Abstract
Objective:
An 18 year old male with a hypoplastic midface, low anterior hairline, heavy brows and marked frontal bossing presented for evaluation. Laboratory evaluation for acromegaly was negative. He did have impairment of his bilateral visual fields as confirmed by visual field testing by ophthalmology. His nasal radix was also of particular concern to him as it formed a significantly depressed crease between his nasal bridge and his brow. He requested surgical correction of these deformities from both a functional and aesthetic standpoint.
Methods:
We performed thin-cut CT maxillofacial scanning with 3D reformats and submitted this for virtual surgical planning (VSP). We were able to create a template with which to remove the anterior table of the frontal sinus safely, confidently, and without the aid of a craniotomy. The operation was performed through a preexisting bicoronal incision. The anterior table of the frontal sinus was removed in one piece. His forehead and superior orbits were contoured with a burr. After contouring, the anterior table was fixated in a more recessed position. Nasal radix augmentation was also performed using bone grafting. A coronal brow lift was then performed.
Results:
The patient’s post-operative course was uneventful. He noted marked improvement in his superior visual fields. He had complete resolution of his nasal radix deformity and his frontal bossing. This was confirmed by thin-cut CT maxillofacial scanning postoperatively. His frontal branches were functionally intact and his hairline was raised to a more appropriate position.
Conclusions:
Virtual surgical planning allowed us to perform an osteoplastic forehead reduction safely and without older methods such as Caldwell x-rays with coin reference, transillumination, or the bayonet forcep technique. It also allowed us to avoid the use of surgical navigation which can be time consuming and cumbersome. This VSP-based access to the frontal sinus has applications in many aspects of reconstructive cranial surgery as well as aesthetic forehead reductions for patients that do not require a craniotomy.
Introduction
Frontal bossing is a prominence of the forehead and supraorbital regions that can be associated with a myriad of diagnoses across a wide age range. It is often associated with craniofacial anomalies such as Apert and Crouzon syndromes but can also been seen in older patients suffering from acromegaly. 1 In addition, forehead and orbital rim remodeling is becoming an increasing trend in facial feminization surgery and is commonly addressed as a sequela of severe facial trauma. Regardless of etiology, frontal bossing can have severe functional, psychological, and aesthetic implications for patients. While several methods of correction of frontal bossing have been described from the use of the traditional open bicoronal approach to the newer endoscopic approach, the use of virtual surgical planning for recontouring of the forehead due to frontal bossing has not been described in the literature. We present a case of severe frontal bossing leading to aesthetic and functional limitations for a patient and our use of virtual surgical planning for forehead contouring and discuss the benefits of using this approach.
Patient History
An 18 year old male with a history of epilepsy requiring craniotomy for grid placement 2 years prior presented for evaluation of severe frontal bossing with bilateral brow descent and acute nasal radix angulation (Figures 1 and 2). Endocrinology evaluation for acromegaly including testing for IGF-1 was within normal limits. Ophthalmological assessment demonstrated impairment of his bilateral visual fields.
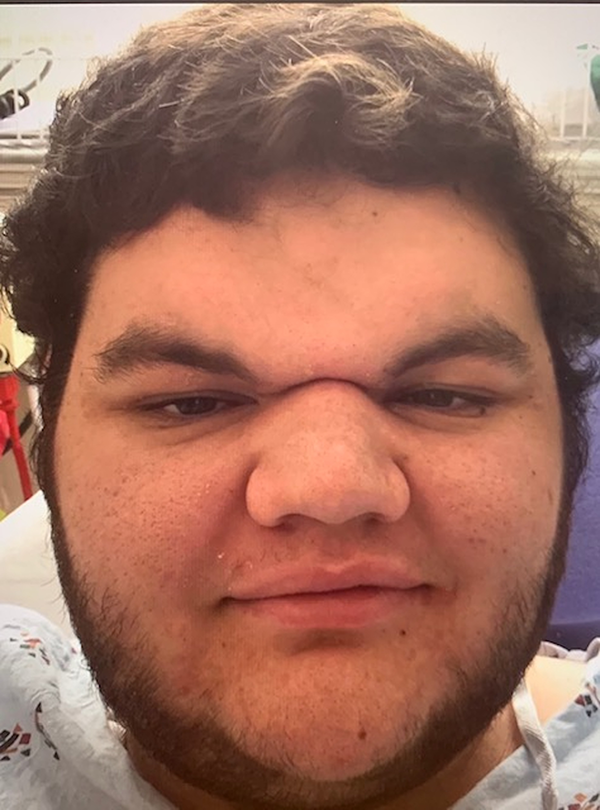
Severe frontal bossing with bilateral brow descent and acute nasal radix angulation (frontal view).
