Abstract
Accumulation of lipids and hyalinosis in the splenic arteries of aged dogs are frequently detected by routine histopathologic examinations. The purpose of this study was to pinpoint the localization of canine apolipoprotein B-100 (CApoB-100) and immunoglobulins (IgA, IgM, IgG) in the splenic arteries of aging dogs (n = 80) through the use of immunohistochemical techniques. CApoB-100 deposits were found in the subendothelial space, extracellular matrix, and atheromatous lesions in the tunica media of the arteries in dogs ≥ 6 years of age. Foamy cytoplasm of the infiltrated macrophages was also CApoB-100 immunopositive. In dogs ≥10 years of age, almost all central arteries were CApoB-100 immunopositive. Hyaline deposits within the wall were characterized by immunopositivity against canine IgA, IgM, IgG, and albumin. Lipid accumulation in splenic arteries may be an age-related lesion and a precursor of the atheromatous plaques associated with splenic hemorrhage and infarcts later in life. In addition, deposition of immunoglobulins, probably mediated by immune complexes, may play an important role in the development of canine vascular diseases similar to human disease.
Atherosclerosis is one of the most important vascular diseases in human medicine, along with chronic ischemic heart disease, gangrene of the legs, mesenteric occlusion, and ischemic encephalopathy. 11,24 Atherosclerosis is characterized by the accumulation of large amounts of lipoproteins, mainly low density lipoprotein (LDL), in the arterial wall. 5,8,11,14,18,24 Subendothelial accumulation of lipids begins in childhood and progresses slowly for a long time, thereby increasing atherosclerotic risk factors such as aging, hyperlipidemia, hypertension, diabetes, and obesity. 11,24 Atherosclerosis is less important in domesticated carnivores 8,22 and has been described in only a few dogs. 1,2,9,10,13,21 Severe atherosclerotic lesions with clinical significance rarely appear in the heart, brain, and kidney even in a dog involved with systemic atherosclerosis. 9,10,13,21 Immunohistochemical distribution of apolipoprotein in the peripheral arteries has been rarely detected in dogs. 10 No reports have indicated whether aging is a factor in the occurrence of lesions in dog. However, routine histopathologic examinations of the dog, with or without hyperlipidemia and systemic atherosclerosis, frequently reveal the accumulation of lipids and hyaline materials in the central and penicillar arteries of the spleen, occasionally associated with hemorrhage and infarction.
The purpose of this study was to pinpoint the distribution of apolipoprotein B-100 and immunoglobulin (IgA, IgM, IgG) in the splenic arteries of aging dogs and to compare the histopathologic changes with those found in human disease.
Materials and Methods
Animals
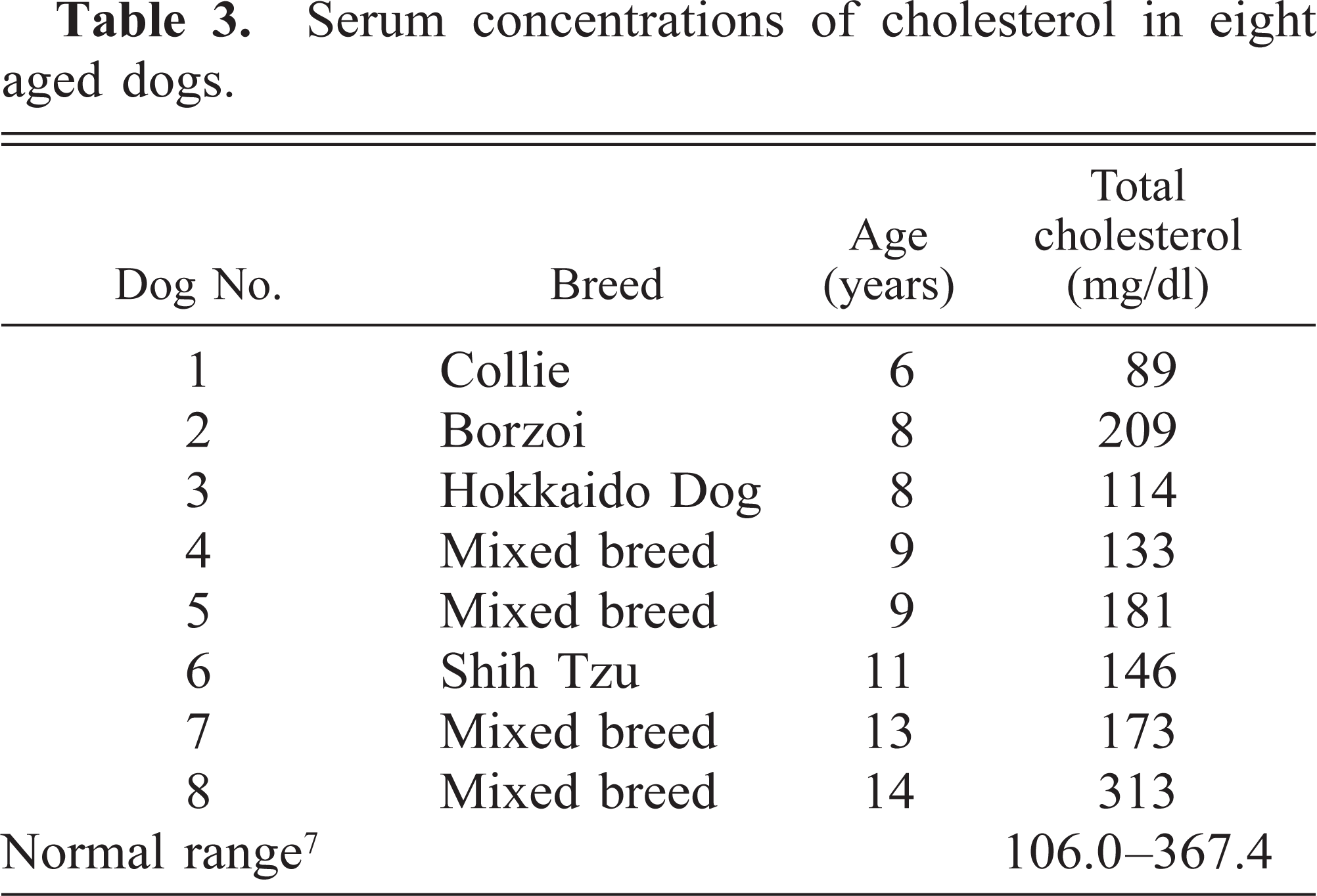
The dogs were 40 females and 40 males of various breeds and ranging in age from 1 to 18 years (Tables 1, 2). The animals were clinically diagnosed with various diseases (Table 2), and necropsies and routine histopathologic examinations were performed at the Department of Veterinary Pathology, School of Veterinary Medicine, Rakuno Gakuen University. Serum concentrations of cholesterol were measured in eight dogs ≥6 years of age, and the level was within the normal range (Table 3). 7 Histopathologically, there were no significant changes indicating hypothyroidism in any animals, although serum concentrations of thyroid hormone were not measured.
