Abstract
Background
Chronic pain is one of the most common drivers of healthcare utilization and a marked domain for health disparities, as African American/Black populations experience high rates of chronic pain. Integrative Medical Group Visits (IMGV) combine mindfulness techniques, evidence-based integrative medicine, and medical group visits. In a parent randomized controlled trial, this approach was tested as an adjunct treatment in a diverse, medically underserved population with chronic pain and depression.
Objective
To determine race-based heterogeneity in the effects of a mindfulness based treatment for chronic pain.
Methods
This secondary analysis of the parent trial assessed heterogeneity of treatment effects along racialized identity in terms of primary patient-reported pain outcomes in a racially diverse sample suffering from chronic pain and depression. The analytic approach examined comorbidities and sociodemographics between racialized groups
Results
At baseline, African American/Black participants had higher pain severity and had significantly different age, work status, and comorbidity profiles. RMANOVA models also identified significant race-based differences in the response to the parent IMGV intervention. There was reduced pain severity in African American/Black subjects in the IMGV condition from baseline to 9 weeks. This change was not observed in White participants over this time period. However, there was a reduction in pain severity in White participants over the subsequent interval from 9 to 21 week where IMGV had no significant effect in African American/Black subjects during this latter time period.
Conclusion
Interactions between pain and racialization require further investigation to understand how race-based heterogeneity in the response to integrative medicine treatments for chronic pain contribute to the broader landscape of health inequity.
Introduction
Chronic pain is one of the most common reasons adults seek medical care in the United States (U.S.). While estimates of chronic pain prevalence range from 11% to 40%, historically medically underserved populations often have higher rates of untreated chronic pain. 1 Chronic pain is a prototypical condition demonstrating marked health disparities stemming from racialization processes. It is also associated with other conditions, such as overall poor health and several comorbidities such as depression and insomnia.2,3
These extend to widely acknowledged racial healthcare disparities in the assessment and treatment of chronic pain management, wherein the healthcare experience is differentially beneficial based on one’s identity. Driving these trends, in part, are reports that some medical professionals hold false beliefs, rooted in slavery-era medicine, about pain and pain treatment in Black populations.4-6 For instance, past studies have shown that some clinicians see Black patients as less sensitive to pain than white patients.7,8 This bias manifests in differential and often inadequate care. Namely, clinicians are less likely to prescribe opioids to Black patients as compared to White patients.9-11 In contrast to these misconceptions, there is evidence that both hypervigilance 12 and other effects of racial discrimination13-15 play important roles in higher reported pain in Black populations. Provider bias itself may exacerbate chronic pain in racialized patients.
These phenomena, in concert with adverse consequences of opioid pain medication dependence, have increased interest in non-pharmaceutical therapies such as mindfulness-based interventions for both majority and minoritized populations.16,17 Common interventions practiced for chronic pain reduction include Mindfulness-Based Stress Reduction (MBSR), Mindfulness-Based Cognitive Therapy (MBCT), and integrative treatments that combine mindfulness techniques with other conventional and complementary therapies. Mindfulness elements are postulated to allow individuals to reframe experiences such as chronic pain by refocusing the mind on the present and increasing awareness of external surroundings and inner sensations. 18 Mindfulness meditation is associated with statistically significant improvements in depression, physical and mental health, pain self-efficacy, and sleep in majority White samples.17,19,20
However, the magnitude of health improvement from mindfulness trials varies across studies. Cross-sectional cohort studies of people engaging in long-term meditation practices find that higher levels of mindfulness are associated with lower pain intensity ratings and changes in the structure of brain regions related to pain perception. 21 Mindfulness intervention studies as a treatment for chronic pain have heterogeneous results overall. While some studies focus on specific types of pain such as low back pain,20,22 fibromyalgia 23 or chronic migraines, others broadly target chronic pain. Systematic reviews16,24 indicate that treatment of chronic pain with mindfulness interventions has moderate success, and more comprehensive research is needed to support a recommendation for the use of mindfulness meditation for any chronic pain symptomology. While mindfulness interventions are covered under some health insurance plans for certain conditions such as chronic low back pain due to the inclusion in several guidelines,25-27 provider recommendation varies and is still not common. In addition, despite the potential for effective pain management in minority populations which may suffer from elevated rates chronic pain, inclusion of minorities in mindfulness based interventions is relatively rare. 28
