Abstract
Background and Aims:
(a) To evaluate insulin resistance (IR) in individuals with Type 2 Diabetes Mellitus (T2DM) and periodontal disease (PD) in a local South Indian population. (b) To study the correlation between surrogate markers of IR—namely HOMA-IR (using insulin), HOMA-IR (using C-peptide), and Triglyceride-Glucose Index (TGI).
Materials and Methods:
This is a cross-sectional study conducted at Indra Diabetes Centre, Tuticorin, Tamil Nadu. A total of 145 T2DM patients aged 30–85 years were screened for PD and enrolled. A control group of 145 age-matched, non-diabetic genetic relatives of the T2DM group was also screened and recruited similarly. PD severity was classified into four stages by the dentist, as per the Periodontitis Consensus Report 2017. The demographic details, namely age, gender, as well as BMI and fasting blood samples for Glucose, Insulin, C-peptide, Triglycerides, and HbA1c, were collected from T2DM (D) and non-diabetic control (ND) participants enrolled on the study.
IR was estimated using three methods: HOMA-IR (insulin-based, HOMA-IRi), HOMA-IR (C-peptide-based, HOMA-IRc), and TGI. Statistical analysis was performed using JASP software. IR levels were compared between the D and ND groups. Subgroup analyses by gender and PD stage were also performed. Then, correlation analyses of the IR of HOMA IRc and TGI with HOMA IRi were conducted.
Results:
Using a regional HOMA-IRi cut-off of 1.23, IR was observed in both diabetic and non-diabetic groups, with significantly higher values in the diabetic group. No significant differences in IR were found between genders or across the various stages of PD in either group. HOMA-IRc and TGI showed a strong positive correlation with the standard HOMA-IRi method.
Conclusions:
(a) IR was observed in both diabetic and non-diabetic groups with PD; however, it was significantly higher in the diabetic group. There was no significant difference in IR between genders or among the four stages of PD in either group. PD appears to aggravate IR in diabetic individuals and may contribute to the development of IR in non-diabetics, potentially increasing their risk of developing diabetes. (b) Since HOMA-IR using C-peptide correlates well with the standard insulin-based HOMA-IR, it may be preferred for research or clinical use in laboratories where maintaining an ideal cold chain is challenging, which is an important consideration in the Indian setting. (c) As lipid profiles are routinely performed in primary care for all diabetic patients, the TGI can be easily calculated and included in laboratory reports. It is simple, cost-effective, and widely accessible, and may assist clinicians in identifying IR and selecting appropriate therapeutic strategies.
Keywords
Background
Insulin resistance (IR) is associated with Type 2 Diabetes Mellitus (T2DM). 1 Inflammatory response may be caused by pathogenic oral microbes and mediated by inflammatory cytokines in humans. Periodontal disease (PD) and T2 DM have a mutual causal relationship. 2 Diabetes may be a risk factor for PD, and PD may aggravate hyperglycaemia through the mechanism of IR. 3 It is known that PD causes an inflammatory response and IR in non-diabetic individuals, thereby PD may be a risk factor for diabetes. 4 Based on this hypothesis, we wanted to study IR in both T2 DM and non- diabetics with PD of a similar age group who were genetically related in southern Tamil Nadu. HOMA IR index is the standard surrogate marker of IR. But there are other surrogate fasting indices, such as HOMA IRc and TGI, having advantages over HOMA IRi for practical reasons. HOMA IRc overcomes the challenge of cold chain maintenance of samples from the point of collection to the laboratory and has a long half-life with good stability. TGI offers additional advantages like affordability, accessibility and cost-effectiveness, especially in a resource-limited country like India. So, we wanted to compare these fasting indices as well while testing IR.
Aims
To evaluate IR in individuals with T2DM and PD in a local South Indian population.
To study the correlation between surrogate markers of IR—namely HOMA-IR (using insulin), HOMA-IR (using C-peptide), and Triglyceride-Glucose Index (TGI).
Materials and Methods
It is a cross-sectional study done between 2020 and 2023 at Indra Diabetes Centre, Tuticorin, Tamil Nadu. We screened for PD in Type 2 Diabetics attending the centre between the age groups of 30 and 85 years. Dentists screened for PD and categorised them into four stages depending upon the severity as recommended by the Periodontitis Consensus Report 2017 (Table 1).
