Abstract
Objective:
Supporting sonographers’ health and well-being requires targeting the workplace factors they identify as most influential. This study examined sonographers’ perspectives to guide priorities for resource allocation and solution development.
Materials and Methods:
An online survey of 1276 U.S. and Canadian sonographers asked participants to rate 30 workplace factors across four categories—workflow, equipment/physical environment, administrative/organizational environment, and training/health practices—on their perception of impact on well-being and importance for understanding and improving. Respondents selected up to five factors as the highest priorities for immediate action and resource allocation.
Results:
Five factors ranked among the top 10 across specialties and were rated as significantly impactful and important by more than two-thirds of respondents: productivity requirements (76.9% impact, 74.3% importance), staff scheduling policies (73.2%, 74.4%), supervisor support (72.1%, 71.2%), exam room furniture (73.1%, 68.0%), and ultrasound machine design (69.3%, 75.6%). Exam scheduling was the top priority across all practice areas and the only factor identified in the top five by a majority of all respondents.
Conclusion:
While specialty area differences exist, sonographers consistently identified administrative and organizational factors as the most impactful, important, and of highest priority for immediate action. Addressing these concerns requires contextualized solutions developed with direct practitioner input.
Keywords
The sonography profession remains entrenched in a decades-long crisis of work-related musculoskeletal disorders (WRMSDs),1,2 recently intensified by reports of poor sonographer well-being amidst growing levels of burnout.3–5 WRMSDs and declining well-being result from an intricate interplay between ultrasound equipment, furniture, and physical workspace arrangements, various aspects of patient interactions and imaging processes, and factors related to the broader organizational and administrative environment of the workplace.6,7 Despite marked improvements in selected aspects of sonography, primarily focused on the enhanced ergonomic design of machines, transducers, support devices, and furniture, WRMSDs and burnout remain persistent among sonographers. Evidence suggests the need for an expanded focus on aspects of workflow and patient factors 8 alongside improvement in organizational and administrative policies and practices.9,10
Solutions to worker health issues tend to be more effective when workers are actively and meaningfully engaged in identifying, designing, and implementing those solutions. 11 Participatory approaches have been successfully used to develop supportive interventions for work processes in other healthcare settings, for example, reducing stress and burnout within emergency departments 12 and improving workplace culture and employee flourishing within maternity wards. 13 Exceptionally limited evidence exists that reports on participatory approaches or first-hand accounts from the sonography workforce. The handful of studies that exist have focused primarily on the physical aspects of sonography work, such as improvements to ultrasound equipment, 14 exam support devices, 15 and patient room designs, 16 or have been small-scale, exploratory studies in specific work contexts with limited generalizability. 17
The noticeable lack of firsthand accounts from the sonography workforce, especially regarding non-physical workplace factors affecting health and well-being, hampers a comprehensive understanding of worker perspectives, meaningful solution development, and successful implementation in practice. This study aimed to elucidate sonographers’ perspectives on the impact of various workplace factors on their health and well-being and to identify priorities for improving sonography work environments. Understanding sonographers’ perspectives on these factors is a crucial step in setting priorities, providing actionable insights, and creating practical solutions that effectively promote sonographers’ health and well-being. Ultimately, these practitioner-identified priorities can facilitate the development of interventions and strategies to improve the work environment and promote a culture of health, safety, well-being, and excellence in patient care.
Materials and Methods
Study Design and Participants
This report presents analyses of a subset of data collected from a prospective, longitudinal survey study that tracks personal circumstances and job-related factors associated with WRMSDs and well-being among a registry of sonographers from the United States and Canada. A detailed description of the recruitment methods, inclusion criteria, and demographic data collected in the initial questionnaire has been published previously. 9 The data examined and described in this paper consist of responses from members of the study registry who completed a one-year follow-up questionnaire between June and July 2022. Respondents who were not actively employed, were students, or were working outside the United States or Canada at either time point were excluded from this analysis. All study procedures were reviewed and approved by the Ohio State University’s institutional review board; respondents indicated their consent for the use of any information provided before completing each survey, and all personal data were securely stored according to institutional guidelines. No incentives were offered for survey completion.
Data Collection
Participants accessed the closed survey on the Qualtrics online platform through a unique link sent to their email address. While they could resume the survey at any time, each unique link allowed only one submission of a complete response. All participants answered questions in the same order; adaptive questioning was used to display only relevant follow-up questions as needed. Prompts informed participants when they skipped questions to promote complete responses, and they could use the back button to review and update their answers. Before launching the survey, three members of the research team tested the usability and functionality of the questionnaire to ensure all data could be collected as intended.
At the outset of the survey, respondents confirmed or updated their demographic characteristics as recorded in the study registry database based on responses to the initial questionnaire (e.g., primary practice setting, primary sonography practice area, credential). Updated responses to the primary sonography practice area were used to group respondents into five practice specialties. Specifically, respondents who only selected cardiac (pediatric or adult), OB/GYN, or vascular were grouped into their respective practice specialties. Respondents who indicated conducting abdominal exams, either only or in combination with any other type of exam, were placed into an abdominal+ (i.e., Abd+) practice specialty group. All remaining respondents, who either had combinations of areas that did not include abdominal or who worked in other areas such as musculoskeletal and veterinary, were placed into a multi-specialty group.