Another non-pharmacological intervention for treating chronic pain is an Integrative Medical Group visit (IMGV) where multiple patients are seen at once in a group setting. Within the environment of group medical visits, there is benefit from peer support from group members, increase self-management, and overall relationships built with both the clinician and other participants.29,30 Our prior work evaluating racially and ethnically diverse patients with chronic pain during group medical visits reported decreases in pain level, perceived stress, and depression as well as improvements in sleep quality. 31 IMGV, which combine integrative therapies such as MBSR and a medical group visit, have been particularly effective in managing and treating chronic conditions in diverse groups.30,32 We conducted a pilot study combining culturally adapted MBSR program (see methods for details) with a medical group visit for 20 low-income minority adults with chronic pain and comorbid depression in 2017 which indicated enhanced coping with chronic pain and improved sense of control over one’s health condition. 33 This model can be used as adjunct to standard care, particularly in underserved diverse, low-income populations with limited access to non-pharmacological therapies. 32 There are benefits to both the patients and clinicians participating in IMGV, with improvements in patient physical and mental health. 32 Our recent randomized control trial (RCT) assessed the effectiveness of an Integrative Medical Group Visit (IMGV) intervention compared to a Primary Care Provider (PCP) visit control in patients with chronic pain and depression in a 9-week single-blind two arm randomized control trial with a 12-week maintenance phase. 34 Participants (N = 155) were recruited from low income racially diverse neighborhoods surrounding Boston Medical Center and randomized (1:1) to either intervention (IMGV) or control group. Since the study took place in a racially and ethnically diverse communities in the Boston area, we felt was a priority to have a people of color deliver the intervention and (a Black certified MBSR facilitator) and act as research assistants, coordinators, and scientific advisor group. In this sample of predominantly low income racially diverse adults with nonspecific chronic pain and depressive symptoms, there were no group differences between the primary outcome of average pain level between the intervention and the control group. However, the IMGV group had fewer emergency department visits at 9 weeks, and this group reported reduced pain medication use at 21 weeks compared to controls. Further quantitative analyses, using machine learning, identified and characterized a predictive relationship between depression and chronic pain interference. This relationship was mediated by increased perceived stress, decreased pain self-efficacy, and reduced sleep quality, highlighting potential targets for attenuating the adverse effects of pain related depression on functional outcomes. 35 Given the known role of racialization in driving health and healthcare disparities, the present study sought to assess the moderating effect of racialized identity on the primary pain outcomes of the parent culturally adapted IMGV RCT.
Methods
The full methodology and initial findings of the parent RCT is available in prior publications. 36
Study Setting
The study was approved by the Boston University Medical Campus Institutional Review Board (IRB) and the community health center’s (CHC) research committees (IRB Approval Number: H33096). We registered this randomized controlled trial (RCT) in the international trial register [ClinicalTrials.gov: Identifier NCT02262377]. The RCT was conducted at an ambulatory primary care clinic in the outpatient building at Boston Medical Center (BMC) in Boston MA and at two community health centers: Codman Square Health Center (CSHC) and Dorchester House Health Center (DHHC). BMC and the two affiliated federally qualified health centers serve income-disadvantaged, racially diverse and ethnically diverse populations with health disparities in the treatment of chronic pain and depression. These locations were chosen because they are the setting where there is a high prevalence of income-disadvantaged diverse patients with chronic pain and depression who do not have access to non-pharmacological treatments. All three sites were accessible by public transportation.