Dogs used in this study.
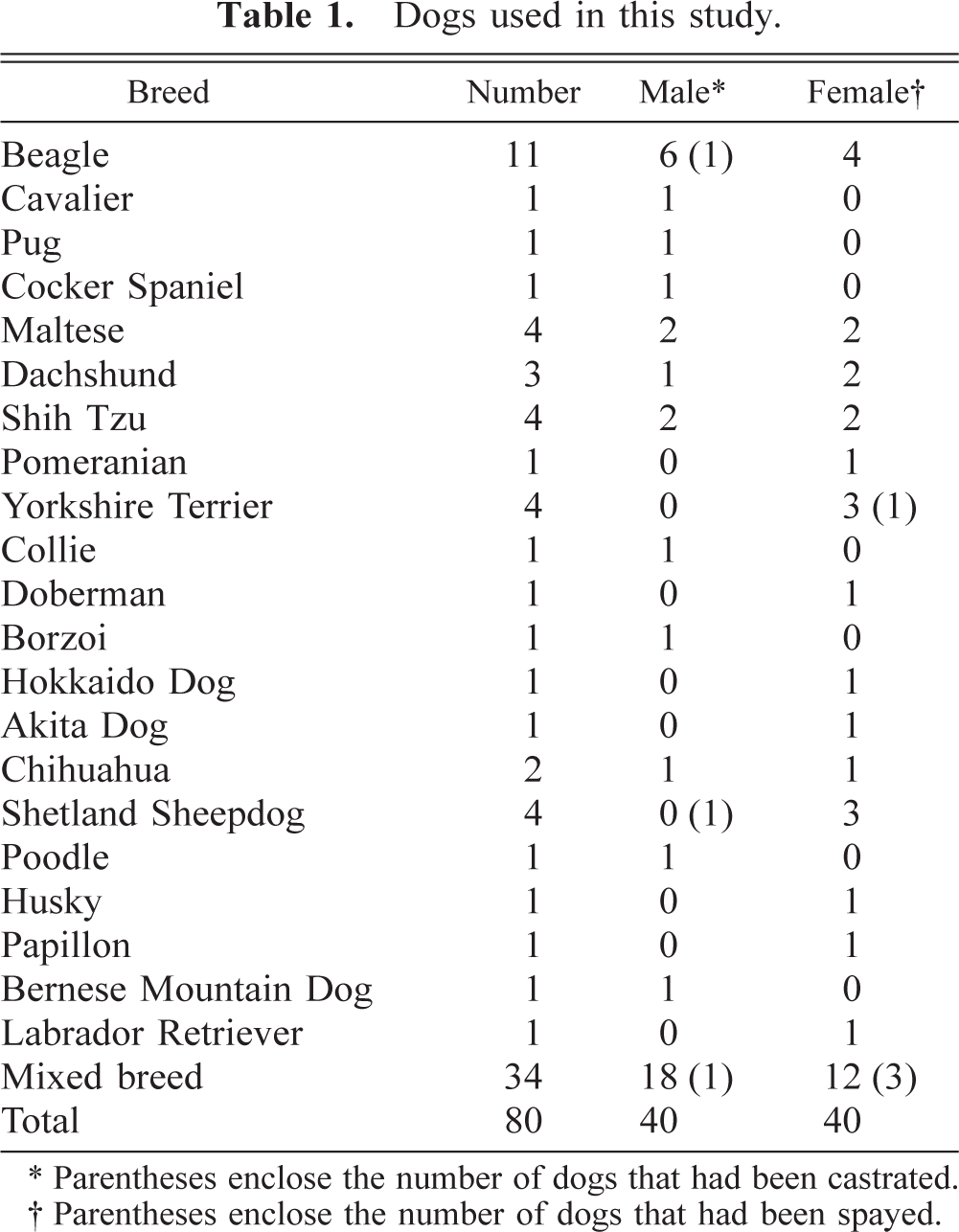
∗ Parentheses enclose the number of dogs that had been castrated.
† Parentheses enclose the number of dogs that had been spayed.
The clinical diagnosis of 80 dogs used in this study.

∗ Dog numbers as indicated in Table 3.
Serum concentrations of cholesterol in eight aged dogs.
Histopathology
Tissue samples of the spleen were fixed in 10% neutral buffered formalin and dehydrated in a series of alcohols. For histopathologic examination, 4-µm sections were cut from paraffin-embedded blocks and stained with hematoxylin and eosin (HE), elastica HE, periodic acid–Schiff (PAS), Congo red, von Kossa's stain, and Berlin blue. Frozen section from 10% neutral formalin–fixed tissues were cut at 10 µm in a cryostat at −20 C and stained with Sudan black B.