The core component of the follow-up questionnaire included 13 questions distributed across 5 pages that collected respondents’ perceptions of sonography work system factors and other commonly reported training, education, or supports outside of the work system associated with sonographers’ health and well-being. Perceptions of a total of 30 factors, divided into four categories, were explored:
Workflow (n = 8): cognitive load associated with exam performance; coding and billing; communication with co-workers, physicians, and staff; communication with patients, caregivers, and families; emerging technologies to support image acquisition and analysis; exam scheduling; patient factors (e.g., body habitus, comorbidities); generating reports and other documentation.
Equipment and Physical Environment (n = 8): exam room environment; exam room furniture; exam room layout; exam support devices; patient transfer devices; sonography machine design; transducer design; workstation setup.
Administrative and Organizational Environment (n = 7): continuous quality improvement processes; co-worker support; lab or workplace accreditations; policies and procedures related to staff scheduling; productivity or performance requirements; supervisor support; workplace culture regarding worker health and well-being (i.e., workplace health culture).
Training and General Health Practices (n = 7): diet, sleep, and general health education or support; employee assistance programs; employer health incentive programs; ergonomics workshops or seminars; exercise, stretching, and physical activity interventions; mindfulness meditation and other stress reduction techniques; peer mentoring and work coaching supports.
Respondents rated the impact of each factor on sonographers’ health and well-being, considering both negative and positive effects, using a 4-point scale with anchors of (1) No Impact, (2) Minor Impact, (3) Moderate Impact, and (4) Significant Impact. Then, they used the same 4-point scale to rate the importance of dedicating resources to examine or address each factor to promote sonographer health and well-being: (1) Not Important, (2) Minor Importance, (3) Moderate Importance, and (4) Significant Importance. When rating each factor on these two dimensions, respondents were encouraged to consider not only their own experiences but also those of the broader ultrasound community. After rating the items across the four categories, respondents selected up to five factors from the full list of 30 that they believed should be prioritized for immediate action.
Data Analysis
The percentages of respondents rating each factor across the four categories, from “not impactful/important” to “significant impact/importance,” were calculated and visually displayed to illustrate the distribution of ratings. Then, each response was assigned a numeric value based on the ordinal categories (i.e., 1–4), and approximated averages were calculated for each factor, both overall and by practice specialty. The term “approximated” is used intentionally because measures of variability were not computed, and the distributions for each item were not thoroughly assessed for normality before treating the ordinal data as continuous. Instead, these approximated averages serve as a way to explore potential differences in ratings of impact and importance across all factors and the four main work system categories. In addition to calculating ratings across all respondents, approximated averages were also computed within each of the five practice specialty groups.
Multiple analysis steps were completed to understand respondents’ perceptions of the most critical factors requiring immediate action. First, the percentage of respondents who selected each factor as one of the top five most critical was recorded within each practice specialty area. These factors were then ranked by response frequency to establish a within-group priority order for each practice area. Finally, an overall rank order was determined using a process that treated all practice areas equally. Specifically, if the overall ranking was based solely on how often each factor was selected across all respondents, it would favor practice areas with more respondents and potentially mute the perspectives of those in areas with fewer respondents. Therefore, the overall rank of the 30 factors was calculated by averaging the within-group selection percentages for each factor and then sorting from highest to lowest.
Results
A total of 1276 from the study registry of 3659 sonographers provided complete responses to the survey and were included in the analysis (i.e., 34.9% response rate). These respondents had an average age of 49.9 years (SD = 11.3) and were primarily White (n = 1129, 88.5%), non-Hispanic (n = 1215, 95.2%), and female (n = 1119, 87.7%). Nearly half of the respondents (n = 585, 45.8%) indicated that they conducted abdominal exams (i.e., the Abd+ group). Respondents practicing within single areas included adult and/or pediatric cardiac (n = 270, 21.2%), OB/GYN (n = 152, 11.9%), and vascular imaging (n = 139, 10.9%). The remaining 130 individuals reported practicing across multiple areas or other specialties (e.g., veterinary, musculoskeletal). Among the places where the respondents worked, noting that some worked in multiple types of settings, the majority conducted imaging in hospital settings (754, 59.1%), nearly half worked in outpatient clinics (596, 46.7%), and 293 (23.0%) worked in a physician’s office. Fewer than 10% of the sample indicated that they worked in other settings, including education or urgent care.
Impact and Importance of Selected Factors Relative to Sonographer Health and Well-Being
The distribution of response frequencies on the impact and importance rating scales across all 30 factors, organized into the four work system categories, is shown in Figure 1. As indicated by the frequencies displayed as bolded percentages in Figure 1, the largest number of respondents rated almost all factors in the administrative/organizational environment and the equipment/physical environment categories as having both a significant impact and significant importance relative to sonographer health and well-being. Notably, except for lab accreditation and co-worker support, more than 90% of respondents identified the other five administrative and organizational environment factors as having a moderate or significant impact on health and well-being, and as being important for allocating resources.
