Abstract
Study Design:
This is a prospective study for 3 year duration.
Objective:
The aim of this study was to observe the incidence and patterns of orbital fractures and discuss their treatment options.
Methods:
A total 29604 trauma patients visited our emergency department within May 2017 to Oct 2019, where 1230 (4.15%) patients presented with orbital fractures, of which only 44 (3.6% of orbital fracture) patients required surgical reconstruction, and were enrolled in our study and evaluated for their fracture patterns, size of bone defect, clinical presentation, timing of surgery, reconstruction, and complications.
Results:
The incidence of orbital fracture was 4.15%, of which only 20.5% were pure blow out. Associated fractures included 72.7% zygomatic complex, 50% LeFort, 31.8% mandible and 20.5% pan facial fractures. The most common pattern was the 1 wall orbital defect in 38.6%, 2 wall in 27.3%, 3 wall in 29.5% and 4 wall in 4.5%. The orbital floor fracture was seen in 100%, medial wall in 27.3%, lateral wall in 61.4%, roof in 15.9%. Different reconstruction options used included calvarial bone (2.3%), ear cartilage (2.3%), medpore (36.4%), polycaprolactone sheet (6.8%), titanium mesh (52.3%), patient specific implant (6.8%) and navigation (4.5%).
Conclusion:
Orbital fractures are mostly impure fractures, associated with zygomatic complex fractures, hence lateral wall fractures are seen more commonly. Patient specific implants, navigation guided reconstruction, autologous calvarial bone graft and preformed titanium mesh show better results, and fulfill the objectives of orbital reconstruction by restoring the normal anatomy and volume of the orbit.
Keywords
Introduction
An orbit forms from 7 bones namely frontal, zygomatic, maxilla, sphenoid, ethmoid, lacrimal, and palatine; and contains the eye globe which has a crucial functional and aesthetic significance, the extra ocular muscles, and orbital fat. The orbital lateral wall and the roof are thick cortical bones but the inferior and medial walls are thin and frail. An impact around the orbit usually leads to fracture of these weaker areas, however a bigger impact may involve other areas too. Fractures of orbit may occur after road traffic accidents, assault, fall from height and sports injuries. A blunt trauma to the orbital region is one of the commonest cause of its fracture, and may be pure or impure type of blowout fracture. 1 The importance of exact reconstruction of orbital floor and rigid fixation is to prevent and reduce the sequelae.
Orbital trauma reports for a substantial fraction of traumatic injuries with varied patterns. The basics remain the same, but the observations differ. Additional cognizance is provided in this article from the skills of a maxillofacial surgeon and an algorithm has been formulated with diverse treatment options. The noteworthy point is that the best possible management plan is often variable which rests upon the clinical circumstances, patterns of trauma as well as on the surgeon with their own discernment, proficiency and comfort.
The aim of this prospective study was to observe the incidence and patterns of orbital fractures and assess their treatment options.
Materials and Methods
The number of patients who visited the emergency unit at our University hospital from May 2017 to Oct 2019, and those with clinico-radiologic evidence of orbital floor fractures, who reported to the outpatient departments or trauma units of Oral and Maxillofacial Surgery and Ophthalmology were recorded. After obtaining institutional ethical approval, only those 44 patients (3.6%) who presented with persisting diplopia, hypoglobus of > 2 mm, enophthalmos of > 2 mm, paresthesia or post traumatic residual deformity were enrolled in the study after obtaining their informed consent and planned for surgical management, while the rest either not willing for surgery or had no indication for surgical reconstruction, had pathologic fractures, hyphema, globe perforation, retinal detachment, only seeing eye, or were medically unstable, were managed conservatively. Detailed history of each patient was recorded on a set pro forma designed for the study, and their clinical and radiological examination using non contrast CT Face or cone beam CT. Data was analyzed for gender, age, mechanism of injury, classification of fracture, diplopia, extrinsic ocular motility, enophthalmos, hypoglobus, impairment of infraorbital nerve, vision loss, epiphora, corneal abrasion, lower lid malposition, scarring, site and size of bone defect, timing of surgery, reconstruction, success, quality of life and complications like pain, swelling, infection, dry eyes, implant rejection and residual deformity.
Various reconstructive options included autografts from calvarial bone, iliac crest, auricular cartilage etc. and allografts such as titanium mesh, porous polyethylene-medpore (BioporeTM), Polycaprolactone (PCL) sheet (Surgiwear®). Intraoperative navigation was used when feasible. Residual deformities were corrected using CAD CAM technology, and customized orbital floor reconstruction was done for better accuracy. The materials used were chosen by the surgeon, based on their comfort with a specific technique, training and availability of material which allowed them to take the decision.
All patients were observed overnight for a minimum of 24 hours for immediate postoperative complications. Special care was given to check for raised intraocular pressure, proptosed eyeball and retrobulbar hematoma. Subsequent to careful observations patients were discharged after 3-4 days. Follow up period was minimum for 1 year. Patients were assessed post operatively after 1 week, 6 months and 1 year for any late complications.
