Abstract
The zinc disc implantation-induced urinary bladder calculi model in the rat is commonly used for preclinical evaluation of the antiurolithiatic activity of test compounds. Certain published reports state that relatively long durations for which zinc discs must be implanted in the bladders of rats. Hence, there is a need to refine this model. These investigations aimed to determine whether long-term studies using the zinc disc implantation model provide any additional data that affect the final outcomes of the study. In this study, we evaluated the effects of a well-known antiurolithiatic polyherbal drug, Cystone, for different treatment durations of 10, 20 and 48 days postimplantation. Our results indicate that even the shortest duration of 10 days is sufficient to reveal antiurolithiatic effects of a test drug. Hence, in the zinc disc implantation-induced urinary bladder calculi model, the study duration is proposed to be minimized so as to reduce the distress caused to the rats due to long-term exposure to the implant. Further, it is suggested that the growth of the bladder calculi can be monitored by taking X-ray radiographs of the bladder deposits to decide the time to terminate the study. Use of preformed calcium oxalate crystal instead of zinc discs, as suggested in earlier reports by others, may also be considered to avoid the sacrifice of rats at the end of the study.
Formation of calculi (uroliths) in the kidneys, urinary bladder and ureters is a common urological disorder affecting approximately 12% of the world population with a considerable recurrence even after surgical removal. 1 The preclinical evaluation of antiurolithiatic activity of drugs is carried out in the experimental models that represent the process of formation of kidney calculi and urinary bladder calculi. The in vitro models used for this purpose simulate the initial events in the urolith formation such as nucleation, supersaturation and crystal growth. 2 However, such models do not encompass the activities of endogenous urolith inducers/inhibitors and biological processes that are actually involved in the stone formation in vivo. Hence, in the evaluation of the antiurolithiatic effect of test drugs, in vivo animal models are preferred.2,3 Rats are generally used as experimental animals for this purpose because there are considerable similarities in the structure and physiology of the urinary systems in humans and the rats. 3
The models of urinary bladder stones include either chemical induction of stone formation or surgical implantation of foreign material like a zinc disc in the urinary bladder of rats that subsequently leads to deposition of an urolith around the implant. The formation of renal calculi can be chemically induced in the experimental animals by oral administration of ethylene glycol, ammonium chloride, vitamin D3, calcium gluconate, ammonium oxalate, gentamicin sulphate or L-hydroxyproline. 4 These chemicals either alter the biochemical processes leading to excessive oxalate formation or alter the composition of urine to cause precipitation of calculi. However, the chemically-induced calculi also induce severe renal damage and hence may not represent the actual disease as it appears clinically. 2 Due to this, the models such as zinc disc implantation-induced urinary bladder calculi are considered more relevant and better represent the aetiology of the urine stone formation in humans. 3
In the zinc disc implantation model, zinc discs of known weights and dimensions are surgically implanted in the urinary bladders of rats. The rats recover from this surgical procedure by the third day postimplantation after which the test drug treatment is initiated. At the end of the specified treatment period, the rats are killed and weights of the deposits around the zinc discs are determined to evaluate the antiurolithiatic potential of the test drug. This model is employed to study the effect of drugs that either inhibit the growth of the preformed uroliths and/or those which accelerate their dissolution. Apart from zinc discs, certain other materials like calcium oxalate crystals, plastic discs and pieces of non-absorbable surgical threads can also be implanted in the urinary bladder to induce the urolithiasis. 3 However, zinc disc implantation model is the most widely used model and has been more extensively reported in the scientific literature. 5 The majority of the in vivo models of chemically-induced urolithiasis simulate the formation of calcium oxalate crystals, whereas the zinc disc implantation model represents the process of magnesium ammonium phosphate crystal growth.6-8 After implantation of a zinc disc, if ethylene glycol is orally administered to the rat, then the crystal developing around the implant mainly constitutes calcium oxalate. 3
In the reports on the zinc disc implantation-induced urolithiasis model, there is significant variation in the duration for which the animals are observed after implantation. Certain studies report observations of as long as six to eight weeks postimplantation.9–11
In one of these reports, treatment with the test drug itself has been started four weeks after the implantation surgery. 8 The weights of the implanted zinc discs also vary from 10 mg 12 to 48 mg. 10 Such long-term exposure of the rats to the urinary bladder implants leads to the formation of larger crystal deposits, which may lead to severe perturbations in the kidney functions and urinary tract infection.
