Abstract
Study Design
Case Report.
Objective
To discuss the case of a 55-year-old man who complained of swelling and pain in the left cheek.
Methods
Computed tomographic images showed a shadow of retained electric toothbrush head in the left infratemporal fossa, heterotopic free air, and abscess formation in the masticatory space. Foreign body removal and surgical drainage were performed under general anesthesia.
Result
The patient was discharged 6 days postoperatively.
Conclusion
Computed tomography should invariably be performed on patients with intraoral impalement injury.
Introduction
Oral and oropharyngeal trauma due to falling while holding an object in the mouth is often experienced by pediatric patients, but is less common in adults. Here, we present a case of an adult patient who had an intraoral impalement injury with an electric toothbrush head that reached the infratemporal fossa caused by a fall.
Materials and Methods
Case Description
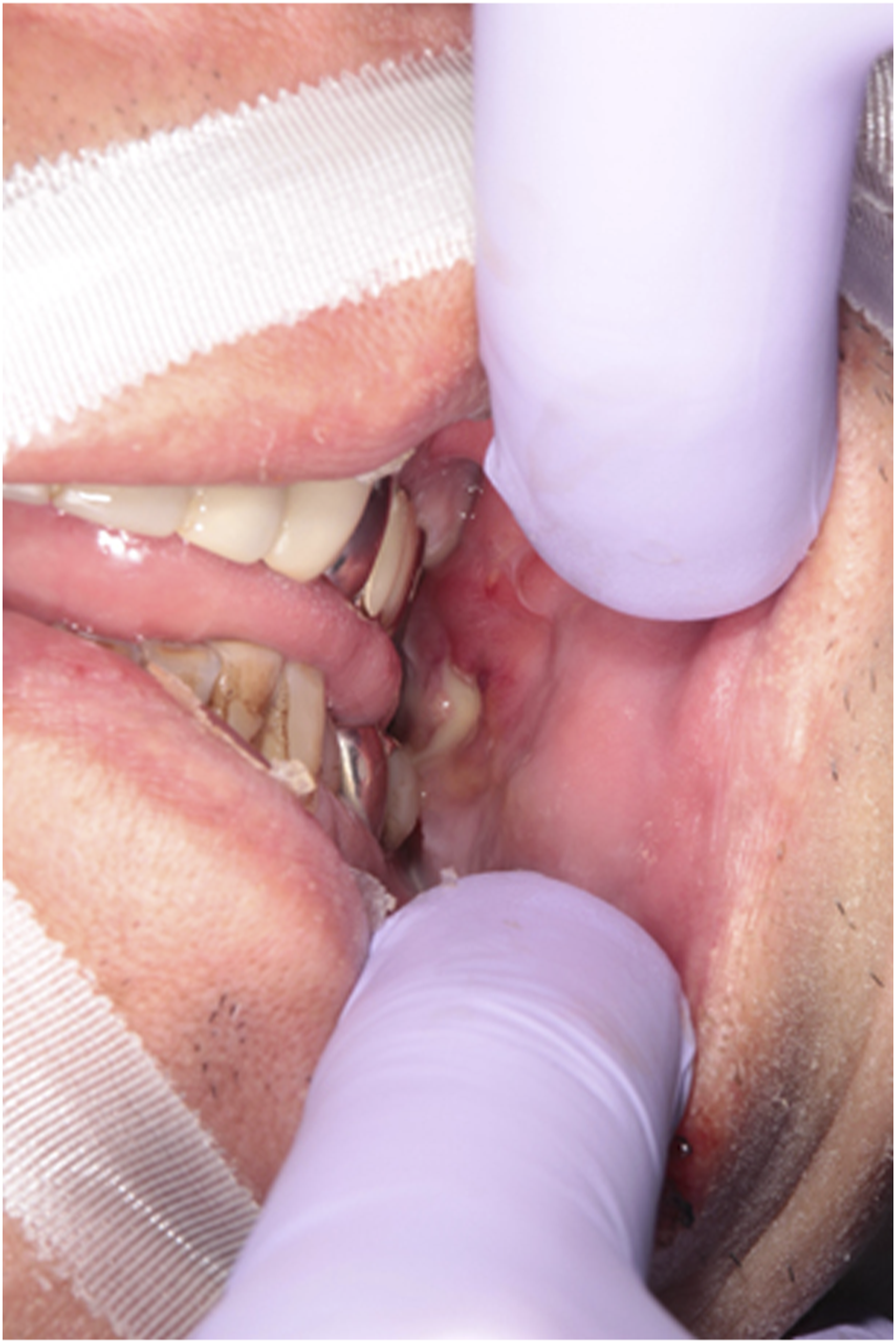
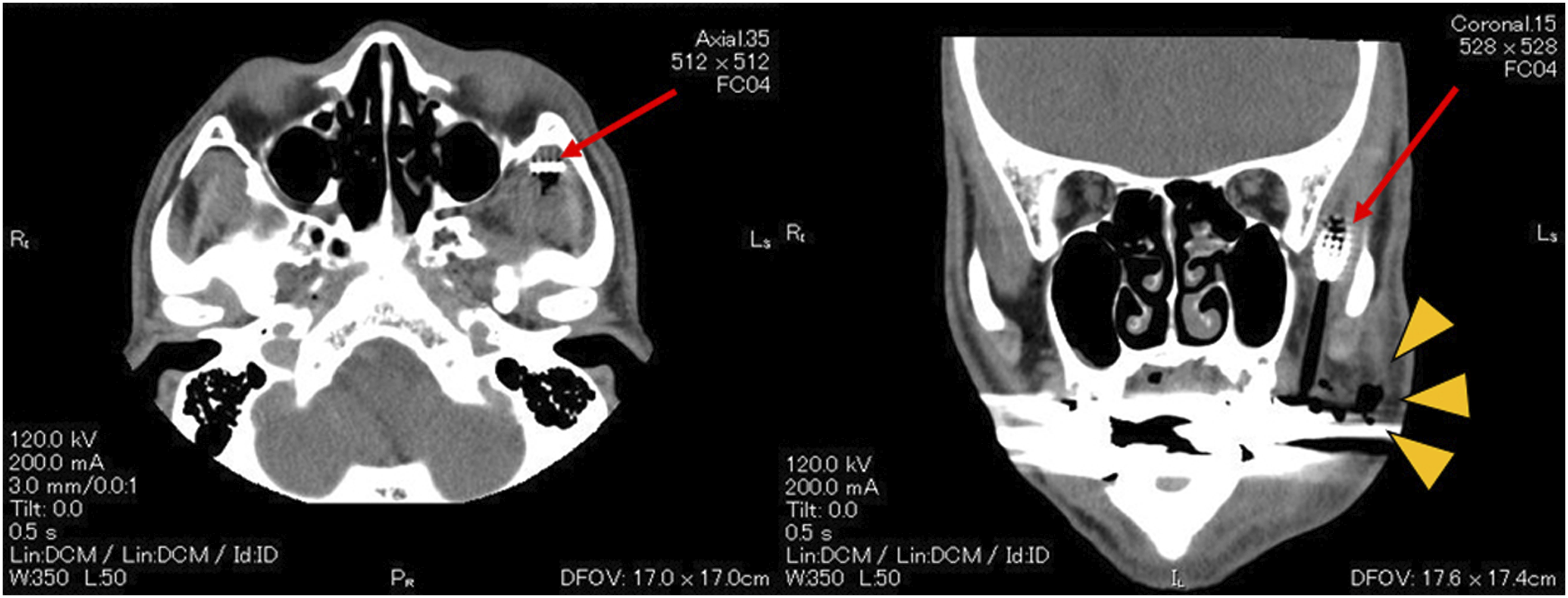
A 55-year-old man was referred to our outpatient clinic with a complaint of swelling and severe pain in his left cheek. He had no pertinent medical or surgical history. He had fallen down while using an electric toothbrush in a state of inebriation after drinking and lost the replaceable toothbrush head. He felt pain in his left cheek but was untreated. Three days after the injury, he visited the oral and maxillofacial surgery department in another hospital complaining of swelling and pain in his left cheek area and was sent home with a prescription of oral antibiotics. One day later, the patient visited the same hospital again because of