Abstract
Objective
Postoperative complication rates were compared between obstructive sleep apnea surgery (OSAS) and hypoglossal nerve upper airway stimulation (UAS).
Study Design
Cohort.
Setting
Multi-institutional international databases.
Methods
OSAS data were collected from the NSQIP database (2014; American College of Surgeons National Surgery Quality Improvement Program). UAS data were obtained from the ADHERE registry (Adherence and Outcome of Upper Airway Stimulation for OSA International Registry; 2016–December 2019). ADHERE comorbidities and complications were categorized to match NSQIP definitions. A chi-square test was used for proportion P values.
Results
There were 1623 UAS procedures in ADHERE and 310 in NSQIP. The UAS group was older than the OSAS group (mean ± SD, 60 ± 11 vs 42 ± 13 years) but similarly male (75% vs 77%) and overweight (body mass index, 29 ± 4 vs 29 ± 3 kg/m2). There was a higher proportion of hypertension, diabetes, and heart disease in the UAS cohort. Palatopharyngoplasty was the most common surgical procedure (71%), followed by tonsillectomy (25%). UAS operative time was longer (132 ± 47 vs 54 ± 33 minutes). Postoperative length of stay was not normally distributed, as 71% of UAS stays were <1 day as opposed to 40% of OSA stays (P < .0001). Thirty-day return to the operating room related to the procedure was 0.1% for UAS and 4.8% for OSAS (P < .0001). Surgical site infections were 0.13% for UAS and 0.9% for OSAS (P = .046).
Conclusion
The UAS cohort was older and more likely to have comorbid hypertension, diabetes, and heart disease. Despite baseline differences, the postoperative complication rate was lower with UAS than with OSAS.
Obstructive sleep apnea (OSA) is a common condition with well-known long-term complications if untreated. 1 Positive airway pressure (PAP) treatment during sleep has been shown to reduce some cardiovascular complication, 2 but 40% to 60% of patients cannot tolerate PAP3,4 and thus seek surgical alternatives. OSA surgery (OSAS), such as palatal and/or tongue base treatment, is a common option 5 but has variable efficacy 6 and limited long-term benefit. 7 Hypoglossal nerve upper airway stimulation (UAS) has recently been shown to be a safe and effective long-term surgical option for selected patients.8-10 Given that retrospective comparisons between OSAS and UAS have shown lower efficacy rates for OSAS,11-13 the next question is to compare procedural safety and postoperative complications between the procedures. Palatopharyngoplasty in particular has known complication rates, predominantly around pain, dysphagia, and bleeding.14,15 To date, there have been no studies comparing complication rates between OSAS and UAS. This study was designed to provide information to the patient and clinician when choosing between surgical approaches (OSAS vs UAS), with the understanding that approaches need to be tailored to patient variables and that neither approach will completely replace the other. 11 The hypothesis in this investigation was that UAS demonstrates lower complication rates than OSAS in retrospective databases.
Methods
Two large OSA treatment outcome databases were queried to compare the complication rates between UAS (ADHERE registry; Adherence and Outcome of Upper Airway Stimulation for OSA International Registry) and traditional OSAS (NSQIP database; National Surgery Quality Improvement Program). This analysis was exempted from human subject oversight (University of Iowa Institutional Review Board 202010547).
The NSQIP database is a nationally validated, risk-adjusted outcomes registry maintained by the American College of Surgeons. All outcomes were prospectively collected via chart review by trained surgical/clinical reviewers, including assessment of patient condition at 30 days after the procedure. The 2014 edition of the database was queried, which is prior to the introduction of UAS. The data set was selected to comprise those who would have met UAS criteria (adults aged ≥18 years, body mass index ≤35). OSA airway surgery was defined as palate surgery per Current Procedural Terminology codes for the primary diagnosis of OSA (palatopharyngoplasty, tonsillectomy, tonsillectomy and adenoidectomy, uvula excision, palatoplasty, or pharyngoplasty). NSQIP contains predefined comorbidities (hypertension, diabetes, heart disease, chronic obstructive pulmonary disease) and surgical metrics (inpatient/outpatient status, length of stay, operative time), as well as postoperative complications at 30 days (readmission, surgical site infection, unplanned reintubation, bleeding and/or return to operating room, sepsis, pneumonia, urinary tract infection, and mortality). Palatal procedures were selected primarily because they are the most commonly performed for OSA, while tongue base procedures are less commonly employed. 5
The UAS cohort was derived from the ADHERE registry, a prospective international multicenter registry tracking standard-of-care outcomes in patients receiving UAS for continuous PAP–intolerant OSA. The study is registered as NCT02907398 on ClinicalTrials.gov and has been ongoing since 2016. Data for this analysis were based on the 2016-2019 period. The registry collects information at multiple time points, such as baseline (preimplant), implant, and 6 and 12 months postimplant. Data are composed of baseline demographics, OSA outcomes, implant statistics, and adverse events.
