Abstract
Objective:
The purpose of this literature search was to review the benefits of high-intensity focused ultrasound (HIFU) and its application for different pathologies.
Methods:
This review summarizes the implementation of HIFU for different pathologic conditions. An National Center for Biotechnology Information, PubMed, MEDLINE, Medscape, and Google Scholar database search (1992–2016) was done with the following keywords: high-intensity focused ultrasound; uses of HIFU; and applications of HIFU in the liver, bones, uterine fibroids, prostate, breast, thyroid, pancreas, kidneys, brain, urinary bladder, and so on. Tables and graphs were created for all the variables included in the study, and descriptive statistics were applied.
Results:
In total, 110 records were identified, through database search. In addition, 20 articles were identified through other sources. Screening of the articles was performed, and 20 were removed due to duplication; further screening was performed for 110 articles, and 30 records were further excluded. Full-text articles were assessed for eligibility and 30 were retained. Full-text articles were excluded (N = 36) on the basis that research was performed on animals, and this review article was performed solely for human application. There were 42 qualitative syntheses that researches added to the review. In addition, 42 quantitative synthesis (meta-analysis) were added to the review.
Conclusion:
The conclusion of this narrative review indicates that HIFU is noninvasive, nonharmful, and effective in treating diseases and tumors of the brain, breast, bone, hepatic, renal, pancreas, and prostate; uterine fibroids; and many other solid tumors. Recent technological development suggests that HIFU is likely to play a significant role in future surgical practices. Further research works should be conducted on a large sample size to obtain more accurate results in the application of HIFU.
Keywords
High-intensity focused ultrasound (HIFU) is a very appealing modality used as a minimally invasive procedure. HIFU is based on the well-established principles and is used as an ablative therapy for benign and malignant tumors, with some side effects. Many research studies have been conducted on HIFU and it has been practiced by radiologists for many years, but was introduced by Wood and Loomis in 1920. 1 The first clinical application of HIFU was for the treatment of Parkinson’s disease, which is a focal neurologic disorder, and it was performed by Fry et al in 1950.2,3 The problem that these pioneering scientists faced during their era was to target the exact location of the lesion for ablation due to lack of 3D sonography. With the help of 3D and 4D sonography, it is easier to approach, target, and monitor the tumor, for the purpose of ablation. Due to the limited availability of state-of-the-art medical facilities, many patients experienced side effects that were reported in the literature. 4
HIFU works on the same principle as diagnostic sonography and relies on pulse-echo instrumentation. Based on that principle, pulses are sent into the body and the transducer receives reflections. But the energy levels, in HIFU, are several times greater in magnitude, compared to diagnostic ultrasound levels. 5 If the intensity of the beam is increased and focused, the temperature at the location can rapidly rise above 80°C, which, even in very short exposures, can lead to effective cell death.6,7 There are two mechanisms by which bioeffects can occur with the use of ultrasound, that is, heat and cavitation. 7 The sound waves have mechanical energy, which is converted into heat as the waves propagate through the soft tissues. Normally, ultrasound waves are spread across the soft tissues that are being insonated. If the heating rate is rapid, compared to the cooling rate, it will result in a rise in local temperature. The HIFU transducers transfer energy rapidly into a specific area, which results in a rapid rise in the temperature and can reach 56°C for 1 second. 8 This increase in local temperature can result in cell death due to the coagulative necrosis process. 8
In HIFU, heating and its factors, including thermal properties, of targeted tissues and their acoustic properties are the predominant mode of ablation. Cavitation is another mechanism, which can cause bioeffects. In the process of cavitation, mechanical vibration causes the generation of microbubbles within the cell cytoplasm. These air-filled microbubbles, in the cytoplasm, are the result of cavitation. Cavitation can be classified into two types: stable and transient. Stable cavitation is not considered to be harmful, but transient cavitation creates macrobubbles that burst and release thermal energy in excess of 2000–5000 K into the surrounding tissues. 9 The basic HIFU principles that relate to underlying tissue damage are coagulative thermal necrosis, due to absorption, during tissue transmission (aka thermal effect) and ultrasound-induced cavitation. 10