Participants were recruited through Boston Medical Center and surrounding community health centers their clinicians’ outpatient referral, clinicians’ letter to patients about the study, or self-referral. After being contacted by the research assistant (RA), patients then consented to be screened. Our inclusion criteria included: age 18 years or older, able to communicate in English language, score of ≥5 on the Patient Health Questionnaire-9 (PHQ-9), score of ≥4 on a 0-10 scale measuring daily chronic pain intensity for at least 12 weeks, and having a PCP located at the site where the IMGV was being held. The exclusion criteria included: self-reported symptoms of psychosis or mania, active substance abuse (alcohol, cocaine or heroin use in the last 3 months), previous participation in an IMGV, a new pain treatment in the past month or plans to begin any new pain treatments in the next three months, active suicidality, any other severe disabling chronic medical or psychiatric co-morbidities preventing attendance to the IMGV, or no access to the internet during the study period. If the eligibility was verified and there was patient written consent, the patient was enrolled in the study.
IMGV Intervention
As previously reported, racially diverse patient advisors were very involved throughout the study serving on the Patient Advisory Group assisting with intervention development. 34 The IMGV intervention included three concurrent deliveries of the same self-management curriculum delivered with different formats–an in-person MGV, and two adjunct companion technologies available on a computer tablet provided to the intervention participant. The first technology was the Our Whole Lives (OWL), an e-Health toolkit platform, and the second technology was an Embodied Conversational Agent (ECA). A detailed description of the IMGV self-management intervention which was adapted from MBSR has previously been described. 34 The IMGV consisted of a total of ten in-person medical group visits each lasting 2.5-hour conducted weekly from week 1 to week 9 (9 in-person sessions plus OWL/ECA). This is followed by a 12-week maintenance phase where there is access to technology only (OWL/ECA). A tenth and final in-person session is conducted at week 21.
To ensure our intervention was culturally adapted, we used a patient advisory group (PAG) and community partners, from neighborhoods surrounding Boston Medical Center, to provide feedback on the curriculum content, visuals, and presentations. The Principal Investigator (PI) invited patients with chronic pain who had attended past IMGV groups to serve on the PAG. We asked our community health center champions to nominate patients to serve on the PAG, thus, we had a wide representation of perspectives. Patients with chronic pain and depression have contributed key insights by providing feedback throughout the IMGV pilot groups and through our PAG. PAG members provided valuable feedback on the development of group visit curriculum, study design, recruitment methods, data collection and data analysis. The study staff presented to the PAG all changes made as a result of their feedback to give them the results of their recommendations. Before the start of the Randomized Controlled Trial (RCT), as a result of PAG feedback, we altered the following: (1) added the Brief Pain Inventory; (2) excluded the marriage demographics question (the PAG felt patients would react negatively to it); (3) revised the IMGV curriculum (eg, added more pictures representative of the BMC patient population, information on tablet use, a new chair mindful movement protocol, and goal setting exercises); (4) improved our OWL website design (5) and revised the study logos and images for meditation assignments. Another example of PAG engagement was our analysis of the pilot focus groups. During this process, we presented de-identified data to PAG members and solicited their opinions in order to ensure our conclusions reflected their experiences as IMGV participants.31,33,37
At the beginning of each session of the IMGV, participants measured their vital signs, mood, and pain levels. They then met individually with a trained physician (a co-facilitator) for a medical assessment. A Black certified MBSR facilitator (see below) then led mindfulness practices adapted from Mindfulness Based Stress Reduction (meditation, body scan, etc.). Patients were instructed in the principles of mindfulness and other self-management techniques (such as acupressure and self-massage). Each week, the physician facilitated a discussion on health topics such as stress, insomnia, depression, chronic pain cycle, activity, and healthy food choices. Finally, the IMGV ended with a healthy meal, which mirrored the healthy nutrition topic in each session. A physician and an experienced co-facilitator with training in mindfulness (certified MBSR instructor, yoga, and meditation teacher) attended all groups. Facilitators were mentored via direct observation of two pilot group visits, one-on-one meetings, and phone calls by an experienced MBSR trained faculty.
