Abstract
Study Design
Retrospective Case Series
Objective
This study’s objective is to identify gaps in facial trauma care by exploring 4 cases of delayed onset facial nerve palsy after temporal bone fracture.
Methods
A retrospective chart review was performed on 4 patients who presented to the emergency department with facial palsy after a previous trauma. Relevant physical exam findings, radiological images and follow-up was documented.
Results
We present a case series of young, previously healthy patients who presented to the emergency department days or weeks after traumatic temporal bone fracture with delayed onset unilateral facial nerve paralysis. None of these patients were warned of this potential complication, connected to an outpatient physician and all received a costly workup.
Conclusions
Patients presenting with temporal bone fracture and intact facial nerve function can develop delayed-onset facial paralysis several days after their injury. To offset costly and stressful return visits to the emergency department, patients with temporal bone fractures along the course of the facial nerve should receive education regarding the possible delayed development of facial palsy prior to discharge and otolaryngological or primary care follow-up within 2 weeks of the injury.
Introduction
Facial nerve palsy is relatively uncommon after traumatic temporal bone fracture, occurring in 7-10% of cases. 1 While immediate onset paralysis is the most common presentation, delayed onset paralysis can occur up to 2 weeks after the traumatic event. The timing of this paralysis is an important consideration in management, as immediate onset facial paralysis suggests a potential facial nerve transection, while delayed onset facial palsy is believed to be due to inflammation and swelling compressing the facial nerve. In one series of 115 patients from 1984 to 1990, Darrouzet et al recorded delayed presentation of facial palsy in approximately 15% of cases of post-traumatic facial palsy after temporal bone fracture. 2
Electroneurography (ENOG) and electromyography (EMG) are common forms of facial nerve testing, and can be valuable diagnostic tools in the weeks following facial nerve paralysis.2,3 Surgical decompression may be indicated in cases with an immediate onset of complete facial paralysis and CT imaging suggestive of a facial nerve transection, or ENOG testing within 14 days demonstrating greater than 90% reduction in the amplitude of an evoked EMG compound muscle action potential. 4 Cases of delayed onset can be treated medically with a 10 day high-dose steroid taper (Prednisone is administered as 60 mg PO daily for 5 days, followed by a taper of 50 mg on day 6, then 40 mg, 30 mg, 20 mg, and 10 mg on day 10).4-6 Clinical tools such as the House-Brackmann scale, a 6-point score of upward eyebrow and outward mouth movement, are often utilized for assessment of facial palsy severity and to monitor improvement. Fortunately, prognosis in cases of delayed-onset facial palsy is good. In one series, 88% of patients with delayed-onset House-Brackmann grade V or VI facial palsy achieved grade I or II facial function within 12 months. Follow-up with a facial nerve specialist is often indicated for monitoring recovery and workup for any for complications (persistent hearing loss, CSF otorrhea or rhinorrhea, tympanic membrane perforation, persistent facial palsy or development of synkinesis).2,7
The sudden onset of facial paralysis, without prior knowledge of this potential adverse event, can be concerning for patients. Patients suffering temporal bone fractures tend to be younger and may not have a dedicated primary care physician or medical insurance; thus, delayed onset facial palsy can prompt costly return visits to the emergency department and unnecessary workups. 8 These ED trips cost the hospital system an average of nearly $3200 per visit. 9 At our institution, any patient with loss of consciousness or external signs of head trauma are screened with a head CT scan, undergo neurological checks every 2 hours, and stay for 24-48 hours depending on the severity of associated injuries. The otolaryngology service is consulted for all temporal bone fractures. 10 Specific guidance in addition to primary care or specialized otolaryngological follow-up should be offered at the time of discharge in patients with temporal bone fracture. Here we present a series of patients with temporal bone fractures whose onset of facial nerve palsy is 5 or more days after their initial trauma.
