Abstract
Objective
Present a case of a young patient with bilateral bony ankylosis of the TMJ with zero mouth opening treated with TMJ prosthesis.
Methods
The ankylosis was studied in detail with computed tomography (CT) and we used virtual surgical planning in the pre-operative phase to provide splints and cutting guides. The patient was treated with bilateral custom-made alloplastic TMJ prosthesis.
Results
Optimal functional improvement at the 5.5 year follow up after total joint reconstruction without any adverse effects. Mouth opening was 35 mm and the patient was free from pain. CT-images showed no signs of pathology or increased remodeling and bone formation.
Conclusion
Ankylosis of the TMJ in young and adult population presents unique challenges given the need to account for growth of the mandible and anatomical variations. This report supports the use of total joint reconstruction for end-stage TMJ disease.
Keywords
Introduction
Temporomandibular joint (TMJ) ankylosis is a pathologic condition where the mandible is fused to the base of the skull, most commonly at the glenoid fossa by bony or fibrotic tissue. 1 It can occur in both children and adults. Multiple etiologies account for TMJ ankylosis. Trauma is the most common cause. Other causes include arthritis, local and systemic infections, psoriasis, previous TMJ surgery, radiation therapy, internal derangements, perinatal events, idiopathic factors and iatrogenic causes.1,2
The condition of TMJ ankylosis alter the patients’ eating habits, speech ability, oral hygiene, facial symmetry, and growth development. Consequently, it can affect normal life activities and quality of life.1,2 Having TMJ ankylosis can be potentially life threatening in situations where free airway is essential. 1
Classification of TMJ ankylosis can be made by location, type of tissue (fibrous or bony) and extent of fusion (partial or complete). 3 There is a wide variety of surgical methods for the treatment of TMJ ankylosis, such as surgery that includes gap arthroplasty with or without interpositional tissue, distraction osteogenesis and joint reconstruction using autogenous grafts or alloplastic material.4,5
In recent years, a total joint prosthesis (TJP) has become a widely used method of TJR. Compared with autologous bone grafts, TJP has no risk of alteration in size over time and no need for a donor site.2,3 Advantages of alloplastic joint replacement are immediate function, lack of donor site morbidity, reduced operative time and more predictable outcomes. TMJ prosthesis can be divided into two major categories, custom-made and stock products. The benefits of stock prostheses for alloplastic reconstruction are easy intraoperative adaption, cost-effective and they are readily available. Lately, the use of custom-made devices has been extensively used with preoperative surgical planning, resulting in resection guides and patient specific implants. 6 Evidence from several studies show significant improvement in function and pain after alloplastic joint replacement.7,8 Studies demonstrate low incidence of infection and device failures with TMJ prosthesis. 9 TMJ reconstruction with alloplastic prosthesis is considered a reliable, safe, and effective treatment option for selected pathologies of the TMJ.10,11
Case Report
A 21-year-old female was referred to the Oral and maxillofacial surgery department of Uppsala University hospital for treatment of bilateral TMJ ankylosis. The subject, whom have been suffering with total TMJ ankylosis since the age of 16 with zero mm range of motion (ROM), had before referral already undergone TMJ surgery. Initially, bilateral discectomies were performed and secondarily a gap arthroplasty with temporalis muscle fascia flap. TMJ ankylosis relapsed 6 months later.
Her medical history revealed a diagnosis of Juvenile Rheumatoid Arthritis since the age of 10. The fact that she couldn’t open her mouth had caused her severe nutritional disability. She had low BMI, acquired enteral tube feeding and had subcutaneous venous port for delivering her medications. For as long as she and her parents could remember she had never experienced any trauma towards her face during childhood.
