Abstract
Background
Socioeconomically disadvantaged populations have a high prevalence of chronic pain, exacerbated by social isolation, intersectional stigma, and disparities in pain assessment and treatment. Effective interventions using a multilevel, biopsychosocial approach are needed to decrease the unequal burden of pain. Group-based integrative pain management in primary care safety net clinics is a promising model to improve pain care for racially and ethnically diverse low-income people.
Objective
To describe a study protocol to test the impacts of 2 group-based models – group acupuncture and integrative group medical visits – on multilevel pain-related outcomes.
Methods
The study uses a 2x2 factorial randomized clinical trial to test two 12 week group-based models: group acupuncture and integrative group medical visits (IGMV, with psychoeducation, mind-body approaches, and social support). English or Spanish-speaking adults with chronic pain for ≥3 months receiving care in San Francisco Department of Public Health primary care clinics are eligible for the trial. All participants will receive usual care and be randomized to group acupuncture, IGMV, both, or waitlist control. The primary outcomes are changes from baseline to 3 month follow-up in pain impact and in social support for chronic pain. Secondary outcomes include pain interference, pain intensity, depression, anxiety, quality of life, and social isolation. Data will include patient-reported outcomes, electronic health record data, and qualitative interviews, focus groups and observations to assess multilevel individual, interpersonal and organizational outcomes.
Discussion
Multilevel approaches are needed to advance health equity in pain management. Our study contributes to knowledge of group-based integrative pain management in primary care safety net clinics to address multilevel barriers and disparities in pain care.
Keywords
Background/Rationale
Socioeconomically disadvantaged patients face considerable disparities in pain assessment and treatment. Prevalence of chronic pain is higher among U.S. adults with low income, less education, and public insurance. 1 The burden of pain is exacerbated by multilevel barriers to pain care, including undertreatment for individuals of lower socioeconomic status, 2 and those who identify as Black or Latine.3,4 Limited insurance coverage of optimal treatment at the structural level, lack of access to multimodal and nonpharmacologic care at the organizational level, and provider bias and other forms of discrimination at the interpersonal level contribute to unequal assessment, treatment, and quality of pain care.2,5-7
Cross-cutting all levels, stigmatization of chronic pain intersects with systems of oppression (eg, racism) to contribute to disparities, leading to delayed healthcare seeking, social isolation, depression, and other negative health outcomes. 8 Addressing the biopsychosocial experience of pain is an accepted paradigm for chronic pain treatment, but the ‘social’ is often missing from ‘biopsychosocial’ approaches. 9 Pain treatments focus predominantly on physical symptoms or psychological aspects of pain (eg, coping and reappraisal) with little regard for the profound impacts of social context. Chronic pain has a bidirectional, cyclical relationship with social isolation,10,11 which itself is a risk factor for all-cause morbidity and mortality at a level comparable to smoking and lack of exercise.12,13 The health threats of social isolation among individuals with chronic pain (eg, worse pain severity, emotional and physical functioning)14,15 are critical amidst the repercussions of the COVID-19 pandemic. 16 The impacts of social isolation are more pronounced for those experiencing racism and other forms of social inequality.16,17 Multilevel approaches inclusive of social factors are critically needed to abate the unequal burden of pain for socioeconomically disadvantaged populations.
Primary care safety net clinics are a critical resource for the publicly insured, uninsured, and underserved, and are uniquely positioned for providing care to marginalized populations and addressing disparities. 18 However, significant barriers impede optimal pain assessment and treatment in primary care safety net clinics. Pain is one of the most common reasons for primary care visits. Yet, primary care physicians (PCPs) in safety net clinics report low confidence in their chronic pain management abilities and low levels of satisfaction with the treatment they can provide.19,20 Foremost among the barriers PCPs report is time pressure, limiting their ability to adequately assess their patients and safely manage opioid prescribing. 19 PCPs also indicate that system-level constraints include lack of access to multimodal, integrative treatment which cannot be offered in brief primary care visits. 19 Clinical guidelines and a growing body of evidence endorse nonpharmacologic approaches as first line treatment for pain, 21 and as a core part of multimodal chronic pain management.22-24 However, availability and affordability limit use of nonpharmacologic treatment in primary care. 25
Group-based integrative pain management has emerged as a promising strategy to address time constraints and provide multimodal care in primary care. Group-based models improve access by providing care to multiple patients simultaneously. While many integrative approaches are offered as classes (eg, mindfulness instruction or yoga), here we focus on two group models involving clinician-delivered, billable care: integrative group medical visits (IGMVs) and group acupuncture. Some Federally Qualified Health Centers serving low-income, publicly insured patients have implemented IGMVs as a strategy to increase access to complementary and integrative health approaches including nutrition, yoga, and mindfulness. 26 IGMV programs have been implemented in multiple locations in Spanish and English, demonstrating feasibility in safety net settings serving low-income people from multiple racial and ethnic backgrounds.27-31 IGMVs for chronic pain confer a range of benefits including decreased pain interference, increased self-efficacy, 27 improved quality of life, 30 lower healthcare utilization, and reduced opioid use. 31 Qualitative research on IGMVs points to interpersonal level benefits, such as decreased social isolation, increased social support and improved patient-provider relationships.28,32 The presence of peers has the potential to reduce discriminatory or stigmatizing clinical practices. 33 These potential interpersonal benefits are understudied, and may fill a significant gap in current pain treatment by incorporating the ‘social’ in a biopsychosocial approach.