worsened swelling. A computed tomography (CT) scan showed a shadow in the left infratemporal fossa that appeared to be the head of an electric toothbrush, and the patient was referred to our hospital for treatment. Diffuse swelling and erythema were observed from the cheek to the mandibular region. Erythema was also observed in the submandibular and anterior neck (Figure 1). Intraorally, an approximately 1 cm fistula in the left buccal mucosa and a significant amount of pus discharge were detected (Figure 2). The CT images revealed a shadow in the left infratemporal fossa, which appeared to be a retained head of the electric toothbrush. Furthermore, there was heterotopic free air and abscess formation in the masticatory space (Figure 3). However, we could not detect the toothbrush head due to severe trismus of one fingerbreadth and pain. Diffuse swelling was noted from the cheek to the mandible on the left side. Erythema extended to the anterior neck region. The fistula and the pus discharge from the impalement were found in the left buccal mucosa. The computed tomographic images indicate the retained head of the electric toothbrush in the left infratemporal fossa (red arrows) and the heterotopic free air and abscess formation in the masticatory space (yellow triangles).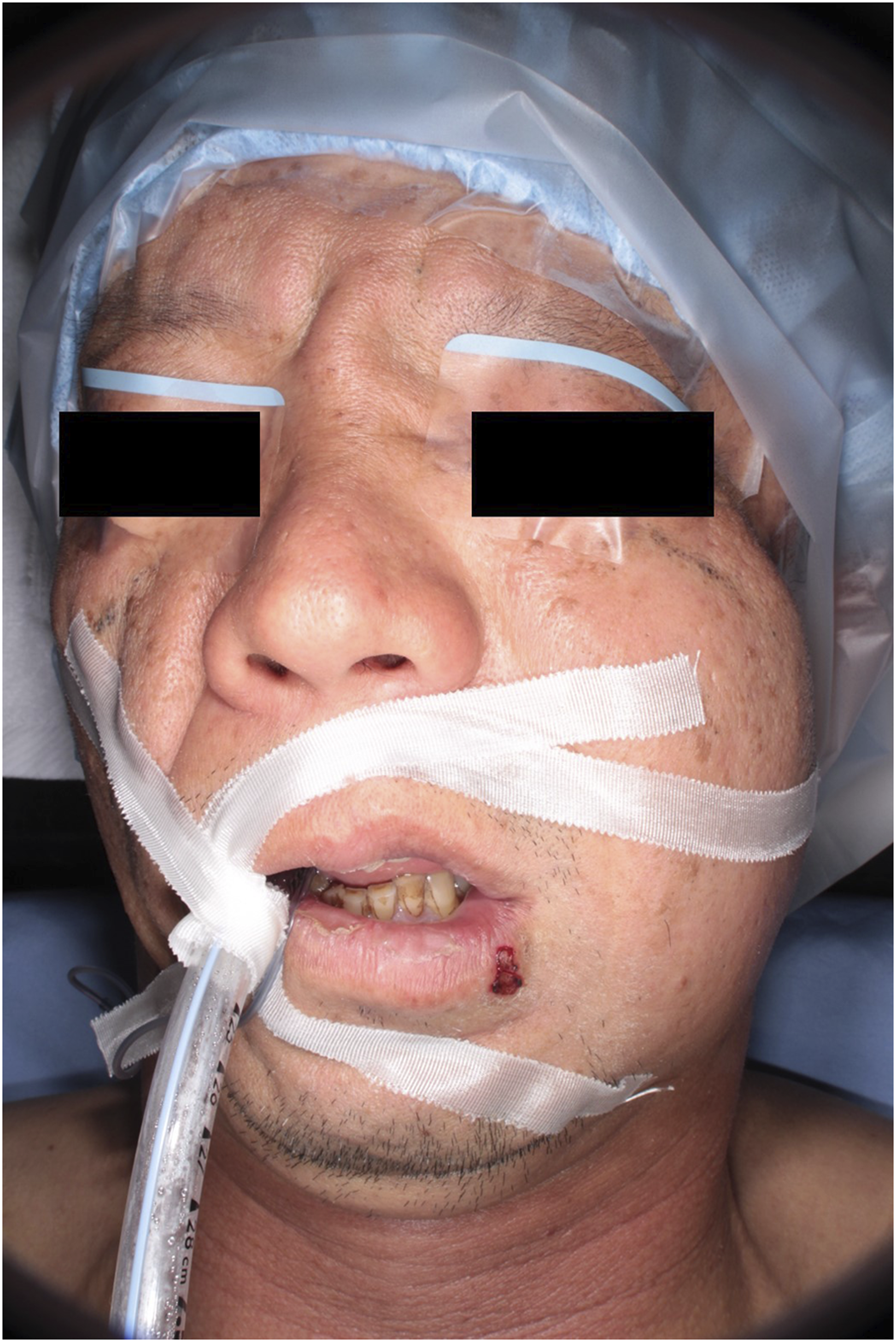
We decided to admit the patient on the same day and performed foreign body removal and surgical drainage under general anesthesia. We detected the retained toothbrush head in the fistula of the left buccal mucosa. The surgical incision was made from the fistula to the oral vestibule of the left maxilla through the posterior portion of the parotid papilla. We