Abstract
Traditional assessments focus on identifying deficits and determining diagnoses, but there is growing recognition of the importance of honoring neurodiversity in our clinical work as a result of the neurodiversity paradigm and movement. Therapeutic Assessment has emphasized greater collaboration between the client and clinician. We suggest that ideas from the neurodiversity paradigm can be combined with traditions from Therapeutic Assessment to create a more effective process. We introduce principles of Neurodiversity Affirming Collaborative Assessment using the acronym CARES: Collaborative Understanding, Accessibility, Recognizing Intersectionality, Empowerment, and Strengths Recognition. We offer practical strategies that can be applied to assessments across the lifespan.
Lay Abstract
Clinicians are already aware that providing assessments to individuals and families can help them learn about themselves and figure out next steps toward improving their lives. Traditionally, most assessments have focused on finding problems. The neurodiversity paradigm is the idea that there is no one right way of thinking and no one right type of brain and different ways of thinking should be celebrated. Therapeutic assessment involves clients and clinicians working together to figure out more about the client. We suggest that it is helpful to combine the neurodiversity paradigm and therapeutic assessment to complete better assessments. We offer some principles and strategies for combining neurodiversity with therapeutic assessment so that clinicians can be more successful in helping their clients.
Despite growing awareness of neurodiversity, most psychological assessments are still largely deficit-focused (Kaufman, 2022). When people seek out an assessment for themselves or their children, professionals still tend to approach assessments by asking “What is the name for the things that are wrong with this person?,” sometimes followed by, “What should I recommend to make them better (or more normal)?” Approaching people in this problem-focused way leads to short-sighted, inadequate, and inaccurate assessments, but there is an alternative that offers hope and empowerment.
A thorough, affirming assessment can be life-changing for many people. For example, some have described the assessment process as the most important event in their lives (Arnold et al., 2020) and research suggests that people who are assigned an affirming diagnosis that matches their self-identity (e.g., autism or ADHD) experience fewer symptoms of depression, anxiety, and self-harm (Kroll et al., 2024). A recent review found that an important ingredient for parent satisfaction in assessments is collaboration between professionals and the parents, including open and effective communication throughout the process (McCrimmon & Gray, 2021). Research suggests that clinicians who work collaboratively in assessing their clients have improved rapport and longevity (Ackerman et al., 2000) and effectiveness (Poston & Hanson, 2010).
Influence from the neurodiversity movement has gradually helped us better understand forms of neurodivergence like autism, allowing us to recognize it as more than just a set of deficits and instead as a different way of being, with both strengths and struggles that depend on the social context (Cope & Remington, 2022; Kapp et al., 2013; O’Neil, 2008; Russell et al., 2019; Woods & Estes, 2023). The sensory processing difference that leads an Autistic person to be overwhelmed by certain sounds, for example, may also lead them to have more accurate auditory perception (Remington & Fairnie, 2017). The same characteristics that contribute to off-task behavior in people with ADHD also seem to be associated with increased creativity (White & Shah, 2016).
While individual clinicians have gradually started embracing the concept of neurodiversity and thinking about how it applies to their work, and groups of clinicians have started discussing ways to apply the neurodiversity paradigm (Chapman & Botha, 2023; Dallman et al., 2022; Dundon, 2023; Kroll et al., 2024), there is no specific framework for what a neurodiversity-affirming approach to assessment looks like. Combining reflections on our clinical experience with research and knowledge from the Autistic community, this article aims to provide a set of five principles and a five-step approach to support clinicians who want to take a neurodiversity-affirming collaborative approach to assessment.
Neurodiversity itself refers to the concept that there is variability in human brains, including attention, mood, sociability, and other mental functions. The concept of neurodiversity was created within online Autistic communities in the mid-1990s (Botha et al., 2024). It was further explored, especially within academia, by sociologist, Judy Singer (e.g., 1999) and discussed by journalist, Harvey Blume (e.g., 1998). Although the neurodiversity movement has been primarily associated with autism, neurodiversity also includes other forms of neurodivergence like ADHD, Bipolar, Posttraumatic Stress Disorder, and Obsessive Compulsive Disorder. The idea that there is variation in how our brains work is an accepted reality. The idea that this is a good thing, to be celebrated, is more controversial. That is the crux of the neurodiversity paradigm. According to Nick Walker (https://neuroqueer.com/neurodiversity-terms-and-definitions/), there are three key principles of the neurodiversity paradigm (Walker, 2024):
Neurodiversity is a natural and valuable part of human diversity. The idea that there is one “normal” or “healthy” type of brain or mind, or one right style of neurocognitive functioning is a culturally constructed fiction. The social dynamics that manifest in regard to neurodiversity are similar to the social dynamics that manifest in regard to other forms of human diversity (e.g., the diversity of ethnicity, gender, or culture). These dynamics include the dynamics of social power inequalities, and also the dynamics by which diversity, when embraced, acts as a source of creative potential.
