Abstract
Evaluation of the airway is the first step in any trauma protocol, and this is particularly important in instances of facial trauma. While airway compromise is not uncommon in blunt or penetrating facial trauma, it is rarely a significant concern in instances of an isolated mandibular fracture. We report a rare case of immediate airway compromise in an elderly, edentulous female who sustained an isolated mandibular subcondyle fracture, complicated by her history of a remote hemimandibulectomy for management of her oral cancer. Initial airway management was performed conservatively with prone or lateral positioning under continuous pulse oximetry monitoring in the intensive care unit, followed promptly by open anatomic reduction and internal fixation of the fracture under more optimal operative conditions. After stabilizing the subcondylar fracture, the patient followed a mechanical soft/no-chew diet for 6 weeks until the fracture was healed. She has experienced no airway concerns since her surgery. This case report stresses the importance of a comprehensive evaluation of the airway in facial trauma patients with altered baseline anatomy, as well as highlights the considerations for emergent surgical airway versus immediate or delayed surgical fracture fixation.
Introduction
Evaluating and securing an airway are universally considered the first priorities in any trauma protocol, and this is especially relevant in instances of facial trauma. In a recent 10-year retrospective review at a level 1 trauma center, nearly 17% of patients suffering any facial fracture required airway intervention. However, the need for airway intervention after isolated mandibular fractures was significantly less, especially after blunt trauma. 1 Despite mandibular fracture incidence being as high as 25% of facial trauma cases in the young adult population, its incidence drops to less than 10% of facial fractures in those aged 65 years and older. 2 Elderly patients have higher rates of medical co-morbidities, coupled with atrophic edentulous mandibles with thinner bone and fracture patterns that are, on average, more displaced. As a result, nearly 1 in 5 mandible fractures results in chronic non-union, and this rate is shown to be even higher after attempting open reduction and internal fixation. 3,4 This has led some authors to advocate for closed reduction of mandible fractures in the elderly population when possible. 5
However, specific mandibular fracture patterns mandate operative fixation, sometimes emergently, even in the atrophic edentulous mandible where dental occlusion is not a concern. There have been several reports of flail segments of mandible, especially after multiple anterior fractures or severe comminution, with subsequent traumatic glossoptosis leading to airway compromise requiring urgent surgical intervention. 6,7 However, there has yet to be described in the literature an instance of profound airway compromise after a single, isolated mandibular fracture.
Case Report
An 89-year-old edentulous woman with a remote history of a right hemi-mandible resection for recurrent oral cancer suffered a mechanical fall at home, striking her face on the ground. She presented to the hospital emergency room several hours later complaining of left-sided facial pain and swelling, as well as immediate and significant difficulty breathing when lying supine or in a right lateral decubitus position. She was initially evaluated in the trauma bay, where her Glasgow Coma Scale (GCS) score was 15 and her first recorded vital signs were a blood pressure of 152/95, heart rate 70 beats per minute, respirations 19 per minute, and oxygen saturation of 97% on room air while sitting up. Physical examination revealed an edentulous oral cavity with deviation of her mandibular symphysis to the right. Palpation of her left oral vestibule revealed a prominent (closed) fracture line with the contiguous bony segment comprising the mandibular ramus, angle, and body being freely mobile. Notably, she was without the right hemi-mandible. Lying the patient supine in a controlled fashion resulted in complete collapse of the oral airway, resulting in immediate thrashing of the patient’s arms, air hunger, and oxygen desaturation. A standardized computerized tomography (CT) scan of her facial bones was challenging to obtain due to the inability to tolerate lying supine, but lateral position CT revealed a displaced left subcondylar fracture (Figure 1). The 3D reformat highlights both the left subcondylar fracture and the right mandibular resection (Figure 2). Cervical spine CT was negative for injury, as was the rest of her trauma evaluation.