Results
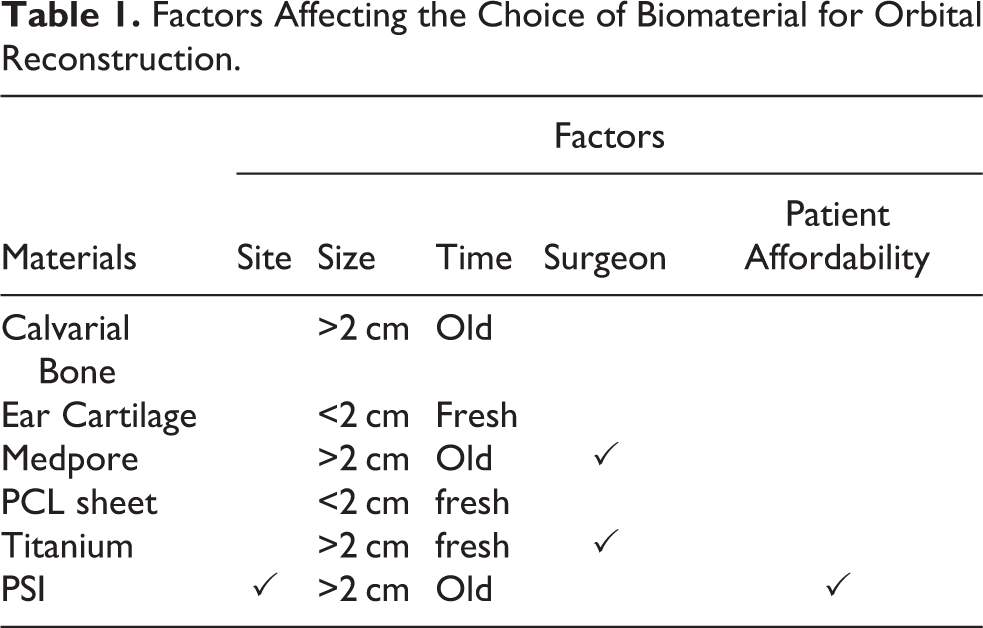
A total 29604 trauma patients visited the emergency department within this time span, where 1230 (incidence: 4.15%) patients presented with orbital fractures, that included 1120 impure blowout fracture,608 ZC (92OI, 92Z), 434 LF (92J, 92m) and 43 combination of ZC and LF fractures (92Om, 92U, 92UI, 92Z) as depicted in Figure 1 and 110 (92Oi) pure orbital blow out fractures. Although 16 patients were surgically explored for entrapment, only 44 (3.6% of orbital fracture) patients required surgical orbital reconstruction. 1051 patients were treated by open reduction and internal fixation (ORIF) for their respective fractures, with no indication for orbital reconstruction. Remaining 34 patients were managed conservatively as were either unwilling for surgery or excluded because of hyphema, globe perforation, retinal detachment, only seeing eye, or medically unstable. Our choice of biomaterial for reconstruction depended up on 5 factors: Site, Size, Time, Surgeon’s choice (Table 1) and Patient’s affordability and is explained as an algorithm (Figure 2).
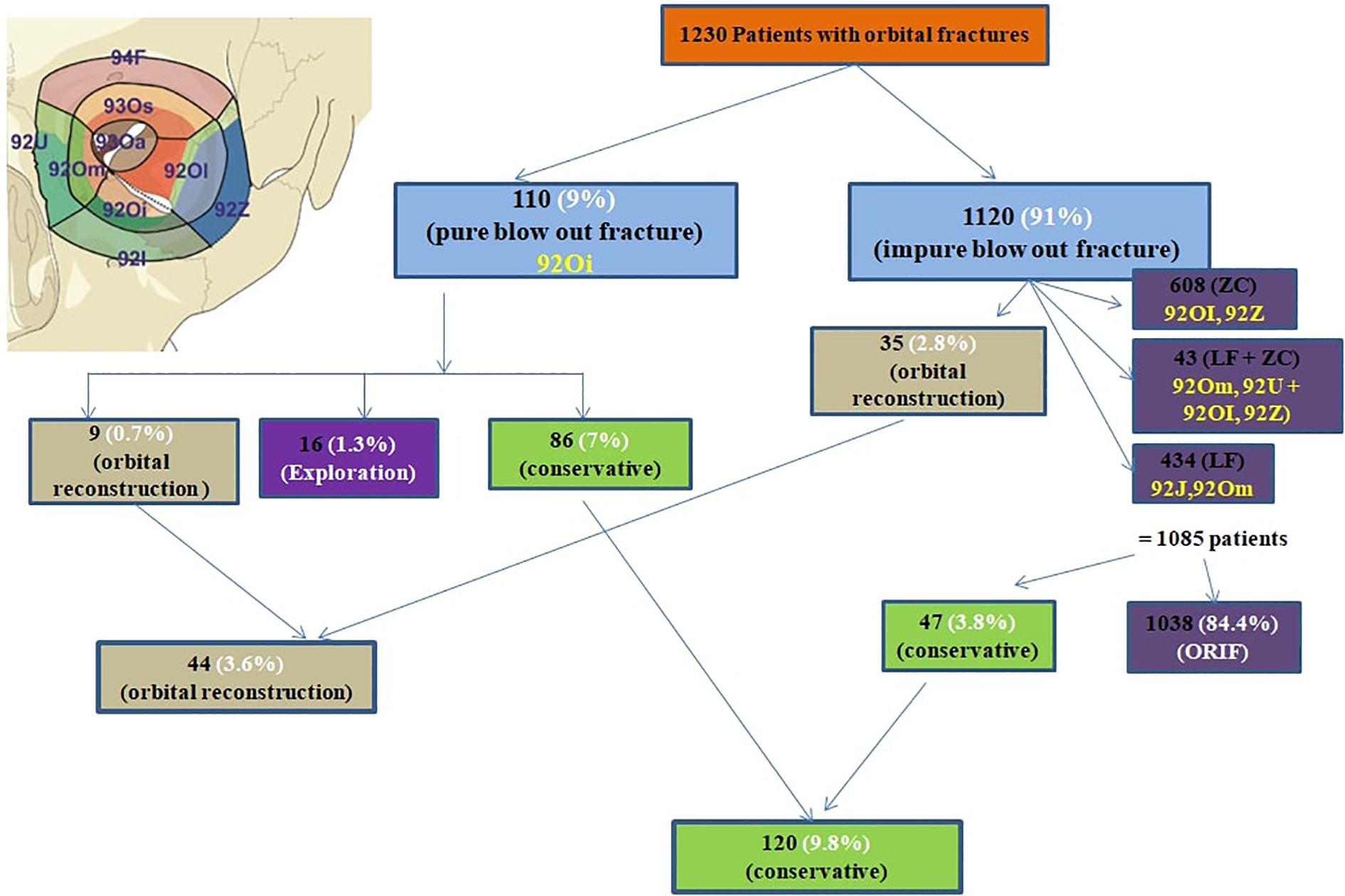
Distribution of orbital trauma patients as per AO classification and their management (n = 1230).
Factors Affecting the Choice of Biomaterial for Orbital Reconstruction.
