Abstract
Study Design
Case report.
Objective
A sialocele is a subcutaneous cavity containing saliva, caused by trauma or infection in the parotid or submandibular gland parenchyma, by ductal stenosis or glandular duct laceration with subsequent asymptomatic dilation and swelling. Many cases of parotid sialoceles have been published, but few cases of submandibular sialoceles occurring as a result of surgical trauma have been reported. The purpose of this article is to inform clinicians and to raise awareness about an unusual post-operative condition of a sialocele of the submandibular gland after treatment of a sequele of a mandible fracture.
Methods
We report a case of a 33-year-old male with a submandibular sialocele in the submandibular gland, that presented on computed tomography as a 10 × 4 × 3 cm right submandibular fluid collection in the submandibular space, and developed after an open reduction and internal fixation of a mandibular fracture through a submandibular approach.
Results
In the clinical case, the patient presented with sequelae of untreated fractures of the right angle and parasymphysis of the mandible. Both fractures had unfavorable deviations for 2 months, with a diagnosis of pseudoarthrosis, or non-union. In the first surgical stage, extensive debridement at the stie of non-union and precise anatomical reduction and fixation of the bone segments were performed via a submandibular surgical approach. The treatment of the post-operative sialocele occurred in a second surgical procedure, which included surgical exploration and right submandibular gland excision. No complications related to the post-operative approach were observed in a follow-up of 1 month.
Conclusions
Given the paucity of publications and treatment strategies for submandibular gland sialoceles in the literature, we hope to build a foundation to guide clinicians who encounter these rare adverse events. Surgeons will have a better understanding of the risks involved when they encounter cases like this, where extensive surgical debridement was necessary due to skewed consolidation and extensive pseudoarthrosis after the absence of immediate treatment following the initial trauma.
Introduction
Open treatment of mandibular fractures is typically regarded as a safe procedure with the more common complications including infection, hardware failure, osteomyelitis, non-union, malunion, and wound dehiscence. 1 Sialoceles are not commonly reported following this intervention. Sialoceles are characterized by extravasation of saliva into the surrounding soft tissue, and may be idiopathic, post-traumatic, or iatrogenic. 2 When they do occur, they typically involve the parotid gland since it is transected during the trans-parotid retromandibular approach.3,4 Accordingly, trauma to the parotid gland and subsequent sialocele formation is well described in the literature, as well as the management strategies.5,6 Trauma to the submandibular gland is comparatively less common than in the parotid due chiefly to the anatomic protection by the mandible.7,8 Therefore, there have been only a few cases of sialocele formation due to submandibular gland trauma reported in the literature. 8 Even more scarce are cases of submandibular gland sialocele formation from an idiopathic cause, for which 3 have been described. 9 To our knowledge, there is only one reported case of an iatrogenic, post-operative submandibular gland sialocele, which occurred after sialoadenectomy for sialolithiasis. 3 Management strategies for sialoceles include aspiration, drainage, botulinum toxin A injections, and surgical excision of the involved gland. 3 We present a case of an iatrogenic post-operative submandibular gland sialocele likely secondary to more extensive surgical intervention necessary to treat a non-union mandible fracture. This ultimately was treated with surgical excision of the submandibular gland.