Immunohistochemistry
Serial histologic sections fixed in 10% neutral buffered formalin were used for immunohistochemical analysis by the avidin–biotin–peroxidase complex (ABC) procedure (Vectastain Elite ABC Kit; Vector Laboratories, Burlingame, CA). Specific antisera used in this study were rabbit anti-canine apolipoprotein B-100 (CApoB-100) polyclonal antibody described previously, 8,9 mouse anti–α-smooth muscle actin (αSMA) monoclonal antibody (Sigma, St. Louis, MO), goat anti-canine IgG (gamma chain) polyclonal antibody (Kirkegaard & Perry, Laboratories, Gaithersburg, MD), rabbit anti-canine IgM (mu chain) polyclonal antibody, rabbit anti-canine IgA (alpha chain) polyclonal antibodies (Bethyl Laboratories, Montgomery, TX), and goat anti-canine albumin (Bethyl Laboratories). The deparaffinized sections were treated in 0.1% trypsin solution for 10 minutes. After washing with distilled water, the sections were treated with 0.3% H2O2 in methanol for 10 minutes to suppress endogenous peroxidase activity, followed by incubation with 10% normal goat serum for 30 minutes. The primary antibody was reacted at 4 C for 12 hours. The sections treated with the primary antibody were reacted with biotinylated rabbit anti-mouse IgG, rabbit anti-goat IgG, and sheep anti-rabbit IgG antibodies. The ABC reaction products were visualized with 3,3′-diaminobenzidine tetrahydrochloride and then counterstained with the Berlin blue method and Mayer's hematoxylin. Control incubations using excess antigen to immune or nonimmune sera as the primary antibody and omitting the primary antibody resulted in the absence of specific staining.
Scoring of immunohistochemical CApoB-100 localization
The number of CApoB-100–immunopositive vessels was individually counted in 10 trabecular, central, penicillar, and sheathed arteries and in the trabecular vein of the spleen.
Results
Histopathologic findings
Significant changes in the splenic arteries were not detected in dogs 1–5 years of age but were found in those ≥6 years of age. In mild lesions of the splenic arteries, the subendothelial space of central and penicillar arteries was dilated by an extracellular network that contained a small amount of sudanophilic material in sections stained with Sudan black B. A small amount of amorphous eosinophilic material that was PAS positive and Congo red negative was occasionally found in the subendothelial space in sections stained with HE (Fig. 1). In moderate lesions, the subendothelial space of the artery was severely dilated and contained abundant sudanophilic material. Occasionally, sudanophilic and amorphous eosinophilic materials were seen in the tunica media in the arteries. In severe lesions, the tunica intima, tunica media, and cystic space contained abundant sudanophilic material, amorphous eosinophilic material, debris, intimal erosion, enlarged macrophages with pyknotic nuclei and foamy cytoplasm, and occasionally mineralized material (Fig. 2), which was positive with von Kossa's stain and the Berlin blue method. A small number of macrophages infiltrated the subendothelial space; some were enlarged and had foamy cytoplasm (Fig. 3) filled with sudanophilic material. The intimal elastic lamina had partly or completely disappeared in the lesion. These lesions occurred frequently in dogs ≥10 years of age.
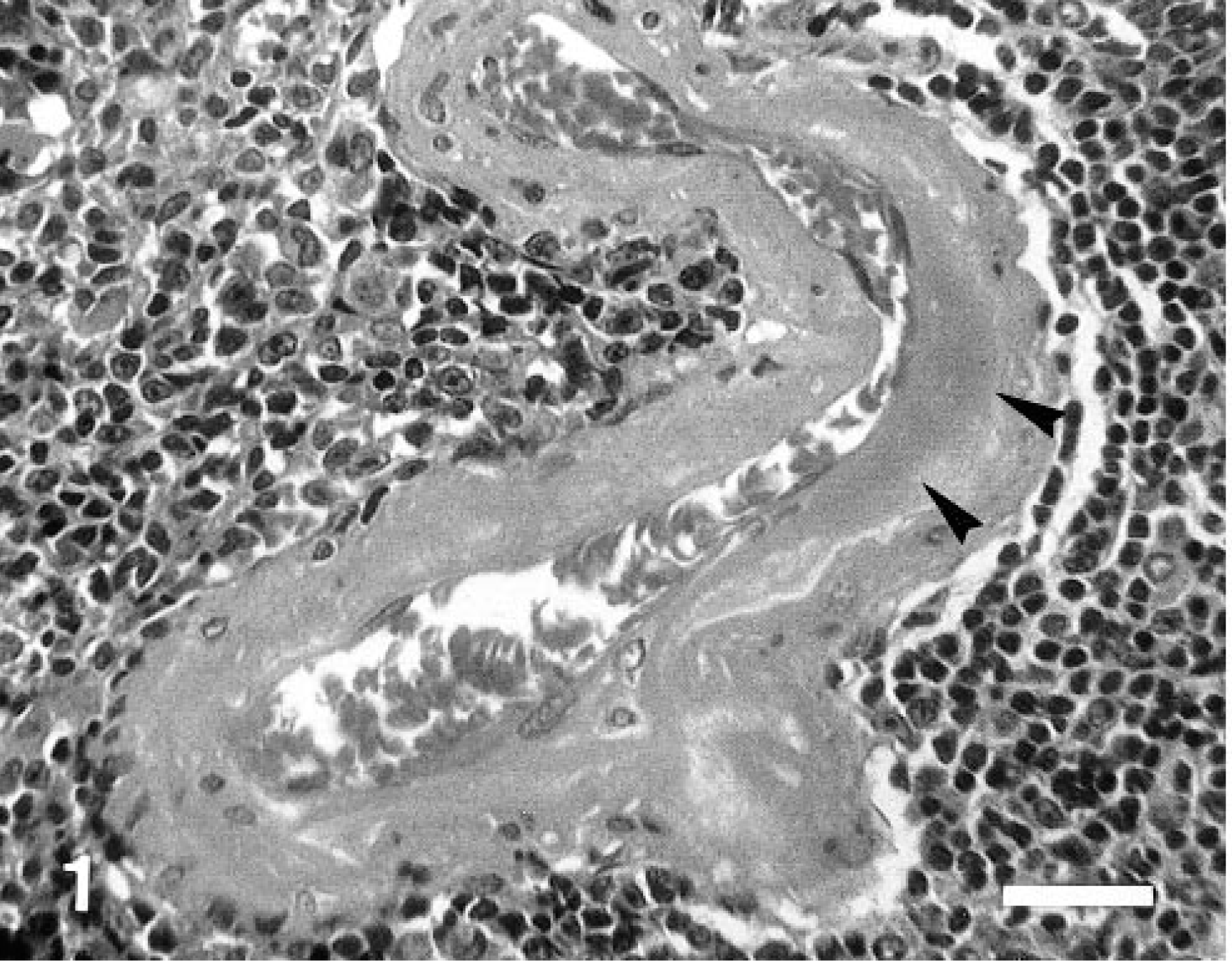
Spleen; 14-year-old dog. A small amount of amorphous eosinophilic material (arrowheads) is accumulated in the subendothelial space of the central artery. HE. Bar = 30 µm.