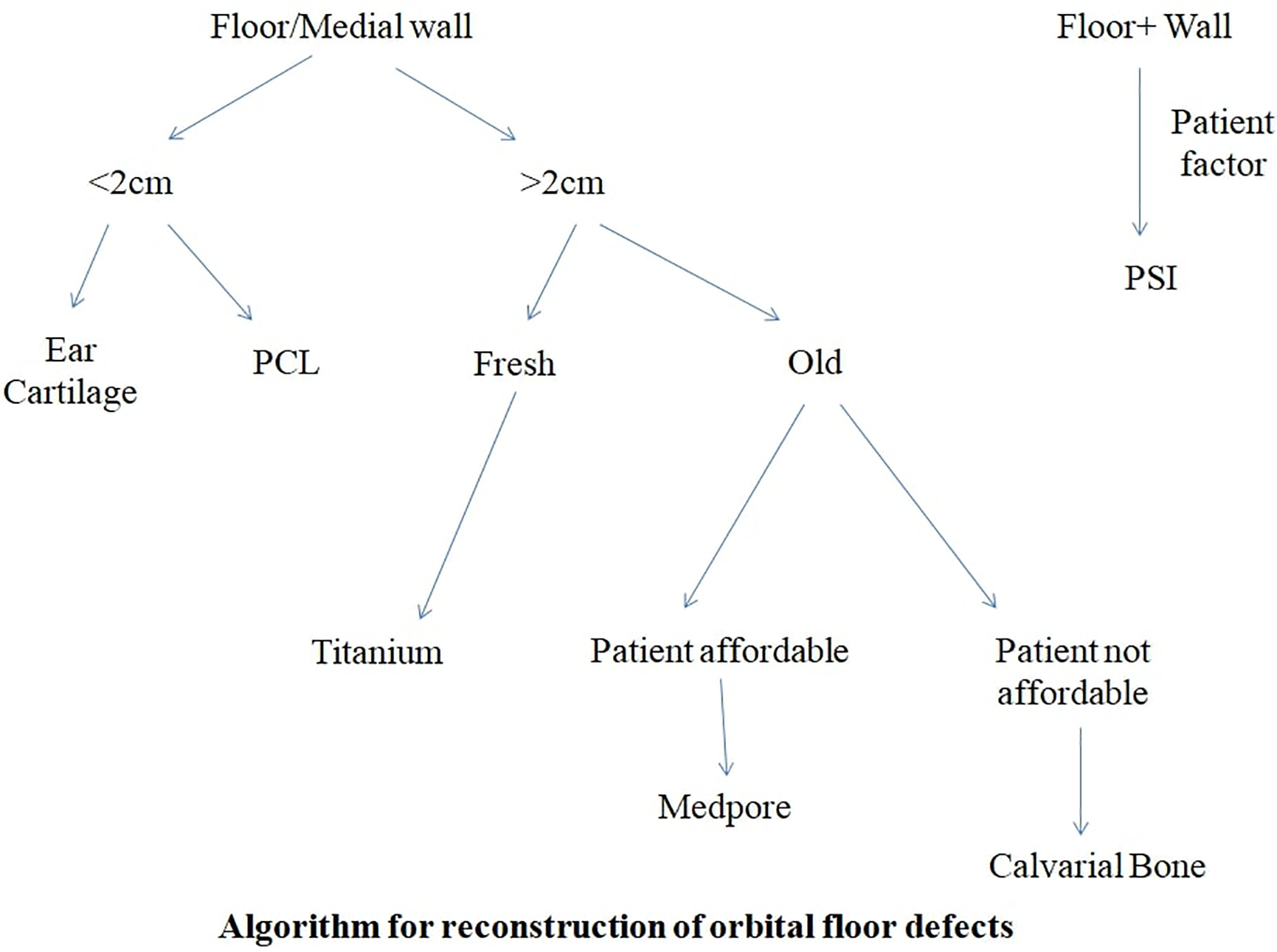
Algorithm for reconstruction of orbital floor defects.
Among the 44 patients managed surgically, 29.5% patients were less than 20 years, while the majority of patients (47.7%) were between 20-30 years of age. (Figure 3a). Our study included only 6 (13.6%) females while majority 38 (86.4%) were males. Most of the patients 38 (86.4%) had road traffic accident, 3 (6.8%) patients assault and 2 (4.5%) had a history of fall from height. Only 1 (2.3%) reported animal injury (Figure 3b). Twenty eight (63.7%) patients had right side involvement in injury while the rest 16 (36.4%) had left side injury.
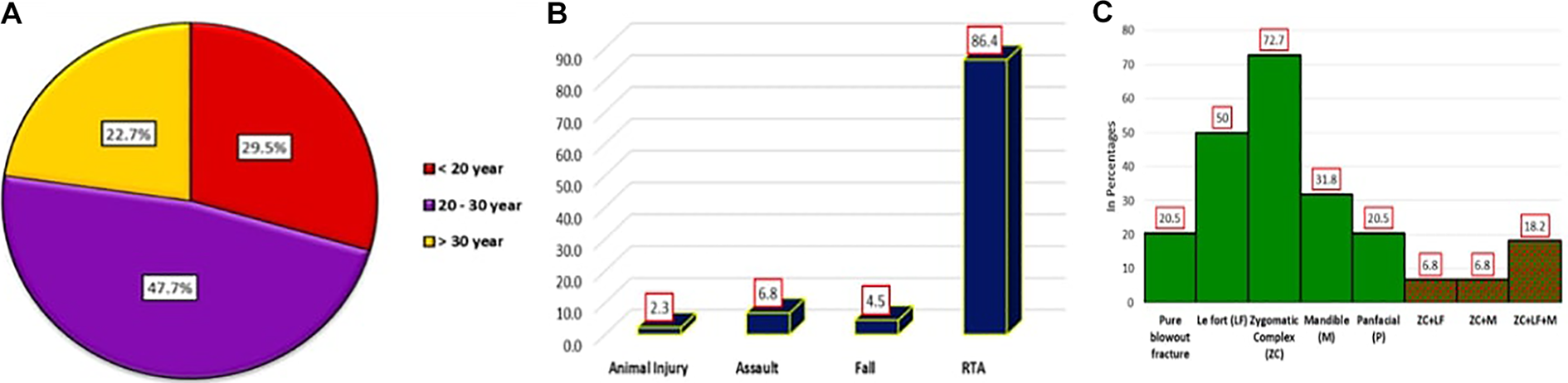
a. Age Distribution of orbital reconstruction patients (n = 44). b. Distribution of orbital reconstruction patients as per Mode of injury (n = 44). c. Distribution of orbital reconstruction patients and associated fractures (n = 44).
