Abstract
Background:
Previous evidence suggests that a short myotomy does not reduce the efficacy of peroral endoscopic myotomy (POEM) or increase intraoperative complications. However, the available studies are still limited and there has been no research in Latin America.
Objectives:
This study aims to evaluate whether POEM with a short myotomy differs significantly from a long myotomy in terms of efficacy and safety in patients with achalasia.
Design/Methods:
A retrospective cohort study including patients who underwent POEM for achalasia between 2017 and 2024. Efficacy was assessed according to the Eckardt scale at 6 months and at 1 year of follow-up. Safety was assessed for perioperative adverse events according to the iPOEM classification.
Results:
A total of 57 patients were included, 44% underwent short myotomy (median esophageal length of 5 cm; interquartile range (IQR) 4–5), and 56% long myotomy (median 11 cm IQR 10–13). 35% had previously undergone surgery for achalasia. The long myotomy group had more frequently minor complications such as emphysema (15.6% vs 0%; p = 0.039), capnoperitoneum (65.6% vs 16.0%, p < 0.001) and required more abdominal punctures (56.2% vs 12.0%, p < 0.001). There was no difference in the incidence of other complications. The probability of symptomatic response, defined as an Eckardt score ⩽ 3 at 12 months, was similar between groups (84.3% vs 88%, p = 0.69). The median operative time for the short myotomy was shorter (median 80 min; IQR 70–95 vs 127.5 min; IQR 102–155 min; p < 0.001).
Conclusion:
Short myotomy is not inferior to long myotomy in terms of clinical success and long-term reflux disease in the management of patients with achalasia. Furthermore, it offers advantages such as shorter procedure times and potentially lower rates of minor complications, making it the preferred option in most cases.
Keywords
Introduction/Background
Achalasia is a rare esophageal disorder. The prevalence has been reported to be between 7 and 27 per 100,000 people,1,2 and the incidence between 1.9 and 26 per 100,000 people per year.2,3 In Colombia, the prevalence is 21.8 cases per 100,000 inhabitants. 4 It is characterized by an alteration in esophageal motility with obstruction of the gastroesophageal junction (GEJ) outlet tract due to altered relaxation of the lower esophageal sphincter (LES), with absent or spastic contractions of the esophageal body in the absence of structural obstruction. 5 The most common symptoms are dysphagia for solids and liquids, regurgitation, chest pain, and weight loss. 6
Esophageal motility dysfunction in achalasia is irreversible, so therapeutic efforts have focused on reducing obstruction of the GEJ with the aim of restoring esophageal emptying, relieving esophageal symptoms and improving quality of life. Peroral endoscopic myotomy (POEM) is an innovative technique that arose from the need to find a less invasive treatment with efficacy rates equal to or better than traditional methods. 5 Several studies have shown POEM to be effective and safe, with immediate symptom improvement in 82%–98%, and reported efficacy of 90% at 2–3 years and 80% at 5 years. One of the largest series reported sustained efficacy of 91% at 7 years.7–11 One of the most common adverse events reported is the development of symptoms of gastroesophageal reflux disease (GERD), which has been reported in between 9% and 43% of patients.11,12 Moderate to severe esophagitis has been reported in 40% of patients with symptoms of GERD, as well as endoscopic esophagitis even in those without symptoms. 13
The traditional length of an esophageal myotomy varies from 6 to 10 cm, with an extension of 2–3 cm for gastric myotomy.14–17 There are several studies suggesting that further extension of the myotomy length does not improve GEJ distensibility. 18 Studies on the ideal length of esophageal myotomy are scarce, and the cut-off points for defining short esophageal myotomy vary between 3 and 6 cm. So far, these studies suggest that a short myotomy is not associated with a lower clinical success as measured by the Eckardt score, nor with differences in the frequency of intraoperative complications or the incidence of gastroesophageal reflux compared with a long myotomy, but it is associated with a shorter procedure time.19–21 However, this evidence is still insufficient and there are no studies in Latin America.
