Abstract
The use of murine models to investigate human diseases has been an invaluable tool. In the areas of inflammation and oncogenesis, such models have provided unique insights into pathogenesis and mechanisms to evaluate potential therapy. As such, one facet of these disease processes links inflammation and cancer. Inflammation is associated with at least 15% of the world's malignancies. One example of this relationship is documented in the association between colitis and colorectal cancer. To date, the precise molecular events linking inflammation and cancer remain unclear. A new paradigm that may bridge these processes includes the cancer stem cell hypothesis. In this review, murine models of colitis, colon cancer, and colitis-associated cancer are discussed in reference to the potential of this paradigm to clarify the relationship of these devastating diseases.
The development of cancer is complex and involves multiple common attributes. These features have been outlined in the landmark paper of Hanahan and Weinberg, 40 in which they state that these acquired features common to all cancers include: 1) the evasion of apoptosis, 2) self-sufficiency in growth signals, 3) sustained angiogenesis, 4) insensitivity to antiproliferative signals, 5) tissue invasion and metastases, and 6) limitless replication. In addition, tumors are able to evade the immune system. These findings hold true for colorectal cancer, the third most common cause of cancer and cancer deaths in the United States. 48
Recently, discoveries in the field of stem cell biology have led to a paradigm shift in the field of oncology. This new paradigm is called the “cancer stem cell” hypothesis 95 and posits that cancer is caused by a small population of stem cells constituting less than 5% of the tumor cell mass. These cancer stem cells are pluripotent, that is, they are capable of reconstituting the entire phenotype of the tumor. More important, they exhibit a property known as “self-renewal,” in which the stem cells replicate and produce one copy of the pluripotent cancer stem cell and another, more-differentiated cell. The result of the self-renewal property is that the primitive cell type is maintained after cell division and can thus reconstitute the entire tumor. Implications of this property are that 1) without destruction of these cancer stem cells, the tumors will continue to propagate; 2) signaling pathways may be able to distinguish the primitive cells from the more differentiated daughter cells; 3) late and distant recurrences may be due to the perpetuation of a tiny nidus of these cells; and 4) cells surrounding the tumor (the microenvironment or “niche”) may have important influences on the quiescence, division, proliferation, and invasion of cancer stem cells. So far, the clonal nature of colon cancer stem cells has not been definitively established.
Estimates suggest that currently, inflammation is associated with at least 15% of cancers. 23,55 This finding has at least three implications. First, these associations intimate that other types of cells, besides the epithelium, are involved in the pathogenesis of cancer and may serve as targets for therapy. Second, the relationships of these cells as they “cross-talk” may also be targeted in strategies for intervention. Third, these relationships may be discovered and defined early in the pathogenesis of malignancy and may serve as biomarkers.
Multiple examples of the relationship between inflammation and cancer have been noted for years, if not centuries. A recent discussion by Dvorak in the work entitled “the wound that will not heal,” 27 recalls the description of such an association since antiquity. Examples of these relationships are summarized in Table 1. With the exception of gastric cancer, in which the inciting pathogen is Helicobacter pylori, the pathogenesis of the other associations is incomplete.
Disease processes in which chronic inflammation is linked to cancer.∗
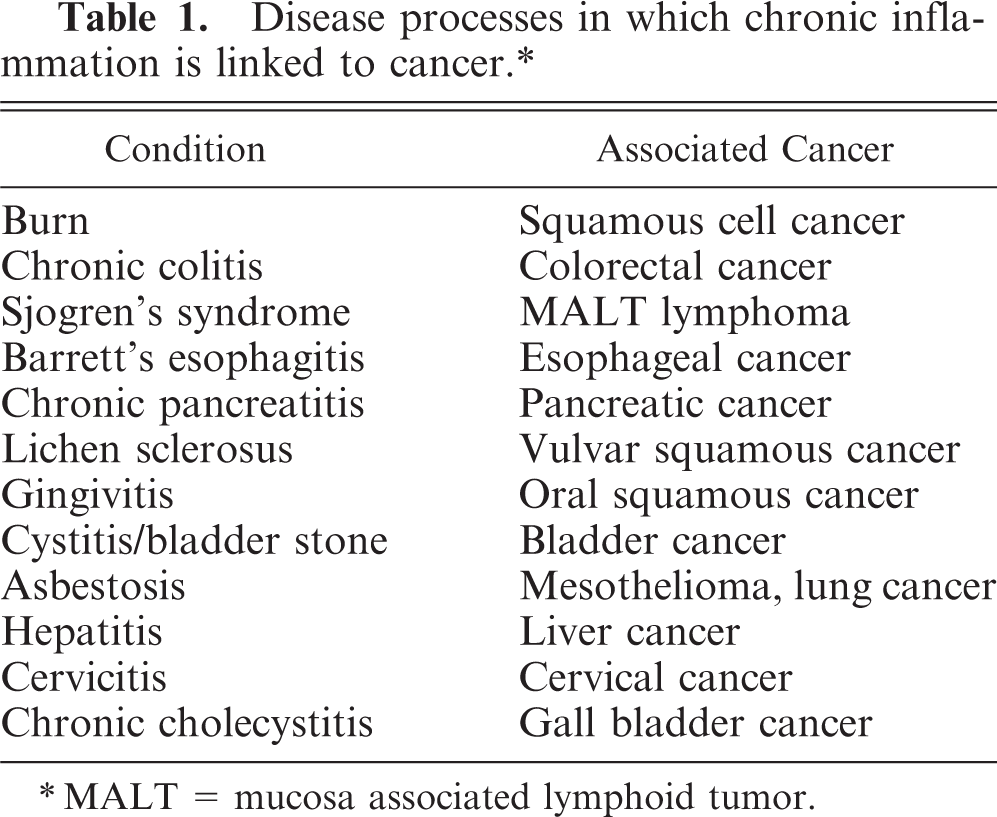
∗MALT = mucosa associated lymphoid tumor.
In the gastrointestinal tract, there are at least three examples of the link between inflammation and cancer. First is the relationship of H. pylori with gastritis and gastric cancer, second is the association of Barrett's esophagitis and esophageal cancer; and third is the link between colitis and colon cancer. Colitis, or inflammation of the colon, is a form of inflammatory bowel disease (IBD). The two dominant types of inflammatory bowel disease include Crohn's disease and ulcerative colitis (UC) (Table 2). Crohn's disease is an illness that affects the gastrointestinal tract anywhere from the mouth to the anus. The disease most often presents in the distal small bowel and usually manifests as abdominal pain owing to fistulas, abscesses, and strictures. The pathogenesis of this disease is unknown but is believed to be due to a combination of host bacterial flora, genetics, and the host immune system. This disease generally presents with “skip lesions” with discontinuous patches of disease in the alimentary tract.
