Abstract
Genial tubercle fracture (GTF) is rare and represents a diagnostic challenge as plain film radiography often fails to identify the fractured segment. Traumatic avulsion of the genial tubercle in conjunction with mandibular symphysis fracture may lead to posterior displacement of the tongue with the potential for airway compromise and difficulty in speech and swallowing due to loss of tongue anterior suspension. Fine cut computed tomography (CT) scan is required to confirm the diagnosis and assist further management. To our knowledge, all published cases of surgical intervention in the management of avulsed genial tubercle combined with fracture of the mandibular symphysis used an extraoral approach via submental skin incision to expose the fractured segment. To the authors’ knowledge, this is the first report to describe a transoral approach in the surgical management of GTF associated with a mandibular fracture.
Introduction
The genial tubercles serve as muscle attachments for the genioglossus and geniohyoid muscles which ensure optimal tongue movement and the suspension of the larynx during deglutition and speech. Genial tubercle fractures (GTFs) can be classified based on the mechanism of injury to type I: spontaneous unprovoked fractures associated with an edentulous mandible; and type II: associated with a mandible fracture.
Type I GTFs are thought to be due to propagation of microfractures secondary to trauma from a denture flange against the tendinous attachment of the genioglossus muscle. 1,2 Type II GTFs are rare with few reports in the literature. 2 –7 Risk factors for type I GTF include osteoporosis, female sex, and old age. 1 In contrast, type II GTF is often due to macro-trauma leading to avulsion of the genial tubercles with sudden loss of function, swelling, and potential airway compromise. 3 Given the nature of traumatic injuries, open reduction and internal fixation (ORIF) of GTF in order to reestablish tongue and airway support has been advocated.
Clinical signs of a GTF include sublingual and submental hematoma, dysphagia, odynophagia, and impaired tongue movement. The fractured segment can occasionally be palpated in the floor of mouth. Commonly used radiographs for diagnosing mandibular fracture, such as orthopantomogram (OPG) and posterior–anterior (PA) skull views, may not show GTF due to the superimposition of the mandibular symphysis over the cervical spine. Fine cut computed tomography (CT) scan (<1.0 mm thickness) is the imaging modality of choice when a GTF is suspected clinically.
The purpose of this report is to describe, for the first time, a case of surgical management of a type II GTF via transoral approach and to review the literature.
Case
An intoxicated 26-year-old male was a restrained driver of a vehicle with no airbags that rolled at 50 km/h. After self-extrication, the patient was brought to the Emergency Department of the local tertiary level hospital by ambulance. A primary survey showed no head or cervical spine injuries.
