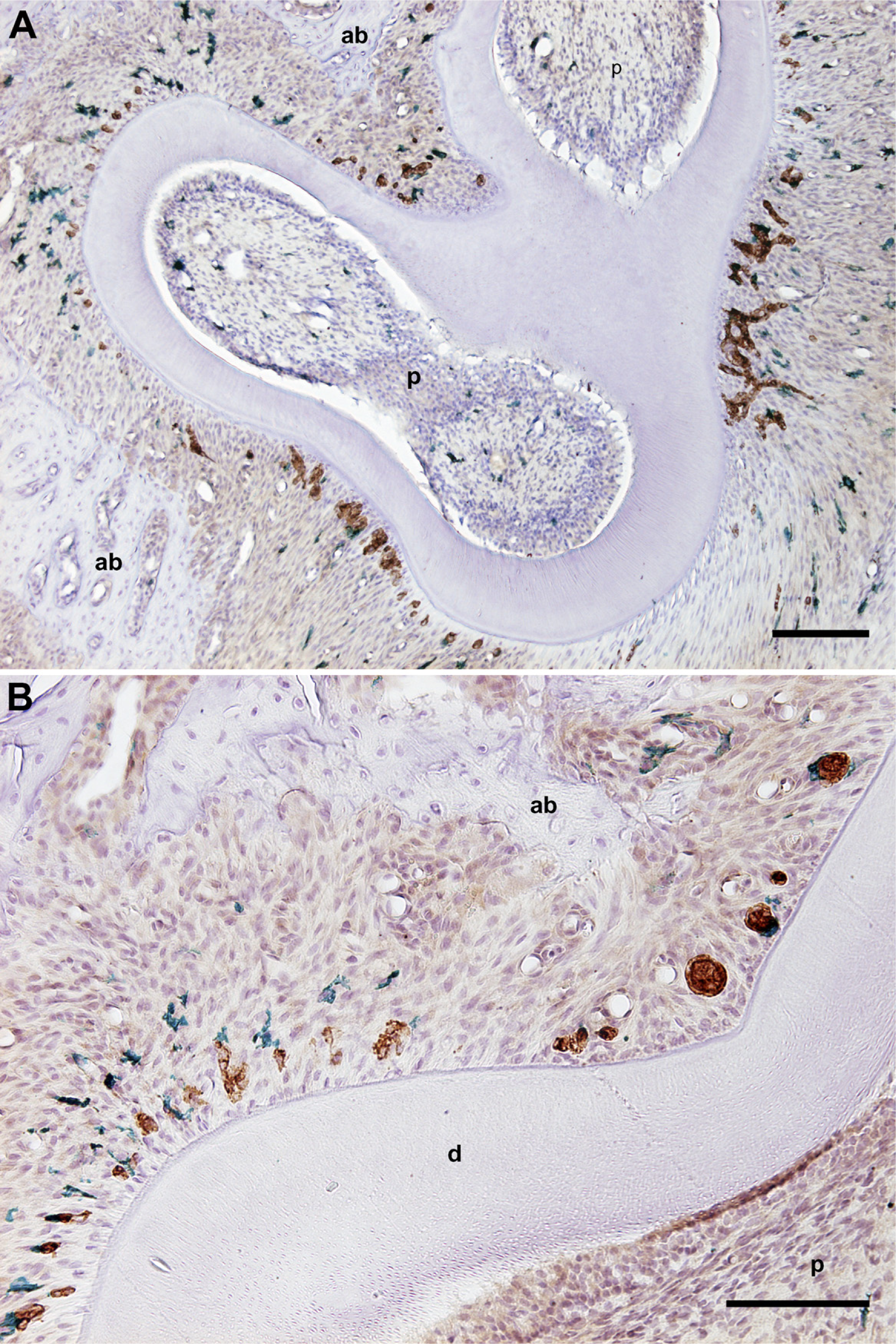
In the cervical and furcational region, double-immunostained sections with CK and OX6 antibodies showed that these immunopositive cells were frequently close to or in contact with each other (Figures 4A and 4B). This was confirmed by confocal scanning microscopy, identifying OX6-immunopositive cells in contact with large CK-immunopositive cell clusters (Figure 5). The immunoelectron microscopic examination confirmed the presence of cytoplasmic processes of OX6-immunopositive cells in the space between the epithelial cell clusters in the PDL (Figure 6). The immunopositive reaction products were observed at the plasma membrane within the epithelial cell clusters. The cytoplasm of the OX6-immunopositive cells did not contain keratin filaments, but lysosomes and vesicles. A basal lamina surrounded the epithelial cell clusters, which contained keratin filaments, abundant vesicles, and mitochondria. The cell membranes of epithelial and OX6-immunopositive cells were in contact with each other. Cell junctions could not be observed between both cells.