Both databases report patient demographics, surgical time, inpatient and outpatient procedure rates, and length of stay. To standardize comparisons of complication rates between databases, the 30-day postoperative complications predefined in the NSQIP were used to search for all adverse events in the ADHERE database within a 30-day period.
Data are reported as mean and standard deviation. To compare the baseline characteristics of the 2 patient groups, t tests were performed on numeric data. Chi-square tests were performed to compare frequency data. When sample sizes were small, a Fisher’s exact test was performed to compare frequency data. P values <.05 were considered significant.
Results
The OSAS cohort included 447 patients meeting the criteria of a preoperative OSA diagnosis as well as an airway procedure. After filtering for body mass index ≤35, a total of 310 patients remained. The cohort was predominantly middle-aged overweight males with hypertension as the most common comorbidity. There were a variety of airway procedures in the database, but palatopharyngoplasty was the most common, representing 71% of the cohort ( Figure 1 ).
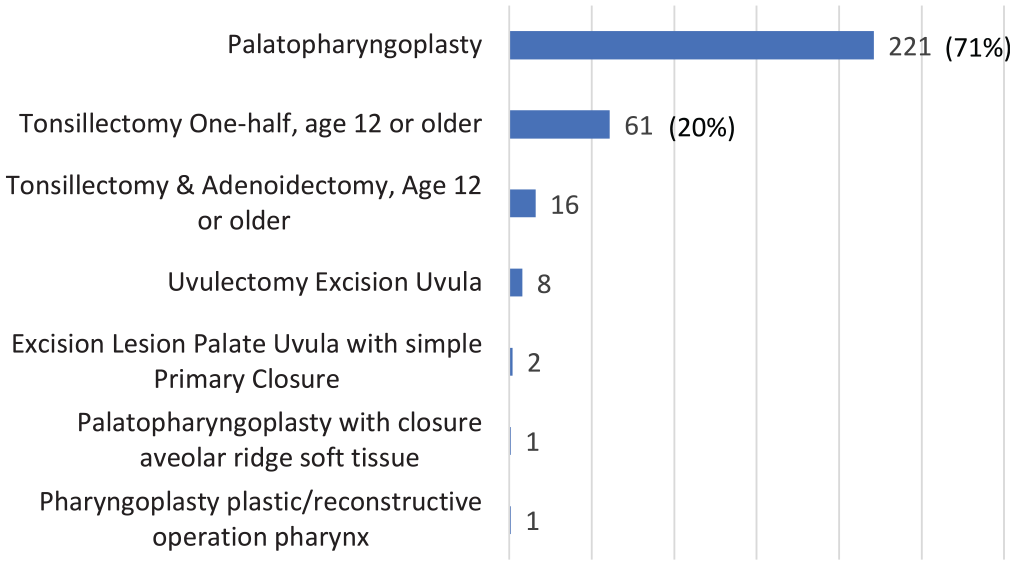
Distribution of obstructive sleep apnea procedures.
The UAS cohort contained 1623 patients. The UAS cohort was older than the OSAS cohort but included similarly overweight males. Hypertension was the most common comorbidity in both cohorts. However, the UAS cohort had a statistically higher percentage of patients with comorbidities than the OSAS cohort ( Table 1 ).
