Abstract
Background: Hip fractures are highly prevalent in the geriatric population, accounting for significant morbidity, mortality, and health-care associated costs. Geriatrics hip fracture comanagement is a systems-based approach to optimize care of these patients, prevent further decompensation, and reduce costs associated with the inpatient stay and consequent sequelae. This study examines preliminary results after implementation of orthopaedic and geriatrics hip fracture comanagement at our large, urban, single center academic medical center.
Methods: This is a program evaluation comparing a novel multidisciplinary service with usual care in 120 consecutive, operatively managed hip fracture patients, aged 65 years or over, in 2011. Patients with pathologic fractures, multiple injury trauma, or requiring a monitored unit were excluded. Groups were compared for age, sex, revised cardiac risk index (RCRI), presence of delirium, and admission disposition. Outcome measures included time to surgery, perioperative complications, in-hospital mortality, length of stay (LOS), and 30 day readmission. Institutional Review Board approval was obtained prior to the implementation of this initiative.
Results: Mean age, sex, admission disposition, RCRI score, time to surgery, perioperative complications, in-hospital mortality, and 30 day readmission did not differ between the two groups. In the comanagement cohort, there was a significant increase of delirium diagnosis (3.8% versus 22%, p = 0.007) and a reduced length of stay (7.1 versus 4.9 days, p = 0.008).
Conclusions: The results from this preliminary programmatic implementation suggest that orthopaedic-geriatrics comanage-ment reduced LOS by 2 days. Complications, readmissions, and in-hospital deaths were similar. There were higher rates of delirium noted in the comanagement group, which we attribute to increased surveillance, detection, and documentation and similar to rates seen in comparable programs. Our investigation supports the experience in other centers in which a systems-based program with well-defined principles and protocols improves processes and outcomes for a common condition in a high-risk population.
Geriatric hip fractures constitute a life-defining, sentinel event, and frequently foretell functional decline and downward spiral in those afflicted. Hip fractures accounted for 258,000 hospital admissions in 2010 and are expected to rise 12.3% by 2030 as longevity and the proportion of older Americans increase. Hip fractures account for 72% of osteoporotic fractures, costing $13.5 billion per year. Thirty percent of patients sustaining a hip fracture require care in skilled nursing facilities, and the associated mortality is 20% within 1 year. 1 The goals of surgical intervention are pain control, return to prior functional status, and reducing morbidity while improving quality of life.
Throughout the last decade, there has been significant effort to reduce morbidity and mortality among elderly hip fracture patients, resulting in heightened use of evidence- based approaches based on research findings. Rapid time to surgery, and early and aggressive physical therapy, osteoporosis management, early and continued comprehensive medical care have been demonstrated as effective strategies and have determined the direction of optimization.2-4 A systems-based approach of coordinated medical and surgical care between services has focused on postoperative optimization, decreasing length of stay, reducing morbidity and mortality, and enhancing functionality. Several models of care have been proposed and implemented: 1. orthopaedics as the primary service with medicine or geriatrics consulted as needed, 2. orthopaedics as the primary service with immediate, proactive medical consultation, 3. medicine or geriatrics as the primary service with orthopaedics consulted for surgery, and 4. shared medical and orthopaedic comanagement. 5
Hospitalist comanagement has been in existence since 2005, with 85% ofhospitalist programs participating; the longest track record is for patients with orthopaedic diagnosis related groups (DRGs).
6
To date, there have been few studies worldwide examining geriatrics comanagement. In Australia, it was shown that morbidity and mortality rates decreased with geriatrics co-care when compared with a consultation model.
7
The “Sheba” model from Israel evaluated 3,114 hip fractures comparing an orthopaedic service with the geriatric hip fracture unit and found the geriatric hip fracture unit to have lower 90 day mortality rates despite an older population with a greater prevalence of comorbidities.
8
In 2008, Friedman and coworkers developed the Rochester (NY) Model which outlined specific principles upon which to base a geriatric hip fracture comanagement program: 1. most patients benefit from surgical stabilization, 2. short time to surgery limits iatrogenic illness, 3. frequent communication between services limits iatrogenesis, 4. standardized protocols decrease unwarranted variability, and 5. discharge planning begins at admission.
9
Clinical implementation of these principles include daily assessment by geriatrics and orthopaedics, rapid preoperative medical optimization, early identification of individual goals for multidisciplinary rehabilitation, continued and coordinated re-evaluation of clinical data, and clinical and service responsibilities for all stages ofcare.