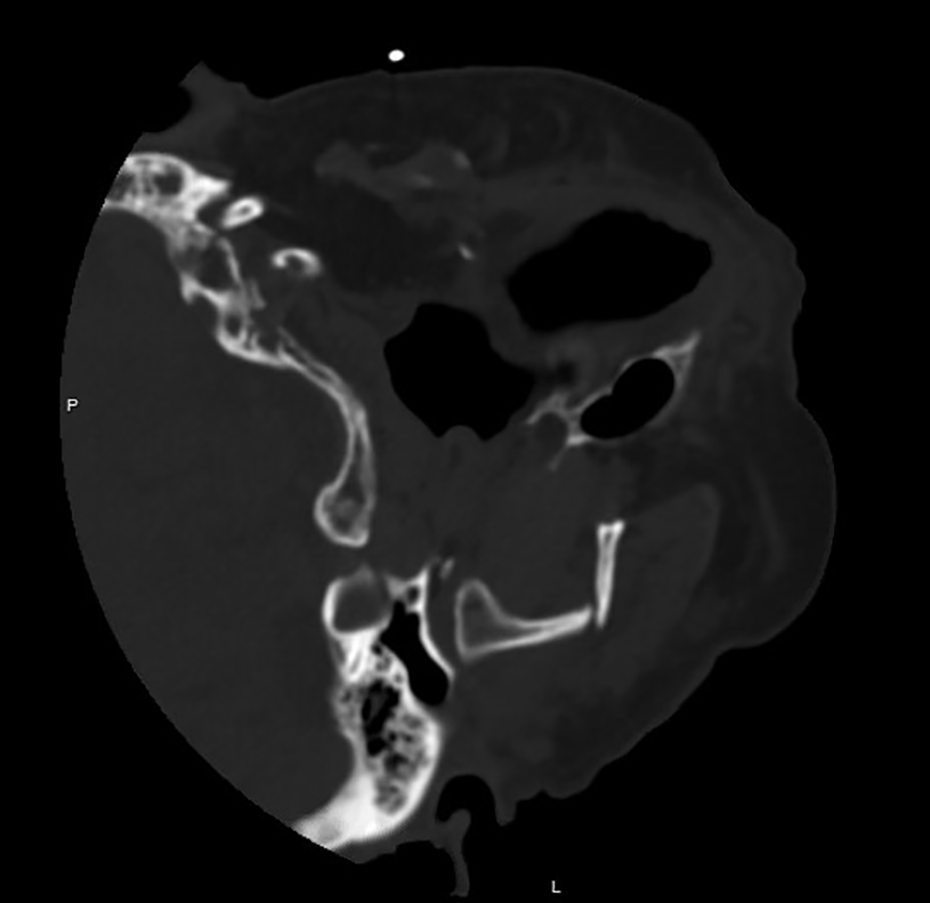
2D axial cut facial CT with patient in left lateral decubitus position revealing a displaced, angulated left mandibular subcondyle fracture.