Clinicopathologic features of Ulcerative Colitis versus Crohn's disease.∗
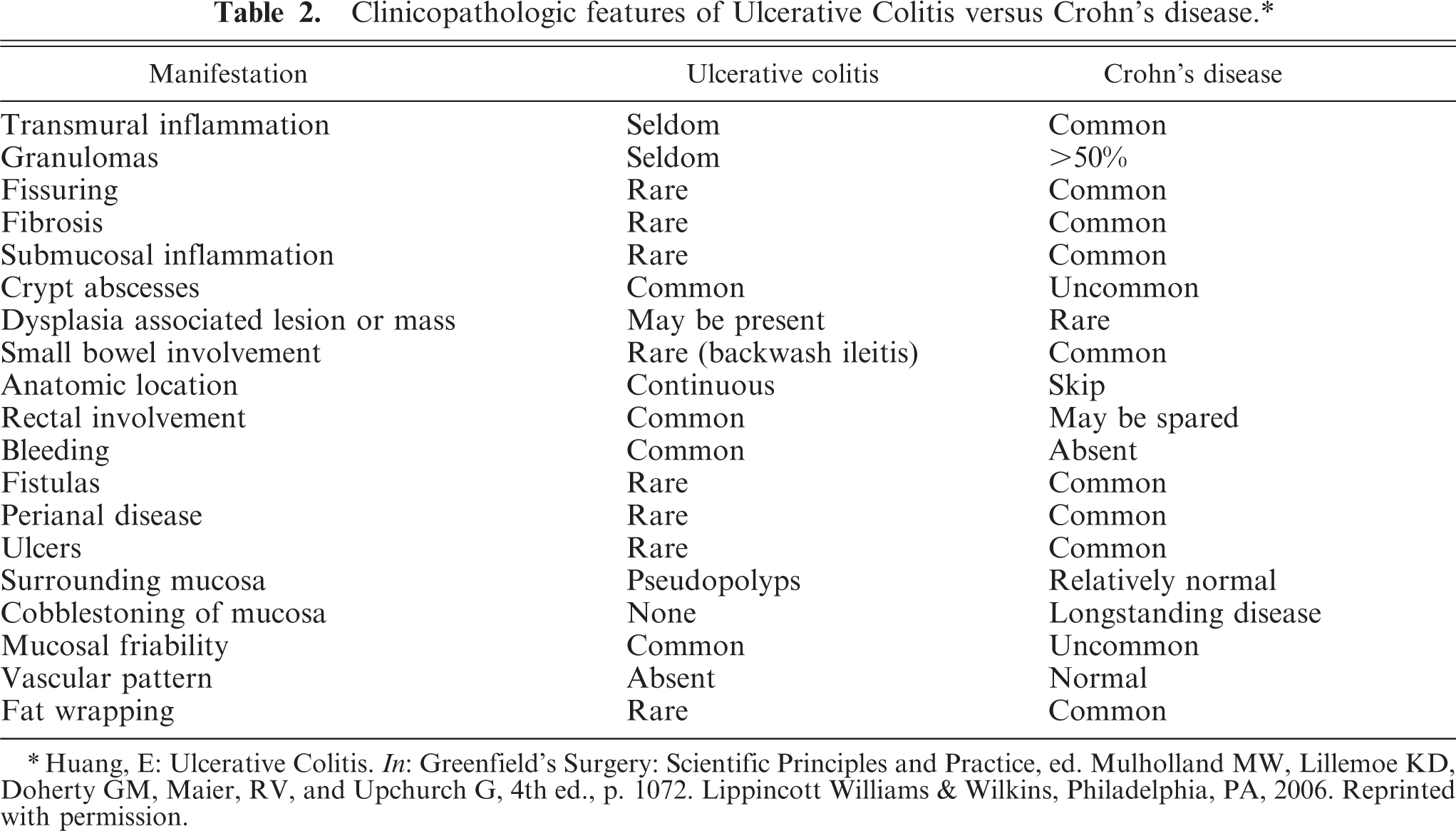
∗Huang, E: Ulcerative Colitis. In: Greenfield's Surgery: Scientific Principles and Practice, ed. Mulholland MW, Lillemoe KD, Doherty GM, Maier, RV, and Upchurch G, 4th ed., p. 1072. Lippincott Williams & Wilkins, Philadelphia, PA, 2006. Reprinted with permission.
Markers used in the isolation of colon cancer-initiating cells.
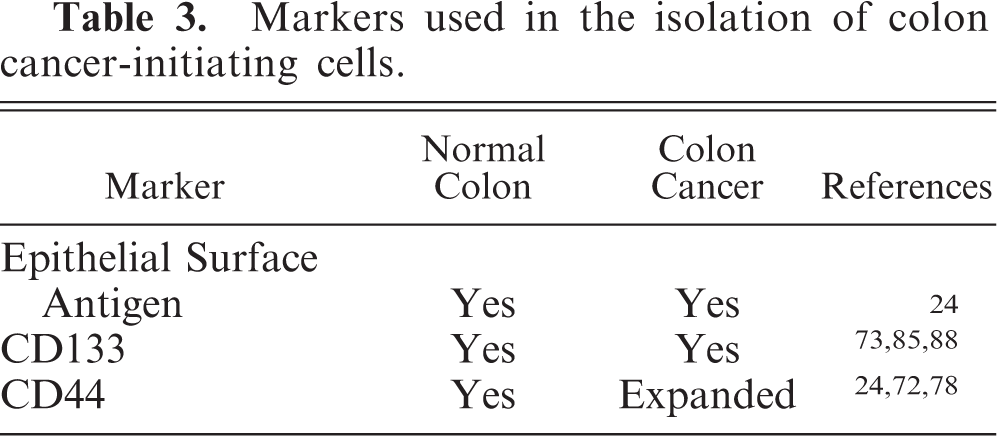
Whereas Crohn's disease has manifestations dominantly in the small bowel, UC is dominantly presented in the colon. The presentation normally begins in the rectum and extends proximally within the colon. If the disease affects the entire colon, then the distal small bowel may be affected as well, and this manifestation is known as “backwash ileitis.” In contrast to Crohn's disease, UC affects the mucosa and manifests with bleeding. In addition, the affected mucosa in UC does skip areas of involvement, and thus, is continuous. Like Crohn's disease, the pathogenesis for UC is unknown.
Both Crohn's disease and UC share multiple features and effect 4–6 people per 100,000 in the United States. 63 Extra-intestinal symptoms are present in both and may represent the protean manifestation. These symptoms include ophthalmologic manifestations such as iritis and uveitis; joint arthralgias and arthritis; skin abnormalities such as pyoderma gangrenosum; liver pathology, including sclerosing cholangitis; and back pathology, as in ankylosing spondylitis. Both diseases have indications that the pathogenesis involves a complex interplay of the host immune system with genetics and local flora. Most important, both diseases share an increased risk of malignancy, dominantly in the areas where lesions are found.
Current methodology to survey the small bowel is challenging; however, the advent of colonoscopy over 50 years ago has permitted both diagnosis and therapy of colonic pathology. For UC, the advent of colonoscopy has permitted establishment of the primary diagnosis with the extent of disease and biopsies to assist with the diagnosis. However, even with these tools, the diagnosis of colitis-associated cancer is quite challenging since the regions of malignant transformation may appear grossly normal. Though recent improvements in colonoscopic detection include special dye techniques, these techniques are not widely available. 26,68 Therefore, those patients who undergo surveillance colonoscopy to detect malignancy routinely are subjected to multiple biopsies—that is, 4–6 biopsies every 10 cm or so. As the length of the colon is between 1.5 and 2 m long, these patients receive 50–60 biopsies in order to obtain adequate sampling. 12,13,28 Since the progression in the pathogenesis is believed to include “inflammation to dysplasia to cancer,” histopathology that includes dysplasia nearly mandates the resection of the colon. Historically, this histology is associated with an incidence of 30% of occult colon cancer. 14 Indeed, patients with chronic colitis have an incidence of colon cancer which is five- to sixfold greater than the incidence of sporadic colon cancer. 14,28
The etiology of inflammatory bowel disease remains unclear, and the current battle against colon cancer is ongoing. Therefore, both colitis and colon cancer represent ripe models for analysis, not only of the primary disorder, but of the associations which likely link their pathogenesis. The molecular pathogenesis of each disease cannot be fully delineated within the confines of in vitro examination. Thus, animal models are required for interrogation. While primate models for inflammatory bowel disease do exist, practical limitations of cost and ease of manipulation limit the feasibility of use. Murine models of inflammatory bowel disease are the most suitable, in terms of cost. In addition, the advantages of well-established mouse genetics and the ability to manipulate the mouse genome through transgenic and gene “knock-in” strains greatly facilitate disease study in mice.
For oncologic purposes, many murine models of cancer have attempted to mimic human tumors as fully as possible. To replicate human tumors, the following criteria have been suggested:
The mice must carry the same genetic lesions as the human tumors;. The mutations must be engineered within endogenous loci;. The mutated genes must be silent during embryonic and early postnatal development;. Mutations must be induced or activated in specific target tissues or in selected cell types;. The mutations must occur in a limited number of cells;. The model should allow the induction of well-defined sporadic tumors with high penetrance but low numbers, such that the animal does not die from an overwhelming tumor burden; and. The tumors must develop within a predictable time period, such that analysis will occur during the lifespan of a mouse.
Many murine cancer models have helped elucidate molecular pathways, define mutations/deletions in cancer development, and validate key genes as therapeutic targets. 38 For oncologic models, the pathogenesis may be evaluated at multiple levels, including prevention, establishment, propagation/localized proliferation, and metastases. Of course, each model has its limitations, as well as its specializations.
For inflammatory bowel disease, several factors make the evaluation of mouse models of disease more complex. For example, strain differences and the presence of differing bacterial flora strongly influence the disease phenotype. Compounding this challenge is the fact that the pathogenesis of inflammatory bowel diseases is not as well understood. As a result, the models only mimic certain aspects of the disease processes. Nevertheless, like the other oncologic murine models, these models offer unique insights for prevention and intervention, and thus are invaluable for therapeutic and evaluation strategies.
In this review, we will discuss the use of murine models in the discovery and characterization of colon cancer stem cells (CSCs). In addition we will review the mechanisms by which murine models have been used to determine the implications of the CSC hypothesis on colonic oncogenesis, and the use of murine models for therapy directed against colon CSCs. Further, with reference to the microenvironmental contribution to colonic oncogenesis, we will explore the potential to use the CSC model to interrogate the detection, pathogenesis, and therapy of colitis-associated colon cancer.