The patient complained of pain through his mandible and under his tongue. The patient’s airway was patent, but he was unable to speak in full sentences. He was tachycardic but the remainder of his vital signs were within normal range. There was swelling and a sublingual hematoma in the submental region, as well as the floor of mouth. The tongue was soft but superiorly and posteriorly displaced. OPG and PA mandible radiographs demonstrated mandibular symphysis fracture extending between the lower left central and lateral incisors (Figure 1).
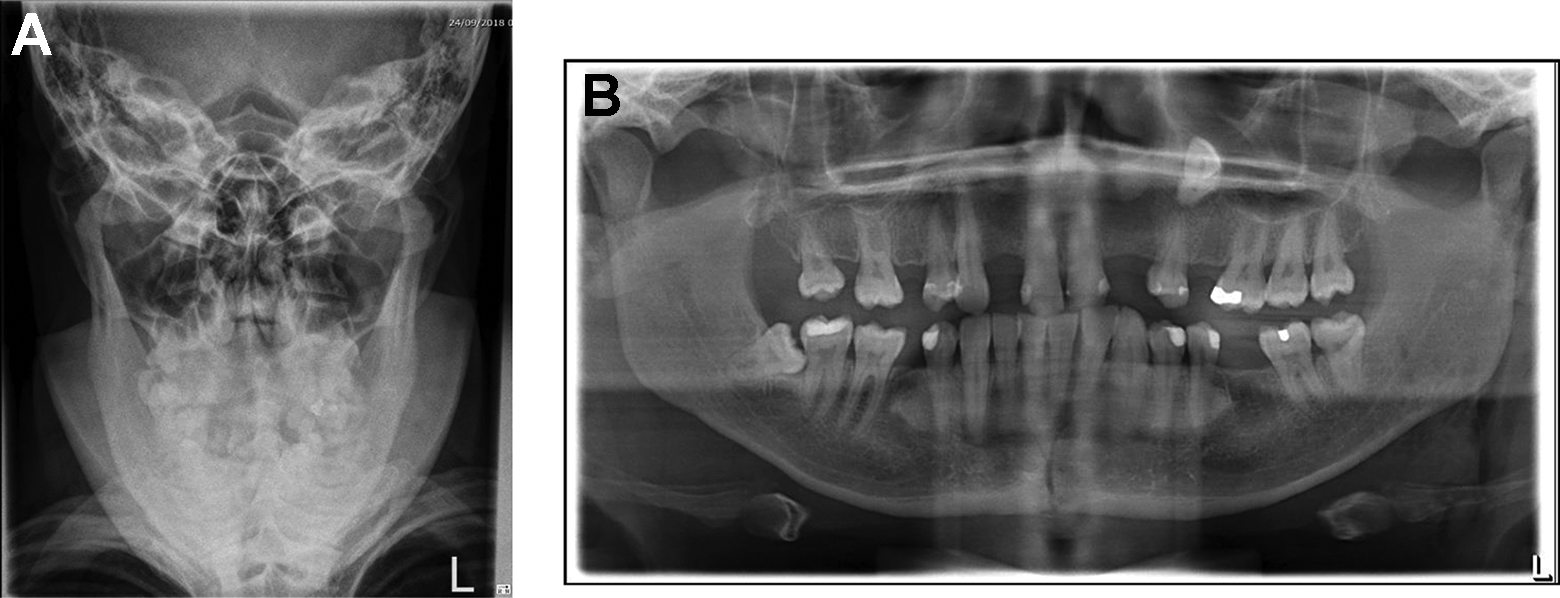
(A) Preoperative orthopantomogram and (B) posterior–anterior skull films showing symphysis of mandible fracture.
A CT brain and face revealed an avulsion fracture of the genial tubercle, posterior tongue displacement, reduced posterior airway space, and submucosal emphysema in the floor of mouth (Figure 2). Considering the patient’s symptoms and radiological findings, the decision was made to perform routine ORIF of the mandibular symphysis and associated genital tubercle fracture to suspend the tongue anteriorly.
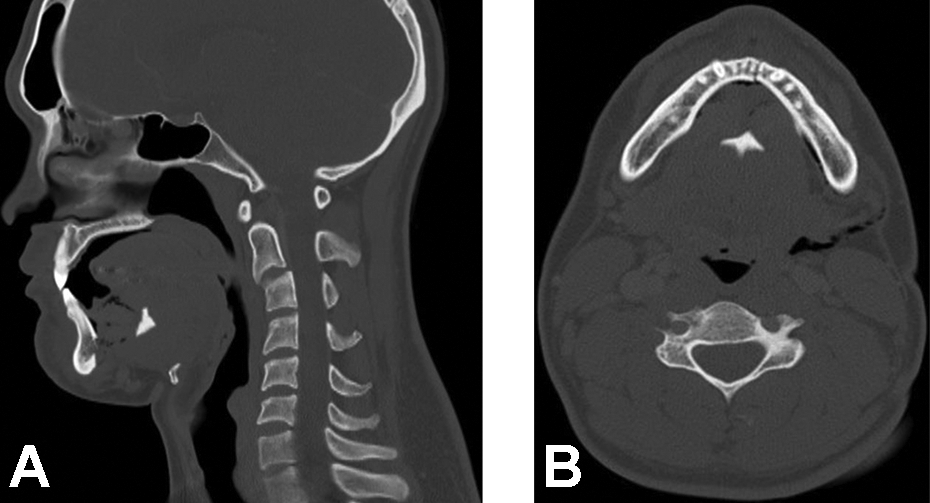
(A) Preoperative sagittal and (B) axial computed tomography images showing displacement of the avulsed genial tubercle in a posterior and superior direction relative to its native position at the symphysis of mandible. Gas locules are also seen within the soft tissue. There is reduced airway space at the naso- and oropharynx.
Surgical Procedure
The patient was anaesthetized via an awake fiber-optic nasal endotracheal intubation. The symphysis fracture was exposed via standard labial vestibular incision. A midline incision was made in the floor of the mouth identifying and preserving the two submandibular duct papillae. Dissection was performed through the midline avascular plane. The avulsed bone segment was identified with intact muscle attachment. This was manipulated and reduced to position. An 8-mm screw was secured to this bone fragment anteriorly and a 21-gauge stainless steel wire was then secured to the screw (Figure 3A). The wire was then passed through the fracture line to the labial aspect of the mandible. This was held temporarily with an artery clip and the symphyseal fracture was then anatomically reduced to achieve a stable dental occlusion. The fixation was carried out using superior and inferior border mono-cortical titanium bone plates and screws (Synthes Matrix Mandible Plating System). The stainless-steel wire was then pulled anteriorly to reduce the avulsed genial tubercle fragment. The wire was passed around and anchored to the inferior border plate (Figure 3B). The wounds closed with absorbable sutures. The tongue and airway were carefully inspected, and the patient was safely extubated. The patient was given intravenous steroid and antibiotics to reduce risk of postoperative infection and surgical site swelling.
