Abstract
Background
Granular cell tumor (GCT) is a very rare, slow-growing, benign neoplasm with a controversial etiology, recently believed to be derived from Schwann cells. Hardly grows large and is also infrequently seen in children. Seventy percent of this tumor is seen in the head and neck with 1/3 in other parts of the body. Seldom occurs in the parotid gland and more so, the deep lobe of the parotid, where it may initially be asymptomatic but when large, it may result in respiratory obstruction.
Case report
Conclusion
Granular cell tumor is a rare neoplasm, treatment is local surgical excision. Recurrence is uncommon, even if the lesion is not entirely removed. Microscopically this tumor may mimic a malignancy because of pseudoepitheliomatous hyperplasia of the overlying epithelium. The pathologist should be aware of this possibility to avoid a mistaken diagnosis of cancer.
Introduction
The deep lobe of the parotid gland is a rare location for tumors of the head and neck, most especially in children, and when encountered they are most of the time pleomorphic adenoma. 1 Granular cell tumor (GCT) or granular cell myoblastoma is an uncommon mesenchymal tumor with an uncertain histogenesis that may occur in any organ but has a predilection for the oral cavity. 2 Abrikossoff in 1926 presented the first report of this lesion, and because its cells are in an intimate relationship with adjacent skeletal muscle, he proposed a myogenic origin for this lesion, recently, however, some authors suggest the lesion is most likely derived from Schwann cells.3,4 The common appearance is a solitary asymptomatic firm nodule, rarely more than 2 - 3 cm in diameter, involving subcutaneous or submucosal tissues. Parotid gland GCTs are rare and seen most frequently in young to middle-aged adults with 2:1 female predilection. 2 Most of the time, patients are not aware of the lesion for a long time before diagnosis.
Case Presentation
An 8-year-old female presented with right lateral upper neck-facial swelling of 3 months duration with associated change in voice, difficulty swallowing, and respiratory distress. The swelling was initially the size of a grain, then slowly, progressively increased in size with no pain, bleeding, pus discharge, or ulceration. No similar swelling in any other parts of the body. She was otherwise healthy with no remarkable medical history. Physical examination of head and neck revealed a large solitary firm swelling, non-tender, non-adherent to the intact overlying