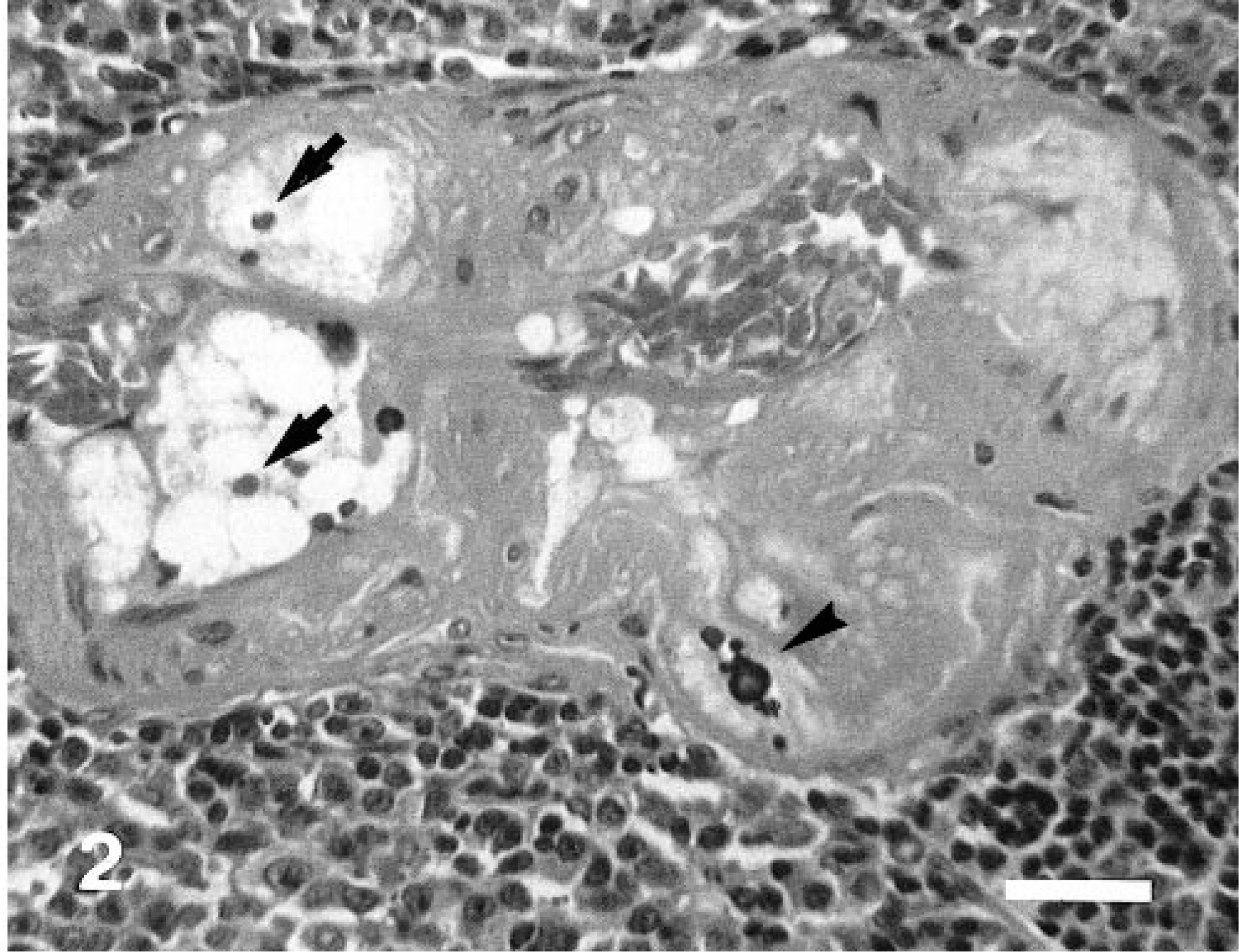
Spleen; 18-year-old dog. The tunica intima, tunica media, and cystic space contain abundant amorphous eosinophilic material, enlarged macrophages with pyknotic nuclei and foamy cytoplasm (arrows), and mineralized material (arrowhead) in the severe lesion. HE. Bar = 30 µm.
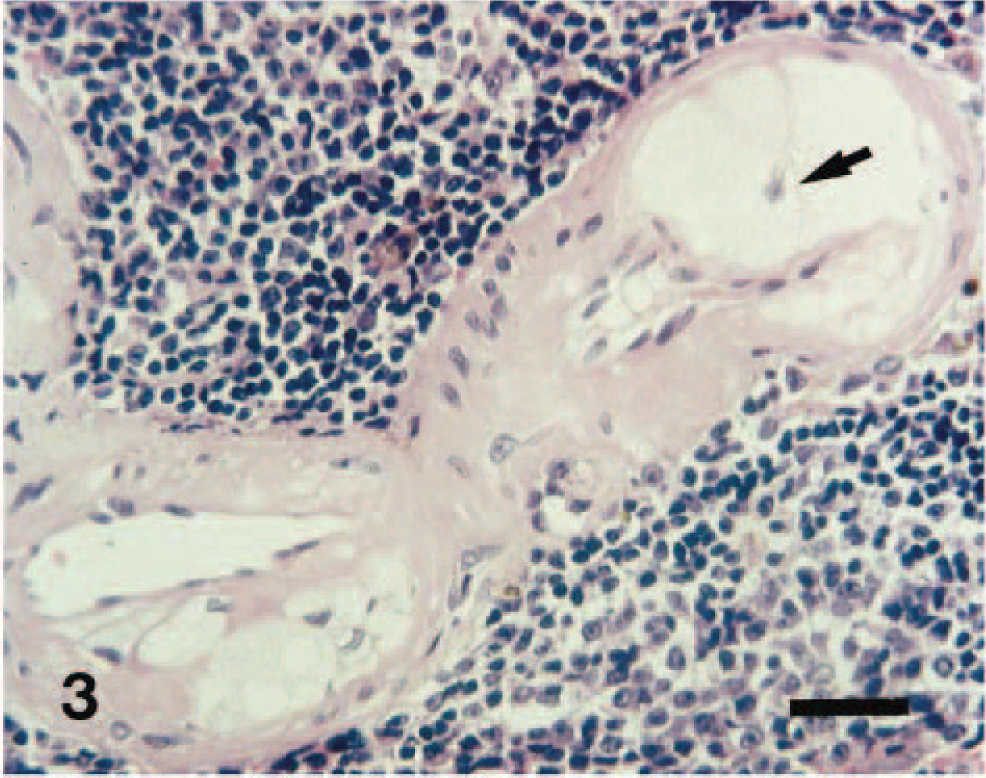
Spleen; 13-year-old dog. A small number of macrophages have infiltrated into the subendothelial space; some are enlarged with abundant foamy cytoplasm (arrow). HE. Bar = 30 µm.