While the medical model frames types of neurodivergence like autism, ADHD, and Bipolar, as problems characterized by some deviation from an arbitrary norm (Anderson-Chavarria, 2022), the neurodiversity paradigm acknowledges that variation in brains is a natural part of human society and this variability in brains is something to be valued. As a result, when we assess people, as neurodiversity-affirming providers, we are not looking for differences to identify problems, we are exploring differences to better understand people and help them better understand themselves. While we acknowledge that the idea that there is one normal type of brain or way of being is problematic, we also acknowledge the reality that we are surrounded by measures, tools, books, and articles that send the message that “normal” (which often means “average”) is the best way to be. As a result, we have to make a concerted effort to work against that messaging that affects not only how our clients view themselves, but how we view them. Furthermore, we recognize that our clients live in a world where people with certain types of brains are celebrated and rewarded and others are shamed and rejected. We take active efforts to understand that experience and we empower our clients to withstand and overcome those negative social dynamics. Instead of telling them all of the ways in which they deviate from the norm and what they must do to fit in, we help them understand and embrace their differences and support them in figuring out how to apply them to meet their own needs and goals.
Several previous papers and books have explored what a neurodiversity-affirming assessment process for autism might look like (Curnow et al., 2023; Gabrielsen et al., 2023; Hartman et al., 2023; Henderson et al., 2023a, 2023b; Lowry, 2021; Pritchard-Rowe & Gibson, 2024; Schwartz, 2020; Woods, 2020). Curnow and colleagues (2023) emphasize a collaborative approach (“nothing about us without us”), recognizing strengths as well as challenges (“difference not deficit”), using “strengths focused language” (“language matters”), recognizing situational factors affecting the Autistic experience rather than centering the cause of disability in the person (“environment first”), framing the autism diagnosis positively and in a way that supports self-advocacy (“diagnosis matters”), and recognizing co-occurring diagnoses (“neurodevelopmental lens.”) Hartman and colleagues (2023) emphasize the importance of considering intersectionality, masking or camouflaging, collaboration, accessibility, and attending to strengths. Henderson and colleagues (2023a, 2023b) emphasize recognizing less stereotypical presentation of autism, intersectionality, and strengths. Lowry (2021) emphasizes recognizing environmental factors disabling Autistic people and Autistic strengths. Woods (2020) argues for directly assessing individual and family strengths as part of the autism assessment process. Schwartz (2020) points out the importance of recognizing common myths about autism and actively avoiding them. Gabrielsen and colleagues (2023) highlight the need to consider more nuanced presentations of autism. And based on interviews with professionals who serve Autistic people in the UK, Pritchard-Rowe and colleagues (2024) emphasize taking the client's perspectives seriously, “balanced assessment” of strengths and needs, using neutral to positive rather than deficit-based language, and attending to “person-environment fit.” The current framework builds on these recommendations in several ways. Specifically, we broaden the recommendations to be applicable to any assessment, not just autism evaluations. Also, and most significantly, we explicitly combine neurodiversity-affirming principles with a collaborative approach derived from collaborative/therapeutic assessment. While previous authors recommended a collaborative approach, we think that linking neurodiversity-affirming assessment with the very well-developed and highly regarded collaborative/therapeutic assessment framework provides a helpful roadmap for assessors.
If variations in the ways brains work and the ways people think are valuable, and if there really is no one right “normal” or “healthy” brain, how does this change the assessor's role? Their role is no longer focused solely on identifying deficits, but rather determined in collaboration with the client. In fact, it is impossible to do a neurodiversity-affirming assessment without using the principle of collaboration because the purpose, meaning, and outcome of the assessment itself cannot be determined without the client's input (and in the case of young clients, parents’ input).