Demographics Comparison Between OSAS and UAS. a
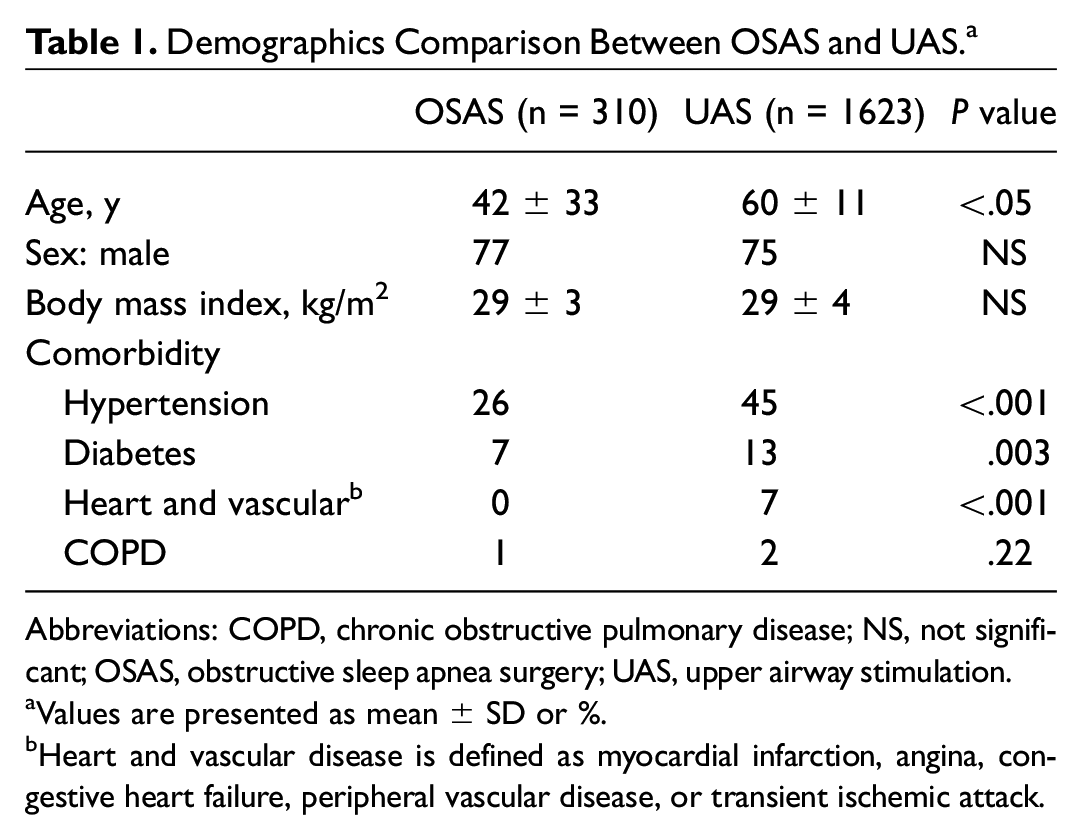
Abbreviations: COPD, chronic obstructive pulmonary disease; NS, not significant; OSAS, obstructive sleep apnea surgery; UAS, upper airway stimulation.
Values are presented as mean ± SD or %.
Heart and vascular disease is defined as myocardial infarction, angina, congestive heart failure, peripheral vascular disease, or transient ischemic attack.
Differences were identified in the surgical metrics between the cohorts. OSAS operative time was shorter than UAS by slightly more than an hour. OSAS was mainly outpatient, and when compared with UAS, the proportion of outpatient cases with UAS was slightly lower than OSAS (69% vs 75%, P = .04); however, this difference was predominantly driven by region. UAS implantations performed in the European Union were less likely to be outpatient than OSAS (5% vs 75%, P < .001); this was due to local medical policy, as opposed to the United States, where UAS cases were more likely to be outpatient than OSAS (94% vs 75%, P < .001). Length of stay was slightly shorter for OSAS (0.7 ± 0.8 vs 1.0 ± 1.7 days, P = .002); this was also predominantly driven by region. Length of stay for UAS was 0.1 ± 0.3 days in the United States, shorter than for OSAS (P < .001), and 3.6 ± 1.2 days in the European Union, longer than OSAS (P < .001; Table 2 ).
Operative Metrics.