Immunohistochemical findings
In the mild and moderate lesions, the tunica intima and the extracellular matrix in the tunica media showed positive immunoreactivity against CApoB-100 antibody. The foamy cytoplasm of infiltrated macrophages was also positive (Fig. 4). In severe lesions, the tunica media and cystic space contained abundant CApoB-100–positive material. Loss of smooth muscle cells was frequently seen in the tunica media (Fig. 5). Some of the amorphous eosinophilic material in the lesions seen in HE-stained sections reacted to anti-canine IgA, IgM, IgG, and albumin antibodies with ABC procedures (Figs. 6–8). The foamy cytoplasm of infiltrated macrophages also reacted to anti-canine IgA, IgM, IgG (Figs. 6–8) and albumin antibodies.
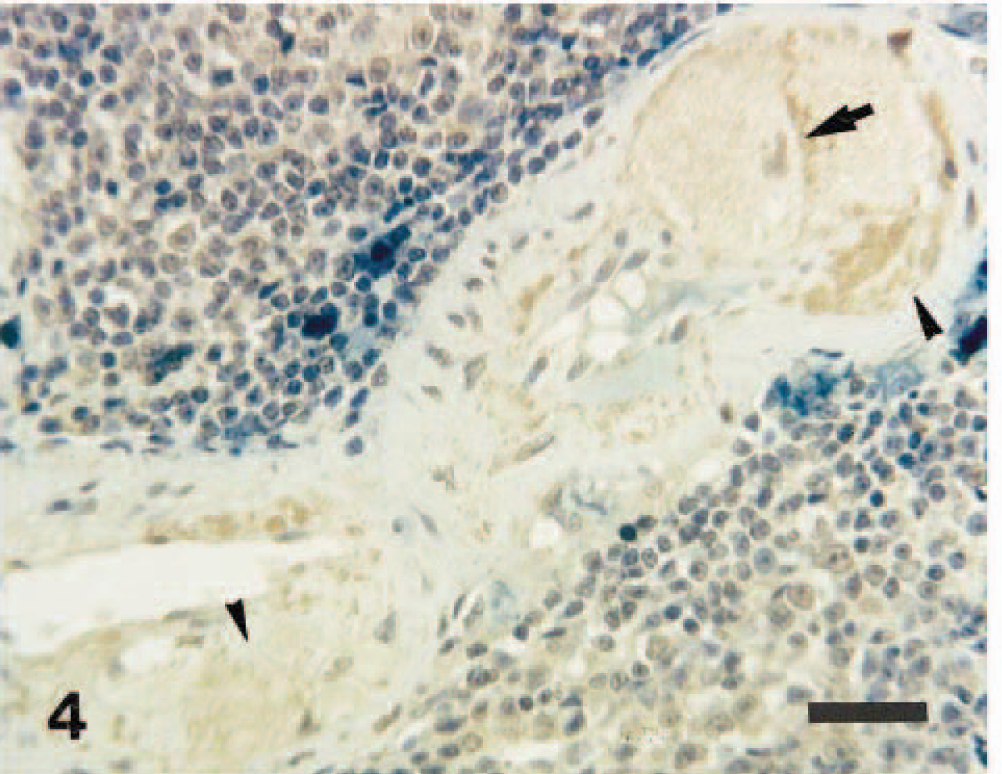
Spleen; 13-year-old dog. Enlarged foamy cytoplasm of infiltrated macrophages (arrow) and the extracellular matrix in the tunica media (arrowheads) are positive against CApoB-100. ABC method, Berlin blue, and Mayer's hematoxylin counterstain. Bar = 30 µm.
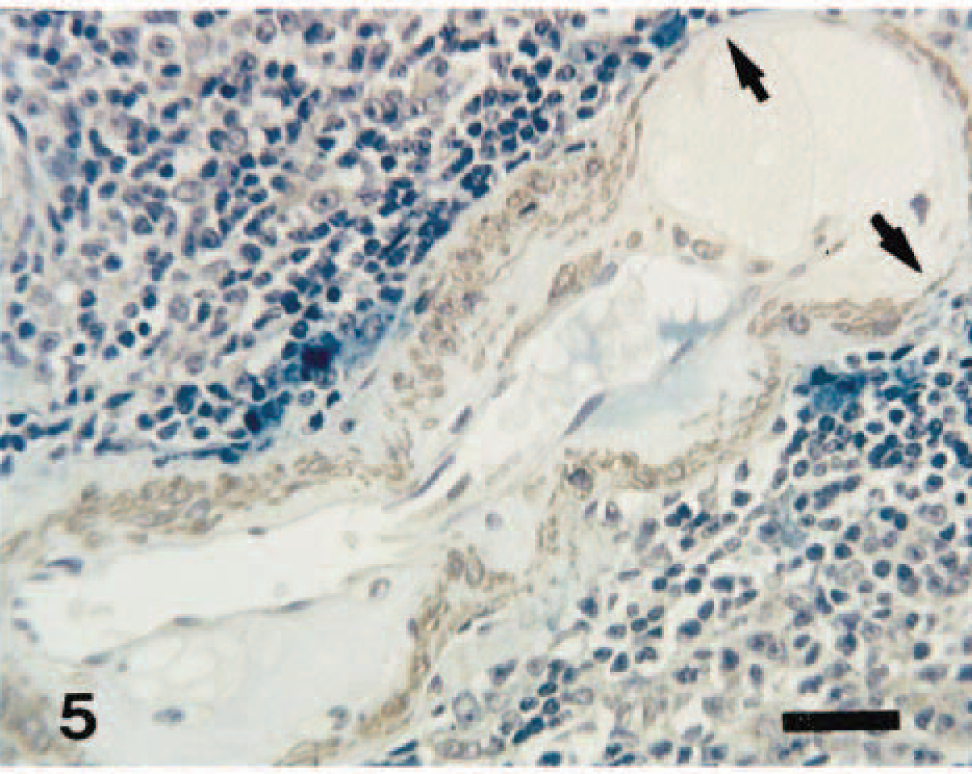
Spleen; 13-year-old dog. Loss of smooth muscle cells (arrows) is seen in the tunica media due to infiltration of enlarged foamy macrophages in the tunica intima. ABC method with anti-α-SMA antibody, Berlin blue, and Mayer's hematoxylin counterstain. Bar = 30 µm.
