Abstract
Presacral cysts are rare lesions not typically evaluated with sonography, due to their location between the rectum and sacrum. This case study reviews the imaging and biopsy of a presacral lesion, in a patient presenting with gastrointestinal symptoms, back, and leg pain. The patient underwent numerous diagnostic imaging examinations, with multiple identified differential pathologies. After biopsy, the pathology report identified features of an epithelial squamous cyst, with the main differential of an epidermoid cyst. Presacral lesions have a wide variety of differential diagnoses and should be evaluated with diagnostic imaging and possibly tissue sampling. This anatomical site is often diagnostically evaluated with magnetic resonance imaging or computed tomography. Transvaginal sonography has rarely been reported as imaging technique that can be used in the presacral space but proved valuable in this patient case. Utilizing transvaginal sonography may be a diagnostic option considered, to evaluate lesions in this location.
Presacral, or retrorectal, epidermoid cysts are rare, congenital, and developmental lesions arising from the ectoderm. 1 Epidermoid cysts, in the presacral location, are primarily found in middle aged women. 2 The prevalence of presacral epidermoid cysts, specifically, have not been reported consistently in the literature. The prevalence of presacral lesions, as a general pathology, lack an updated occurrence. Most publications reference a 1938 source that reported an incidence of presacral lesions as one in every 40 000 patient records, at the Mayo Clinic. 3 These cysts, also often referred to as inclusion cysts, can be classified as stratified squamous epithelium cysts. They are surrounded by a squamous epithelial wall with internal contents including keratin, water, cholesterol, and desquamated debris. 4 There is a broad list of diagnostic differentials for lesions in the presacral space, with several being reviewed in this case report. This patient case represents a unique diagnostic imaging evaluation of a presacral mass, based on a patient presenting with a recent history of back pain and gastrointestinal symptoms. Transvaginal sonography was useful in evaluating lesion characteristics, prior to biopsy.
Case Report
A 35-year-old woman with a medical history of abdominal situs inversus, including left-sided inferior vena cava, and polysplenia, was seen for persistent lower back pain. Her pain only slightly improved after completing physical therapy. The patient had previously been diagnosed with sciatica. The pain and muscle fatigue returned after physical therapy treatment and progressively worsened. The patient also reported that she experienced an overactive urinary bladder and loose bowel movements.
A magnetic resonance imaging (MRI) examination was recommended to further evaluate the cause of pain, but was contraindicated, due to the patient’s cardiac device. Instead, a computed tomogram (CT) of the lumbar spine, without contrast, was ordered to evaluate the lower back pain, given persistent symptoms for more than 6 weeks after treatment. On the initial CT examination, a presacral hypodense lesion was identified that measured 4 × 2 × 4 cm, with differentials listed as a meningocele or teratoma. To further evaluate this lesion, a CT pelvis, with contrast, was performed, based on an indication of a cystic presacral lesion. The second CT examination demonstrated a stable chronic caudal sacral deformity, with homogeneous internal density, just anterior to the coccyx. It measured 4.2 × 3.5 cm with stable size and no contrast significant enhancement, compared to recent lumbar spine CT. The patient was referred to a higher-level facility for further diagnostics, to address this lesion.
At the next facility, 2 months after the initial CT, a radiograph was completed. The radiographic result identified a sacral deformity, partial sacral agenesis, and a presacral mass. Based on this radiograph, the mass was thought to represent a possible sacrococcygeal teratoma, or a tailgut cyst. An additional CT pelvis, without contrast, was obtained, which documented a presacral lesion that was nonspecific, without diagnostic differentials provided. This CT identified a well-circumscribed soft tissue mass abutting the anterior aspect of the sacrum, which measured 2.3 by 3.5 by 4.3 cm (See Figure 1). This was again reported as a known sacral deformity with partial agenesis of the inferior portion. The musculoskeletal interventional radiology department was consulted, and a CT guided biopsy was the next recommended step. A sonogram was requested by this team to characterize the mass and assess for benign or malignant features, which would help to evaluate the risk of tumor seeding, prior to biopsy.