There has been some gradual recognition of the importance of collaboration with clients in certain assessment circles, especially in the collaborative/therapeutic assessment community. Fisher pioneered the idea of collaborating with clients as part of the assessment process in the 1970s (e.g., 1970, 1971, 1972, 1979) recommending that clinicians follow these steps to effective collaborative assessment: collaborate, contextualize, intervene, describe, and respect complexity, holism, and ambiguity. Finn (2007) later developed Therapeutic Assessment, which is a semi-structured form of collaborative assessment that involves collaboratively gathering and strategically sharing assessment information with clients with careful consideration of what is least and most discrepant from how they already view themselves. The Therapeutic Assessment community has played a major role in pushing back on traditional pathologizing techniques and we are grateful for these contributions. Collaborative and Therapeutic Assessment (TA) can also benefit from the tension of applying the neurodiversity paradigm to traditional practice. For example, TA is still based primarily on finding problems and assumes that the clinician knows more about the client than they know about themselves and that disagreements in findings are evidence of a lack of insight on behalf of the client, rather than a possible misunderstanding on the part of the assessor. Combining a collaborative approach with the neurodiversity paradigm offers a new and empowering step forward.
Combining the neurodiversity paradigm with collaborative/therapeutic assessment (as summarized in Figure 1) brings us five main principles, which, if followed, will lead to more fulfilling, useful, and accurate assessments for people of all ages: (1) Collaborative Understanding, (2) Accessibility, (3) Recognizing Intersectionality, (4) Empowerment, and (5) Strengths Recognition (these are summarized in Figure 2). These principles can be applied to assessments across the lifespan as long as the clinician has the appropriate background knowledge and expertise. Likewise, clinicians who are culturally competent and show the appropriate cultural humility will benefit from applying these principles to work with people of different backgrounds. These principles are not meant to apply solely to diagnostic assessments, which are generally aimed at identifying diagnoses, but instead focus on psychological assessments more broadly, which aim to identify strengths and challenges as well as answering the assessment questions of the individual being assessed.
Elements of Neurodiversity Affirming Collaborative Assessment.
Neurodiversity-Affirming Collaborative Assessment Principles: CARES
Collaborative understanding: It is increasingly recognized that to be effective and neurodiversity-affirming, researchers and clinicians must collaboratively engage with Autistic people as partners (Pellicano & den Houting, 2022). Similarly, in Neurodiversity-Affirming Collaborative Assessment, instead of formulating assessment questions from our own perspectives, tabulating the results of questionnaires and tests, and telling clients what the outcome means, we collaborate with our clients in figuring out what they want to know about themselves and then understanding, together, what the results mean for them. We turn to them as experts on their own experiences and invite them to help us discover together what the implications of the assessment are. We also work towards helping them to be their own authentic selves, rather than trying to be something else. To start the collaborative process from the beginning, we encourage assessors to follow the tradition of Therapeutic Assessment and develop collaborative questions that can be answered as part of the assessment (Finn, 2020). More suggestions follow later in the How-To section.
Shared understanding does not refer to simply deferring to the clients and confirming whatever they expect to hear. Instead, it involves an active discussion and exploring hypotheses together (sometimes involving parents and other family members). For example, a client who presents with symptoms of depression could very well meet criteria for Major Depressive Disorder, but it will not be until after we have engaged in a thorough clinical interview and gathered multiple types of data (including from collateral sources of the clients’ choosing), that we figure out whether it could also be described as Autistic burnout (Raymaker et al., 2020) or a reaction to chronic invalidation, ableism, abuse, or poverty. Knowing this offers insight to the client and guides recommendations.
In order to engage in collaborative understanding, effective clinicians also educate themselves about the experiences of the populations they work with. For example, anyone who works with Autistic people should be well-acquainted with the concept of masking and able to engage in discussion about it. Autistic people, in particular, often face rejection based on nonautistic people's negative ways of viewing their behavior (Boucher et al., 2023; Sasson et al., 2017). This leads to shame, the fear of further rejection, and rejection sensitivity (a hypervigilance for and anticipation of further rejection) (e.g., Lin et al., 2022). Shame leads to masking or camouflaging, hiding their true selves under a neurotypical-appearing veneer (Hull et al., 2019). This masking is exhausting and can compromise attention available for things like learning and true social connection. But it is reinforced by others, including certain therapies like social skills training, which leads to more shame and more masking. It also leads to other people, including assessors, being even less likely to recognize the needs that the neurodivergent person is hiding, and therefore more invalidation (Shenk & Fruzzetti, 2011). After so much hiding, people may not even know who they are or what they want. Because masking is exhausting and unsustainable, it can lead to burnout (Raymaker et al., 2020). It also far too commonly leads to suicidality (Cassidy et al., 2018), as people conclude that the way they are is fundamentally unacceptable. Masking is not unique to autism (Miller et al., 2021) and is believed to have similar negative effects on other people. For some people, masking is a matter of survival, especially if they are part of other marginalized groups (Lopez et al., 2022), and suggesting that they should stop it all together could be harmful. Working together with our clients to understand how and why they use masking is an essential part of the assessment process. Research efforts to identify and measure masking are still in their infancy so over relying on masking scores is to be avoided, but offering clients space to describe their own experiences and reasons for masking is useful.
