Abstract
Introduction
Sialolithiaisis is a common disease of the major salivary gland predominantly among the submandibular (80-90%), followed by the parotid (5-20%), Sublingual (1-2%) and it rarely affects the minor glands.1,2
The submandibular gland has a very long duct that winds around the mylohyoid muscle against gravity prior to its opening in the floor of the mouth, probably the reason it’s mostly affected. The size of the calculi vary to those that are <1 milimeter (mm) and 7% that are >15 mm are classified as giant sialoliths. 3 Sialoliths either cause mechanical obstruction of the gland or the excretory portion of the duct by mineral deposition decreasing the flow of saliva.
The anterior or the posterior position of the submandibular stones is determined by its relation to the mandibular first molar. The anterior ones are sometimes visible with occlusal radiography and may perforate intra-orally.4,5 The duct is dilated for the ones that do not perforate to aid their removal. The posterior ones however, are close to the hilum or parenchyma of the gland and not palpable. Therefore, the entire gland will have to be excised in order to remove the stone.4-6 Submandibular sialoithiasis perforating the Oral cavity (floor of the mouth has been documented especially upon reaching a certain sizes > 3 cm × 2 cm.
The presence of calculi can manifest with pain and swelling around meal times involving the affected gland, or may be discovered incidentally on routine radiography and sometimes are completely asymptomatic. They may also be accompanied with bacterial suppurative infectious process and exude pus.2,7 Other modes of management that have been previously used include shock wave lithotripsy, sialoendoscopy, endoscopically video-assisted transoral retrieval of stones and intraductal laser fragmentation. 8
The aim of this case report is a patient presenting with large sialolith having perforated the posterior floor of the mouth.