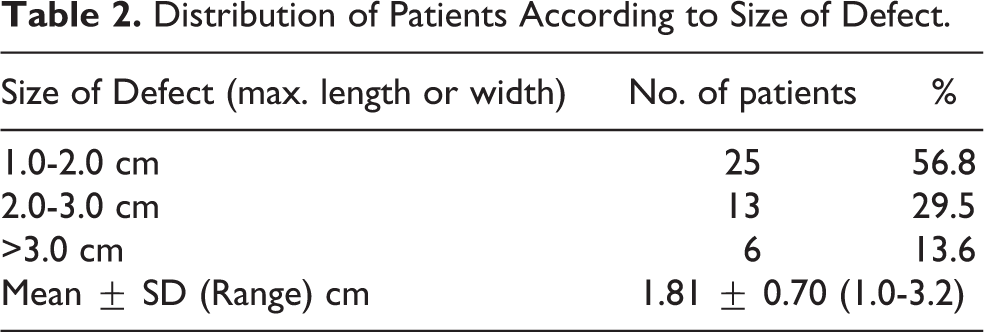
Pure blowout fracture was seen in only 9 (20.5%) cases, while the remaining 35 (79.5%) had impure blowout fracture with Le Fort (LF) and zygomatic complex (ZC) fractures. Associated fractures included 72.7% ZC, 50% LF, 31.8% mandible and 20.5% pan facial fractures. (Figure 3c). Clinical presentation showed diplopia 34.1%, hypoglobus 97.7%, enophthalmos 84.1%, paraesthesia 75%, and vision loss 6.8% (Figure 4). Orbital floor was involved in all the 44 cases. Except for the 9 cases of pure floor fracture, other wall fractures were seen in combination to floor fracture, and included medial wall fracture in 27.3%, lateral wall fracture 61.4%, roof in 15.9%, and 2 wall involvement in 27.3%. Incidence of zygomatic complex fractures is high and in this study we have included the lateral wall fracture in combination with the floor fracture. Only 4.5% cases showed fracture involvement of all the 4 walls of orbit. (Figure 5a & 5b). Most of the patients (56.8%) presented with an orbital defect size between 1-2 cm and only 13.6% had a defect size more than 3 cm (Table 2).
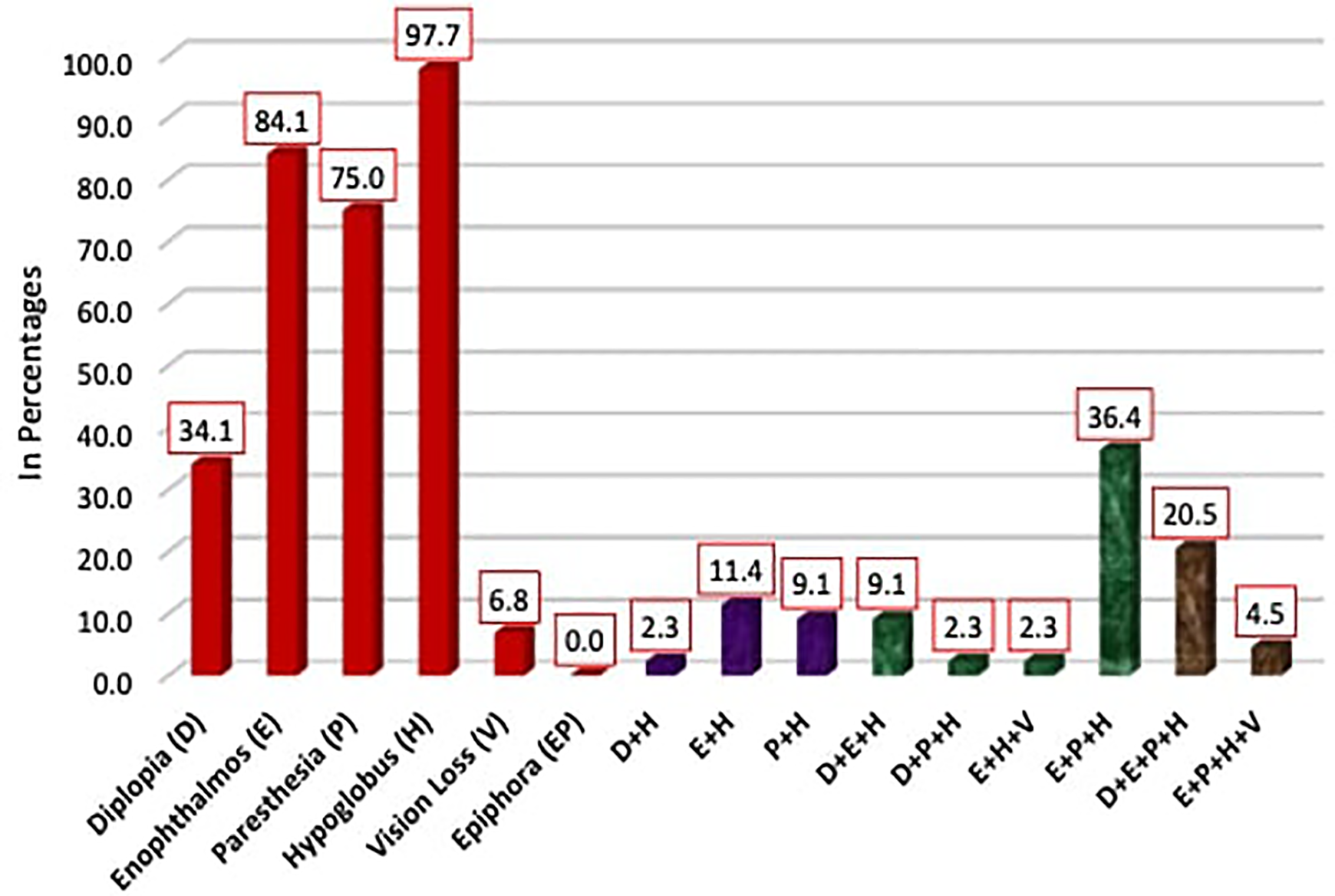
Distribution of orbital reconstruction patients as per clinical features (n = 44).
