Abstract
Objective:
The purpose of this study was to explore the occupational burnout levels among a cohort of sonographers practicing in the United States and their perception of administrative support and resources for burnout prevention.
Materials and Methods:
This study used a quantitative descriptive design with a cross-sectional online survey administered to the Society of Diagnostic Medical Sonography members. The survey consisted of demographic information, administrative support questions, and burnout measurements using the validated Oldenburg Burnout Inventory.
Results:
A total of 1393 sonographers participated in the study. The results of this sonographer cohort indicated that 55.7% experienced moderate burnout. Although 30.9% reported feeling their employers cared for their well-being, 36.6% of respondents indicated no administrative support, and 30.7% said their administration did not provide resources to help them cope.
Conclusion:
Occupational burnout levels among this cohort of sonographers was moderate and could increase without adequate intervention. Addressing sonographer burnout and managing stressors will help organizations to retain staff, continue providing quality patient care, and maintain patient outcomes.
Keywords
Occupational stress and burnout have been well documented globally and reported in an estimated 30% of the working population. 1 Recent evidence indicates a concerning increase in occupational burnout among health care professionals and sonography may be no exception.1,2 Burnout is a work-related syndrome, resulting from continuous exposure to emotional stressors in the workplace, if left unmanaged, may lead to an incapacitating state characterized by emotional exhaustion, depersonalization, detachment, and a sense of diminished personal accomplishment.1 –4 Emotional exhaustion, a hallmark of burnout, is defined as the physical and mental fatigue resulting from long-term workplace stressors. 2 Depersonalization and detachment occur when individuals struggle to empathize with others, responding with indifference. 3 A decline in personal accomplishment accompanies these feelings, eroding a sense of proficiency and achievement in one’s work. 3 The literature indicates that the recent global COVID-19 pandemic, itself a significant stressor, has increased the challenges faced by health care workers including sonographers.5 –7
Most research has focused on professionals like nurses and physicians, leaving sonographers overlooked and overwhelmed without adequate support and coping resources.2,8 Recent studies highlighted the increased prevalence of burnout in sonographers, identified the causes of sonographer burnout, and suggested prevention strategies.2,8 –12 Occupational burnout in sonographers can occur because sonographers are expected to do more with fewer resources, have demanding work schedules, and frequently being on-call outside of regular working hours.2,8 –10,13,14 Despite evidence demonstrating the existence of sonographer burnout, many organizations and administrators lack an understanding of the causes of burnout among sonographers and have been slow to grasp the causes of this problem leaving sonographers with limited support and resources.2,8 –13 Researchers have focused on exploring the predictors of burnout among sonographers to identify and implement prevention techniques to mitigate burnout syndrome.8 –12 These predictors include variables such as clinical settings, psychological job demands, job dissatisfaction, staffing shortages, compassion fatigue, administrative constraints, and greater productivity demands.2,5,8,11,13
Occupational burnout not only affects health care workers’ quality of life but also necessitates the maintenance of a work-life balance. However, a lack of awareness often prevents employees from using available resources to combat adverse health effects such as long-term diseases and emotional fatigue.1,6,15 Several studies documented the effects of occupational burnout on health care workers, including job dissatisfaction, absenteeism, personnel turnover, and staffing shortages caused by health care workers leaving their profession prematurely. 15 Furthermore, implications of burnout extend beyond the individual, influencing health care organizations. Staff members experiencing emotional exhaustion are more likely to become disengaged, leading to poor staff-patient relationships, reduced patient safety, and poor health care outcomes.15,16 Despite extensive documentation of burnout, a significant lack of awareness of this looming crisis persists.1,15
Recognizing the importance of addressing sonographer burnout, the paucity of data on administrative support, the limited research focused on this issue, and mitigation efforts, this study was motivated by a need to expand understanding of sonographer’s occupational burnout.2,8 -14,15
Knowledge of sonographers’ level of burnout and managing it is vital for both the well-being of these health care professionals and the ability of organizations to maintain patient safety, quality of care, and positive health care outcomes. Understanding the definition of burnout and the contributing stress factors can enable employees to determine their stress levels and use available preventive techniques effectively.1,2,17
Research has promoted awareness and education among all stakeholders and prompts administrators to take the lead in developing strategies to manage and prevent occupational burnout.3,15 The purpose of this cross-sectional, descriptive survey study was to explore the level of occupational burnout among sonographers practicing in the United States and their perception of administrative support and resources for burnout prevention.