removed the head of the toothbrush and opened the masticatory space using forceps (Figure 4). After the wound was carefully irrigated with normal saline, a Penrose drain (6.0 mm outer diameter, 10 cm in length) was inserted, and an anchoring suture was placed on the surrounding mucosa. The removed toothbrush head was heavily soiled but not broken. (a) Intraoperative findings indicate that the foreign body was found in the fistula, and (b) A Penrose drain was inserted into the wound after the removal of the toothbrush head. (c) Removed toothbrush head was heavily soiled.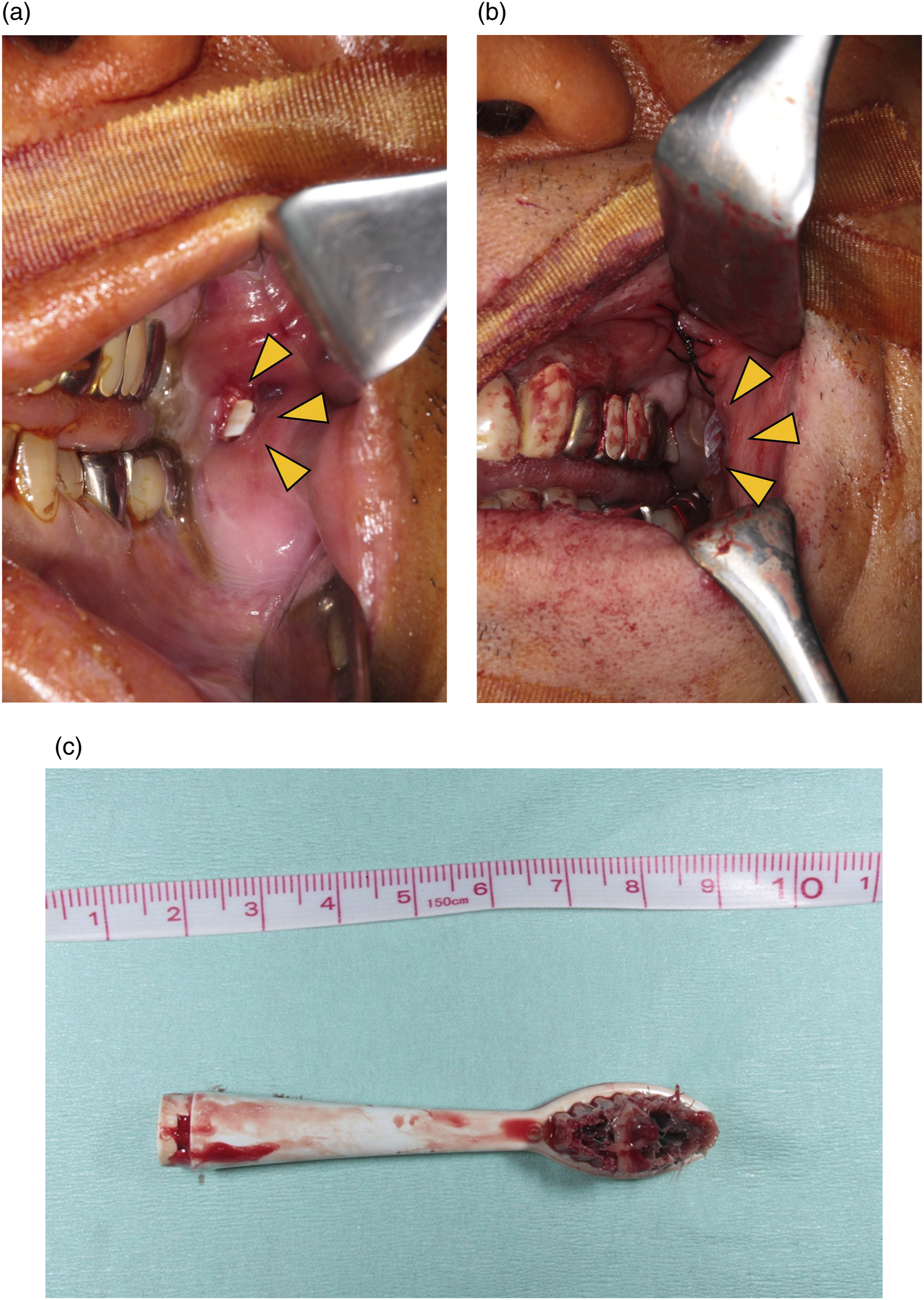
The patient was admitted to the intensive care unit (ICU) with tracheal intubation because the anesthesiologist observed glottal edema during tracheal intubation. One day postoperatively, the patient was extubated after confirmation of improvement of glottal edema with a leakage test. Two days postoperatively, the patient was discharged from the ICU and transferred to the general ward. Antibiotic treatment with sulbactam/ampicillin (3.0 g every 8 hours) was infused intravenously until 4 days postoperatively, and the drain was removed. The swelling of the cheek was reduced, and the patient was discharged 6 days postoperatively. He had been followed up in the outpatient service for 1 month, and the degree of mouth opening improved to the normal range.
Discussion
Impalement injuries in the oral and oropharyngeal areas are common in children who cannot understand the risk of moving while holding objects in their mouths. The most frequent mechanism of injury is falling while holding an object in the mouth or hands. The most common objects associated with these