HIFU is used as the ablative therapy for many diseases, such as liver tumors, kidney tumors, uterine fibroids, tumors of bones, prostate carcinomas, pancreatic cancer, and brain tumors, in humans and animals. HIFU uses a transducer, similar to that used in diagnostic imaging, but with much higher energy. The transducer focuses sound waves and generates heat, at a single point, within the body, which destroys the target tissue. The tissue can get as hot as 150°F in just 20 seconds. There are some merits and pitfalls to this treatment, due to the many side effects seen before and after the procedure in the patients. The complications can include local pain; mild discomfort; fever; first-, second-, and third-degree skin burn; swelling and hardness in the ablated area; hyperpigmentation; ecchymosis; erythema; hypopigmentation; dimpling; numbness; hyperpigmentation; and edema.11–16 Clinical manifestations such as biliary obstruction, symptomatic pleural effusion, pneumothorax, and fistula formation between an abdominal wall abscess and the ablated hepatic tumor have been noted.11–16 There have also been reports of urethral stricture, postoperative dysuria or urinary tract infection, urinary retention, bladder outflow obstruction, transient incontinence, bladder neck stenosis, subcutaneous sclerosis, pancreatic pseudocyst, abdominal firmness, rectourethral fistula, bowel perforation, and portal vein thrombosis, which provided major or minor complications for patients.11–16 During some HIFU procedures, mild sedation and pain medication are given to minimize side effects.
Further applications of HIFU are being investigated, as well as researched for use in humans because most reported studies were performed on animals. HIFU is a very versatile option in the treatment of many diseases. During the last few years, there has been a great deal of work in advancing our knowledge of HIFU. There is an ever-increasing body of evidence to support the use of HIFU as a minimally invasive tool. The work to date has shown that as a generic technique it can be regarded as safe and feasible for the treatment of a wide range of problems. HIFU offers a very favorable safety profile. The most important notable risk is that of a skin burn. In order to minimize this risk, cooling devices and procedures are used to protect the skin during the treatment procedure. The purpose of this literature review was to demonstrate the importance of HIFU, across a variety of diseases and clinical applications.
Methods
Two reviewers (I.M. and R.B.) conducted a search with Google Scholar, PubMed, NCBI, MEDLINE, and Medscape databases, from 1992 up to 2016. The key search terms used were high-intensity focused ultrasound; uses of HIFU; and applications of HIFU in the liver, bones, uterine fibroids, prostate, breast, thyroid, pancreas, kidneys, brain, urinary bladder, and so on. Two reviewers (I.M. and R.B.) independently screened the titles and abstracts of the relevant articles and full-text downloads to determine whether inclusion or exclusion criteria were met. Any disagreement between the reviewers was resolved by means of a consensus. Studies were eligible if they included information about HIFU and clinical applications to humans. The HIFU research, done with animals, was excluded from this review process. The eligible studies were first categorized and then analysis of the data was performed according to specific pathologic conditions.
This literature review retrieved studies’ sample size, HIFU application, study design, duration of the procedure, mean age of the patients, success rate of the treatment, and complications of the procedure. From all the data retrieved, descriptive statistics were gathered for analysis. A table was created, with predefined subgroups, for all variables included in the study (Table 1). The variables included were as follows: year of the study, the first author of the research article, country, application of HIFU, sample size, study design, duration of the procedure and study, mean age of the patients in years, the success of treatment, and complications of the study. The number of patients who recovered and those who did not recover were labeled as either successful or unsuccessful.
Variables of the Study.