Materials and Methods
This study used a quantitative descriptive design with a cross-sectional online survey. A nonprobability, consecutive sampling methodology was employed. Study participants were recruited from the Society of Diagnostic Medical Sonography (SDMS) national professional organization with an accessible population of more than 18 211 active members. Inclusion criteria were sonographers employed in clinical settings who resided in the United States. Students were excluded from participating. The A.T. Still University Institutional Review Board reviewed and approved this study (ATSU-AZ IRB #2021-250).
Dr. Bakker, one of the contributors to the Oldenburg Burnout Inventory (OLBI), granted permission for reuse of the survey instrument. The survey consisted of 34 items grouped into four sections: demographics, work environment, administrative support, and the 16-item OLBI. Demographic questions included age, gender, race/ethnicity, location, number of years practicing sonography, employment status, employment shift hours, and the number of hours worked per day. The OLBI comprises 16 items with subscales of emotional exhaustion and disengagement from work. The OLBI is scored by a 4-point Likert-type scale ranging from (1
The SDMS contacted study participants via email with an invitation letter and a link to the survey. The first page of the survey included a recruitment letter and a participation statement that served as consent for the study. The first three questions asked participants to confirm that they were employed in a clinical setting, residing in the United States, and were not students. If all three criteria were met, participants could progress through the survey. If any requirements were unmet, participants were rerouted to a thank you page and could not complete the survey. The survey was available for 40 days, from the end of February to early April 2022.
Statistical Analysis
The data were extracted from the survey platform Qualtrics, and an item-by-item analysis was conducted using the SPSS Statistics package (IBM corporation v 28). Descriptive statistics (frequencies and valid percentages) were calculated for the nominal variables, Shapiro-Wilk’s normality testing (
Results
A total of 18 211 sonographers from the SDMS were invited to participate. A total of 1393 responses were collected. The inclusion criteria of living in the United States, being employed within a clinical setting and not being a student were not met by 195 respondents. An additional 79 respondents did not adequately complete the survey and were thus excluded from data analysis. The total sample for analysis was 1119 responses, representing a completion rate of 80.3% for those opening the survey.
Demographic characteristics are reported in Table 1. Respondents were predominantly female (89.1%) with the most frequent age range of 56–64 (27.0%) and were employed full-time (78%). The registered diagnostic medical sonographer (RDMS) was the most frequently reported professional credential (85.8%), while the registered vascular specialist (RVS) was the least reported (2.3%). Most respondents had scanning experience over 30 years (29.3%), were employed in hospitals (49.8%), and worked 7 to 11 hours per day (82.5%) on the day shift (90.3%).
The Sonographer Cohort’s Demographics and Characteristics.