Description of Case
A 33-year-old healthy male was referred to the oral & maxillofacial surgery clinic after sustaining a mandibular fracture of unknown mechanism 2 months prior while intoxicated. He had no recollection of the incident, and did not seek medical evaluation initially. He presented with a chief complaint of malocclusion and Hypoesthesia of the right mental nerve distribution. Cone-beam computed tomography (CBCT) revealed displaced fractures of the right mandibular parasymphysis and right mandibular angle (Figure 1). Top Left: axial cut of CBCT; Top Middle: coronal cut of CBCT; Top Right: 3D rendering of CBCT; Lower: panoramic reconstruction of the CBCT.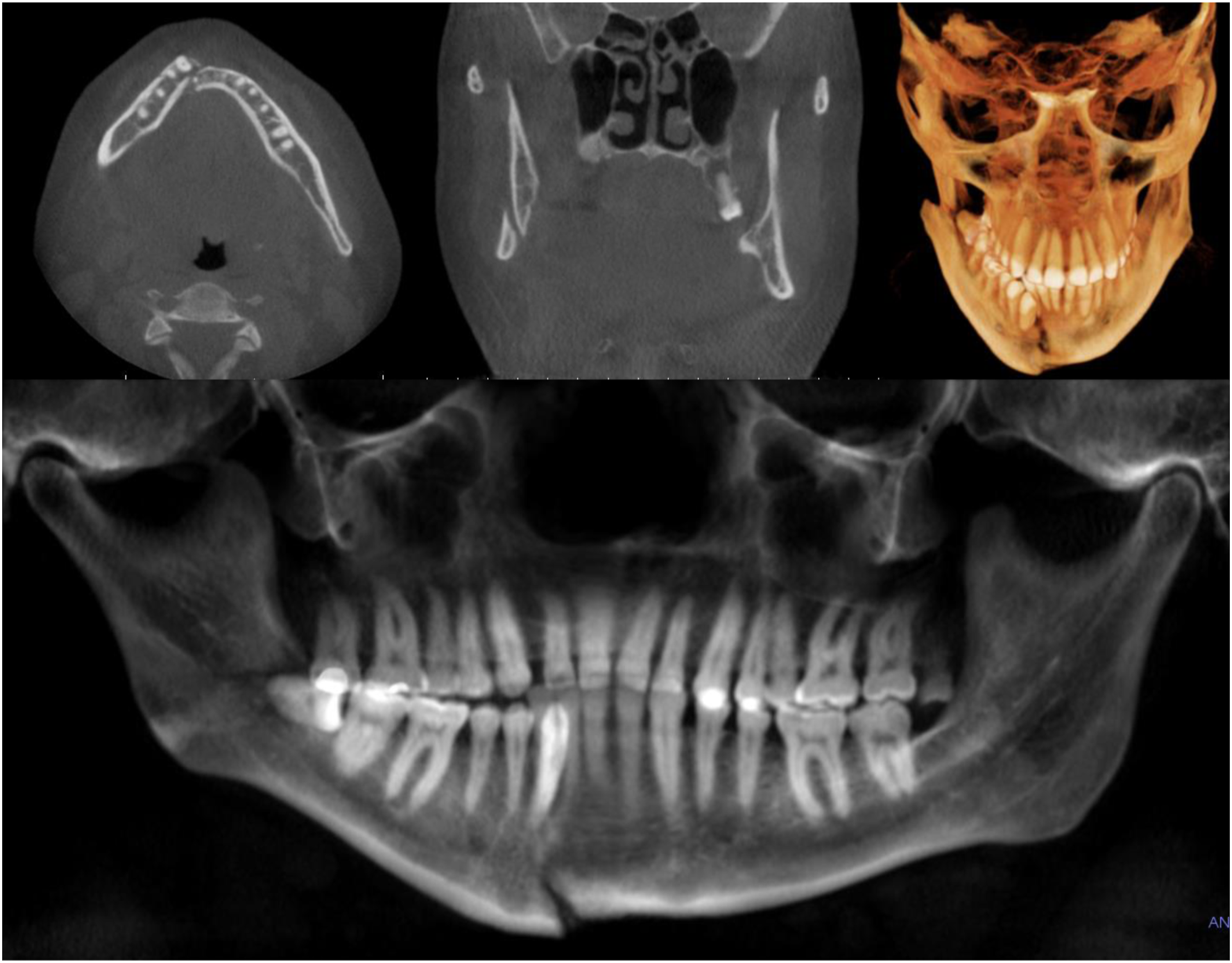
The decision was made to perform open reduction and internal fixation of the right mandibular parasymphysis and a right mandibular angle fractures via a submandibular approach. The submandibular gland capsule was incised and facial vein identified, ligated and reflected superiorly to protect the marginal mandibular nerve. Dissection was continued to the inferior border of the mandible. A periosteal elevator was used to expose right mandibular angle and parasymphysis fractures. Given the time lapsed from initial fracture and patient presentation, fibrous union of the segments was noted. This required significant debridement and re-osteotomizing at the site of fracture prior to reduction and fixation. Post-operative imaging was obtained showing condyles positioned within the glenoid fossa bilaterally, intact hardware, and radiographic alignment of the mandible (Figure 2). Post-operative panoramic radiograph showing anatomic reduction of the mandibular fractures, intact hardware, and condyles positioned well within the fossa.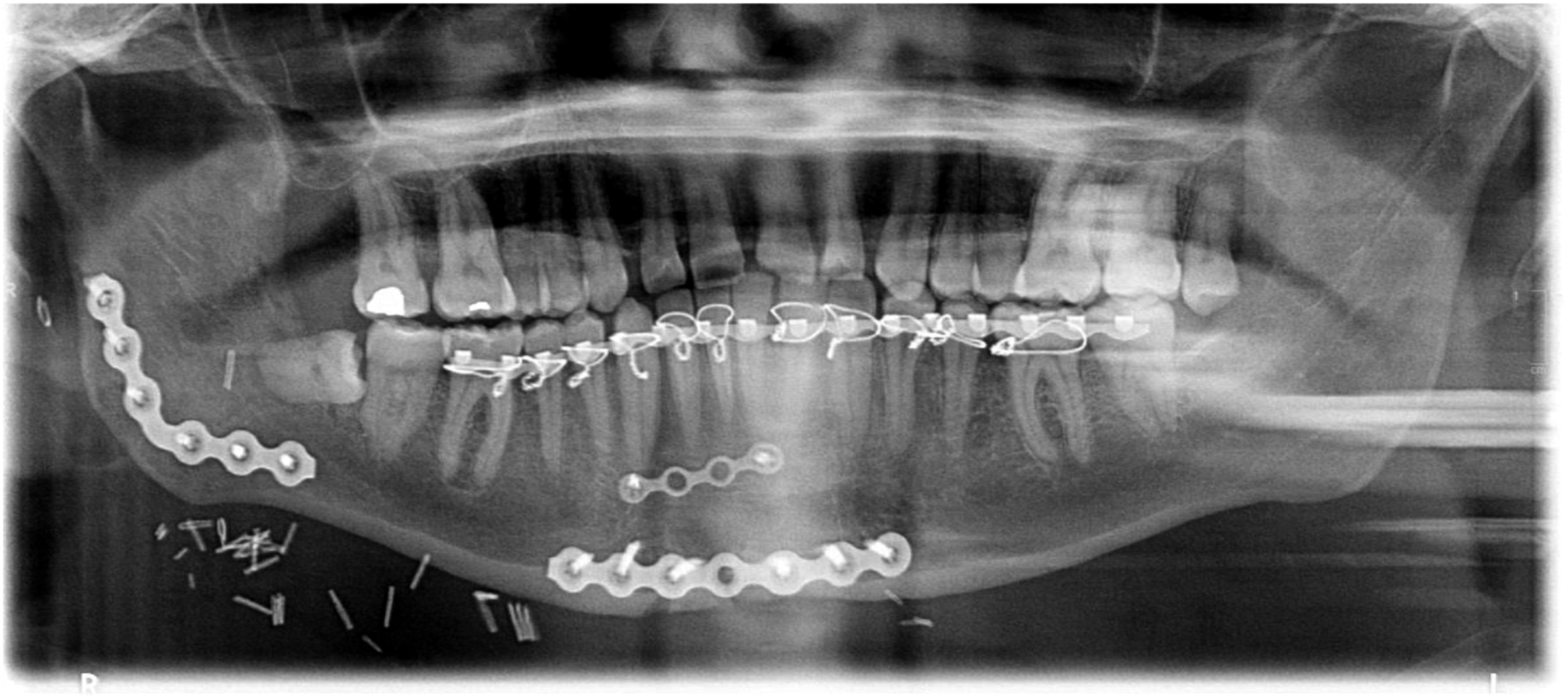