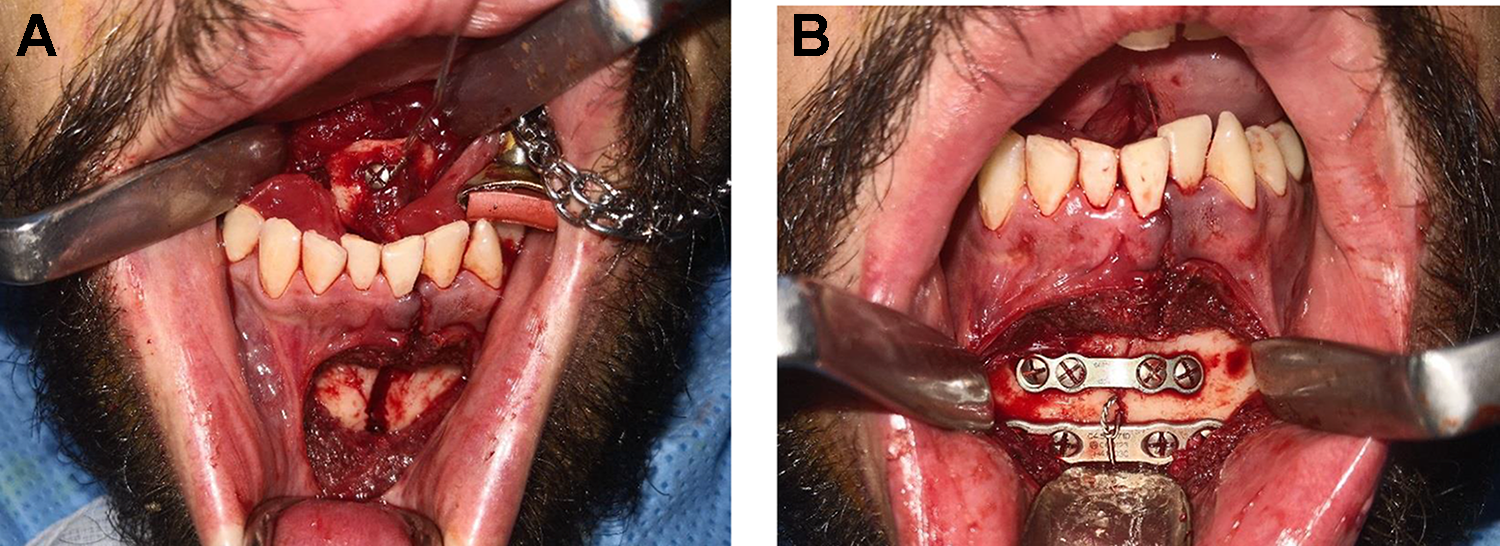
Intraoperative photographs. (A) Dissection between the bellies of the genioglossus muscles was performed to expose and secure the avulsed genial tubercle with an 8-mm screw. (B) Reduction of the symphysis of mandible fracture and resuspension of the avulsed genial tubercle with a 21-gauge wire to the inferior boarder plate.
Postoperative OPG and lateral cephalometric radiographs showed favorable reduction of the symphysis fracture and adequate repositioning of the avulsed genial tubercle (Figure 4). The patient was discharged uneventfully the next day.