The Adenomatous Polyposis Coli Murine Intestinal Neoplasia Mouse as a Model of Colonic Oncogenesis
This murine model of bowel tumorigenesis is perhaps the most widely employed model. The genetic abnormalities present in the oncogenesis of sporadic colon cancer were summarized in a landmark article by Fearon and Vogelstein in 1990. 30 Of importance, this manuscript provides the rationale for the current use of colonoscopy to remove polyps. This publication codifies the “adenoma to carcinoma pathway” paradigm in which genetic alterations in the pathway to cancer are paired with phenotype. As such, the earliest mutation, and the one most commonly identified in this pathogenesis, occurs in the adenomatous polyposis coli (APC) gene, a member of the WNT signaling pathway (Fig. 1). Though this pathway is commonly implicated in the homeostasis of the colonic epithelium, mutations in APC are found in 50% of colorectal neoplasms. 82 This gene is so named because of the association with the human condition known as familial adenomatous polyposis, or FAP (Fig. 2). In this autosomally dominant condition, FAP patients classically begin with the development of hundreds to thousands of polyps in their teen years. Without intervention, nearly all FAP patients will develop invasive cancer by their fifth decade of life. At the molecular level, many FAP patients carry a truncation mutation in APC. As a result, the tumor suppressor activity of APC is compromised, leading to a failure to sequester β-catenin and target its ubiquinylation and destruction. Thus, unabated passage of β-catenin from the cytoplasm into the nucleus results in the activation of multiple transcription factors including c-myc, cyclin D1, and c-jun culminating in cell proliferation. 20 Some FAP patients have normal APC but display mutations in other genes in this pathway. For example, 40% of affected patients display mutations in K-ras, downstream of APC. In addition, in approximately 60% of tumors, inactivating mutations or deletions of the tumor suppressor p53 are present. 6,7,17 There is also evidence that mutations in genes within the Smads/TGFβ (transforming growth factor β is a multifunctional peptide that controls proliferation and differentiation) pathway may also play roles in the pathogenesis of colorectal malignancies. Smads are transcription factors involved in the TGFβ signaling pathway and are so named because they are the mammalian homologs of the drosophila Mad protein and the Caenorhabditis elegans SMA protein. 43
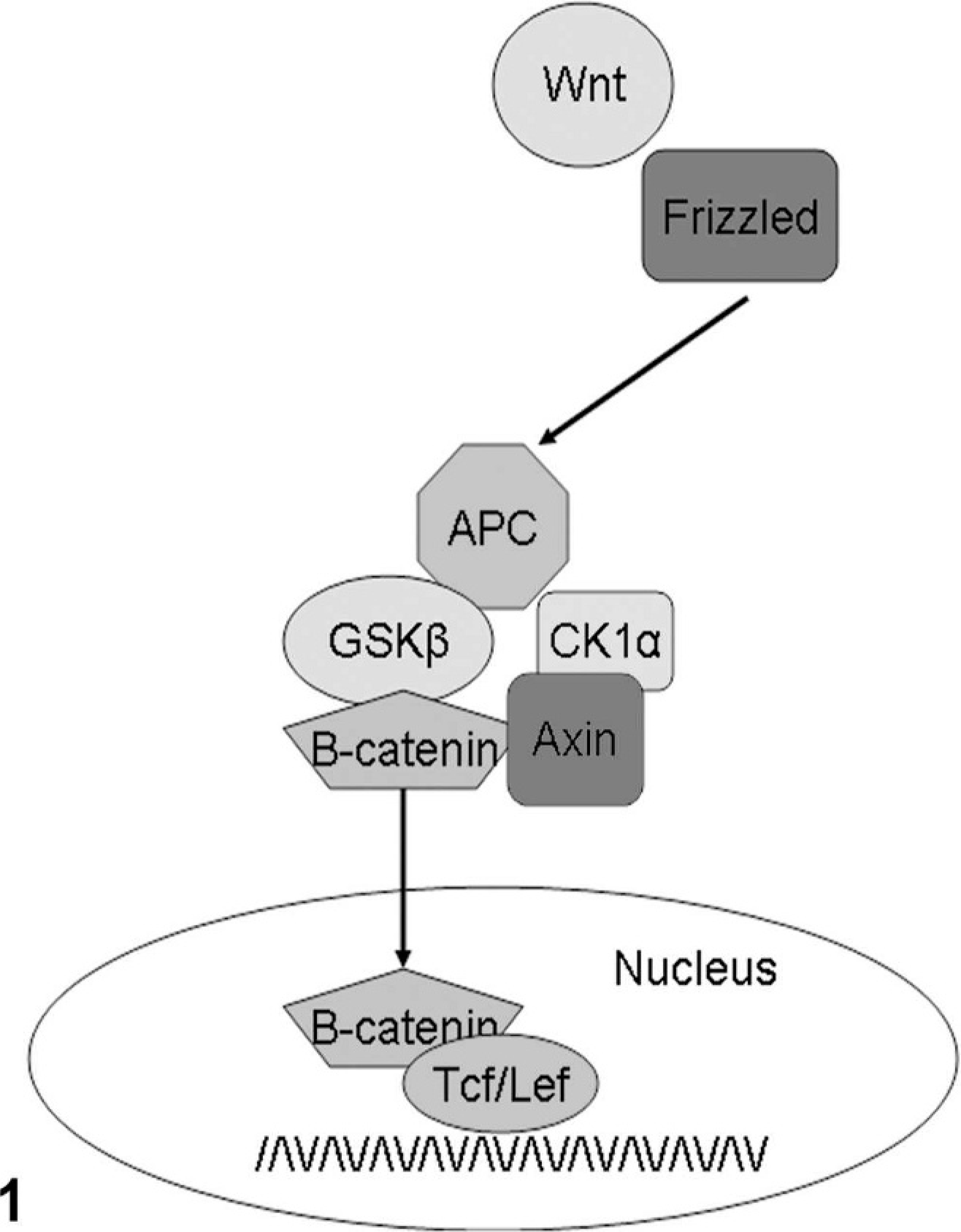
Schematic of WNT signaling pathway. Shown is the canonical WNT pathway. Briefly, a WNT agonist binds and activates β-catenin. If β-catenin is phosphorylated it will undergo ubiquinylation by the proteasome and degradation. If members of the complex, including APC glycogen synthase kinase (GSK3β), or axin, for example, are mutated and sequestration is incomplete, β-catenin will translocate to the nucleus where downstream target genes including cyclin D1 and c-myc will be activated.
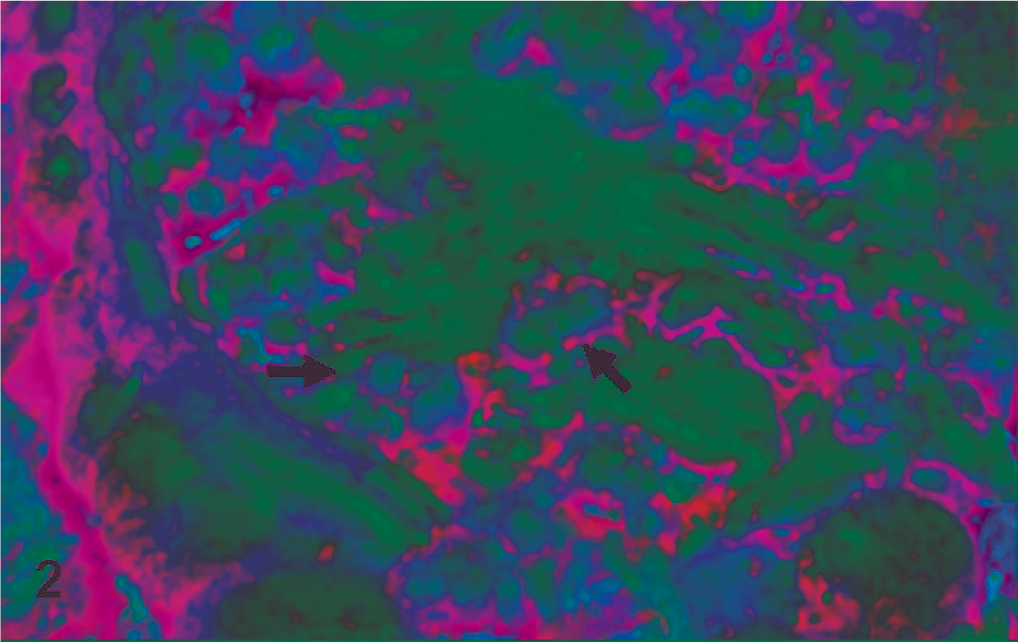
Colon from a patient with FAP. In the most common form of this disease, mutations in the tumor suppressor, APC, result in a truncated protein. Unable to sequester β-catenin, downstream target genes activated by this transcription factor result in multiple expressions of the phenotype, including hundreds to thousands of polyps in the colon (arrows). Without intervention, each of these polyps has malignant potential and will result in colon cancer during the fourth or fifth decade.