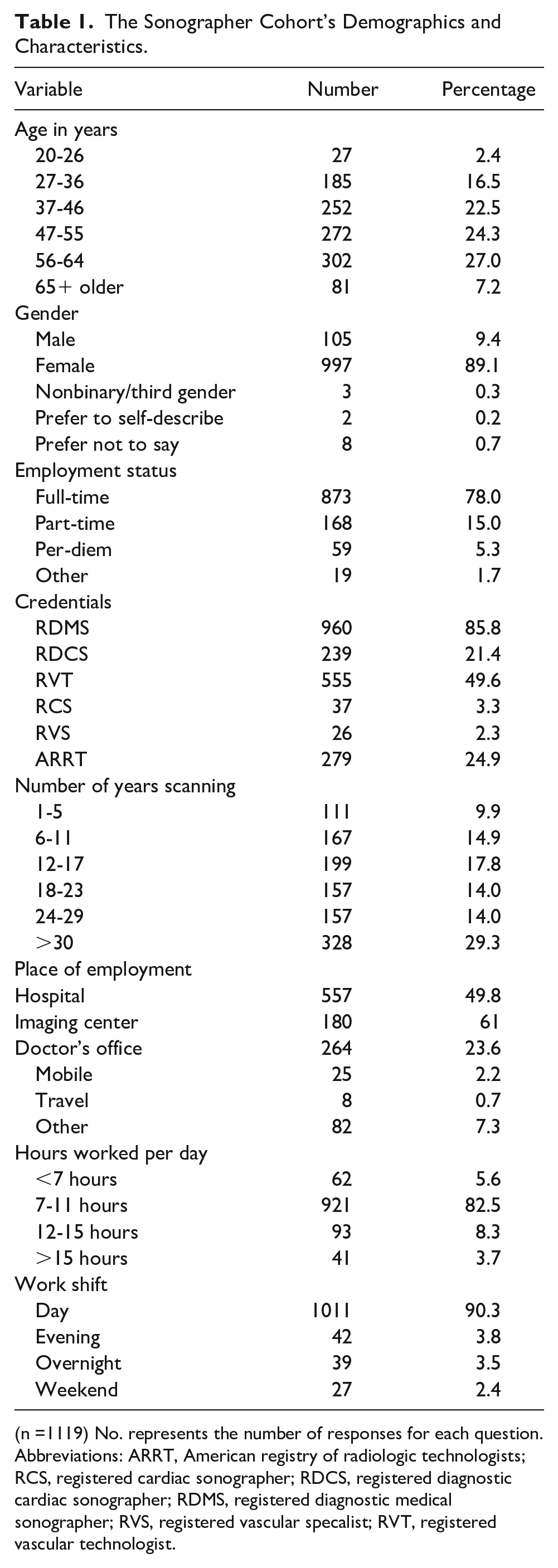
(n =1119) No. represents the number of responses for each question.
Abbreviations: ARRT, American registry of radiologic technologists; RCS, registered cardiac sonographer; RDCS, registered diagnostic cardiac sonographer; RDMS, registered diagnostic medical sonographer; RVS, registered vascular specalist; RVT, registered vascular technologist.
Level of Burnout Among the Sonographer Cohort Practicing in the United States
Participants’ stress levels related to workload and the COVID-19 pandemic are reported in Figure 1. A total of 31% of participants
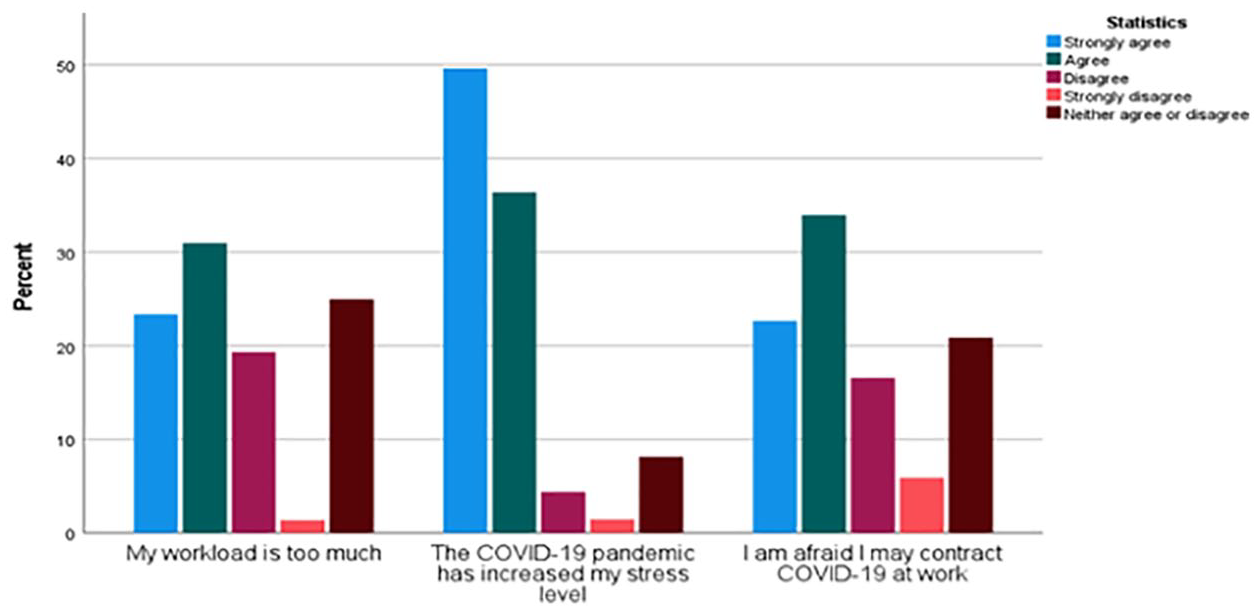
Bar chart of participants’ stress level responses related to COVID-19. This figure demonstrates the participants’ responses to stress levels. Scores are on a 5-point scale with response options from 1 =
The returned thresholds for the total OLBI using the percentiles 25, 50, and 75 were 38, 47, and 48, respectively. As shown in Table 2, the burnout scores were classified as
The Levels of Occupational Burnout as Indicated by the Oldenburg Burnout Inventory (OLBI).