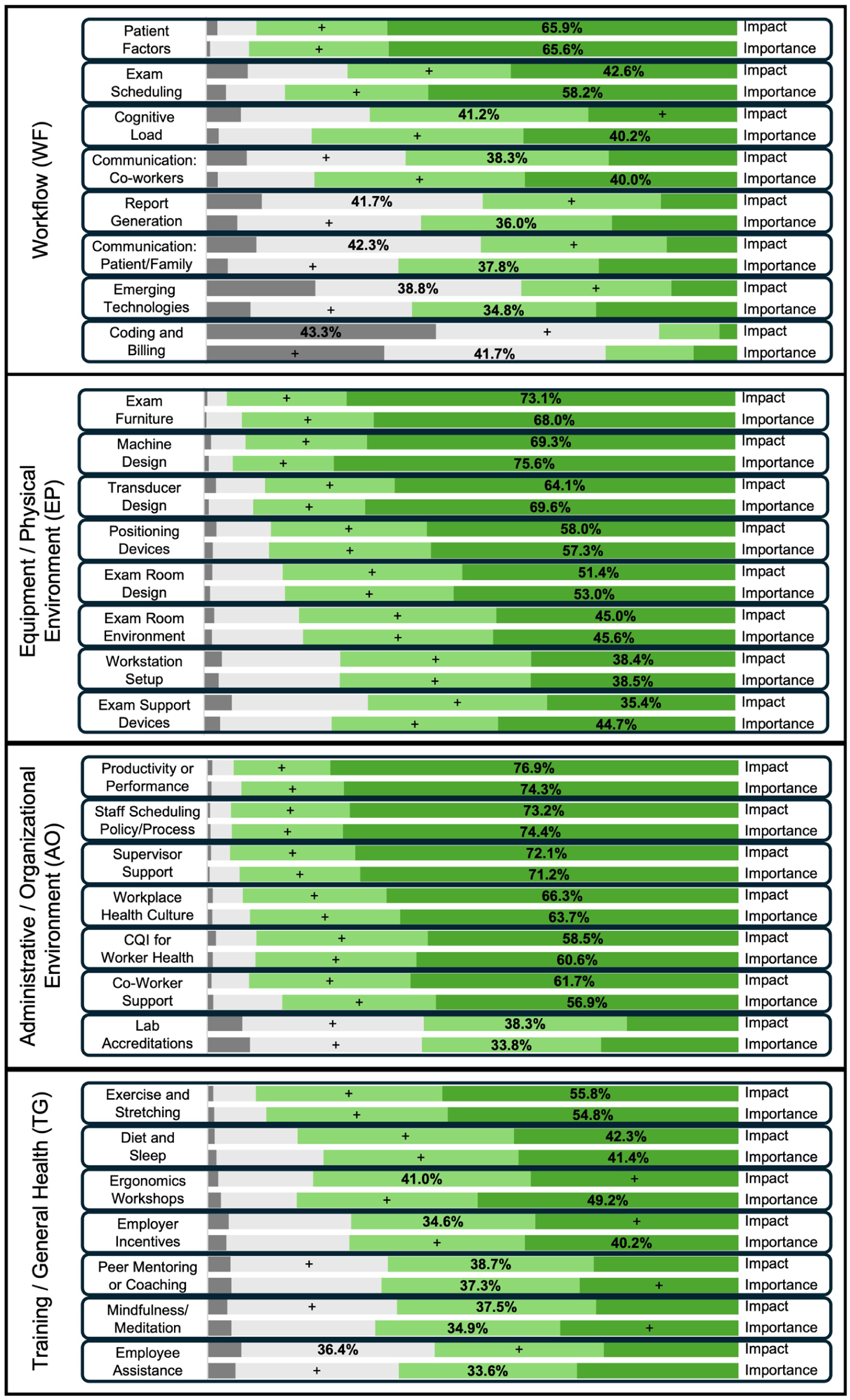
Distribution of sonographer perceptions of the impact on worker health and well-being and the importance for dedicating resources to address each of 30 factors. The distributions of rating options displayed from left to right for each item include no impact/importance (dark gray), minor impact/importance (light gray), moderate impact/importance (light green), and significant impact/importance (dark green). The frequency of the most selected response is shown as a percentage in bold font, and a plus sign (+) indicates the second most frequently selected categorical response for each item.
In total, six of the seven factors within the administrative and organizational environment were identified as significant in both impact and importance by more than 50% of respondents, while five of the eight equipment/physical environment factors met this majority criterion. Although ratings were more evenly spread, all factors in the training/general health and workflow categories were rated as having moderate or significant impact and importance by over half of the respondents, with only one factor (i.e., exercise and stretching) rated as significant by the majority on both scales. The perceptions of impact and importance for factors within the workflow category varied more widely than in the other three categories.
Eight of the 30 individual factors were identified by more than 60% of respondents as significant both in terms of their impact on sonographer health and as important for guiding resource allocation to address them. (1) Productivity and performance requirements, (2) staff scheduling policies and processes, and (3) supervisor support were identified as the most critical factors, with more than 70% of respondents rating these factors as significant on both measures; approximately 95% of respondents rated the impact and importance of these factors as at least moderate. The impact of (4) exam room furniture on health and well-being was rated as significant by 73.1% of respondents, with a slightly lower percentage regarding the importance of dedicating resources to this factor as being significant (68.0%). Conversely, a higher percentage of respondents indicated that dedicating resources was significant for (5) machine design (75.6%) and (6) transducer design (69.6%), compared with the percentage that considered these factors to have a significant impact (69.3 and 64.1%, respectively). (7) Patient factors affecting exams and (8) workplace health culture were among the final most critical factors, with each receiving roughly two-thirds of respondents’ ratings as significantly impactful and important for resource dedication.