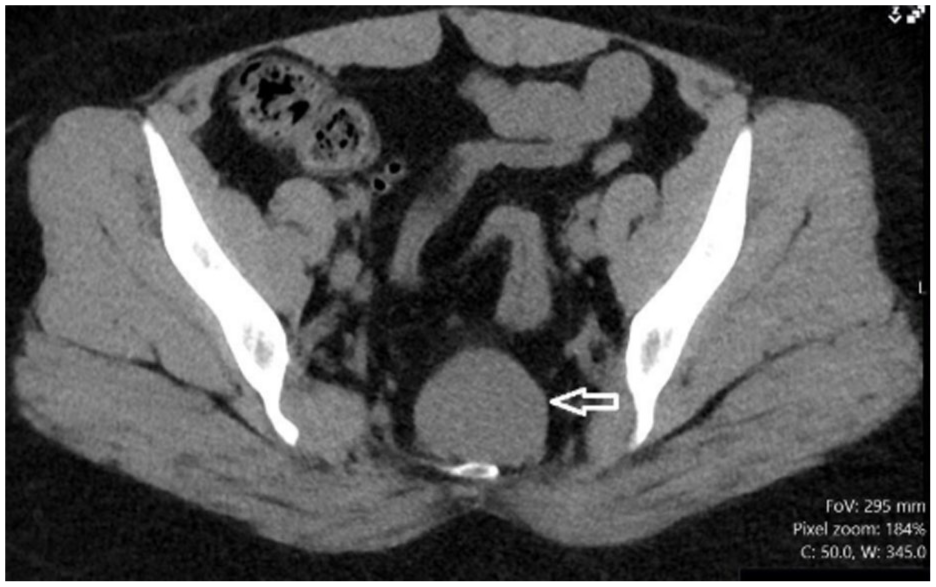
An axial computed tomographic image, without contrast, is provided and demonstrated a 4.3-cm-well-circumscribed soft tissue mass abutting the anterior aspect of the sacrum (mass denoted by the white arrow).
Six weeks after secondary evaluation at the new facility, the sonogram was performed using a Sequoia ultrasound equipment system (Siemens Healthineers, Malvern, PA) with a 9EC4 endocavity transducer. During the pelvic sonogram, the uterus was identified using the standard vaginal transducer position (See Figure 2). The transducer was then angled posteriorly into the vaginal posterior fornix. It was in this position and view that the presacral mass was documented.
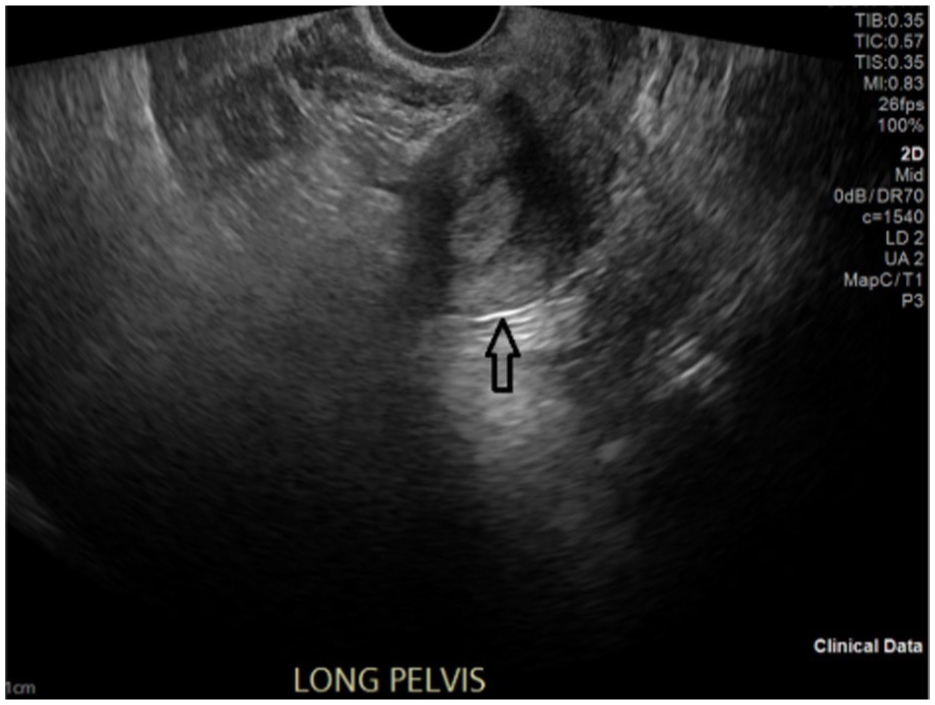
A transvaginal sonographic image, captured in the sagittal plane, demonstrated the uterus (denoted by the black arrow) with the transducer in the standard vaginal position for imaging pelvic organs. The suspected mass was not appreciated in this sonographic view.