The aim of this study is to evaluate whether POEM with a short myotomy compared to a long myotomy in patients with achalasia is associated with significant differences in the efficacy and safety of the procedure, based on the experience of a referral center in Colombia.
Methods
Design, setting, and population
A retrospective cohort study based on the institutional gastrointestinal neurophysiology registry of the Hospital Universitario San Ignacio in Bogotá, Colombia, was performed. All patients aged 18 years or older, with a diagnosis of achalasia 22 (confirmed by clinical signs, endoscopy, barium esophagram with typical findings of esophageal dilatation and a characteristic “bird’s beak” appearance at the GEJ, 23 and compatible findings on esophageal manometry with high-resolution impedance), and who were referred to POEM between January 2017 and August 2024, were included. Patients lost to follow-up before 6 months were excluded from the analysis. The reporting of this study conforms to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement. 22
The study was approved by the Research and Ethics Committee of the Pontificia Universidad Javeriana and the Hospital Universitario San Ignacio in Bogotá (FM-CIE-0086-25).
Data collection
The data were obtained from an institutional registry where a gastroenterology physician systematically collected relevant information based on information recorded in the medical record system, including procedures performed and outpatient visits. In case of loss to follow-up or missing information, the information was completed by telephone call to the patients. The information collected was kept strictly confidential and securely archived by the research team.
Information collected included sociodemographic data (age, body mass index, weight, height, BMI, and sex), clinical characteristics (type of achalasia, time of symptom onset, and comorbidities), previous interventions (pneumatic balloon dilatation, Heller myotomy, or POEM), clinical symptoms and severity (assessed using the Eckardt score), manometry findings, and esophagram. In addition, procedure characteristics (myotomy length, type and thickness of complete or circular muscle layer myotomy, and procedure time), hospital stay and procedure-related complications (emphysema, capnoperitoneum, capnothorax, bleeding, pleural effusion, abdominal puncture, thoracotomy, and premature muscle perforation), as well as the need for ICU admission, readmission, urgent surgery, transfusion, hospital stay > 5 days, and mortality were evaluated. Finally, safety and efficacy were assessed at 1 year according to reflux symptoms measured by the Eckardt scale.
Definition of variables
The manometric diagnosis of achalasia was made according to the Chicago Classification v4.0, including the three subtypes described based on manometric findings. All three share an elevated mean integrated relaxation pressure (IRP) and an absence of esophageal body contractility. Type I achalasia is characterized by the presence of 100% failed contractions. Type II also has 100% failed contractions plus esophageal pressure in 20% or more of swallows. Type III is characterized by 20% or more of swallows with spastic/premature contractions (defined as distal latency < 4.5 s) and absence of peristalsis. 24
For this study, a short esophageal myotomy was defined as ⩽6 cm and a long one >6 cm. An anterior myotomy was defined as one made with an incision at the 2 o’clock position, or a posterior myotomy (modified technique) where the posterior wall was incised at the 5 to 6 o’clock position. Regarding the length of the myotomy, a “circular layer myotomy” was defined as one that preserved the outer longitudinal muscle layer of the esophagus, as opposed to a full-thickness myotomy. The length, position, and extent of myotomy were at the discretion of the performing gastroenterologist, with decisions based on previous procedures (POEM or previous Heller myotomy), type of achalasia, sigmoid morphology, and expertise of the third-space endoscopist. In addition, there was a greater tendency for endoscopists to perform long myotomies in the first patients in our cohort who underwent POEM.
We used the Eckardt scale to assess symptom severity and treatment effectiveness. This scale uses a scoring system of 0–3 points for each of the four cardinal symptoms (dysphagia for solids and liquids, regurgitation, chest pain, and weight loss). 0 represents the absence of the symptom and 3 represents its greatest severity, with a maximum score of 12. A score ⩽ 3 indicates adequate treatment response. 25 Effectiveness was assessed at 6 months and 1 year after the procedure.