Acupuncture therapy is an evidence-based treatment for a range of pain conditions,34,35 but is rarely available to safety net patients due to nonexistent or limited insurance reimbursement.36,37 Group acupuncture – a well-established delivery model where multiple patients simultaneously receive treatment in a common space, seated in chairs or recliners – lowers costs, improves availability, and increases utilization. 38 Licensed acupuncturists providing group treatments use acupuncture points accessible on patients who remain clothed during treatment; patients are instructed to wear loose fitting clothes to ensure comfort and access to points. Notably, patient perspectives on group acupuncture indicate high quality of care and value with this model.39,40 In low-income primary care patients with chronic neck, back, or shoulder pain or osteoarthritis, group acupuncture is associated with decreased pain severity, pain interference, and depression based on a quasi-experimental study, 41 and with reduced chronic pain and improved physical function at 12 weeks based on a randomized clinical trial. 42 Beyond pain relief, group acupuncture is associated with improved quality of life, decreased stress, increased engagement in chronic disease self-care,43,44 and reduced barriers to care through ease of scheduling and social learning (eg, less fear of needles seeing others receiving treatment). 40 While evidence supports use of acupuncture, including in primary care,41,42,45 less is known about the multilevel benefits of acupuncture as part of a comprehensive multimodal program for chronic pain.
We propose testing IGMVs and group acupuncture to improve pain management and to address multilevel barriers to guideline-concordant care for racially and ethnically diverse low-income patients seen in primary care safety net clinics. Our research seeks to: (1) Determine the effects of study interventions on pain-related outcomes (primary outcome: pain impact; secondary outcomes include pain intensity, pain interference, depression, physical function). (2) Assess the effects of study interventions on social factors related to chronic pain (primary outcome: social support in chronic pain; secondary outcomes: social isolation, stigma). (3) Examine multilevel impacts of study interventions on patient experiences with pain management, patient-clinician relationships, and clinical care in primary care safety net settings.
Methods
Study Context and Framework
An interprofessional team at the San Francisco Department of Public Health (SFDPH) developed and tested an Integrative Pain Management Program (IPMP) as a quality improvement project. 46 Using a biopsychosocial model, IPMP provided multimodal pain management embedded in primary care through integrative group visits; individual and group acupuncture; massage therapy; health coaching; and therapeutic movement. 46 IPMP development was informed by focus groups with primary care staff, patient needs assessments, and iterative feedback from patients who participated in the program. 46 A quasi-experimental study found that IPMP participants experienced decreased pain interference, increased pain self-efficacy, and greater social support from pre to post intervention. 27 Qualitative findings highlighted pain relief through social connection with group members, feeling understood by people who also experienced pain-related stigma, and new capacity for empathy and ease with other people. 28 We sought to better understand which program components accounted for observed benefits.
For the current study, we are evaluating 2 components of the original IPMP program: 1) integrative group medical visits (IGMVs) with pain education, social and behavioral support, and mind-body approaches (meditation, yoga) and (2) group acupuncture. These were selected based on their potential to be widely implemented in primary care and the potential of group-based interventions to improve psychosocial factors in chronic pain management. We propose group-based integrative pain management as a multilevel intervention, as illustrated in Figure 1, adapted from Purnell et al.