Overall, collaborative understanding involves making sense of the findings together and understanding what they mean for that particular client in their particular situation, whether they are a child or adult. We solicit their input in whatever way makes the most sense, combining our expertise as clinicians with their expertise on their own life experience, which informs what it is like to be them and what they need in the social context they currently live in.
Accessibility: Because we celebrate different types of brains, we make room for different ways of thinking and expressing ideas. The first step in helping our clients learn to advocate for their own accessibility needs is making the assessment itself accessible. Neurodiversity-affirming assessors allow clients to communicate their thoughts and experiences through a range of different means. Some might prefer to write out long documents or even create Powerpoint presentations to share their thoughts. Others respond better to structured clinical interviews. For autism, many respond well to the flexible nature of the Monteiro Interview Guidelines for Diagnosing the Autism Spectrum, Second Edition (Monteiro, 2021). Questionnaires can often be overwhelming for many Autistic people (Stacey & Cage, 2023), but allowing them to write notes and share how they think the statements apply to them can empower them to share their experiences more fully. Some children may respond especially well to communicating their ideas and experiences through drawing. Nonspeaking people may use technology to communicate. Clients with Bipolar might benefit from keeping mood diaries and having a chance to share them over time. We acknowledge that effective assessments integrate multiple types of data rather than relying on one main modality (Wright et al., 2022). We gather multiple types of data and elicit feedback from our clients, not only based on what their responses to the questions are, but we check in about the assessment process itself. We agree to contact multiple informants of the client's choosing to help us have a more comprehensive picture. We also go out of our way to make the testing spaces comfortable and accessible to people with mobility difficulties and sensory differences (e.g., using suggestions gathered from Autistic researchers (Doherty et al., 2023). We use open, clear communication and help our clients know what to expect as part of the assessment right from the beginning. If something is not working for them, we remain flexible and responsive to what might make them more comfortable. By making the assessment process itself accessible, we are sending the message: “You deserve access. Your access needs matter.”
Recognizing intersectionality: Intersectionality is defined as “a way of thinking about identity and its relationship to power” (Crenshaw, 2015). It was originally developed because Black women were being discriminated against, but the discrimination was discounted because it was not purely based on sexism or purely based on racism, but based on a combination of the two. Intersectionality refers to the fact that different types of discrimination and privilege interact. The experience of having a particular neurotype (e.g., being Autistic, having ADHD, or being Bipolar) depends on many other aspects of a person's identity (e.g., age, gender, race, profession, religion) so recognizing that people may face multiple types of discrimination that interact with each other is especially important. In addition, discovering that one has a particular neurotype involves integrating multiple identities as well. As a result, we make ourselves aware of cultural differences and connect our clients with other individuals who might have some of the same experiences as them. For example, we might connect Black Christian Autistic clients to people like Lamar Hardwick, PhD and we might connect trans Autistic clients to resources created by trans Autistic leaders like Finn Gratton, LMFT. We might suggest that people in the medical field connect with other clinicians with disabilities through an organization like Docs with Disabilities or the Autistic Social Caring Network.
Making blanket recommendations drawing from “best practices” that are developed based on populations other than the people we are actually working with, is commonplace, but often ineffective. Effective clinicians must also be aware of intersectional invisibility (Lopez et al., 2022), in which people with different combinations of identities (e.g., Native Autistic people) are often left out of research altogether. We practice cultural humility (Ramclam et al., 2022) and invite clients to collaborate with us in finding the communities and practices that work for them.
We also consider how physical health difficulties might intersect with certain neurotypes. For example, people with conditions like Ehlers-Danlos syndrome often endure a significant amount of traumatic invalidation by the medical establishment that dismisses or misdiagnoses their symptoms (Halverson et al., 2023). As a neurodiversity-affirming clinicians, we consider how these invalidating experiences may lead to fear about allowing yet another medical professional to evaluate them and we express an attitude of gratitude that they allow us into their worlds.