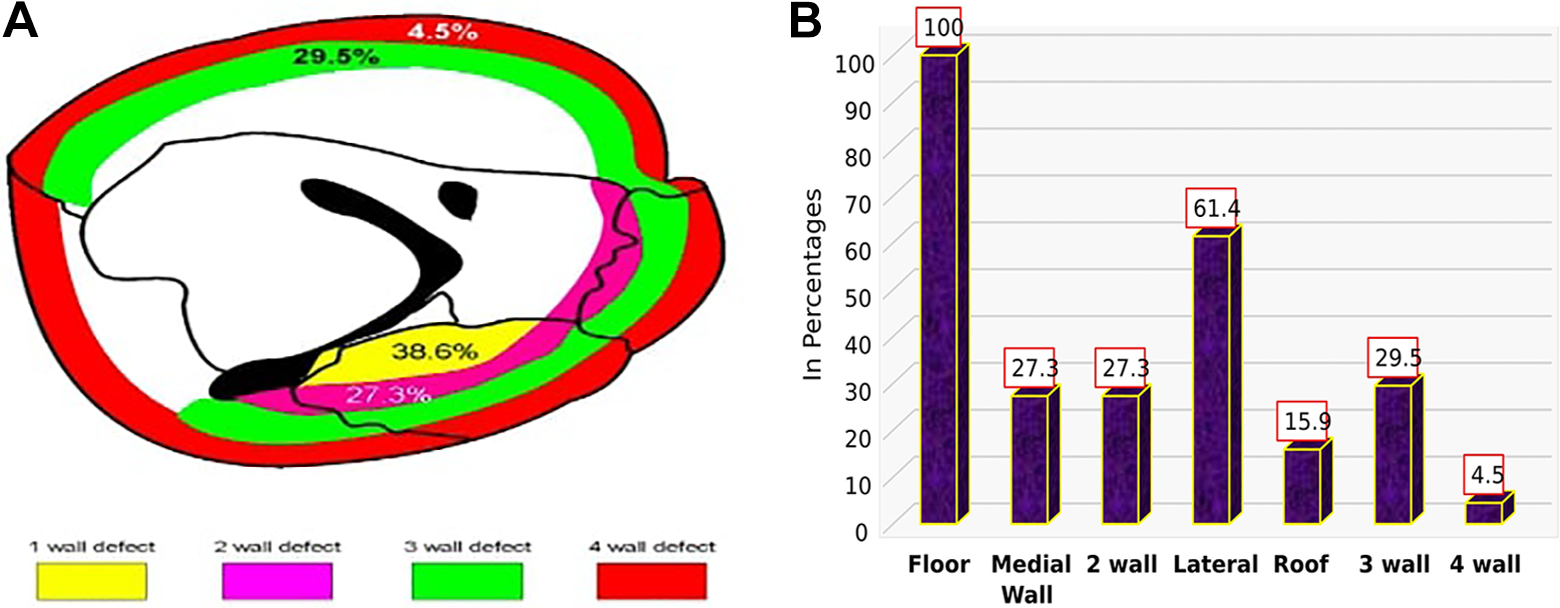
a and b. Distribution of orbital reconstruction patients according to orbital Wall Involvement (n = 44).
Distribution of Patients According to Size of Defect.

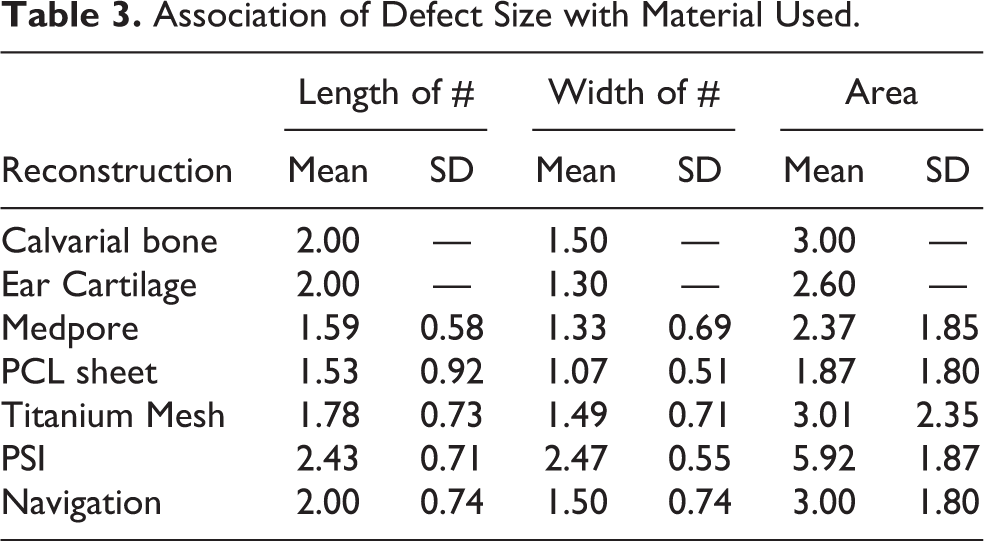
Reconstruction of the orbital defect was done using calvarial bone and ear cartilage in 1 patient each (2.3%), medpore in 16 (36.4%), PCL sheet in 3 (6.8%), titanium mesh in 23 (52.3%), patient specific implant in 3 (6.8%) and intra-operative navigation in 2 (4.5%) (Figure 6). Smaller defects (max. length 1.53 cm, width 1.07 cm and area 1.87 cm2) were reconstructed by PCL and larger defects (max. length 2.43 cm, width 2.47 cm and area 5.92 cm2) was reconstructed with a patient specific customized 3D implant (Table 3).