Clinical Examination
Prior to surgery the clinical examination revealed bilateral TMJ ankylosis with zero (0 mm) mouth opening. The oral cavity could only be inspected from the vestibular/buccal aspect. The patient was almost fully dentate, except missing anterior left lateral incisor (tooth nr 22) and second left molar (tooth nr 27). She had a Maryland-bridge which closed the gap in the area of anterior left lateral incisor. Furthermore, she had generalized dental plaque and gingivitis buccally in the lower and upper jaw (Figure 1). Oral cavity inspected from the buccal aspect. Patient was unable to open the mouth. Clinical examination revealed 0 mm mouth opening.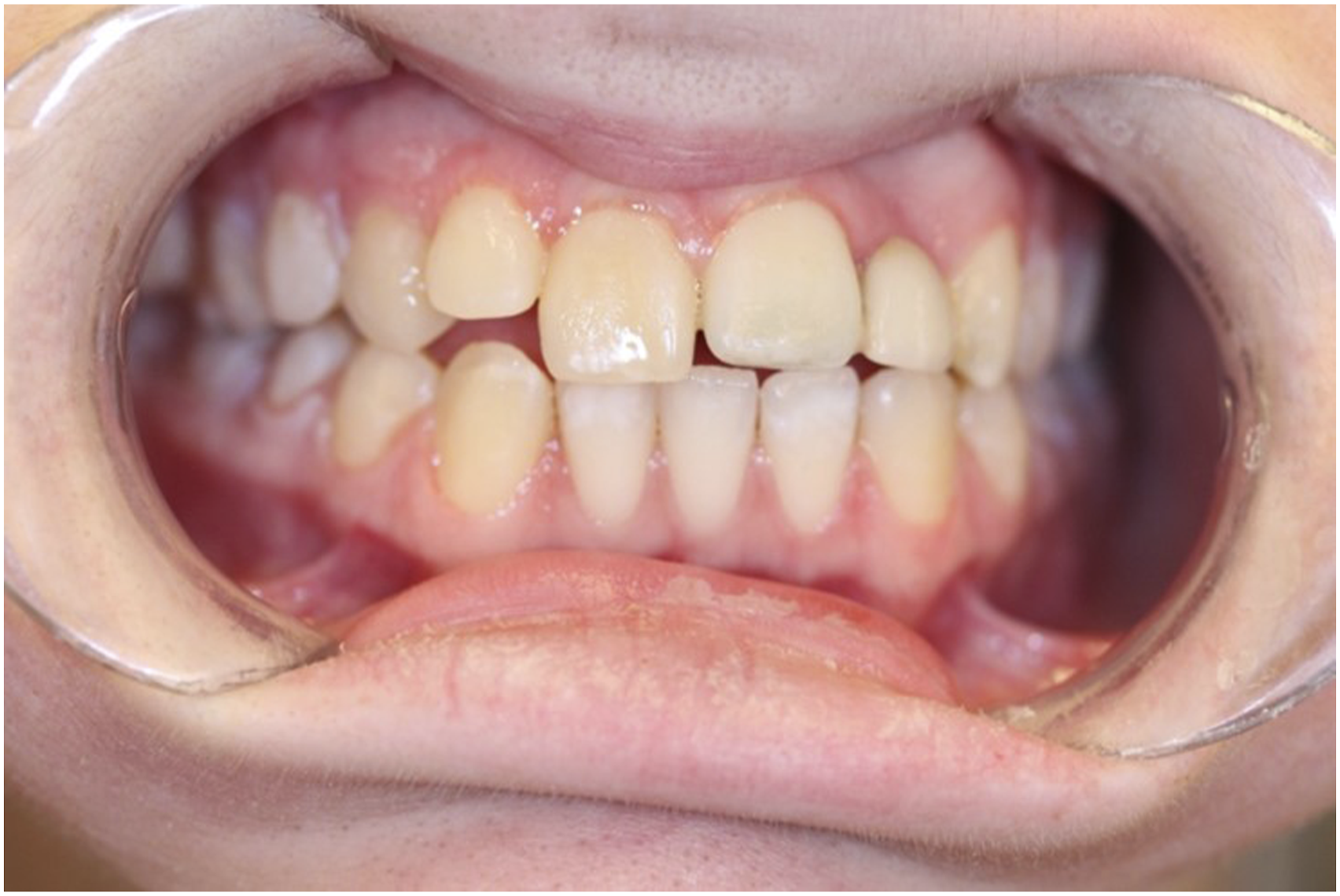
Preoperative Radiological Features
CT images revealed bilateral bony ankylosis of the right and left TMJ.