Although the overall distribution of ratings on impact and importance generally followed the same pattern across all practice areas, some subtle nuances in practice-area-specific ratings can be observed (See Figure 2). These differences were most noticeable in the ratings of OB/GYN sonographers, who rated the impact on sonographer health and well-being and the importance for understanding of patient factors, exam scheduling, workstation setup, communication with patients and families, emerging technologies, and coding and billing higher than other practice areas, while assigning lower importance to positioning or transfer devices. Cardiac sonographers also rated the impact and importance of emerging technologies higher than other areas, but aligned with vascular sonographers in indicating a slightly lower impact of exam scheduling. Although similar to other practice areas in impact ratings, vascular sonographers placed slightly more importance on dedicating resources to positioning and transfer devices.
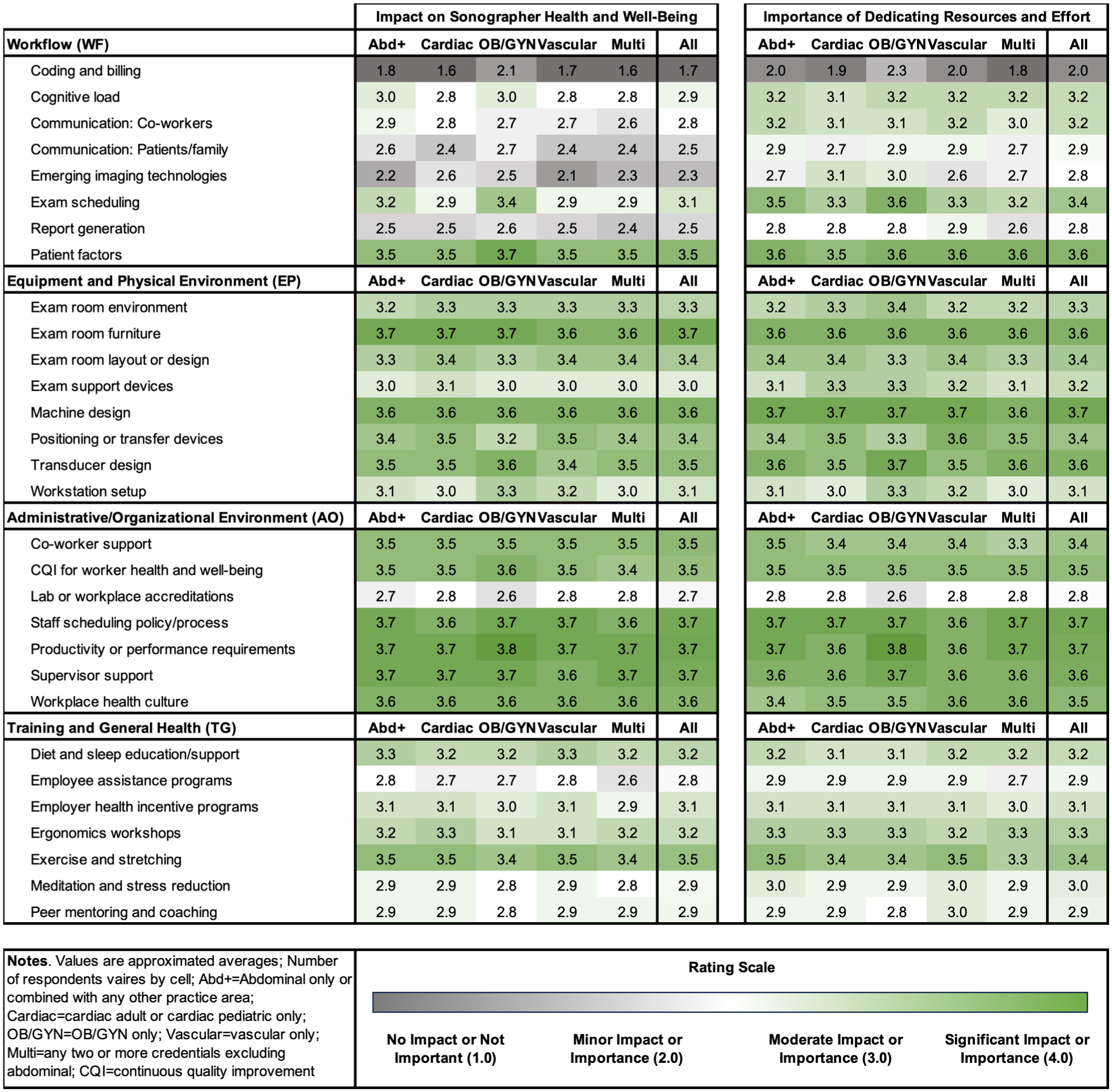
Approximated average ratings of impact on sonographer health and well-being and the importance of dedicating resources toward addressing the factor compared across respondents from different sonography practice areas, ranging from no impact or not important (1.0) to significant impact or importance (4.0).