injuries include toothbrushes, toys, writing instruments, sticks, and in Asia, chopsticks.1,2 On the other hand, in adults, it is often associated with foreign bodies of medical origin (gauze, broken-off needles, or maxillary molars) or trauma in head and neck lesion.3-8 Except in cases of medical origin, foreign body oral intrusion into the infratemporal fossa is considered to be extremely rare.
If a foreign body remains in the soft tissue, it is relatively easy to remove it from the shallow layers. However, active intervention may be required if it remains in a deeper layer or if there is concomitant inflammation or a tissue defect that requires suturing. 1 Although there exist reports of the removal of foreign bodies using the intraoral approach, as in our case,6,8 the nasal approach3,4 or percutaneous approach is often chosen.5,7 In addition, several reports have described the removal of foreign bodies from the infratemporal fossa using intraoperative fluoroscopy, 7 navigation system, 3 or endoscopy.4,6 Most of the reported cases present with trismus or swelling of the head and face, all of which have been improved by surgery. Even after the removal of the foreign body, it is recommended that CT imaging be performed at the initial examination. It will help confirm the location of the retained foreign body or the presence of emphysema. It is also used to estimate the depth and length of the wound. 9 Impalement injuries in the oral cavity can cause damage to the facial nerve and maxillary artery and its branches. 10
