Abstract
Hypoglossal nerve stimulation (HGNS) has emerged as a successful surgical treatment strategy for moderate to severe obstructive sleep apnea in patients failing first-line positive airway pressure therapy. HGNS explantation due to adverse events such as pain and infection is rare and has yet to be well described. Here, our correspondence describes the first case series of patients who have undergone explantation of the Inspire HGNS system. Five patients were identified who underwent HGNS explantation. Three patients underwent explantation due to magnetic resonance imaging (MRI) incompatibility. One patient underwent explantation due to poor cosmesis. One patient underwent explantation due to surgical site infection. Average operative explant time was 163 minutes. MRI incompatibility, poor cosmesis, and device-related infection are reasons for HGNS explantation. Future need for MRI or chest wall surgery should be considered in patients being evaluated for HGNS implants.
Obstructive sleep apnea is a common disorder that can cause a significant reduction in quality of life and has associations with many comorbid diseases, such as hypertension, coronary artery disease, congestive heart failure, and type 2 diabetes.1-5 Hypoglossal nerve stimulation (HGNS) has been shown to be an effective treatment method for moderate to severe obstructive sleep apnea in patients failing first-line positive airway pressure therapy. Studies of HGNS have demonstrated a significant reduction in apnea-hypopnea index (AHI) among implanted patients, with excellent overall patient satisfaction of the device.6,7
Given an increasing number of HGNS implantation cases over the last several years, the need for device explantation has emerged and has been described to address adverse events, such as pain, device expulsion, neuropraxia, and most notably infection. 8 As HGNS explantation can be technically challenging, understanding the reasons for device explantation is necessary to guide patient selection and mitigate adverse events, explantation, and reoperation.
The goal of this correspondence is to describe the first case series of patients who have undergone explantation of a HGNS system by a single high-volume surgeon having performed >100 implants.
Methods
A series of patients who underwent HGNS (Inspire Medical Systems) explantation at an academic tertiary care center were evaluated. Demographic information, body mass index, comorbidities, preoperative Epworth Sleepiness Scale, and AHI were identified. Postimplant AHI, indication for explantation, explant case length, and operative complications were also identified. No cases were excluded from analysis. Descriptive statistics were performed. This study was approved by the University of Michigan Institutional Review Board (HUM00155002).
Results
Five explant cases were identified. The mean age of study participants was 65.4 years (SD, 6.5); 40% were male; and the mean preoperative body mass index was 31.0. Mean preimplant AHI and Epworth Sleepiness Scale were 45.2 and 15.6, respectively. Average postimplant AHI was 42.1. Average time to explantation was 163.4 minutes. Of 5 patients, 3 were explanted given the need for magnetic resonance imaging (MRI) and suboptimal device use. The reasons for MRI included characterization of cardiomyopathy, characterization of new renal mass, and investigation of unresolving back pain. One patient was explanted given poor cosmesis and gender affirmation surgery, and 1 patient was explanted due to surgical site infection ( Table 1 ). There were no complications related with explantation.