Case 1
A 30-year-old man with no significant medical history presented to our emergency department after a recent trauma. Six days prior, he was struck by a vehicle as a pedestrian and found to have a transverse fracture of the right parietal bone. This extended through the right parietal squamous cell suture inferiorly through the mastoid portion of the right temporal bone with extension through the external auditory canal (Figure 1), exiting along the posterior wall of the right temporal fossa and through the region of the petrous sphenoid suture. At the time of the trauma, he was found to have multiple small subarachnoid hemorrhages which remained stable on repeat imaging. No surgical interventions were indicated, and he was discharged one day later. On day 5 post trauma, he developed right facial numbness and weakness while eating. These symptoms persisted and prompted a call to the trauma service who sent him to the emergency department for evaluation. Transverse fracture of the right parietal bone extending through the right parietal squamous cell suture inferiorly through the mastoid portion of the right temporal bone (arrow).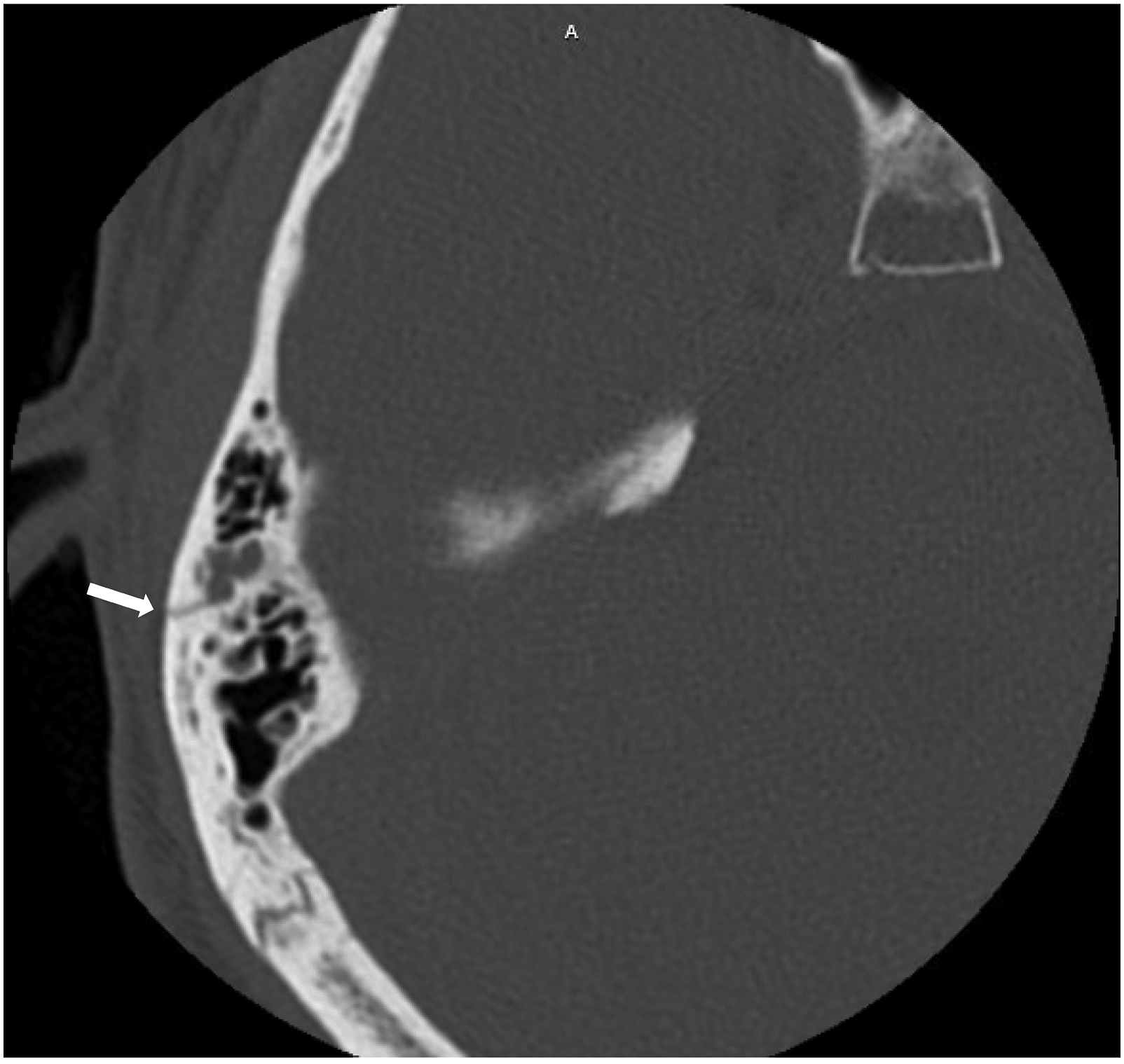
On exam the patient was noted to have facial asymmetry involving the right lip and upper eyelid. Mild sensory deficits in the V2 distribution were also noted. Repeat imaging was unchanged from previous and he discharged with urgent otolaryngological follow up. At his clinic visit 2 days later, he had a complete right facial nerve palsy (House-Brackmann VI), and was prescribed a six-day prednisone taper starting at 60 mg and eye drops. One week later he was seen by a facial nerve specialist with no improvement in his facial nerve palsy (Figure 2). He was concerned about returning to his work in the service industry in his current state and received an additional 10-day taper of oral prednisone starting at 60 mg. Demonstration of complete (House-Brackman VI) right facial nerve paralysis that developed 6 days after his initial injury. Note right brow weakness (b), incomplete eyelid closure (d), and asymmetrical smile (e and f).
