Abstract
Splenic cysts are extremely rare. We present the case of a young female child who presented with a massive splenic cyst arising from the lower pole of the spleen. We offered surgical intervention in view of persistent abdominal pain and the large size of the cyst, which was predisposing it to traumatic rupture and restricting the child’s normal activities. Cyst excision with splenic preservation was successfully achieved via a laparoscopic lower pole splenectomy. Histology confirmed a benign epidermoid cyst. The case presentation is followed by a brief review of literature.
Introduction
Cysts of the spleen are extremely rare, with 0.07% incidence in large series.1,2 Of all splenic cysts, epidermoid cysts account for about 10% of the mainly non-parasitic primary splenic cysts.3,4 They tend to occur in younger age groups and show a female preponderance.5,6 Splenic cysts are mostly asymptomatic at presentation, with only 39% presenting with symptoms directly attributed to the cyst – the commonest symptom being left upper abdominal pain. 7 They are most commonly discovered incidentally in imaging studies performed for other reasons. A few patients may present with complications such as rupture and bleeding or infection. Traditionally, surgical treatment with total splenectomy has been recommended, 8 although there has recently been an increased interest in spleen preservation, especially in younger age groups.
Case report
A 9-year-old female of Indonesian nationality presented to us with chronic left upper abdominal discomfort for a period of nearly one year. Her past medical history was unremarkable except for an accidental fall from a chair prior to the onset of symptoms, when she sustained significant trauma to the left upper quadrant of the abdomen. She was initially investigated in Indonesia with ultrasound (US) imaging followed by computed tomography (CT) of the abdomen (Figures 1 and 2). Differential diagnoses based on imaging findings were either an epidermoid cyst or a post-traumatic pseudocyst. She was offered open total splenectomy in view of the large size of the splenic cyst and persistent abdominal pain. Her parents, however, were keen for splenic preservation and sought a second opinion in our tertiary centre.

Massive lower pole splenic cyst showing thinning out of splenic parenchyma. C: cyst; SP: splenic parenchyma which has been thinned out; K: kidney.
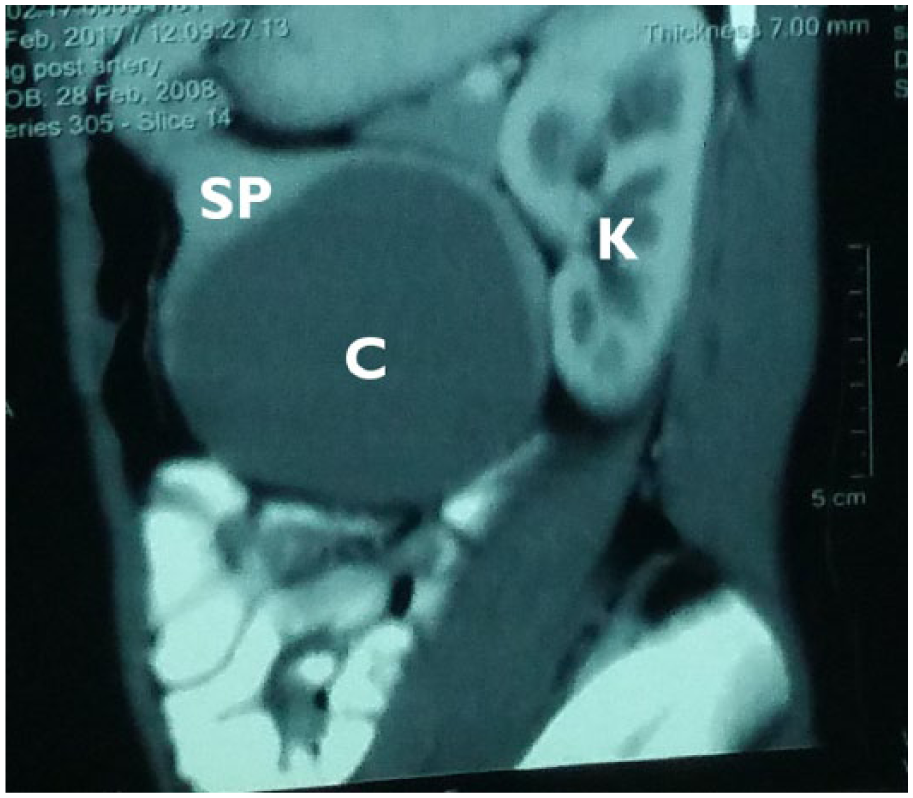
Massive lower pole splenic cyst causing displacement of the left kidney posteriorly and small bowel antero-inferiorly. C: cyst; SP: splenic parenchyma which has been thinned out; K: kidney.