(
(
(
In the apical region, CK- and OX6-immunopositive cells were scattered, and the close relation between both cells was less often observed (Figure 7).
Discussion
In this study, we focused on the total distribution of epithelial cells and their relationship with immuno-competent cells in the PDL of rat maxillary molars. The results clearly demonstrate that CK-, ED1- and OX6-immunopositive cells are widely distributed in rat periodontium and that these cells are in close contact with each other, indicating possible interaction and functional activity.
Developmental and evolutionary studies reveal that the epithelial cells in the PDL are remnants of Hertwig's epithelial root sheath (HERS) (Luan et al. 2006). This transient structure is fenestrated by mesenchymal cells from the dental follicle and reduced to ERM. Several studies support the concept that these epithelial cells are not only embryonic remnants without function, but that they play an important part in the maintenance of PDL homeostasis, prevention of root resorption (Luan et al. 2006), cementum repair, and cell migration (Hasegawa et al. 2003; Leonardi et al. 2005).
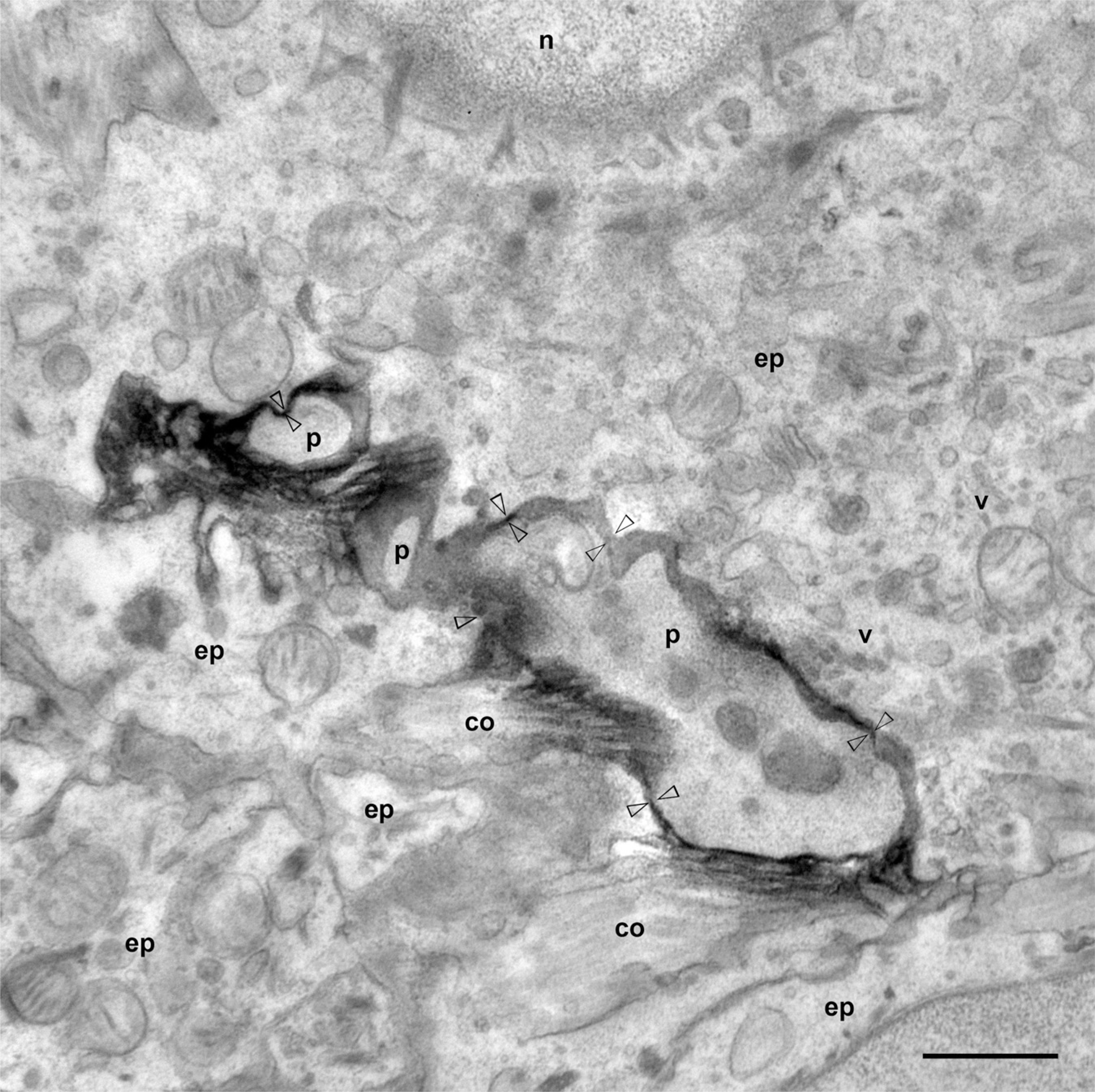
An electron microscopic photograph showing cytoplasmic processes (p) of OX6-immunoreactive cells in contact with epithelial cells in the PDL (arrowheads). co, collagen; ep, epithelial cell; n, nucleus; v, vesicles. Bar = 1 μm.