Priorities for Immediate Action and Dedication of Resources
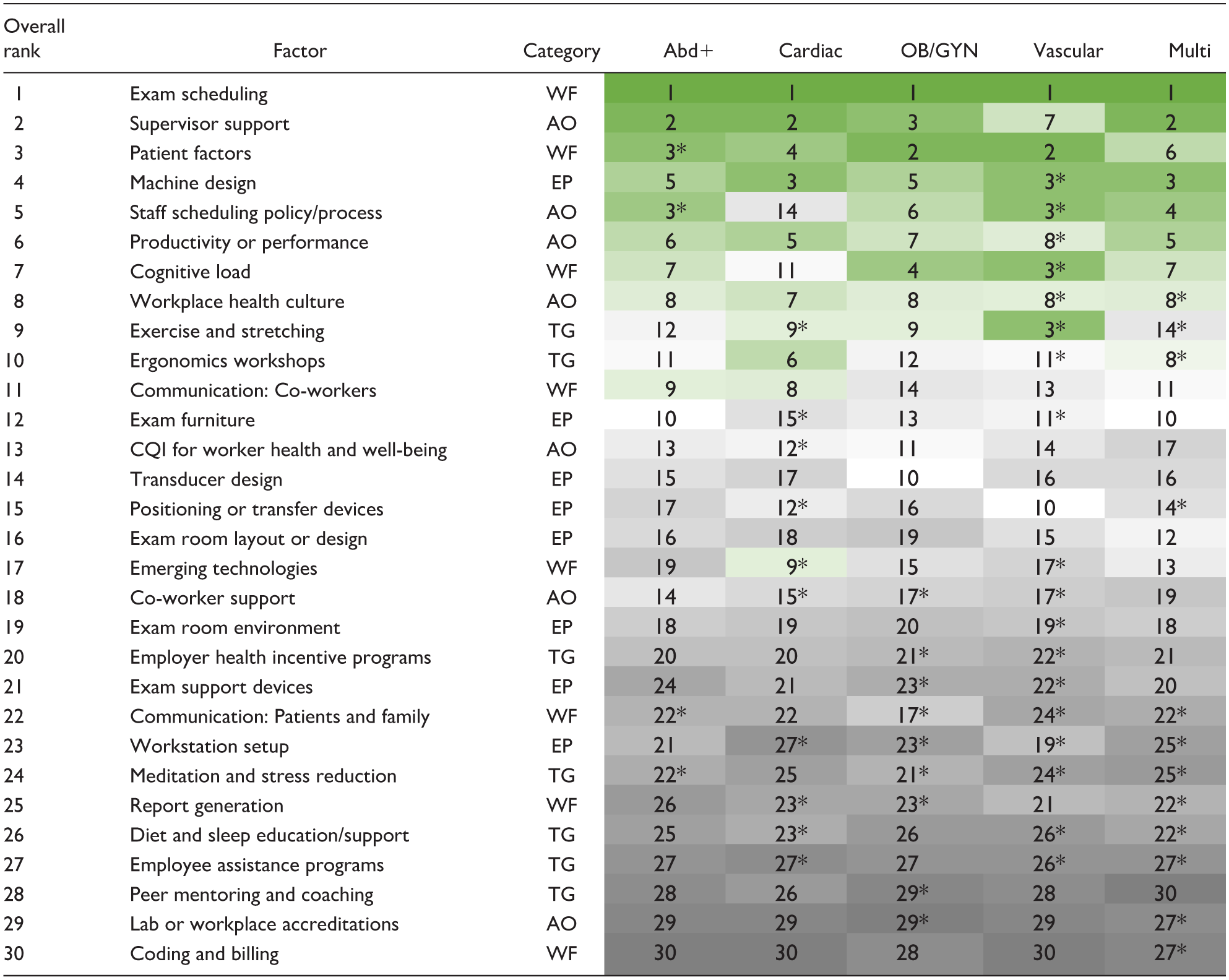
Table 1 presents the priority ranking of all 30 factors, both overall (first column) and within each practice area, based on how often respondents selected them as their top five priorities. Six items were identified as priorities for immediate action and resource allocation across all practice areas. (1) Exam scheduling, although not among the top eight most critical factors based on impact and importance ratings, was ranked as the top priority for immediate action and resource allocation across all specialties. In fact, with a selection frequency of 55.9% (n = 680), exam scheduling was the only item chosen as a top five priority by the majority of respondents, including more than two-thirds of OB/GYN sonographers. (2) Supervisor support was the second most frequently chosen factor, with about one-third of the sample (n = 413, 33.9%) selecting it. Four other factors were mainly ranked in the top ten across the different practice areas: (3) patient factors, (4) ultrasound machine design, (5) productivity and performance requirements, and (6) workplace health culture.
Prioritized ranking of factors, overall and by practice area, for resource allocation and immediate action to support and promote sonographer health and well-being.