skin, not fixed, with visibly palpable overlying neck and facial vessels (Figure 1) No paresis/paralysis of branches of the facial nerve or enlarged lymph nodes. The right external auditory canal and right tympanum were normal. Intra-orally the tumor could be seen projecting from the right lateral wall of the oropharynx, crossing the midline and obliterating the oropharynx, with intact overlying oral mucosa. An ultrasound scan revealed a huge well-defined hyperechoic mass over 7.3 cm x 5.27 cm in the right lateral aspect of the neck, displacing the right carotid and its main branches inferiorly and compressing the superficial parotid gland. Fine-needle aspiration cytology was not contributory. Patient with a large tumor at the right lower jaw—upper neck region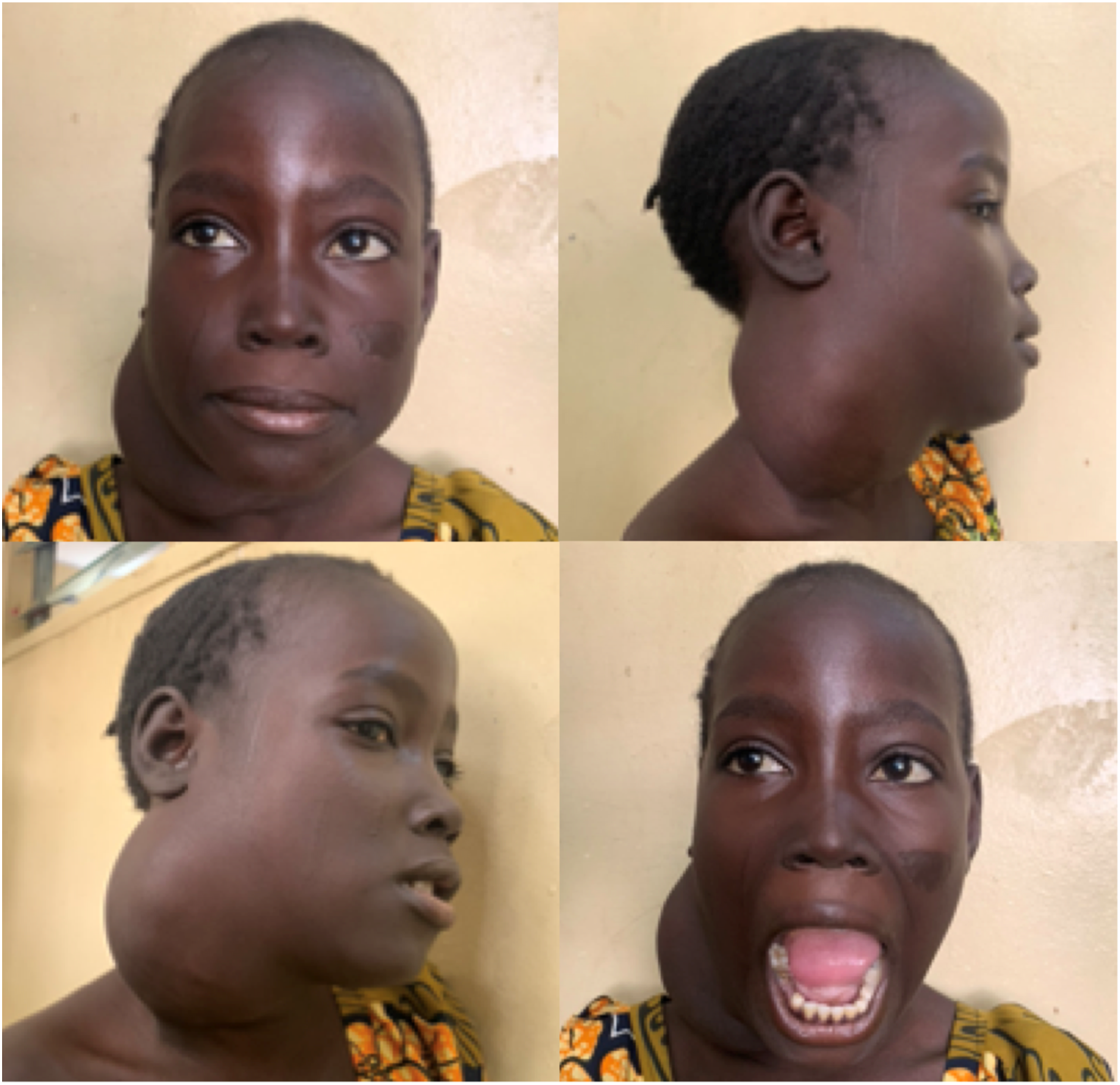
Magnetic resonance imaging (MRI) was not readily available in our city because of technical errors at the time, it would have been appropriate considering the soft-tissue nature of the pathology and its large size, compromising the airway. Computed tomography (CT) scan showed a huge fairly oval well-circumscribed homogenously hypodense mass, measuring 10.3 cm x 8.0 cm x 7.7 cm in its dimension, in the right lateral neck extending from the