47
A Multilevel Approach to Improving Pain Management in Primary Care Safety Net Clinics (adapted from Purnell et al, 2016). Barriers to optimal pain care exist at the organizational, interpersonal, and individual levels. We propose group-based integrative pain management to address these multilevel barriers. We hypothesize that the study interventions increase access to non-pharmacologic therapies, address time constraints that contribute to disparities in pain management, improve interpersonal communication, foster belonging and social connectedness, and improve pain-related outcomes.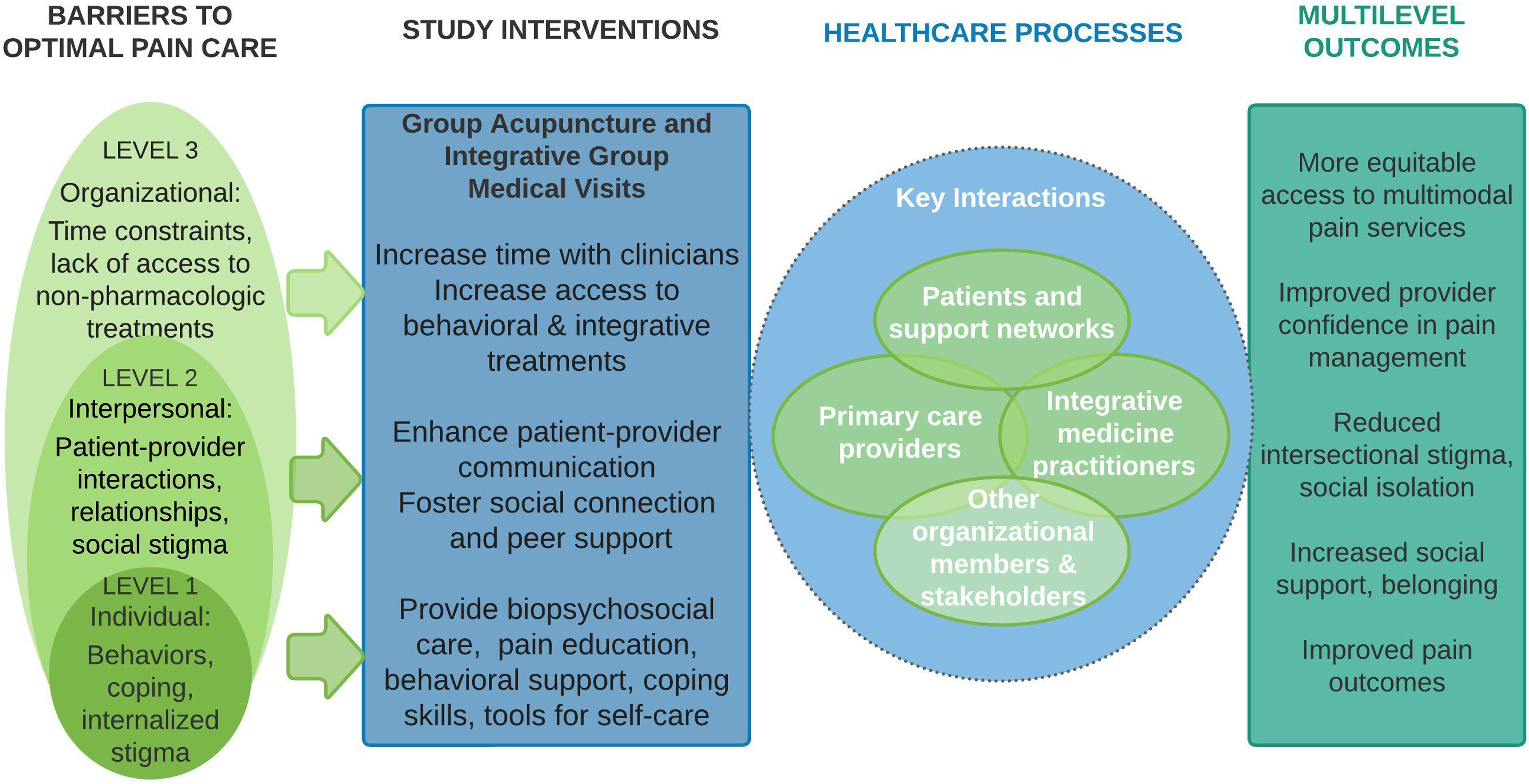
Study Design and Intervention Development
Group-Based Integrative Pain Management 2x2 Factorial Study Design.