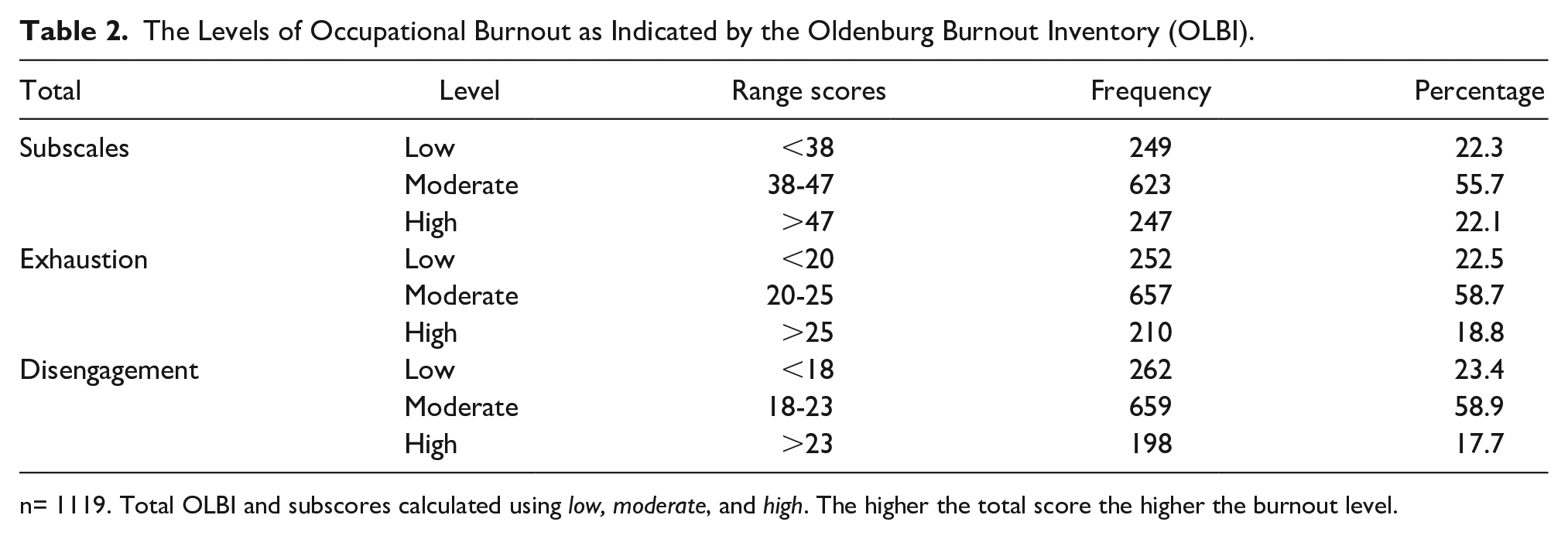
n= 1119. Total OLBI and subscores calculated using
The Descriptive Statistics Which Include Means, Standard Deviations, Median, Minimum to Maximum for the Oldenburg Burnout Inventory (OLBI).