Upon examination we noted a firm splenic mass extending from below the left costal margin down to the left flank. Initial blood investigations were all within normal range. Repeat imaging with US prior to surgery confirmed the persistence of a large cystic lesion with low-level echoes within the spleen, measuring 8.1 × 7.8 × 8.1 cm.
After discussing fully with the parents, we offered laparoscopic lower pole splenectomy with upper pole preservation. The parents were counselled on the possibility of total splenectomy should there be intraoperative haemorrhage or ischaemia of the splenic remnant. Preoperative vaccination was not performed as it was felt that the risk of a total splenectomy was extremely low and should that have been required, there was still an option of vaccination post-splenectomy.
Intraoperatively, the diagnosis of a massive lower pole splenic cyst was confirmed. It was necessary to sacrifice the splenic hilar vessels as the cyst was extending to the hilum. We preserved the short gastric vessels as collateral supply to the remnant spleen and good back-bleeding was noted from the cut surface of the remnant spleen (Figures 3 and 4). Postoperative recovery was complicated by a peri-splenic haematoma and small left basal pleural effusion, both of which were managed conservatively. Postoperative US demonstrated vascularity within the remnant spleen. The patient was discharged well and stable on postoperative day 10. Histology confirmed the diagnosis of a benign epidermoid cyst. She remains well to date.
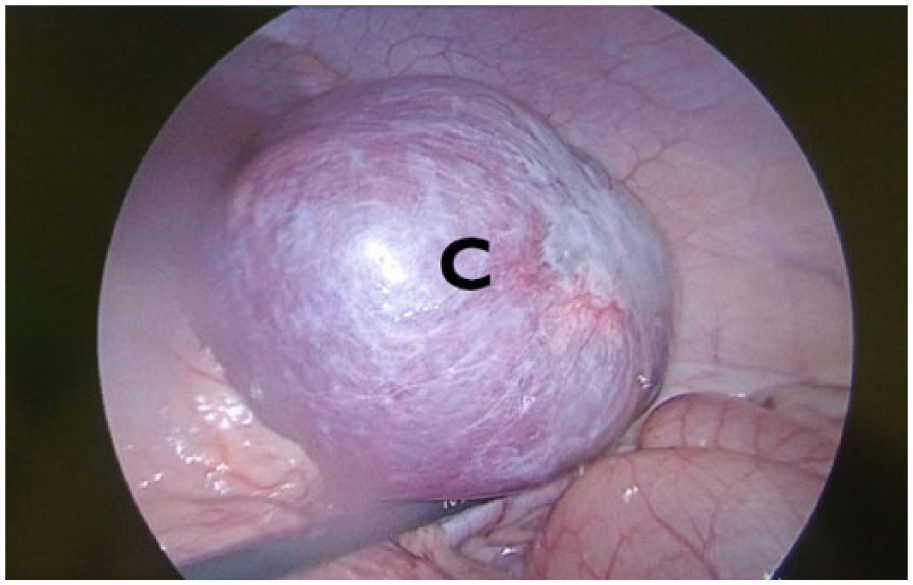
Intraoperative findings of a massive 8 cm well-circumscribed splenic cyst arising from the lower pole. C: splenic cyst.