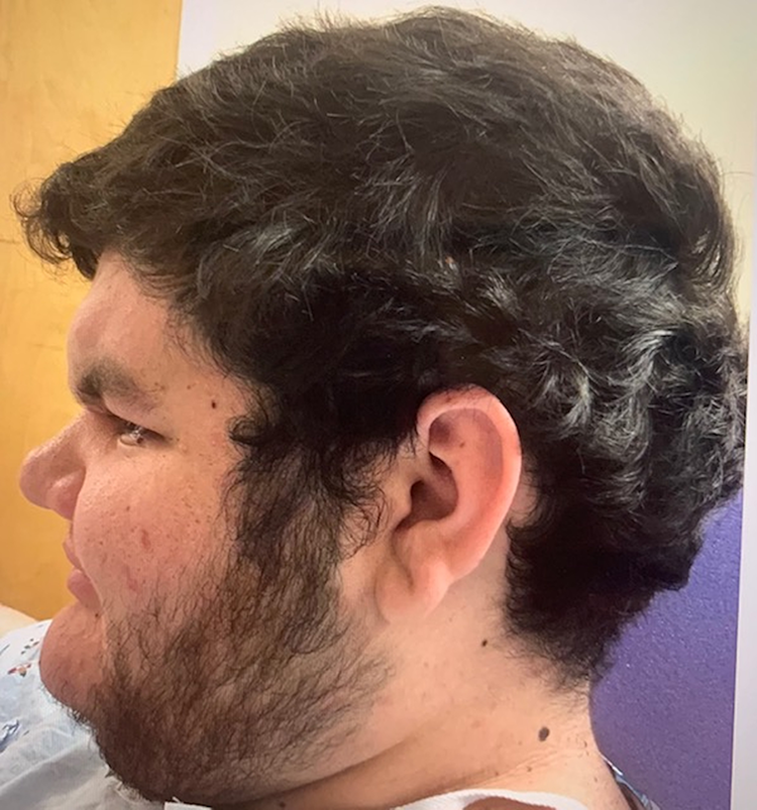
Severe frontal bossing with bilateral brow descent and acute nasal radix angulation (lateral view).
Virtual Surgical Planning
A thin cut CT maxillofacial scan was obtained with 3D reformats which confirmed clinical examination findings. These were submitted for virtual surgical planning. Computer generated images were created to depict where surgical cuts and osteotomies needed to be performed in relation to the frontal sinus (Figures 3 and 4). 3D models and a prefabricated template were then generated from these virtual surgical images to be used to guide patient discussions and for intraoperative use.
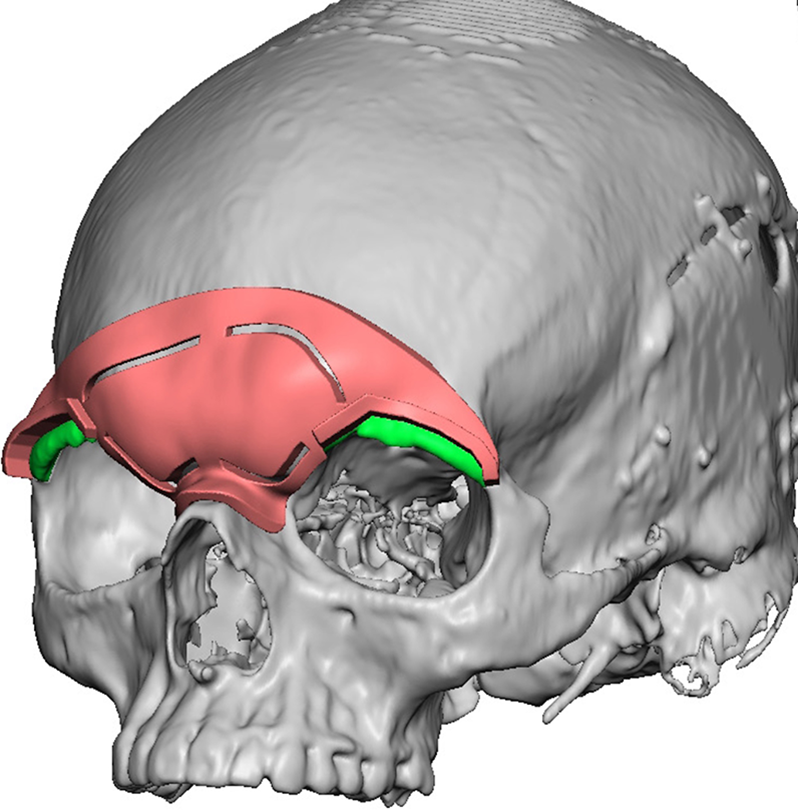
VSP image demonstrating prefabricated template and placement of osteotomies.