10
Particular features requiring attention in geriatric patients include serial cognitive assessments, screening for depression and substance abuse, risk factors for postoperative delirium, nutritional and functional status, polypharmacy, postoperative goals, expectations, and caregiver support (Fig. 1). To address these concerns, our program has implemented a protocol beginning on arrival to the emergency department and continuing through outpatient follow-up (Fig. 2).
Principles of an orthopaedic-geriatric hip fracture comanagement model. Adapted from Friedman and coworkers.
9

This study examines the effect of the orthopaedic-geriat- rics comanagement (OGC) program at Montefiore Medical Center in the Bronx, NY, compared with a usual care model in geriatric hip fracture admissions during 2011. Based upon the precepts of the Rochester model, we sought to investigate if OGC would lead to a constellation of improved outcomes, including reduced time to the operating room, lowers rates of postoperative complications, shorter length of stay (LOS), less mortality, and fewer readmissions.
Material and Methods
This is a program evaluation comparing a novel multidisciplinary service with usual care in 120 consecutive, operatively managed geriatric hip fracture patients admitted to a large urban academic medical center in the Bronx during 2011. Institutional Review Board approval was obtained prior to the implementation of this initiative.
Male and female patients 65 years or older (range: 65 to 99 years of age) were included in the analysis. All fractures of the proximal femur were included (ICD 9 codes: 82000-82003, 82009-82013, 82019-82022, 82030-82032, 8208, and 8209). Exclusions were pathologic fractures, multiple injury traumas, critical patients requiring cardiac or intensive care monitoring, and patients already admitted to medical units. The intervention consisted of an OGC model designed to improve processes of care to enhance outcomes for the test cohort. This involved both services independently assessing the patient in the emergency department before admission with continued care through patient discharge. All hip fracture patients admitted to the orthopaedic service that did not have a PCP with admitting privileges to our hospital were included in the OGC cohort. All other patients were included in the usual care cohort which functioned as the control group and utilized the traditional medicine consult practice on an as-needed basis with the consult service signing off once the patient was stabilized (Fig. 3).
Timing and specific interventions as outlined by our orthopaedic-geriatrics comanagement protocol from evaluation in the ED to continued outpatient follow-up.
Patient characteristics including age, sex, admission disposition, RCRI category, and presence of delirium (defined as a change of mental status at any time from presentation to discharge as compared to baseline) were compared between the two groups (Table 1). The Revised Cardiac Risk Index (RCRI) is a validated tool that is used to estimate patient risk of perioperative cardiac complications, described in 1999 derived from 2,893 patients and validated in 1,422 patients, aged greater than or equal to 50 undergoing major noncardiac surgery. The RCRI combines six independent variables that predict an increased risk for cardiac complications: supra- inguinal, vascular, intraperitoneal, or intrathoracic surgery, history of congestive heart failure, history of cerebrovascular disease (stroke or transient ischemic attack), history of diabetes requiring preoperative insulin use, and chronic kidney disease (creatinine > 2 mg/dL). Based on this risk calculator, patients may be stratified as low cardiovascular risk (0 predictors = 0.4% risk of cardiac death, nonfatal cardiac arrest, and nonfatal myocardial infarction), intermediate (1 to 2 predictors = 1% to 2.4% risk), and high risk (3 to 6 predictors = > 5.4% risk). 11
Outcome measures included time to surgery, length of stay, perioperative complications, in-hospital mortality, and 30-day readmission rates.
Study flow diagram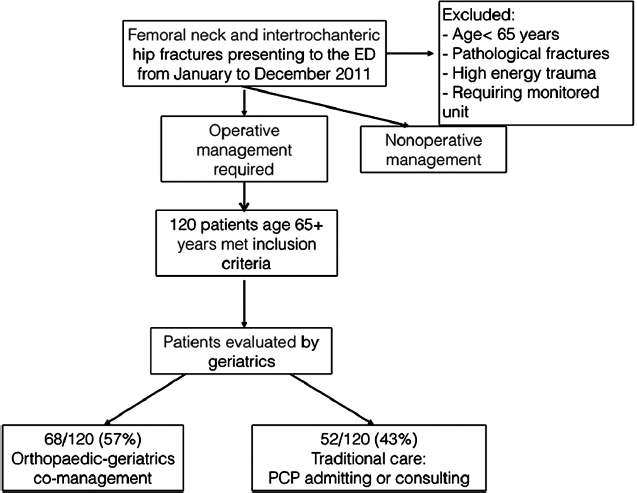
Statistics
Data were analyzed using SPSS version 20.0 with alpha level set at 0.05 and beta level at 80%. We calculated measures of central tendency (means, medians, and standard deviations) and compared continuous data with t-tests and ANOVA. All data was assumed to be parametrically distributed. Categorical variables were compared using the chi-square test and in the case of small cell frequencies, Fisher’s exact test.