In our case, removal of the retained electric toothbrush head succeeded with ablation directly from the insertion wound. Since the CT images showed free air in the soft tissue and abscess formation, we were able to perform surgical drainage by opening the infratemporal fossa. However, an additional contrast-enhanced CT scan should be considered to evaluate the extent of the abscess. If the retained foreign body had been smaller, additional approaches, such as endoscopy, fluoroscopy, and navigation, as mentioned above, may have been necessary. Depending on the location of the foreign body, multidisciplinary surgical management with vascular surgeons or interventional radiologists in case of damage to the arteries or venous plexus might be necessary. 5
When we contacted the manufacturer, they stated that the following tests were conducted at the manufacturing plant for the electric toothbrush: ensuring that there was no tightness, inability to connect, or looseness in the connection part; repeat connection and disconnection for 100 times and confirmation of non-loosening at the connection part; application of a load of 300 g to the brush part; testing for 48 h, and confirmation of no loosening after operation. Therefore, it was thought that an external force greater than the manufacturer’s expectation was applied, which caused penetration and retention in the soft tissue. We believe that it is important to encourage consumers to use the product appropriately.
Conclusion
Here, we present a case of an intraoral impalement injury with an electric toothbrush head reaching the infratemporal fossa in an adult patient. CT is the key to diagnosis and follow-up in this type of trauma.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Consent for Publication
The patient has provided informed consent for publication.