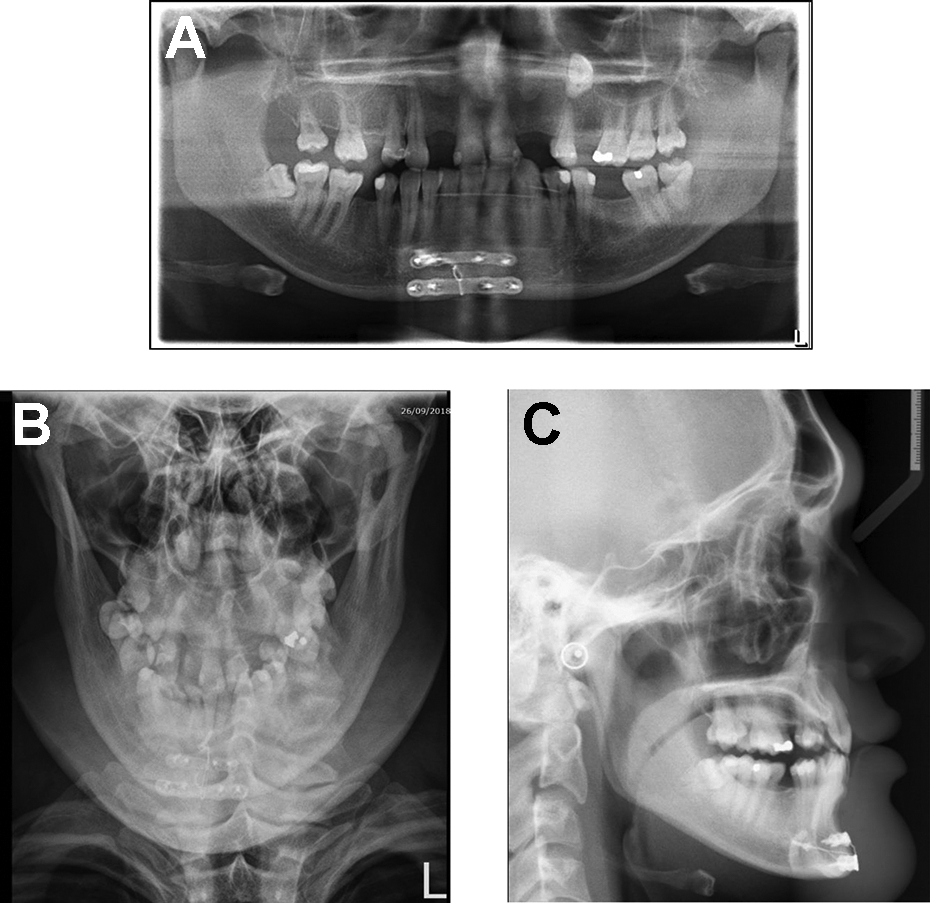
Postoperative (A) orthopantomogram, (B) posterior–anterior skull, and (C) lateral cephalometric films showing adequate reduction of the symphysis of mandible fracture and satisfactory repositioning of the fractured genial tubercle segment.
Discussion
There have been 6 documented cases of combined fractures of the mandibular symphysis and GTFs (type II). 3 –7 In these cases, when preoperative tongue mobility was normal, ORIF of the symphysis fractures only, leaving the genial tubercle to remain in an ectopic position yielded favorable results. 3,4 In contrast, three cases of type II GTFs had extensive floor of mouth edema, intraoral hemorrhage, and posterior displacement of the tongue causing obstruction of the parapharyngeal airway. 5 –7 This necessitated open reduction of GTF through either wire resuspension or screw fixation, all performed via extraoral submental skin incision. In these cases, fixation of the genial tubercle resolved respiratory distress and restored speech and deglutition.
Plain film radiography and tomography have great value and remain first-line imaging modalities for assessing mandible fractures in the emergency setting. 8 However, CT scan is more sensitive in fully characterizing mandibular fractures, particularly in the anterior mandible, compared with conventional OPG (100% vs 86%, respectively). 9
GTFs can be a diagnostic challenge due to the limited ability of plain films to clearly visualize this region 6,7 (Figure 1). In the present case, CT imaging was invaluable in determining the cause of pharyngeal obstruction and facilitated surgical planning. The authors recommend that fine cut CT should be the imaging modality of choice in cases where there is significant floor of mouth edema, hematoma, and acute loss of tongue support.
The decision to reduce and fixate a fractured genial tubercle in a type II pattern is based upon the presence of immediate threat to the airway, breathing, speech, and swallowing. While it has been reported that nonoperative management and protrusive tongue exercises can achieve a functional result with GTF, the authors advocate treating cases where there is a deterioration in aerodigestive symptoms and there is significant displacement as seen in the reported case, especially given the minimal morbidity of the described transoral approach.
In the reported case, the fractured genial tubercle fragment was retrieved transorally and secured with a 21-gauge wire. This did not impair fracture reduction anatomically nor affect the patient’s dental occlusion. A potential limitation of a nonrigid screw retained wire fixation is the risk of loosening of fixation and therefore close follow-up is recommended.
To date, publications of ORIF of GTFs have only been carried out through a submental skin incision via an extra oral approach. To our knowledge, this is the first report where a type II GTF was reduced and suspended through a midline floor of the mouth incision via a transoral approach. Such an incision is safe, simple, and bloodless. This approach avoids facial skin scarring, allows direct access to the floor of mouth and fracture segment, and dissection is associated with less morbidity, neck swelling, and bleeding compared with a submental approach. When there is an intraoral soft tissue laceration over the fracture line, a transoral approach simplifies tissue plane complexity and limits multiple surface contamination between skin and the oral cavity. One potential challenge with managing these fractures is the difficulty in locating the displaced fragment, which can occur regardless of approach. This was not encountered in the reported case, but the use of intraoperative imaging or navigation would be a useful adjunct for retrieval as well as confirmation of reduction.
While the authors acknowledge the limitations of this single case report, the described modified approach to managing a GTF adds to the body of literature. This intraoral approach can restore function without significant morbidity and should be considered as an alternative to an extraoral approach.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written and verbal consent obtained.