Safety was assessed using the iPOEM classification, which classifies adverse events as clinically insignificant minor events (pneumoperitoneum requiring intraprocedural puncture, inadvertent mucosal perforation of the mucosal flap, and premature perforation of the muscularis layer at the start of the submucosal tunnel), or as a clinically significant major event (need for surgical conversion, ICU admission, prolonged hospital stay > 5 days, readmission, need for invasive intervention such as surgery or interventional radiology, transfusion, disability, or mortality). 26 The updated Lyon criteria were used to define the presence of gastroesophageal reflux after POEM. 27
Statistical analysis
The sample size was calculated assuming that a 30% difference in clinical efficacy was clinically significant, with an alpha error of 0.05 and power of 80%. The estimated sample size was 54 patients in total (27 in each group).
Descriptive statistics were used to summarize population characteristics. Categorical variables are reported as absolute values and percentages. Continuous variables were expressed according to their distribution. The mean and standard deviation were used for variables that met the criteria for normal distribution according to the Shapiro–Wilk test, and the median and interquartile range for variables with non-normal distribution.
Differences between groups (short vs long myotomy) were assessed using the chi-squared test for categorical variables and the t-test or Mann–Whitney U test for continuous variables, depending on the data distribution. A p-value < 0.05 was considered statistically significant. All statistical analyses were performed using STATA® software. 28
Results
Characteristics of patients with short and long myotomy
A total of 57 patients were referred to POEM between 2017 and 2024. The 57 patients were analyzed, all of whom had a 6-month follow-up, but three patients were lost to 1-year follow-up (one patient in the long myotomy group and two patients in the short myotomy group). The characteristics of the patients who underwent long and short myotomy are shown in Table 1. The most common type of achalasia was type II (66.7%) and most patients had normal weight. Twenty patients (35%) had undergone previous procedures, the most common being laparoscopic Heller myotomy.
General characteristics of patients undergoing long versus short myotomy.

They had received two interventions prior to POEM.
ASA, American Society of Anesthesiologists; IQR, interquartile range; IRP, integrated relaxation pressure; LES, lower esophageal sphincter; POEM, peroral endoscopic myotomy; SD, standard deviation; sigmoid esophagus: tortous and S-shaped esophagus.
Of the total population, 25 (44%) patients underwent a short myotomy. There were no differences between the long and short myotomy groups in terms of age, BMI, comorbidities, disease progression, previous interventions, ASA classification (American Society of Anesthesiologists), 29 and type of achalasia. There were also no differences in manometric variables or esophagram findings. The only difference was a higher frequency of heartburn in the long myotomy group, but the Eckardt score was similar between groups (7.7 ± 1.7 vs 7.6 ± 1.9; p = 0.63).
Procedure characteristics
Table 2 shows the characteristics of the procedure and the associated complications. The median length of the esophageal myotomy was 5 cm (IQR 4–5) in the short myotomy group and 11 cm (IQR 10–13) in the long myotomy group. Gastric myotomy length, myotomy thickness, myotomy type, and number of clips used were similar between the two groups.
Procedural characteristics and complications of long versus short myotomy.

IQR, interquartile range.
Regarding complications, emphysema occurred in five patients in the long myotomy group and none in the short myotomy group (15.6% vs 0%; p = 0.039). Similarly, patients who underwent long myotomy had more capnoperitoneum (65.6% vs 16.0%, p < 0.001) and required more abdominal punctures (56.2% vs 12.0%, p < 0.001). There was no difference in the incidence of other complications (Table 2).
Operative time was significantly longer in patients who underwent long myotomy (median 127.5 min, IQR 102–155, vs 80 min, IQR 70–95; p < 0.001). Length of hospital stay was similar between the two groups (Table 2).