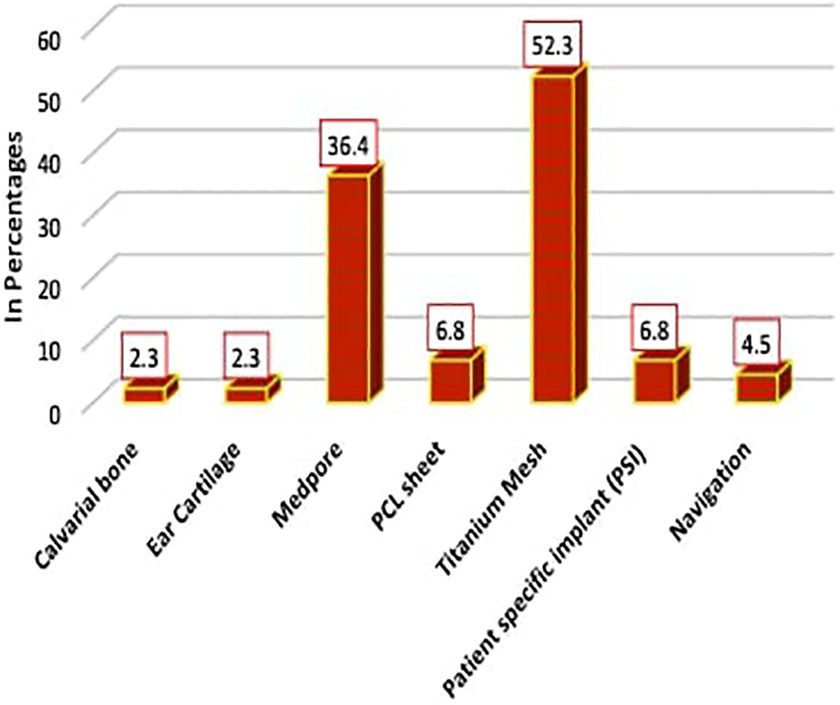
Distribution of orbital reconstruction patients according to Reconstruction procedure (n = 44).
Association of Defect Size with Material Used.
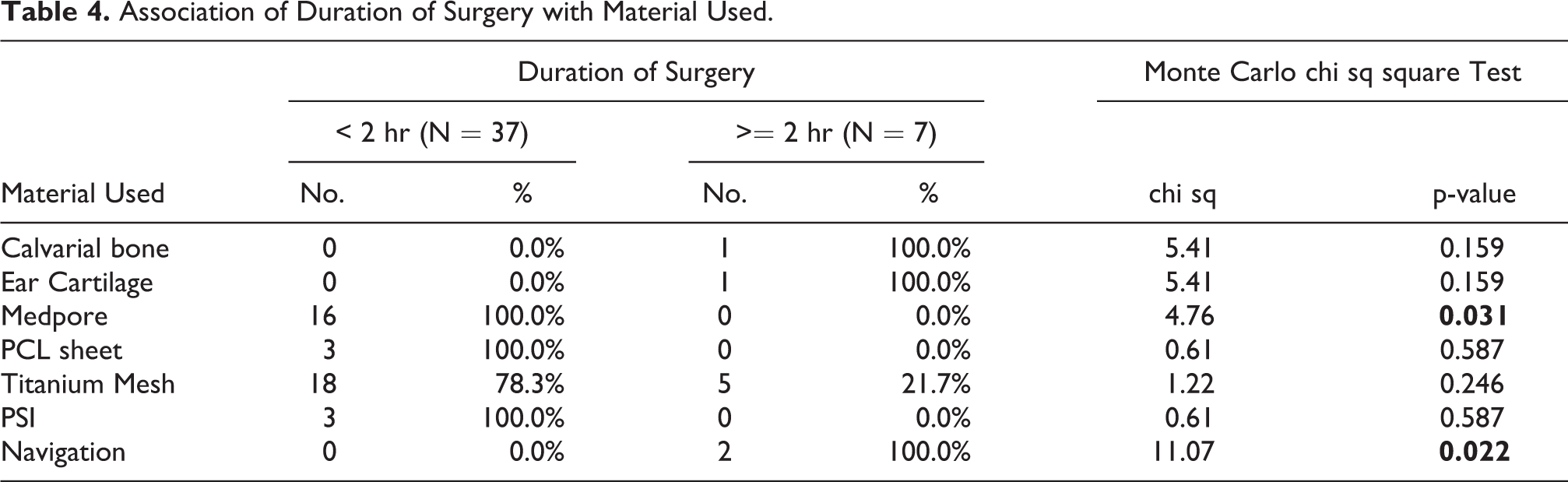
The duration of surgery was less than 2 hr in (81.8%) cases, and included all cases of medpore, PCL and PSI. The significant association of duration of surgery was found with medpore (p = 0.031, shorter duration) and Navigation (p = 0.022, longer duration) Table 4.
Association of Duration of Surgery with Material Used.
Complications included ectropion in 27.27% patients, watery eyes in 31.81% patients, 13.6% had persistent diplopia and enophthalmos, 16% had persistent paresthesia, and 6.8% patients had postop infection.
Discussion
Orbital fractures cause severe injuries like loss of vision and disfigurement of face, leading to lifelong morbidity. 2 In a study on pediatric ocular trauma reported, eye globe was involved in 76.7%. 3 In another study from 2001 to 2014, 15 pediatric patients were identified as having sustained an NOE fracture. 4 A total of 1378 adult patients with orbital wall fractures were enrolled from 2004 to 2014 in another study, of which 10.6% were ≥65 years, mean age of 74.0 years. 5 Our study showed 4.15% incidence of orbital fractures, which is similar to Vats 6 who too reported 4.6% incidence. Majority of the patients in our study were aged between 20-30 years, mean age 29.3 years, similar to 24.2 years reported in another study. 6 In our study 86.4% were males, similar to the study by Abosadegh et al, 7 where males were 86.6% and females 13.4%. The culture and lifestyle of a society confines the women and men to their traditional chores. While men work outside, majority of women are responsible for household work, this is the reason why more men succumbed to trauma than the females.
Slipping was the most common cause of orbital wall fractures in the elderly group (43.8%, p < 0.001), whereas violence in the non-elderly group (37.3%, p < 0.001). 5 In our study 86.4% patients had orbital trauma due to road traffic accident. The younger generation many a times is inexperienced, lacks driving skills, careless, and tends to violate traffic laws by not using helmets, running red lights, and exceeding the speed limits, thereby justifying more road traffic accidents. Twenty eight (63.7%) patients sustained right sided orbital trauma while rest 16 (36.4%) had left sided.