The patient presented for follow-up 2 weeks postoperatively and reported progressive swelling and persistent clear serous drainage from the submandibular incision which began 1 week after surgery. Physical examination revealed considerable fluctuant submandibular swelling with clear, serous fluid draining from the inferior portion of the surgical incision. (Figure 3). Computed tomography (CT) revealed a well-defined, hypodense ovoid fluid collection to the right submandibular space, measuring 10 × 4 × 3 cm (Figure 4). Extraoral photos showing fluctuant right sided submandibular swelling. CT scan showing a large (10 × 4 × 3 cm) right submandibular fluid collection in the submandibular space.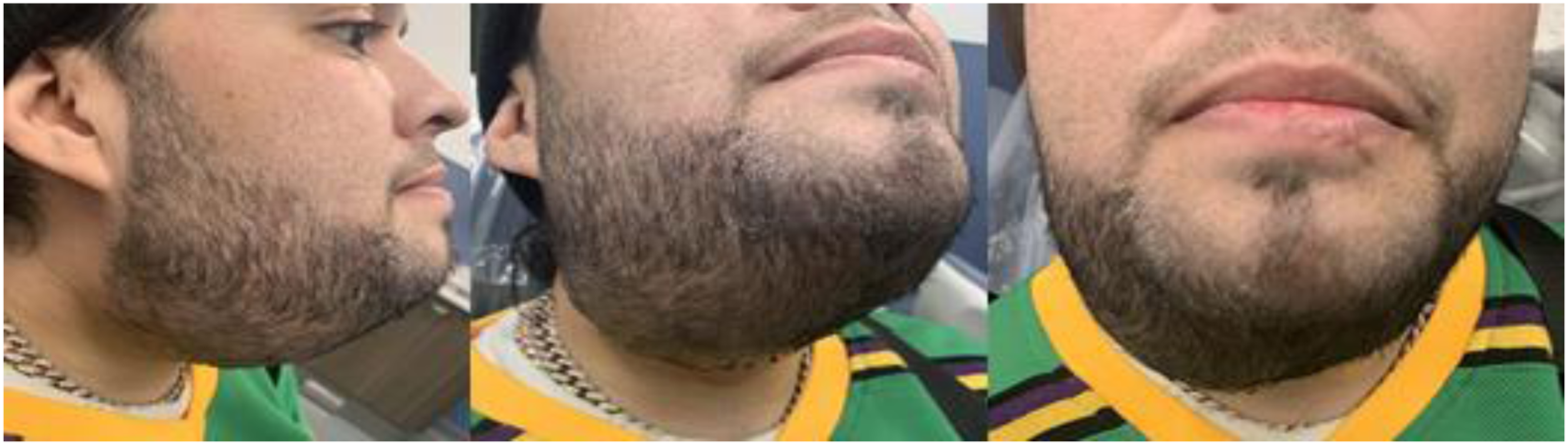
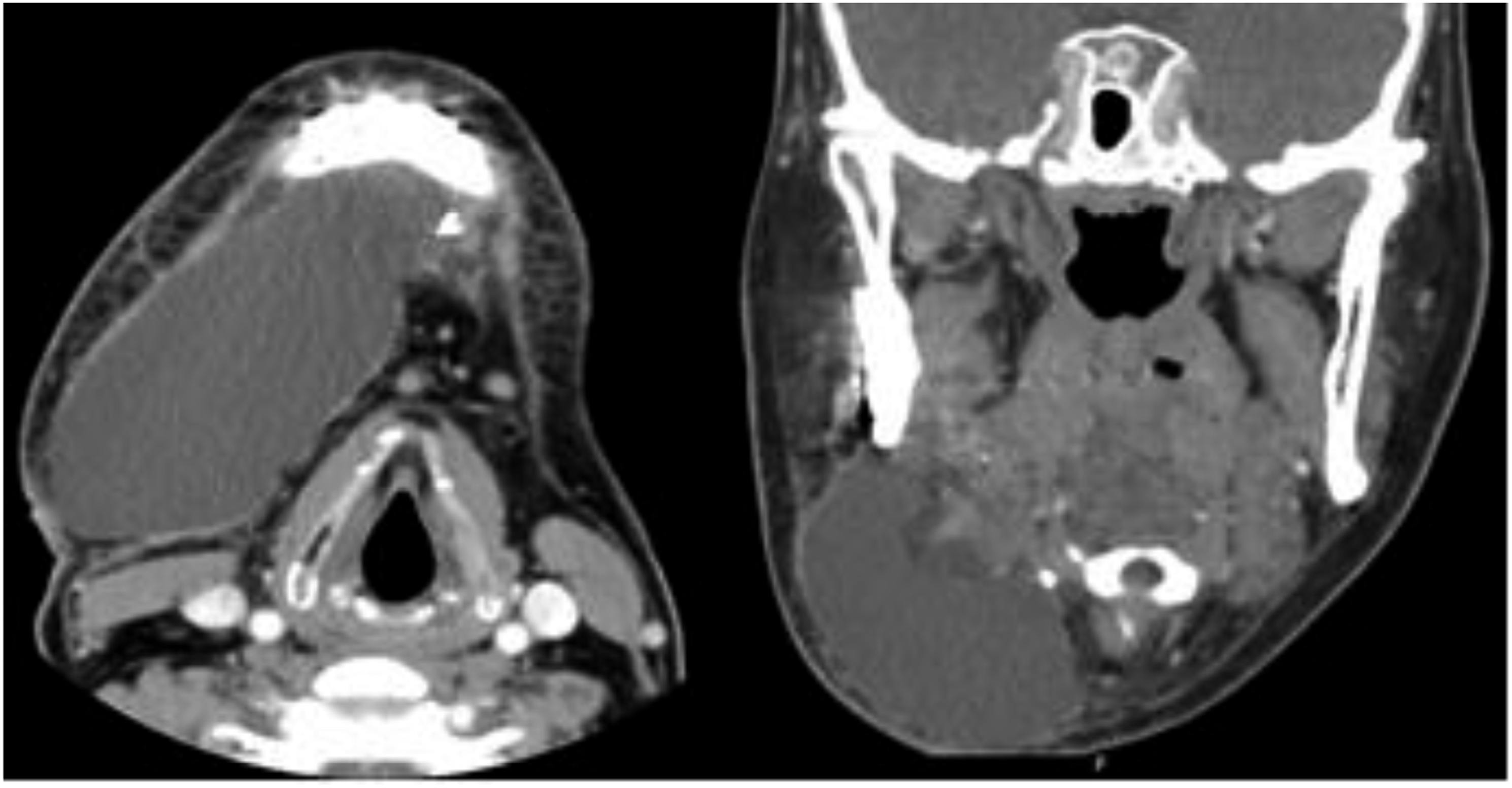
The decision was made to take the patient to the operating room for surgical exploration. The surgical incision was reopened, and a large volume of clear serous fluid was expressed. This was sent for fluid analysis which revealed an Amylase level of 620 U/L. The right submandibular gland was extensively scarred to the surrounding tissues and was dusky in appearance. The decision was made to perform excision of the right submandibular gland. The patient presented for follow-up 1 month postoperatively and the right submandibular swelling had improved and his occlusion