base of the skull and peri-auricular region superiorly to the supraclavicular and root of the neck regions inferiorly (Figure 2A-D). It showed heterogeneous enhancement of the mass at the arterial phase (Figure 2C) but homogenous enhancement post intravenous contrast injection at the delayed phase (Figure 2D). The mass compressed the ipsilateral superficial lobe of the right parotid gland and displaced it superior-laterally as seen in Figure 2B. The mass extended to the midline and compressed the pharynx and the larynx and also extended to the posterior part of the adjacent submandibular region. It also compressed and displaced the adjacent vessels anterolaterally. No erosion or destruction of the adjacent bones. A provisional diagnosis of giant pleomorphic adenoma of the parotid gland was made based on the imaging finding. (A–D): Computed tomography of the Head & Neck. (A) Axial precontrast image shows a huge hypodense mass (upward arrow) at the right lateral neck which extends to the midline and compresses the pharynx (Star), (B) Coronal reformatted precontrast image shows the mass (upward arrow), (C) Sagittal postcontrast image shows the enhancing mass compresses and displaces the adjacent carotid arteries (Star), (D) coronal reformatted post-contrast image shows the enhancing mass (downward arrow).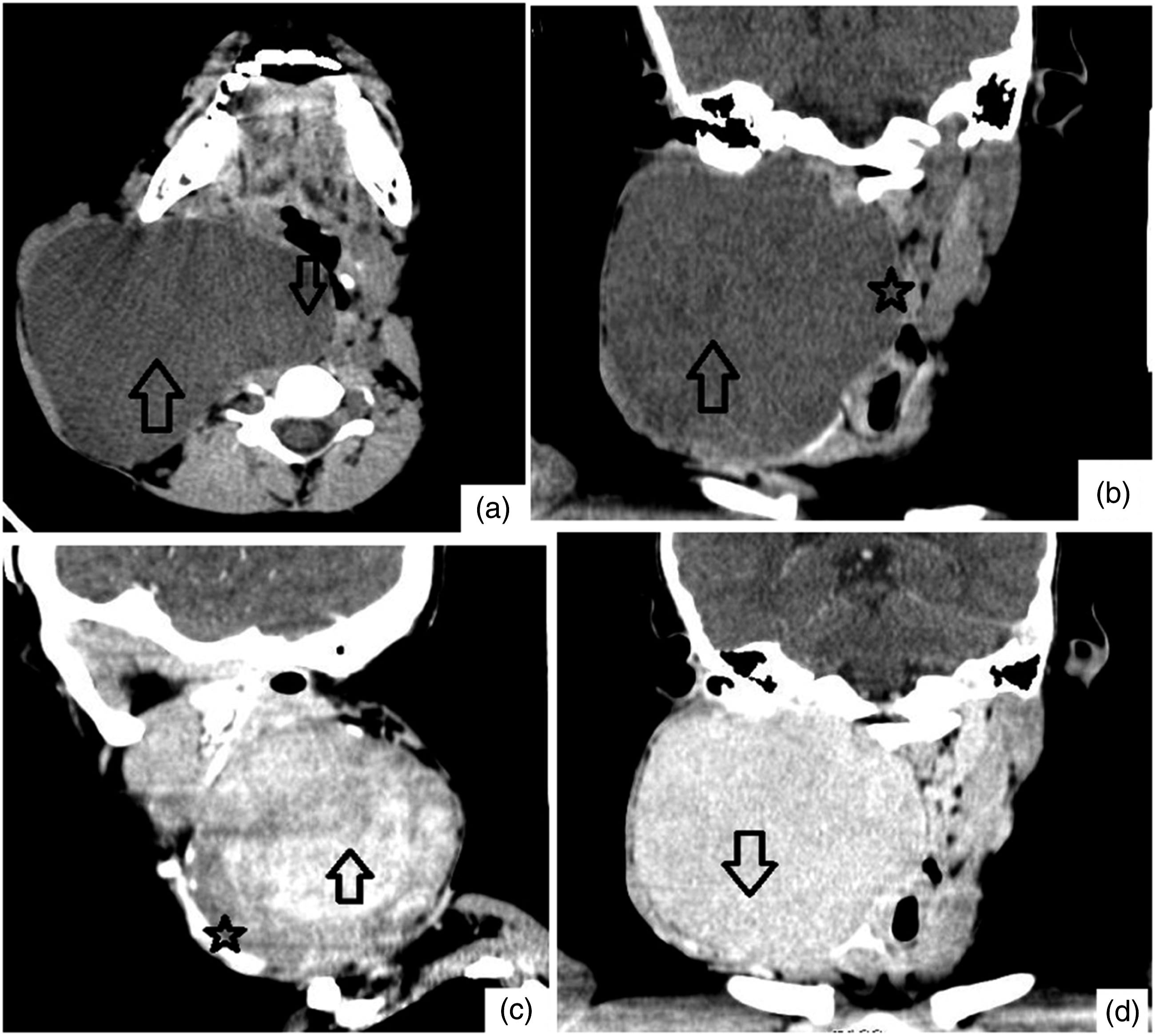