PD - Stages by Periodontitis Consensus Report 2017.

Similarly, we also screened for PD among non-diabetics who were first or second-degree relatives of the diabetic patients of the D group.
Of those screened, 145 in the diabetes (D) and non- diabetes (ND) groups were recruited for the study after their consent. They were matched for age and gender.
Inclusion criteria (D):
T2DM with onset of diabetes of more than 1 year and less than 5 years.
Exclusion criteria (D):
BMI less than 23 or more than 30 to exclude specific phenotypic clusters of T2D, insulin therapy, acanthosis nigricans, patients with micro or macro vascular complications, fasting blood sugar more than 150 mg/dl, smokers, Immune deficiency conditions like HIV, malignancies, lymphoproliferative disorders, steroid or immunosuppressive therapy, and bacterial or viral infections.
Inclusion criteria (ND):
Healthy volunteers, first or second-degree relatives of diabetic patients enrolled in the D group.
Exclusion criteria (ND):
Type 2 Diabetes, hypertension, BMI less than 23 or more than 30, acanthosis nigricans, Immune deficiency states like HIV, malignancies, lymphoproliferative disorders, steroid or immune suppressive therapy, bacterial or viral infections.
The study was approved by the ethics committee of Thoothukudi Government Medical College, Tamil Nadu. Patients enrolled on the study were requested to come in a fasting state. History and physical examination, including BMI and blood pressure, were done. Metformin and Pioglitazone therapy were stopped in the D group 1 day prior to blood sampling. Blood samples for Glucose, Triglycerides, Insulin, C-peptide, and HbA1c in the fasting state were collected.
The blood glucose was done using the glucose peroxidase method. Both glucose and triglycerides were done using a fully automated Erba analyser. Insulin and C-peptide assays were done by chemiluminescent immunoassay (CLIA) using TOSOH. HbA1c was done with the high-pressure liquid chromatography method using BIORAD D10. HOMA IR was done by calculation method [HOMA IR = (Fasting Blood Glucose in mmol/L × Fasting insulin in (mIU/ml)/22.5], HOMA IR using C peptide was done using the formula [HOMA IRc = (Fasting blood sugar in mmol/L × Fasting C peptide (mIU/ml)/22.5], TGI was calculated using the formula [TGI = Ln (Fasting TGL (mg/dl) × Fasting glucose (mg/dl)/2].
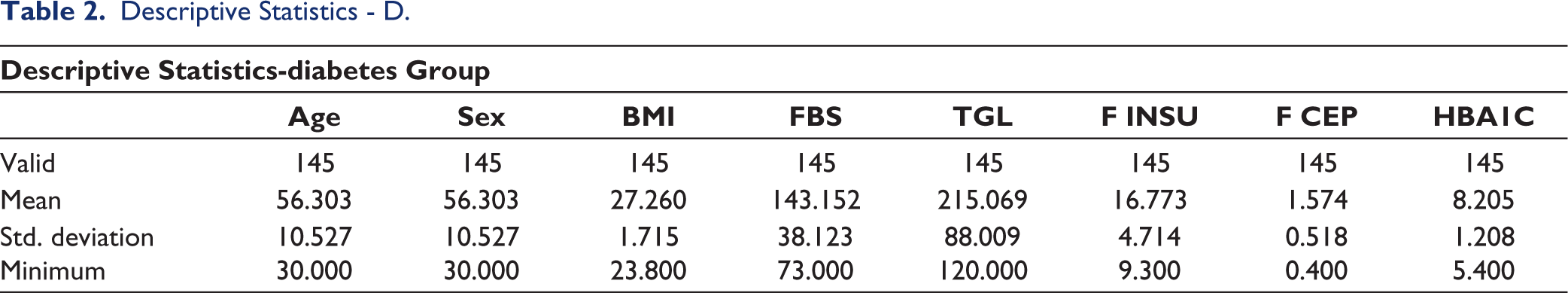
Descriptive Statistics - D.