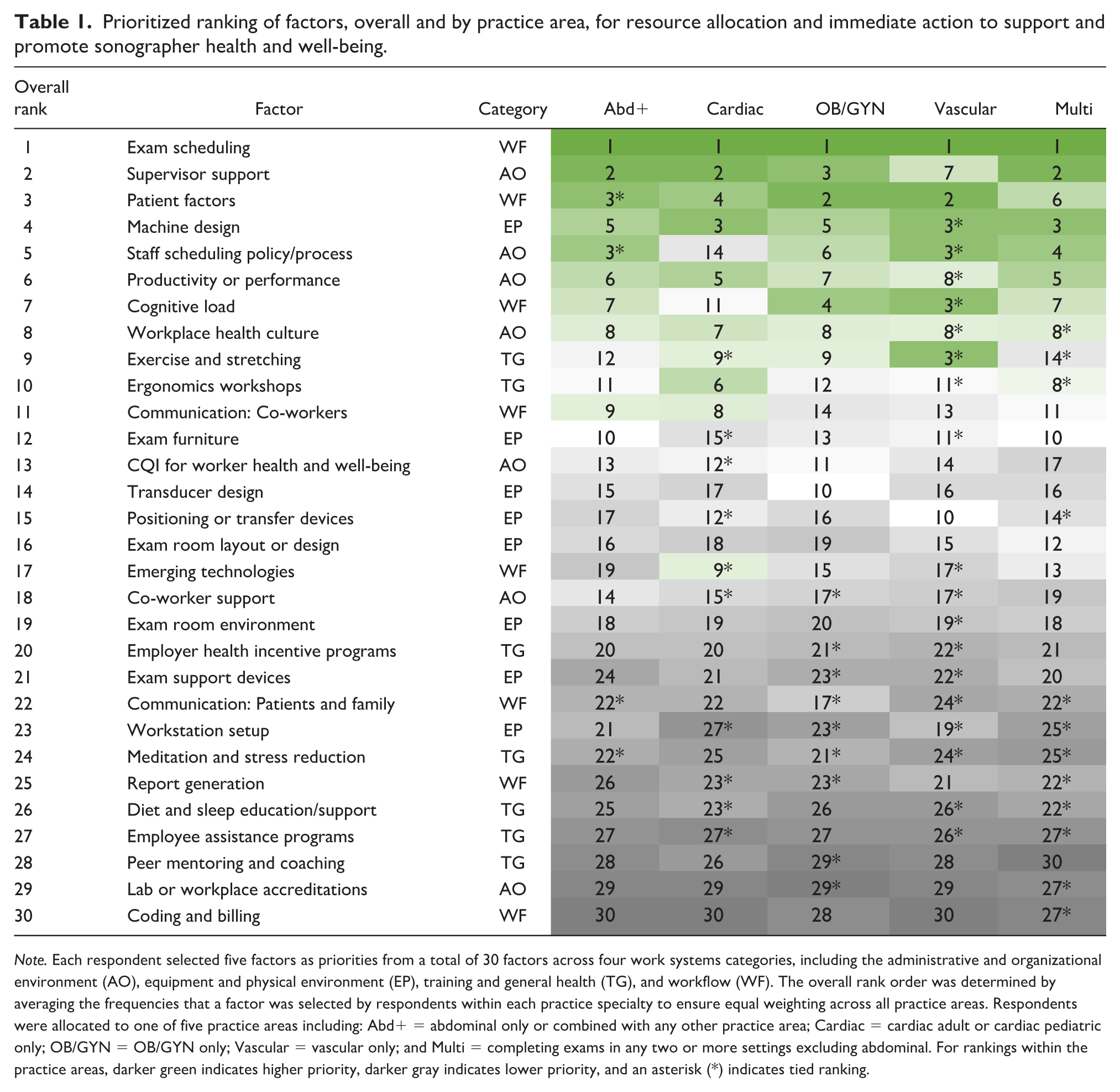
Note. Each respondent selected five factors as priorities from a total of 30 factors across four work systems categories, including the administrative and organizational environment (AO), equipment and physical environment (EP), training and general health (TG), and workflow (WF). The overall rank order was determined by averaging the frequencies that a factor was selected by respondents within each practice specialty to ensure equal weighting across all practice areas. Respondents were allocated to one of five practice areas including: Abd+ = abdominal only or combined with any other practice area; Cardiac = cardiac adult or cardiac pediatric only; OB/GYN = OB/GYN only; Vascular = vascular only; and Multi = completing exams in any two or more settings excluding abdominal. For rankings within the practice areas, darker green indicates higher priority, darker gray indicates lower priority, and an asterisk (*) indicates tied ranking.
Six additional factors, for a total of 12, were identified as top priorities by sonographers in specific practice areas, with cardiac sonographers showing the most divergent perceptions of priorities compared with other practice areas. (7) Cognitive load tied for the third most important priority among vascular sonographers and was the fourth highest priority among sonographers in OB/GYN, but this factor was not within cardiac sonographers’ top ten priorities. Similarly, (8) staff scheduling ranked fifth overall, yet cardiac sonographers ranked this factor as 14th. Two training factors were ranked substantially higher within practice areas than in the overall ranking: (9) exercise and stretching were tied for third among vascular sonographers, and (10) ergonomic workshops were ranked sixth among cardiac sonographers. (11) Communication with co-workers was also ranked slightly higher by abdominal+ and cardiac sonographers than by others. Finally, although ranked 17th overall, cardiac sonographers identified (12) emerging technologies as one of the top ten priorities for immediate action and resource allocation.