Average times of reporting after trauma was 20 days as patients reported after the orthopaedic or neurosurgical intervention. Patients were evaluated according to Burnstine 8 criteria for immediate (within 24 hours) or early (1-14 days) repair. Some patients visited even 7-8 months late for correction of post traumatic residual deformity. These patients were operated after planning and customized orbital implant fabrication.
Although orbital floor was involved in all the 44 cases, except for the 9 cases of pure floor fracture, other wall fractures were seen in combination to floor fracture; hence the 1 wall fracture included these floor fractures (20.5%) and other single walls, making it a total of 38.6%. Incidence of zygomatic complex fractures is high and in this study we have included the lateral wall fracture in combination with the floor fracture. Only 4.5% cases showed fracture involvement of all the 4 walls of orbit.
Total trauma patients who visited the emergency department were 29604, out of which the patients with orbital fracture were 1230 (4.15%), which is similar to the study by Vats et al 6 who reported the incidence as 4.6%. 1230 patients presented with orbital fractures, that included 1120 impure blowout fracture,608 ZC (92OI, 92Z), 434 LF (92 J, 92 m) and 43 combination of ZC and LF fractures (92Om, 92U, 92UI, 92Z) and 110 (92Oi) pure orbital blow out fractures. Figure 1 briefly outlines the level 3 fractures 9 of the orbit and the treatment provided. In a study done by Wong et al 10 the 5 year incidence of ocular trauma was 1.6% (57/3681). Our data of (20.5%) pure blow out fracture is similar to Kirby et al 11 in which pure blow out fracture was 17.6%. In our study, the most common associated fracture was ZC 72.7%. In a recent study in Pakistan, naso-orboto-ethmoid complex was fractured in 7%, isolated ZC in 19%, maxilla in 36%, mandible in 71%, and dentoalveolar trauma in 50%. 12
The most common clinical presentation in our study was Infraorbital nerve paresthesia (75%) and the least common was loss of vision (6.8%). Orbital floor was involved in 100%, lateral wall in 61.4%, medial wall in 27.3%, and roof in 15.9%. The lateral orbital wall was more common fracture site in the elderly group, with associated fractures including the mandible, maxilla and zygoma. After adjusting for sex and mechanism of injury, the elderly group was a significant risk factor for fracture of the lateral wall (OR 1.658; 95% CI 1.074 to 2.560) and concomitant facial Le Fort fractures (OR 1.625; 95% CI 1.111 to 2.377) and zygoma (OR 1.670; 95% CI 1.126 to 2.475). 5
A systematic review and meta-analysis 13 on subciliary vs. transconjunctival approach indicated a high rate of ectropion and sclera show with the subciliary approach (14.5%), and of entropion with the transconjunctival approach (8.8%). We used subciliary, subtarsal, transconjunctival or any existing laceration to approach the fracture site. The main lower lid complication noted was ectropion and sclera show in 27% patients. They were treated conservatively with gentle massage and none required secondary surgery.
An ideal orbital implant should have the thickness of orbital floor, similar visco-elastic properties, should be easy to manipulate but at the same time should be rigid enough to prevent deformation, not lead to infection or extrusion, fixable, easily available and cost effective. Autogenous calvarial bone undergoes lesser resorption and greater graft volume survival as compared to endochondral bone of the iliac crest or rib; has low risk of infection and extrusion; and also, the scar is usually not visible as the incision is placed within the hair-bearing skin. A resorption rate of up to 75% has been reported for endochondral, and of 20-30% for membranous bone grafts. 14 However, its major disadvantage is the donor site morbidity whose strength reduces to 50%. We also experienced increased surgical time with calvarial graft harvesting. Care was taken to prevent dural tears, subarachnoid hemorrhage and subdural hematoma. Cranial bone is brittle so to contour it to a precise thickness cannot be achieved, and may lead to globe malposition and volumetric asymmetry. Calvarial bone graft cannot be extended posteriorly so chances of residual orbital dystopia and enophthalmos are always present.
Harvesting technique for autologous auricular cartilage is simple and can be used in repairing defects as large as 2 x 2cm. 15 It is biocompatible, has a shape similar to the orbital floor, limited donor site morbidity, is malleable, but provides limited structural support and is prone to resorption. Seven studies 16 using autogenous cartilage (nasoseptal and conchal auricular cartilage) were reviewed, where grafts were not fixed, but placed well posterior to the inferior orbital margin. Of the 23 patients treated with conchal cartilage, only 6 cases of persistent diplopia were documented. Autogenous cartilage was found to be durable, resilient, malleable, pliable to the orbital walls, had reduced resorption rate compared with bone, had longer viability and structural integrity. Critics find conchal cartilage too flexible to provide support. Others find the inherent curvature of the conchal cartilage advantageous for a better adaptation to the orbital floor. Autogenous cartilage grafts are suggested to best suit for repair of orbital defects of up to 2x2cm. 15
Medpore being porous allows in-growth of surrounding soft tissue and bone leading to decreased scarring, capsular formation, foreign body reaction and infection rates. 17 Infection does not occur for 5 weeks that is till the vascularization is going on. It gets anchored into position within 2 weeks. The implant can be easily cut with scissors, contoured, and is not seen in radiographs. It has a thickness of 1.5 mm compared to titanium which has a thickness of 0.85 mm 18,19 and can accept plate fixation to surrounding bone. 19 A total of 529 cases from 9 studies were analyzed. 16 Among the 10 patients with postoperative surgical-site infection, only 2 cases eventually required removal of implants. One patient had residual enophthalmos, but there were no instances of orbital infection, visual loss, worsening diplopia or loss of structural support. It was concluded that high-density porous polyethylene implants are stable, resilient, and enable fibrovascular ingrowths. They do become nidus for infection, but their stabilization offers resistance to infection and risk of migration or extrusion.