The condyles were fused with the posterior portions of the zygomatic arch and completely obliterated the articular space. No anatomical structures of the TMJ could be detected. Abnormal bone formation was detected in and around the TMJ. (Figure 2). Preoperative CT images showing the bilateral bony ankylosis. (a) Axial view, (b) coronal view, and (c) 3D CT-reconstruction.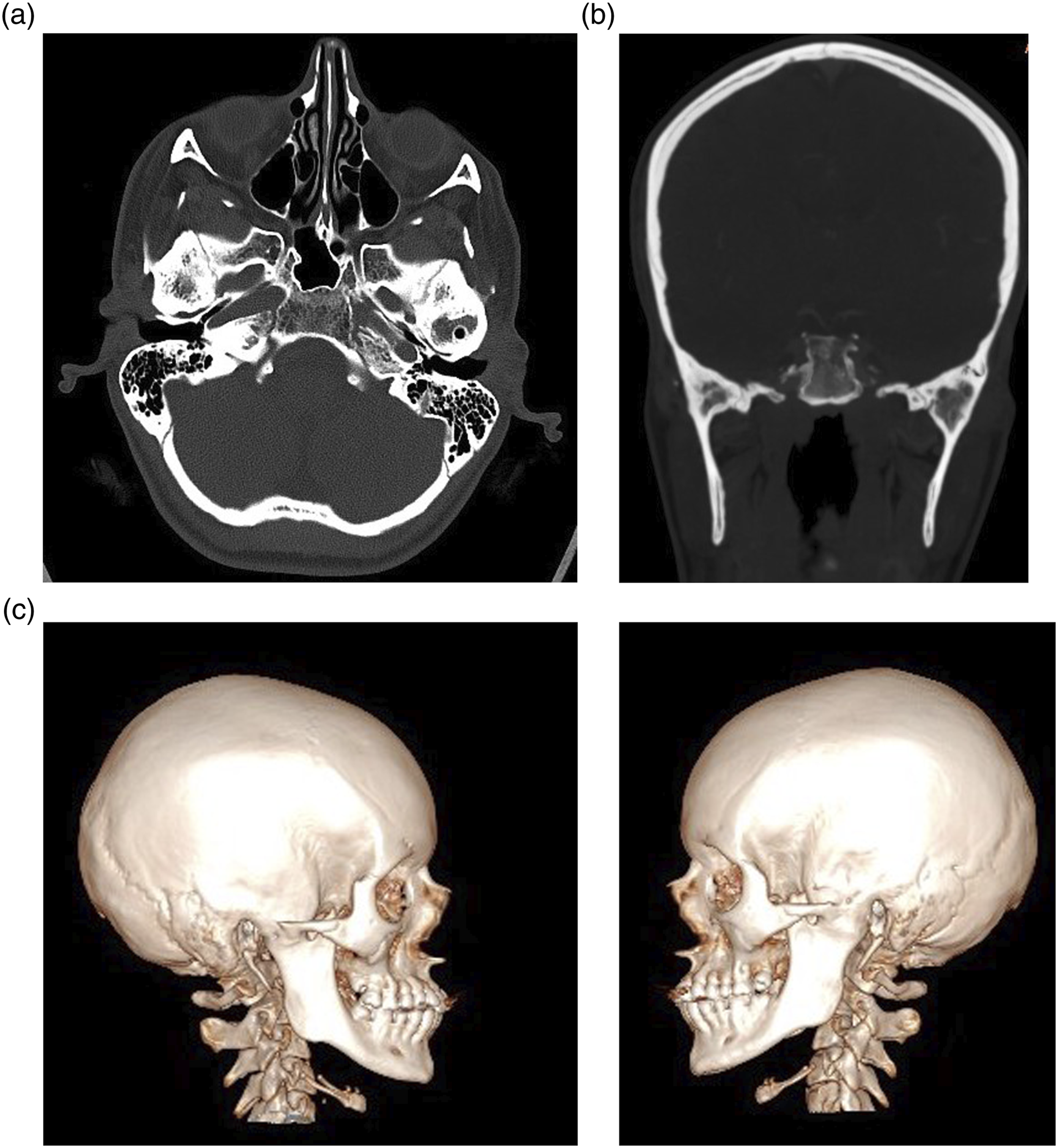
Virtual Surgical Planning (VSP)
We used VSP in order to provide splints to guide occlusal relationship and cutting guides for precise resection. Preoperative CT scans were taken, and our case was uploaded to the manufacturer (Zimmer-Biomet, Total Joint replacement system, Biomet Microfixation Jacksonville, FL, USA). The manufacturer uses a milling method in the acquisition of data from CT till making the TMJ prosthesis. Important data concerning the case were summarized in a case-specific documentation. (Figure 3) Resection margins in the preoperative virtual surgical planning.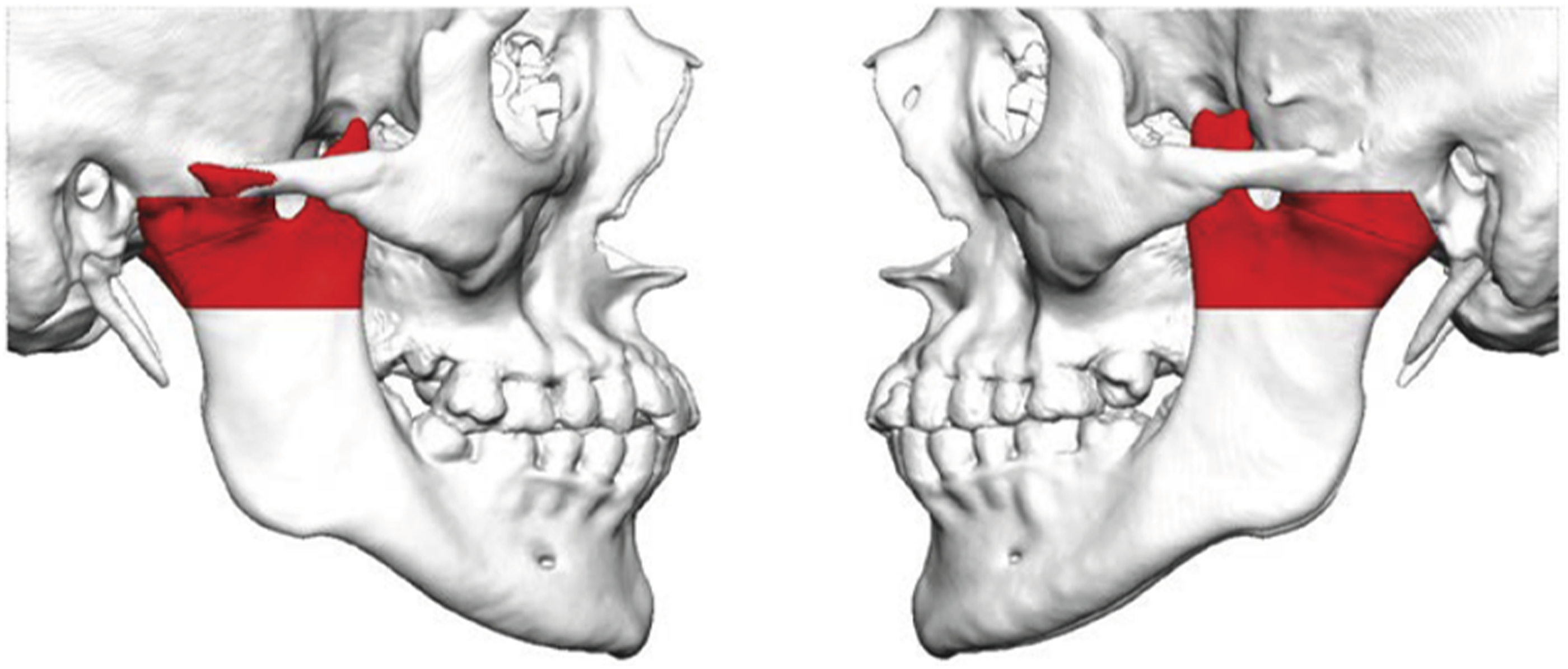