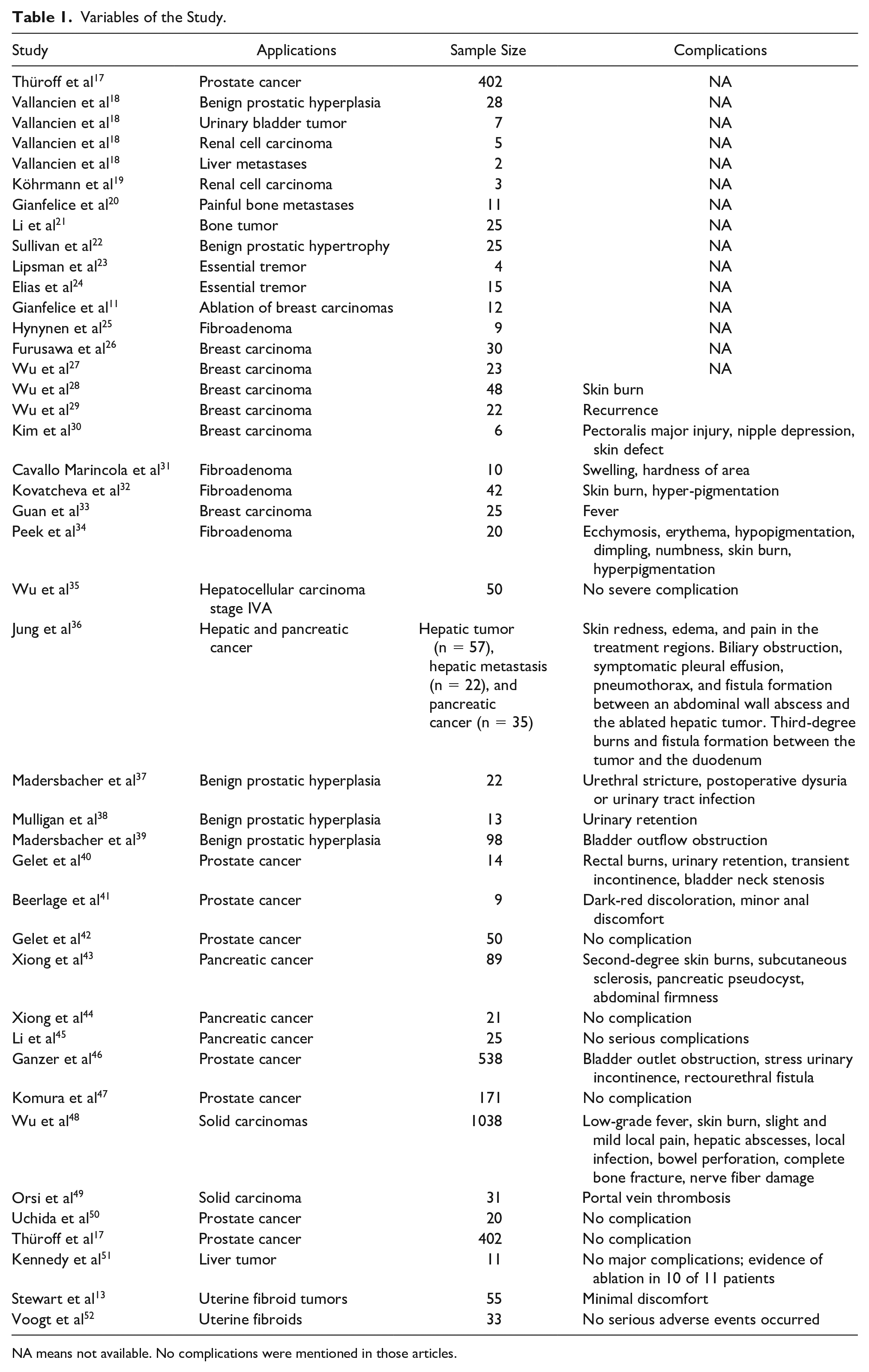
NA means not available. No complications were mentioned in those articles.