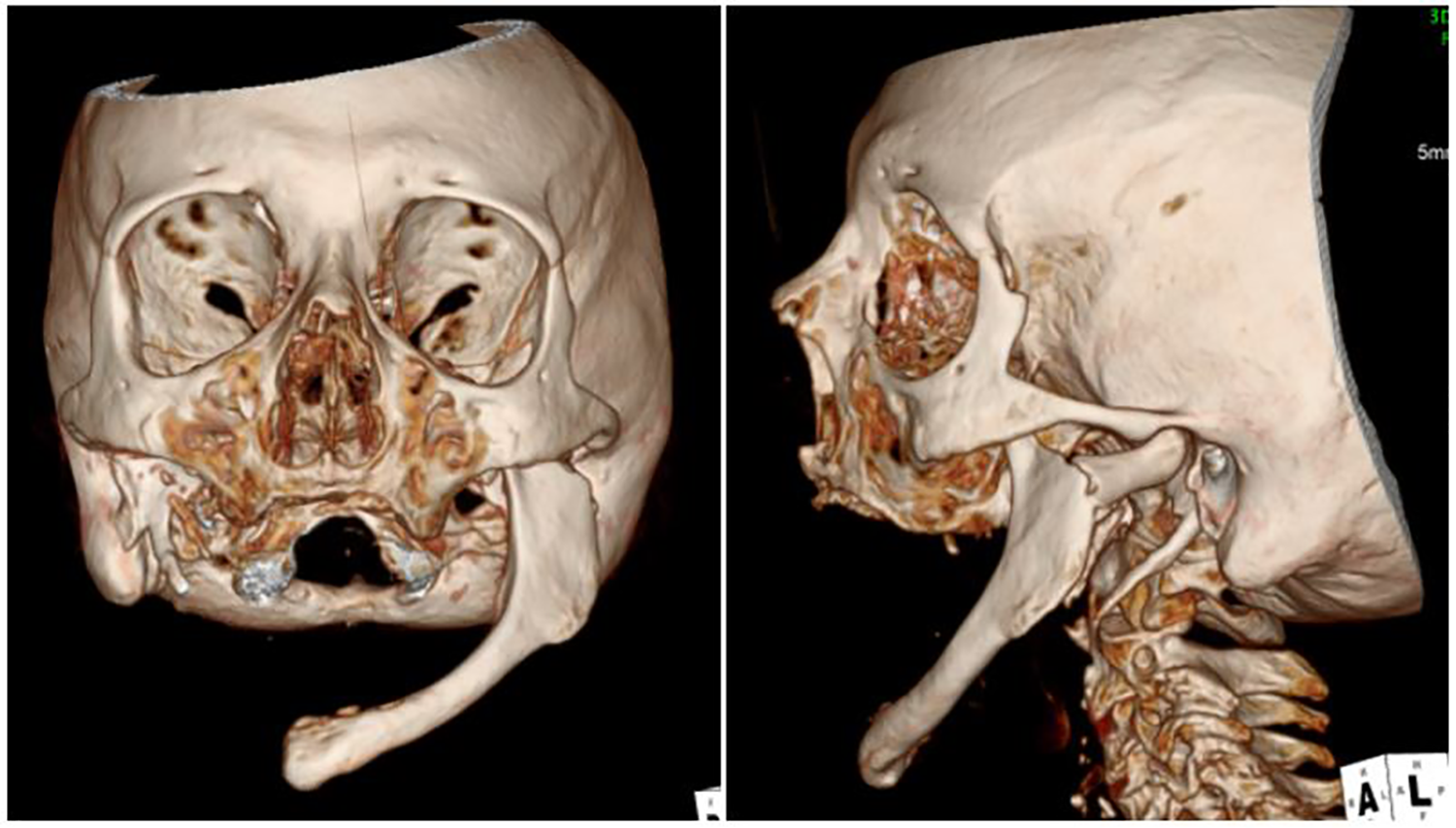
3D reformats of the preoperative facial CT highlighting the patient’s left hemi-mandible and associated fracture of the left mandibular subcondyle, with rightward rotation of the free-floating mandibular segment relative to the rest of the facial skeleton.
A conversation with the patient and her children revealed that the patient had lived with the absence of her right hemi-mandible since the 1970s when a previously reconstructed right hemi-mandible was resected after a recurrence of her oral squamous cell carcinoma. She had subsequently lost all of her mandibular and maxillary teeth. She ate by pushing food against her maxillary denture with her fingers to mechanically masticate the food, which she tolerated well for nearly 5 decades with little dietary restriction. Importantly, the patient also had active metastatic melanoma that was poorly responsive to current treatments. The patient and her designated medical power of attorney had previously expressed wishes to not attempt resuscitation (DNAR) of the patient in the instance of a medical emergency. However, in this circumstance, given the patient’s overall medical well-being, the patient and her family wished to temporarily suspend her DNAR order and proceed with intervention to stabilize her airway and mandible, albeit without attempting “heroic measures” or complete reconstruction. This would ultimately guide much of our decision-making.