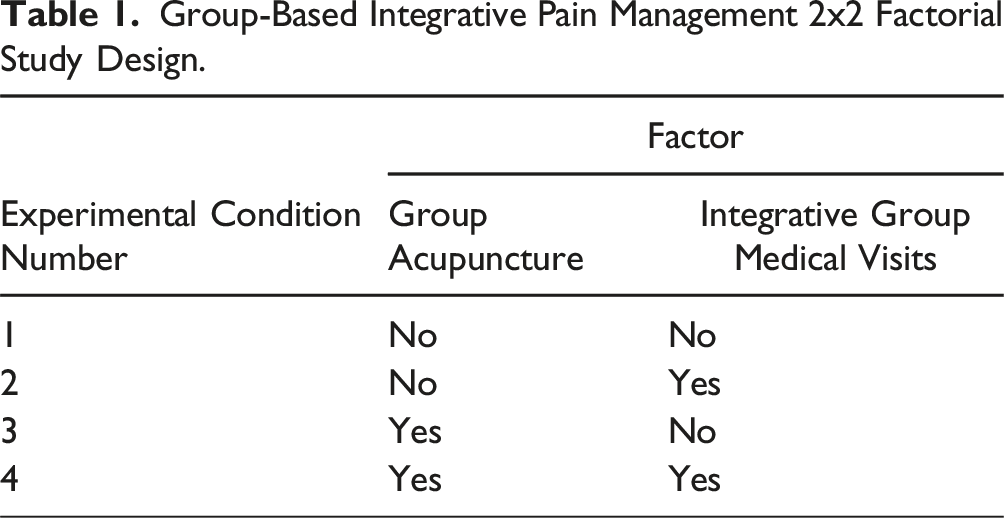
In 2022 as part of a phased award funded through the National Institutes of Health HEAL Initiative, we refined and optimized the study interventions with the goals of: (1) explicitly addressing social isolation and intersectional stigma through community engagement, (2) manualizing core and modifiable components, and (3) translating and adapting for Spanish speaking patients. To achieve these goals, we held a series of meetings to finalize study protocols. For the IGMV intervention, we convened 2 expert panels and prior IPMP group facilitators to inform intervention development. The first panel, which included 5 national experts in implementing IGMVs in safety net clinics, met 4 times to focus on core and modifiable elements of IGMVs, and on how to explicitly address intersectional stigma and social isolation. Transcripts of the meetings were reviewed and summarized for recommendations on addressing intersectional stigma and social isolation through structure, process, and content of IGMV. We convened a second panel of 5 consultants with expertise delivering IGMVs in Spanish. These meetings included reviewing materials from a Spanish IPMP pilot that was interrupted by the COVID-19 pandemic and discussing cultural and linguistic adaptations.
For the group acupuncture protocol, we met with 4 licensed acupuncturists, each with over a decade of experience providing group acupuncture treatments to diverse patients. We discussed their clinical practices for treating chronic pain, acupuncture point selection, how they aligned or diverged from 1 another and from existing group acupuncture study protocols.41,43,48 We discussed strategies for reducing stigma and providing social support during group acupuncture based on our pilot work and prior research.40,44 We reviewed chart notes from 50 acupuncture treatments delivered as part of a pilot for the current study to evaluate treatment principles, point selection, and other key details of acupuncture delivery. We also conducted a focus group with patients who had graduated from IPMP (n = 8, 50% people of color) to elicit patient input on both interventions. Clinical and research consultants and a patient advisory group will continue to provide feedback throughout study implementation.
Setting and Participant Recruitment
The upcoming study will be conducted at primary care safety net clinics in San Francisco, California. Sites were selected based on their diverse patient populations and the feasibility of delivering the study interventions, with support from clinic leadership committed to expanding access to integrative pain management and to providing accessible, culturally responsive care. Leveraging the strength of existing community and clinic resources supports the feasibility of the research and is an important strategy for sustainability beyond the study. 49
Study participants will include racially and ethnically diverse, socioeconomically disadvantaged patients of primary care safety net clinics in San Francisco. Inclusion criteria are adults aged ≥ 18; fluency in English or Spanish; paneled to a primary care provider at 1 of the study clinics; diagnosis of chronic pain ≥ 3 months; primary care visit for chronic pain within the past 6 months; ability to provide a phone number; able to participate in groups; intent to be available for up to 24 weeks. Exclusion criteria are active cancer treatment, inability to provide informed consent due to mental illness or cognitive impairment, acupuncture treatment for pain or participation in pain groups in the past 3 months.
