Abstract
Objective:
To understand the dynamics of vaccination conversations between obstetrician/gynecologists and pregnant women and the factors influencing vaccine acceptance and differences by patient race and ethnicity.
Methods:
In this qualitative study we used linguistic analysis to analyze vaccination conversations between 40 unique patients and 10 unique providers from the 2020 to 2021 influenza season. The results were stratified for non-Hispanic White (“White”) patients compared to non-Hispanic Black and Hispanic patients (“patients of color/POC”) to assess differences in the strength of provider vaccine recommendations, initiation of vaccination conversation, the patient reaction to vaccination prompts, and association of these factors with vaccination intent as the primary outcome.
Results:
The linguistic analysis demonstrated that 22 (55%) out of 40 patients intended to get vaccinated. More POC delayed or refused influenza vaccination (3/6) than White patients (2/10), while more White patients (5/5) than POC demonstrated intent to get the Tdap vaccine (6/10). While providers consistently explained the value of vaccination, greater emphasis was placed on communicating the benefits of Tdap compared with influenza vaccination to POC. Providers used fewer techniques indicative of strong vaccine recommendations when recommending influenza vaccination to POC compared with White patients.
Conclusion:
This hypothesis-generating study suggests some aspects of provider communication about prenatal vaccination may differ by patients’ race and ethnicity. Provider-based interventions to improve communication with pregnant women about prenatal vaccines may improve vaccine uptake and reduce racial and ethnic disparities.
Introduction
The Centers for Disease Control and Prevention’s (CDC) Advisory Committee on Immunization Practices and the American College of Obstetricians and Gynecologists recommend all people who are or who will be pregnant during the influenza season receive one dose of influenza vaccine during every pregnancy.1,2 Additionally, it is recommended that pregnant people receive one dose of tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap) vaccine in the earlier part of the 27th–36th gestational weeks of each pregnancy.3–5 In the 2022–2023 influenza season, 47.2% of all pregnant women in an Internet panel survey reported receiving the influenza vaccine before or during pregnancy, 55.4% received the Tdap vaccine during pregnancy, and 25.6% of women received both the influenza and Tdap vaccines. While coverage estimates were low overall for both vaccines, they were lowest among non-Hispanic Black pregnant women. 6 Vaccination coverage estimates among pregnant women for influenza were 46.1% for non-Hispanic White (“White”) women compared with 39.5% for non-Hispanic Black (“Black”) women and 52.7% for Hispanic women; Tdap vaccination coverage was 62.2% for White compared with 31.4% for Black and 50.8% for Hispanic women.
Understanding the dynamics of provider and patient vaccination conversations is instrumental in enhancing the effectiveness of provider vaccine recommendations and improving vaccine uptake among pregnant women. 7 However, there is limited evidence about the framing and content of vaccine recommendations given by prenatal care providers to pregnant women, or about any differences when providers communicate with pregnant women across different race and ethnicity groups.
This exploratory study analyzed conversations that took place between September 2020 and April 2021. This study aimed to understand vaccination conversations between health care providers and patients by focusing on how conversations were initiated, the factors influencing physician recommendations, pregnant women’s reaction to these vaccination discussions, and the ultimate outcomes of these conversations by exploring the actions pregnant women took, such as intending to get vaccinated, delaying vaccination, or refusing it. The critical importance of these aspects of maternal vaccination has become more pronounced in the past few years, driven by both the COVID-19 pandemic and the broader, evolving immunization landscape.
Methods
We analyzed conversations between 10 health care providers and 40 pregnant women aged 18 years and older that took place between September 2020 and April 2021 (see Table 1). This activity was reviewed by the CDC, deemed not research, and was conducted consistent with applicable federal law and CDC policy. Conversations were prospectively recorded by providers and submitted to a market research database, “Verilogue”; all women and providers had agreed to participate in this market research, and all identifiable information was redacted from the audio and transcripts prior to review for this study. Provider race and ethnicity were not linked with included conversations. Recordings from English-speaking pregnant women who were able to give consent on their own at the time or had a caregiver/legal guardian present providing consent were selected for sample inclusion.
