Abstract
A 38 year-old female suffered an orbital blow out fracture and oculomotor palsy due to blunt orbital trauma. After surgical treatment she developed an occlusion of the superior temporal branch of the central retinal artery. At 6 month follow-up, the oculomotor palsy was resolved and visual acuity improved, but with a residual left inferior scotoma.
Introduction
Isolated third cranial nerve palsy following orbital trauma is an uncommon condition, and is usually diagnosed in association with other cranial nerve palsies in cases of high-energy central nervous system (CNS) trauma.1,2 Similarly, central retinal artery (CRA) occlusions following orbital trauma3-7 or after surgical correction of an orbital blow out fracture8-11 have only been reported in the form of a few case reports in the literature. The low incidence and high clinical variability of these conditions often lead to delayed diagnosis and suboptimal treatment outcomes.2,4,6,11 We present the case of a patient who, after orbital trauma with blow out fracture, presented with third nerve palsy and, as a complication of the orbital reconstruction surgery, occlusion of the central retinal artery.
Case Report
A 38-year-old woman suffered a blow to the left orbital region. 2 days after trauma, she attended the Emergency Department (ED) for pain and diplopia. The patient had no relevant medical history and her previous refractive compensation was: right eye (RE)−1,5–2,5/20 and left eye (LE) +0,25 – 1,5/165 but she did not wear optic compensation.