All primary care providers at study sites will be informed about the study and invited to refer eligible patients. We will also generate a list of patients from SFDPH clinics based on ICD codes for chronic pain and other eligibility criteria. We will then contact primary care providers to approve or decline eligibility of their patients for the study. Clinical research coordinators (CRCs) will contact patients by telephone to gauge interest in participating in a study on group-based pain management in primary care, confirm eligibility, and invite eligible patients to participate in an orientation session.
To support participant recruitment and retention, gift card incentives will be provided for each data collection timepoint. Refreshments will be offered at study visits. Reminder messages will be sent prior to each visit. Additional outreach will be conducted for participants more than 10 days late for scheduled follow ups.
Study Procedures
Study staff will include CRCs, primary care and mental health clinicians, and licensed acupuncturists. Bilingual staff will implement study procedures with Spanish-speaking participants. All study staff will be trained in human subjects research, cultural humility, patient-centered care, key concepts in integrative health equity, and strategies to reduce bias and stigma (eg, perspective taking). Additional training will be provided to staff based on role. For instance, IGMV facilitators and acupuncturists will be trained in research principles of reproducibility, intervention fidelity, and protocol consistency. Staff involved in qualitative research will receive training in interview skills, participant observation, and qualitative data analysis.
The research team will host group orientation sessions in Spanish and in English for prospective participants who have been pre-screened for eligibility. These sessions will provide an overview of the study procedures including data collection, randomization, and interventions; and provide prospective participants an opportunity to meet study staff and interventionists. Bilingual team members will ensure that English- and Spanish-speaking patients have thorough comprehension of what research involvement entails, including the voluntary nature of participation; and will allow for safe and high-quality experiences and accurate data collection. CRCs will obtain informed consent from patients who are interested in enrolling in the study. Written materials will be available in both English and Spanish.
Following the consent process, a 45-60 minute baseline assessment will be administered using a tablet computer and Qualtrics,
50
a web-based software that facilitates the creation and distribution of surveys. To support individuals with different levels of literacy and to minimize participant burden associated with data collection, participants will have the choice of completing surveys on their own or aloud with a research team member. After completion of the baseline survey, participants will be randomized using a computer-generated list with randomly permuted blocks of 4 and 8, stratified by language. The database manager, who will not be involved with enrollment, will program the random allocation sequence; no other study staff will have access to generating the randomization sequence. The CRCs will access the allocation sequence using a programmed database that cannot be altered once randomized condition is revealed. Study participants will be randomized to 1 of 4 experimental conditions: (i) Usual care (waitlist control). Participants will receive care as usual through their primary care providers. Usual care includes medical diagnostic evaluation, analgesic drug therapies, recommendations for physical activity, and sometimes referral to physical therapy or other clinical services. Usual care was chosen as a comparison arm for this study because it is practical and clinically relevant. One challenge with using a usual care arm in a clinical trial is the potential variability in the care provided.
51
EHR data will be extracted and reviewed to accurately describe usual care for study participants. To reduce disappointment bias, participants randomized to usual care will have the option to receive IGMV or group acupuncture after 6 months. (ii) Integrative Group Medical Visits (IGMVs) for Pain. The IGMV structure, process and content were developed based on chronic pain treatment guidelines; feedback from clinicians, and patient and consultant input. IGMV will consist of a 12-week, in-person program located at primary care clinics and offered in English and in Spanish. Each session will include education on the biopsychosocial model of pain and multimodal treatments; gentle physical movement; mind-body practices; and peer support through facilitated discussion. Weekly, two-hour IGMV sessions will be co-facilitated by 2 or more clinic staff including a primary care or behavioral health clinician, as well as a facilitator with training in therapeutic movement and mindfulness. The group structure and process will focus on cultivating supportive peer relationships and reducing pain-related stigma, as well as providing tools for pain self-management, and psychoeducation on topics including neurobiology of pain, medication safety, and connections between mood and pain (see Table 2 for sample content based on prior IGMV).46,52,53 Participants will receive a binder with educational materials. To monitor intervention fidelity, IGMV facilitators will complete surveys with questions on content covered, time spent on each core component, open ended questions on group dynamics and any protocol deviations after each session. Additionally, a trained CRC will observe at least 3 sessions of each cohort and take structured field notes on intervention delivery. We anticipate offering 3-4 English cohorts and 2-3 Spanish cohorts of IGMV per year. (iii) Group Acupuncture. Acupuncture was selected based on: (1) strength of supporting evidence and inclusion in clinical guidelines for pain management,24,34,35,52,54 and (2) high acceptability and feasibility among safety net patients with chronic pain. Participants randomized to acupuncture will receive 12 weekly sessions of acupuncture treatment delivered in a group setting. Acupuncture will be offered 2 afternoons per week; participants can choose which session to attend based on individual availability. Acupuncture point selection follows responsive manualization, using points developed for the protocol of the largest RCT of group acupuncture conducted in the U.S. to date, the Acupuncture Approaches to Decrease Disparities in Outcomes of Pain Treatment (AADDOPT-2) trial.