The tumor was excised under general anesthesia using a Modified Blair Incision for access, with dissection and preservation of the facial nerve. The mass was situated immediately deep to the facial nerve, dissection was easy as the mass was not adherent to surrounding structures, hard, well-circumscribed, and not encapsulated. The mass was situated beneath the trunk and branches of the facial nerve and easily delivered with blunt finger dissection around the tumor margins and adequate tissue and gently retraction the 2 trunks of the facial nerve apart with the inferior cervicofacial trunk retracted below the lower margin of the tumor to allow its delivery (Figure 3). The immediate postoperative period and recovery were satisfactory. However, 24 hours after, the patient developed respiratory obstruction that necessitated immediate airway control which was suspected to be caused by soft-tissue edema and possibly hematoma collection. She was taken to the theatre and a tracheostomy was placed to secure the airway and adjust the surgical drain to decompress the swelling was removed after 3 days and the tracheostomy was decannulated after a week (Figure 4). The histology report was as follows: ‘sections show tissue showing a neoplasm composed of nests of cells within fibro collagenous stroma. The individual cells are uniform, having round to oval nuclei and abundant granular, eosinophilic cytoplasm with distinct cell borders features are in keeping with GCT (Figure 5). (A) Tumor exposed, deep to the lower trunk of the facial nerve. (B) Tumor removed completely. (C) Tumor bed showing the branches of the carotid vessels. (D) Incision site a week postoperatively Patient at 3 months postoperatively with no signs of tumor recurrence no complications A and B show photomicrographs of granular cell tumor composed of nests and single large cells having fairly uniform nuclei with abundant granular cytoplasm. The background show spindle smooth muscle cells. H and E; A = X100, B = X200.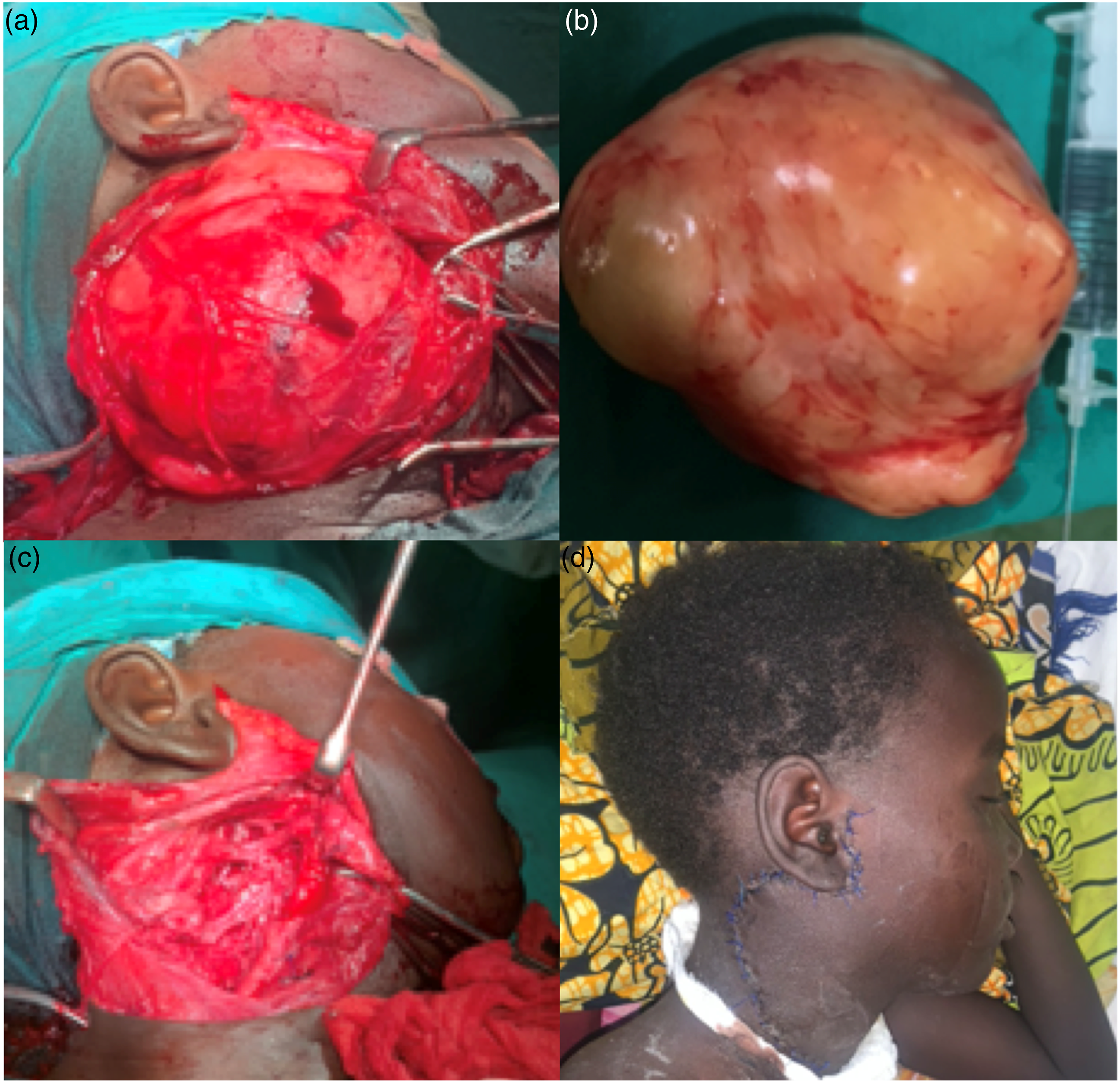
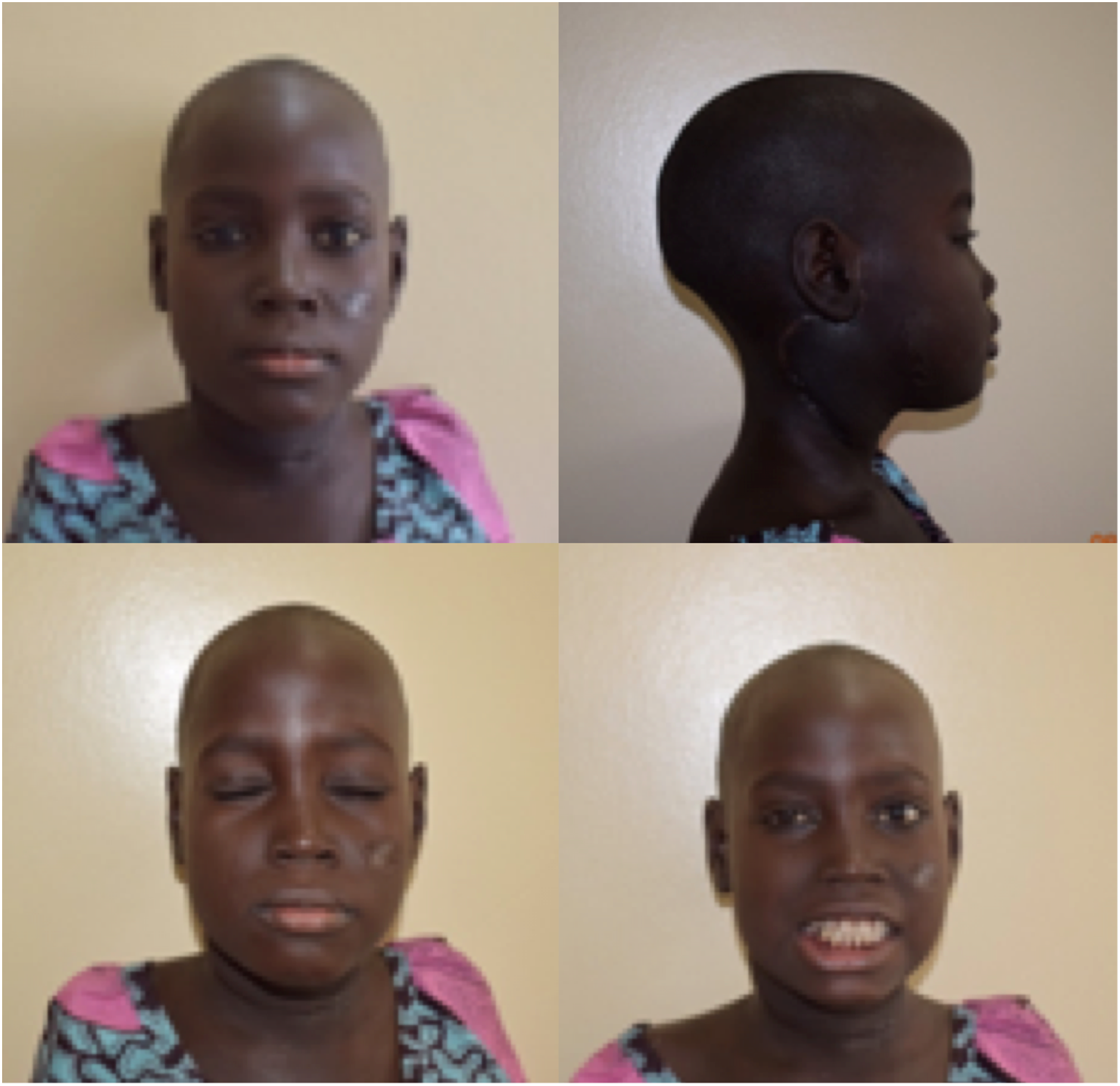
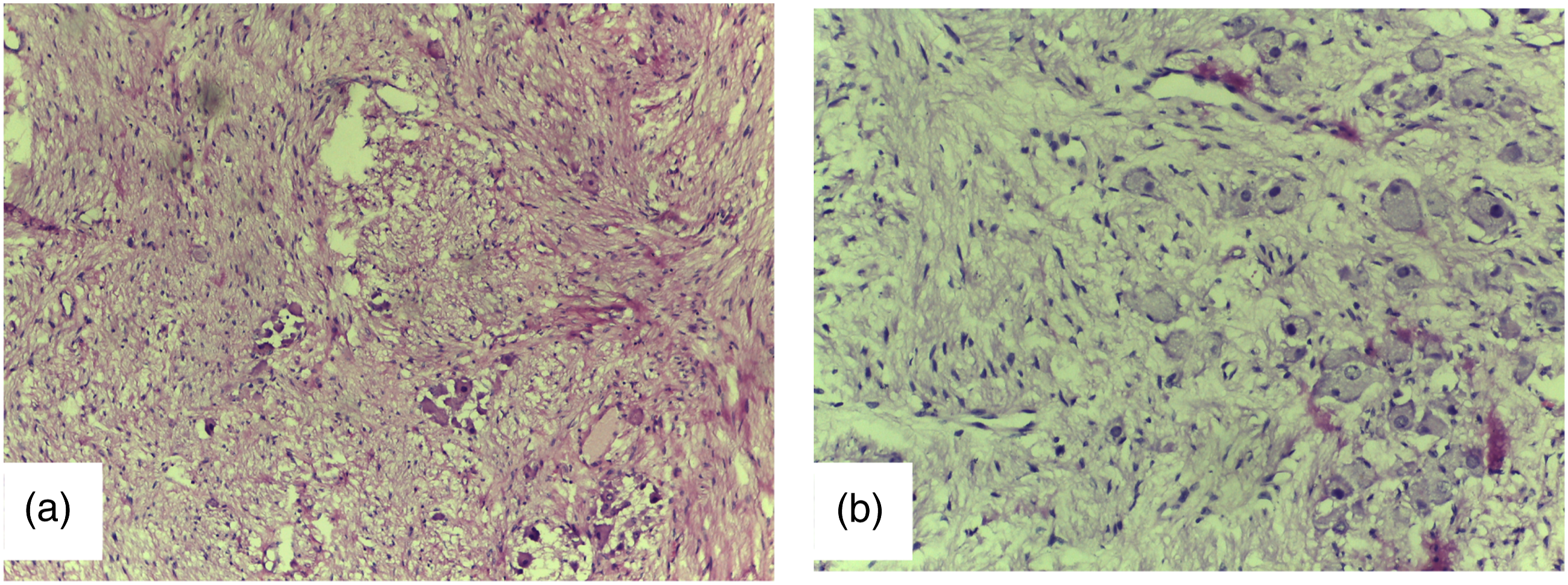
Immunohistochemical analysis was, however, not done because of a lack of availability at our local facility. The patient was discharged home after a week and reviewed 6 months after with no complications or recurrence. The patient is on continuous long-term monitoring and follow-up.