The patient complained of acute pain related to limited eye movements and inability to open the left eye. She had left periorbital oedema and ecchymosis, extensive subconjunctival haemorrhage and infraorbital nerve hypoesthesia. The left pupil was mydriatic and hyporeactive. The left eye was exotropic and hypertropic with limited adduction and infraversion (Figure 1). All these findings together suggested third cranial nerve paresis. The patient referred diplopia in all gaze positions. Visual acuity (VA) without optic correction was 0,5 in RE-0,8 with pinhole- and 0,2 in LE, 0,6 with pinhole. Intraocular pressure (IOP) and fundus examinations were normal. 9 positions of gaze demonstrating left III nerve palsy.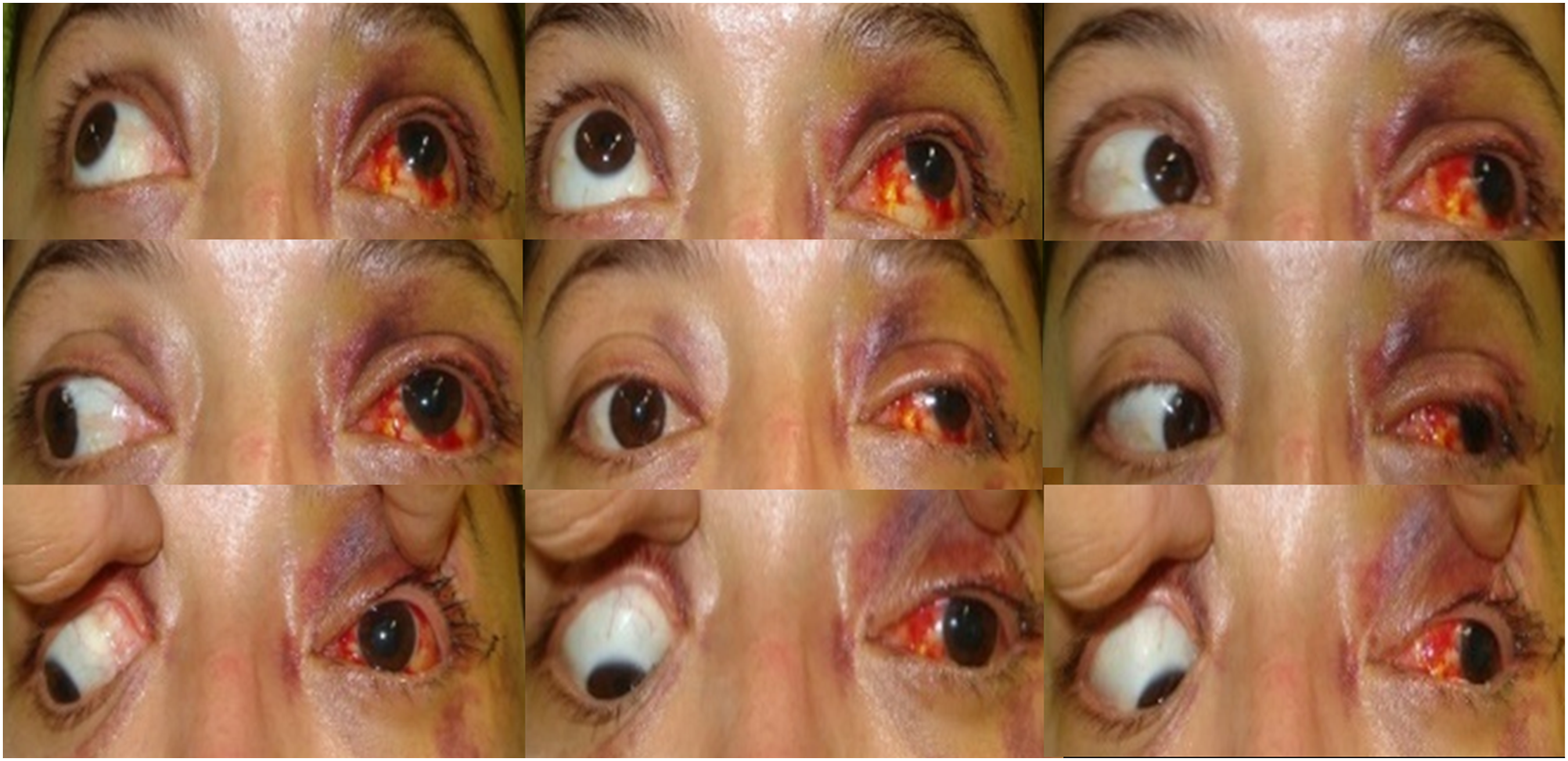
Orbital computed tomography (CT) revealed a left blow out fracture involving the floor and medial wall, pneumoorbitus, soft tissue oedema and possible entrapment of medial and inferior rectus muscles (Figure 2). Presurgical CT with left floor and medial orbital wall fracture. From left to right: Frontal, axial and sagittal view.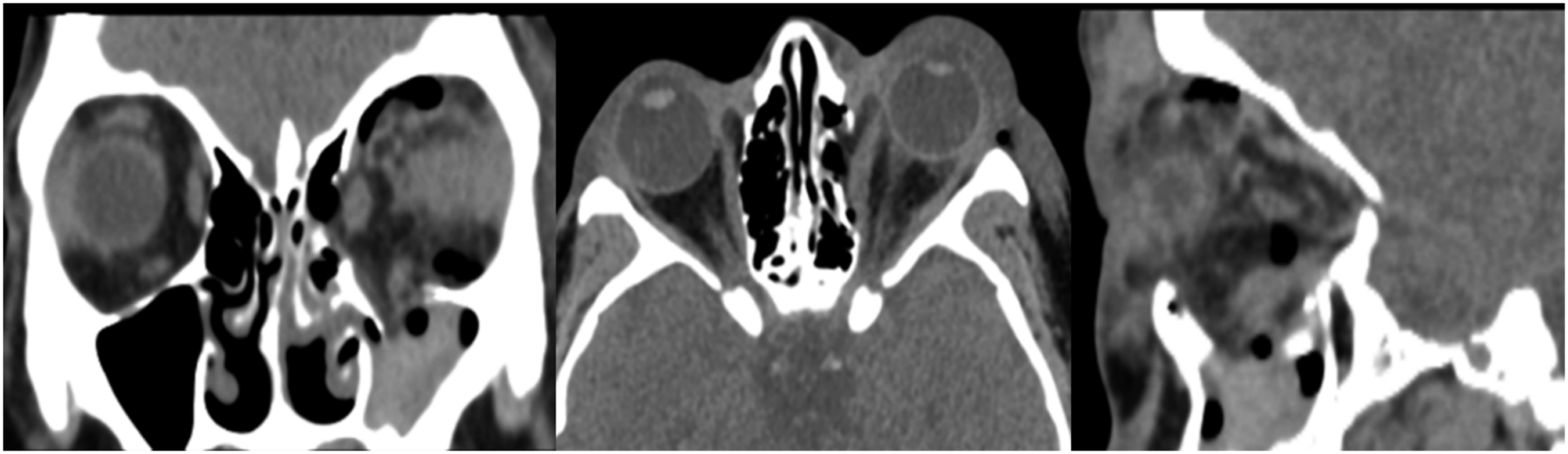
Although no intraconal processes were found despite the pneumoorbitus, due to the presence of diplopia with suspected muscle impairment and pain related to eye movements, urgent surgical treatment was deemed necessary.
After 24 hours the patient underwent surgery. An intraoperative forced duction test (FDT) was performed under general anaesthesia with a negative result, ruling out fat or orbital musculature entrapment. A transconjunctival, retroseptal and retrocaruncular approach was performed, and the orbital fracture was reconstructed with a small preformed orbital mesh (Synthes®), fixed to the infraorbital rim with 2 4 mm self-drilling screws. Prophylactic intravenous antibiotics, methylprednisolone 40 mg/8 hours and painkillers were prescribed for postoperative recovery.