Reasons for HGNS Explantation. a
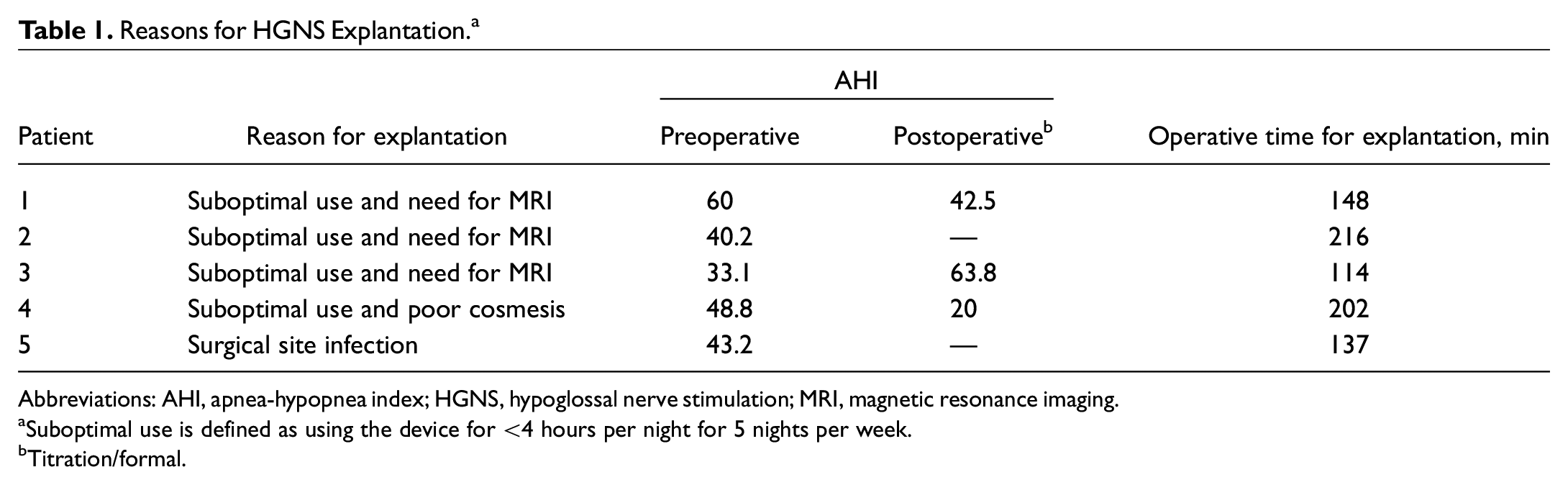
Abbreviations: AHI, apnea-hypopnea index; HGNS, hypoglossal nerve stimulation; MRI, magnetic resonance imaging.
Suboptimal use is defined as using the device for <4 hours per night for 5 nights per week.
Titration/formal.
Discussion
This correspondence is the first to evaluate a case series of explants of this HGNS system and describes overall themes for explantation, notably MRI incompatibility, poor cosmesis, and risk of infection ( Figure 1 ).
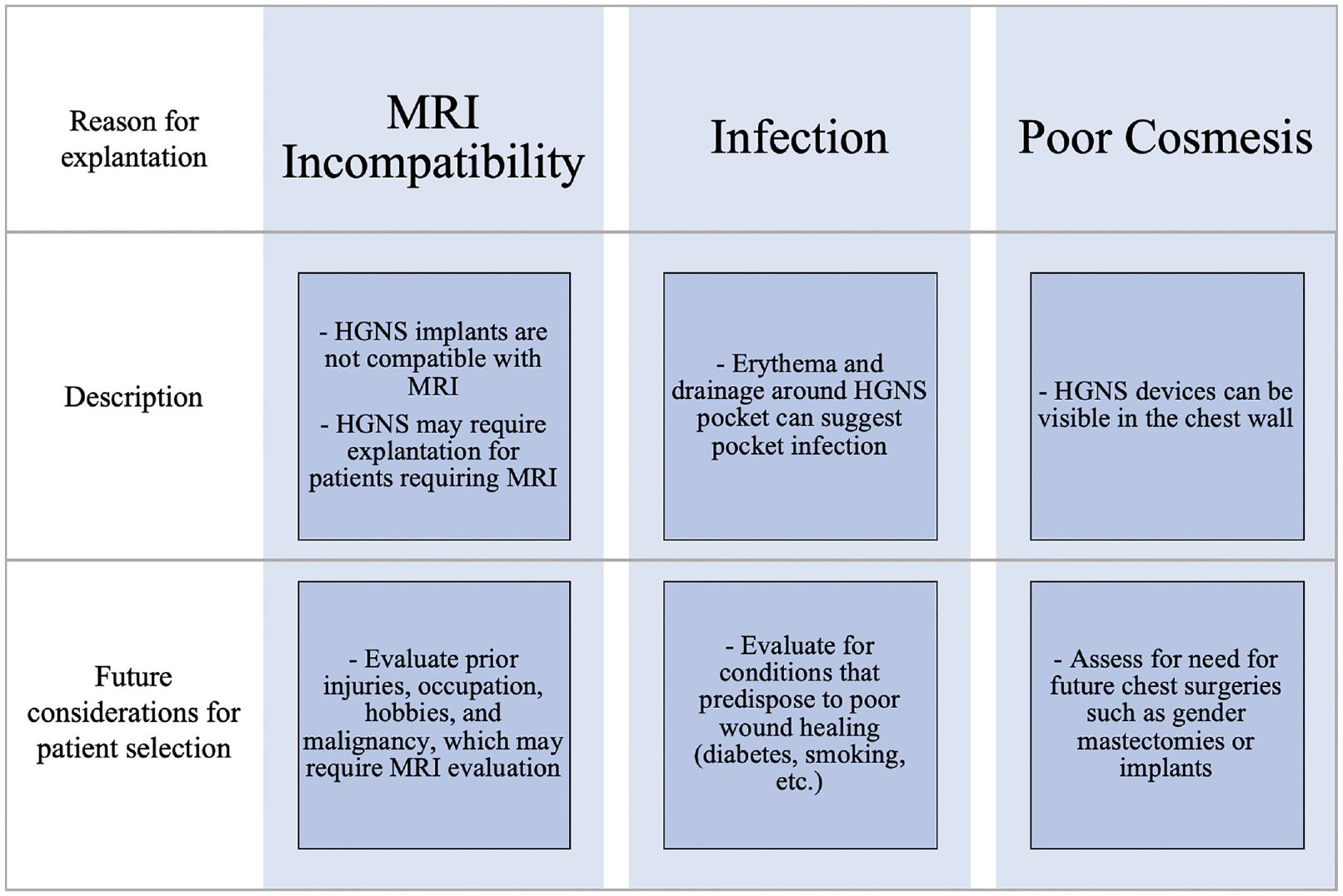
Future considerations for hypoglossal nerve stimulation (HGNS) explants. MRI, magnetic resonance imaging.
The need for MRI was the most common reason for explantation, demonstrating a significant limitation of this device. These patients also reported suboptimal device use; however, the need for MRI was the ultimate reason for explantation. Future need for MRI is an essential component of preoperative evaluation for HGNS implantation. Assessment of the patient’s prior injuries, hobbies, as well as occupation is necessary for a complete understanding of the patient’s need for future MRI, which may prohibit HGNS implantation. Similarly, a study of the Apnex Medical stimulator noted MRI incompatibility as a reason for explantation. 9 Future generations of HGNS devices that are MRI compatible could mitigate this limitation. MRI-compatible HGNS devices such as the Genio system (Nyxoah) are currently under investigation and may prove advantageous over MRI-incompatible implants.
This case highlights an important aspect of HGNS implants in that they can often be visible under the skin. Preoperative counseling should include discussions regarding visibility of the device under the skin and may need to incorporate questions about future chest surgery, such as gender mastectomies or implants in transgender patients.