48
The protocol uses acupuncture points accessible in a group context; participants are instructed to wear comfortable loose fitting clothing. Licensed acupuncturists (LAcs) with a minimum of 5 years of licensure and experience with group acupuncture will provide treatments. Due to limited availability of licensed acupuncturists who are bilingual in Spanish and English, interpreters may be used for Spanish-speaking participants randomized to acupuncture. The LAc will interview participants using standard questions for pain assessment and traditional East Asian medicine diagnosis and use palpation as part of evaluation and treatment. LAcs will use the AADDOPT-2 point selection based on location and level of participant’s pain, and administer 4-20 acupuncture needles per session. Duration of assessment, needle placement and retention will be 35-55 minutes. Details of acupuncture treatments – needle retention time, session duration, intake, number of needles and points used and other items recommended in STRICTA guidelines
55
– are provided in Table 3 and will be documented in standard EHR charting.
56
To monitor intervention fidelity, acupuncturists will complete session forms on protocol adherence, any protocol deviations, and rationale. As with IGMV, a trained CRC will observe at least 3 sessions of each cohort and take structured field notes on intervention delivery as part of assessment of multilevel effects. (iv) Both group acupuncture and IGMV. Along with usual care, participants in this study arm will be offered weekly group acupuncture treatments and integrative group medical visits as described above. Both treatments will be offered on the same day to reduce the number of trips necessary for study visits. Sample Content for Integrative Group Medical Visits. aFour core components – psychoeducation, mindful movement, skills practice, and peer support through facilitated discussion – are included as part of every IGMV session. Group Acupuncture Intervention Details Based on STRICTA Guidelines. Notes: STRICTA = STandards for Reporting Interventions in Clinical Trials of Acupuncture; AADDOPT = Acupuncture Approaches to Decrease Disparities in Outcomes of Pain Treatment; IGMV = integrative group medical visit.


Measures
We will test the hypotheses that compared to usual care, group acupuncture and IGMV improve pain management among diverse socioeconomically disadvantaged patients with chronic pain. The study will assess core outcome domains recommended by the Initiative on Methods, Measurement, and Pain Assessment in Clinical Trials (IMMPACT) for trials of chronic pain,
57
and core pain domains of the HEAL Initiative Common Data Elements at baseline, 3-month, and 6-month follow up. Outcomes include the following: ∙ Pain impact (primary outcome of interest), a combination of 9 items from NIH Patient Reported Outcomes Measurement Information System (PROMIS) measures on pain intensity, pain interference with normal activities, and physical function.
58
Pain impact is recommended by the NIH Task Force on research standards for chronic low back pain and is relevant for other types of chronic non-cancer pain.
58
People experience pain in multifaceted ways and a composite measure can provide a comprehensive assessment that is more clinically relevant than single measures.
59
∙ Secondary patient-reported, pain-related outcomes: individual constructs of pain impact (ie, pain intensity, pain interference, physical functioning), depression, and anxiety using PROMIS Short Form measures (v1.1 Pain Interference 8a, v2.0 physical functioning 6b, v1.0 Depression 4a, v1.0 Anxiety 4a).60-62 ∙ Social factors related to pain: social support in chronic pain (co-primary outcome), a six-item measure of perceived support related to pain
63
; and PROMIS Short Form v2.0 Social Isolation 8a, an eight-item scale on lacking companionship, feeling left out, and feeling isolated.
64
∙ Internalized stigma of chronic pain (ISCP) scale, 21 items with 5 subscales on enacted and internalized chronic pain stigma: alienation, stereotype endorsement, discrimination experience, social withdrawal, and stigma resistance.
65
∙ Additional aspects of health-related quality of life using measures for sleep, social functioning, global physical, mental, and social well-being (PROMIS Short Form measures v1.0 Sleep Disturbance 6a, v1.2 Global Health). ∙ Pain beliefs and attitudes (Pain Catastrophizing Scale
66
and Pain Self-efficacy Questionnaire).