Case Report
A 38 year old male patient was referred by the Dental surgeon as a result of a hard swelling protruding from the soft tissues of the oral cavity for over 2 years. It had been growing gradually was asymptomatic, sometimes tiny pieces of stones like substances would appear in his mouth There was no reported discomfort during meal times over the submandibular region. He was concerned about hard swelling over the neck region as it progressively increased in size. He had been prescribed an antibiotic course 2 months prior to his visit by his Dental Surgeon and an Orthopantomogram (OPG) and Computed Tomography (CT) scan had been recommended. The medical history was unremarkable.
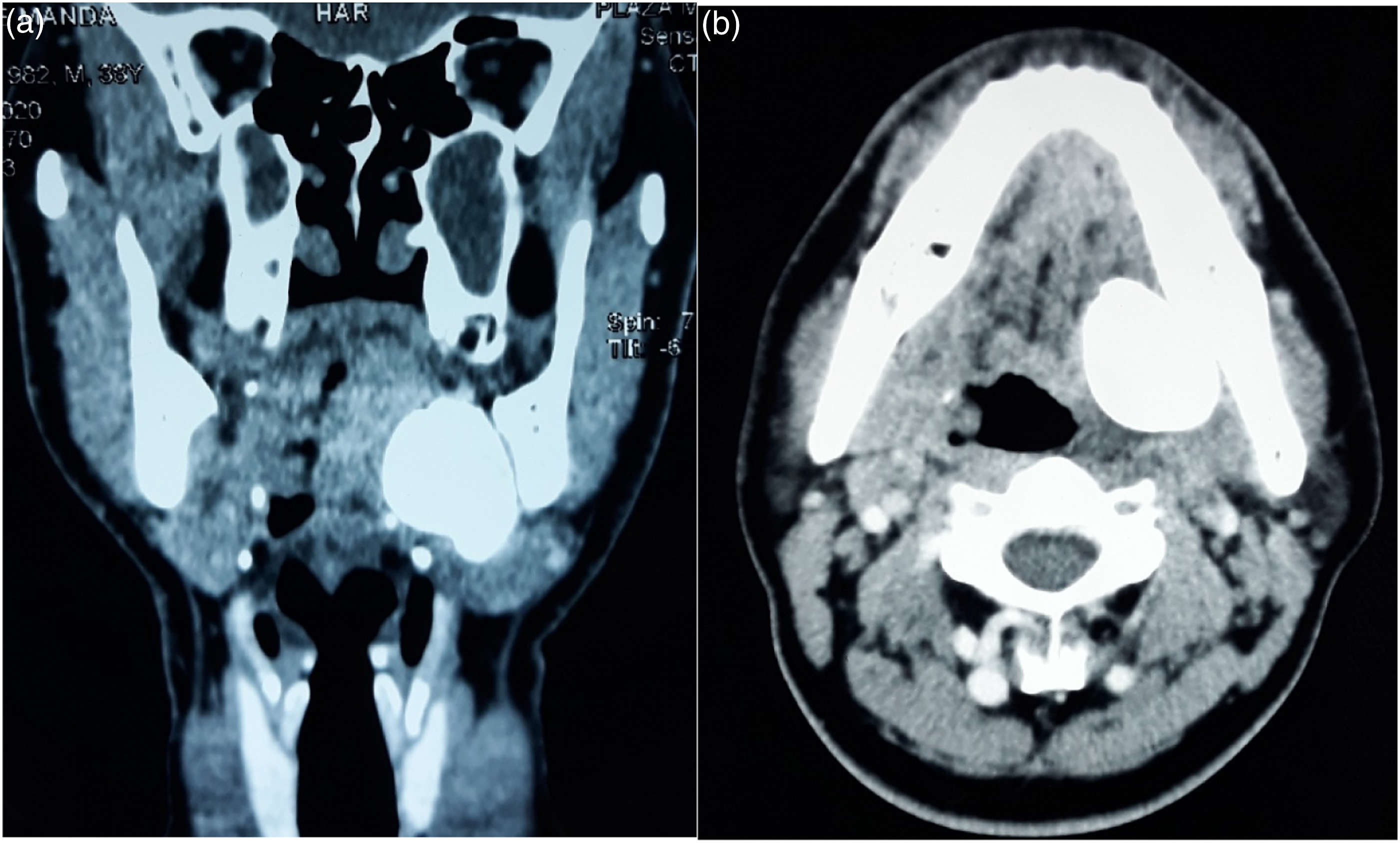
On Extra-oral examination, there was a non-tender hard mass felt at left submandibular region, there were no palpable lymph nodes. On intra-oral examination there was a creamish coloured protrusion seen from the floor of the mouth in the retromolar region lingual to the lower molar (36). It was stone like in consistency and moved on bimanual palpation, the surrounding mucosal margins were mildly eyrthematous. An impression of a sialolith was made. The OPG showed a “mushroom” shaped radio opacity behind the left angle of the mandible with the large dome appearing at the floor of the mouth with a stalk-like end towards the neck region. (Figure 1). The CT imaging a revealed a 39 × 38 × 26 millimeter (mm) calcification involving the submandibular and sublingual space (Figure 2A and B). The left Wharton’s duct was not dilated and left submandibular gland was normal. It was reported as a left sialolith. Orthopantomogram showing “Mushroom” shaped radiolucency behind the left angle of the mandible. (A) CT scan coronal cut showing dense radiodensity medial to ramus of the mandible. (B) Axial cut show sialolith floor of the oral cavity.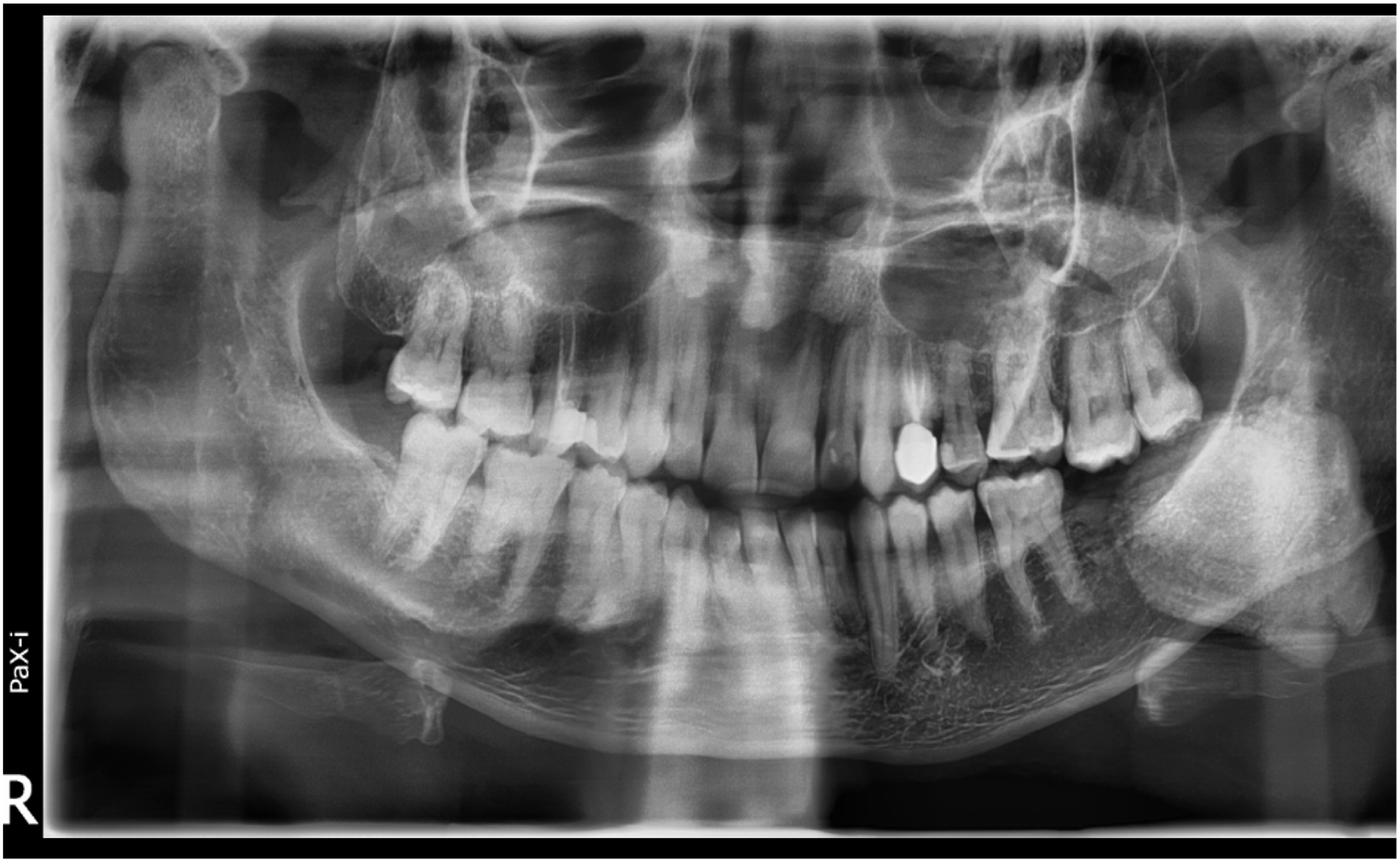