Options for urgent management of her airway were presented, including intubation and immediate surgery versus observation in an ICU with prone or left lateral decubitus positioning and continuous pulse oximetry monitoring. Any delay would be followed by timely surgical open reduction and internal fixation of her fracture during daytime hours with more optimal operating room conditions. Because of the patient’s relative airway stability while sitting up or with left lateral decubitus positioning, the decision was made to observe the patient in the ICU overnight and take her to the operating room the next morning during daytime hours. Overnight, the patient maintained oxygen saturations in the mid to high 90 s in the ICU while sitting up or lying left side down.
She was taken to the operating room the following morning, where her left subcondylar fracture was accessed through a retromandibular incision. Anatomic alignment was achieved via direct visualization of the fracture while manually distracting the hemi-mandible. The fracture was reduced and secured with bone reduction clamps, and a single 6-hole locking reconstruction plate fixated the fracture with 3 screws on each side of the fracture line (Figure 3). The patient was extubated at the end of the case and was taken back to the ICU in stable condition for continued monitoring.
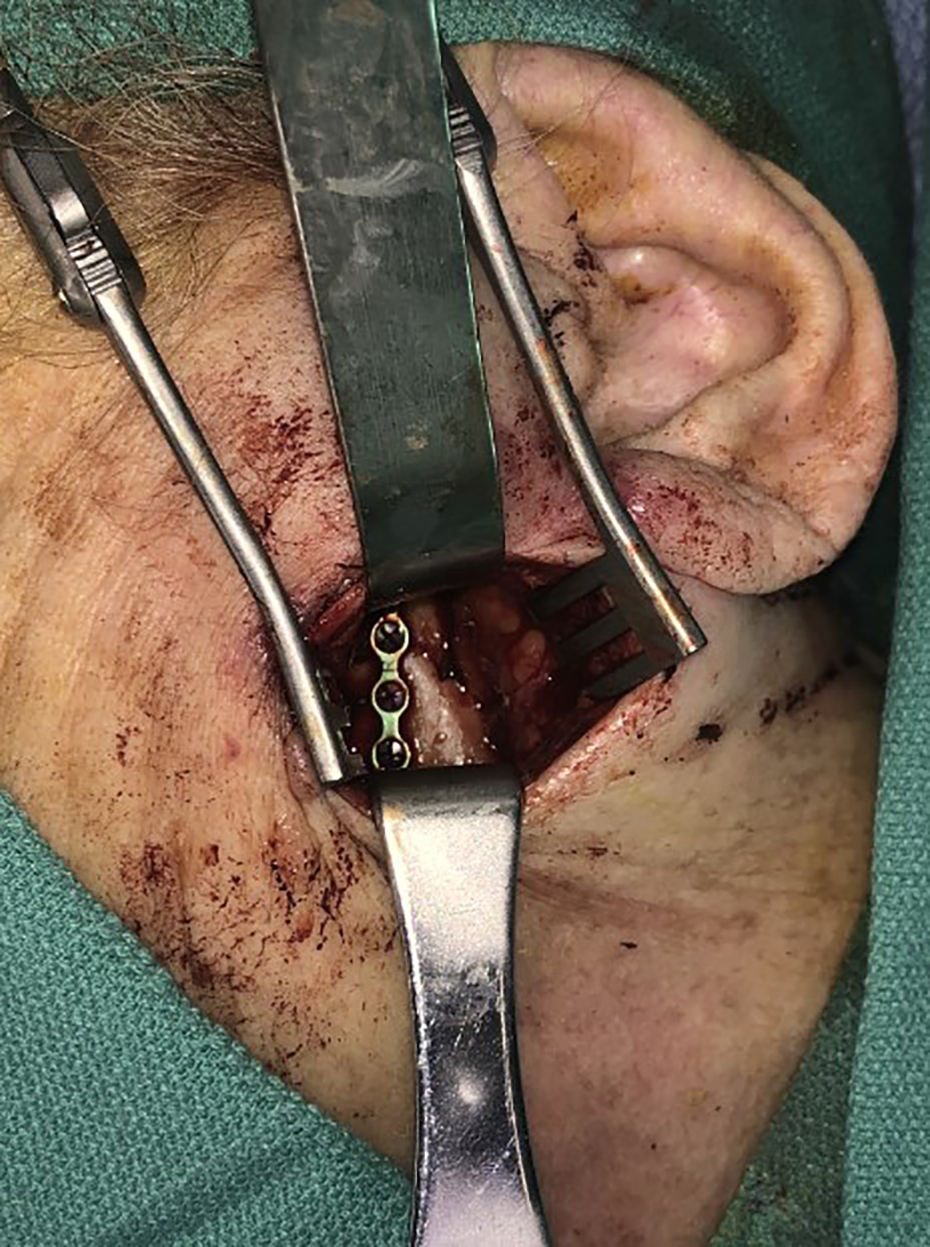
The fracture was accessed through a retromandibular incision and plated with a locking reconstruction plate, with 3 screws on each side of the fracture.