Demographic Information of Health care Providers and Pregnant Women (September 2020–April 2021, Verilogue Database)
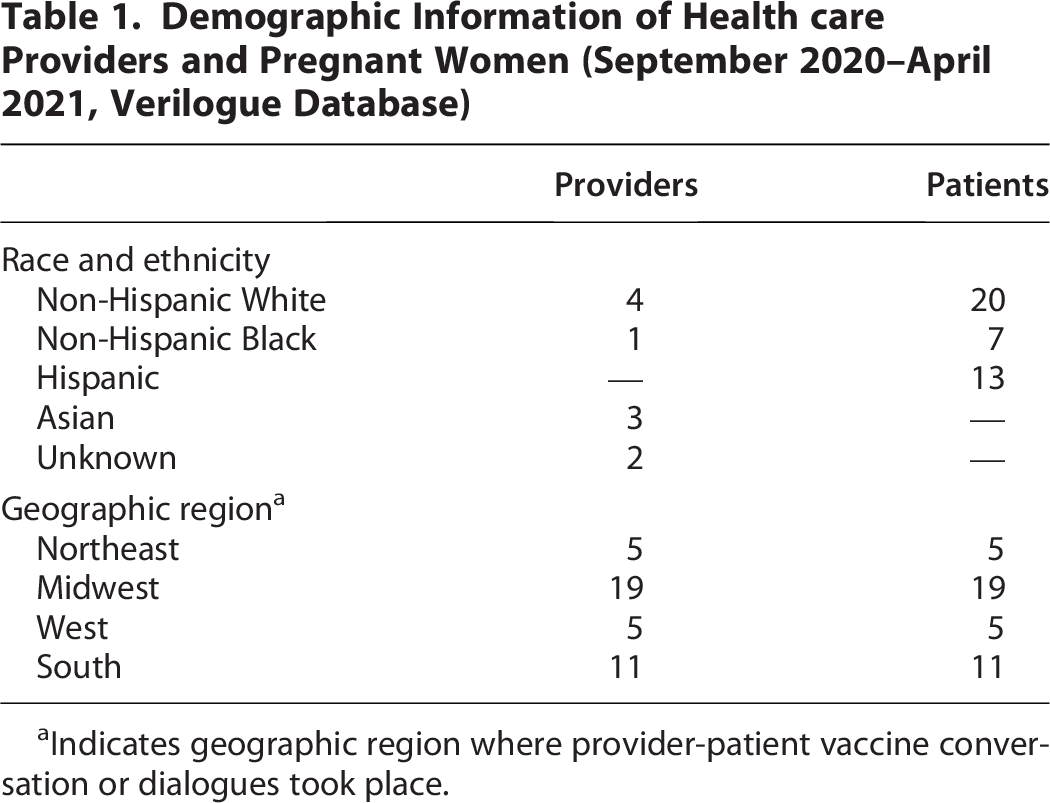
Indicates geographic region where provider-patient vaccine conversation or dialogues took place.
A total of 389 prenatal conversations were collected during the study period. Keyword searches were performed to identify conversations containing discussion of either influenza or Tdap vaccines, which resulted in a candidate pool of 89 conversations. From these, 75 were selected by prioritizing the ones with the most discussion pertaining to the vaccination recommendation/decision and with the clearest vaccination decision outcomes. To limit individual physician bias and maximize the number of unique providers included, analysts listened to recordings and selected conversations so that no provider contributed more than 5 conversations to the study sample. Conversations were purposively selected based on quality criteria, which included a vaccine offer, patient response, uptake rates, and refusal reasons. Higher-quality conversations were preferentially retained. Additionally, conversations were selected for variation in visit timing (first prenatal visit, first trimester, third trimester through 36 weeks), and patient race and ethnicity. The purpose of choosing different time points during the pregnancy was to maximize the possibility of capturing conversations on influenza and Tdap vaccines. Geographic region was not used as a selection factor due to the small pool of eligible conversations, although selected conversations include providers from across the United States. For providers who had submitted five or fewer conversations, all were included regardless of quality.