The studies were included if complete information was provided for all the variables in a human study. The studies were excluded if incomplete information was given about the variables of the study.
Results
In total, 110 records were identified through the database search. In addition, 20 records were identified through other sources. Then, screening was performed, and 20 records were removed due to duplication. A further screening was performed for 110 articles, and 30 records were excluded due to insufficient information. Thirty full-text articles were assessed for eligibility. There were 36 full-text articles excluded due to research performed on animals, and this study was determined as a review of only human studies. Forty-two studies were included that had a qualitative synthesis. We also included 42 quantitative syntheses (meta-analysis). A flow chart is provided that summarizes the records reviewed (see Figure 1).
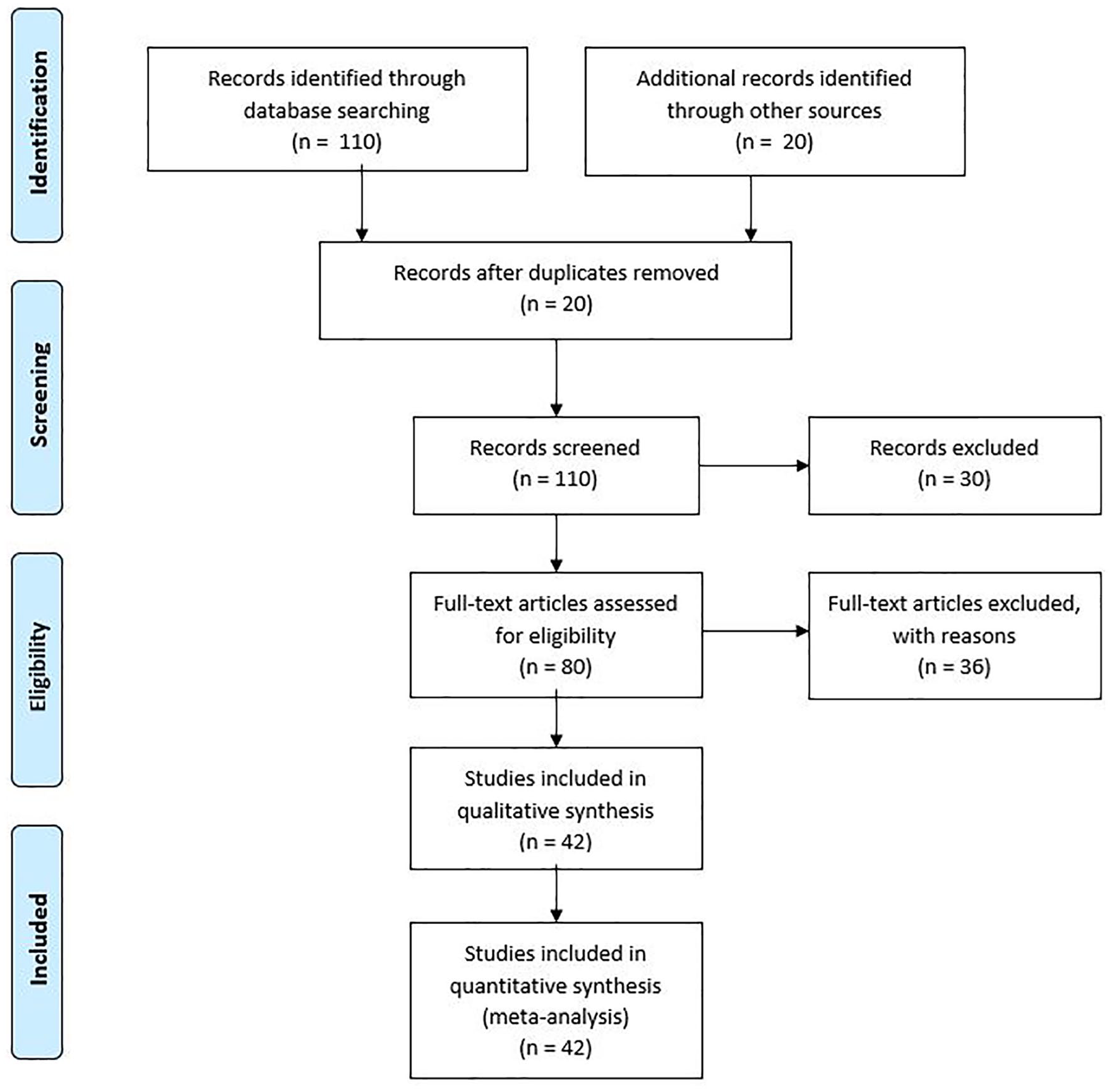
Flow diagram of literature review.