Likewise, nonspeaking people and/or people with intellectual disabilities are especially likely to be stereotyped, discriminated against, and have their voices discounted (Lebenhagen, 2020; Llewellyn et al., 2015). In order to best serve our clients, we select tools that have been researched on the groups they belong to, interpret the findings according to their actual cultural context, and support our clients in integrating new information into the other aspects of their identity.
Empowerment: The assessment tools that we use, the books we have been trained to study from, and even the broader communities that we work in tend to be based in the medical model, in which the average, typical brain is framed as ideal and variations from it are framed as problematic (Chapman, 2023). Empowering our clients in a pathologizing world requires an active choice. It is not enough for us to add the element of looking for strengths as part of our assessments. Instead, we engage in ongoing deliberate action to prevent ableism from infiltrating our assessment processes and having a negative effect on our clients. We consider the social model of disability (Olkin, 2002) and consider the ways in which the social context itself can be disabling instead of placing blame on the individual. We avoid using tools that conceptualize a neurotype based solely on its associated deficits and we actively encourage one another to move toward developing tools and strategies that value different neurotypes. As part of the assessment process, we make our clients aware of the discrimination that exists related to different neurotypes and we support them in finding ways in their own lives to overcome them, for example, by providing parents with lists of affirming books and websites to read to their children to build them up and support their development of a positive self-concept as a disabled child. For people with Bipolar, we might offer examples of successful Bipolar role models like Carrie Fisher, Mark Vonnegut, MD, and Justin Bullock, MD.
Collaborating with teachers as part of the assessment process and modeling a neurodiversity-affirming view while also providing instruction in self-advocacy to children and adolescents can make a world of difference. Offering guidance to teachers and parents on creating neurodiversity-affirming environments can also be part of the neurodiversity-affirming collaborative assessor's role. Helping clients select affirming therapies that work with their neurotype instead of against is part of the empowerment process (like DBT modified for Autistic people, Brook et al., 2024). Empowerment can also include figuring out what types of accommodations a client might ask for at work to help their work environment align more with their brain style. It can include figuring out sources of funding and programs a child qualifies for, helping them figure out how to apply, and giving them the correct documentation and wording to access what they need. As clinicians, we can support our clients in considering philosophical concepts like what it means to be neurodiversity-affirming while also supporting them with real-world practical steps to ask for what they need.
Strengths recognition: To complete effective assessments, we begin with the assumption that, in addition to challenges, everyone has strengths that can be useful to them. Thus, in addition to identifying challenges, we aim to identify strengths—what is already working well for people and what additional potential they have that we can help them discover. In sum, we focus on identifying differences in each assessment client, both challenges and strengths. The latter may include personality strengths that can be assessed using tools like the 16 Personality Factor Inventory (Cattell & Mead, 2008), strengths associated with certain neurotypes (like autism) using tools like the Survey of Autistic Strengths Skills and Interests (Woods & Estes, 2023), family strengths, and strengths associated with being part of certain communities like the Autistic community (Botha et al., 2022). Starting a clinical interview by asking about interests helps build rapport (Powell et al., 2024). Recognizing strengths also means that we use neutral to affirming language, rather than deficit-based language (Bottema-Beutel et al., 2021). For example, we use identity-first language (e.g., Autistic person not person with autism) and refer to different co-occurring conditions instead of “comorbidities.” Of course, in addition to talking about strengths, we also make room for a discussion of challenges because focusing solely on strengths can be invalidating of clients’ actual experiences. Helping clients to better understand themselves requires us to make room for a discussion of suffering (P. Wright et al., 2024). Furthermore, we respect that different neurotypes are associated with different types of strengths and we reject biases that lead to some neurotypes being elevated above others. For example, we avoid messages of “Aspie supremacy” (Hooge, 2019) in which certain types of autism are elevated above other forms of autism. We also resist efforts to ineffectively categorize people using poorly substantiated evidence, as is the case with terms like “severe” or “profound” autism (Kapp, 2023).