To reinforce all content delivered in the in-person group, OWL delivered the same in-person curriculum. OWL was accessed with a computer, smart phone, or tablet. The ECA, an automated female character, emulated the conversational behavior of an empathic coach. The ECA (Gabby) reviewed all the content discussed in the IMGV with the participants outside of the in-person group. A Dell Venue 8 Pro tablet was distributed to all intervention participants in the first session of the group.
After the 9-week in-person group visit phase concluded, the intervention participants entered a 12-week maintenance phase. The intervention participants retained the study tablet and continued to have access to the ECA and the OWL website. At the end of the 21 weeks, there was one final in-person group visit. A trained study RA directly observed all groups and assessed the facilitator’s adherence to the intervention components through a monitoring and evaluation checklist. These checklists were used to assess each IMGV session at all sites during the study.
Control Condition
All participants randomized to the control group were asked to visit their PCP during the study period (baseline to 21 weeks). We verified a PCP clinical visit via electronic medical record (EMR) documentation. We did not collect data on the duration or content of the visit.
Clinical Outcomes
Outcome data were collected at baseline, 9 weeks, and 21 weeks. Baseline demographic data included: age, gender, racial identification, ethnicity, income, work status, and education. Our primary outcomes included in the present analysis consist of: (1) self-reported pain measured by the Brief Pain Inventory (BPI) (pain interference, pain severity, and average pain score in the last 7 days) 38 and (2) depression level measured by the PHQ-9, a self-reported depression screen. 39 BPI pain interference, and pain severity are on a 0-10-point scale. The higher the score, the more severe the pain. PHQ-9 is on a 0-27-point scale. The higher the score, the more severe the depression. Secondary outcomes included were perceived stress. The Perceived Stress Scale (PSS) is a self-reported questionnaire designed to assess “the degree to which individuals appraise situations in their lives as stressful.” 40 Data on interpersonal discrimination, perceived racism and related trauma were not collected.
Analytic Plan
One-way ANOVAs were performed to evaluate differences in separate pain outcome values by participant race at each time point. Pain outcome values (interference, severity) were then each analyzed separately using a 2(condition)× 2(race)× 3(time) mixed analysis of variance, with repeated measures at on the third factor (baseline, 9 weeks, and 21 weeks). That is, the interaction between study condition and participant race was tested in relation to the trajectory of pain outcome values across the study observation period.
Demographics Split by Race Variables.

Note. sd = standard deviation.
adenotes significance (P < .05).
bComorbidity Profile includes hypertension, obesity, insomnia, diabetes, vitamin D deficiency, PTSD, and substance use disorders (alcohol, tobacco, opioid, cocaine, marijuana).
Results
Three hundred forty-three patients were assessed for eligibility. Of these, 209 patients were eligible, and 159 were enrolled and randomized to intervention (n = 80) or control. The consort diagram and baseline characteristics were previously published. 34 Of the 159 participants, 58% self-identified as African American/Black and 19% as White participants. All participants were experiencing chronic pain and depression at baseline. The average PHQ-9 score for depressive symptoms was 11.9 at baseline, which is characterized as moderate depression. The average age was 51 years old, and 86% identified as female. Sixty three percent earned less than $30,000 a year. Only 21% worked full or part time; 14% were unemployed; and 42% were on work disability. Common comorbidities in this sample were hypertension (41%), insomnia (26%), anxiety (28%), Post-Traumatic Stress Disorder (PTSD) (16%), and any substance use disorder (25%).
Demographics Split by Race and Treatment Group.

Note. sd = standard deviation.
adenotes significance (P < .05).
bComorbidity Profile includes hypertension, obesity, insomnia, diabetes, vitamin D deficiency, PTSD, and substance use disorders (alcohol, tobacco, opioid, cocaine, marijuana).