Surgical Technique
Since mouth opening was restricted a fiber-optic guided endotracheal tube intubation was carried out. The patient was anesthetized and a sterile preparation of the face and neck was performed. Outline incisions were made in old scars for preauricular access and new retromandibular incisions were performed bilaterally. The condylar region was accessed via the preauricular incision, and the pretragal avascular plane was followed using blunt and sharp dissection. Preservation of the retromandibular vein and marginal mandibular branch of the facial nerve was secured (Figure 4). Retromandibular access and preservation of the retromandibular vein and marginal mandibular branch of the facial nerve.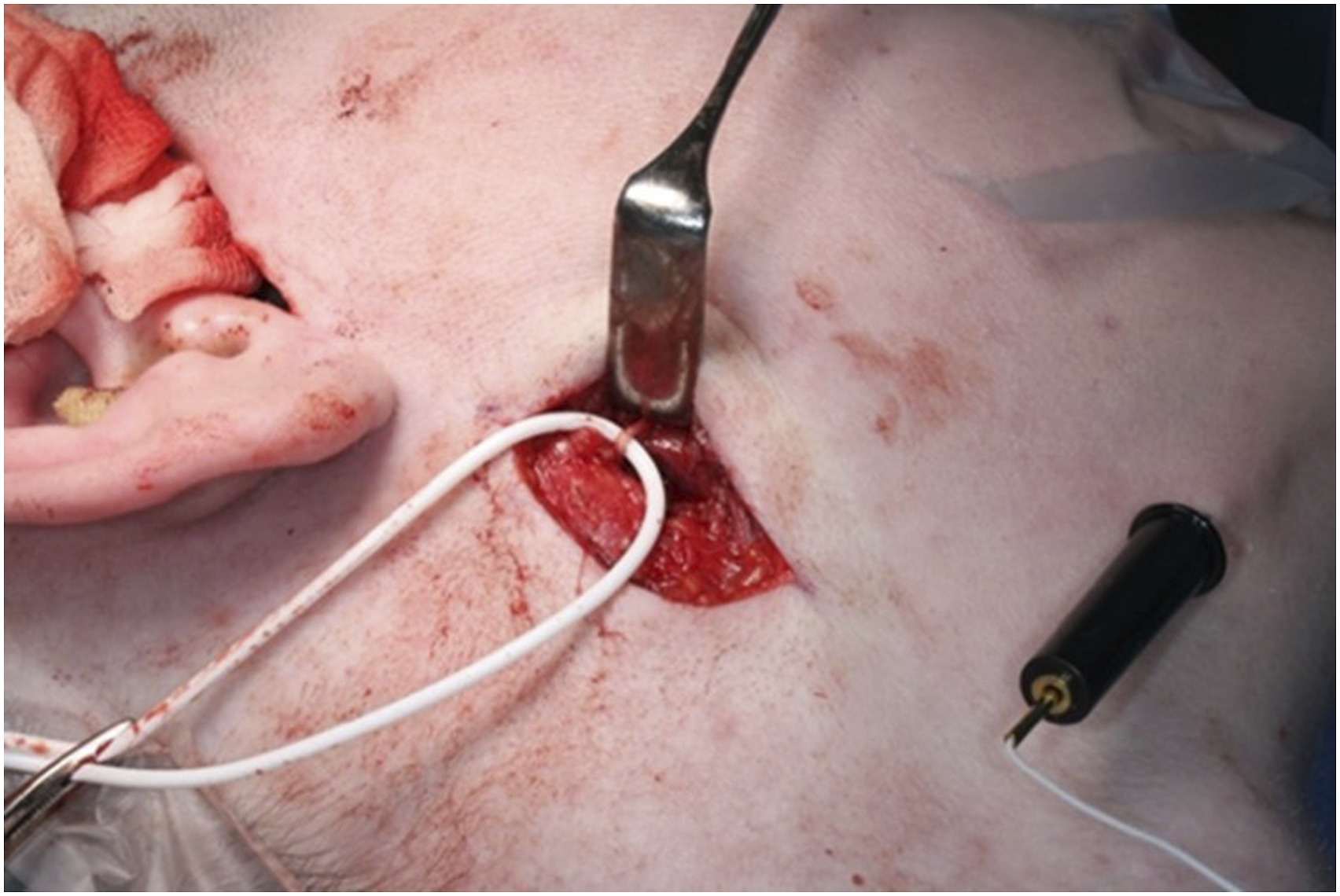
A retromandibular incision through skin and dissection through subcutaneous and platysmal layers were completed with positive identification of the platysma, marginal mandibular nerve and parotidomasseteric fascia. The masseter muscle was then divided, and the inferior border of the mandible was