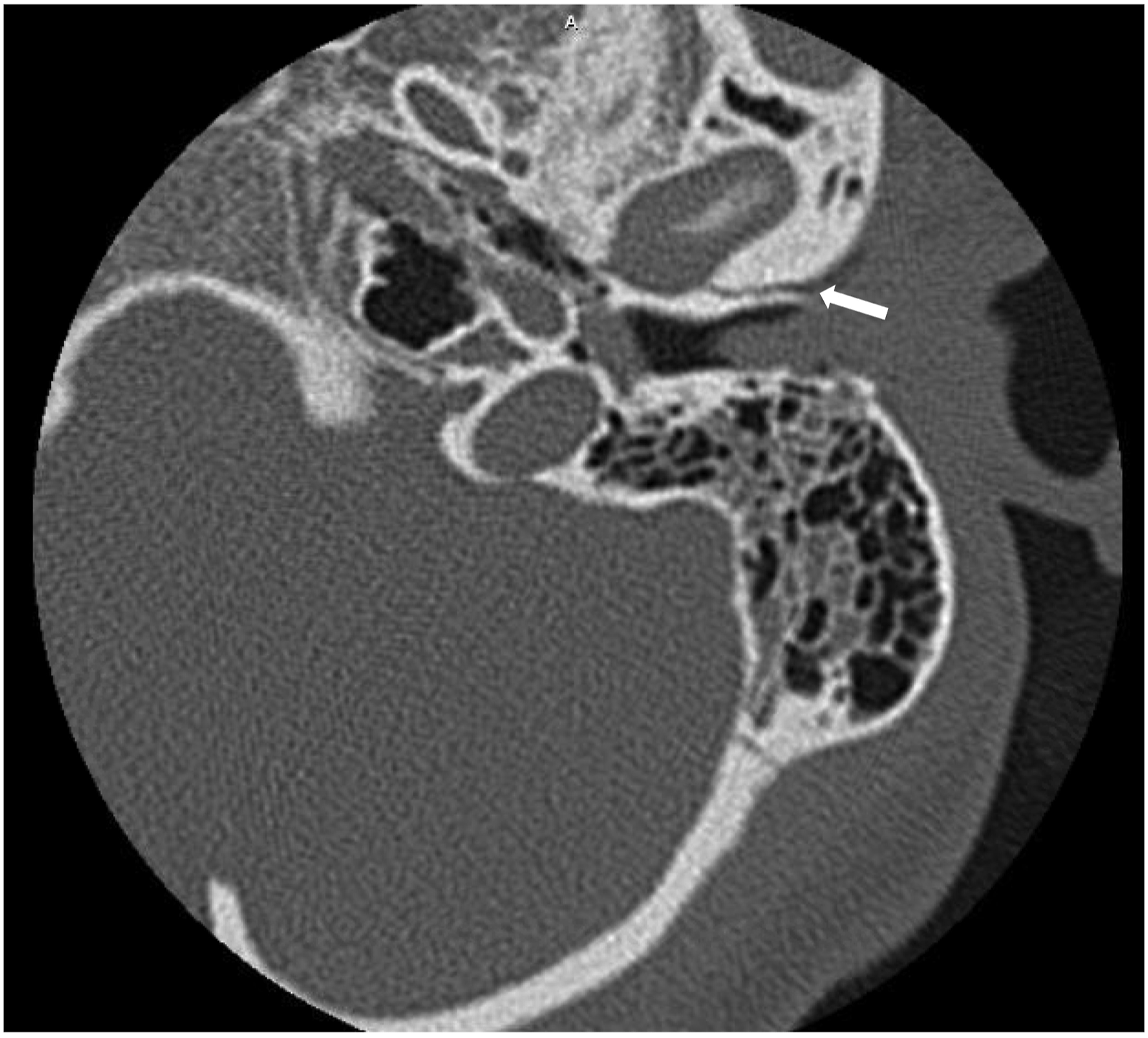
Two months after this visit, he returned to clinic with full facial nerve recovery (Figures 3 and 4). He endorsed complete resolution of his symptoms 5 days into his second course of prednisone. The chronicity of his symptoms and improvement did not warrant an EMG and indicated a low risk of developing synkinesis; therefore, he is currently followed as needed in clinic. Demonstration of complete recovery of facial nerve function for Case 1 after 2 months following treatment with 2 courses of oral prednisone for a total of 16 days. Longitudinal left temporal bone fracture involving the involving the mastoid and squamous portions and external auditory canal (arrow).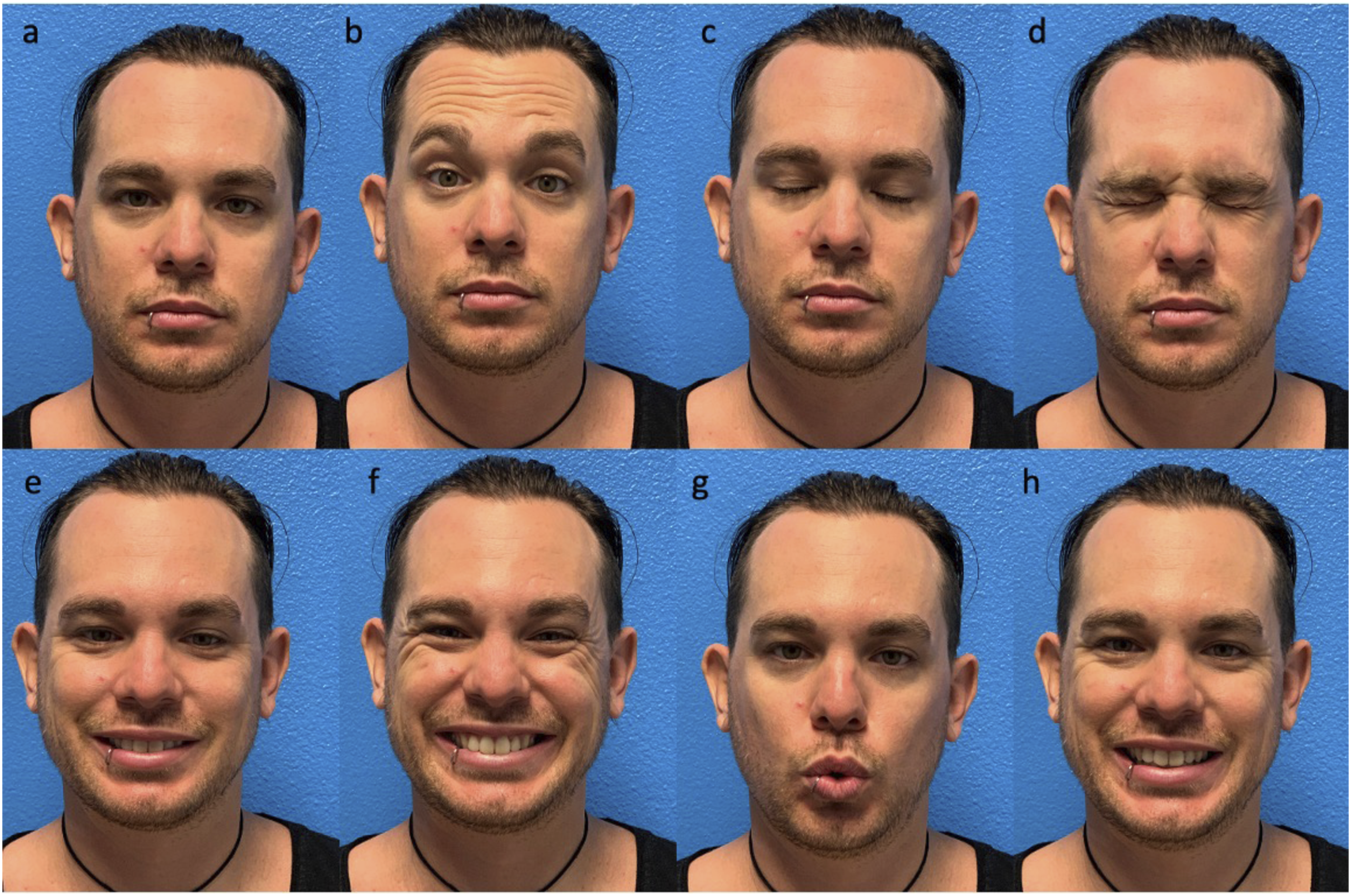
Case 2
A 25-year-old man with no significant past medical history presented to the trauma department after being hit by a car while crossing the street. On arrival, GCS was 14 and the patient was alert and oriented only to his name and location. He was assessed in the trauma department and found to have lacerations on his right eyebrow and left scalp. Physical exam was significant for subjective hearing loss, anisocoria, right face ecchymosis and right periorbital edema. No facial asymmetry or weakness was noted on exam.