The APCMin (multiple intestinal neoplasia) murine model was generated by Moser in 1990. 70 Though the mutation created mimics that in the human, the location of the phenotype is quite different. While polyps are formed, the dominant location is in the small bowel, not in the colon. Often, the small bowel has 30 or more polyps, while the colon may have 1 or 2. The anemia resulting from slow bleeding from these lesions and obstructive lesions contribute to a decreased lifespan of these mice (approximately 16–20 weeks). Despite these differences, the APCMin mice remain the workhorse for prevention and therapeutic intervention.
The evaluation of additional mutations that occur in conjunction with the APC locus has added significantly to our understanding regarding the pathogenesis of colorectal cancer. For example, truncating APC mutations at codon 716 and mutations at codon 1638 result in very different phenotypes. The phenotype likely reflects the degree of APC that is lost. Though both mutations present as lesions in the small bowel, the mice have very different polyp numbers. The APCδ716 mice exhibit approximately 300 polyps, while the APC1638N may have only 3 polyps. 7,32,76 Though the dominant presentation in the APCMin mice presents as polyps in the small bowel, a mutation in the Cdx2 gene correlates with presentation of the polyps to the colon. 3 This shift in lesion location is thought to be due to the loss of heterozygosity of Apc caused by chromosomal instability.
Another interesting example of co-operating mutations in APC mice is the introduction of a cyclooxygenase (COX)-2 gene knockout, which dramatically decreases the polyp number in the APC model. 75 In these studies, the researchers conducted a retrospective analysis of polyps and found that COX-2 was present in polyps of all sizes. By introduction of the COX-2 gene into the APC mouse, both the number and size of polyps were reduced. Further, the APCδ716 mouse was then challenged with COX-2 inhibitors and it was found that the number and size of polyps were reduced. These data were substantiated in patients with FAP, who were given oral COX inhibitors. However, the chemoprevention trial prior to consideration of the broad introduction of COX-2 inhibitors for sporadic polyps was stopped due to an incidence of cardiovascular events. 39 The introduction of other mutations, for example, in the DNA helicase gene responsible for Bloom syndrome, also increases the number of polyps in the APCMin mouse, 37,64 while mutations in the matrix metalloproteinases, MMP-7, reduces the polyp number. 96
With reference to pathways that are implicated in self-renewal, the APCMin model has much to offer as well. Not only are β-catenin and the WNT pathway implicated in self-renewal, but cross-talk with other pathways may modify the expression. It is possible that the bone morphogenic proteins and members of the Notch signaling pathway may modify self-renewal by inhibition of WNT signaling. 41 In addition, mice that lack the Math1 transcription factor reveal that Math1 is necessary for determining cell fate of secretory cells. In colon cancer cells, Hath1, the human analog of Math1, shows decreased expression. As an example of how Hath1 influences differentiation and phenotype, its expression in HT29 cells decreases proliferation, anchorage-independent growth, and the expression of the mucin secretion–associated protein, MUC2. 58,59
The Use of Immunocompromised Mice to Isolate and Propagate Cancer Stem Cells
One implication of the cancer stem cell hypothesis is that tumors possess functional heterogeneity. The CSC hypothesis, therefore, posits that a rare subset of more primitive cells is responsible for the generation of the tumor, and that the majority of the tumor is composed of more differentiated cells without the capacity for self-renewal. This hypothesis is often portrayed in contrast to more traditional models of oncogenesis, in which multiple cells within the tumor have the capacity to generate the tumor. Known as a clonal evolution model, the accumulation of genetic events drives these cells, which are influenced by both epigenetic phenomena and microenvironmental cues. However, the models are not mutually exclusive, since mutations have likely occurred within the CSCs and have perpetuated this more hierarchical series.
Several authors have delineated a frequency of CSCs, within solid tumors, that may be substantially higher than in leukemias. However, these differences have at least two explanations. First, the longest experiences have been with leukemias, in which the first undisputed evidence for cancer stem cells was published over 15 years ago. This advance was possible as a result of improving technology with flow cytometry and surface markers. With the advent of multiple markers and cocktails of these markers, enrichment of CSCs will result in increased efficiency. Second, leukemias are fluid rather than solid. Thus, methodology for isolation and assays are seemingly less technically challenging than in solid tumor models in which the tumors must be dissociated prior to further discrimination. Furthermore, with the exception of skin tumors in which the orthotopic site is the skin, leukemias are much easier to place and to assay in the orthotopic site than the majority of solid tumors (colon, prostate, lung, and brain, for example).
Currently, the gold standard for CSCs consists of serial passage in xenografts, ideally in orthotopic transplantation assays. As evidence of self-renewal, the transplanted tissue or cells should recapitulate the phenotype of the parental tumor. Challenges with the techniques of cell dissociation, establishing markers for enrichment, and identifying appropriate recipient species for engraftment have all increased the difficulty of studying these rare cells.
Xenograft Models of Colon Cancer
Along with chemically induced mouse models of colon cancer, xenograft models of cancer have been invaluable in expanding our understanding of the biology of colon cancer. Xenograft models of colon cancer may be generated heterotopically, most commonly by implantation of cells subcutaneously, intrasplenically, or into the renal capsule. Alternatively, cell or tissue may be implanted into the organ of origin, in an orthotopic model. To avoid rejection of implanted tissue or cells, recipient mice should be immunocompromised. In hairless, athymic, T-cell deficient “nude” mice, the Nu gene has been mutated, making these mice a common recipient for the injection of established cell lines. 42 Mice with the nonobese diabetic/severe combined immunodeficiency (NOD-SCID) background are often chosen by investigators when implanting fresh tumor specimens. Mice with the SCID mutation have an intact innate immune system, but lack functional B or T cells, and have a DNA repair defect that interrupts normal lymphocyte maturation. 83 Both nude and NOD-SCID mouse models are discussed below.
The first successful heterotransplantation of human tumor tissue into immunodeficient mice was reported nearly 40 years ago, when Rygaard and Povlsen implanted a small piece of breast carcinoma into athymic, T-cell deficient nude mice. They also implanted a small specimen of colon carcinoma into the same type of nude mice and observed tumor growth from only one of the colon carcinomas. 87 Since then, xenograft models of cancer have been widely used in both academia and industry to study cancer biology and to evaluate therapeutics directed at various cancers. Subcutaneous xenografts are commonly used because they may be generated in mice without the use of anesthetics. In addition, the results are often consistent and reproducible and the tumors growing in the subcutis can be easily monitored and measured with a pair of calipers. Testing the efficacy of a potential drug is then simply a matter of allowing the tumor volume to reach an appropriate size, then initiating treatment, and then measuring the tumor volume in the treated and control groups in the weeks that follow. Subcutaneous xenografts established from human primary tumors also provide an efficient vehicle for propagating or expanding populations of primary human tumor cells.
While subcutaneous xenografts are relatively easy to establish and monitor experimentally, there are drawbacks to their use. 10 In a retrospective study by Johnson et al., 39 therapeutic agents were evaluated, comparing the antitumor efficacy of the therapeutics in subcutaneous xenografts to the clinical efficacy of the therapeutics in a phase II clinical trial. In only one case, a non–small cell lung cancer, was a statistically significant correlation found between the antitumor efficacy in the subcutaneous xenograft and the clinical trial counterpart. 50 The lack of correlation in this study illustrates one of the main drawbacks to using subcutaneous xenograft models. If, however, a high-throughput system to assay prolonged survival or tumor shrinkage is all that is required, a subcutaneous xenograft model is a valuable and appropriate model.