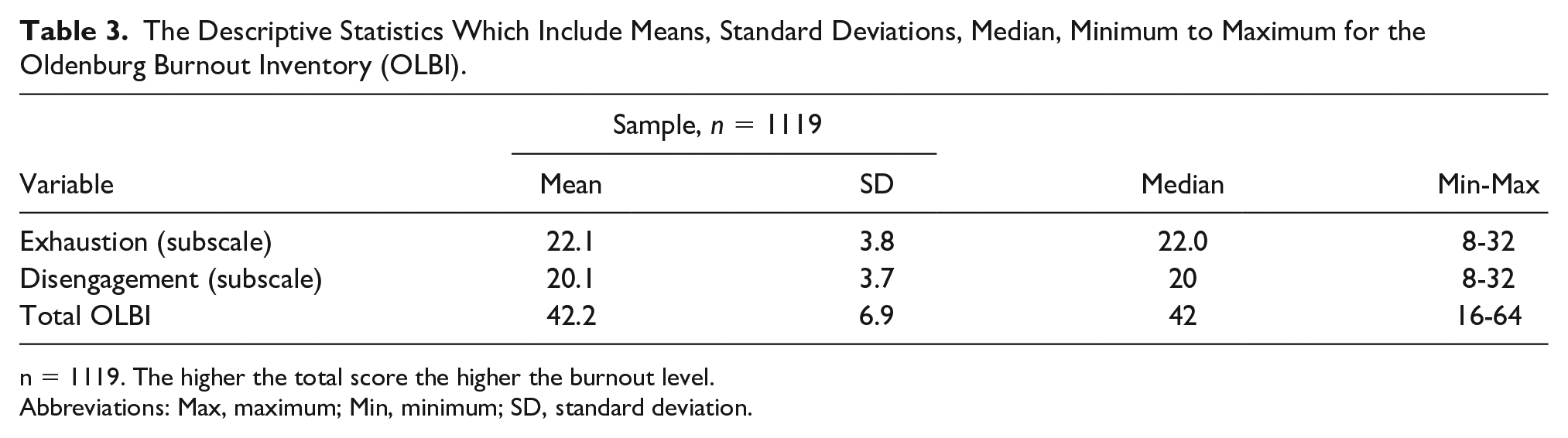
n = 1119. The higher the total score the higher the burnout level.
Abbreviations: Max, maximum; Min, minimum; SD, standard deviation.
Participants’ responses to the OLBI individual questions are demonstrated in Table 4. Although respondents reported moderate burnout in the subscore exhaustion, many participants (62.9%) agreed that they could tolerate the pressures of their job very well, and 73.3% agreed that they could manage the amount of their work very well. The findings were similar for moderate disengagement, in which 61.9% of respondents reported that they always found interesting aspects in their work, and 59.4% found their work to be positive. These were surprising findings in the presence of moderate sonographer burnout for both exhaustion and disengagement.
The Participants’ Response Frequency, Based on the Oldenburg Burnout Inventory (OLBI).