Discussion
This study gathered sonographers’ perspectives to identify the most critical work system factors affecting the health and well-being of the sonography workforce and to develop a list of practitioner-identified priorities for allocating resources aimed at improving ultrasound user health and well-being. Six critical factors emerged due to being rated both significantly impactful and significantly important, alongside being consistently ranked among the top priorities for immediate action and resource dedication across all sonography practice areas. Four of these critical factors are features of the administrative and organizational environment: productivity and performance requirements, staff scheduling policies and processes, supervisor support, and workplace health culture. The other two critical factors include patient factors impacting workflow and ultrasound machine design. Two additional physical factors—exam room furniture and transducer design—were rated as highly impactful and important, but were not among the top priorities. Conversely, two additional workflow factors—exam scheduling and cognitive load—were among the top priorities, but were not consistently rated as having a significant impact on health and well-being.
Addressing Critical Administrative, Organizational, and Workflow Factors
Across all sonography practice areas, survey respondents identified four of the seven work system factors under the category of administrative and organizational environment and three workflow factors among the top ten priorities for immediate action and dedication of resources. To better understand issues within workflow and at the organizational level of the sonography work system, it is important to revisit the historical context of growth in sonography practices. At its outset, sonography began as a clinical area within larger hospital departments, such as radiology and cardiology. A team of pioneering sonographers worked together with support from these larger medical departments to manage their own productivity and performance requirements, staff scheduling, policies, and practices. Due to the growing utility of sonography, imaging began being offered in physicians’ private practices, where teams of sonographers worked in concert with their hiring physician to provide outpatient diagnostic services.
As diagnostic accuracy improved and the benefits of sonography became more widely recognized, sonography gained attention and its use expanded across many areas of medicine (e.g., obstetrics, vascular surgery, emergency medicine). 18 This growth of sonography has often been called the “sonic boom.”19,20 With this exponential growth in practice and utilization, sonographers’ ability to manage their own administrative and organizational environments diminished. The reliance on hospital systems to provide productivity statistics and patient scheduling was essential, allowing more time to be spent on patient examinations and mastering innovations in sonography. As hospital systems expanded and developed teams within administrative areas, it was not always clear how different diagnostic specialties within medicine were managing their input and output. Physicians also fell victim to this surge in diagnostic requests and became further removed from the day-to-day operations of sonography clinics, relying more on sonographers’ notes. 21
The lack of direct interaction and remote administrative support marked a shift from those early clinics’ direct control of their administrative and organizational environment to the current reliance on indirect control. As the diagnostic impact became clearer, tighter controls were recommended to prevent the overuse of sonography and other imaging techniques. 22 Again, external influences were placed on sonography clinics to align with national and international practice standards, which significantly altered clinical performance and protocols. This shift from direct to indirect control of their administrative and organizational environment highlights the perception among respondents that daily work within sonography practice can feel indirectly controlled and not directly supported. Notably, given that survey participants had a mean age of 49.9 years, a majority of respondents may have at least been trained, if not worked, in a more directly controlled work environment that has rapidly evolved into a more indirect administrative setting.
The present analysis makes the need for solutions to sonographer involvement in administrative decisions even more urgent; regardless of the sonography specialty, employees should reasonably expect that supervisors and managers understand the nuances of how their work is executed and completed. Interestingly, although it was only identified as significantly impactful among OB/GYN sonographers, exam scheduling—a critical part of the administrative and organizational environment—was ranked as the top factor requiring immediate action across all practice areas. It was also the only factor chosen as a top five priority by the majority of participants (i.e., >50%). This indicates that the current study participants are expressing a need for more direct control over how work is scheduled and for sonographers to have the flexibility to manage both simple and complex patient cases. Relatedly, the critical factor of workplace productivity and performance has also changed from the early days of establishing sonography clinics to now, where non-sonographers are often responsible for managing the work area and aiming to improve hospital system-wide efficiency in input and output.