Another drawback of the subcutaneous xenograft model of cancer is that tumors grown subcutaneously lack many of the stromal cells and immune cells, and the vascular network of tumors growing in the organ tumor of origin. 25 In this way, they are not a true representation of the biologic situation. Of interest, most cells or tissues implanted subcutaneously rarely metastasize. 31 The absence of metastasis in the subcutaneous model is of particular importance for the study of colon cancer, where hepatic metastases will ultimately be found in nearly 50% of patients with the disease. 15 Other heterotopic xenograft models, including intrasplenic implantation and injection under the renal capsule, have a demonstrated ability to metastasize. 34 However, there are still shortcomings with these models as cells injected into the spleen and renal capsule do not completely mimic the pathway taken by cells metastasizing from the original tumor site. 31 For this reason, and particularly if a more accurate metastatic model of colon cancer is needed, many investigators choose to implant cells, or preferably tissue if available, orthotopically. 34,35
If the goal of an in vivo model of colon carcinogenesis is to examine aspects of the tumorigenic microenvironment of the original organ, then an orthotopic model is clearly preferable to a subcutaneous xenograft model. Unlike the subcutaneous model, the orthotopic model has all of the elements of the microenvironment, including fibroblasts, endothelial and immune cells, and all of the angiogenic factors, growth factors, and cytokines these cells produce. Recent evidence provided by Le et al. has suggested that stromal cells within the colon tumor microenvironment help maintain a putative cancer stem cell population, and this microenvironment enables these cells to metastasize. 56 A mouse model that accurately recapitulates these conditions would be extremely useful. There are a number of studies that have shown that the orthotopic site of implantation is required for the metastasis of cells. 31,35,44 In addition to a greater metastatic efficiency, an orthotopic model would also allow elements of the microenvironment, such as fibroblasts, cells of the vasculature or immune system, to be manipulated and studied experimentally.
The orthotopic model is not without drawbacks, however. Orthotopic procedures are more challenging technically and require more time to establish than subcutaneous models. Furthermore, unless cells are labeled with an appropriate reporter (such as luciferase [Figs. 3, 4], green fluorescent protein [GFP], or red fluorescent protein [RFP]), measuring tumor growth or the efficacy of a drug treatment is more difficult. In the orthotopic model, tumor growth may no longer be measured simply with calipers, as is done in the subcutaneous model. Indeed, analysis may require animals to be sacrificed at a predetermined time point. Ultimately, the end point or goals of the experiment will dictate the type of model used.

Colon cancer cells transduced with luciferase cassette. One method of detection of microscopic foci of cells in murine models is by labeling them with a reported construct. In this case, the luciferase cassette has been transduced via lentivirus into the SW480 colon cancer cell line. An imaging system that detects luminescence proffers a colorized input corresponding to signal intensity.
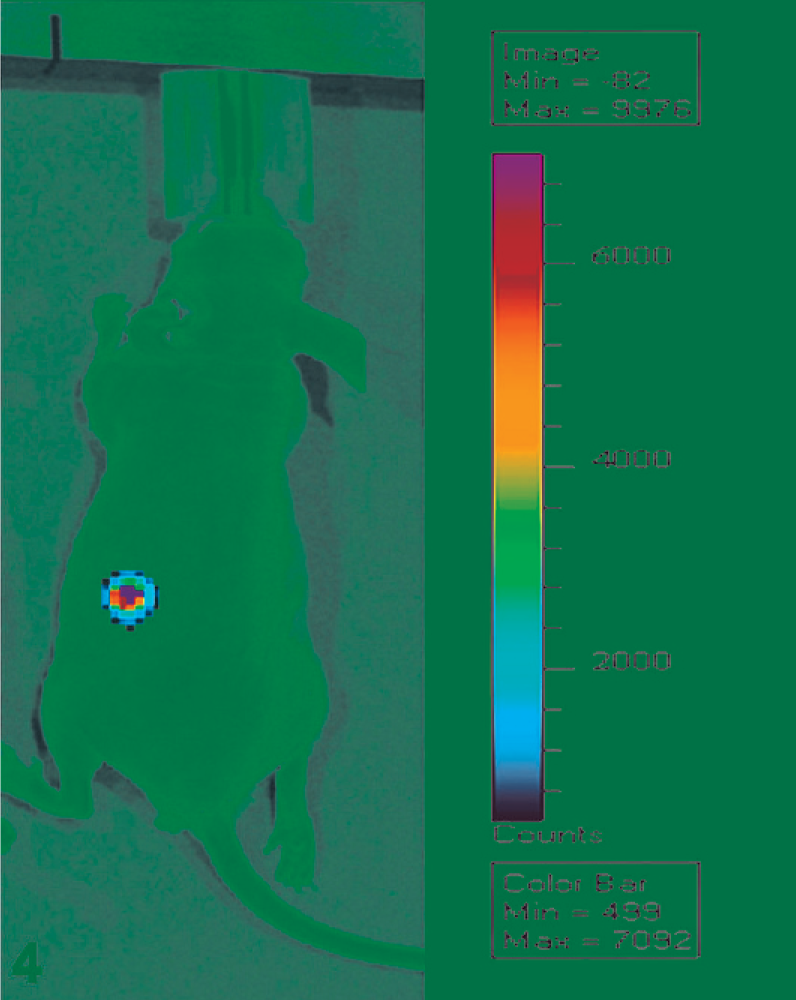
Luciferase-bearing colon cancer cells; subcutaneous tumor. In the skin, tumorigenic growths may be palpable. However, small lesions may defy palpation. In this image, 10,000 luciferase-bearing colon cancer cells have been placed into the subcutaneous position of an athymic nude mouse. The substrate for luciferase, luciferin, has been administered, and the mouse has been maintained in a sedated state for image analysis.
Xenographic Mice made with Cancer Cells/Tissue
For either type of xenograft mouse model, established, commercially available cell lines represent an accessible, reproducible source for establishing tumors. However, cell lines grown after repeated passages in culture are subject to varying selective pressures and may develop mutations that are not truly reflective of the genetic characteristics of the original tumor. Therefore, many investigators choose to use human tumor specimens, when available, to establish colon cancer xenografts. Both orthotopic and subcutaneous xenografts have been generated using a number of commercially available cell lines, including HCT116, HT29, SW480, DLD-1, and LS174T (Figs. 5–7).

Luciferase-bearing colon cancer cells; orthotopic injection. A relatively small number of luciferase-transduced colon cancer cells have been placed in the orthotopic position of the colon known as the cecum. By imaging the mouse with luciferin, the areas of luminescence correspond to organs bearing the tumorigenic cells.

Luciferase-bearing colon cancer cells; metastatic location. Evidence of metastatic disease is visualized in the liver, following an initial cecal implant of luciferase-labeled colon cancer cells.

Luciferase-bearing colon cancer cells; orthotopic imaging. The cecum of a mouse with a successful orthotopic xenograft demonstrates luciferase activity.
Human colon tumor specimens may also be used as a source to generate xenografts. For this technique, fresh tumor specimens should be placed in a sterile tissue culture dish. After cutting away any necrotic tissue with a sterile scalpel and scissors, the remaining tissue should be trimmed into 2 × 2 mm pieces, before implanting into an immunocompromised mouse.
Human tumor specimens may also be enzymatically dissociated and injected as a single cell suspension of bulk tumor cells. A single cell suspension of bulk colon cancer cells may be made from an intact colon tumor specimen in 2 to 3 hours. The tumor is first minced into fine fragments, and then digested with a mild collagenase. A study by Fu et al. has shown that disrupting the architecture of the original tumor by enzymatic dissociation may reduce its metastatic capacity. 33 Nevertheless, many investigators find that injecting a single cell suspension is easier and less time consuming than implanting an intact tumor. If, however, this bulk cell suspension is processed one step further, and the bulk tumor cells are stained with fluorescently conjugated antibodies directed at specific cell surface markers, the process of fluorescently activated cell sorting may identify the truly tumorigenic cells within the human colon cancer tumor specimen.
Cancer Stem Cells and Colon Cancer
As mentioned above, recent discoveries in stem cell biology have led to a paradigm shift in oncology. Cells capable of initiating tumor growth when heterotransplanted into immunodeficient mice were first identified in acute myeloid leukemia. 16 Since then, the cancer stem cell concept has been expanded to include solid tumors of the breast, brain, pancreas, and prostate. 1,21,60,90 Three recent studies have provided evidence for the existence of colon cancer stem cells, or colon tumor–initiating cells. 24,73,85 O'Brien et al. 73 isolated cells from 17 human colon tumor specimens by flow cytometric analysis based on the cell surface marker CD133. When injected under the renal capsule in immunodeficient mice, cells with the CD133+ phenotype consistently resulted in tumor growth, while cells that were CD133− failed to initiate tumor growth when injected at the same dilution.
Ricci-Vitiani et al. 85 also isolated and expanded colon cancer cells based on the CD133 cell surface marker. To test the self-renewal capacity of these putative colon cancer–initiating cells, CD133+ cells were repeatedly passaged as spheres in culture. An initial, single cell suspension of CD133+ cells was able to self-renew and grow into spheres containing both a CD133+ and CD133− population. When tested for tumorigenicity by injection into immunodeficient mice, the CD133+ cells and not the CD133− cells were able to initiate tumor growth.