Discussion
Granular cell tumor is a benign neoplasm with a predilection for the oral cavity but may occur in any organ.2,4 Its etiology is unclear, it was originally thought to arise from striated muscle, histiocytes, fibroblasts, myoepithelium and nerve cell connective tissue1,3,5 and the cells often show an intimate relationship with striated muscle and other tissues, it has been variously referred to as either granular cell myoblastoma, granular cell neurofibroma, or granular cell schwannoma. 4 Recently, authors now agree that because the unique granular cells that make up the lesion are of neural (primitive Schwann cell) origin, predominantly, based on immunochemical studies which have identified neuron-specific enolase and S-100 protein markers on the tumor cells6-8 presence of eosinophilic granules within the cytoplasm of the tumor cells gives it the name GCTs.
The reported case is unusual; as this tumor is very rarely seen in children, the present case seen in an 8-year-old, which is below the average age of occurrence of the tumor. Though it may occur in all ages, it is more frequently encountered in the fourth to sixth decades of life. The occurrence of GCT in the deep lobe of the parotid is also striking, to the best of our knowledge this seems to be the first report affecting such a location. The observed and reported size of GCTs are rarely exceeding 3 cm, in this case, we report large size of 7 × 5 cm. The unique location of the present case and its slow pattern of growth means it may have to grow to grotesque proportions before presenting signs and symptoms and cause the patient to seek medical care, especially in our resource-limited setting. Treatment is by local surgical excision and recurrence is rare even when the lesion is not completely excised. Microscopically, sometimes this tumor may mimic a lipoma, some may develop multiple GCTs have also been observed and reported.
Microscopically some GCTs may induce pseudoepitheliomatous hyperplasia of the overlying epithelium, which may mimic an invasive squamous cell carcinoma. The pathologist needs to be aware of this possibility to avoid a mistaken diagnosis of cancer.
The differential diagnoses of this mass based on imaging include pleomorphic adenoma, teratoma, hemangioma, lymphoma, and nasopharyngeal carcinoma. The mass was large which is against pleomorphic adenoma. Pleomorphic adenoma when large shows heterogeneous patterns in pre-and post-contrast images and multiple foci of calcifications. 9 These findings were not observed in this case. Teratoma usually shows a heterogeneous pattern with calcifications and fat on imaging which was not present in the index case. The mass had no cystic components that will suggest vascular origin like hemangioma and also its homogeneity. The enhancement of mass is not typical of lymphoma. No involvement of the adjacent bones but only pressure effect on adjacent soft tissues was noted and showed well-defined margin in this case which ruled out the possibility of malignant tumors. Other differential diagnoses of GCT include benign connective tissue and neural tumors such as fibromas, lipomas, neuromas, neurofibromas, or schwannomas with their malignant variants, minor salivary gland tumors, and even oral carcinomas.3,8 Although granular cell tumors are benign, about 10% of cases show clinically malignant behavior. 10 This is more likely to present in the extremities rather than the head and neck region. The present case, however, did not present with clinical or histologic features of malignancy. Worthy of note also is that microscopically some GCTs can mimic invasive squamous cell carcinoma by inducing pseudoepitheliomatous hyperplasia of the overlying epithelium. They have been reported cases of initially wrongly diagnosed as squamous cell carcinoma of the oral cavity. 11 Pathologists should be aware of this likelihood to avoid an incorrect diagnosis of cancer.
In summary, GCT involving the parotid gland is very rare occurs largely in women, and is often encountered in the superficial lobe and treated by superficial parotidectomy. This case reports a deep lobe Parotid GCT in an 8-year-old successfully treated by surgical excision with preservation of the facial nerve.
Learning Points
• Granular cell tumors are majorly small tumors but can grow to a grotesque proportion. • When found in the neck large GCTs may result in airway obstruction that will require close monitoring even in the postoperative period. • Some GCTs can mimic invasive squamous cell carcinoma microscopically.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