Recognizing strengths also includes making some recommendations that build on these strengths. For example, instead of asking “what is wrong with this person and what can I recommend to make them more normal?,” we ask “what strengths does this person have and how can we use them to help the client achieve their goals?” For example, many Autistic people thrive when they are allowed to focus on their special/intense/focused interests. Gaining insight into what a client enjoys and how that might be applied is invaluable. For example, children who love dinosaurs thrive in a classroom that incorporates that interest into the curriculum (Winter-Messiers et al., 2007). Autistic people, especially, who are encouraged to embrace their focused interests may find that these interests lead them toward successful careers as well as increased life satisfaction (Laber-Warren, 2021; Woods & Estes, 2023). An assessment that recognizes strengths also explores coping strategies that are already being used that may be harnessed to further support the individual. For example, although “stimming” has traditionally been seen as nonfunctional and targeted for reduction or elimination, recent research has shown that these repetitive movements often help Autistic people cope with sensory input (Kapp et al., 2019). Similarly, if parents share that their children respond especially well to music, it may be helpful to explore how they might benefit from using music as a way to modulate emotions. Highlighting strengths in a memorable way during the feedback session is also important (e.g., using Brain-Building books by Angoff, 2021, 2022). Strengths can sometimes also be used to compensate for struggles. For example, clients with ADHD who work especially well under time pressure can make use of that response by creating numerous deadlines for themselves to compensate for a tendency to procrastinate.
We are excited to contribute to the growing movement of people applying the neurodiversity paradigm to the clinical world. We hope that others can build on our suggested principles and that, as a community, we can continue to collaborate on defining what it means to be neurodiversity-affirming.
In order to integrate these steps into the assessment process, we suggest a five-step process.
Transparency and accessibility in testing: Giving children, adults, and their families a clear outline of the assessment process and a clear avenue to access
Many clients come to an assessment with no idea of what to expect or how the assessment process works. An important part of empowering the client from the beginning involves helping the client and/or family know what will happen, including what tools might be used, how long it might take, and how much it will cost. Getting their input from the beginning is also an important way to empower the client. Furthermore, creating a sensory friendly environment from the start is an important way to communicate that we value and acknowledge different ways of experiencing the world. For example, most Autistic people experience sensory differences and these can affect multiple domains (Doherty et al., 2023). Taking steps to offer comfortable lighting (e.g., sunlight, instead of fluorescent lights), reduced noise, comfortable seating, reduced visual distractions, and fidget toys to fiddle with, not only leads to people feeling more comfortable, but sends a message that you are aware of sensory differences and you see the value in considering them. Some clients may not be able to come to sessions in person due to distance, mobility issues, or for financial reasons so accommodating people remotely is also important. Many Autistic people also have difficulty with executive functioning (St. John et al., 2022). We can reduce executive functioning demands by not including unnecessary paperwork, sending reminders for appointments, and offering grace if people are late.
Creating assessment questions with clients: For both children and adults, creating assessment questions collaboratively to understand what is most important to them and how the answers will help them meet their goals.
Traditional assessments often start with the assumption that the goal of an assessment is to identify a problem, find a name for it, and recommend a treatment to fix it. Under the neurodiversity paradigm, we understand that difficulties do not result from one specific issue that is inherently “wrong” with an individual, but instead from a mismatch between an individual and their social context. Furthermore, as collaborative clinicians, we understand that the client can play a role in deciding what we learn. This opens the door, not only to greater complexity, but to more opportunities. Instead of asking, “what is wrong and how can we fix it?”, clients might want to know the answers to questions like “What are my strengths?” “What kind of work would be a good fit for me?” “Why is math hard for me, but reading is easy?” “Why does the same issue keep coming up in my relationships?” “How are my childhood experiences connected to what is happening for me now?” “What should I work on in therapy?” “What accommodations should I ask for in school?” The question will also often include “What diagnosis best describes me?” but the client is encouraged to think beyond the label itself to the individual meaning it has for them. By allowing the client to decide what questions to ask, we are placing them in the driver's seat and giving them some control over both the process and the results of the assessment.
Shared information gathering and co-interpretation of results: Clients, including children, are invited to help give meaning to the findings within the context of their lived experience.