Effectiveness
Efficacy was similar between groups at both 6 months (Eckardt score 1.4 ± 0.98 for long myotomy vs 1.08 ± 0.75 for short myotomy; p = 0.945) and 12 months (Eckardt score 2.09 ± 1.92 vs 1.65 ± 1.55; p = 0.816). The probability of symptomatic response, defined as an Eckardt score ⩽ 3 at 12 months, was similar between groups (84.3% vs 88%, p = 0.69; Table 3).
Evaluation of long and short myotomy efficacy at follow-up.
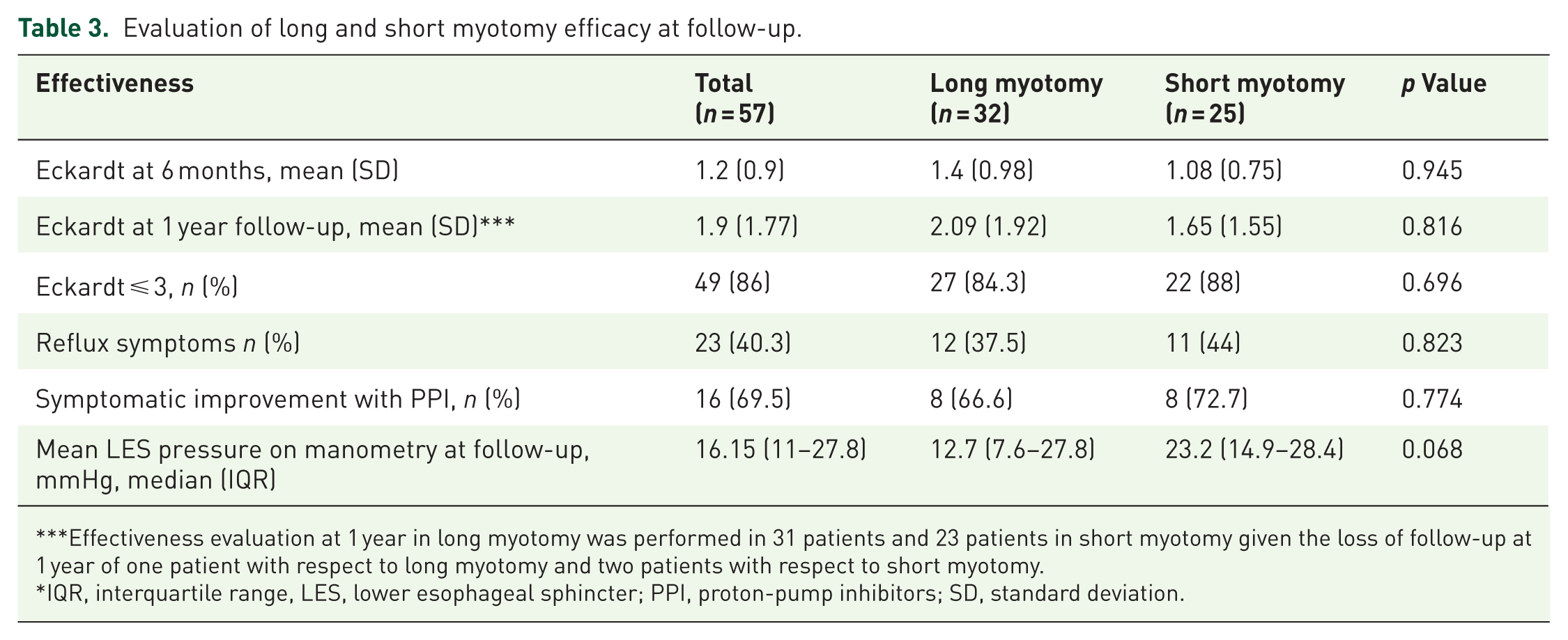
Effectiveness evaluation at 1 year in long myotomy was performed in 31 patients and 23 patients in short myotomy given the loss of follow-up at 1 year of one patient with respect to long myotomy and two patients with respect to short myotomy.