67
∙ Participant ratings of global improvement: a single item, seven-point rating on the Patient Global Impression of Change scale will assess minimal clinically important difference in changes in pain since enrolling in the study.
Descriptive covariates collected at baseline will include socio-demographic variables (age, sex, race and ethnicity, place of birth, level of education, household income, marital status, employment status, and health insurance status). We will also collect data on key constructs of interest including the Intersectional Discrimination Index, which measures anticipated, day-to-day, and major discrimination across multiple axes of discrimination (eg, racism, homophobia) to capture intersectional categories. 68 Participants’ self-management for pain (medications and nonpharmacologic approaches) and current substance use will also be collected. Clinical data including chronic pain diagnosis, concomitant conditions, and pain treatments will be obtained from participants’ medical records.
To examine the multilevel impacts of study interventions on patient experiences with pain management, patient-clinician relationships, and clinical care in primary care safety net settings, we will collect multiple forms of qualitative data throughout the study. This will provide an in-depth understanding of pain care at multiple levels, as well as ongoing assessment of intervention fidelity. Interview and focus group questions have been developed based on existing literature and our past studies of IGMVs and group acupuncture, with a focus on the social aspects of pain.28,44 We will finalize questions with input from our consultants and patients. (1) (2) (3) (4) (5)
Sample Size and Data Analysis
Quantitative Data
We hypothesize an
Our analytic sample of 360 primary care patients with chronic pain will be randomized to N1 = 90 (usual care), N2 = 90 (integrative group medical visits - IGMV), N3 = 90 (group acupuncture), N4 = 90 (IGMV + group acupuncture). A key distinction of factorial trials is that main effects compare the means of a set of conditions. Traditional RCTs generally have a single control group. With factorial experiments the comparison group depends on which main effect is being estimated. Since each main effect and each interaction is based on all study participants, a key strength of factorial design is its efficient use of power. We will assess main effects in intent-to-treat analysis with n of 180 in each group [eg, acupuncture (N3 + N4) vs no acupuncture (N1 + N2) and IGMV (N2 + N4) vs no IGMV (N1 + N3)]. We define per protocol as participants who have completed at least 6 intervention visits among those randomized to an arm receiving study interventions. We estimate a sample of 220 for per protocol analysis.
Baseline characteristics of participants, including sociodemographics and clinical descriptives, will be summarized to determine sample generalizability, and compared to assess group equivalency. Treatment effects will be estimated using a repeated measures ANCOVA approach. The framework is similar to linear mixed models but it includes the baseline of the outcome as a covariate (and omits the baseline from the outcome vector), and the models will include indicators for assignment to acupuncture, IGMV, a categorical variable for time, and interactions between treatment indicators and time, as well as random intercepts for person nested within group to account for within-group and within-patient correlation of the repeated measures. We will assess a three-way interaction between the 2 treatment indicators and time to assess for synergy between IGMV and group acupuncture. We will also calculate an interaction ratio to assess clinically meaningful antagonism or synergy between the 2 interventions, specified as interaction ratios of ≤0.80 or ≥1.25. 69 Our primary models will assess marginal effects of each intervention, with models that omit the three-way interaction term, to focus on main effects of each treatment type. This approach will optimally weight data for patients with different numbers of responses, and will provide valid estimates in the presence of missing data under relatively mild assumptions about how the missing data arise. 70 We will use models including the 3-way interaction between time and the 2 treatment indicators to estimate effects of each treatment within levels of the alternate treatment, as a sensitivity analysis. We will conduct intent-to-treat, per protocol, and complier average causal effects analyses; and exploratory as treated analysis (receipt of any group integrative health intervention and dose-response based on number of sessions attended). Outcomes will be normalized as needed to meet model assumptions; for outcomes which do not meet distributional assumptions of normality, other generalized linear mixed models or non-parametric approaches such as Kruskal-Wallis tests will be used. Secondary outcomes will also be analyzed using this approach.
Qualitative Data Analysis
Qualitative data will be rigorously analyzed using well-established approaches. After each qualitative data collection episode, research assistants will take brief, structured notes focused on study implementation and fidelity. These notes will include 3 categories: what is going well, opportunities for improvement, and insights from the interview, focus group or observation. Study team members will compare and discuss these notes during team meetings to concurrently improve study implementation and begin early qualitative analysis. On a quarterly basis, we will synthesize these notes to create “lightning reports”, 71 an accessible summary of interim findings that will be shared with the intervention team and broader groups of stakeholders (eg, patient advisory group, clinic administrators).