Results
Clinical and Demographic Characteristics in Operatively Managed Hip Fracture Patients in the Usual Care and the Orthopaedic-Geriatrics Comanagement Groups

Discussion
The results from this preliminary programmatic implementation suggest that in patients with operatively-managed hip fractures, OGC leads to a reduced length of stay by approximately 2 days at our institution. Baseline characteristics were similar between the two groups; however, there were higher rates of delirium noted in the OGC group: a paradoxical finding. It would be expected that delirium would be decreased with OGC involvement due to an amplified focus on population-specific adjustments to pain control, environmental stimuli, polypharmacy, and geriatric syndromes such as constipation, urinary retention, poor nutrition, and immobilization. However, we believe that this finding arises from an increased awareness and diagnosis of delirium with the continued evaluation by a geriatrician trained in its detection. This phenomenon is supported by similar rates of delirium found in the Rochester Model, 24.1% compared to the 22% in our investigation. Of note, the Rochester comanagement model found similar rates to our model with respect to inhospital deaths (2.6%), 30-day readmission (10.4%), length of stay (4.3 days), with a 21.2% mortality rate at 1 year, and total cost of care of $15,188 versus $33,693 before the implementation of their program.
10
Comparison between orthopaedic-geriatric comanagement of hip fracture patients at Montefiore Medical Center and the Rochester Model at Highlands Hospital.
10

Comparison Between Patients Undergoing Hip Fracture Surgery in and the Orthopaedic-Geriatrics Comanagement Groups the Usual Care

Length of stay is a significant outcome with implications for cost of admission, regaining function, minimizing iatrogenic illness, delirium, and mortality. After implementation of a multidisciplinary geriatric hip fracture center in Fort Worth, TX, investigators found a significant decrease in time from medical clearance to surgery as the sole factor contributing to overall length of stay. 16 Preventing delays in medical clearance has been a major focus of our protocol with early, prophylactic evaluation by both the orthopaedist and geriatrician. The geriatrician is responsible for directing medical optimization and minimizing unnecessary consults and tests which would delay time to surgery. At the other end of the inpatient stay, the geriatrician has increased familiarity with transitional care to skilled nursing facilities, family decision making, and managing goals and expectations throughout admission.
The strengths of the present study include its contribution to the small literature base about OGC, its utilization of institutional resources without external funding, and its demonstration that the methodology of health services research can improve patient outcomes. This study is limited by its small sample size, retrospective design, lack of formal group allocation, and lack of blinding which may introduce evaluation bias. The high rates of delirium in the OGC group may be attributed to surveillance bias as a geriatrician is more likely to detect delirium than other specialists.
As a result of the successful outcomes of the initial phase implementation, in 2015 our center adopted the OGC hip fracture program. This is similar to the program outlined in this article but with all non-pathologic hip fractures in our hospital system cohorted to a single center hip fracture comanagement service. The team consists of the usual orthopaedic inpatient team (intern with or without physician assistant for inpatient care, two operative second years, one third or fourth year, two fifth years, and operative physician assistants), a geriatrician dedicated full time to the hip fracture patients, unit social workers, and specialized orthopaedic physical and occupational therapists.
We will continue to assess and evaluate processes and outcomes in the OGC hip fracture program and believe that it will serve as a platform from which to develop comanagement between other specialties within and outside of our institution.
As hip fracture in geriatric patients frequently reveals underlying comorbid conditions and triggers functional decline, a geriatrician is essential to the management of non-orthopaedic manifestations before and after injury. The investigators believe that cohorting patients to a dedicated OGC program will benefit patients and has the potential to utilize health care resources effectively.
Footnotes
Conflict of Interest Statement
None of the authors have a financial or proprietary interest in the subject matter or materials discussed, including, but not limited to, employment, consultancies, stock ownership, honoraria, and paid expert testimony.