Device-related infection has been recognized as an adverse event requiring HGNS explantation. 8 One patient in this series experienced an implant-related infection. In this case, the patient’s infection became clinically apparent 3 weeks postoperatively by erythema, drainage, and fullness of the implant pocket. This complication of HGNS should be especially considered in the case of patients who may have diabetes, smoking, or other comorbidities that could predispose the patient to poor wound healing.
This study also demonstrates that HGNS explantation requires significant operative time. On average, explant operative time for the cases presented in this study was 163 minutes. The significant scar tissue at the chest wall pocket and below the mandible due to reoperation in these areas makes explantation technically challenging. Of note, the presented cases were each performed via a 3-incision approach, which may have led to longer operative times. Patients who undergo a 2-incision implantation would likely have had reduced explantation operative time.
Limitations of this study include its retrospective nature and relatively small number of explantation cases. Additionally, given the experience of a single academic center with highly experienced sleep surgeons, our findings may be limited in generalizability to similar facilities, and future multi-institutional experiences may be beneficial. Ultimately, proper patient selection is critical to the success of HGNS implantation, and this communication offers insight into factors that affect long-term use of HGNS beyond strict inclusion and exclusion criteria.
Conclusion
MRI incompatibility, poor cosmesis, and device-related infection, often in combination with suboptimal device use, are reasons for HGNS explantation. Future need for MRI or chest wall surgery should be considered in patients being evaluated for HGNS implants.