exposed. The condylar neck, sigmoid notch and the coronoid process was exposed and the ankylosis displayed total bony fusion. Since a VSP approach was used, the resection of the condylar head and coronoid process was completed with piezoelectric oscillating saw (“piezo”) and the use of custom-made cutting guides. The glenoid fossa was remodulated and reconstructed with ultra-high molecular weight polyethylene (Zimmer-Biomet, Total Joint replacement system, Biomet Microfixation Jacksonville, FL, USA). The mandibular component was made of cobalt-chromium-molybdenum alloy for the condylar head and titanium alloy for the body. At this point, a standard approach following the manufacturers recommendation and standard-of-care guidelines was used to complete the total joint replacement. The custom-made TMJ prosthesis were inserted and fixated with specified screw lengths after establishing intermaxillary fixation (IMF) (Figure 5). (b) Custom-made TMJ prosthesis installed via the preauricular and retromandibular approaches. (a) Intermaxillary fixation (IMF) with IMF screw and 0.5 mm wire to control the occlusion.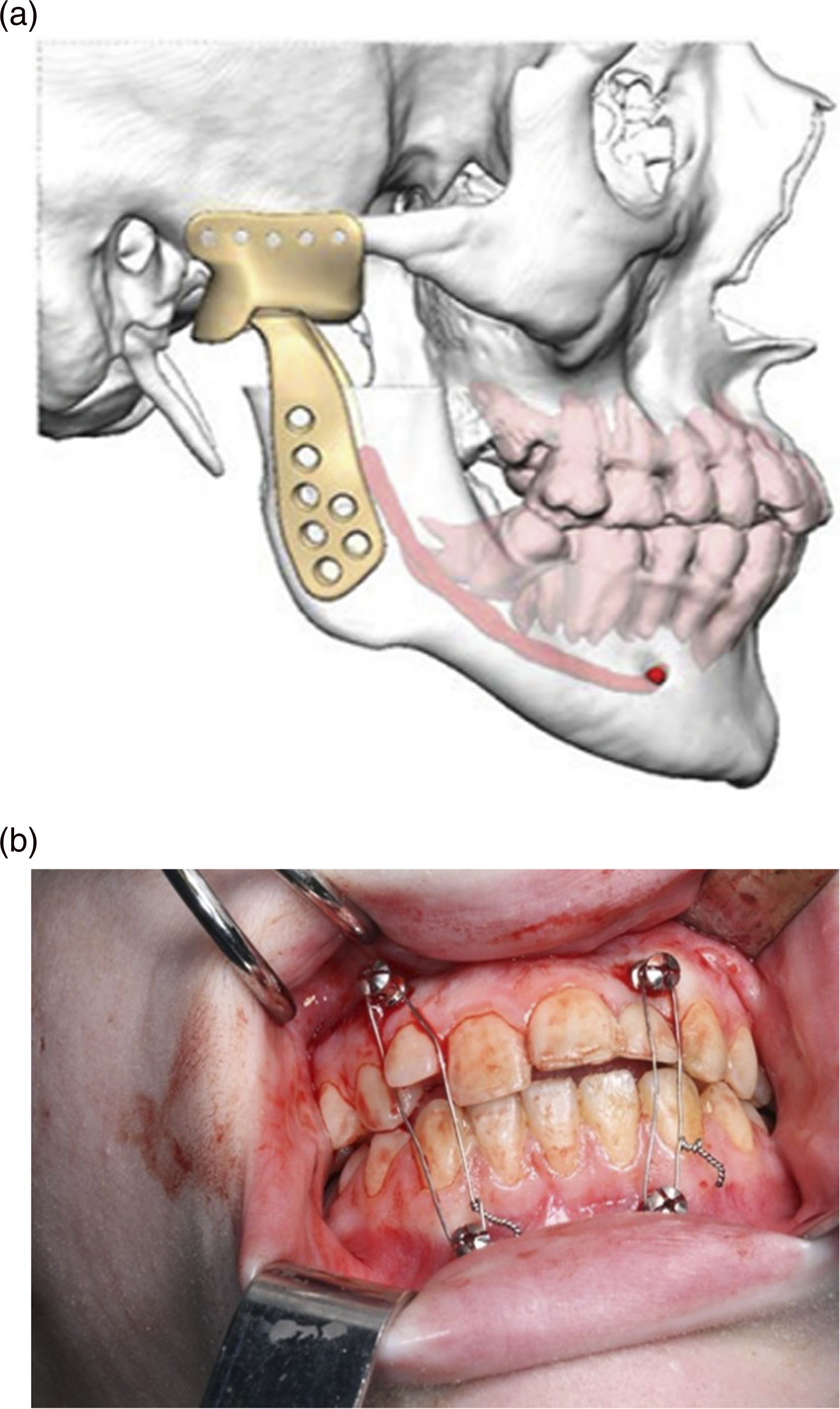