IQR, interquartile range, LES, lower esophageal sphincter; PPI, proton-pump inhibitors; SD, standard deviation.
Twenty-three patients (40.3%) reported reflux symptoms at follow-up, with symptomatic improvement in 16 (69.5%) patients receiving PPIs. Although the short myotomy patients were more likely to have reflux symptoms at 6 months than the long myotomy patients (44.0% vs 37.5%), this difference was not statistically significant between the groups (p = 0.823) and the majority (72.7%) showed symptomatic improvement with PPI use. Eleven patients had esophagitis on upper gastrointestinal endoscopy between 3 and 6 months of follow-up.
Mean LES pressure on control manometry taken at 6–12 months follow-up tended to be higher in the short myotomy group (23.2 mmHg IQR 14.9–28.4 vs 12.7 mmHg IQR 7.6–27.8, p = 0.068), a difference that was not statistically significant (Table 3).
Discussion
The present study suggests that in patients with achalasia undergoing POEM, short myotomy is associated with similar efficacy as measured by symptoms at 6 and 12 months, with no difference in reflux symptoms, compared with long myotomy, but with several advantages such as shorter procedure time, lower incidence of emphysema and capnoperitoneum, and less need for abdominal puncture.
The most common achalasia subtype was type II (67%), followed by types I and III (21% and 13%, respectively). These data are consistent with studies showing that subtype II accounts for between 50% and 70% of achalasia cases.23,30 The need for reintervention has also been shown to depend on the type of achalasia. One study showed that only 62% of patients with type I achalasia were free of reintervention after 5 years, a lower percentage than for types II and III achalasia (74% and 87%, respectively). 31
The most common symptoms in patients with achalasia are dysphagia for both solids and liquids, non-cardiac chest pain, and regurgitation, which can lead to weight loss. 6 In our cohort, at baseline, dysphagia was present in 100% of patients, followed by regurgitation and chest pain in 47.4% each, weight loss in 45.6%, and heartburn in only 8.7%, with an average Eckardt score of 7.6. All patients had an Eckardt score > 3, which is the cut-off point suggested by various studies for starting treatment. 25
Eighty-six percent of patients in our study had an adequate symptomatic response at 1 year, defined as an Eckardt score ⩽ 3, comparable to those reported in the literature. A meta-analysis of long-term results showed that the clinical efficacy of POEM was maintained in 87% of patients with achalasia. 32 In another study, POEM was shown to be non-inferior to laparoscopic Heller myotomy with Dor fundoplication in controlling achalasia symptoms at 2 years, with a clinical success rate of 83% for POEM; 33 however, clinical success rates as high as 98%, defined by an Eckardt score ⩽ 3, have been reported, according to a meta-analysis that included 36 studies with 2373 patients. 34 In our study, the reported clinical efficacy was lower; this may be explained by the fact that a significant percentage of our patients had previously received treatment for achalasia (35%), of which 26.3% had previously undergone Heller myotomy. This is to be expected as approximately 18%–27% of patients may require additional treatment at 5 years after Heller myotomy. 35 However, prior intervention has been associated with a lower clinical response in patients undergoing POEM for the treatment of achalasia compared to patients with achalasia undergoing POEM without prior intervention. A retrospective multicenter cohort study compared POEM with prior surgical Heller myotomy to POEM without prior surgical Heller myotomy and demonstrated a significantly lower efficacy (defined as Eckardt score ⩽ 3) in the group with prior Heller myotomy (81%) compared to the group without prior Heller myotomy (94%), but no significant differences in safety and adverse events were observed. 36
In our study, there was no statistically significant difference in the proportion of patients with an Eckardt score ⩽ 3 1 year after POEM. This finding is similar to that reported in several studies that have shown no inferiority of short myotomy compared to long myotomy.19,21,37,38 LES pressure at follow-up manometry at 6–12 months was lower in the long myotomy group compared to the short myotomy group, (12.7 ± 7.6–27.8 vs 23.2 ± 14.9–28.4) but did not reach statistical significance (p = 0.068). This finding may be partly explained by the variability inherent in manometric measurements, the wide interquartile ranges observed in both groups, and the small sample size, which reduces statistical power to detect significant differences.