An ED1-immunopositive reaction is observed in the lysosomes of bone marrow monocyte-derived, immuno-competent cells, and most of the ED1-immunopositive cells are considered to be macrophages, dendritic cells (DCs), and/or osteoclasts (Kawahara and Takano 1995; Suzuki et al. 1999; Kan et al. 2001). An analysis of the distribution of ED1-immunopostive cells in the PDL of first mandibular rat molars reported that they were most abundant in the tooth root bifurcation (Kan et al. 2001), in the same area where large ERM cell clusters can be seen. Moreover, the same area houses DCs that have the characteristics of activated antigen-presenting cells and show cell-to-cell contact with lymphocytes (Hamamoto et al. 1998; Kaneko et al. 2008; Tadokoro et al. 2008). In a recent study, we found that ERM were in contact with OX6+ immunocompetent cells, and that OX6-immunopositive cells surrounding epithelial cells showed ultrastructural diversity, suggesting the involvement of several types of immunocompetent cells with periodontal epithelial cells (Tadokoro et al. 2008). The present study demonstrated that not only OX6- but also ED1-immunopositive cells were close to or in contact with epithelial cells. The observation of the relation of cells immunoreactive to CK and ED1 was difficult because the immunoreaction products of ED1 were recognized only on organelles belonging to the phagolysosomal apparatus of macrophages and DCs, and did not define their shape near the root surface. On the other hand, the observation of the relationship between CK- and OX6-immunopositive cells was relatively easy, because the immunoreaction products of OX6 are recognized on the cell membrane (Kan et al. 2001; Tadokoro et al. 2008). It appeared that most of the OX6-immunopositive cells, which were close to or in contact with CK-immunopositive cells near cervical and furcational cementum contained few ED1 immunoreaction products.
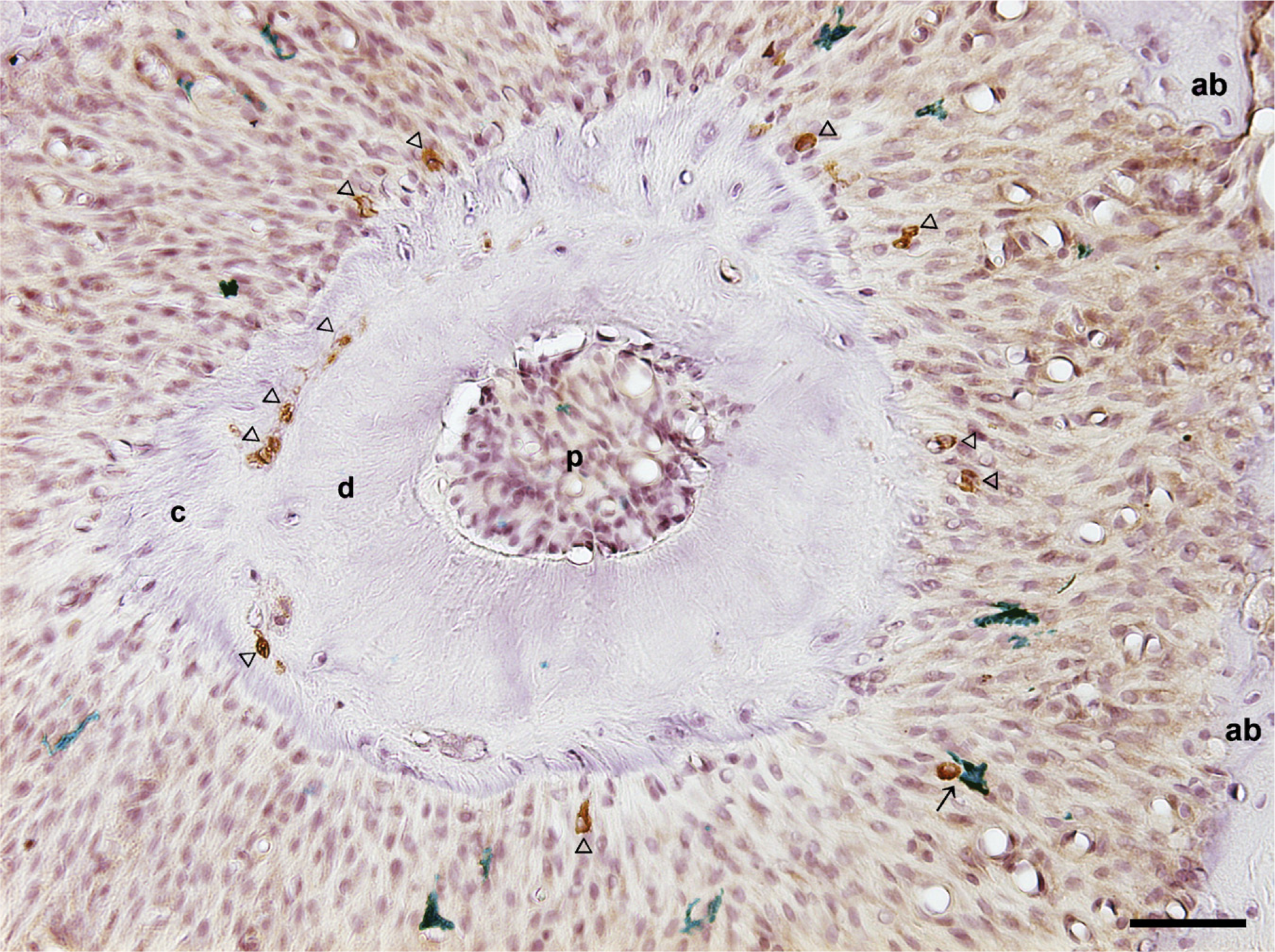
A horizontal section of the periapical region of a third maxillary rat molar. CK-immunopositive cells (brown) are found close to the root cementum and between the cementum and dentin (arrowheads). The close contact between CK- and OX6-immunopositive cells (green) is rarely seen in the periapical PDL (arrow). ab, alveolar bone; c, cementum; d, dentin; p, pulp. Bar = 50 μm.