The patient was advised removal of the stone under General anesthesia but due to the Covid pandemic he postponed the procedure. This was done 2-years later under nasotracheal intubation. Local anesthesia was infiltrated around the mucosal margins of sialolith, and via a mucosal incision the entire stone was removed as continuous digital pressure was applied extra-orally beneath the sialolith to aid in stability and help in its elevtion (Figure 3). The incision was left unsutured and allowed to heal by secondary intention after copious irrigation with normal saline. The specimen measured 45 mm × 40 mm × 25 mm and histopathology confirmed it to be a Sialolith composed of eosinophilic granular material with excessive calcification. The patient is being followed up 6 months post operatively and doing well. (A) Intraoperative photo showing transoral approach used for removal of the sialolith. (B) Sialolith measuring 45 mm × 40 mm × 25 mm.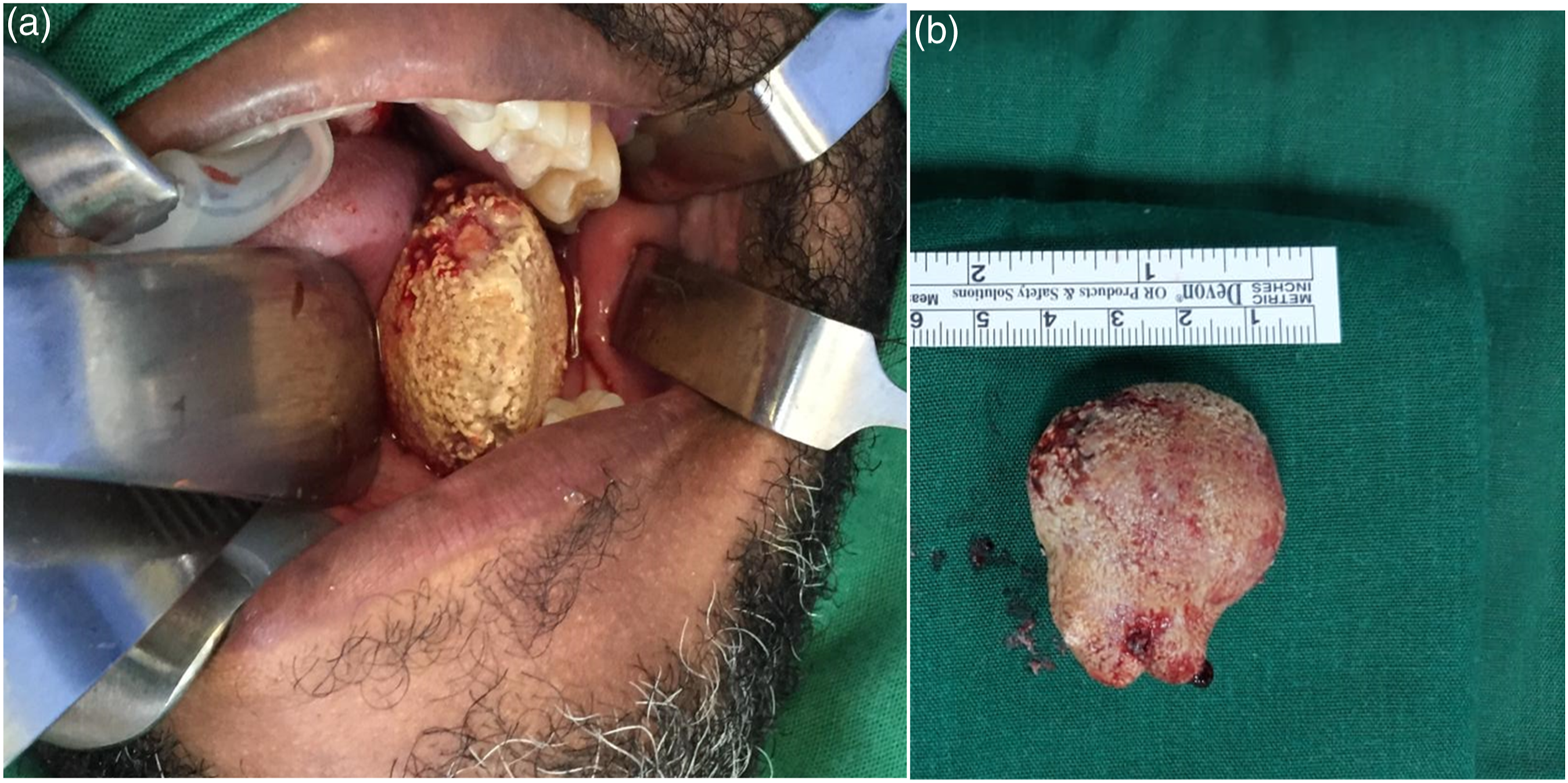
Discussion
Sialoliths are composed of calcium phosphate and hydroxyapatite in addition to magnesium, potassium, and hydroxyapatite. They often lead to sialolithiasis a disease affecting approximating 60 million people annually.
9
The submandibular salivary glands are the commonly involved glands with an 80% prevalence with specific regard to giant sialoliths.11-14 Apart from the duct having a tortuous morphology, the most narrowed part of the duct is referred to as comma shaped area located near the duct outfall and as a result mineral deposition begins creating a nidus for sialolith formation.14,15 The tortuousity of the duct in addition to it’s course being initially inferior to the lingual nerve than crosses it medially makes it identifiable hence, sparing the nerve during surgery.