In a more recent study, Dalerba et al. 24 identified a population of colon cancer–initiating cells based on the cell surface marker CD44. Cells with a CD44+ phenotype isolated from human colon cancer xenografts were tumorigenic when injected into immunodeficient mice, whereas cells with a CD44− phenotype were not. In the same study, Dalerba et al. also found the tumorigenicity of the CD44+ population was further enhanced when the cell surface marker CD166 was also positively identified on the surface of the CD44+ cells. These 3 studies provide evidence for the existence of colon cancer stem cells that are able to self-renew, are capable of both initiating tumor growth and maintaining tumor heterogeneity, and may be prospectively identified on the basis of cell surface markers. Some of the cell surface markers relevant to colon cancer–initiating cells are discussed below.
Markers Used to Enrich Colon Cancer Stem Cells
Epithelial specific antigen, (ESA) is widely expressed in proliferating cells of the intestinal epithelium and may be considered a general marker for tumor cells of epithelial origin. 61,97 When isolating cells by fluorescence-assisted cell sorting using multiple cell surface markers, ESA is often used as a broad epithelial marker to limit the nonspecific staining of other markers. For example, CD133 marks endothelial cells, but ESA used in conjunction with CD133 eliminates this lack of specificity. Other investigators have examined the role of the epithelial cell adhesion molecule (EpCAM) as a potential cancer stem cell target. While EpCAM may be a marker for tumor epithelium, however, most consider that EpCAM is present on normal epithelium as well. Not unlike the reports of CD44 antagonism, this report involved the construction of an EpCAM/CD3 bispecific antibody construct. 2 These authors showed that intravenous injections of the construct were highly effective in both reducing growth of the human colon SW480 xenograft model and, at a 10-fold higher dose, completely inhibiting tumor growth.
CD44 is a cell surface glycoprotein involved in cell adhesion and cell–cell interactions. 72,78 CD44 is a receptor for many ligands of the ECM including, collagen, fibronectin, laminin, and hyaluronan. 36 There is evidence that CD44 is pro-oncogenic, due to its cell–ECM interactions. 67 Furthermore, CD44, along with its ligand hyluronan, may confer a degree of chemoresistance in cancer cells. 93 Recent evidence has also suggested that CD44 is a target of the WNT pathway in affecting tumor initiation in APCMin mice. 98
The contribution of CD44 has been queried in multiple studies. As detailed above, CD44 is a downstream member of the WNT signaling pathway. However, CD44 also has a broad distribution in the normal crypt, detected in up to one third or one half of the lower portion of the crypt (Fig. 8). Antibodies to CD44 were used in a study by Jin et al. in a leukemic model of cancer. 49 By prevention of homing to the respective niche, the use of a stem cell marker in a therapeutic fashion disabled the further progression of leukemia. These studies support the targeting of an inflammatory and stem cell marker as a therapeutic strategy.
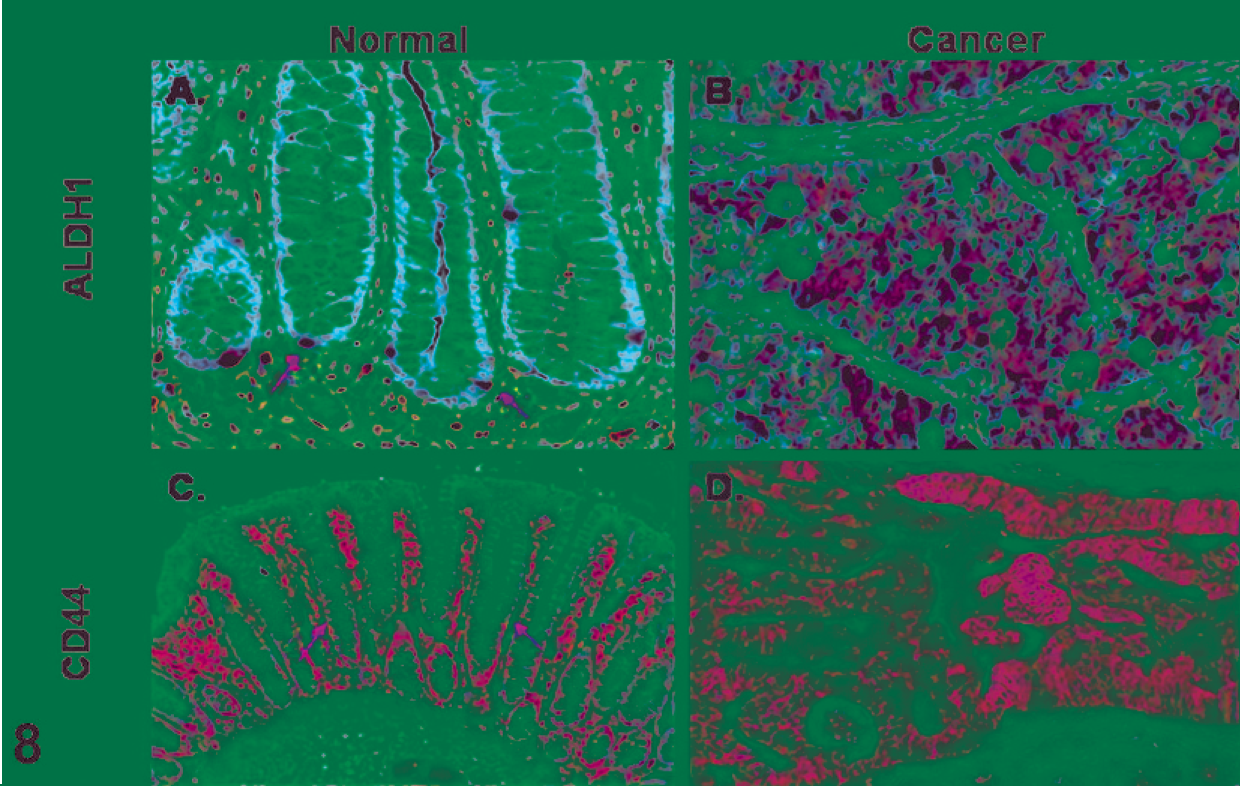
Immunohistochemistry for CD44/ALDH on normal colon and colon cancer. Immunohistochemistry ALDH1 on normal colon and colon cancer demonstrates rare cells with ALDH expression at the base of the crypt in the normal colon (Figs. 8A, arrows), which may expand to encompass the entire tumor (Fig. 8Brpar;. CD44 expression is seen in the basal third to half of the normal crypt (Fig. 8C), with expansion to the entire tumor (Fig. 8D). Magnification 200× for Fig. 8A, C; 100× for Fig. 8B, C.
Another role for the stem cell/progenitor marker CD44 is seen in a study in which CD44 null mice were crossed with APCMin mice (see section The Adenomatous Polyposis Coli Murine Intestinal Neoplasia). Constitutive activation of the WNT transcription factor, β-catenin, results in increased CD44 expression. The investigators posited that absence of this marker would therefore, be associated with diminished tumorigenesis. Indeed, the CD44−/APCMin mice had approximately 50% fewer adenomas. 98
CD133, or Prominin 1, is a five-transmembrane domain cell surface glycoprotein of unknown function. In spite of the lack of knowledge pertaining to its function, CD133 is used as a marker for stem cells in both normal and cancerous tissues. Expression of CD133 has been reported in normal endothelial progenitors, 72 and in normal hematopoietic, 94 fetal brain, 90 and prostatic, epithelial stem cells. Cell surface expression of CD133 has also recently been used to identify cancer stem cells of the prostate, 21,86 pancreas, 44 and colon. 73,85
To date, a few markers, including CD133 and CD44, have been utilized to enrich colon cancer stem cells. Compared with CD44, immunohistochemistry for CD133 has been less successful, although commercially available antibodies do work well for flow cytometry. CD133 has been reported to be present both in multiple adult organs, putative adult stem cells, and putative adult cancer stem cells 77,86,89,90,92 suggesting a broader distribution for this protein, which would be inconsistent with the cancer stem cell hypothesis. Thus, Shmelkov et al. 88 used elegant murine–based technology in an attempt to reconcile conflicting data. In these studies, Shmelkov et al. created a transgenic mouse model using a murine CD133 endogenous promoter to drive expression of the lacZ reporter gene. The lacZ gene product β-galactosidase catalyzes the hydrolysis of the substrate 5-bromo-4-chloro-3-indolyl-β-D-galactopyranoside (X-gal) to produce a blue color that is easily seen with a microscope. Limitations of commercially available antibodies for immunohistochemistry would thereby be obviated by the increased efficiency of X-gal. Specifically, within the colon, these authors found that CD133 was expressed in the full spectrum of undifferentiated and differentiated colonic epithelial cells. In their CD133lacZ/+ mice they documented β-galactosidase activity along the entire crypt, especially near the luminal surface, where the differentiated columnar epithelial cells exist.