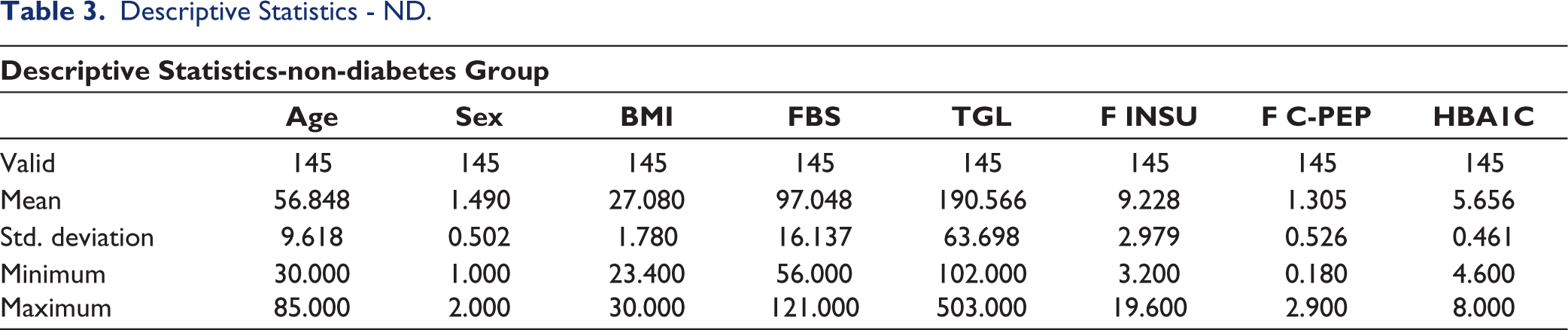
Descriptive Statistics - ND.
Statistical Workup
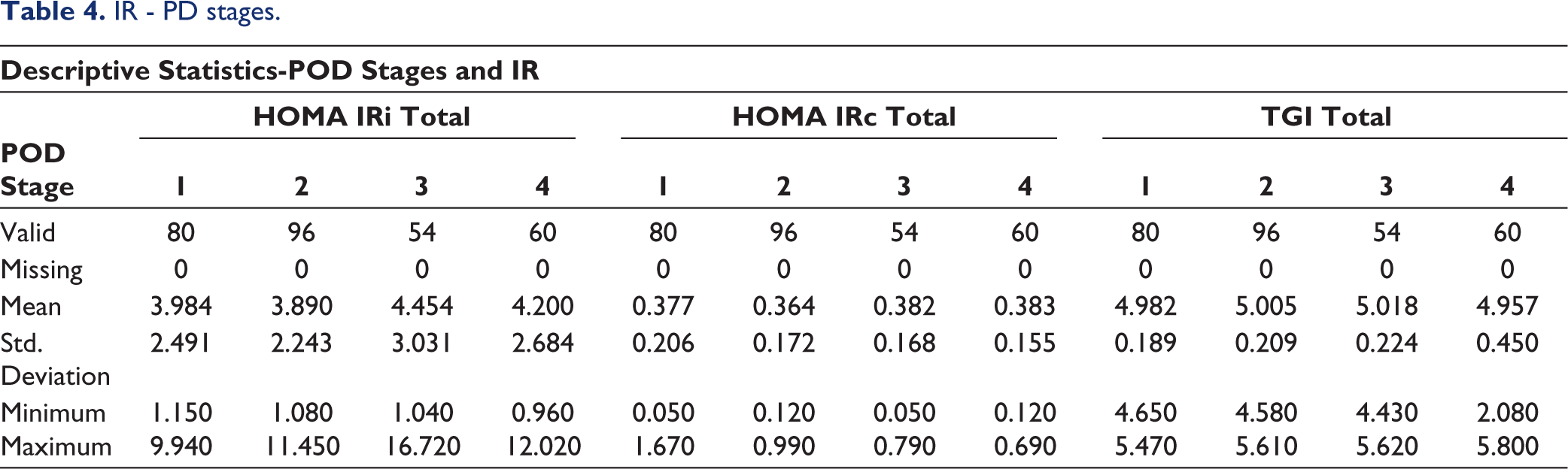
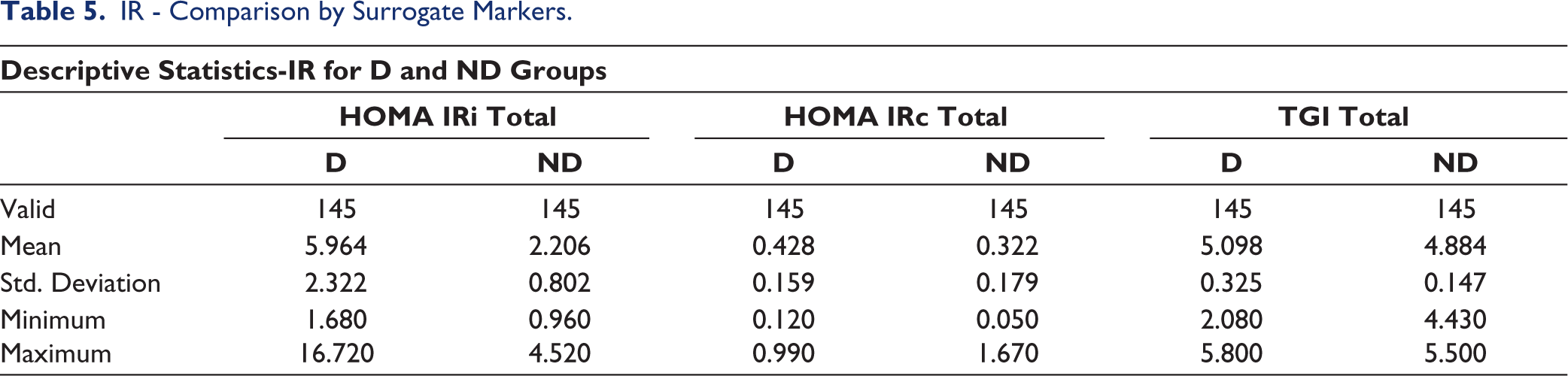
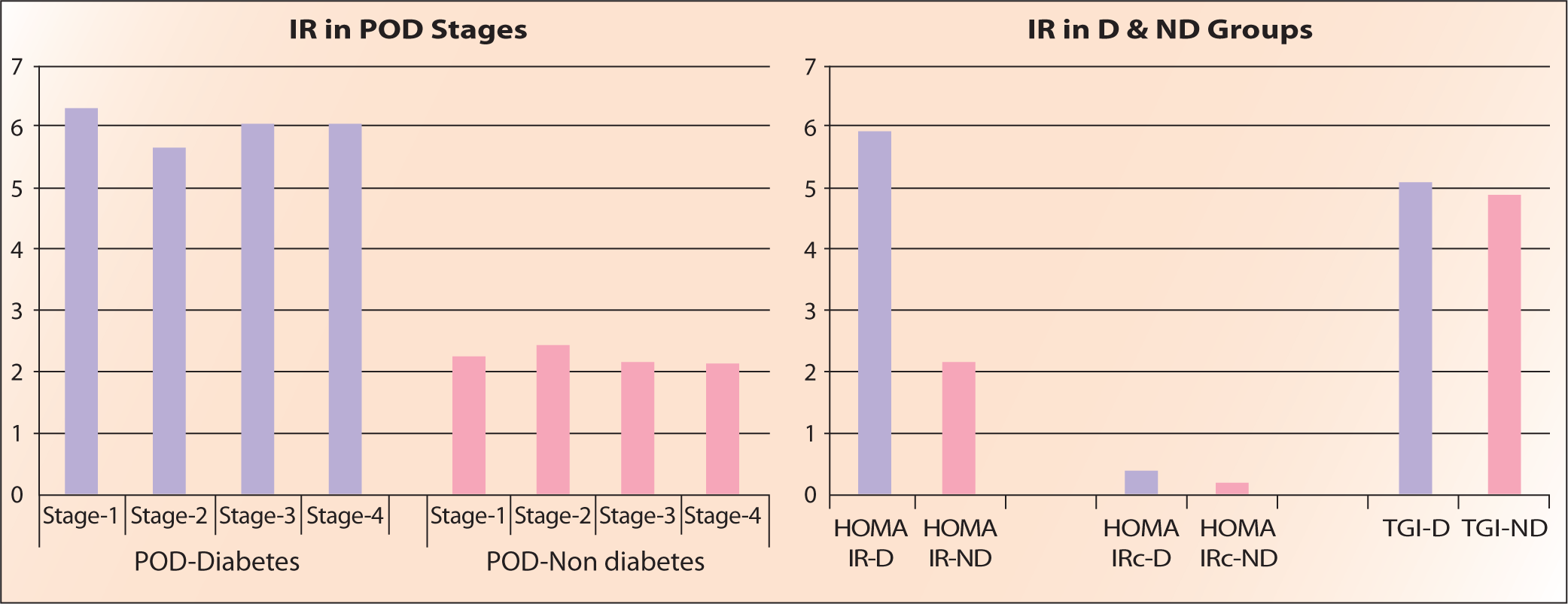
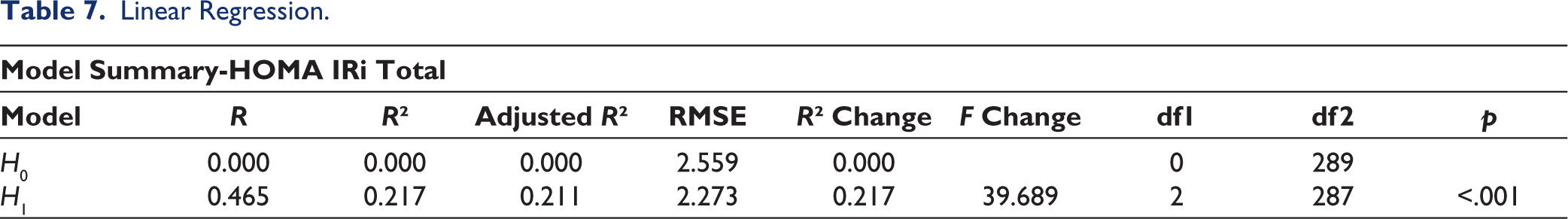
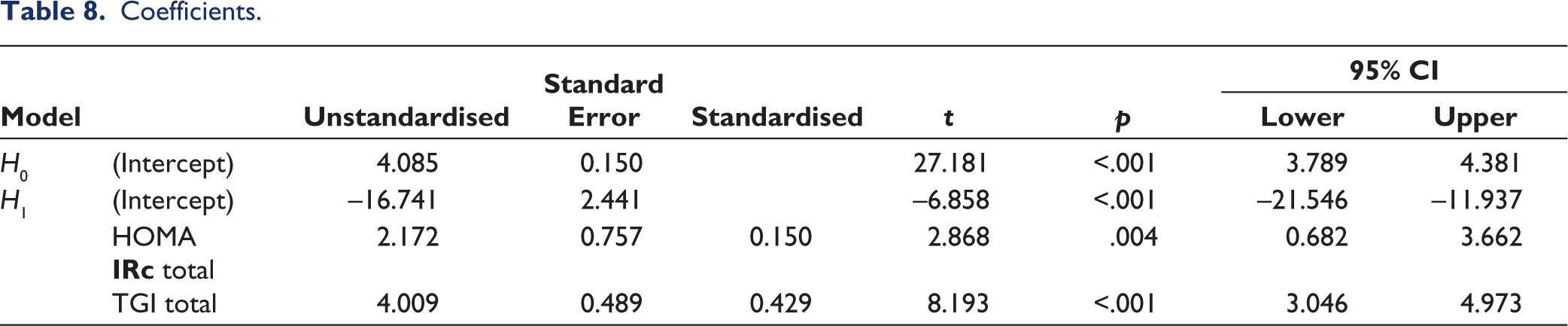
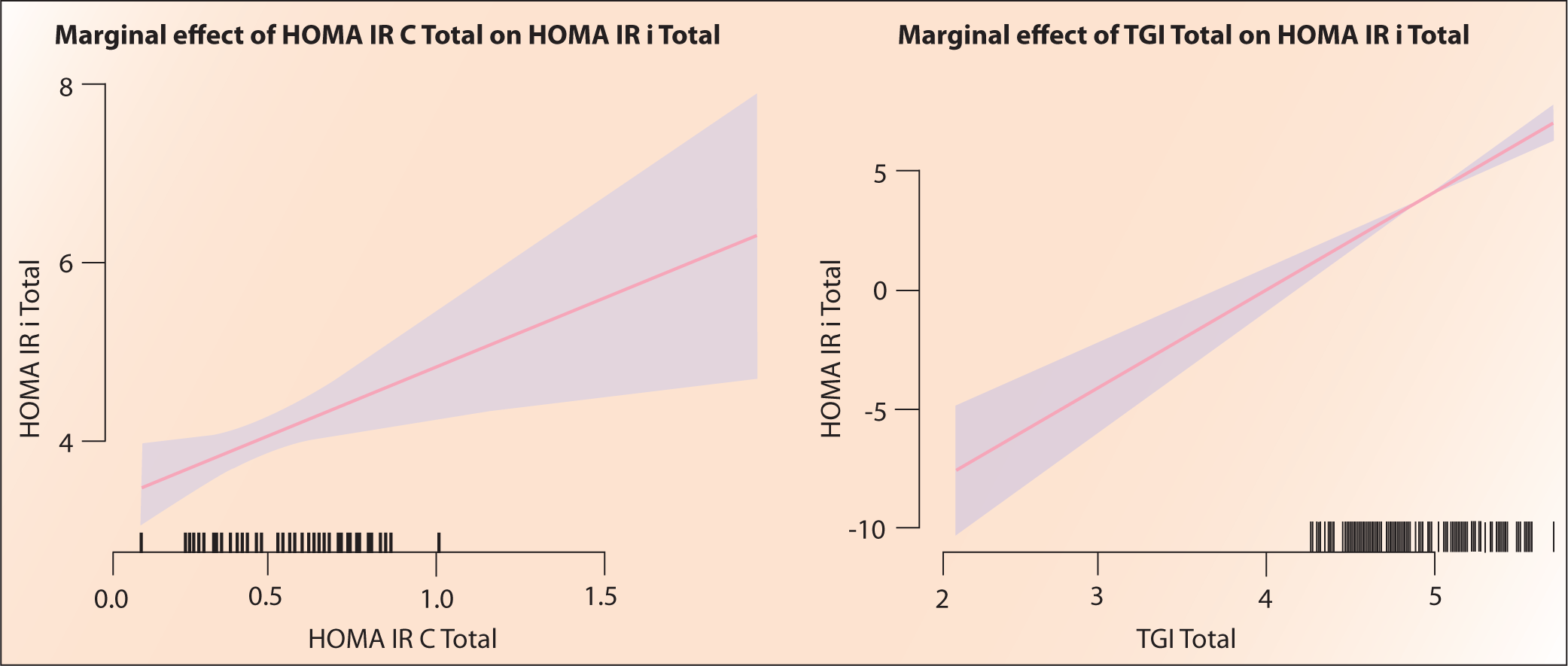
The sample size was calculated using the positive predictive value of the biomarker. The statistical analysis was performed using JASP software. The Shapiro-Wilk test was done to assess