This selection resulted in an analytic sample of 40 conversations from 40 patient encounters. The patient sample included 7 participants who identified as Black and 13 who identified as Hispanic, who were classified as persons of color (POC, N = 20) and compared with 20 White patients (Table 1). Information on race and ethnicity of patients was provided by the physicians.
The objective of this study was to examine conversations based on four key research areas with findings stratified by race and ethnicity. The first research area explored the nature of vaccination-related conversations between providers and patients to determine the tone and direction of the conversation and how conversations were initiated. The second research area was about the factors associated with strong physician vaccination recommendations; utilizing strength strategies that include urgency, value or benefit of vaccination, and presumptive language associated with physician vaccination recommendations. Presumptive language is a communication frame that functions to convey personal endorsement rather than to issue an imperative or directive. The third research area assessed how pregnant women respond to vaccination conversations. The fourth research area explored the outcome or actions taken by pregnant women (vaccine intent) based on physician conversations or recommendations (intent, delay, and refusal).
The linguistic analysis utilized conversation analysis techniques to examine the unstructured dialogic data in the recorded conversations. Conversations were coded with both inductive and deductive coding systems by analysts whose research backgrounds are in linguistics, conversation analysis, or discourse analysis with deep expertise and experience of working with unstructured dialogic data. The conversations were reviewed and coded by analysts, and quantifiable results were reported. During the coding process formal coding memos were not developed; however, individual notes may have been drafted. This approach focused on understanding and analyzing conversational tone and functional, emotional, and conversational behaviors that may influence patient and provider attitudes and decision-making. The aim was to identify relational and transactional communication dynamics and ways in which rhetorical styles and the use of narratives affect the efficacy of communication and structure conversational outcomes and may result in communication gaps. The unit of analysis was patient encounters (n = 40).
Through this study we explored the nuanced meanings patients attached to their choices; whether they expressed an intention to get vaccinated after having a vaccination conversation with the provider or had already planned to get vaccinated prior to having the vaccination conversation is identified as “intend to get vaccine,” a non-committal response is identified as a decision to “delay,” patient refusal to take the vaccine after seeing the provider is identified as “refusal,” and those vaccinated prior to provider recommendation is identified as “vaccinated before provider recommendation.” Through the linguistic analysis applied to this textual data, we sought to generate grounded hypotheses by delving into the context surrounding their choices. We did not conduct statistical analysis, as the goal was to describe and interpret approaches, attitudes, and decision-making phenomena and not to measure or generalize outcomes.
Results
Results are presented by vaccination conversation initiation, patient’s reaction to vaccination prompts, strength of vaccine recommendation based on utilization of strength strategies, and the outcome (intend to get vaccine, delay, and refusal).
Vaccine conversation initiation
Vaccination conversations were mostly initiated by health care providers as a recommendation to get the vaccine by asking a confirmatory question (e.g., did you get?, have you had?), informing the patient that the vaccine is something to get in the future but not in the form of a recommendation or sharing information on the vaccine verbally or with physical documents. The most common method for initiating vaccine conversation was a confirmatory question, particularly for the flu vaccine. This approach was likely favored because the appropriate time for a flu vaccine is calendar-based, making it relevant to all eligible patients regardless of their specific pregnancy stage. In contrast, for the Tdap vaccine, conversations were less frequently initiated with a simple confirmatory question. Instead, providers were somewhat more likely to inform patients that the Tdap vaccine was something to be received later in the pregnancy. This is because the Tdap vaccine is recommended during a specific gestational period, making it less immediately relevant to patients who had not reached that stage. There were no patterns that emerged in the use of confirmatory questions by patient race.
For patients who initiated vaccine conversations, they mainly did so to ask for information about the Tdap vaccination or about the safety of getting the influenza vaccine while pregnant or to express a desire or intention to receive the vaccination.
Strength of recommendation
Overall, the strength of the recommendation strategies utilized varied by vaccine, but health care providers in our sample consistently explained the value or benefits of vaccination.