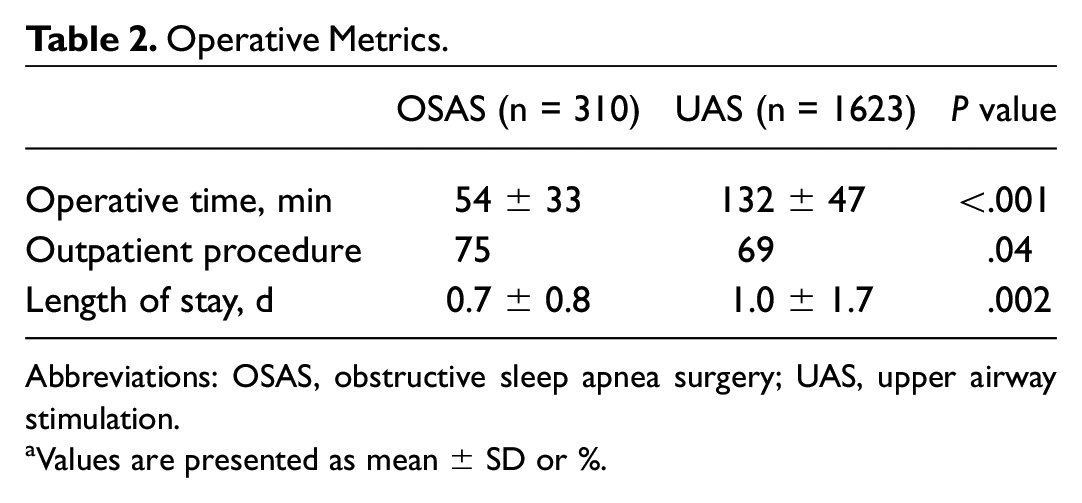
Abbreviations: OSAS, obstructive sleep apnea surgery; UAS, upper airway stimulation.
Values are presented as mean ± SD or %.
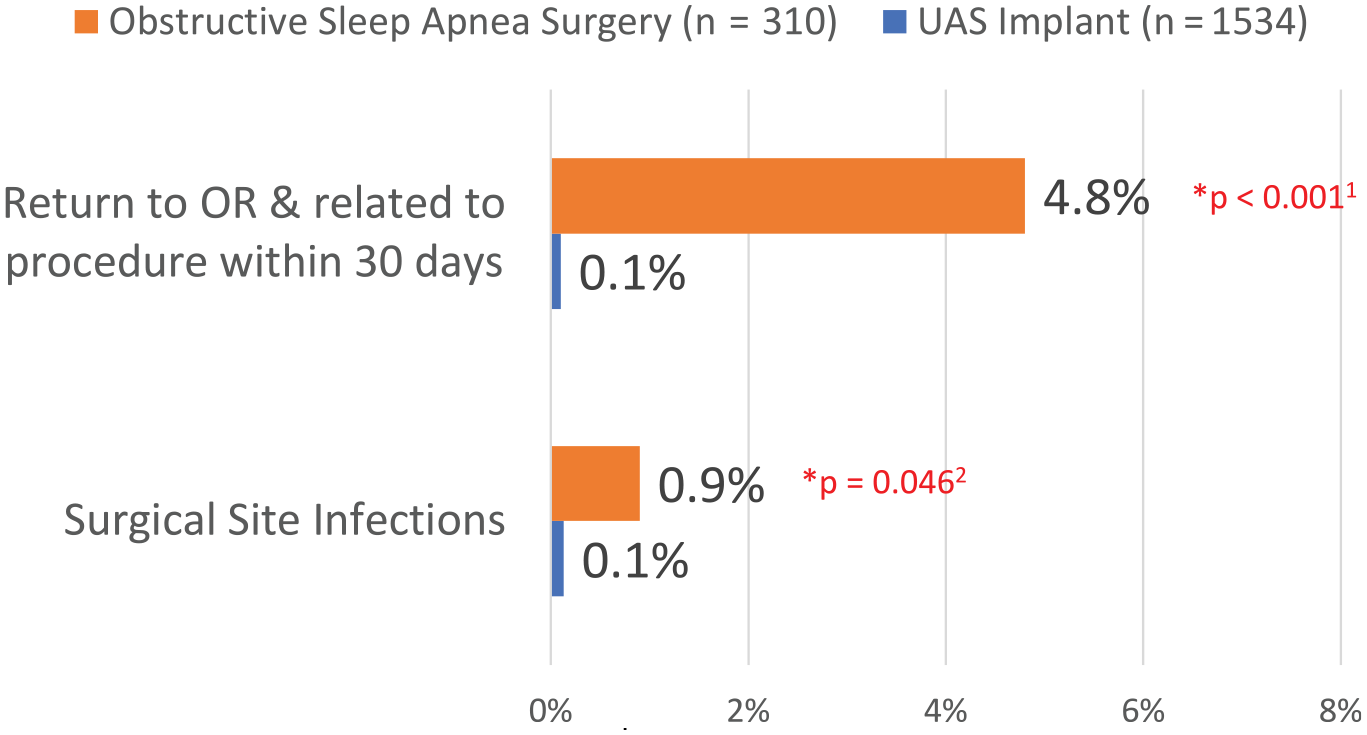
Thirty-day postoperative complication rates were significantly different between the cohorts. As compared with UAS, OSAS had significantly higher rates of return to the operating room (related to procedure) and surgical site infections ( Figure 2 ). Both groups had 0% rates of 30-day death/mortality, urinary tract infection, sepsis, or unplanned reintubation. While the OSAS cohort had predefined complications at 30 days, UAS had 9 revisions (0.6%) that occurred >30 days postprocedure. These revisions were not in this analysis because they did not meet the predefined airway surgery cohort definition of complications within 30 days postoperatively.