All interviews and focus groups will be digitally recorded and professionally transcribed. Transcripts will be de-identified before formal data analysis begins. Transcripts and field notes will be organized and analyzed using Dedoose, 72 a database application for managing, analyzing, and presenting qualitative and mixed method research data. A codebook will be developed through an iterative process known as flexible coding, 73 combining inductive and deductive codes. Coders will confer at regular intervals after initial coding of every 2-4 interviews to refine the coding structure. Field notes from interviews and observations will also be included in the analysis. Once the coding structure has been finalized, the research team will independently code all interviews and field notes and adjudicate any discrepancies in coding through negotiated consensus.
Codes will be assigned by each team member to the narrative text using Dedoose. In accordance with principles of flexible coding, we will begin with “index coding” across large sections of text to facilitate data reduction. We will then use more focused codes for subsections of interviews. The ability to match qualitative data with individual participants’ survey responses will allow us to conduct mixed-methods analysis with a nuanced analysis of multilevel contextual factors related to pain, social isolation, and intersectional stigma. The lightning report approach will facilitate frequent study implementation feedback while the flexible coding approach will support in-depth data analysis for multiple areas of interest. 74
Discussion
This study protocol offers 2 primary innovations: (1) a focus on the ‘social’ elements of biopsychosocial pain care, and (2) a multilevel approach to conceptualizing and researching pain management in diverse, socioeconomically marginalized individuals. Our study interventions directly target social aspects of the biopsychosocial model with a focus on addressing social isolation and intersectional stigma. Most pain treatments focus on alleviating physical symptoms or improving psychological coping. Social factors such as social isolation and stigma are acknowledged as an essential part of the biopsychosocial model, but few chronic pain interventions directly address them. We use a multilevel approach to address pain care disparities, with potential to improve individual-level pain outcomes, interpersonal-level relationships (patient-clinician, peer-peer), and community-level access to guideline-concordant pain care. This approach is guided by a multidisciplinary team of clinicians and researchers who have identified the potential of group-based pain management interventions to reduce stigma, social isolation and loneliness, and increase social support and belonging. 75
Addressing inequities in care for chronic pain requires intervention at multiple levels. Factors such as time constraints during appointments, limited access to multimodal and nonpharmacologic options, stigma and discrimination contribute to the unequal burden of chronic pain. Multilevel, multicomponent interventions are complex, with potential challenges during design, implementation, and evaluation. The effects of complex, ‘messy’ interventions targeting healthcare disparities may not be limited to individuals but can have broader public health impact. 76 We intentionally developed a pragmatic mixed methods design to bridge rigorous research and everyday practice, to collect patient and provider-level data, and to capture interactions between levels and draw meta-inferences. 77
Our clinical trial design uses a pragmatic approach focused on effectiveness and broad eligibility criteria, strengthening its external validity and generalizability. Inadequate enrollment of people of color and people with limited English proficiency has been a serious concern in clinical trials. Our study sites are urban primary care safety net clinics serving low-income patients from diverse racial and ethnic identities, and the interventions will be offered in Spanish and English.
Conclusion
This study is part of an important shift towards evaluating integrative health care among historically marginalized and underrepresented populations. Pragmatic clinical trials have an important role in addressing pain inequities as they occupy a space between rigorous “research, healthcare delivery, and the complexities of everyday life.” 78 We draw from multidisciplinary theoretical frameworks to further optimize nonpharmacologic options available in safety net clinics. In combination, this approach can advance the field of pain management through testing sustainable multimodal care in primary care settings and addressing inequities in pain care for socioeconomically marginalized populations.
Footnotes
Acknowledgements
The authors thank the many people who have contributed to the San Francisco Health Network’s Integrative Pain Management Program (IPMP), especially Barbara Wismer, MD and Kristina Leonadakis-Watts who launched the initial program, as well as the IPMP Steering Committee, integrative health practitioners, primary care and behavioral health clinicians, SFDPH primary care leadership, research staff, and all the patients who have participated in the program. This research is supported by the NIH HEAL Initiative Advancing Health Equity in Pain Management Program. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute for Minority Health and Health Disparities and the National Institute of Neurological Disorders and Stroke (K01MD015766, R61MD018333 and R33MD018333).