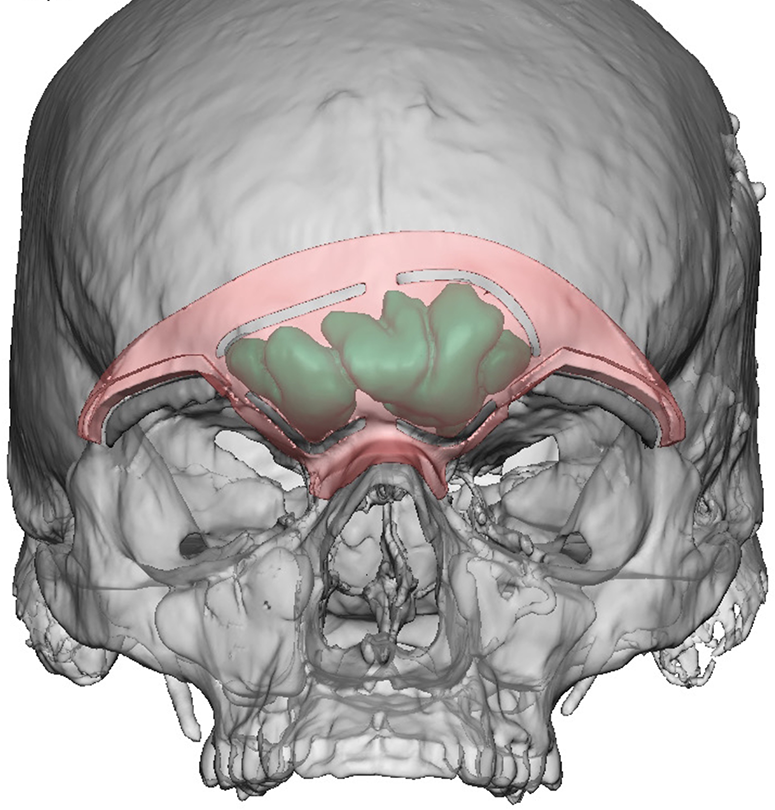
VSP image of prefabricated template in relation to frontal sinus.
Operative Procedure—Frontal Sinus Setback
The patient’s bicoronal incision was utilized to access the cranium. A pericranial flap was harvested upon exposure of the orbits and zygomaticofrontal junctions. The VSP template was affixed to the cranium and a burr was used to remove the anterior table of the frontal sinus around the template (Figures 5 and 6). The patient had patent nasofrontal ducts. An osteotome was used to obtain a bone graft from his nasal bones. An iliac corticocancellous bone graft was also obtained. These 2 grafts were contoured for nasal radix augmentation using semi-rigid fixation and the forehead and anterior table were contoured utilizing a burr to achieve a more aesthetic contour. The anterior table was then affixed to the forehead using cranial and midface plates by setting the inferior portion of the table deep to the nasal bones to create a setback contour (Figure 7). A 15 french drain was placed in the subgaleal space.