remained stable (Figure 5). CBCT revealed intact and stable position of hardware and increased density between fracture segments. The patient was subsequently lost to follow-up. Extraoral photos showing improved right lower facial third edema consistent with surgical procedure and right submandibular incision well approximated.
Discussion
Sialoceles may arise idiopathically, from iatrogenic causes, or as a result of trauma. 2 Submandibular sialoceles occur infrequently and are especially uncommon as a result of a complication following open treatment of mandibular fractures. 8 When encountered, several treatment modalities exist, which range from conservative management to surgical excision. Post-traumatic sialoceles have been managed conservatively with regular aspiration, compression dressings with or without a Jackson-Pratt drain, sialagogue administration, or even radiation therapy.3,10
This was a rare case of a submandibular gland sialocele that developed from an iatrogenic cause following open reduction and internal fixation of mandibular fracture. This particular case involved delayed presentation of this patient following traumatic injury of over 2 months and a fibrous union of fracture segments. As a result, extensive debridement and re-osteotomizing the fracture segments was required prior to reduction and fixation. We suspect this is likely related to iatrogenic damage to glandular or ductal structures. Of note, there has been a reported case of a parotid sialocele associated with a mandible fracture, and it was treated successfully with conservative management. 11 We found one other reported case of an iatrogenic, post-operative submandibular gland sialocele, and this was treated with injections of botulinum toxin A. 3 In this case, concern for infection of hardware, presence of a large neck mass, and leakage of serous fluid through the neck made surgical excision the treatment of choice. The treatment of submandibular gland sialoceles with surgical excision has been observed to be effective in 3 cases of sialocele formation, but these were of idiopathic origin. 9
The purpose of this article is to inform clinicians and raise awareness about an unusual post- operative condition of a sialocele of the submandibular gland following treatment of sequelae of a mandible fracture. Given the paucity of publications and treatment strategies for submandibular gland sialoceles in the literature, we hope to build a framework to guide clinicians who encounter these rare adverse events. Surgeons will have a better understanding of the risks involved when they encounter cases such as this one, where extensive surgical debridement was necessary due to skewed consolidation and extensive pseudoarthrosis after the absence of immediate treatment following the initial trauma. While submandibular gland sialoceles are relatively rare entities, mandible fractures are not. As the result of this paper, operators will be better suited on how to inform patients of and how to manage the possible sequela that may occur following the treatment of mandible fractures.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