Nevertheless, it is important to emphasize that despite this difference, no significant differences were observed in major clinical outcomes, including clinical response and overall procedural success. This suggests that both short and long myotomy approaches achieved adequate functional decompression. In both groups LES pressure was lower than before surgery (downward amplitude was greater than 50%) and is considered a measure of efficacy for the treatment of achalasia. 39 Similarly, longer myotomy lengths have not been shown to improve GEJ compliance. Teitelbaum et al. 18 analyzed the effectiveness of extended proximal esophageal myotomy in POEM using an intraoperative functional lumen imaging probe (FLIP) to assess GEJ compliance. GEJ compliance was significantly increased by creating a submucosal tunnel and performing GEJ myotomy, but there was no further increase with extended proximal myotomy. This suggests that a shorter myotomy is sufficient to improve esophageal physiology and that an extended proximal esophageal myotomy is not necessary.
We used the iPOEM classification to assess procedural complications, a classification specific to the POEM procedure. 26 There were no differences in major/clinically significant events between the long and short myotomy groups. In fact, no patient in the short myotomy group required ICU admission, urgent surgery, transfusion, or hospitalization for more than 5 days, while in the long myotomy group, only one patient (3.1%) required urgent surgery, and the same patient required a blood product transfusion and hospitalization for more than 5 days. However, we found significant differences in the incidence of minor complications, including emphysema, capnoperitoneum, and the need for an abdominal puncture during the procedure.
Other studies that have compared short myotomy with long myotomy have not shown a difference in complications.19–21 and a meta-analysis suggested that short myotomy may be associated with fewer adverse events OR 0.67 (95% CI 0.29–1.53), but the estimate did not reach statistical significance (p = 0.34). 38 Our study provides new evidence in favor of short myotomy in terms of the incidence of complications and improves the accuracy of this estimate. The lower rate of adverse events associated with short myotomy may be related to a shorter procedure time, as demonstrated in our study.
Previous studies have already demonstrated the advantage of short myotomy over long myotomy in terms of procedure time. Huang demonstrated that a short myotomy ⩽ 7 cm (esophageal myotomy length < 4 cm and gastric myotomy length 2–3 cm) required less time (46.6 ± 18.5 min vs 62.1 ± 25.2 min, p = 0.001). 19 Similar to that reported by Nabi et al. (44.03 ± 13.78 min and 72.43 ± 27.28 min, p < 0.001) 20 and Familiari et al. 21 (40 vs 50 min, p < 0.0001). A systematic review and meta-analysis of five trials with a total of 521 patients (241 min for short myotomy and 280 min for long myotomy) confirmed the same finding. 38
There was no difference in hospital stay between the groups. This finding is similar to that reported in a meta-analysis of five trials with a total of 225 patients who underwent short myotomy and 222 who underwent long myotomy (MD 0.17, 95% CI −0.09 to 0.44, p = 0.20). 37
Twenty-three patients (40.3%) reported reflux symptoms at follow-up. Several studies have reported less frequent reflux symptoms, with percentages ranging from 9% to 43%, reflux esophagitis in 40% to 68%, and positive ambulatory pH monitoring for reflux in 38% to 57%.11,23,30,40,41 One study reported that 60% of patients had endoscopic evidence of esophagitis 1 year after the procedure, and 43.1% had reflux symptoms. 42 The higher reported frequency of reflux symptoms in our study could be explained by the fact that we did not have an objective variable such as 24-h pH monitoring to assess whether it was true reflux, as true acid reflux symptoms in patients with post-POEM achalasia are not always the cause of reflux symptoms, they can also be due to esophageal acidification without reflux due to stasis of ingested acidic foods or acid fermentation, or esophageal hypersensitivity to chemical or mechanical stimuli, and in these scenarios, 24-h impedance pH monitoring is essential to differentiate the causes of esophageal acidification. 43 Additionally, risk factors for GERD have been described after POEM. Mota et al. 44 performed a meta-analysis reporting the risk factors for predicting the development of GERD after POEM. They found that full-thickness myotomy was associated with a higher incidence of GERD (CI: 0.05 (−0.00, 0.10], p = 0.06), as was anterior myotomy (CI: −0.09 (−0.20, 0.01), p = 0.07, I2 = 0%), both with borderline significance. In our study, the vast majority underwent posterior myotomy (96.5%) and a significant percentage underwent full thickness myotomy (28%), which may also explain the higher reported frequency of reflux symptoms in our cohort.