the normality of the data. Descriptive statistics were performed for both D and ND groups (Tables 2 and 3). Comparison of HOMA IRi, HOMA IRc and TGI of all stages of PD in both groups was done (Tables 4 and 5, Figure 1). The chi-square test was done for gender association. Results were considered significant if the p value was less than .05. Then, IR methods were compared using a student t test with HOMA IRi being a dependent factor and HOMA IRc, and TGI as covariates (Table 6). Correlation of HOMA IRc and TGI with HOMA IRi was done using linear regression with Pearson and Spearman’s rank correlation (Tables 7 and 8, Figure 2).
IR - PD stages.
Results
Among a total of 145, there were 73 males and 72 females in the D group and 75 males and 70 females, respectively. The mean age was 56.3 in the D group and 56.8 in ND group. The mean BMI was 27.2 in D group and 27 in ND group. The mean HOMA IRi was 5.96 in the D group and 2.20 in the ND group. If we take the Indian cut-off point of 1.23, both groups have increased IR. The mean HOMA IRc was 0.428 and 0.322 in D group and ND group, respectively. HOMA IRc was increased in both groups if we consider the cut-off value of 0.3. TGI was 5.098, 4.884 in the D and ND groups, respectively. If we consider the TGI cut off of 4.65, then both have increased IR, but there is no significant difference between the groups. There is no significant difference in IR between genders or across all stages of PD in both groups. A strong positive correlation of HOMA IRc (Figure 1) and TGI (Figure 2) with HOMA IRi was noted.