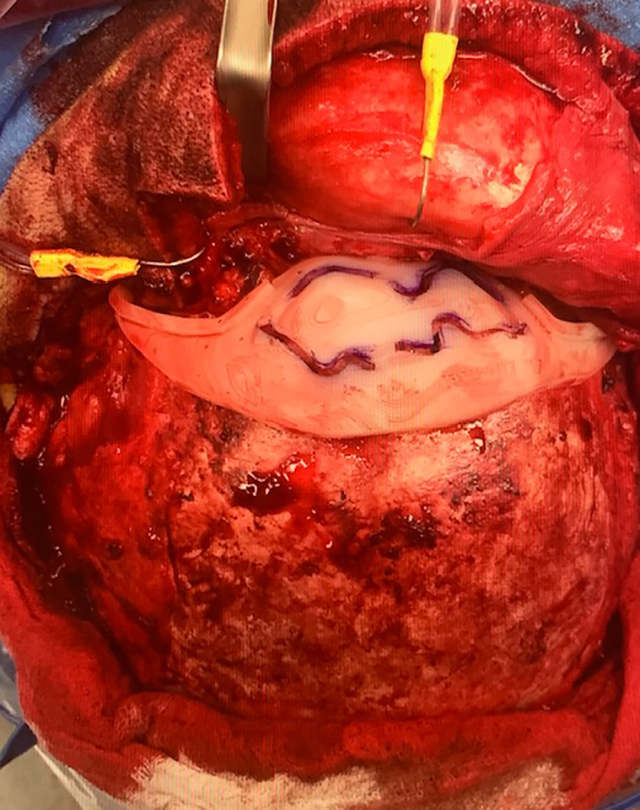
VSP template was affixed to the cranium as template.
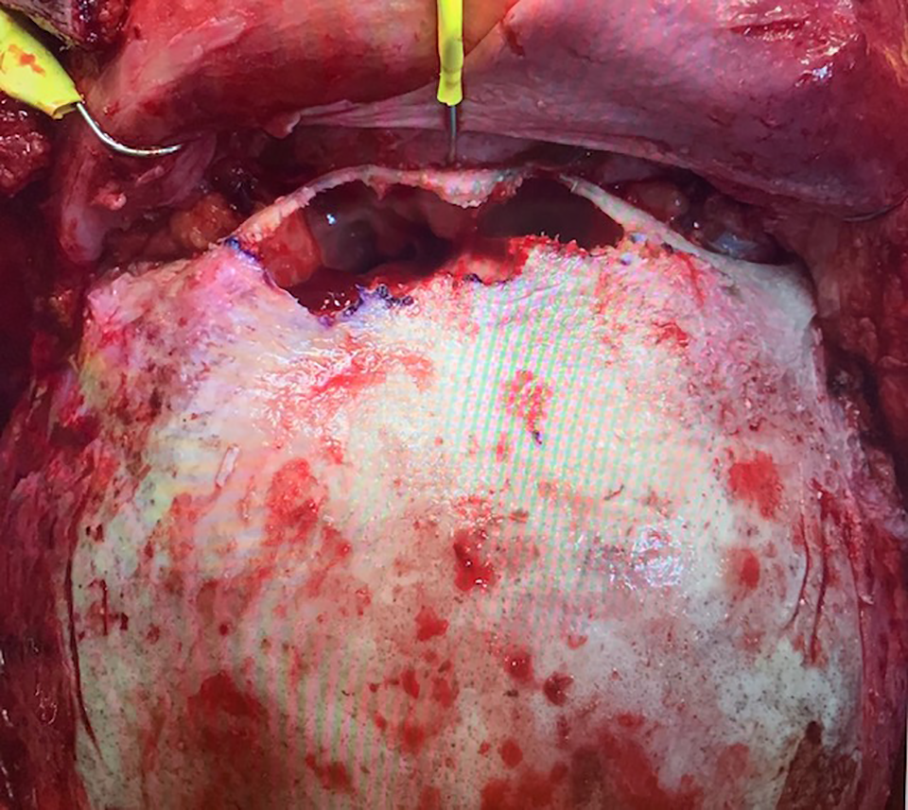
Defect created by removal of anterior table of frontal sinus based on prefabricated template from VSP.