The linguistic analysis categorized strength strategies utilized by providers as urgency, value, and presumptive language/personal endorsement. All Tdap conversations contained at least one strength strategy, and 96% contained two or more. All Tdap recommendations touched on urgency, 88% included a reference to value, and providers used presumptive language in 58% of recommendations. POC were presented with more strength strategies when discussing the Tdap vaccine than White patients.
In influenza vaccine conversations, 36% included no strength strategies, while 43% contained two or more. Additionally, 50% of influenza vaccine recommendations include no urgency markers, 86% did not mention the value of vaccination, and in 57% of the conversations, providers did not use presumptive language when making a recommendation. In influenza vaccine conversations where strength strategies were used, POC were presented with fewer strategies overall than White patients. For both influenza and Tdap, using more strength strategies appeared to be associated with higher vaccine intent; however, we were unable to evaluate this relationship statistically given the small sample size.
Provider: Okay. The, the only reason we would, um, encourage it is that if a pregnant woman gets influenza it can be harmful for both you and the baby.
Patient: Okay.
Provider: And we’re worried about with COVID, you know, the impact of two things at once so -
Patient: Yeah. So, my sinuses have kind of been like [INAUDIBLE]. I was thinking maybe it was the weather.
-Provider to POC ID 193283
Provider: “Flu shot, yes, no? Did you get one? Do you believe in flu shots? Okay.
Patient: Nope.
Provider: TDAP. You’ve got to do the TDAP for the baby.
Patient: I, yeah, I’ m going to do the TDAP.
-Provider to POC patient ID194934 regarding Tdap vaccine
Patient reaction
Patient reactions to the influenza and/or Tdap vaccination conversation were generally positive.
In the linguistic analysis, patients had a few questions regarding the vaccine being discussed. Patient questions were geared toward seeking guidance and/or educational information from the provider regarding the timing of the vaccines and the coadministration of Tdap and influenza vaccines. Questions related to influenza vaccination centered on the patient’s interest in receiving the vaccine, such as eligibility, optimal timing, and if co-administration with the Tdap vaccine was possible. On the other hand, Tdap vaccine questions were typically more informational, with patients seeking clarification on its purpose (whether it was for them or their baby), its duration of efficacy, the meaning of “Tdap,” and, similar to the flu vaccine query, whether it could be administered concurrently with the flu shot. There were no specific patterns that emerged in the type of questions patients asked based on patient race.
The linguistic analysis showed that providers bundled influenza and Tdap vaccination recommendations for five patients, and all patients (3 White, 2 POC) accepted both vaccine recommendations (Table 2). Providers bundled the flu and Tdap vaccines, presenting them to patients as a “package deal” to emphasize their importance and encourage vaccination. Providers frequently discussed the flu and Tdap vaccines sequentially in the conversation, bringing up one after another. Some providers explicitly recommended both vaccines in the same conversation.