IR - Comparison by Surrogate Markers.
IR - by PD stages and D & ND Groups..
Independent Samples t-test.

Linear Regression.
Coefficients.
Marginal Effects Plots.
Discussion
PD is a multifactorial oral disease characterised by chronic inflammation of the supportive tissues of the tooth. This results from an inflammatory response induced by altered oral microbiota. Periodontitis is epidemiologically linked with several diseases such as Type 2 diabetes, cardiovascular diseases, obesity, neurodegenerative pathologies and non-alcoholic fatty liver disease. The pathological process is mediated through elevated plasma levels of TNF-α, IL-6 and C-reactive protein (CRP). 4 Dysglycaemia and elevated IR markers such as HOMA-IR were noted in non-diabetic individuals with PD in an Indian study. 5 We also noted HOMA-IR was raised in the Diabetes and non-diabetes groups when we applied the regional cut-off value of 1.23. PD appears to have increased IR in the non-diabetes group, but it is difficult to extrapolate the same to the diabetes group since it is a cross-sectional study with a small sample size. Moreover, the selection of BMI between 23 and 30 and the genetically related non diabetes during sampling may have eliminated the phenotypic clusters like Severe insulin deficiency diabetes (SIDD) and severe insulin resistance diabetes (SIRD), but the small sample size may have offset the efforts. That is the limitation of our study.
The hyperinsulinaemic euglycemic clamp technique is the gold standard for the estimation of IR, which was first developed by DeFronzo et al. in 1979. 6 However, this technique is cumbersome and cannot be routinely used in less resourceful settings. The most widely used alternative test is the HOMA-IR index, which was first proposed in 1985 as a surrogate marker and then updated in 1998. 7 There are different cut-off values in diabetics and non-diabetics.
But there are a few practical difficulties in using an insulin assay-based index when screening.8,9 The samples need to be transferred to the laboratory by maintaining a cold chain, as insulin is so fragile and temperature sensitive. This makes HOMA IRc a better option as C peptide is more thermo stable compared to insulin. This was studied in Saudi Arabia and Africa, where HOMA IRc had a good correlation with HOMA IRi.10,11 We also found that HOMA IRc had a strong correlation with HOMA IRi. CLIA is widely used for HOMA IRc, but it has to be standardised before routine use. Lipid-based surrogate markers of IR have been recommended, including TG to HDL cholesterol (TG/HDL-C) ratio, the visceral adiposity index, the lipid accumulation product (LAP), and TGI. 12 So, we considered TGI as it has more advantages like accessibility, affordability and the results are readily available at the primary point of care. The cut-off value of TGI for South Indians devised in the study by Jogg KS et al. is 4.6. But we found both groups had similar mean values TGI, but fell in the range of IR. 13 Perhaps the diabetic arm may have been on therapy for elevated triglycerides, leading to relatively low TGI.
Conclusions
IR was observed in diabetic as well as non-diabetic groups with PD; however, it was significantly higher in the diabetic group. There was no significant difference in IR between genders or ºamong the four stages of PD in either group. PD appears to aggravate IR in diabetic individuals and may contribute to the development of IR in non-diabetics, potentially increasing their risk of developing diabetes.
Since HOMA-IR using C-peptide correlates well with the standard insulin-based HOMA-IR, it may be preferred for research or clinical use in laboratories where maintaining an ideal cold chain is challenging—an important consideration in the Indian setting.
As lipid profiles are routinely performed in primary care for all diabetic patients, the TGI can be easily calculated and included in laboratory reports. It is simple, cost-effective, and widely accessible, and may assist clinicians in identifying IR and selecting appropriate therapeutic strategies.
Footnotes
Acknowledgements
Acknowledge the staff of the lab and the Office of Indra Diabetes Centre, Thoothukudi, for their support in the study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
Ethical committee approval was obtained from Thoothukudi Medical College.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed Consent
Consent from the patients was obtained.