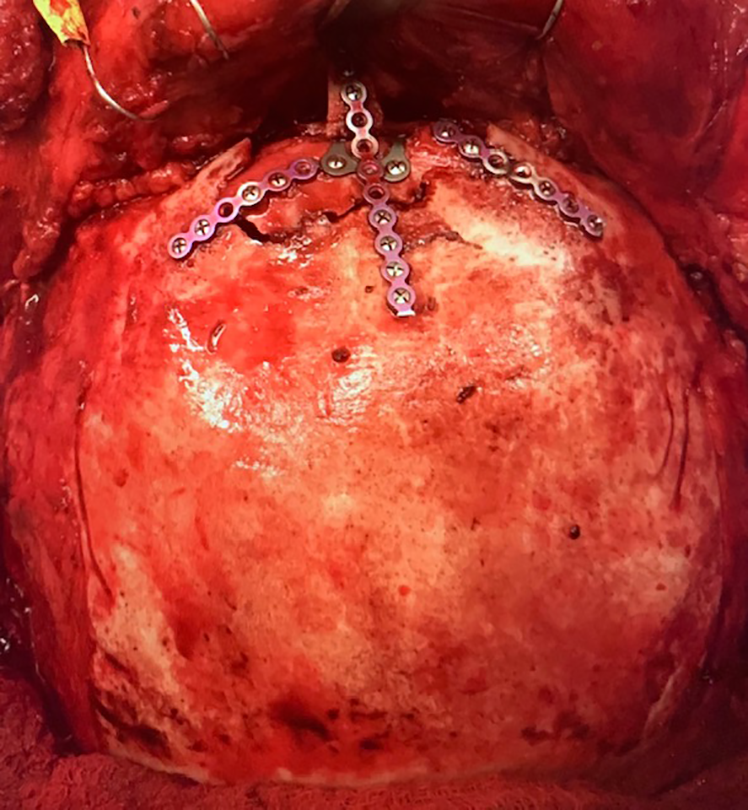
Contoured and plated anterior table with nasal radix augmentation via bone grafting.
Operative Procedure—Coronal Brow Lift
The frontalis muscle was elevated completely down to the superior orbital rims. Partial resection of the corrugator and procerus muscles was performed while preserving the supratrochlear and supraorbital neurovascular bundles. The pericranial flap was draped over the recontoured anterior table. The frontalis muscle was then advanced cephalad and inset to the occipital extension of the frontalis muscle (Figures 8 and 9). A drain was placed and the bicoronal incision closed.
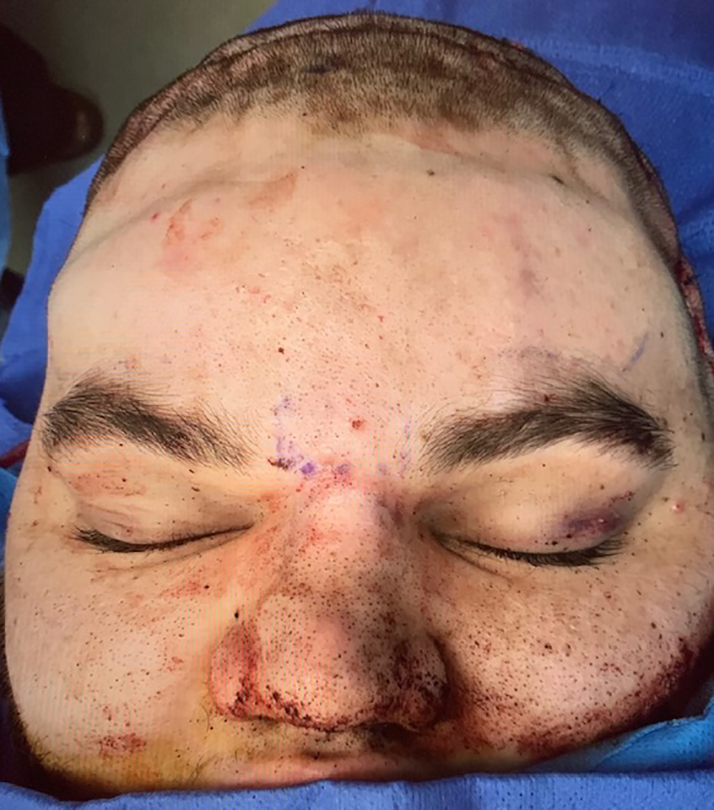
Immediate postoperative result with correction of frontal bossing and severe angulation of nasal radix (frontal view).