In the immediate postoperative period, the patient reported persistent diplopia with worsening VA in LE (perception of hand movement). The pupil remained mydriatic and hyporeactive with impaired ocular adduction and infraduction. Fundoscopy revealed occlusion of the superior temporal branch of the CRA, associated with retinal oedema and macular involvement (Figure 3). Left: eye fundus with retinal oedema affecting the macula and occlusion of the superior temporal branch of the Central Retinal Artery (arterial stop pointed with blue arrow). Right: Resolution of the oedema and of the previous occlusion (resolution of arterial stop pointed with blue arrow).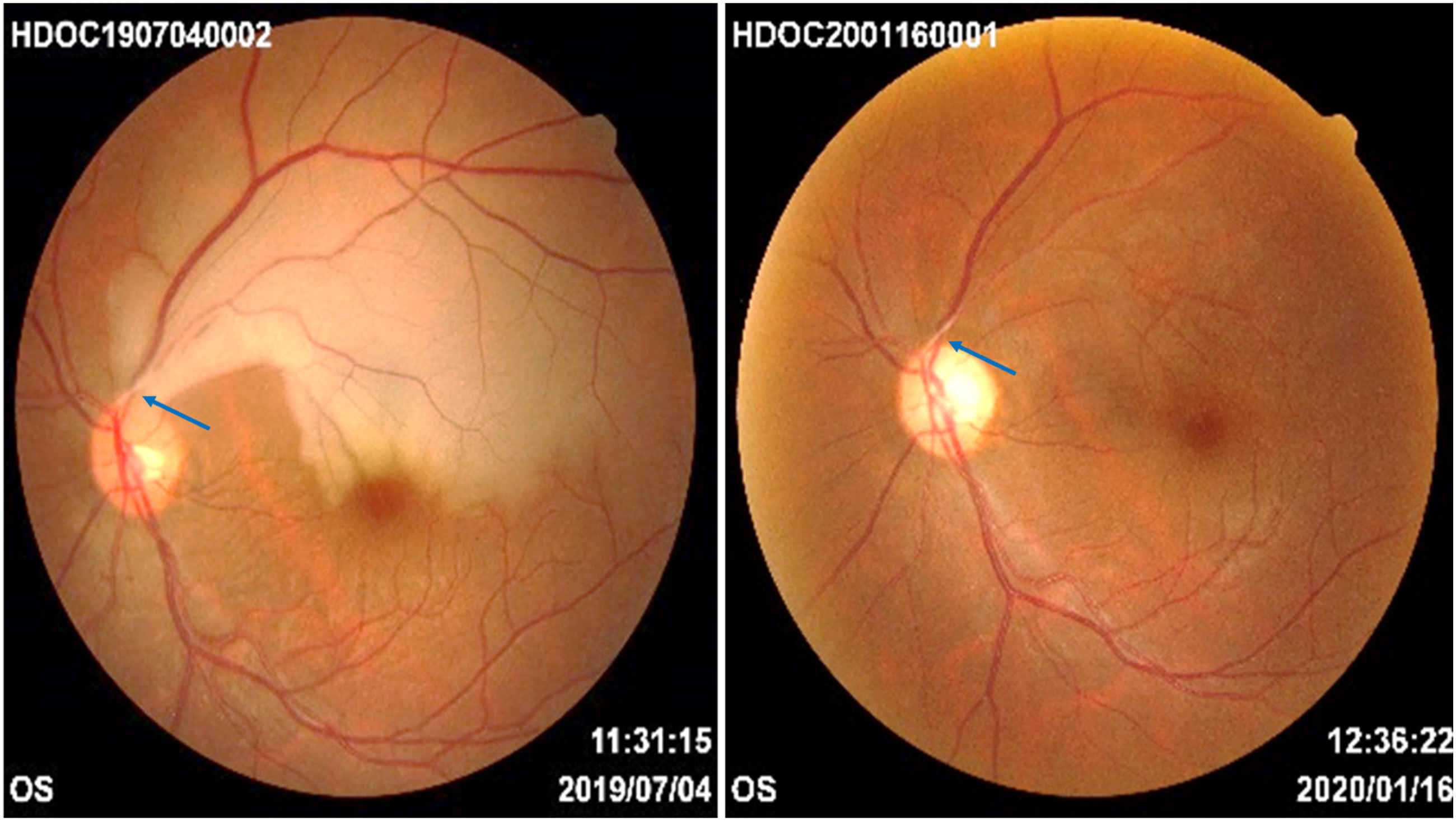
A new CT scan again showed the absence of intraconal processes, although the retrobulbar emphysema remained unchanged. The orbital mesh was well positioned, without compression or entrapment of any orbital structure. The IOP was normal.