Descriptive Statistics and ANOVA Results of Pain Differences by Race.
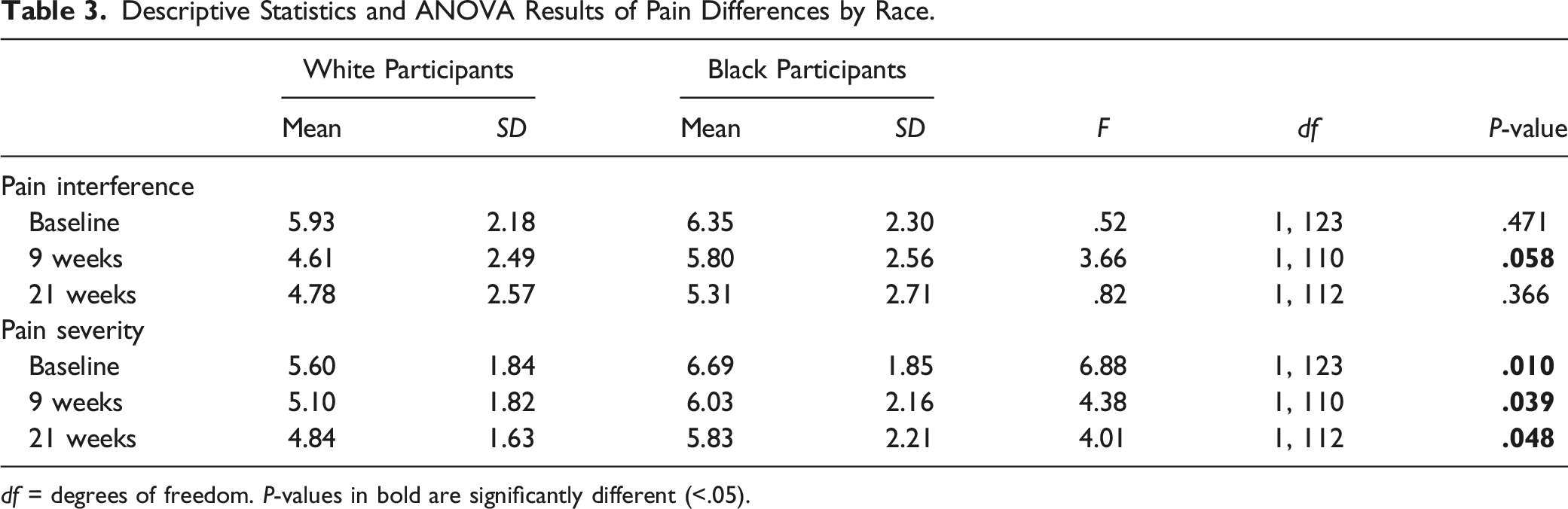
df = degrees of freedom. P-values in bold are significantly different (<.05).
Pain Interference and Severity Over Time by Treatment Condition and Race.

df = degrees of freedom. P-values in bold are significantly different (<.05).

Pain Severity Across Treatment Groups. * denotes differences by race at each timepoint (P < .05). # denotes significant overall interaction between pain severity, treatment condition and race (P < .05). African American/Black-identifying participants denoted here as “Black.”
Discussion
The current analysis revealed marked group differences in the effects of the IMGV for chronic pain severity based on racialized identity. African American/Black subjects experienced higher pain severity at baseline compared to White subjects. While they experienced an initial decrease in pain severity during the intervention, there was no additional benefit through the follow-up period from 9 to 21 weeks. In contrast, White participants experienced a further decrease in pain severity during the follow-up period. This suggests that African American/Black groups may experience less benefit from interventions such as this. Although many mind-body interventions for chronic pain are generally effective, these findings underscore a critical need for a greater understanding of their efficacy in African American/Black patients and other minoritized groups.