With respect to the relationship between inflammation and cancer, these same authors used another mouse model to discern the role that CD133 might play in a spontaneous murine model. To accomplish this task, the authors created a complex transgenic mouse consisting of CD133lacZ crossed with the IL10−/− mouse 11,54 IL10 is a regulatory cytokine produced mainly by T cells and macrophages. IL10 is a potent inhibitor of macrophages in the Th1 cell subset, normally down-regulating T-cell reactivity to enteric bacteria. The IL10−/− mice develop anemia, growth retardation, and chronic inflammatory bowel disease. The inflammation occurs in both the small intestine and the colon, and is reduced in germ-free environments. 66 The pathology consists of thickening of the intestinal wall, with depletion of goblet cells, degeneration of the epithelium, and an increase of major histocompatibility complex (MHC class II) expression in the colon. In the appropriate environment, up to 60% of these mice develop colon cancer. 11 In the IL10−/− CD133lacZ mice, the spontaneously developing colon cancers all expressed CD133 and all expressed ESA, an epithelial marker.
Due to additional concerns regarding the specificity of CD133+-enriched cells in human colon cancer, these authors obtained colon cancer metastases and performed flow cytometry to enrich for both the CD133+ and CD133− populations. Of interest, from these isolates, both populations grew in vivo and in vitro. Furthermore, the CD133− populations grew faster in vivo, and expressed CD44.
Aldehyde dehydrogenase (ALDH) is a detoxifying enzyme necessary for the oxidation of intracellular aldehydes. ALDH, by virtue of its role in oxidizing retinol (vitamin A) to retinoic acid, is believed to be involved in the differentiation of stem cells. 19 ALDH is highly expressed in hematopoietic stem and progenitors cells, 4 and in stem cells of the brain 22 and acute myeloid leukemia. In the colon, ALDH expression is limited to rare cells at the base of the colonic crypts (Fig. 8). This expression expands, particularly at the leading edge of colon cancer.
Self-renewal Pathways in Colon Cancer Stem Cells
As stated above, the APC-Min mouse bears the same genetic mutation as patients with FAP. That is, they bear a defect in the canonical WNT pathway. Murine models have confirmed the necessity of this pathway in order for proper colon development to occur. In fact, when key controls of normal transcription fail, normal crypt development fails, as do those genetic alterations resulting in mutations in inhibitory pathways. As in all development, the WNT pathway (Fig. 1) is not the only operative or required signaling pathway. At least 2 other pathways likely influence homeostasis and pathology. The first of these pathways is the Notch pathway. The Notch pathway and the WNT pathway act in concert to maintain undifferentiated cells in the normal state.
Another pathway implicated in gut homeostasis is the bone morphogenic pathway (BMP/SMAD). Evidence for this pathway emanates from another disease process called Juvenile Polyposis Syndrome. In this disease, mutations in either the SMAD4 gene (20%) or in the BMP receptor 1A (25–40%) account for the phenotype and are manifested as intestinal hamartomas, which may become malignant (20%).
These pathways have crossroads at another level, involving a downstream signaling cascade involving phosphatase and tensin homologue (PTEN). Of interest, PTEN mutations are responsible for Cowden's disease, which causes hamartomas of the skin and polyps in the colon. In a study by He et al. 41 , a cre-conditional BMPR1a mouse mutant was created in which the receptor was deleted within the small bowel. As PTEN is a negative regulator of Akt, phosphorylated Akt was detected in proliferating intestinal cells. Akt is an enzyme serine/threonine kinase important in cell survival. He et al. elegantly demonstrate that phosphorylated or inactive PTEN, via Akt, acts in concert with WNT to activate β-catenin.
Further, these researchers demonstrate that both phosphorylated PTEN and phosphorylated Akt are present in the BMPR1a mutant mice. Histologic evidence of nuclear accumulation of β-catenin in these mice reveals that the WNT pathway is inhibited by BMP via regulation of PTEN. Taken together, this evidence connects these pathways and suggests that these pathways have important roles in self-renewal.
Experimental Murine Models of Inflammatory Bowel Disease
Though progress has been made, the pathogenesis of inflammatory bowel disease has not been fully elucidated. It is widely felt that a combination of factors, including innate and adaptive immunity, barrier function, genetics, and environmental factors such as the colonic microbes, all contribute to the inflammatory bowel disease phenotype. Within the last 10 years, advances in genetics and high throughput analysis have identified the susceptibility gene known as NOD2 (CARD15 and IBD1). 74 The discovery of this gene was seminal, as the gene was linked to the host response to bacterial challenge. However, only 20% of the patients with Crohn's disease have a NOD2 genetic defect. 74 Recent advances in the fields of immunology have also linked new T-cell subsets to colitis, including those known as Th17 with cytokine IL23. 71 Many investigators categorize UC as a Th2-dominant disease with a cytokine profile of IL4 and IL10, while Crohn's disease is believed to be Th1 predominant, with expression of IL2 and gamma interferon. 5,69
In mice, the effect of host genetics may also be expressed as their susceptibility to colitis. Indeed, different strains may have completely different responses to both engineered genetic changes or different responses to the same agent. For example, the response to dextran sodium sulfate (DSS) is completely dependent on strain. As an example, the C3H/HeJBir mouse has proven highly susceptible to DSS colitis; whereas the C57Bl/6 mouse is somewhat resistant. 65 This observation led researchers to seek areas within the murine genome that might predict susceptibility. 91
Our attempts to interpret the impact of the immune system on colon disease processes have been quite focused. As a result, the role of the epithelium in preventing colon cancer often goes understudied. Indeed, the epithelium forms a barrier to stool and to the bacterial flora. These epithelial cells release chemokines when in contact with pathogens and thus cross-talk with other members of the cellular environment. Furthermore, breaches in the epithelium will affect how the epithelium responds. Therefore, the study of the epithelium in light of the cancer stem cell paradigm may help us understand the basis for regeneration and repair.
Colitis-derived Tumor-initiating Cells
Humans with longstanding inflammatory bowel disease are at increased risk for the development of colorectal cancer. As stated in the introduction, inflammatory bowel disease, which includes UC and Crohn's disease, affects 4–6/100,000 people in North America. 63 In the colon, the dominant presentation of colitis is UC. In UC, the initial risk of neoplastic transformation is 0.5–1%/year in the first 7 years; thereafter, the risk increases 1%/year to 18% by 30 years, representing a relative risk of colon cancer that is 2.6- to 5.4-fold over the general population. 14,28 These colitic patients are often maintained on immunosuppressive agents in attempts to ameliorate their symptoms. Though the presence of dysplasia is largely believed to precede the advent of invasive adenocarcinoma, the molecular events that control the latency and the progression from dysplasia to cancer are not well understood. One strategy used to identify neoplastic transformation is surveillance colonoscopy of UC patients, which involves multiple biopsies, obtained every 5–10 cm for a total of 40–60 biopsies per colon. 12,13,28 Unfortunately, this colonoscopic sampling procedure is associated with morbidity, and the possibility of sampling error, because the dysplastic or malignant lesions often appear grossly normal.
Though alternative techniques for the detection of dysplasia include chromoendoscopy and narrow band imaging, these techniques have not yet been standardized or widely adopted. 26,69 Of significance, the identification of high-grade dysplasia in these patients mandates colectomy due to the 30% incidence of occult invasive cancer. 14
The relationship between chronic inflammation and cancer is provocative, yet the precise mechanisms for this pathogenetic link are not clear. One compelling example of the link between chronic inflammation and neoplastic transformation is the infectious agent, H. pylori. This bacteria causes chronic gastritis and gastric cancer and has added credence to yet another model where chronic inflammation potentiates neoplastic transformation. 46 Colitis-associated cancer (CAC) involves the “inflammation-dysplasia-carcinoma” sequence while the “adenoma to carcinoma” sequence is the prototype for sporadic carcinoma. 30,47 The molecular events associated with the evolution of these 2 cancers also appear to proceed in different orders. For example, sporadic colon cancers are associated with APC mutations early in their pathogenesis. In contrast, colitis-associated cancer is believed to possess p53 mutations or loss of heterozygosity early in the pathogenesis, with APC aberrations later in the pathogenetic pathway. 30,47
Though long-standing colitis is associated with a risk of cancer that is at least fivefold increased over sporadic cancer, tumorigenic stem cells directly from colitis have not yet been reported. However, evidence exists that stem cells must exist in the normal colon and that they are likely present in the colitic milieu. The colon is an organ in which the epithelium is shed into the lumen every 3 to 5 days. With this turnover, the crypts repopulate. The stem cells are believed to be located at the base of the crypts. 57,62,79,80,84 However, the challenge has been to identify markers that define these stem cells. As discussed above, flow cytometry or other techniques for enrichment have been used as techniques to enrich for cells with tumorigenic potential from frank colon cancer. These studies 24,57,62,73,85 employed the surface markers CD133 or CD44. Whether the expression of CD133 is unregulated in colitis is not known; however, the expression of CD44 in colitis is increased. 53 The increased CD44 expression is expected, as CD44 is expressed downstream in the WNT signaling pathway.
