Abstract
Corynebacterium striatum is considered to be notoriously associated with multidrug resistant nosocomial infections with high mortality. This article encases an unusual case of C. striatum associated postoperative surgical site infection in post-operative case of oral submucous fibrosis. The prognosis depends majorly on meticulous debridement and regular dressing with concomitant anti-microbials. Patient factors such as immunodeficiency and debilitating comorbidities contribute equally to final outcome.
Introduction
Among the omnipresent Corynebacterium species Corynebacterium diphtheria is medically relevant and is causative pathogen for diphtheria. Whereas C. striatum, C. amycolatum, C. minutissimum, C. xerosis, and C. freneyi are grouped as nondiphtherial, Corynebacteria were considered concomitant part of mucosal and epidermal microbial flora.
Corynebacterium striatum is recognized as a true pathogen when isolated in several samples from sterile body sites or from indwelling medical devices. 1 So, it truly follows the quote “The most dangerous germs in the hospital may be those you bring with you.”
In this study, we report a case of C. striatum associated postoperative wound infection in patient surgically managed for oral submucous fibrosis.
Case Report
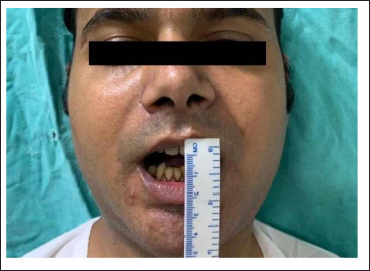
A 27-year-old male patient reported to oral and maxillofacial surgery unit with the chief complaint of reduced mouth opening for the past one year. Clinical examination and history revealed progressive decrease in mouth opening—history of tobacco chewing for last 3 years. Intraoral examination revealed blanched bands on upper and lower labial mucosa and thick fibrous bands were present on left and right buccal mucosa. Preoperative mouth opening was 3 mm (Figure 1). Hence, the patient was planned for bilateral fibrotomy along with reconstruction with platysma myocutaneous flap under general anesthesia. Preoperative examinations and investigations were within normal limits. As per the surgical plan, patient underwent resection of fibrotic bands along with extraction of third molars and reconstruction with platysma myocutaneous flap under general anesthesia (Figure 2). After the surgery, patient was shifted to postoperative ward and then to general ward as his general condition was stable. The flap was healthy and showed good signs of vascularity. After 3 days of surgery he developed blisters on commissure of lips and had intermittent fever. He was advised general medicine and oral medicine reference and was advised antiviral drugs as clinical signs and symptoms were in adjunct with Herpes simplex infection. After 7 days of treatment there was no improvement and clusters of blisters appeared on neck, palate, and chest along with high grade fever. Close clinical observation of wound showed serous discharge from suture site (Figure 3). The serous discharge was sent for antibiotic culture and sensitivity testing. Confirmation of Corynebacterium striatum was done after staining the sample with gram stain which revealed gram-positive bacilli. According to the antibiotic sensitivity report, administration of intravenous dose of meropenem (1 gm 8 hourly) and clindamycin (600 mg 12 hourly) were given for a week. Routine blood count was carried out every third day to monitor the total leucocyte count. Patient was followed every week and regular dressing of the surgical site was done (Figure 4).
Pre-operative Clinical Photo Showing Reduced Mouth Opening.
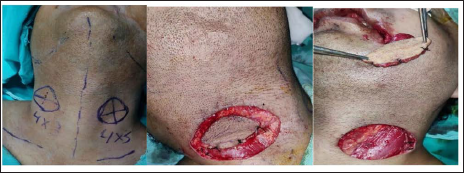
Intraoperative Marking and Flap Harvest.
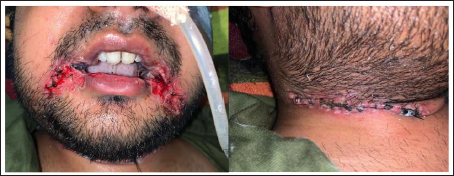
Fulminating Infection Even after 7 Days of Antibiotics and Antiviral Drugs.
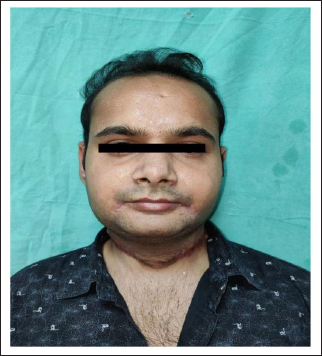
One Month Follow up.
Discussion
C. striatum is a commensal micro-organism found on skin and oral mucous membranes but targets the debilitated patients with immunosuppression or indwelling medical implants. 2 Interestingly, case discussed in this article had no underlying history of any comorbidity.
Wound infection is the most common infective process after surgery (38%) and often requires antibiotic therapy and may increase the length of hospital stay thereby increasing medical cost. 3 Postoperative wound infections cause considerable recipient and donor site morbidity.
The overzealous use of antibiotics disrupts symbiosis between the microbes and host and causes overgrowth of commensals like C. striatum, which then colonizes the host resulting in active infection. C. striatum is recently being reported as a multidrug-resistant pathogen causing long standing open wound infection. Although initial management of suspected cases should include vancomycin, because in vitro resistance to vancomycin has not been reported in any of the Corynebacterium species, 4 the infection in this patient was only sensitive to meropenem and clindamycin. This can be attributed to acquired vancomycin resistance by C striatum. Case of Corynebacterium striatum in post-operative wound infection of patient with squamous cell carcinoma is reported in the literature. 5 But to the best of our knowledge, this is the first case of Corynebacterium striatum in post-operative wound infection of oral submucous fibrosis patient without having history of any comorbidity. Prompt diagnosis of pathogen and administration of antibiotics according to sensitivity hold key to better prognostic outcome in spite of which this case still showed signs of flap necrosis and fibrosis leading to partial relapse.
Conclusion
Emergence of this nosocomial pathogen C. striatum is associated with bacteremia, endocarditis, valvular damage, meningitis, vaginitis, and infections of the urinary tract, the respiratory tract, wounds, skin, and eye. Immunodeficiency or comorbidities are predisposing factors for this opportunistic infection. Surprisingly this case with absence of any such comorbidities developed fulminating C. striatum infection, but fortunately, pin-point identification of causative pathogen and prompt management were key factors in containment of the disease process.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent and Ethical Approval
Written Informed consent obtained.