At the completion of resection, remnant spleen with collateral blood supply from the short gastric vessels. RS: remnant spleen; L: liver; ST: stomach.
Discussion
While the reported incidence of splenic cysts are less than 1% in literature,1,2 the true incidence may be higher as most cysts remain asymptomatic and are noted only as incidental findings in imaging studies. They tend to occur more commonly in females and under the age 40 years. 4 The most widely used pathological classification system was proposed by Martin. 5 He classified splenic cysts as Type I cysts, which are primary (true) cysts with cellular linings, and Type II cysts as false (secondary) cysts without cellular linings. Type I cysts were further classified into parasitic and non-parasitic origin. Non-parasitic cysts can be further classified into congenital and neoplastic lesions (Table 1). Epidermoid cysts are the rarest of all primary splenic cysts, accounting for only 10%. 9
Differences between true and false cysts of the spleen.

Splenic epidermoid cysts are thought to arise from infolding or entrapment of peritoneal mesothelial cells in the splenic parenchyma during embryogenesis in the intrauterine life, although the exact mechanism is unknown. 10 Histologically they are characterised by an inner squamous epithelial lining which differentiates them from false cysts.
Imaging studies are helpful for delineating anatomy and surgical planning, thought they cannot reliably differentiate between true or false cysts. On US, epidermoid cysts appear as well-defined, thin-walled, anechoic cystic lesions. Peripheral calcifications occur more frequently in post-traumatic or false cysts. 10 CT scanning remains the gold standard for preoperative planning.
Once diagnosed, elective surgical management is advised for larger symptomatic splenic cysts to prevent complications. Although complications such as cyst rupture, bleeding and infection of the cyst have been reported,10,11 the exact incidence of each is unknown, as there are no large case series because of the rarity of the condition. For smaller asymptomatic splenic cysts of benign aetiology, conservative management is possible. Location of the cyst in relation to the hilum is a major determining factor with respect to the surgical options: total versus partial splenectomy.
More recently, conservative management of superficially located splenic cysts with marsupialisation or decapsulation have been suggested as an alternative to splenectomy. 12 Earlier attempts to treat splenic cysts by percutaneous aspiration have resulted in limited success rates owing to rapid reaccumulation. Splenic decapsulation has emerged as a more viable alternative; 13 however, no centre has reported significant experience with this technique. Marsupialisation of splenic cysts using a laparoscopic approach has also been suggested. 14
Currently, a more conservative and minimally invasive approach is preferred for benign, symptomatic cysts larger than 5 cm. If anatomically and technically feasible, spleen preservation with laparoscopic partial splenectomy can be attempted. 15 For larger cysts, a hand-assisted laparoscopic approach is advocated. 8 Uranüs et al. described partial splenectomy using surgical stapling devices. 16 As mentioned before, owing to the rarity of splenic cysts, there is a paucity of evidence-based guidelines for management of splenic cysts in the paediatric population.
Conclusion
Partial splenectomy using a laparoscopic approach was successfully performed for this case with a massive splenic cyst encroaching the hilum. Even though the hilar vessels had to be sacrificed, the remnant spleen was vascularised by collateral supply from the preserved short gastric vessels, suggesting the feasibility of such an approach in cases of hilar involvement. Because of the rarity of splenic cysts in the paediatric population, there is a paucity of definitive guidelines for management of splenic cysts, but the importance of a spleen-preserving approach is well received as the immunological function of the spleen can be preserved.
Footnotes
Acknowledgements
None.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Availability of data and materials
Not applicable.
Authors’ contributions
LBS conceptualised the project and performed the literature survey. LBS and SG prepared the initial manuscript. CYL and OLY revised the manuscript and made critical revisions. CYL and OLY were responsible for the overall surgical care of the patient. All authors read and approved the manuscript.
Conflict of interest
None declared.
Informed consent
Written informed consent was obtained from a legally authorised representative for anonymised patient information to be published in this article.
Ethical approval
Not applicable.