Based on this review, most of the research, performed on HIFU, was conducted in China, and that was based on nine articles included from the literature search. The remaining articles originated from France (N = 8); Canada (N = 4); Germany, Japan, Korea, the Netherlands, and the United States (N = 3); Austria, Italy, and the United Kingdom (N = 2); and Bulgaria, California, Great Britain, Ireland, and Switzerland (N = 1). Most of the research was conducted on breast and prostate cancer. HIFU was used as a clinical application for a variety of diseases.
This literature review was productive in securing a variety of HIFU treatments for a variety of diseases and conditions. The success rates were variable from a high of 100% to a low of 50% (see Table 2). These articles and the information provided represent the most current use and success for utilizing HIFU across selected pathologic conditions.
Different Applications of High-Intensity Focused Ultrasound.
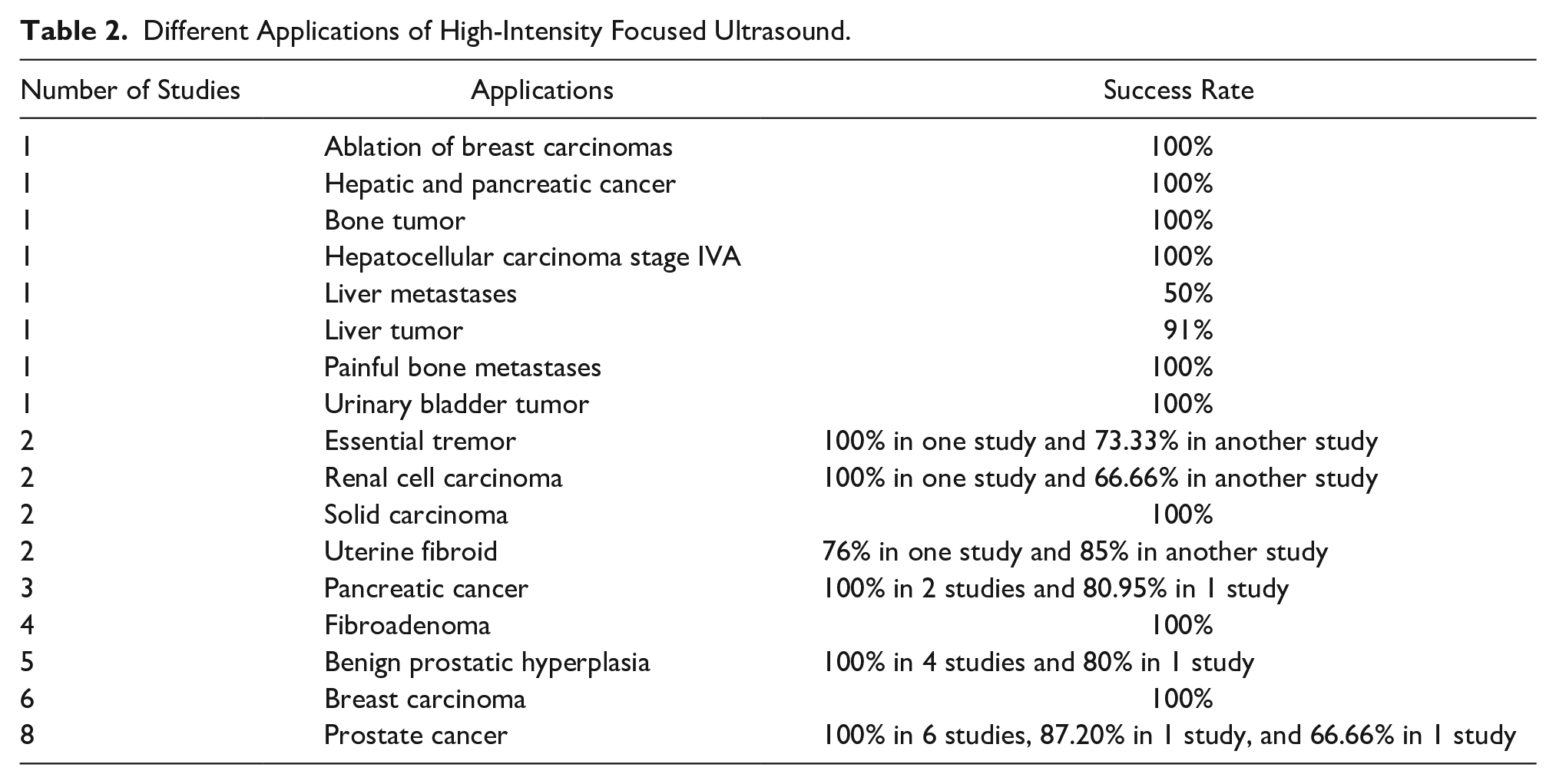
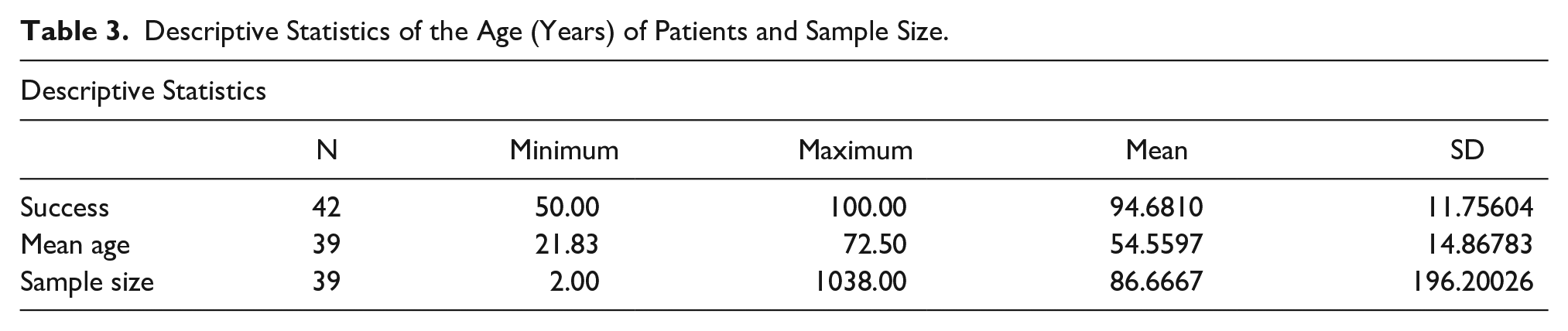
Various patient complications were also noted post-HIFU, and these included skin erythema, recurrence of the disease, pectoralis, portal vein thrombosis, evidence of ablation in 10 of 11 patients, and minimal discomfort. The mean age of the patients in which the HIFU was applied was 54.5 years. The mean success rate of the treatment in various diseases was 94.68% ± 11.75604 SD with a range of 50%–100% (see Table 3).
Descriptive Statistics of the Age (Years) of Patients and Sample Size.