Linguistic Analysis: Vaccine Acceptance, Delay, and Rejection of Recommended Vaccine by Patient Race and Ethnicity
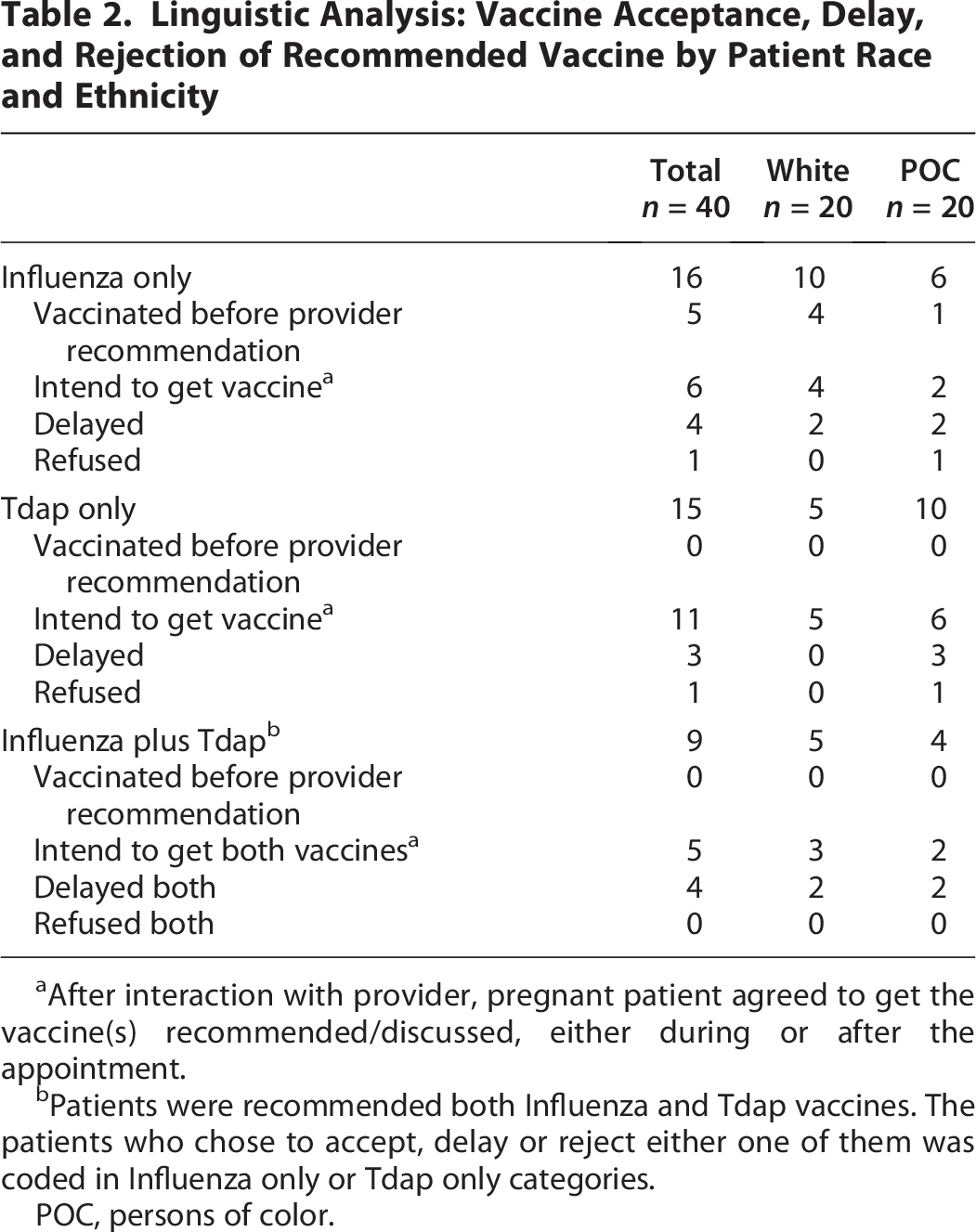
After interaction with provider, pregnant patient agreed to get the vaccine(s) recommended/discussed, either during or after the appointment.
Patients were recommended both Influenza and Tdap vaccines. The patients who chose to accept, delay or reject either one of them was coded in Influenza only or Tdap only categories.
POC, persons of color.
Provider: You can get it at your own pharmacy. But that’s one-
Patient: Okay.
Provider: Important that you need to do is the flu shot.
Patient: Okay.
Provider: And after 28 weeks you’ll come get the Tdap.
-Provider to White patient 197900
Provider: You should be feeling baby moving every day. We’re going to remind you on, in terms of vaccines, two vaccines, actually three now. So, one is the flu vaccine.
Patient: Uh-huh.
Provider: Second, Tdap is what you should get between 27 and 36 weeks. So, that’s something you should get. Can be done at the pharmacy or your, or your primary care.
Patient: Okay.
Provider: That’s to protect your newborn from whooping cough.
-Provider to White patient 201185
Vaccine intent
The outcome of the vaccination conversation was measured by patient intent to get vaccinated. In the linguistic analysis 55% (22 [12 POC, 10 White]) patients in the sample showed intent to get vaccinated for influenza, Tdap or both (Supplementary Table). More White patients (5/5) than POC intended to get vaccinated for Tdap (6/10). Two patients firmly refused influenza and Tdap vaccination (2/20).