Initial CT head showed a longitudinal left temporal bone fracture involving the mastoid and squamous portions and external auditory canal, with opacification of the right sphenoid sinus and focus of gas within the R cavernous sinus (Figure 5). Temporal Bone Reconstruction CT showed a possible right temporal bone fracture with trace mastoid air cell opacification and left hemotympanum along with the previously demonstrated left temporal bone fractures. He was assessed by ENT and neurosurgery who determined no urgent surgical intervention was necessary and he was discharged 2 days later. Longitudinal left temporal bone fracture (arrowhead) with extension through the lateral aspect of the mastoid bone (arrow).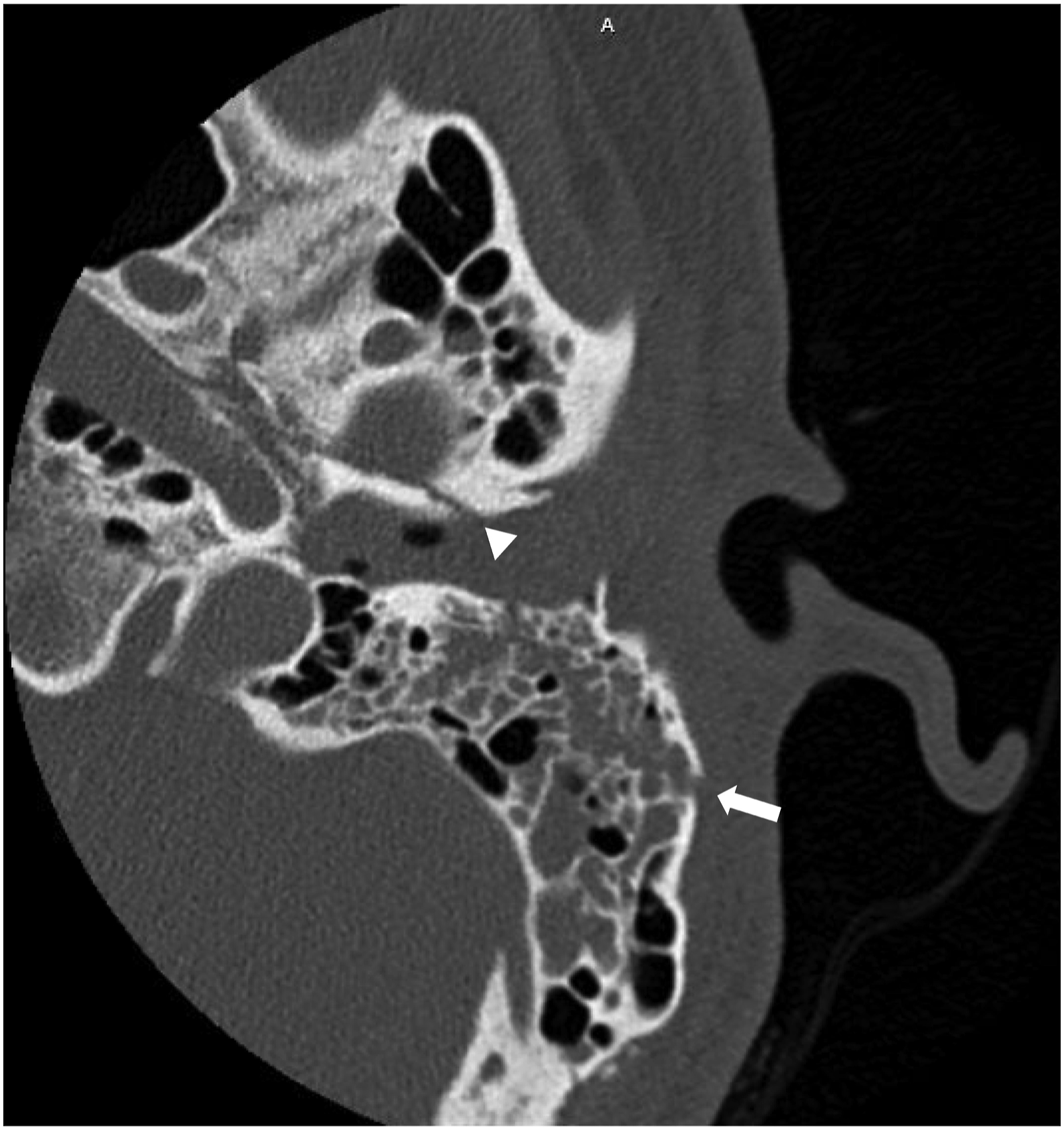
Fourteen days later he presented to the same ED with a complete left facial nerve paralysis (House-Brackmann VI). Conductive hearing loss secondary to the hemotympanum on the left had partially resolved. He was started on a prednisone burst/taper and was instructed to follow up with EMG and audiology testing along with a facial nerve