Discussion
HIFU is used as an ablative therapy for the treatment of many diseases, and for this reason, it is sometimes referred to as focused ultrasound surgery (FUS). It can be performed with sonographic guidance and magnetic resonance imaging (MRI) guidance. HIFU is performed with the help of a variety of devices, and most commonly the devices are extracorporeal and transrectal. The extracorporeal devices are comparatively larger than those that are transrectal and are used in the treatment of abdominal tumors due to their longer ultrasonic focal length and MRI guidance. The HIFU device has a 12-cm diameter, single-element, piezo-ceramic crystal, fronted by an acoustic lens, of varying focal lengths. It is driven at a range of 0.8–1.6 MHz frequency. 53 While transrectal devices are used in the treatment of prostate cancer, these are smaller devices that have shorter focal lengths (3–4 cm) and operated at higher frequencies than extracorporeal devices. 54 There are other devices as well, including prototypes, endoscopic, laparoscopic, and small handheld probes. In the past, HIFU has been used in the treatment of a variety of diseases. But in the modern era, the main application of HIFU is in the treatment of solid abdominal tumors, breast, bone, brain, soft tissue tumors, and so on. Research into the assessment of malignant bone tumors with HIFU and its safety and effectiveness was conducted with 25 individuals who were followed before and after the procedure. 21 According to these results, 21 patients were completely relieved of pain, and 24 had significant relief post-HIFU. Of the patients with primary bone tumor, six patients had a complete response, five had a partial response, one had a moderate response, and one suffered from a progressive disease; the overall response rate was 75.0%. It was concluded from this study that HIFU can safely ablate the bone tumor and also relieve pain and can be effectively applied in the treatment of primary bone tumors. 21
Sullivan et al conducted research to evaluate the effectiveness and safety of HIFU for benign prostatic hypertrophy and enrolled 25 patients with a mean age of 67 years. They were all operated with the Sonablate HIFU devices. The symptoms were recorded before and after the treatment. According to the results, five patients were withdrawn from the study due to the enlarged gland and failure rate. The rest of the 20 patients show a positive result, and no complication was seen after the treatment. It is concluded that HIFU is safe and effective, and no major complication was seen with it in the treatment of benign prostatic hypertrophy. 22 In 2006, a study was conducted on the pathologic effects of HIFU in the treatment of patients with breast cancer, and 23 patients were enrolled. All these cases were biopsy-proven and mastectomies were performed on all the patients after treatment with HIFU. Coagulation necrosis was seen, with the help of microscopy, in the targeted tissue after the exposure. It was concluded that heat fixation was observed at the ablated tumor site, due to thermal effects caused by HIFU. 27 No severe complication was observed after the application of transarterial chemoembolization (TACE) and HIFU. In the follow-up images, a reduction in blood supply was noted in the targeted lesion, and the absence of lesion was also observed after the application of HIFU. 35
Research published on HIFU mostly includes clinical, experimental studies or case reports. Many of the studies were multicentric that included different countries and follow-up of their patients. After an extensive literature review, there was only limited evidence in the use of HIFU for one or more clinical applications. According to this extensive literature review, it appears that HIFU is safe, effective, and can be applied for the treatment of many diseases, without any major complications. It would appear that most patient complications were reported in the older studies, when HIFU was newly introduced. It also seems, based on this review, that further HIFU development, in technology, reduced patient complications.
Conclusion
This recent literature review indicates that HIFU is noninvasive, safe, and effective in the treatment of many diseases and tumors of the brain, breast, bone, liver, kidney, pancreas, and prostate; uterine fibroids; and many other solid tumors. Recent technological developments suggest that HIFU is likely to play a significant role in the future of surgical practices. Further research should be conducted with larger sample sizes to provide more accurate results for the application of HIFU.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval was taken prior to the research from the ethical committee of The University of Lahore.
Informed Consent
Informed consent was not sought for the present study because it is a review article.
Animal Welfare
Guidelines for humane animal treatment did not apply to the present study because it is a review article.
Trial Registration
Not applicable.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