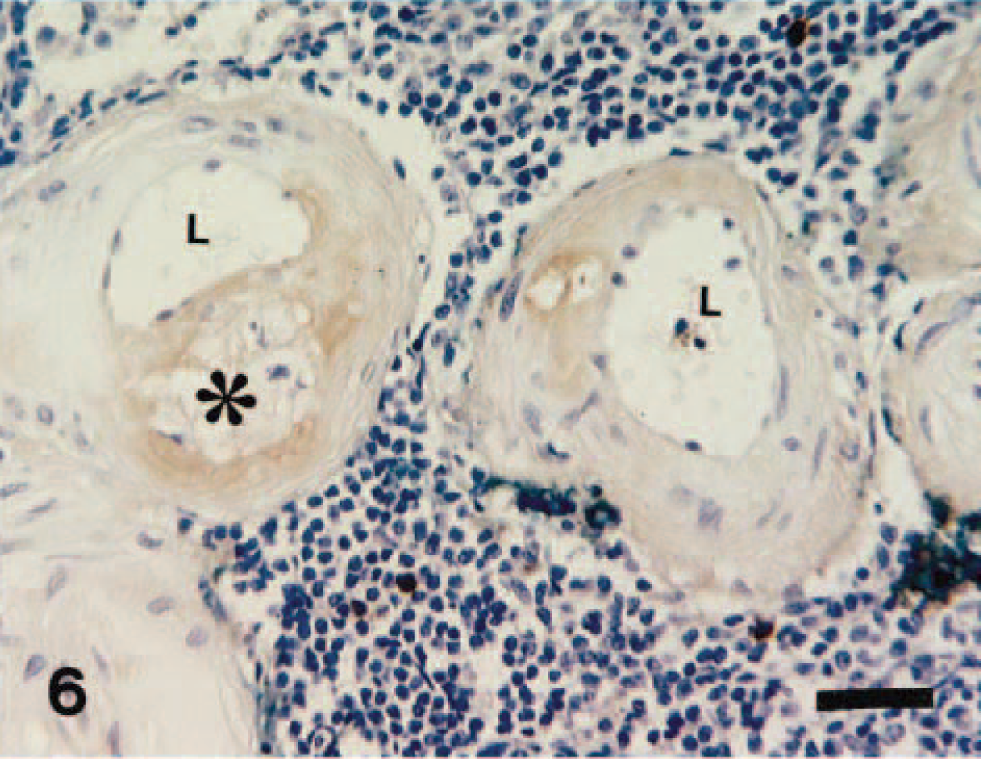
Spleen; 13-year-old dog. Some parts of the amorphous material and foamy cytoplasm of infiltrated macrophages (∗) in the atheromatous lesions react to anti-canine IgA antibody. L = vascular lumen. ABC method, Berlin blue, and Mayer's hematoxylin counterstain. Bar = 30 µm.
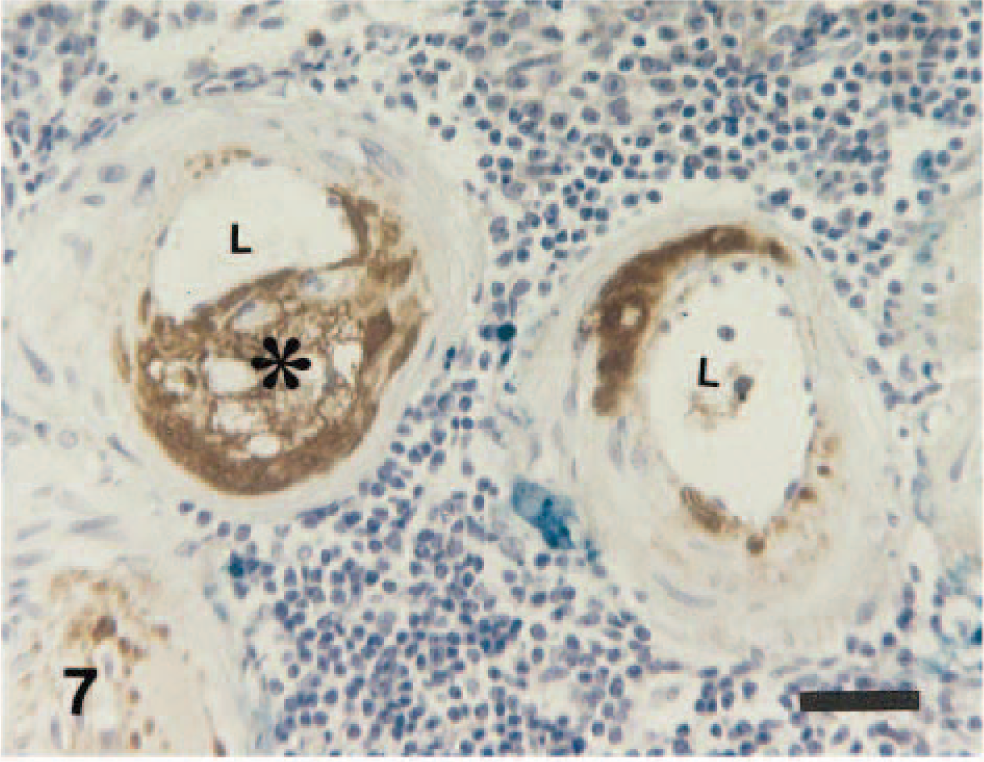
Spleen; 13-year-old dog. Some parts of the amorphous material and foamy cytoplasm of infiltrated macrophages (∗) in the atheromatous lesions react to anti-canine IgM antibody. L = vascular lumen. ABC method, Berlin blue, and Mayer's hematoxylin counterstain. Bar = 30 µm.