Polycaprolactone (PCL) is a biodegradable, non-toxic, biocompatible polymer, degrades in more than 2 years without producing harmful by-products, thereby providing an osteoconductive environment desirable for cellular ingrowths and bone differentiation within the interconnected honeycomb architecture. 20 PCL polyester is readily available, inexpensive, and modifiable to adjust its physio-chemical and biological properties like degradability and mechanical strength without significant loss of properties. Its longer degradation time makes it popular for use for replacement of hard tissues, load-bearing tissues by enhancing stiffness, and for soft tissues by decreasing its molecular weight and degradation time. 21
The advantage of using titanium is that it can accurately be architectured for reconstruction of the internal orbit and complex defects. 22 It is readily available, easily sterilized, biocompatible, integrates into adjacent bone, easily visualized in postoperative imaging, provides good support, does not change its place or shape with time, it requires lesser operative time and equipment. Titanium causes scarring around extraocular muscles due to the perforated plate. Removal of the implant in secondary surgery is difficult. It lacks the viscoelastic property of orbital floor.
Using preoperative DICOM data, a CAD/CAM model can be designed to mirror the unaffected orbit of the patient, on which a Patient Specific Implant (PSI) is made. In our study titanium was used to manufacture these PSI’s. This customized implant reduces intra operative manipulation of material and thus the operating time. There was no post operative visual impairment or foreign body sensation. There are chances of adding impurity to the implant and thus its rejection. 23 –25 Intraoperative navigation can be used to place the implant precisely according to the preoperative planning based upon the normal orbit. 26
When 3 studies with 60 cases were evaluated for use of cranial bone, it was found that, reconstruction with cranial bone graft is less accurate than titanium mesh because of its rigidity and brittleness, 22 although autogenous bone grafts remain the gold standard. 16 However, individually designed titanium mesh allows precise orbital volume. 27 Nine studies that used titanium mesh of various types: non-preformed mesh sheets, individually prefabricated plates and industrially manufactured preformed implants, were reviewed 16 and a surgical-site infection was found in only 1 patient necessitating its removal. Even when used in large defects, the results were excellent because it is rigid enough to support the orbital contents yet deformable, allowing adaptation to the individual anatomy. The precision and consistency of 3-dimensionally preformed titanium mesh plates was the best but even the hand manipulated titanium mesh plates using a computer-aided volumetric measurement of the orbits could reconstruct the orbit with accuracy to within 7% to the contra lateral uninjured side. 28 Patient-specific titanium mesh implants result in better outcomes as compared with those treated with titanium mesh by manual manipulation. 29 It was concluded 16 that titanium mesh is well suited for orbital floor defects of more than 2 cm2.
Our study groups were not of equal number. They were based on the severity of fracture, associated clinical features and choice of reconstruction material to be used. The duration was surgery was <2 hr in 81.8% cases, and varied according to the severity of fracture, type of reconstruction material, use of intra operative navigation and surgeon. A significant association of duration of surgery was found with medpore (p = 0.031) and Navigation (p = 0.022). Use of medpore took minimal mean intraoperative time while reconstruction guided with navigation required maximum time, maybe as we were in a learning phase. The set up of intra operative navigation itself required 30-35 min. Also the reconstruction was done with calvarial bone graft which in itself required more intra operative time.
All patients were observed overnight for a minimum of 24 hours for immediate post operative complications. However Shew et al 2 reported the average length of stay of their patients as 17 hours. Ectropion was seen in 27.27% patients, who were managed conservatively with gentle massage for about 6 months. Watery eyes presented in 31.81% patients either due to infection of eyelid, blocked tear duct or a cut/ scrape on the eye; but resolved with time. Infection was controlled by systemic antibiotics, patients with blocked tear ducts were advised to place warm wet towel on the eye to help clear the blockage and all patients showed improvement. Out of 34.1% patients with preop diplopia, 13.6% still complained of diplopia post operatively which is within the reported range of 8-40% in the literature 30 while it was 21% in non-operated patients. Causes of persistent diplopia may be trauma to the muscle, fibrosis and muscle paresis. According to Hosal and Beatty 31 diplopia is likely to be seen in older patients and during delayed repair, in cases of periorbital tissues entrapment and damage. Out of 97.75% patients with preoperative hypoglobus, 13.6% patients still showed hypoglobus post operatively while it was seen in18% non-operated patients. Out of 84% patients with preoperative enophthalmos, 9% cases had persistent enophthalmos while it was 25% for non-operated patients. The reported incidence of enophthalmos postoperatively ranges from 7% to 27%. 32 Fat atrophy can be the cause of enophthalmos, but it may also be due to inadequate reconstruction of the orbital cone. Out of 75% patients with paresthesia, 16% complained the same postoperatively and 34% in non operated patients; however it improved in a year with a drug combination of methylcobalamin and pregablin. Methylcobalamin is a form of Vitamin B12 and pregablin belongs to the group of anticonvulsant. Post operative infection was seen in 6.8% patients and 11% in non operated patients, which was controlled by use of systemic antibiotics within a week. There was no post operative vision loss or graft/implant extrusion in any patient.
Different patterns of orbital fracture present the possibility of a severity bias. The other drawback of our study is that the groups of respective reconstruction material were not equally distributed as calvarial bone was used in 1 (2.3%), ear cartilage in 1(2.3%), medpore in 16 (36.4%), PCL sheet in 3 (6.8%), Titanium mesh 23 (52.3%), patient specific implant (PSI) in 3 (6.8%) and navigation in 2 (4.5%) cases.
There exists a possibility of surgeon’s bias as 3 surgeons, although of the same professional level and similar surgical skills, operated in our study. The material used was based on surgeon’s preference, their comfort with a specific technique, training and availability of material.
The success of each surgical procedure was scored by a single observer, who was not blinded to the study. So some observer based bias cannot be ruled out.
Conclusion
The incidence of orbital trauma is 4.15%. Orbital fractures are mostly impure fractures (91%), associated with zygomatic complex fractures, hence lateral wall fractures are seen more commonly. Patient specific implants, navigation guided reconstruction, autologous calvarial bone graft and preformed titanium mesh show better results, and fulfill the objectives of orbital reconstruction by restoring the normal anatomy and volume of the orbit. Operated patients had comparatively lesser post traumatic sequelae than non-operated patients.
However, a long term randomized study should be proposed to generate evidence for the best reconstructive option.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