Earlier analyses have pointed out that a lack of understanding about the nature of sonographers’ work can lead to mistrust and complicated work decisions.3,23 A wide range of workflow factors directly affect sonographers’ daily workload, especially the variable cognitive load associated with different types of exams and the implications of numerous patient factors on the performance of an exam, both being top-10 priorities across nearly all practice settings. Take, for example, the need of OB/GYN sonographers to document maternal-fetal information while simultaneously providing personal support for patients grieving the loss of a pregnancy. These unique workflow factors can often be misunderstood or not considered by administrators who do not fully understand the work of sonography, and can be further exacerbated by shifts in sociopolitical culture, perceptions, and other historic events, as was experienced during the COVID-19 pandemic. 24
Ultimately, ensuring sonographers are involved in developing healthy workplace cultures is a continued area of concern. 25 Communication, noted as a unique priority for abdominal+ and cardiac sonographers in this study, is one potentially important mechanism for promoting a healthy workplace culture for sonographers. In a qualitative study of managers and their employees in a different field, direct communication from management to workers, providing information, emotional support, and supervisor assistance, was the most critical form of support, viewed as even more important than financial incentives. 26
Addressing Critical Equipment, Physical Environment, and Training Factors
Four out of eight physical factors were ranked within the top 10 priorities in at least one practice area; each was also rated by more than half of the respondents as significant in impact and importance. Among these, ultrasound machine design was consistently ranked in the top five by sonographers across all practice settings. Exam furniture, transducer design, and positioning or transfer devices were each ranked as the number 10 priority by abdominal+, OB/GYN, and vascular sonographers, respectively. Cardiac, OB/GYN, and vascular sonographers all rated exercise and stretching within the top ten priorities, while cardiac sonographers also ranked ergonomic workshops as a key priority. These practice-area-specific needs are likely related to changes that have led to prolonged exams (e.g., contrast), handling of larger 3-D transducers, and other exam-specific factors. It has been noted that generic ergonomic designs, training, and interventions are less effective when not considered and applied within the context of actual work situations. 27 Development of equipment and training solutions to improve sonographers’ health and well-being will no doubt require consideration of the unique aspects of individual practice areas.
Historically, as with changes in administrative and workflow factors, the approach to purchasing equipment and designing sonography workspaces has evolved. Initially, a team of physicians and sonographers directly selected equipment and designed exam spaces. Over time, this process shifted toward a system-based decision model, moving away from direct decision-making to an indirect purchasing system that often limits broader input on the design, selection, and procurement of work tools. Research indicates that sonographers have specific opinions about furniture, equipment, and other items that support their work within designated spaces and hospital settings, 28 which may not be readily considered in the predominant decision-making models.
Promoting participatory approaches that involve workers in equipment purchasing decisions reflects a return to more direct control over how work is performed. Recently, a criteria-based algorithm was created to help sonographers and doctors with equipment purchases, aiming to lower the risk of WRMSDs. 29 When tested in an Italian hospital system, the criteria-based methodology enabled sonographers and physicians to select the optimal ultrasound equipment system, balancing the need to minimize injury exposure and meet the hospital’s production requirements. 29 According to the current study, there is likely a need for further development, testing, and implementation of collaborative decision-making tools and processes within healthcare organizations involved in purchasing medical equipment, ultrasound transducers, and exam room furniture.
Conclusion
Although sonography has become a key diagnostic tool and an important part of modern medicine, its increased use may have come at the expense of the medical professionals who perform ultrasound exams. Across various sonography practice areas, sonographers in this study shared their perceptions of how important and impactful 30 work system factors are on the health and well-being of ultrasound professionals. Nearly all administrative factors (i.e., supervisor support, co-worker support, workplace culture, productivity/performance requirements, staff scheduling policies/processes, and continuous quality improvement processes focused on worker health and well-being) were rated highly in both importance and impact by more than half of the participants. Several equipment and physical environment factors (including exam room furniture and design, machine and transducer design, and patient positioning devices), along with patient factors during exams and sonographer exercise routines, were also considered significant.
The five most urgent factors for immediate action—such as advocacy, research, education, program development, and policy change—based on the priority for resource allocation are exam scheduling, supervisor support, patient factors, ultrasound machine design, and staff scheduling policies and processes. While providing a crucial diagnostic test remains vital, it is equally important to address the many factors that sonographers believe influence their health and well-being by reinforcing those with positive effects and reducing or eliminating those with negative effects. Considering the intersection of participants’ ratings and priority rankings, efforts to support sonographer health and well-being should primarily focus on exam and staff scheduling, productivity and performance demands (including patient factors impacting exam performance), supervisor support, and workplace health and safety culture, alongside continued improvements in ultrasound equipment design.
Footnotes
Acknowledgements
The authors thank the WRMSD Grand Challenge Alliance and other organizations that provided resources for developing the participant registry used to collect survey responses. These include the American Institute of Ultrasound in Medicine, American Registry for Diagnostic Medical Sonography and Inteleos, American Society of Echocardiography, Intersocietal Accreditation Commission, Joint Review Committee on Education in Cardiovascular Technology, Society for Vascular Ultrasound, Society of Diagnostic Medical Sonography, the Society of Diagnostic Medical Sonography Foundation, and Biodex, part of Mirion Technologies.
Authors’ Note
The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: RJW received training and support for his contributions toward the research reported in this publication from the National Institute on Minority Health and Health Disparities of the National Institutes of Health under Award Number F32 MD020253.
Ethics Approval
Ethical approval for this study was obtained from The Ohio State University’s Institutional Review Board (IRB#: 2021B0113).
Informed Consent
Written informed consent was obtained from all subjects before the study.
Animal Welfare
Guidelines for humane animal treatment did not apply to the present study because no animals were used during the study.
Trial Registration
Not applicable.
Peer Reviewer Guarantee Statement
The Editor of JDMS is an author of this article; therefore, the peer review process was managed by alternative members of the Board, and the submitting Editor had no involvement in the decision-making process.
Peer Reviewer Guarantee Statement
A member of the JDMS Editorial Board is an author of this article; therefore, the peer review process was managed by alternative members of the Board and the submitting Editorial Board member had no involvement in the decision-making process.