After ocular massage, paracentesis of the anterior chamber and a new bolus of 500 mg of intravenous methylprednisolone, no visual improvement was observed. It was then decided to reoperate de patient with a lateral canthotomy, obtaining minimum orbital drainage.
After the second surgery, the patient reported relief of ocular pain, although the third nerve palsy and left inferior scotoma remained. The IOP was in the normal range, and the occlusion of the left superior temporal branch of the CRA persisted along with retinal oedema. Internal Medicine and Haematology studied the case to rule out thrombotic or embolic pathology. Prophylactic clopidogrel 75 mg every 24 hours was administered and Holter, supra-aortic trunk Doppler ultrasound, lower limbs Doppler ultrasound, trans-thoracic echocardiogram and blood tests including autoimmunity profile, cardiolipins, parasites and thrombophilia were negative.
At 6 months follow-up, the VA in LE was 0.3-in the upper field- and ocular motility normalised with complete resolution of diplopia (Figure 4). Only the pupil remained mydriatic with slight contraction under light stimulation (5 mm in the dark, 3 mm in the light). The left inferior scotoma remained, despite occlusion of the CRA and the retinal oedema disappeared. During Optical Coherence Tomography (OCT) a slight thinning of the superior temporal layers of the peripapillary retina was observed in LE. 9 positions of gaze demonstrating resolution of the left III nerve palsy.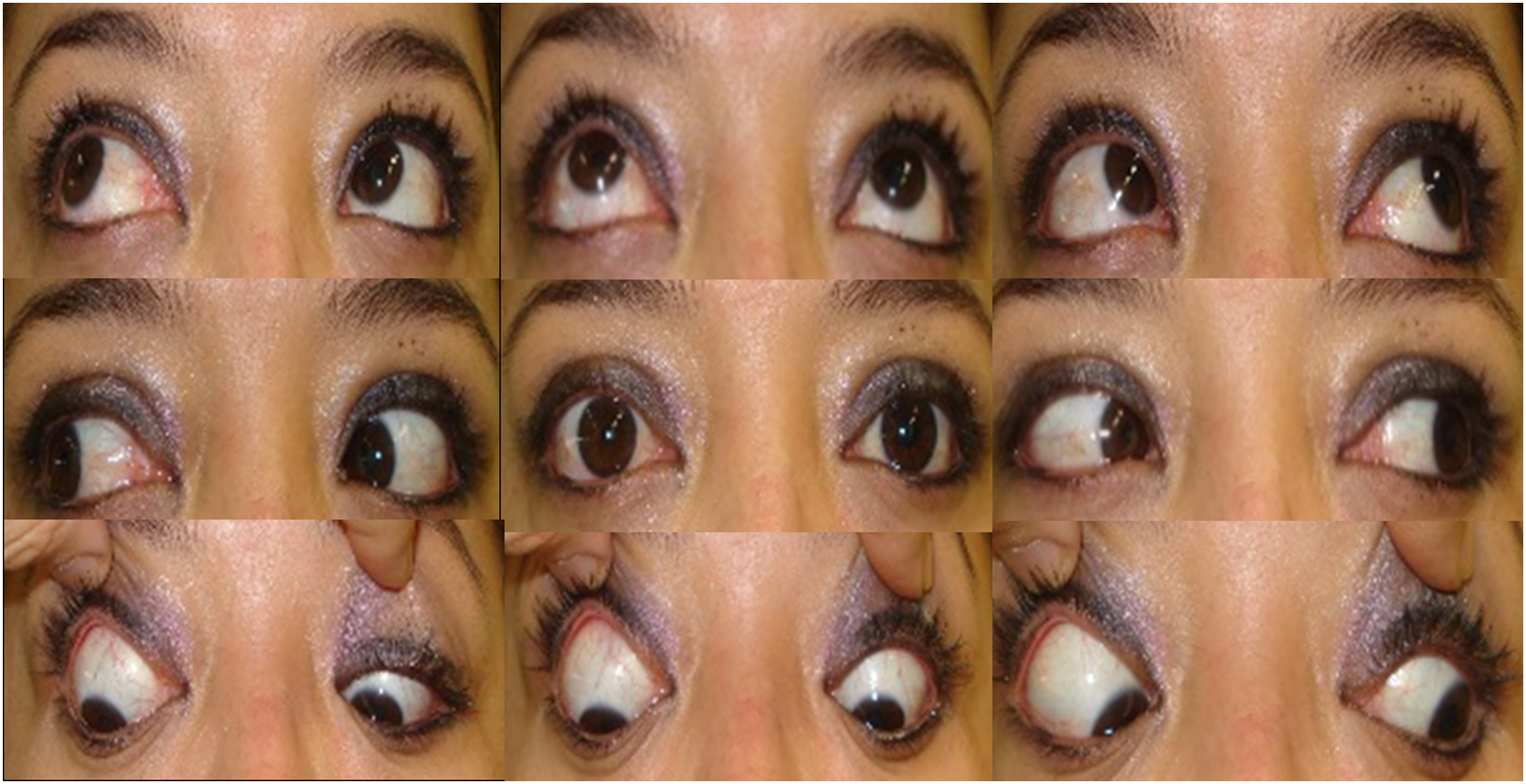
Discussion
Isolated third nerve palsy following orbital trauma is a very uncommon form of presentation, with all known literature consisting of 2 case reports and 1 case series.1,2,9 Likewise, isolated CRA occlusion in patients with orbital trauma and no systemic pathology is a very infrequent condition that has only been reported in a few case reports3,4,6,9-11 and 1 case series of 5 patients. 5 To our knowledge, there is no publication that has documented both complications at the same time.