Despite the increased need for effective pain management and an intervention targeted at high-risk African American/Black communities, the current analyses between racial groups revealed that African American/Black subjects had higher pain severity at every time point compared to White participants, highlighting a persistent health disparity. This is consistent with findings from other interventions. 41 Higher severity may be due to social factors including stress levels, 42 structural and systemic racism, and higher comorbidity. Additionally, these analyses did not account for income, stress level, or housing insecurity, which may also play roles in how minoritized groups respond differently to pain as well as treatment, over and above more generalized measures of SES. However, we do note that all these factors in concert form the complex social pathways that drive racialization and define the daily experiences and health trajectories of racialized and minoritized individuals. Thus, it is impossible to extricate them from one another as they all create the racialized experience.
Two longitudinal observations may help explain the differential pain trajectories between African American/Black and White patients observed in this study. First, both African American/Black and White control subjects reported decreased severity over the first 9 weeks, which could be related to the PCP visit and/or an effect of enrolling in the study. While this decreasing trend continued in the African American/Black control subjects, pain severity plateaued in White control subjects. Second, in the IMGV treatment groups, severity plateaued in African American/Black between 9 and 21 weeks during the maintenance phase, where it decreased in White subjects. In sum, the data from the IMGV groups suggests increased efficacy in White participants during the maintenance phase from 9 to 21 weeks. This suggests that in this group, the intervention could be viable and advantageous in the long term. However, this effect was not observed in the African American/Black participants. It may be that the White patients had more resources and support to maintain their mindfulness practice and therefore continue reaping the benefits. The combination of these differences in control and treatment trajectories, combined with the overall higher pain severity in African American/Black, contributed to the interaction between severity, treatment, and our dichotomized race variable. Factors which may be involved in the longitudinal divergence in pain trajectory are comorbidities, digital health literacy, structural racism and a severity dependent response to IMGV, as discussed below.
The present analyses indicate that African American/Black patients were significantly more likely to suffer from multiple comorbid diagnoses. Three or more comorbidities were observed in 58% of African American/Black participants compared to 28% of White participants. This finding is consistent with the broader healthcare disparities literature and points toward race-based disparities in comorbidities as an important consideration potentially contributing to the observed heterogeneity of treatment effects. For instance, in a study of nearly 6000 patients with COVID-19, African American/Black patients suffered higher prevalence rates of more than two comorbidities compared to White patients. 43 Depression further complicates this scenario. In one study of over 32,000 Black and White adults, Black participants with major depressive disorder had significantly higher odds of several comorbidities (such as sleep disturbances), which may promote underutilization of treatment and greater likelihood of hospitalization. 44 All of this is compounded in the context of chronic pain. Indeed, medical comorbidities have been posited as a chief complicating factor in assessment and treatment of chronic pain in African American/Black patients. 45
We also note the nonsignificant trend in education level, which may perhaps speak to known digital literacy competencies in healthcare, where African American/Black patients are disproportionally affected by these challenges. 46 This echoes a growing concern about digital health literacy accentuating current race-based healthcare disparities. 46 Black and Latino populations are disproportionally affected by challenges in health literacy in general, and racial minorities are less likely to use patient portals, even when adjusting for educational attainment. 47 A 2022 systematic review of qualitative studies of telehealth interventions for people with chronic pain concluded that health literacy was a critical barrier. 48 Encouragement of self-efficacy and empowerment of patients were associated with successful telehealth interventions for chronic pain management.
Structural racism, a power-based value system driven by both norms and laws is likely also at play. Here, this system serves as arbiter of opportunities and places value based on how society interprets one’s physical appearance. This cause of chronic stress and trauma may underlie the observed differences in IMGV intervention response between Black and White participants.49,50 Structural racism is often modeled as a predictive factor which creates the experience of racialization, 51 which in turn moderated the intervention effect. This is consistent with work demonstrating that racism in general and related trauma are preventable sources of chronic pain and related comorbidities.52,53 Highlighting the shared mechanisms between both racism and chronic pain, in fact there is evidence that the adverse effects of both racism and chronic pain are mediated in the brain. The concept of racism as a source of pain is especially relevant to the present discussion, where the mindfulness and social elements of IMGV also affect neural mechanisms which may be inhibited by structural racism. However, the present data source lacked sufficient granularity to test racism and racialization as a driving force in the observed differences.