Discussion
This study compared immediate and 30-day postoperative complication rates between OSAS and UAS in 2 multi-institutional international databases. The complication rates in these cohorts are similar to other patient series and clinical trials. Both approaches demonstrated low 30-day pneumonia, sepsis, intubation, and death rates. OSAS had significantly higher complication rates versus UAS despite a younger population with fewer comorbidities as initially hypothesized, perhaps due to posttonsillectomy bleeding. The lower average age of patients undergoing OSAS as compared with UAS may be a reflection of the concept that palatopharyngoplasty is less commonly performed in elderly patients, given concerns of postoperative complications. 16 UAS has shown good outcomes with low complication rates in elderly patients.17,18 As a consequence, UAS may provide a surgical option for elderly patients who may be underserved by traditional OSAS.
The significantly longer UAS operative time may represent a learning curve of surgeons for a new procedure/implant. The times may never be completely equivalent, but the expectation is that they would become more similar over time.
This study has several important limitations. First, the periods were different between the cohorts, primarily because UAS is a relatively new surgical therapy for OSA. There is also no one comprehensive contemporary database that contains variables regarding patients undergoing OSAS or UAS. This required us to use different databases for comparisons. The NSQIP does not collect preoperative variables, so direct comparisons regarding efficacy are not possible, although retrospective studies would suggest that UAS is at least equal, if not superior, to OSAS in reducing apnea-hypopnea index. 13 The lack of preoperative variables (especially drug-induced sleep endoscopy) additionally makes it difficult to comment on the degree to which multilevel collapse versus single-site collapse exists in either cohort; however, strong data suggest that most patients with OSA demonstrate some degree of multilevel collapse. 13
There were significantly fewer patients in the OSAS cohort than the UAS cohort, which inherently leads to more likelihood for difficulties in comparing techniques. The NSQIP does not contain specific variables regarding the patients’ OSA severity or PAP intolerance. This did not allow for more careful understanding of, or accounting for, the differences or similarities in the underlying OSA of the cohort. The 2 surgical procedures also have different sets of potential complications, such as hematoma, pneumothorax, nerve injury, and device failure in UAS and oropharyngeal bleeding, dehydration, dysphagia, and airway issues in OSAS. However, the NSQIP database in particular cannot delineate the type of complication, such as posttonsillectomy bleed. The OSAS complications may occur weeks earlier than those in with UAS surgery. In particular, UAS devices are not activated for 4 to 6 weeks after surgery, so placement failure may not be detected within the NSQIP 30-day window; however, long-term studies suggest that the 5-year failure rate for UAS is low and in the realm of 4 failures out of 126 implants. 9
Conclusion
The UAS cohort was older and more likely to have comorbid hypertension, diabetes, and heart disease. Despite baseline differences, the UAS postoperative complication rate was lower as compared with OSAS.
Author Contributions
Disclosures
Footnotes
This article was presented at the AAO-HNSF 2020 Virtual Annual Meeting & OTO Experience; September 13-15, 2020.
The American College of Surgeons National Surgical Quality Improvement Program and the hospitals participating in it are the source of the data used herein; they have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors.