Traditional assessments typically involve the evaluator tabulating the scores and interpreting them for the client, telling the client what they mean, in the same way that a doctor might interpret an X-ray or the results of a blood test. The process often involves quantifying how far a person is from some ideal (which is often defined as “average” or “normal”). As collaborative clinicians, we understand that the results make the most sense and will be most valuable for the client if they are given a chance to explore what the findings might mean for them. We select tools that are appropriately normed for the clients we are working with, considering factors like age, race, and reading ability. Then, we share the results and invite the client to join us in understanding what they might mean for them in their particular context. For example, we might share specific test scores and ask them to help us understand them. If a client receives an elevation on the phobias scale of the Personality Assessment Inventory (PAI), we might ask “this tends to be elevated when people have fears of specific things, what kinds of fears do you think might have caused this to be elevated?” We can also encourage clients to give us feedback on the assessment process as it goes. For example, we might ask, what was it like to fill out that questionnaire? We might also offer opportunities for clients to take notes and clarify their answers. This has been particularly useful among Autistic clients who can often find questionnaires frustrating (Stacey & Cage, 2023). We might also encourage a client to help us understand discrepancies in the data. For example, “in an interview, your coworker reported that you make typical eye contact, but your spouse reported that you make less than typical eye contact. In our interview, you reported that you work hard to make eye contact, what do you think is contributing to people's different impressions of you?” This can then lead to further discussion of masking, burnout, and the toll it might be taking on the individual. It can also help them consider the effects of their social context on their wellbeing. To be neurodiversity-affirming, we also allow clients to share information in a format that works for them. For example, for a writer, artist, or poet, we might invite them to share whatever medium they use to express themselves and use that as a starting place for discussion. For an adolescent, we might make use of memes displaying different psychological experiences (e.g., an interesting meme of a frowning penguin with the caption “When someone asks me to do something I was alreadly planning on doing... Well now I'm not doing it >:(”) (Woods, 2021). For children, we might talk about their intense interests and the satisfaction they get from them. We might also use kinetic drawings (e.g., of their family or school environment and allow them to share their experiences through what they draw.
Meaningful reports and individualized recommendations: Communicating testing results in a way that is meaningful to and actionable for the client themselves, using stories, visuals, metaphors, and the client's own language.
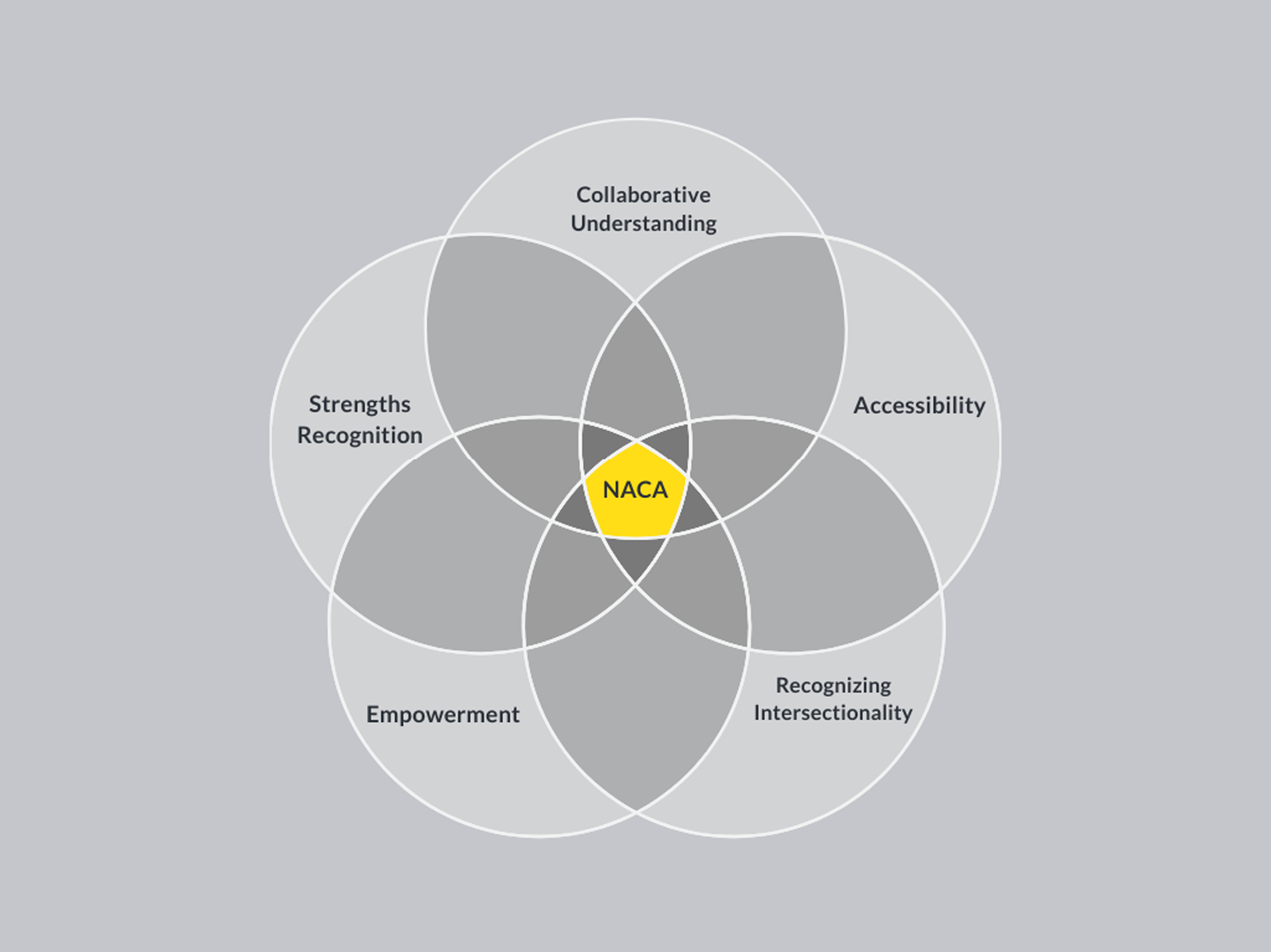
Principles of Neurodiversity Affirming Collaborative Assessment
After spending some time sharing our findings with the client and understanding what they might mean, we can put the information together in a way that most helps the client in the real world. Acknowledging the limitations of the world we live in, we might talk to the client about the need to use certain language in the report in order to help them access services and supports (e.g., in school or through disability services). At the same time, we make it a point to highlight their strengths. For children, we might write metaphors using a topic of interest. For adults, we might consider how the findings translate to their individual workplace and make specific