It is important to note that the patient suffered another fall in her hospital room on post-operative day #1, again with direct, blunt trauma to her face. Although her mandible appeared stable on physical examination and there was no concern for airway compromise, we obtained a repeat facial CT to evaluate the integrity of her mandibular reconstruction. The CT revealed a new small right anterior maxillary sinus fracture, as well as some mild angulation of the left mandibular condyle at the condylar neck (Figure 4). However, acceptable reduction of the fracture was maintained without compromise to the fixation, as well as good clinical and radiographic mandibular alignment with respect to the rest of the facial skeleton. The patient was discharged on post-operative day #13 with instructions to complete a 6-week no-chew diet. She was seen post-operatively in the clinic and was found to have secure rigid fixation of her hemi-mandible with no airway concerns.
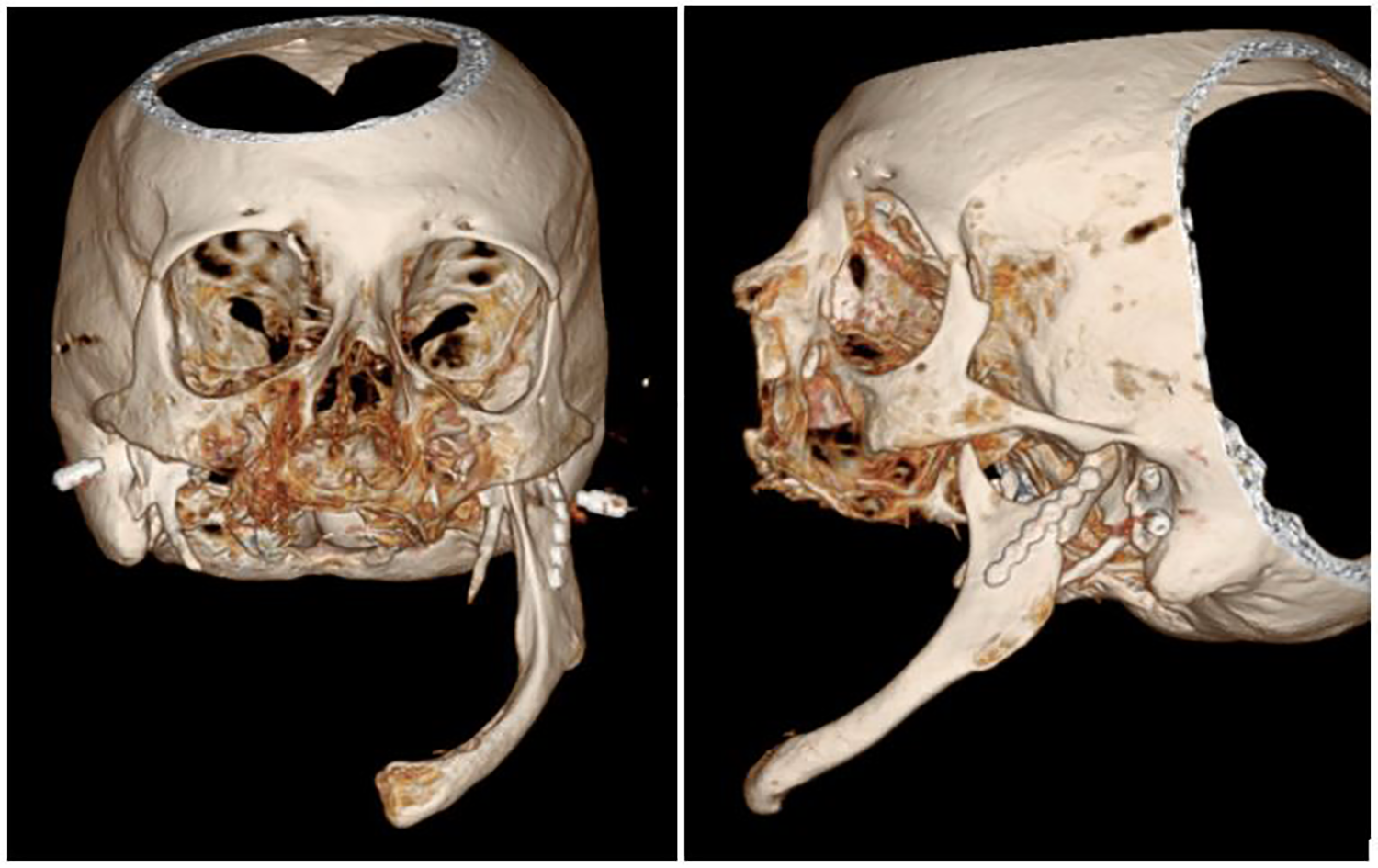
3D reformats of the post-operative facial CT highlighting the patient’s reduced and fixated left mandibular subcondylar fracture, with appropriate alignment of the mandible with respect to the rest of the facial skeleton.
Discussion
Facial trauma from falls in the elderly is hardly a rare occurrence. The Center for Disease Control and Prevention (CDC) reports that falls are the leading cause of fatal and non-fatal injuries in the elderly (≥65 years old). In 2014 in the United States, approximately 29 million falls in adults aged 65 years or older resulted in 7 million injuries, 2.8 million visits to the emergency department, 800,000 hospitalizations, and 27,000 deaths. 8 A large retrospective analysis of emergency department visits for fall-related injuries in the elderly revealed a nearly 11% rate of facial trauma. 9 This research infers that approximately 300,000 emergency department visits for fall-related facial trauma in the elderly population occur each year.