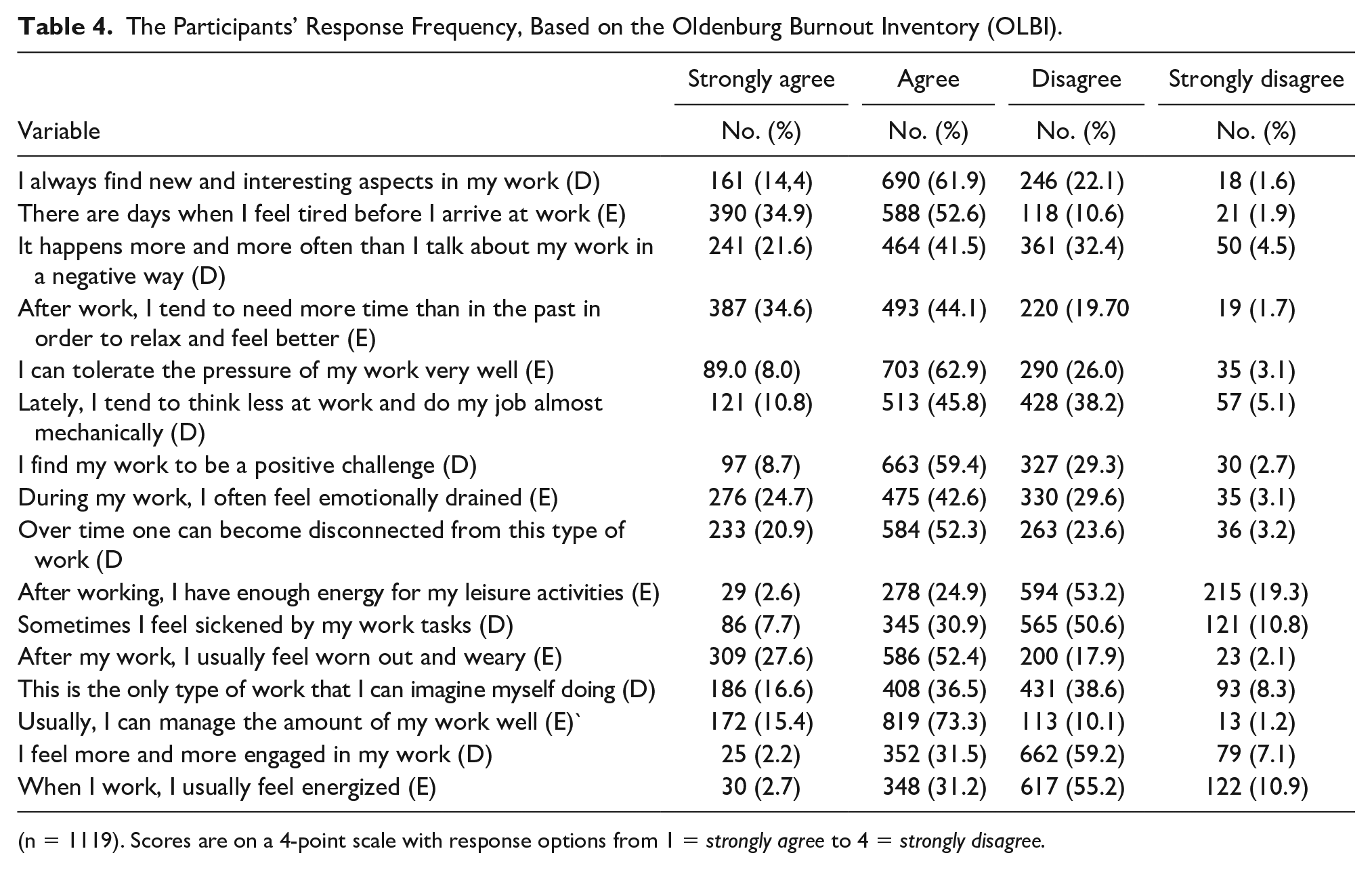
(n = 1119). Scores are on a 4-point scale with response options from 1 =
Administrative Support and Resources
In response to items asking about sonographers’ perception of burnout prevention support and resources provided by the administration, 30.9% of respondents agreed that their employers cared about their well-being, while 36.6% disagreed that their employers provided support. Another 30.7% disagreed that they had access to resources to help them cope (see Figure 2).