specialist. An EMG the following day showed left CMAP amplitude in the nasalis and orbicularis oculi muscles were 29% (71% reduced) compared to the same muscles on the right. Additionally, the left CMAP amplitude recorded at the orbicularis oris was only 64% (36% reduced) of the right CMAP amplitude.
He was seen in clinic one month later and reported mild improvements in symptoms (House-Brackmann III). His facial nerve exam showed left brow weakness, left periorbital weakness but full eye closure with gentle and full effort, an effaced nasolabial fold, and small oral commissure movement with attempted smile but notable asymmetry. He was given artificial tears to use as needed, referred to facial physical therapy, and told to follow up in clinic in 6 months. During a phone call 4 months after the initial trauma, he reported complete improvement of his facial palsy and returned to work without restrictions.
Case 3
A 28-year-old male with no significant medical history presented to an outside hospital after falling from a skateboard at high speed and sustaining a head injury. Physical exam showed left hemotympanum and blood-tinged clear discharge from the left nares. Computed tomography showed multiple left temporal bone fractures, a small subdural hematoma, and pneumocephalus. ENT was consulted, packed the left ear and determined no need for surgical intervention. Serial imaging was stable, and the patient was discharged 3 days later.
Three days post discharge, the patient presented to our emergency department with intermittent confusion and anxiety. He received extensive CT imaging which showed a longitudinal comminuted left temporal bone fracture with involvement of the mastoid bone, basilar extension through bilateral carotid canals, and unchanged intracerebral findings. He was seen by both ENT and neurosurgery who recommended no surgical intervention and outpatient follow up. Six days later and a full 12 days after his initial injury, he presented again to our ED with 2 days of left-sided facial numbness and weakness, concerning for a stroke. He was reevaluated by ENT at this time who noted a left facial nerve paralysis (House-Brackmann III). The etiology of his facial palsy was determined to be edema secondary to his recent trauma, and he was prescribed a ten-day course of high dose prednisone at 60 mg per day followed by a five-day taper.