In reports of oculomotor nerve palsy following blunt ocular trauma, Nagendran et al and Kook et al propose direct injury of the third cranial nerve or indirect compression of the orbital apex, due to inflammation or retrobulbar processes, as the most likely mechanism. They recommend a thorough clinical examination with FDT prior to surgery to differentiate a neurogenic pattern from a restrictive pattern.1,2
Our patient presented with severe adduction and infraversión limitation, associated with a mydriatic pupil. These findings were consistent with an injury to the inferior branch of the third cranial nerve. Recovery time after orbital trauma averages around 10 months, with 60% of patients achieving complete functional recovery. 2 It is usually recommended to wait a minimum of 6 months to evaluate the degree of spontaneous recovery, then if deemed necessary it can be treated surgically, with botulinum toxin infiltrations or with prisms. 12
Regarding the reports of CRA occlusion, Nicholson and Guzak 9 are the first authors to postulate that injury to orbital apex structures - after undergoing surgical treatment of blow out fractures – may be caused by placement of the orbital mesh too posteriorly. Chawla 3 proposed CRA vasospasm secondary to the trauma, and compression due to retrobulbar haematoma, as possible mechanisms. Emery, Huff and Justice reported CRA occlusion due to post-surgical intraconal bleeding. 10 In 2004, Umeed and Shafquat 4 proposed as a mechanism of post-traumatic CRA occlusion the disruption of the intimal layer caused by the shock wave and the local vasospasm, as a natural homeostatic mechanism. This was also endorsed by other authors.5,6 Years later, Himori et al proposed as the mechanism of CRA an overstretching of the optic nerve, due to a case of a massive floor fracture with globe dislocation into the maxillary sinus. 11
Linberg and Cartwright et al mention retrobulbar emphysema as a possible mechanism, as it is known to increase IOP and can lead to optic nerve compression.13,14
We believe that in our case, surgical manipulation may have caused direct injury to the CRA with thrombus formation which, once mobilised, occluded the temporal branch. Direct injury to the temporal branch was ruled out due to the absence of ocular perforation. No retrobulbar haematoma was found on CT scans and - despite intraconal emphysema – IOP remained normal.
For the treatment of non-arteritic CRA occlusions, Rumelt et al 15 proposed a step-based treatment, achieving improved VA compared to patients who had received only part or combinations of the total treatment. Vaitheeswaran et al 7 described a transcaruncular approach for the catheterisation and direct fibrinolysis of the ophthalmic artery as a viable alternative, reducing systemic complications. Although the most recent metanalysis of intra-arterial thrombolysis (IAT) for non-arteritic CRA thrombosis has shown a favourable Odds ratio, the only included randomised trial does not support this. 16
Conclusion
In retrospect to our intervention, the patient in the ED had pain, post-traumatic oedema and oculomotor palsy. Thus, it could be argued that she could have benefited from an initial treatment with systemic steroids and IOP and VA monitorization. Postponing surgery for at least 2 weeks could have avoided the traumatic side-effects of immediate surgical treatment.9,10 Once the CRA occlusion was established, we could have tried a treatment following the step-based approach of Rumelt et al, considering IAT as a possibility.15,16
Footnotes
Acknowledgements
To my fellow residents who are tomorrow’s maxillofacial surgeons
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The Ethical Committee exempted the approval for this article, because it is a case report and the patient has signed the informed consent for the publication of her data.
Patient consent
The Patient signed the informed consent.