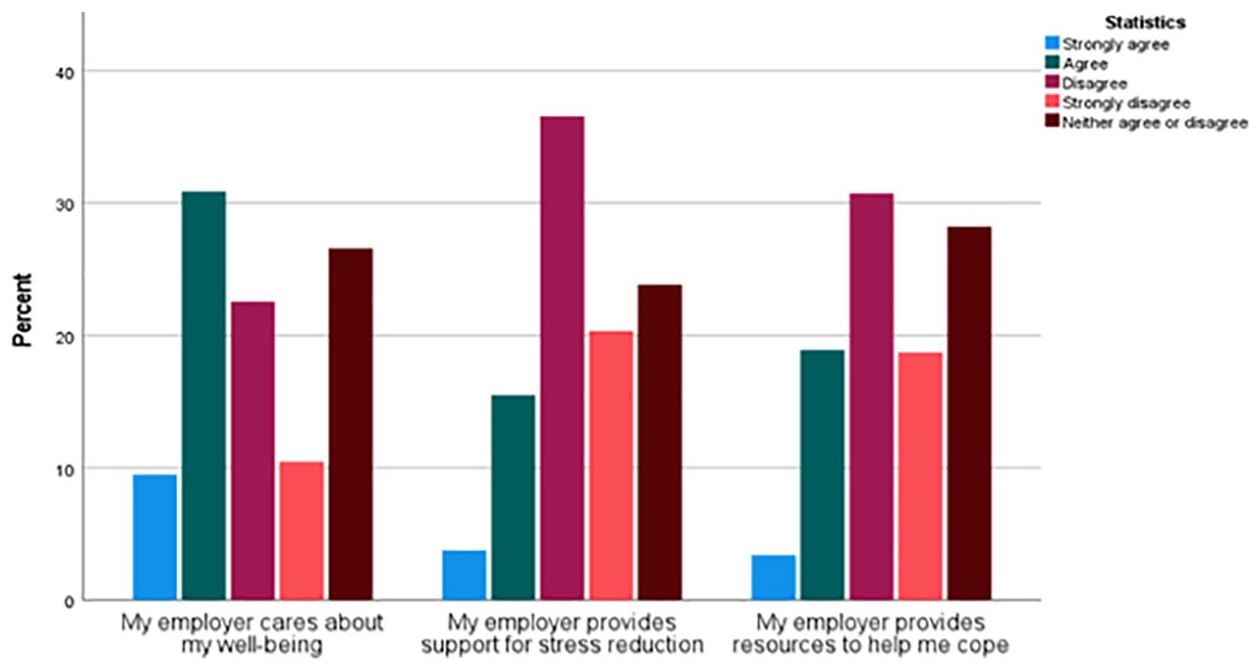
Bar Chart of Participant’s Response to Employer Support and Resources. This figure demonstrates the participants’ responses to employer support and resources provided. Scores are on a 5-point scale with response options from 1 =
Discussion
This study explored the levels of occupational burnout among a cohort of sonographers practicing in the United States and their perceptions of administrative support and resources. Based on the categorization of burnout levels for the standardized OLBI, this study demonstrated moderate levels of burnout in these sonographers for both exhaustion and disengagement. These findings correlated with previous studies reporting moderate to high levels of burnout in sonographers and psychiatric residents.2,8,9,11,19 In comparison to other health care professionals previous studies reported 51% of physicians and 53% of physical therapists experiencing burnout symptoms and 43% of nurses experiencing emotional exhaustion.20,21 While the OLBI uses only two components (exhaustion and disengagement), the MBI uses three components (emotional exhaustion, depersonalization, and personal accomplishment); the results are considered comparable.18,22
In this study, most respondents were female and had worked in the field for over 30 years, suggesting the possibility of burnout being more prevalent in sonographers who have been in the profession longer than those recently hired. 2 However, this study did not test the number of years in the profession as a cause of burnout. Therefore, future research could investigate the relationship between occupational burnout and sonographers who are newer in their career and those who have been practicing longer. Many sonographers work in hospitals, which may contribute to burnout as sonographers in hospitals have heavier workloads, more demanding work schedules, and requirements for on-call duties.2,11,14 Walvoord 2 found that work environment played a significant role in burnout, including perceived environmental uncertainty and lack of supervisor support. Future research should evaluate the relationship between work environment and sonographer burnout.
Although moderate burnout levels existed for the disengagement component, most respondents reported they could tolerate their work well, which contradicted reports from previous studies.8,11 Daugherty 9 reported moderate levels of burnout in sonographers and vascular technologists that caused depersonalization and detachment from their job responsibilities. The cohort of sonographers in this study were still engaged in their duties even when experiencing moderate burnout.