Acute or chronic sialadenitis may develop as a complication of sialolithiasis. The imaging used to detect sialoliths is ultrasonography, CT scanning, magnetic resonance sialography or sialalography and 80% of submandibular salivary stones are radiopaque.6,16 A mandibular lateral oblique radiograph can also be used for posteriorly place stones to visualize them. 17 In this case the OPG showed the posteriorly placed stone in relation to the last lower molar. Both the Axial and Coronal images of the CT scan its precise location occupying the submandibular and sublingual spaces highlighting submandibular gland was normal in size. This finding coupled with the asymptomatic clinical findings were pertinent to spare the gland from excision during surgery.
Although, sectional sialography is a gold standard technique its disadvantage is the utilization of contrast and its contraindicated for those who have an infection and with an existing allergy. 18 Giant Sialoliths usually measuring >15 mm in one dimension the common ones usually measure between 1 to <10 mm (mean size 6-9 mm). 19 Giant sialoliths measuring more than 35 mm are rare, with only around 17 cases published in the literature with an exception that was reported by Babu and Jain in 2011 of a stone measuring 62 × 20 mm; weighed around 40 gm and the present patient appears to be second largest reported.16,20,21 The treatment modalities have included.
Conclusion
A careful clinical examination and radiological imaging will suffice for its diagnosis. It is not necessary that all patients with sialolithiasis will present with recurrent pain and swelling of the affected salivary gland in response to salivary stimuli. A transoral approach can be used to remove a Giant Sialolith with sparing of the gland as long as it is asymptomatic.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
IRB Statement
I have a written consent form the patient allowing the publication of this case report and it has been uploaded a separate file.