Periodontal epithelial cells have been reported to show well-developed spines, lysosomes, and caveolae. These structures, similar to immunocompetent cells, suggest their phagocytic capacity (Birek et al. 1980; Hamamoto et al. 1989, 1998; Tadokoro et al. 2008) and indicate maintenance of their proliferative activity (Reeve and Wentz 1962; Trowbridge and Shibata 1967). In the cervical root area, which is the closest to the oral environment, CK-immunopositive epithelial cells, and immunocompetent ED1 cells or OX6-immunopositive cells, are widely distributed, and an intimate relationship between these cells could be found. This may indicate that the epithelial cell function is not independent, but operates through interaction with immunocompetent cells in the periodontium under a non-inflammatory, homeostatic mechanism of protection against inflammatory factors. Considering that the location of the contact is proximal to the cementoblast layer, their possible involvement in the process of cementum formation and repair cannot be excluded (Tadokoro et al. 2008).
CK-immunopositive cells, which are usually observed near the surface of the tooth root cementum, were found, along with ED1-immunopositive cells, in the perivascular space of the PDL and in the lacunae of the alveolar bone. Previous studies reported that tyrosine receptor kinase A–immunoreactive cells were sometimes located outside the PDL and within the alveolar bone (Woodnutt and Byers 2001). Rat molars intermittently drift distally with active remodeling of the alveolar bone (Vignery and Baron 1980; Robinson and Schneider 1992; Lasfargues and Saffar 1993), and this process may lead to partial incorporation of epithelial cells from epithelial cell cords into the bone. On the other hand, it has been proposed that HERS cells have migratory capacity (Luan et al. 2006), but the mechanisms contributing to their displacement over time are unknown.
In conclusion: (1) CK-immunopositive cells are distributed close to the cementum, near vascular spaces and close to or in the alveolar bone between the molars and between the root dentin and cementum in rat PDL; (2) at the light microscopic observation level, it appears that most of the OX6-immunopositive cells found proximal to the cementum and close to or in contact with CK-immunopositive cells contained few ED1 immunoreaction products; (3) CK-immunopositive cells are sometimes found along with ED1-immunopositive cells in the perivascular space of the PDL and in the lacunae of the alveolar bone; and (4) in the non-inflammatory PDL, the intimate relationship between epithelial and immunocompetent cells reported in the present study indicates their possible involvement in a homeostatic, anti-inflammatory mechanism.
Footnotes
Acknowledgements
This study was supported by a Grant-in-Aid for Scientific Research (No. 19791356) from the Ministry of Education, Science, Sports and Culture, Japan.
We thank Dr. Tanya Franzen for proofreading this manuscript.