The sonogram demonstrated the presacral space with an avascular, well delineated, complex lesion with internal echogenic foci and posterior enhancement. This was reported as a 4.0-cm presacral cystic-appearing structure, containing inspissated debris (See Figures 3–5), which correlated with previous CT findings. These sonographic findings were reported to represent an anterior sacral meningocele/terminal myelocystocele, given the CT evidence of possible caudal regression. Diagnostic differentials were provided as a tail gut duplication cyst or a retrorectal epidermoid cyst.
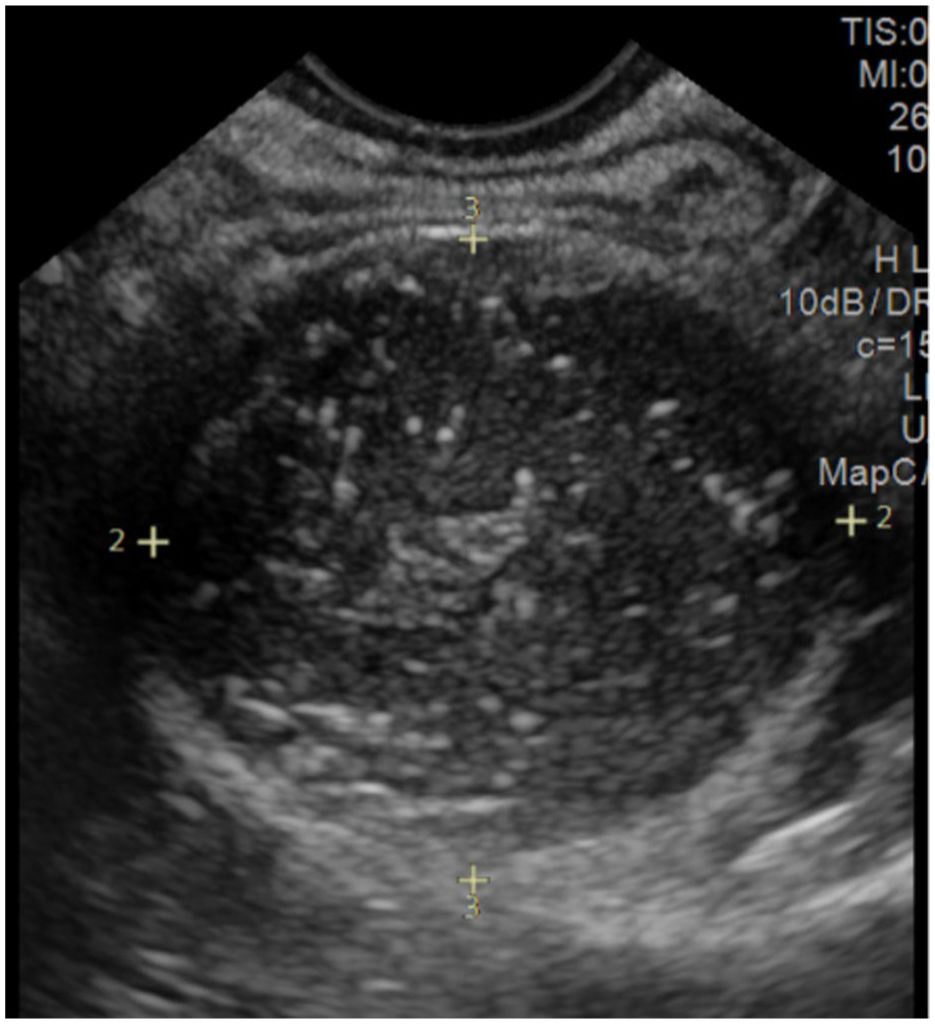
The transvaginal transducer was moved to the posterior fornix, which demonstrated in the transverse plane, a heterogeneous complex mass. The borders of the mass are denoted by the electronic measurement calipers.