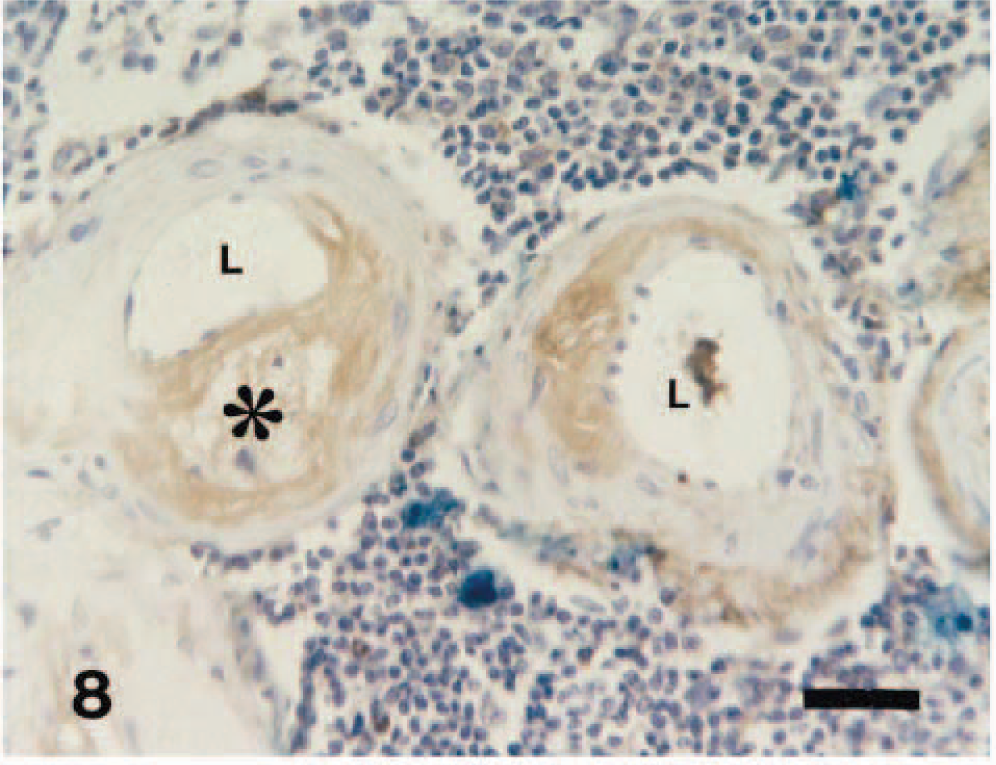
Spleen; 13-year-old dog. Some parts of the amorphous material and foamy cytoplasm of infiltrated macrophages (∗) in the atheromatous lesions react to anti-canine IgG antibody. L = vascular lumen. ABC method, Berlin blue, and Mayer's hematoxylin counterstain. Bar = 30 µm.
Localization of CApoB-100 in splenic arteries
No accumulation of CApoB-100 was found in the splenic arteries of dogs 1–5 years of age. In all dogs ≥6 years old, however, variable accumulation of CApoB-100 was observed in both male and female dogs. Fifty percent of the central artery in each 6-year-old dog had an immunoreactivity against CApoB-100 antibody. With increasing age, the ratio of CApoB-100 positive artery increased (Fig. 9). The central artery showed the positivity more frequently than did the trabecular, sheathed, and penicillar arteries. In dogs ≤5 years of age, no arteries immunopositive against anti-canine IgG, IgM, IgA, and albumin antibodies were found.
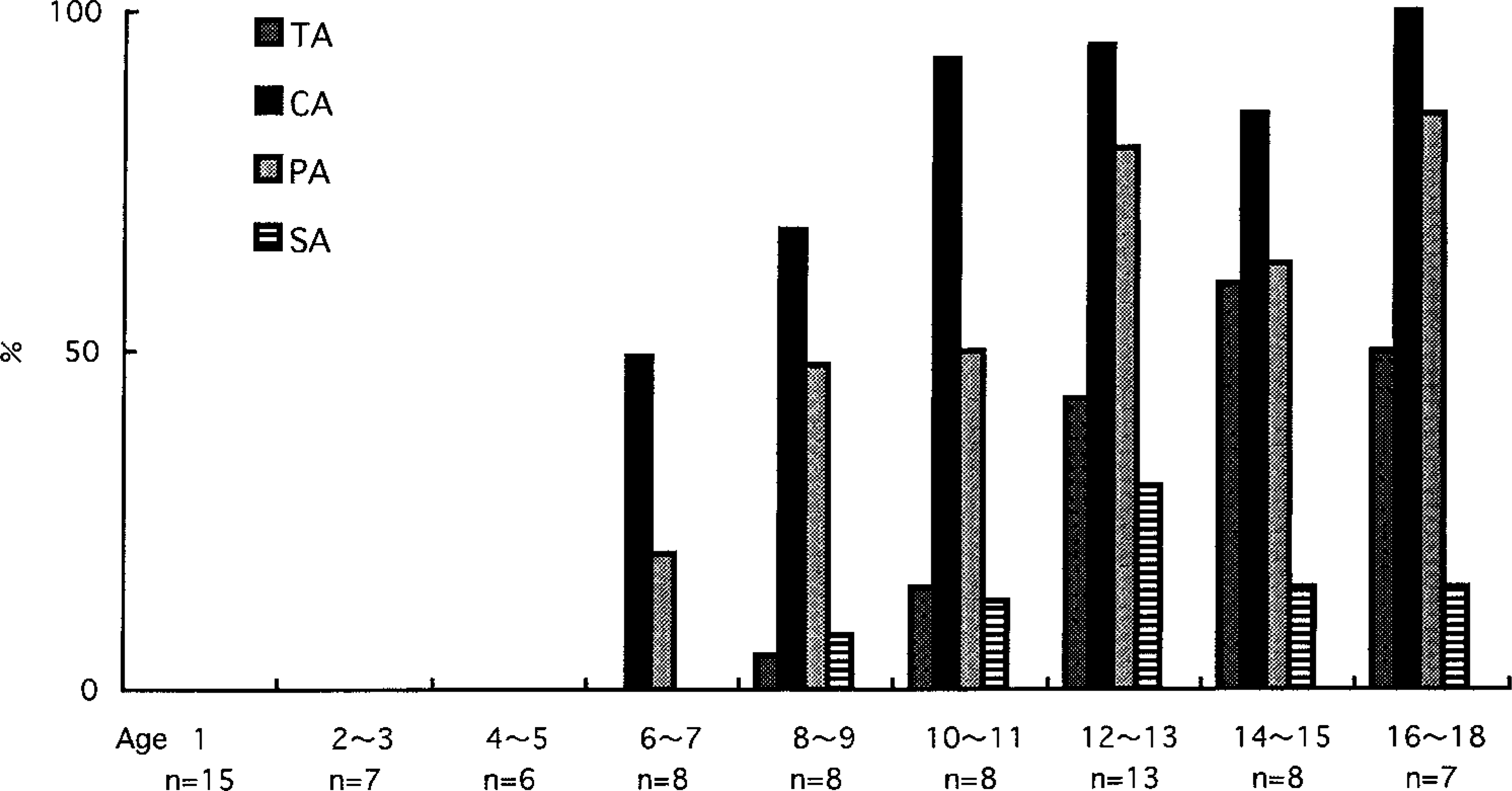
Distribution of CApoB-100 in the splenic vessels. The ratio of CApoB-100 positive artery increases with increasing age. The central artery shows the positivity more frequently than the trabecular, sheathed, and penicillar arteries. TA = trabecular artery. CA = central artery. PA = penicillar artery. SA = sheathed artery.