Worldwide awareness about the Russell and Burch's concept of 3Rs has resulted in considerable efforts to reduce, replace and refine the biomedical experiments involving the use of animals. It has now become mandatory that the researchers dealing with experimental animals must avoid or minimize undue pain, distress and experiment-associated mortality and morbidity of the animals being used. The wellbeing of animals must be observed during all the experiments involving animal use. 13 Even though the model of zinc disc implantation-induced urinary bladder stones is in use since the 1950s, there have been very few efforts to optimize the size of the zinc discs and duration of the study after implantation so that the researchers may be at an advantage while preparing their own protocols and the experimental animals will be spared unjustifiably longer exposures to stressful conditions.
In the present study, the effect of a known antiurolithiatic drug, Cystone (The Himalaya Drug Company, JB Nagar, Mumbai, India), a polyherbal formulation, which is widely used for antilithic activity in traditional medicine,14,15 was evaluated in the zinc disc model for three different durations to check whether long-term studies have any additional advantages. We have also used an earlier reported simple technique of X-ray radiography 16 for monitoring the crystal deposition in the bladders of the rats after implantations.
Materials and Methods
Healthy male albino Wistar rats of 10–12 weeks old and 150–200 g body weight procured from the Advanced Centre for Treatment, Research and Education in Cancer (Mumbai, India) were used for this study. They were maintained under controlled conditions in polypropylene cages. Each cage contained three rats. Other conditions like 12 h light:dark cycle, 40–60% relative humidity, 22 ± 2°C temperature with free access to food (commercially available standard pellet feed; Amrut Laboratory Animal Feed, Bangalore, India) and water (tap water) were also maintained throughout the study. All the experimental procedures were carried out according to the guidelines of the Committee for the Purpose of Control and Supervision on the Experiments on Animals (CPCSEA) constituted under the ‘Prevention of Cruelty to the Animals Act, Government of India’. This study was approved by the Institutional Animal Ethical Committee (Registration No. 51/02/C/CPCSEA).
The rats were divided into seven treatment groups as follows: naïve control, sham-operated, zinc disc-implanted, zinc disc-implanted and Cystone-treated (500 mg/kg/day orally for 7 days), zinc disc-implanted and Cystone-treated (500 mg/kg/day orally for 17 days), zinc disc-implanted and Cystone-treated (500 mg/kg/day orally for 39 days) groups. As the treatment with Cystone was started on the fourth day postimplantation, the total observation periods for the Cystone-treated groups were 10, 20 and 48 days. The zinc disc implanted control group had 18 rats, while the other groups had six rats each. Six rats from the zinc disc-implanted group were killed at each time point by an overdose of halothane anaesthesia and the data obtained were considered for comparison with the corresponding Cystone-treated groups.
The implantations of zinc discs in the rat urinary bladders were carried out according to an earlier reported method. 10 Prior to surgery, rats were fasted for 8–10 h; however, 15 min prior to anaesthesia they were orally administered with 4 mL of water to dilate their urinary bladders. The rats were operated in sterile conditions under ketamine (Aneket, Neon Laboratories Ltd, Thane, India) (80 mg/kg intraperitoneally) and diazepam (Calmpose, Ranbaxy Laboratories Limited, Haryana, India) (4 mg/kg intramuscularly) anaesthesia. When the corneal reflexes and the reflexes to pinching of paws with forceps abated, the urinary bladders were exposed and a small cut was taken to open the lumen of the bladder. In the zinc disc-implanted groups, discs of average weight of 20 ± 2 mg were inserted into the bladder and the incision was closed by suturing the urinary bladder of the rat (1 or 2 stitches) using absorbable sterile surgical sutures (Centenial CNW 2670 6–0 USP). The urinary bladder was pushed back into its earlier position. The muscular layer of the abdomen was separately sutured using sterile absorbable sutures. The skin incision was then stitched with sterile silk sutures. The rats in the sham-operated group were similarly operated on, except for the implantation of a zinc disc in the bladder. All the operated rats were treated topically with antibiotic dusting powder and allowed to recover for three days. As a post-surgical analgesic, ibuprofen (Brufen, Abbott India Ltd, Mumbai, India) (30 mg/kg orally) was administered on the day of surgery when the animals recovered from anaesthesia and this dose was repeated after 24 h. Routine feed and water were provided from the day of surgery onwards.