Nonetheless, mandible fractures make up less than 10% of facial fractures in the elderly and are much rarer than fractures of the nasal bones, orbits, or maxilla. 2 Furthermore, urgent or emergent airway interventions after mandibular fracture for blunt trauma are rare. In a retrospective analysis of 1,025 facial fracture patients by Tung et al., only 3 patients (0.3%) with isolated mandible fractures experienced airway compromise requiring emergent management. However, these were more likely caused by large neck hematomas in 2 of the patients, and disruption of tracheal cartilage in another. 10
As in any trauma protocol, evaluation of the airway is the universal first priority, and this becomes particularly relevant in facial trauma evaluations. Severe comminution or displacement of facial bones, sublingual hematomas, diffuse airway soft tissue edema, nasopharyngeal hemorrhage, or foreign body aspiration should all give clues to potential airway compromise. Yet rarely is a single non-comminuted mandibular fracture in the absence of other soft tissue trauma a predisposing factor. This case highlights the importance of a thorough history and astute physical examination, even before imaging is obtained. Prior to her fall, this patient had a free-floating anterior mandible, with the left temporomandibular joint (TMJ) providing the mandible’s only support. Once the subcondylar fracture disrupted the continuity of the mandibular ramus, angle and body from the TMJ, there was no support to keep the patient’s remaining mandible and its surrounding soft tissues from falling into the patient’s oral cavity and obstructing her oral airway.