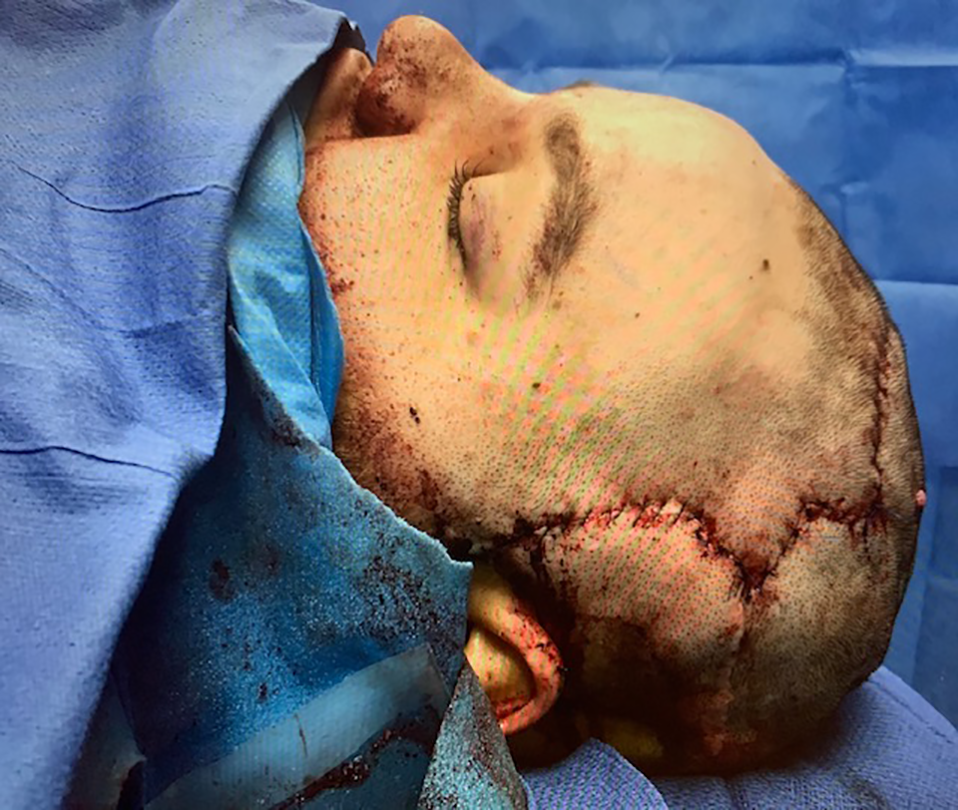
Immediate postoperative result with correction of frontal bossing and severe angulation of nasal radix (lateral view).
Postoperative Course
The patient was admitted to a general floor bed following surgery. A postoperative thin cut CT maxillofacial scan was obtained with 3D reformats immediately postoperatively which showed proper reduction of the forehead with elevation of the nasal radix. The patient was discharged on postoperative day 5 after all drains were removed with normal ophthalmologic examination and intact cranial nerve function. Long term follow-up revealed an improved aesthetic contour with normal visual fields bilaterally (Figure 10).
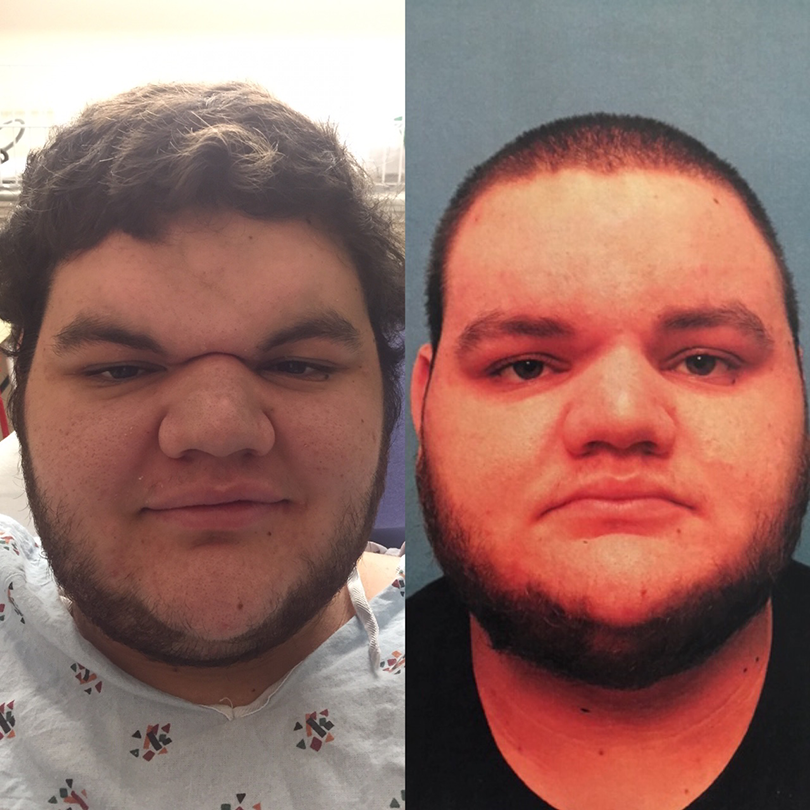
Long term follow-up with successful contouring and correction of visual field impairment.