From the fourth day postsurgery, treatments with orally administered Cystone at a dose of 500 mg/kg/day was initiated in consideration of earlier reports on the effective dose of this drug. 14 X-rays of any three rats from only the zinc disc-implanted group were taken every five days postimplantation with a digital X-ray instrument (GE-525 DX, USA) using the Fuji computerized radiographic system. Before the X-ray the rats were anaesthetized using ketamine (80 mg/kg intraperitoneally) and diazepam (4 mg/kg intramuscularly) anaesthesia to avoid any distress to the animals.
Rats in the respective groups were killed at the end of specified treatments. Prior to sacrifice, 5 h urine samples were collected by placing individual rats in the metabolic cages and the blood samples were collected through the retro-orbital punctures under ketamine (80 mg/kg intraperitoneally) and diazepam (4 mg/kg intramuscularly) anaesthesia. The urine and blood biochemical parameters were estimated using commercially available kits and the glomerular filtration rate (GFR) was calculated accordingly. 17 After collection of blood samples, rats were killed by an overdose of halothane anaesthesia and the contents of the urinary bladder were removed and weighed.
Statistical analysis
Unpaired t-test was used for determining the statistical significance of the difference in the weights of the deposits around the implanted discs between the Cystone-treated groups and the corresponding zinc disc-implanted control groups.