Another hypothesis for the racial difference in the response to IMGV is that this intervention is more effective at treating lower pain severity and patients with no or mild depression, where higher severity requires other treatments, such as medication.54,55 The greater severity also indicates levels that may be more resistant to treatment in general. 56 Careful consideration and implementation of particular facets of mindfulness in customized pain interventions, rather than the use of standardized mindfulness protocols, may improve outcomes for all groups. There is clearly potential for interactions between several factors, including comorbidities, digital health literacy, and racism to affect the levels and trajectory of pain severity in the present and similar studies.
While the current findings are consistent with some previous literature, they do conflict with other work. For instance, a meta-analysis of the effects of racialized identity in mindfulness and acceptance based interventions for depression reported no moderation by the race variable, 57 contrasting with the present study. This is particularly noteworthy given the prior report of the predictive relationship between depression and chronic pain in the IMGV data. 35 This could indicate that aspects of the group medical visits and/or the maintenance phase protocols were key factors in the race-based difference in pain severity trajectories. The presence of the greater divergence in trajectories during the maintenance phase, which involved interaction with the ECA and OWL website (and related digital health literacy), suggests that differential responding during this period was the more substantial factor.
Limitations
The study sample had insufficient representation from other minoritized groups to test for differential treatment effects beyond the African American/Black vs White dichotomy. We were also unable to assess racism, structural racism, or experiences of discrimination as a predictor of racialization, as discussed above. This repositioning of the model – where racism is a predictor of one’s experience of “race,” rather than the other way around – has been recommended specifically for studying the health effects of structural racism in an integrated, biopsychosocial lens. 58 We were similarly unable to look at the interactions with other sociodemographic factors in the analysis to address which demographic factors influence pain severity at a more granular level. A final limitation is the lack of data on participant digital health literacy levels, where racial differences in this factor may have affected the results. Suggestions for future research include larger, more diverse study samples, more comprehensive assessment of other factors that affect pain severity such as catastrophizing and digital health literacy, and the inclusion of longitudinal manipulative studies of omitted factors to determine causality. In particular, it is important to understand drivers of racialization to be able to examine racialized identity as a mediator of these outcomes, rather than a moderator of the observed heterogeneity of treatment effects.
Conclusion
The present analysis indicates that overall efficacy in the associated RCT of IMGV differed by racialized identity. Black subjects suffered from higher pain severity throughout the 21 weeks of the study. Where IMGV reduced pain severity in African American/Black subjects from baseline to 9 weeks, it had no effect in White participants during this period, however, there was a reduction in White participants from 9 to 21 weeks. Racial disparities in pain affect not only the experience of pain, but also how individuals respond to mind body interventions. Due to the urgent need for effective pain management interventions targeted at high-risk populations, increased emphasis should be directed towards aspects of both pain and the response to interventions to address disparities. There is an imminent need for additional studies on the effects of dynamic social factors on differential responses to mindfulness based interventions. This is essential to equitably advance the science of complementary and integrative medicine models for chronic pain, reduce healthcare disparities in pain treatment, and ultimately dismantle longstanding health disparities for racialized groups.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded through a Patient-Centered Outcomes Research Institute (PCORI) Award AD- 1304-6218. The statements in this work are solely the responsibility of the authors and do not necessarily represent the views of the Patient-Centered Outcomes Research Institute (PCORI), its Board of Governors or Methodology Committee. Patient-Centered Outcomes Research Institute (PCORI) Award AD- 1304-6218. NCT from clinicaltrials.gov: 02262377 and NINDS award 1UG3NS135168-01.
Trial registration
NCT from clinicaltrials.gov: 02262377