Discussion
The anatomy of the male forehead includes a flat, sloped appearance with a prominence in the supraorbital region and often looks more square shaped from a frontal view.
2
In addition, the forehead is vertically shorter with smaller orbits compared to the female anatomy.
3
In regards to forehead and orbital rim contouring, the traditional open approach through a bicoronal approach, either trichial or pretrichial, affords the greatest amount of exposure. In our patient, we elected to use a bicoronal incision as the patient had a preexisting incision in this area and would allow adequate exposure for contouring of his forehead and supraorbital rims while allowing for the brow lift to be performed concurrently to improve his visual fields. An alternative approach to correction of frontal bossing is the endoscopic approach. Park et al described their use of endoscopy for both aesthetic and reconstructive facial bone contouring in all areas of the face. Advantages of the endoscopic technique include hidden scars, decreased bleeding, and shorter hospitalization time.
4
Similarly Vasconez et al first described the utility of endoscopy in brow lifting as well as its limitations and de la Torre et al demonstrated that endoscopic brow lift can still be performed in patients with previous coronal brow lifts.
5
–7
While the endoscopic approach is becoming more utilized and requested by patients, we find that virtual surgical planning (VSP) can have additional benefits not afforded by endoscopy. For one, VSP allows for objective surgical planning with quantitative data to provide a visual representation of the final outcome. This replaces the surgeon’s subjective perception of what should be considered normal. In addition, it allows for the patient to participate in their care by being able to visualize before and after models and assists the surgeon in managing patient expectations. In addition, the creation of a prefabricated template for use intraoperatively can lead to decreased operative times and potentially decreased operative blood loss as the proper design has already been formulated. In our patient, VSP also allowed for access to the frontal sinus safely without the need for craniotomy or neurosurgical assistance and replaces older techniques such as Caldwell x-rays with coin reference, transillumination, and the perimeter marking technique with bayonet forceps. It also avoids use of surgical navigation which can be cumbersome and time consuming. Similar applications have been utilized in surgical management of craniosynostosis. Khechoyan et al described their use of prefabricated templates in management of craniosynostosis. They found decreased operative times with the use of computer aided templates. They also found that the ideal reconstructive shape was better achieved and statistically significant in patients who had a prefabricated template used versus those that did not.
8
Saleh et al also found that use of VSP in procedures such as reduction cranioplasty for macrocephaly decreases irregularities seen with free handed osteotomies and thus allows for improved aesthetic results.
9
Similarly, Day et al found utility of VSP in craniomaxillofacial trauma, especially in patients with multiple failed attempts at open reduction and internal fixation. Not only did VSP allow for virtual simulation of the surgery, it also allowed for physical simulation of the operation by utilizing 3D printed skull models based on preoperative CT scans.
10
Utilization of this technique requires that the surgeon coordinate planning with an engineer allowing for more precise measurements and design geared toward a patient’s specific needs. Mazzola et al performed a time and cost-analysis of virtual surgical planning in head and neck reconstruction and found that compared to cases where virtual surgical planning was not used, VSP cases had a shorter length of stay and procedure time and did not impact the overall cost.
11
However, cost analysis does vary between the literature regarding the utility of VSP. Parthasarathy discusses utilization of VSP in cranioplasty for trauma, tumor excision, and decompressive craniotomies, mandibular reconstruction, midface reconstruction, and craniosynostosis.
Conclusions
We combine this method with the use of a traditional brow lift with a successful result as demonstrated by improved contouring and correction of visual fields. This case demonstrates that VSP based access to the frontal sinus can have several applications in reconstructive and aesthetic craniofacial surgery such as allowing for virtual and physical surgical planning prior to actual operative intervention which allows the surgeon to make objective decisions and involve the patient in the surgical planning process, decreased operative times, and more precise osteotomies obviating the need for craniotomy or neurosurgical assistance. All of these factors allow for improved aesthetics in forehead contouring as described in this unique case of osteoplastic forehead contouring.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