For the analysis of statistical significance of the differences in the central tendencies of other parameters, one-way analysis of variance followed by Bonferroni's post-test was used. The statistical tests were carried out in two separate sets. In the first set, values of each study parameter at durations of 10, 20 and 48 days were compared; and in another set of tests, the values of urine creatinine, urine albumin and GFR in the Cystone-treated group at three treatment durations of 10, 20 and 48 days were compared; P < 0.05 was considered statistically significant.
Results
Table 1 shows the effects of various treatments on the weights of the depositions around the implanted discs in different study groups. It was observed that the implantation of zinc discs in the urinary bladders of rats induced characteristic depositions around the discs within 10 days. These deposits were clearly visible in the X-ray radiographs (Figure 1). In the sham-operated group, there was no such deposition in the bladder lumen. Treatment of rats with Cystone significantly reduced the weights of the depositions around the implants. The effect of the Cystone treatment was evident and statistically significant even at the shortest study duration of 10 days postimplantation. In the longer treatments of 20 and 48 days, the findings were similar and the levels of significance, P values, for the statistical tests were similar (P < 0.0001) to that of the 10 days treatment readings.
Cystone treatment significantly reduced the weights of the deposits around the zinc disc implants at all the tested time points
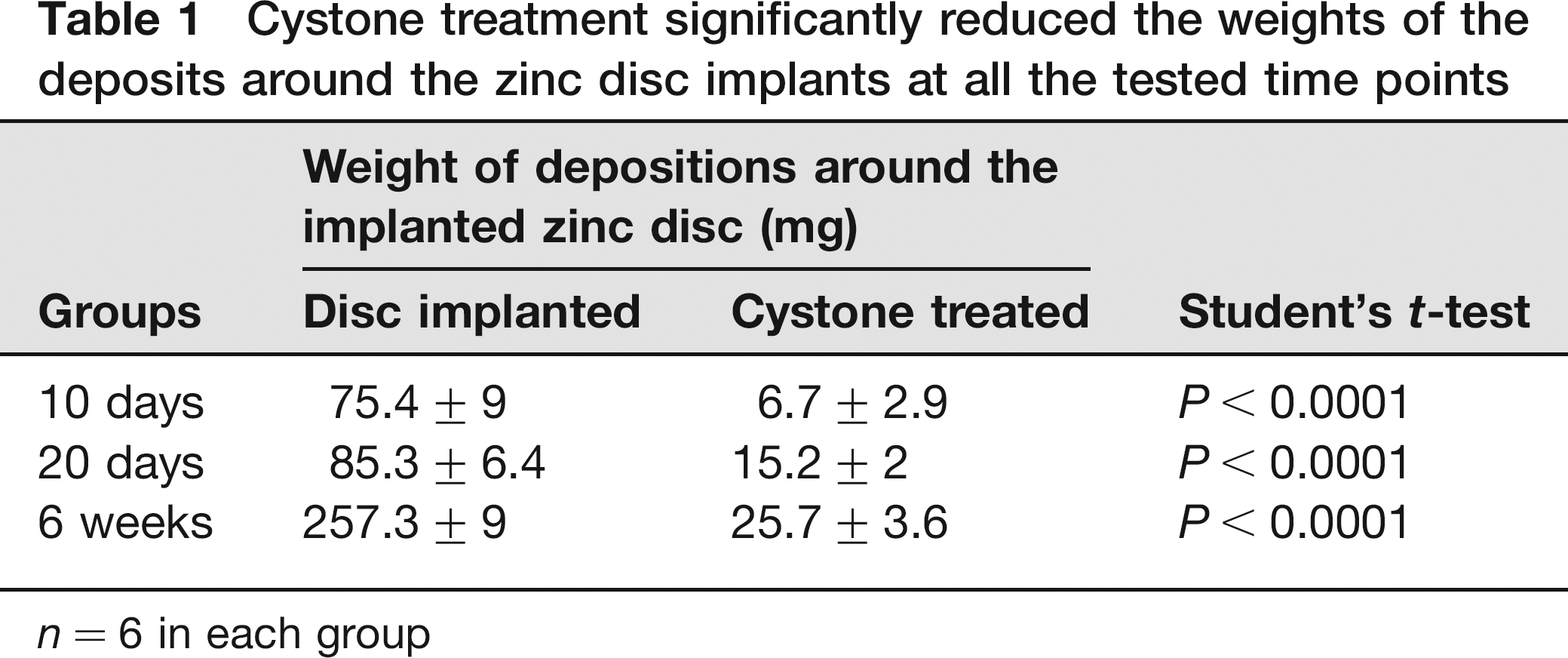
n = 6 in each group
Effect of test drug on the deposits around the implanted zinc discs in the rat bladder could be visualized in X-ray images from 10 days postimplantation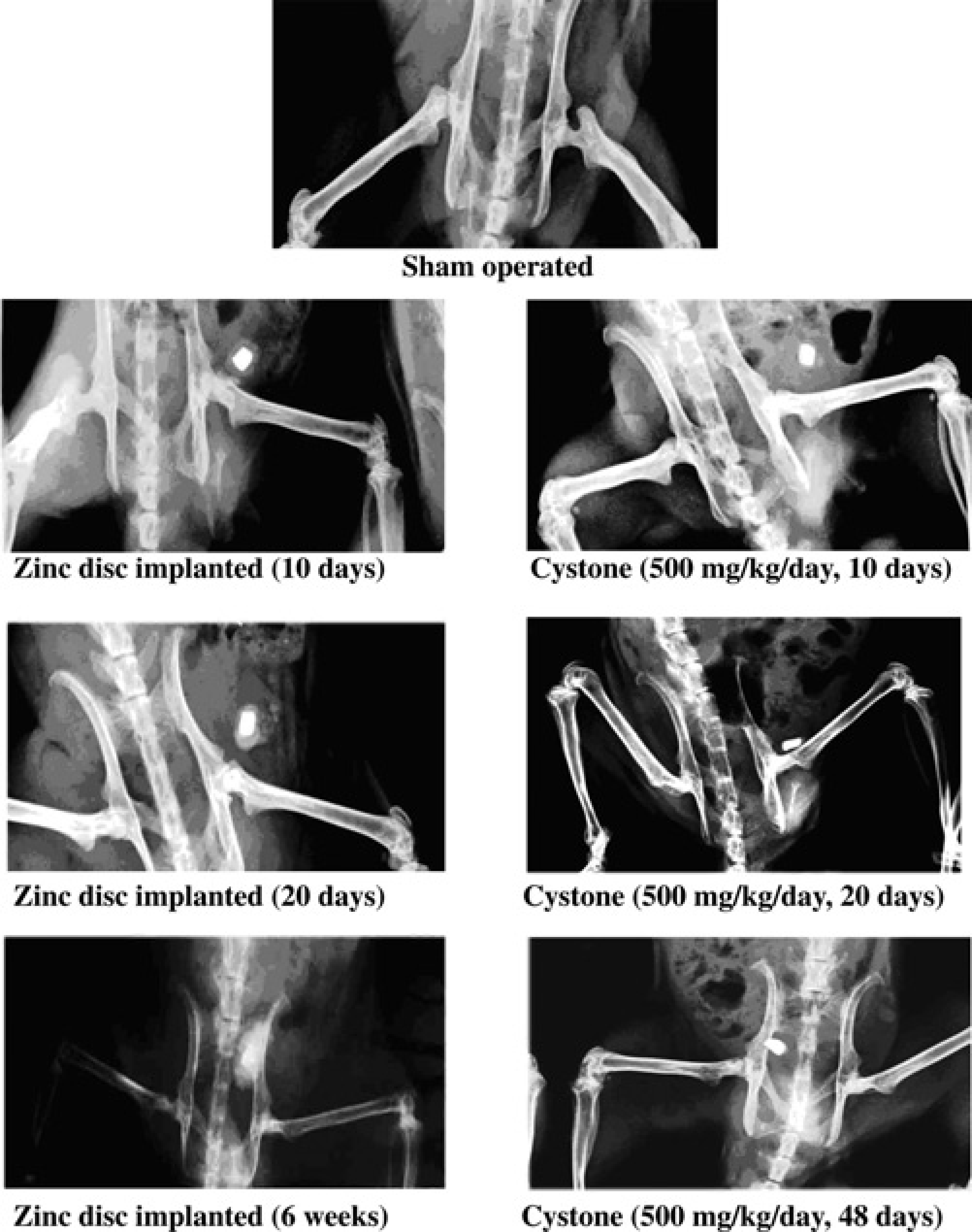
Table 2 shows the average values of urine creatinine, urine albumin and GFR for different study groups. The surgical procedure and disc implantation appeared to reduce the GFR. GFR in the zinc disc-implanted group was significantly decreased at all the time points tested; whereas, Cystone treatment normalized the GFR, rather there was a significant rise in the GFR compared with that of the naïve control group. There was no significant difference in the GFR values in the Cystone-treated groups at days 10, 20 and 48.
Protection from alterations in the kidney function parameters by Cystone treatment was evident from the 10th day postimplantation onwards
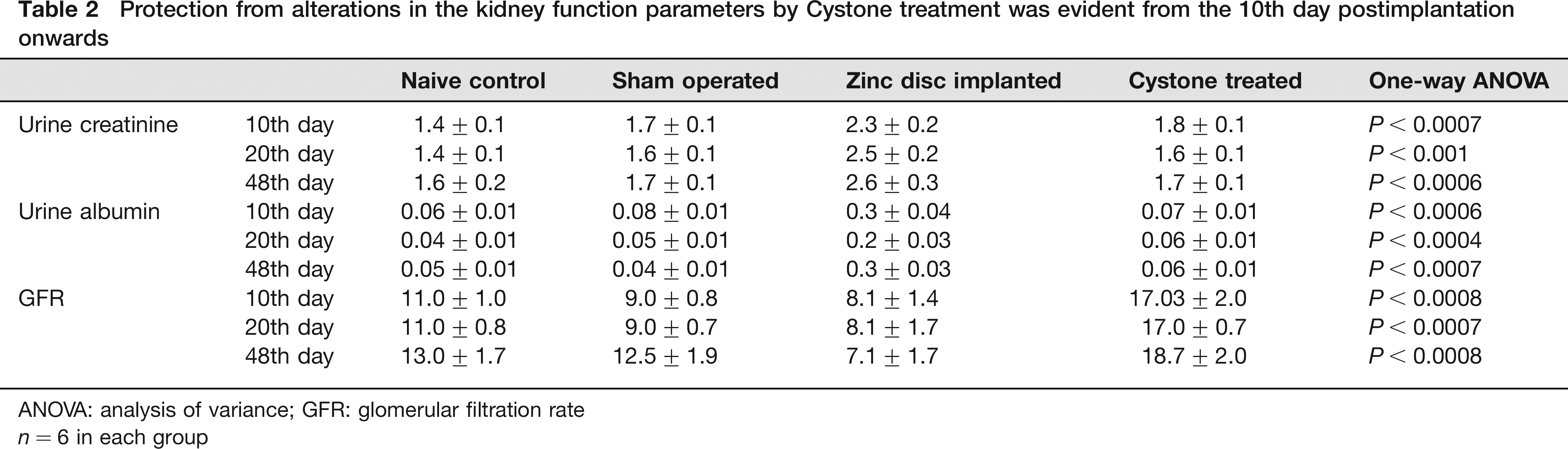
ANOVA: analysis of variance; GFR: glomerular filtration rate
n = 6 in each group
In the zinc disc-implanted group, there was a significant rise in the urine creatinine and urine albumin levels at 10, 20 and 48 days. Cystone treatment reduced the changes in these kidney function-related parameters at all the treatment durations. Comparison between the Cystone-treated groups revealed no significant differences among the urine creatinine and urine albumin levels at the different treatment durations. Urine albumin levels in the Cystone-treated groups were not significantly different from that in the control group.