He was seen in a facial nerve specialist clinic 3 days after discharge and his facial palsy had mildly improved. On exam, he was noted have mild incomplete left eyelid closure with passive effort, asymmetric smile with restricted oral commissure movement, and small weakness of pucker and lower lip depressors. He reported significant stress regarding his condition and was counseled about the favorable prognosis for his symptoms. Given his improvement with steroids, he was not referred for EMG. He was seen 2 months later for follow up of his temporal bone fracture where his facial nerve palsy had completely resolved.
Case 4
A 16-year-old otherwise healthy female presented to the emergency department 4 days after a fall from a motorized scooter. She reported a brief loss of consciousness, right sided otorrhea, and hemotympanum at the time of the accident. She was evaluated by her primary care provider the day after the incident and was discharged home. On the fourth day after the accident, she reported right sided facial asymmetry and difficulty controlling her face. ENT was consulted and physical exam showed blood in the right external auditory canal and a right sided facial paralysis (House-Brackmann V).
Computed tomography scans showed an oblique longitudinal fracture through the right temporal bone, with disruption of the outer cortex of the mastoid, as well as numerous mastoid septae, violation of the middle ear cavity, with mild traumatic widening of the incudomalleolar articulation. There was also noted extension to the geniculate ganglion, through the tegumen mastoideum, and the ventral cortex of the pyramid. Anteriorly, there was minor extension of the fracture into the central sphenoid bone. No surgical intervention was indicated, and she was discharged the same day on a 10-day course of 60 mg daily prednisone with a week-long taper and ENT follow up. She was seen in a facial nerve specialist clinic 8 days after her initial presentation and her facial palsy had not improved. Facial nerve exam was notable for right brow paralysis, right periorbital weakness with ∼1 cm lagophthalmos with gentle closure, effaced nasolabial fold, inferiorly malpositioned oral commissure, and no oral commissure excursion with attempted smile. She was bothered by significant eye dryness and artificial tears were prescribed. On repeat follow up 3 months later, she had a near complete recovery with only trace brow/lower lip depressor asymmetry (House-Brackman II). She is currently being followed as an outpatient and monitored for development of synkinesis.
Discussion
Delayed onset facial nerve palsy is a relatively uncommon outcome after temporal bone fracture. 1 Because of its rarity, patients are not properly educated about the possibility of developing this symptom. This presentation may also become more common given the increases in facial trauma associated with the use of single rider vehicles like electric scooters. 11 The mechanism of injury in these cases is thought to be nerve compression from residual edema, making it a good candidate for medical management. Treatment is a course of high dose steroids, most often prednisone 60 mg for 10 days, followed by a short taper. 12 Additionally, exposure keratitis precautions are suggested, such as artificial tears at least 4 times daily, nightly ocular ointment, and taping or humidification chamber protection.
The prognosis for facial palsy with delayed onset is favorable, with most patient’s achieving House-Brackmann grade I or II. 13 Follow up with a primary care physician and referral to a facial nerve specialist in the event of delayed onset facial palsy is valuable to monitor for the potential complications of facial palsy, including synkinesis, hearing changes and education regarding the timeline for recovery.14-16 In our series, patients with incomplete recovery in the weeks following their trauma were counseled on the favorable prognosis and told to follow up within 3 months to monitor improvement.
In our series, all cases of delayed onset facial palsy presented within 14 days of the initial traumatic temporal bone fracture, and this is a similar timeline to previously published literature.1,2 The 4 patients included here tended to be younger and without significant medical comorbidities. These individuals did not have established primary care providers and received little to no guidance or education about potential sequelae prior to their initial discharge. This led to return ED visits, and prompted extensive, costly and stressful work ups. This series highlights the need for patient education regarding delayed-onset facial weakness and the need for follow-up with a primary care physician or a facial nerve specialist.
Conclusion
Patients presenting with temporal bone fracture can develop delayed-onset facial paralysis. To offset costly and stressful return visits to the emergency department, all patients with temporal bone fractures should receive education regarding the possible development of facial paralysis prior to discharge and have primary care or otolaryngological outpatient follow-up within 2 weeks of the injury.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written consent was obtained from the patient whose identifiable images were included in this study. Verbal consent was obtained from patients for the use of their deidentified case information.
IRB Statement
The Ethical Committee exempted the approval for this article, because it is a case series and the patients had signed the informed consent for the publication of their data.