recommendations to make work go better for the individual. We can also talk to the client and their family about what they think they need in school or work and integrate those suggestions into the report whenever possible. We consider intersectional issues as we help clients process the meaning of the findings and connect them with other people who might share some of the same experiences as them. Another powerful, but unconventional step, is offering the client or parent a chance to read a draft of the report before it is finished and give feedback about whether or not it is accurate for them. Then, we can make changes and improve the report's accuracy. The assumption is not that discrepancies between the client's view of themselves and our view of them is evidence of their lack of insight, but also consider the alternative: that maybe the client understands parts of themselves better than we do and maybe giving them space to educate us will result in a better, more accurate report from everyone's point of view.
Ongoing dialogue and support: Recognizing that learning happens over time, and neurodivergent individuals often need additional time to process information, providing opportunities for check-ins and additional questions as part of the process.
The time after participating in an assessment is often difficult for clients. They are seeing themselves through a new lens and beginning down what might feel like a new path. Connecting clients to supportive resources like support groups or affinity groups with other people who share their neurotype can be empowering and supportive. For example, in Washington state, clients can be connected with Square Pegs, a free group run by an Autistic social worker named Zack Siddeek, MSW. Also, connecting clients directly with therapists who are known to the assessor and doing a “warm hand-off” can also be helpful. Furthermore, being there to check in and offer follow-up support as needed can help clients feel empowered to move forward. Clients may encounter new obstacles along the way such as adjusting to a new work environment or starting a new school program. Being able to reach back out for help with practical support like a letter documenting a need for accommodations for emotional support as they transition to a new setting can be an important part of the assessment process.
Future Directions
Several considerations are beyond the scope of this article, but important for the field to address. First, we hope to see more research about how the types of changes we recommend are experienced by clients. Do they feel more affirmed and are the recommendations more useful to them? Second, availability and affordability of Autism evaluations lag far behind need. Thus, it is important to explore how these principles can be incorporated into evaluations that are as efficient, affordable, and timely as possible. Third, how can systems adapt to consider the social, rather than primarily medical, model of disability, to facilitate implementation of more effective and affirming recommendations?
Footnotes
Acknowledgments
We thank our clients and families who allow us to learn about their lives and help us to become more effective clinicians.
Declaration of Conflicting Interest
Dr. Woods provides continuing education and training to professionals, parents, and community members on neurodiversity, autism, ADHD, differential diagnosis, and assessment. Dr. Brook provides training and consultation to professionals about neurodiversity affirming assessment and DBT, is in contract with Guilford Press writing a manual on tailoring DBT for Autistic clients, and will eventually receive royalties after this manual is published. Dr. Angoff is the author and publisher of the Brain Building Books. She receives proceeds from the sale of these books, which support the creation of all of the resources on explainingbrains.com.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