Provider: Is that something that you think you will get?
Patient: No.
Provider: So you’re going to decline Tdap vaccine?
Patient: Yes.
-Provider to POC patient ID 198923
Provider: Flu shot, yes, no? Did you get one? Do you believe in flu shots? Okay.
Patient: Nope.
-Provider to POC patient ID194934
Discussion
These findings provide insight into provider communication about prenatal vaccination and how it can differ between vaccines and by patients’ race and ethnicity. In this study vaccine conversations were usually provider-initiated regardless of patient race and ethnicity, and the majority of patients accepted vaccinations. Providers often explained vaccine benefits to patients and placed more emphasis overall on the benefits of Tdap compared with influenza vaccination for POC. The effect of bundling recommendations on vaccine acceptance was not clear. Notably, additional time and effort providers spent on POC to discuss Tdap might have contributed to greater acceptance of Tdap among POC than White patients.
There are several limitations to this study. Purposive sampling was used to maximize the content and quality of vaccine-related dialogue, so conversations analyzed may not be representative of all provider-patient vaccine discussions. The market research database used for this study only included patients who agreed to have their appointments recorded, which may also contribute to selection bias. The sample size of the study was small, which is why Black and Hispanic women were combined into one category and did not include patients from other racial/ethnic groups. Due to this constraint, differences in provider conversations with Black versus Hispanic patients could not be assessed. Furthermore, the provider’s race and ethnicity were not associated with the selected conversations, and thus the effect of racial concordance could not be examined; literature is mixed on how provider-patient concordance affects communication. 8 Additionally, interactions between pregnant women and other health care personnel such as nurses that occur independent of provider and patient vaccine conversations during a prenatal visit were not captured, so we may not have examined all the discussion influencing patients’ vaccination decisions. The vaccination conversations analyzed represent a single visit during pregnancy and do not account for other provider-patient vaccination conversations that may have taken place during the pregnancy. Finally, the outcome of interest in this study is vaccine intent and not uptake due to the inability to confirm vaccine administration via medical record review.
Conclusion
The study findings have shed light on interesting differences in provider rhetoric around vaccines between White and POC patients. The two differences by race and ethnicity were that providers placed more emphasis on the benefits of Tdap compared with influenza vaccination, particularly to POC, but used fewer strength strategies when recommending influenza vaccination to POC compared with White patients. The context of maternal vaccination is unique because of a heightened focus on fetal safety, increased vulnerability to misinformation about vaccines during a sensitive time, and a limited window of opportunity to influence not only the mother but also the health of the newborn and future childhood vaccinations. An important step to increase prenatal vaccination uptake could be to give providers feedback on the strategies they use effectively to increase vaccination intent and areas of improvement, including consistent use of strength strategies for vaccine recommendations for pregnant women across all races and ethnicities. 9 Training and use of scripts or talking points may help with consistent messaging of benefits and strong recommendations across patients. Furthermore, bundling recommendations for Tdap and influenza vaccination to increase vaccine acceptance appears to be a promising practice but needs further exploration. Identifying facilitators and barriers in initiating and guiding vaccine conversations with pregnant women from various racial and ethnic groups could help increase vaccine acceptance and uptake.10,11 It is critical to develop and implement interventions, update guidelines, and establish best practices in communication for providers to ensure consistent, clear, and strong vaccination recommendations are given in clinical practice to all eligible patients regardless of race and ethnicity.12,13 Furthermore, bidirectional community-led strategies where trusted messengers partner with health care providers have also been found to reduce disparities in COVID-19 vaccination rates. 14 These strategic efforts can help reduce racial disparities and improve uptake of maternal vaccination.
Footnotes
Author Disclosure Statement
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention/the Agency for Toxic Substances and Disease Registry.
Funding Information
This research was funded by CDC contract number 75D30120P08787.
Supplemental Material
Abbreviations Used
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