Discussion
Dogs are usually considered to be atheroresistant. 8,22 In contrast to humans, dogs have approximately five to six times as much high density lipoprotein (HDL) as LDL. 15,16,20 Some investigators have produced experimental hyperlipoproteinemia and atherosclerosis by feeding euthyroid or hypothyroid dogs a semisynthetic diet containing cholesterol and hydrogenated coconut oil. 15,23,26 Hypothyroid dogs quickly developed hypercholesterolemia accompanied by marked changes in the plasma lipoproteins. The production of arterial lesions in euthyroid dogs occurs only if the plasma cholesterol can be elevated above about 750 mg/dl. 15 The atherosclerotic lesions were recognized in the abdominal aorta, coronary and cerebrovascular arteries, and many of the peripheral arteries. However, there is little information on the histopathology of spontaneous canine atherosclerosis and the distribution of atheromatous and atherosclerotic lesions in the peripheral arteries. 4,9,21,26 Furthermore, there is very little information on when lipid accumulation appears in the aortas, coronary arteries, and peripheral arteries during the lifetime. In human medicine, atherosclerosis is considered to be a slowly progressive disease that begins early in life but does not become manifest until middle age or later, when the arterial lesions precipitate clinical manifestation by virtue of organ injury. 11,24 Fatty streaks composed of extracellular lipid accumulation and lipid-filled foamy macrophages appear almost always in the aortas of children >10 years of age; these fatty streaks are not significantly elevated and thus do not cause any disturbance in blood flow. Fatty streaks in the coronary arteries are less common than aortic streaks, but they begin to form in adolescence. However, aortic and coronary fatty streaks may be precursors of the atheromatous plaques that eventually develop into atherosclerotic plaques later in life. 11,24
In the present study, the morphology of splenic arterial lesions was thought to closely resemble the early stage of atherosclerotic lesions in the peripheral arteries of humans. 11,24 Immunohistochemical examination revealed that a CApoB-100 accumulation appeared in the splenic arteries of dogs 6 years of age. At older than 10 years, almost all of the central arteries were CApoB-100 immunopositive. Thus, lipid accumulations in the peripheral arteries may appear in middle age or later in dogs as well as humans. 11,24 These findings suggest that the lipid accumulation in splenic arteries may be age related, and these accumulation may be precursors of the atheromatous plaques that eventually develop into atherosclerotic plaques, occasionally resulting in splenic hemorrhage and infarcts later in life. In early reports, canine atherosclerosis occurred almost always in association with hypothyroidism or diabetes mellitus, with hypercholesterolemia or hypertriglyceridemia. 12,17,19,25 In the present study, we measured the serum concentration of cholesterol in eight dogs ≥6 years of age. They had serum cholesterol levels within normal ranges 7 but showed immunohistochemically the CApoB-100 accumulations in splenic arteries involved in the atheromatous plaques. These findings suggest that lipid accumulation in the peripheral arteries was not always induced as the result of hyperlipidemia in the dog.
Hyaline deposits or amyloid-like materials in arterioles and arteries of the spleen occur frequently in arteriosclerotic heart disease and hypertensive disease in humans. 3,6 These lesions are characterized by significant deposits of IgG, IgM, β1C- and β1A-globulin, and β-lipoprotein (LDL). 6 However, hyaline deposits or amyloid-like materials are negative with Congo red and with anti-human IgA, fibrin, and fibrinogen antibodies. The composition of hyaline deposits or amyloid-like materials may be based on an abnormality related to filtered and trapped plasma proteins in the wall and subendothelial spaces of vessels. 6 Other investigators have described the presence of immunoglobulins within the vessels with acute atherosis associated with intrauterine growth retardation and suggested that this condition may be related to an immunologic disorder, probably mediated by immune complexes. 12 In the present study, amorphous eosinophilic material coexisting with lipids (CApoB-100) in the splenic arteries was PAS positive and Congo red negative and was positive against anti-canine IgA, IgM, IgG, and albumin antibodies. Thus, amorphous eosinophilic material was not amyloid but immunoglobulin. The IgA positivity of the hyaline deposits differed from that of arteriosclerotic heart disease and hypertensive disease in humans.
In summary, lipid accumulation of splenic arteries may be age related, and these accumulations may be precursors of the atheromatous plaques that develop into atherosclerotic plaques and occasionally result in splenic hemorrhage and infarcts later in life. In addition, deposition of immunoglobulins, probably mediated by immune complexes, may play an important role in the development of canine as well as human vascular disease.