Most cases of reflux esophagitis are mild and respond well to treatment with proton pump inhibitors (PPIs), as seen in our study. The study by Nabi et al. 41 highlights that post-POEM erosive esophagitis responds to PPI treatment in the majority of patients (81.4%). Furthermore, Shiwaku et al. 45 found that PPIs are more effective for long-term treatment of reflux esophagitis, with significant improvement at 5-year follow-up compared with 1-year follow-up. This suggests that PPI treatment is an effective strategy for managing reflux symptoms in patients who have undergone POEM.
When assessing reflux symptoms in long and short myotomy, we found no significant differences, similar to what has been reported by other authors who have also not shown that the length of myotomy has a significant association with GERD rates, whether measured by pH monitoring, reflux symptoms, or esophagitis on upper gastrointestinal endoscopy.19–21,37,38 Only one study showed a shorter acid exposure time as measured by pH monitoring in patients with a short myotomy compared with the long myotomy group (RR 0.58, 95% CI 0.36–0.94, p = 0.03, I2 = 0%). 37
Our study is the only one to date that evaluates perioperative complications using a standardized classification for patients undergoing POEM, and it found a significant difference in the incidence of minor complications. It is also the only one that evaluates the clinical efficacy and safety of short versus long myotomy in the Latin American population.
However, it has limitations that we must acknowledge. First, the retrospective observational design could limit the detection of outcomes of interest; however, symptoms and complications were systematically recorded in the medical records, limiting the risk of bias. Second, treatment assigned by the treating gastroenterologist could have led to systematic differences between the groups with potential selection bias; however, the baseline characteristics of the patients were similar in both groups. Third, the relatively small sample size led to imprecision in the estimates of some of our outcomes of interest. Finally, an important limitation of our study is that we were unable to consistently and objectively assess GERD, as very few patients had 24-h pH monitoring or follow-up endoscopy. However, our results regarding postoperative reflux disease, as assessed by typical symptoms, were consistent with studies conducted elsewhere in the world. Further clinical trials are needed to confirm our results.
Conclusion
Our data suggest that the short myotomy in POEM is non-inferior to the long myotomy in terms of clinical success and long-term reflux disease in the management of patients with achalasia. It also offers advantages such as shorter procedure times and potentially lower rates of minor complications, making it the preferred option in most cases.
Supplemental Material
sj-docx-1-cmg-10.1177_26317745261433142 – Supplemental material for Clinical efficacy and safety of short-length peroral endoscopic myotomy (POEM) compared with long-length myotomy for the treatment of achalasia
Supplemental material, sj-docx-1-cmg-10.1177_26317745261433142 for Clinical efficacy and safety of short-length peroral endoscopic myotomy (POEM) compared with long-length myotomy for the treatment of achalasia by Valentina Dávila-Ruales, Hernando J. Vergara, Oscar M. Muñoz, Alexander Castañeda, Rómulo D. Vargas and Jesús A. Rodríguez in Therapeutic Advances in Gastrointestinal Endoscopy
Footnotes
Acknowledgements
The authors declare that there are no acknowledgments for this manuscript.
Declarations
Availability of data and materials
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