The X-ray images of rats (as shown in Figure 1) revealed clearly visible depositions around the zinc discs within 10 days postimplantation. There was time-dependent increase in the size of the deposits and such rise was visually distinguishable at days 20 and 48.
Discussion
Vermeulen et al. 6 established that implantation of a zinc disc in the urinary bladder of rat induces formation of characteristic urinary bladder stones. Following this, numerous modifications have been suggested in this model. The durations for which zinc disc is implanted in the rat bladder significantly varies among different reports. Hence, it becomes necessary to decide whether the duration of the study affects the quality of data generated through this model.
It is clearly evident from the results of the present study that there is formation of sufficiently large depositions around the implanted discs within 10 days. Further continuation of the study does not appear to add qualitatively to the data generated at 10 days.
It was observed that there was significant decrease in the GFR and rise in urine albumin and urine creatinine levels within 10 days after surgery, which continued to worsen with time. At the end of 20 days postimplantation, the average weight of the crystal depositions was about 85 ± 6.4 mg, whereas the urine albumin and urine creatinine values were also increased to 0.2 ± 0.03 and 2.5 ± 0.2 mg/dL, respectively. The size of crystals on day 48 was as high as 257.3 mg and the GFR was reduced to 7.1 ± 1.7 mL/h from around 15 mL/h. This clearly indicates that the rats were suffering from severely compromised renal functions due to increasing crystal size at durations of over 20 days. The apparent increase in the GFR in the Cystone-treated group may be due to the diuretic effect of this drug.
The data obtained at 10 days postimplantation in the Cystone-treated group clearly indicate the efficacy of this drug as an antiurolithiatic agent. The results obtained at days 20 and 48 are also qualitatively similar. Hence, there is no reason why rats in the control or treated groups should be exposed to further stress of growing depositions in their bladders. If any other drug is to be evaluated in this model, it is proposed that the 10 days postimplantation study will suffice for identifying a pharmacodynamic effect.
Digital X-ray imaging provides a means to easily monitor the crystal growth in the urinary bladder. As evident in this study, within 10 days postimplantation, depositions could be visualized around the implants. Hence, use of this technique can help investigators to determine the time at which the study is to be terminated.
Thus, our data indicate that while evaluating an antiurolithiatic drug by the zinc disc implantation model, X-ray radiography should be used to monitor the growth of depositions around the implants, and as soon as sufficient deposition is revealed in the zinc disc-implanted control groups, the study should be terminated so as to minimize undue stress to the animals. It is further suggested that instead of using zinc disc or other insoluble material, preformed calcium oxalate crystals can be implanted in the bladder so that there will be no need to kill the animals at the end of the study and the remaining depositions can be dissolved with a standard drug treatment. However, the re-use of such recovered animals in another protocol must undergo ethical evaluation.
Based on our data, the duration of exposure of animals to bladder stones should not be longer than 10–20 days and the test drug treatments may be started from the third day postimplantation.
It is proposed in an earlier study that implants such as a plastic disc is implanted to facilitate the subsequent processing of bladder deposits for cross-sectioning and microscopical observation. However, even in this case sacrificing of the animals is not avoided. The use of X-ray examination of formed crystals in the rats has been suggested by Vargas et al. 11 There is a need for this technique to be more extensively used to determine the endpoint of the study in this model. As is evident from our results, the duration of the study in the zinc disc implantation-induced urinary bladder calculi model should not be more than 10 days postimplantation. These refinements in the implantation-induced urinary bladder calculi formation models have been proposed to significantly reduce undue pain and distress to the rats as well as reducing the number of rats killed without compromising the final outcomes of the experiments.
Footnotes
Acknowledgement
The authors are thankful to Dr S J Surana, Principal, R C Patel Institute of Pharmaceutical Education and Research, Shirpur, India, for providing the necessary laboratory facilities for this work.