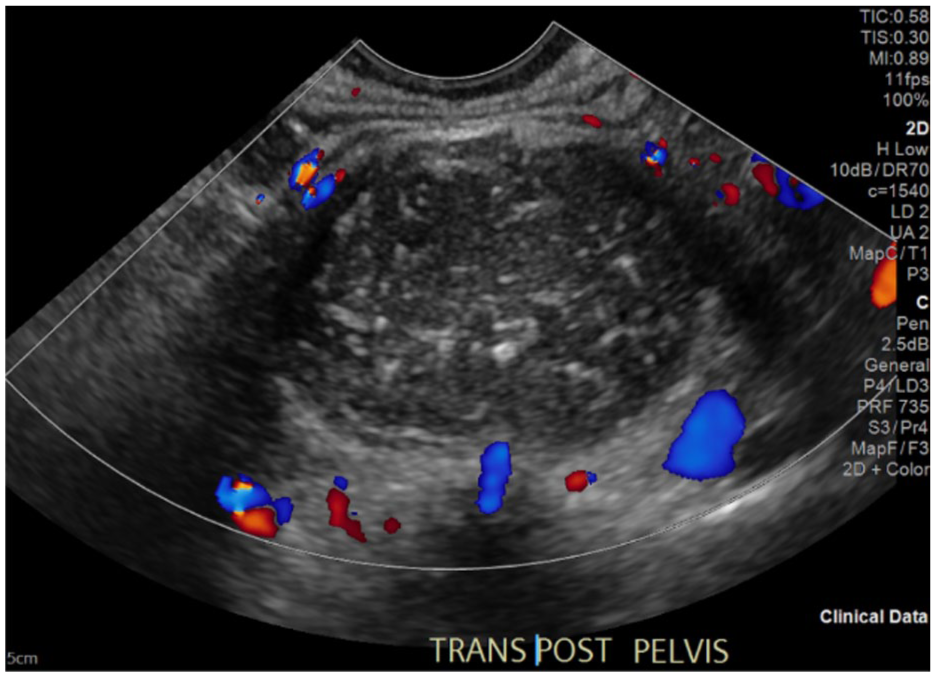
The transvaginal sonographic image, in the transverse plane, demonstrated the presacral mass, with posterior acoustic enhancement and a lack of internal vascularity.
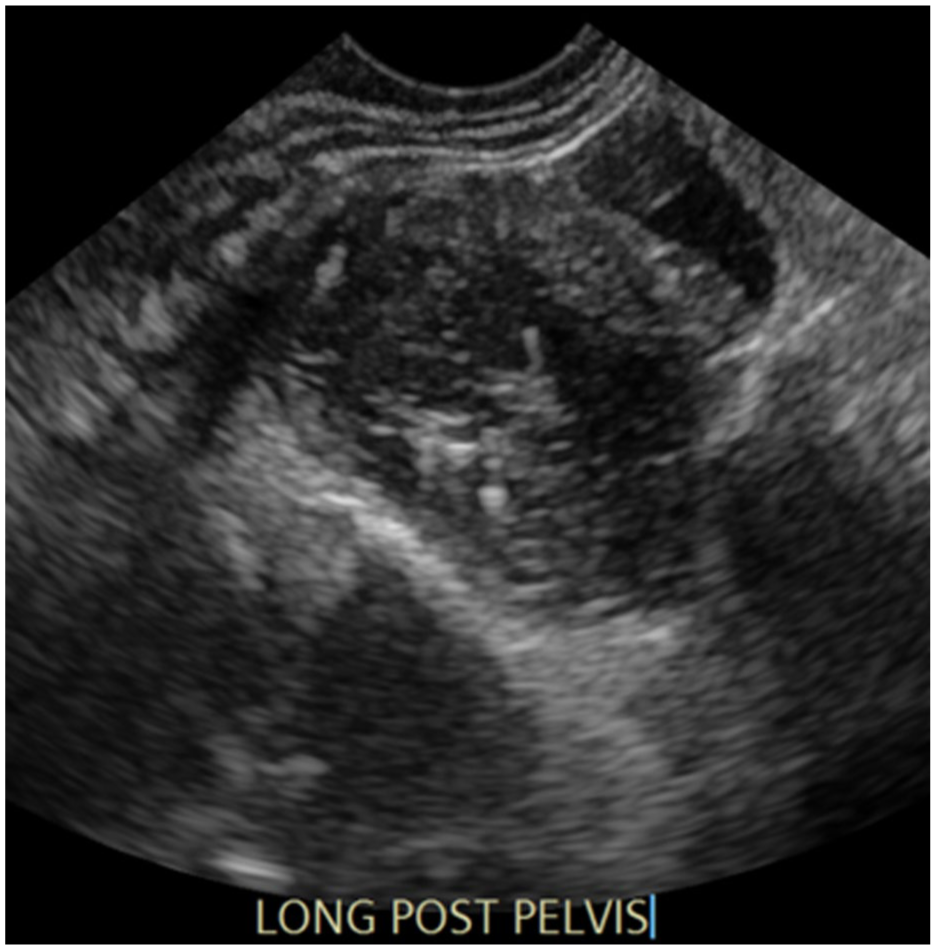
This transvaginal sonographic image, in the longitudinal plane, demonstrates the mass and was accomplished with the transducer positioned in the posterior fornix.