Recently, an elegant set of experiments by Barker et al. 9 revealed that Lgr5 may be a marker of normal stem cells in the mouse. This marker was identified from a screen of proteins downstream of the transcription factor Tcf, 8 which is a downstream transcription factor in the canonical WNT pathway. As mentioned above, the WNT pathway is heavily implicated in the pathogenesis of sporadic cancer. Further, β-catenin is the cytoplasmic molecule that translocates to the nucleus to activate Tcf and has been implicated in the maintenance of “stemness”. Barker et al. 9 implies that the expression of this marker is increased in neoplastic states.
Grossly, a phenotype in the colon indicative of increased stem cell activity is difficult to discern. However, crypt fission, histologically evident as branched crypt structures, may be one method of determining whether there is increased stem cell activity. Crypt fission is believed to result as a consequence to damage to the crypt as a regenerative event, including colitis whether the source of colonic injury is infectious, inflammatory, ischemic, or traumatic. 52,80,81 Recent evidence suggests that the normal stem cell resides at or near the base of the crypt. 9 Destruction of the crypt via any process results in the necessity for regeneration of both the crypt epithelial elements as well as the microenvironmental stromal elements, which include immune cells, endothelia, and fibroblasts.
The finding that stem cells are likely at the base of the crypt is intriguing in light of the evidence of regeneration of the crypt/stem cells by the presence of crypt fission. Taken together, these results suggest the possibility of testing the relationship between stem cells and crypt fissions. Another important finding regarding the cells found in the crypt comes from work on the autosomally inherited condition of FAP. Specifically, Kim and Shibata 52 analyzed methylation patterns in grossly normal appearing mucosa and contrasted these to normal mucosa from non-FAP colons. The methylation pattern diversity was higher in normal appearing crypts from 4/5 FAP colons compared with 6 non-FAP colons. These findings suggest epigenetic phenomena, which may be more similar in mucosa with baseline genetic alterations. Further, they reflect that cancers and their mutations may reflect a lifetime of competition, first between stem cells during pretumor progression, and later between tumor cells during tumor progression.
Similar findings of Chen et al.
18
reveal that genetic instability in the epithelium of patients with UC is present in nondysplastic mucosa of UC patients with dysplasia or cancer elsewhere and persists at a similar level throughout the histologic progression to cancer. In these patients, genetic instability as measured by DNA fingerprinting is widespread, precedes neoplastic transformation, and may be related to the extensive and chronic inflammation that defines UC. These findings are likely due to the accumulation of reactive oxygen species and reduced oxidative defenses. To investigate this possibility, the researchers examined clonal expansion and clonal succession in individual crypts in clusters of crypts (100 adjacent crypts combined). To document such a possibility, they used dual-color fluorescent in-situ hybridization (FISH) to detect and track the specific mutational alterations in individual crypt cells, since FISH can identify chromosome alterations in single interphase cells. Their findings included the following:
Band gains were more common, usually in only 1 or a few crypts. Genomic instability is low in the epithelium from UC nonprogressors. Colonic crypts of UC progressors have 10 to 20% of DNA mutated at any given time.
18
In contrast, the background DNA alteration in normal colon biopsies is <5%. In crypts from UC progressors, the mutational load does not differ between the non-dysplastic and the dysplastic crypts. Using a single nucleotide polymorphism (SNP) array they determine that in the UC patient with colon cancer elsewhere, there is a rate of 27% of loss of heterozygosity compared with a UC nonprogressor, in which the rate is <1. Alterations such as p53, measured by FISH, demonstrated that abnormalities are shared by all of the crypts, fissioning and the surrounding crypts, and supports the view that multiple fission events can lead to a clonal patch with branched crypts surrounded by crypts containing the same mutation. Further the p53 alterations that were present in the cells on one side of the crypt branch were duplicated in the cells of the opposite side branch. These findings suggest that a possible mechanism of mutation expansion could occur through crypt fission. Multiple protective mechanisms within cells may prevent damage from exceeding a catastrophic level, including both p53-dependent and independent apoptosis. One possible mechanism includes the natural progression of the epithelium, which constitutes the crypt, in which mutated cells are lost as daughter cells in the crypts that migrate to the lumen and are sloughed off. Further, the final stages of tumorigenesis in the chronic inflammatory setting occur when an accumulation of select mutations allows clonal progression to overtake the balancing forces of cell death and loss. These results are highly suggestive of a stem cell basis for colon cancer.
Limitations to isolation or enrichment of these cells from colitis include the identification of markers and the appropriate models for study. Perhaps, during an inflammatory event, such as colitis, cells from the bone marrow are recruited to assist with repair. In a parallel system, relationship between gastritis and gastric cancer has been examined in several murine models. Support for a bone marrow origin for neoplasia in this model suggests that these cells may respond to the need for regeneration with increased support, or may even incorporate themselves into the neoplasia. 45 Several studies imply that at least one of the colon cancer stem cell markers, CD44, may be useful as a therapeutic target. The increased expression of a CD44 variant in some patients with colitis, 36,53 CD44v6, suggests that this molecule may be used to enrich for tumorigenic cells. Since this molecule may even be detected in the blood and may parallel disease activity, the possibility that there are shed cells or cells that shed antigen suggests a potential mechanism for metastatic disease. Another potential use of this marker exists in the functional pathway. CD44 is responsible for homing of cells to the bone marrow niche where it has a relationship with osteopontin. The use of antibodies to CD44 was employed in the murine DSS model of colitis in BALB/c mice. 29 These mice were treated with blocking antibodies to CD44v7, which inhibited T-cell extravasation and recruitment to the intestinal mucosa, curing experimental colitis.
Summary/Conclusions
The relationship between colitis and cancer as an example of inflammation-associated neoplasia has been appreciated for decades. Though we have much more knowledge regarding the interactions of the immune system, microbiology, and stem cells, both of the normal variety and in cancer, our understanding of these interactions is in its infancy. The concept of stem cells involved in the pathogenesis of these 2 large areas of investigation is novel and will require significantly more evidence prior to defining inflammation-associated colon cancer as a stem cell–based disease.
Although the relationships are incompletely understood, the areas in which such knowledge would be applicable include pathogenesis. Clinically these concepts would correspond to early detection and prevention. Since current methods for the detection of colorectal cancer in the chronic colitic patient include colonoscopic biopsies with some advantages in utilizing chromoendoscopy as a method to amplify the dysplastic areas, the identification of tumorigenic rather than regenerative stem cells would offer great advantages. These advantages would be further enhanced if the examination was noninvasive. For example, shed mucus or stool would be assayed as a biomarker for shed epithelia or other cell markers indicative of stem cell transitions to neoplasia. Even more appealing would be the identification of these cells in the blood as a circulating biomarker.
Once enriching markers are identified, these isolated cells could be appropriately used to test prevention strategies. Multiple agents (including aspirin, nonsteroidal anti-inflammatory drugs and statins, and active ingredients in foods) have already been assayed in vitro using colon cancer cell lines, and in murine models, and could be used against colon cancer stem cells. Food additives that could be potentially evaluated include 1) resveratrol, the active ingredient in red wine; 2) turmeric, which is a component of curry powder; and 3) piperin, a component of pepper. These are just a few examples in which in vitro and in vivo studies could be mounted in parallel.
The cellular interactions of the stem cells need to be examined as another area ripe for intervention. First, the ability of the microenvironment to enhance tumorigenesis must be investigated. Do the cells in the niche accelerate mutations or augment pathways that increase stemness? Do the cells in the niche develop alterations that precede those of the stem cells? How do these cells communicate and which factors are necessary for this transition?
Within this context, murine models will remain necessary within the clinical armamentarium for the dissection of these relationships and for preclinical trials. The understanding of these interactions and even the isolation/enrichment for putative cancer stem cells remain in the early phases of development. However, these tools and concepts are powerful and will enable significant advances in our understanding of inflammation-associated cancer.
Footnotes
Acknowledgements
We are grateful to Jason Cline for preparation of the manuscript. Funding was provided by the Department of Surgery (E.H.H.) at the University of Florida, and Evelyn F. and William L. McKnight Brain Institute of the University of Florida (E.H.H.).