Most of the participants indicated that the COVID-19 pandemic increased stress levels, consistent with the number of sonographers who reported being afraid of contracting COVID-19 on the job. Previous studies reported a prevalence of psychological distress, secondary traumatic stress, and professional burnout in health care workers, leading to adverse outcomes for the organization.15,17,23
Sonographers in this study reported that their administrators did not provide adequate support or resources for burnout prevention, which correlates with previous research.2,5 For example, Cotel et al. 6 indicated that COVID-19 increased the incidence of burnout in health care workers and highlighted the lack of support and resources for burnout. Cotel et al. 6 also reported on interventions organizations can provide to reduce burnout, including those that minimize exhaustion, such as relaxation techniques, knowledge and training for new roles, and cognitive and behavioral therapy. Similarly, Friganovic and Selic 3 documented the importance of administrative and organizational support for burnout prevention and the implications of well-being in the workplace, such as job satisfaction, work overload, and staffing shortage caused by staff leaving their jobs prematurely.
Theoretical and Practical Applications
The main findings of this study demonstrated moderate burnout levels in this large cohort of sonographers practicing in the United States and a lack of or inadequate administrative support and resources. The standardized OLBI and concurrence with previous research findings suggested the external validity of this study’s results.22,24 This study contributes to developing knowledge related to burnout in sonographers, the implications of the COVID-19 pandemic, and administrators’ role in providing support and resources for burnout prevention, such as physical and psychological support. Awareness of predictors of burnout can help sonographers with self-efficacy and administrators with mitigation efforts. Absenteeism, personnel turnover, cynicism, and staffing shortages because health care workers leave their profession prematurely are effects of burnout reported in previous studies.3,15 High personnel turnover and staffing shortages may harm the quality of care and patient outcomes. Organizational policies should be reviewed to ascertain adequate support and resources to mitigate the symptoms of occupational burnout and its effects.
Limitations
There are several limitations associated with this study. The major limitation is the research design, which is considered pre-experimental and has threats to internal and external validity. Given the purposive sample of participants, these results cannot be generalized to the greater population. This study does build evidence on the level of occupational burnout that may exist among sonographers, in the United States. This postpandemic evidence of burnout adds to the body of previous literature and the paucity of data on sonographer burnout in the United States. Since only SDMS members were surveyed, these data only reflects the attitudes of perceptions of those members. There may have been selection bias because sonographers experiencing burnout at the time of the survey may have responded more frequently, inflating the incidence of burnout. This problem can be seen with surveys, but it should not diminish in comparison with other studies. In retrospect, there could have been more items for the COVID-19 or administrative support and resources sections to delve deeper into those issues to gather more data for better understanding. An item about the number of studies per sonographer would help to determine workload, which has been reported as a predictor of occupational burnout in the United States. 6
Conclusion
This study explored the levels of occupational burnout in a large cohort of sonographers and their experience with administrative support and resources for burnout prevention. Evidence exists of moderate burnout among sonographers surveyed, which is likely to increase without adequate administrative support. Administrators and organizations should recognize and acknowledge occupational burnout and the causes of stressors among sonographers so they can provide support and resources to mitigate burnout effects.15,16 Future research is needed to investigate prevention methods that will enable administrators to provide the appropriate support and resources to improve job satisfaction and reduce the number of sonographers leaving their profession prematurely.8,13,14 Managing stressors will enable organizations to retain staff, continue providing quality patient care, and maintain patient outcomes.
Footnotes
Acknowledgements
The authors would like to thank Dr. Arnold Bakker for his permission to use the OLBI survey and the Society of Diagnostic Medical Sonography for distributing the survey to its members.
Ethics Approval
The A.T. Still University Institutional Review Board reviewed and approved this study (ATSU-AZ IRB #2021-250).
Informed Consent
Informed consent was not sought for this study because all case data were de-identified and/or aggregated and followed ethics committee or IRB guidelines (also referred to as the Honest Broker System).
Animal Welfare
Guidelines for humane animal treatment did not apply to this study because no animals were used in the study.
Trial Registration
Not applicable.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Key Takeaways
There is evidence of moderate burnout among sonographers practicing in the United States. There is a lack of or inadequate administrative support and resources. Administrators and organizations must recognize the causes of stressors among sonographers so they can provide the appropriate support and resources. Managing stressors will enable organizations to retain staff, continue providing quality patient care, and maintain patient outcomes.