An interventional radiologist proceeded with same day CT-guided biopsy, of the mass, given its lack of sonographic malignant features (i.e. posterior enhancement suggesting a large fluid component and absence of vascularity within the lesion). The resulting pathology report identified abundant laminated keratin material, anucleated squames, and cellular debris. No tumor cell necrosis, cytologic atypia, or mitosis activity was noted. The pathologist’s report further described these findings as contents from an epithelial squamous cyst. The differential diagnoses reported by the pathologist include an epithelial inclusion cyst and less likely a neoplasm with squamous features (e.g. teratoma).
Shortly after biopsy, the patient followed up with an orthopedic surgeon, to review imaging and biopsy results. Surgery was not recommended, but the provider suggested continued physical therapy to relieve pain. It was suggested that surveillance diagnostic imaging be completed to track the size and characteristics of the cyst. The 6-month diagnostic recheck included a CT, which again identified the lesion with slight decrease in size, likely caused by biopsy/aspiration. There was discussion of the likely epithelial inclusion cyst and the current state of the patient’s symptoms. The patient reported immense improvement in symptoms with continued physical therapy. The patient’s pain was contributed to a sciatica diagnosis and was determined to be unrelated to the discovered presacral lesion. At the time of the patient’s repeat visit, no gastrointestinal or urinary symptoms were reported.
Discussion
The presacral, or retrorectal, space is bordered anteriorly by the rectal wall and posteriorly by the sacrum and coccyx.5,6 This space is typically not distended unless there is an occupying lesion. A presacral epidermoid cyst, like the present patient case, has a diagnostic differential, which should be distinguished from other superficial pathologies. Skin level epidermoid cysts, which may be acquired lesions, are superficial and can communicate with the dermis. 7 Epidermoid cysts are broadly classified as congenital or acquired, with current patient case likely having a congenital origin, based on its location and diagnostic differential. 8
Presacral epidermoid cysts are congenital and have a developmental origin. Congenital lesions make up about two-thirds of presacral masses.6,9 The epidermoid cyst in the presacral location is thought to arise from embryologic remnants of the ectoderm. 10
Presacral epidermoid cysts do not often cause symptoms, depending on the size and compression of surrounding structures. These lesions are often discovered incidentally during diagnostic imaging. When the lesion becomes large enough to cause symptoms, patients often describe lower back pain. Symptoms worsen in the case of infection, fistula, malignancy, or rectum compression, which are complications of cysts in this location. Secondary infection of developmental cysts, in the presacral location, may occur in up to one-third of cases. 10 While not all congenital cysts are benign, developmental cysts, such as the presacral epidermoid cyst, are mostly categorized in the literature as benign lesions.1,9,11 There has been some documentation of a potential malignant degeneration, with developmental presacral lesions. 1 A study by Uhlig and Johnson reviewed 63 presacral lesion cases and of those nine were deemed malignant, but this included various other types of developmental cysts. 12 The patient prognosis is good in the absence of complications and surgical removal is usually recommended for definitive diagnosis and symptom relief.