In situations of known airway compromise, serious consideration should be given to the type of airway intervention and its timing. Mismanagement of the airway or subsequent respiratory care has been identified as the most common cause of error leading to death in trauma patients. 11,12 However, emergent airway interventions are not without risks and must be considered thoughtfully when the indications are not absolute. In urgent or emergent settings, intubation outcomes are poorly influenced by repeated intubation attempts, inadequate visualization and the need to perform direct laryngoscopy without muscle relaxation, and lack of operator experience. These factors have led to complication rates in urgent or emergent intubations that exceed 20%, including esophageal intubation, aspiration, hypoxemia, esophageal tear, cardiac arrhythmias, or cardiac arrest. 13,14 Because of near-normal respiration and oxygenation of this patient in the sitting position, and after considerable discussion between the ICU trauma surgeon, respiratory therapist, and craniomaxillofacial (CMF) surgical team, the decision was made to carefully observe the patient in a critical care setting with continuous oximetry monitoring and strict position control until she could undergo surgery the following morning under more ideal operative circumstances.
Goals in mandibular reconstructive surgery are generally 3-fold: restoring proper dental occlusion, achieving functional movement, and restoring pre-trauma lower facial aesthetics. This patient was edentulous at presentation, so dental occlusion was not a significant consideration. With no direct trauma to her temporomandibular joint and no intra-capsular fracture, her function could be restored with open anatomic reduction and internal fracture fixation. Lower facial aesthetics would then be restored to the patient’s pre-morbid state. Of critical importance was to secure the fracture with a stable enough construct to stent open the patient’s soft tissues and prevent them from collapsing into the oral airway until the bone was healed.
Given the considerations above, our preoperative surgical plan considered both the approach and the method of osteosynthesis. As opposed to an intra-oral incision, where the fracture would be difficult to expose and visualize, a retromandibular incision would allow for clear identification and avoidance of the branches of the facial nerve, allow for access perpendicular to the fracture for reduction and fixation, and would prevent the need for a transfacial trochar. Compared to the submandibular incision, the retromandibular incision is much closer in proximity to the subcondyle and requires far less dissection. Additionally, the patient had a history of multiple surgeries and radiation to the face and potential for altered facial soft tissue anatomy, so we determined to take the most direct access to the fracture with the best visualization.
Regarding the method of bony reconstruction, free autologous tissue transfer (e.g. free fibula flap) or a right custom TMJ implant may have provided ideal functional and aesthetic outcome in a younger, healthier patient, but these options were appropriately dismissed by the patient, her family, and the surgical team because of the patient’s age and metastatic melanoma prognosis. Once the possibility of complete mandibular reconstruction was excluded, the decision was made to proceed with anatomic reduction and plate fixation of the fracture. While we had planned to use two 4-hole miniplates, 1 along each of the anterior and posterior borders of the subcondyle, the bone proved to be extremely atrophic and thinned, and there unfortunately was room for only a single plate. Given single plate fixation, we opted for a 6-hole plate to allow for 3 screws on each side of the fracture line. The proximal 4 screws extended through the lingual cortex, but given the proximity of the inferior alveolar nerve distally, the distal 2 screws were placed in a unicortical fashion, which ultimately avoided new sensory loss in this patient. This method of osteosynthesis proved to be adequate, as evidenced by continued stability of her hemi-mandible and protection of her oral airway, even after her fall onto her face on post-operative day #1.
Conclusion
This case has significance because it highlights the importance of astute physical examination during trauma evaluations, especially in the vulnerable elderly populations and those with aberrant anatomy. When airway compromise is suspected, particularly from blunt mandibular trauma, the examiner must be extremely cautious when lying a patient supine due to loss of support for the soft tissues of the lower face and oral cavity. Even in such situations, it is not always necessary to perform emergent airway interventions, or even to fix the fracture emergently. As in this case, under scrutinous monitoring in the appropriate setting, patients may be observed for a short time before surgical intervention under optimal conditions.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