While reports of presacral lesions typically rely on MRI and CT results, sonography should be considered to examine the presacral space, due to its relatively low cost and lack of ionizing radiation. A CT examination can locate and document the mass, as a cystic lesion with fluid density, but may not offer enough diagnostic information. MRI is often recommended for presacral masses, as it can provide necessary lesion characteristics, which sonography and CT may lack. Diffusion-weighted MRI imaging of presacral epidermoid cysts can be shown as low signal intensity, on the T1-weighted image and high intensity with diffusion restriction on the T2-weighted image.13,14
It is difficult to describe the typical sonographic appearance of the presacral epidermoid cyst specifically, due to the rare use of sonography in this anatomical space. However, congenital epidermoid cysts (i.e. those of the presacral space, testis, head, and neck that arise during fetal development) have the same histologic appearance of acquired epidermal (e.g. more superficial) inclusion cysts. Because of the identical histologic contents, it has been reported that the sonographic appearances would be similar. Epidermal inclusion cysts have a hypoechoic sonographic appearance with variable echogenic foci, posterior enhancement, and lack of color Doppler signal. 15
There is a broad list of lesions, as part of the diagnostic differential, which should be suspected when a presacral mass is identified. As mentioned, two-thirds of lesions in this space are congenital and include developmental cysts, anterior meningoceles, duplication cysts, chordomas, teratomas, and adrenal rest tumors. Neurogenic lesions, osseous lesions, and inflammatory lesions should also be considered. 6
Meningocele was listed as a differential in the present patient case, based on the CT and sonographic examination of the presacral lesion, with associated sacral caudal regression. An anterior meningocele is also, like presacral epidermoid cysts, a cystic congenital lesion and is more common in females. However, an anterior meningocele is not a developmental cyst. The meningocele is caused by a congenital neural tube defect and arises from a defect in the sacrum. A sacral defect was noted as part of the present case study. This can be differentiated from an epidermoid cyst by the meningocele’s internal contents of cerebrospinal fluid and meninges.6,10,16
Another differential listed on a CT report for the reviewed case was a tailgut cyst. Tailgut cysts, like presacral epidermoid cysts, are classified as congenital and developmental. They can be differentiated histologically. Tailgut cysts have glandular or transitional epithelium, while epidermoid cysts do not. 9
A sacrococcygeal teratoma was listed on the pathologist’s report for this patient case but was considered less likely compared to an epidermoid inclusion cyst., which is also a congenital lesion. Like a presacral epidermoid cyst, sacrococcygeal teratomas are more commonly found in females. These neoplasms commonly have solid and cystic components. Unlike presacral epidermoid cysts, clinically, these tumors are usually diagnosed in utero or shortly after birth, due to an externally protruding mass. Teratomas can contain a wide variety of histological components, including tissues from the ectoderm, mesoderm, and endoderm.10,17,18
Conclusion
Because of the wide variety of diagnostic differentials related to presacral lesions, these masses often require multi-modality imaging, biopsy, or surgical removal. While not commonly used, transvaginal sonography can be a valuable diagnostic option, in the evaluation of the presacral space. While MRI is often necessary, sonography can be of use and add value to identify lesion characteristics, especially for patients where MRI is contraindicated.
In the present case report, sonography was of diagnostic value to describe the avascular and cystic characteristics of a presacral lesion, prior to the biopsy. Pathology reports are necessary to confidently identify a lesion. This case report revealed a pathology of an epithelial squamous cyst, with an epithelial inclusion cyst, as the most likely differential diagnosis, based on the pathology report. Although presacral lesions often are surgically removed, the patient in this case received conservative nonsurgical management, as the treated symptoms were contributed to sciatica.
Future research should focus on recent data collection on the incidence of presacral masses, as the published evidence is based on older published studies. To be able to categorize these presacral lesions would require full evaluation, including diagnostic imaging and pathology reports. Because these lesions are often discovered incidentally, it may be difficult to obtain accurate statistics.
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Ethical Statements
Ethical approval was not sought for the present study because all case data were de-identified. The case study presented is for educational purposes only.
Informed Consent
Informed consent was not sought because all case data were de-identified and/or aggregated and followed the ethics committee or IRB guidelines (also referred to as the Honest Broker System).