After placement of the TMJ prosthesis the IMF was released. The mobility of mandible, occlusion and mouth opening was checked. For the first time in 6 years the oral cavity could be inspected, and the perioperative mouth opening was 30 mm.
Closure was made in a subdermal multilayer fashion with resorbable sutures, and the skin was sutured with intracutaneous non-resorbable sutures.
Follow-Up
The patient underwent physical rehabilitation of the TMJ directly after surgery with the use of TheraBite Jaw Motion Rehabilitation System (Hörby, Sweden).
At the 5.5-year follow up after TJR, the mouth opening was 35 mm. The patient was free from pain. No signs of abnormal facial nerve function were seen, and the patient was satisfied with the performed surgery and felt improved quality of life. CT-images 5.5 year after surgery showed no signs of pathology or increased remodeling and bone formation (Fig. 6). Mouth opening 5.5 years after operation with 35 mm maximal opening. (a) Profile view, (b) Mouth opening measured from the anterior incisors, and (c) 3D CT-reconstruction of TMJ prosthesis 5.5 years after placement.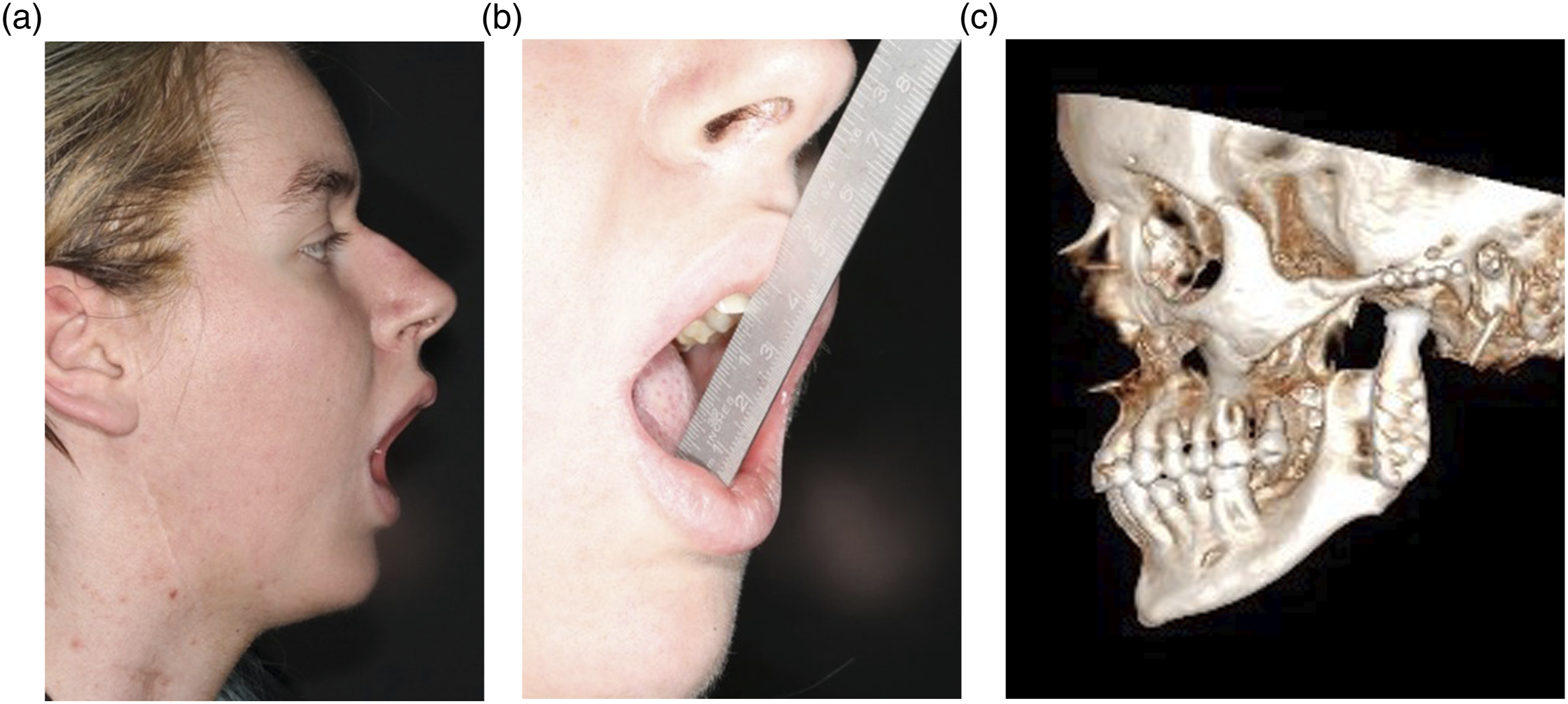
Discussion
We report of a case bilateral, long-standing bony TMJ-ankylosis, resolved by bilateral custom-made prostheses with a 5.5-year successful follow-up.
Coordination of care with other medical specialties especially anesthesiology, radiology and physiotherapy are of outmost importance in the management of individuals with TMJ ankylosis.
We consider the success of the suggested treatment protocol is largely dependent on the proper preoperative planning, experience of the surgeon, consideration of the facial nerve and on patient compliance. Rehabilitation (training for increasing range of motion) after surgery is very important factor for a positive treatment outcome. A complete understanding of the biomechanics and occlusal considerations during planning and surgery for the patient requiring total alloplastic joint reconstruction is necessary. Preoperative information on the restricted jaw function acquired with a prosthesis compared to the natural movement of the natural joint is crucial. An alloplastic joint as the ones installed in our case has the limitation of only offering a rotational pattern of the motion and no translational movement. It is important with frequent follow-up of the patients, and therefore requires active effort from the clinician’s center to monitor and encourage patients intensively.
Advantages of alloplastic joint replacement are immediate function, lack of donor site morbidity, reduced operative time and more predictable outcomes. A great advantage of alloplastic material over autogenous graft is the ability to start physical therapy immediately after the surgery. This reduces scar formation and allow for optimal range of motion. 12 However, when considering pediatric patients, the autogenous reconstruction has the additional advantage of growth potential, especially with costochondral grafts.13,14 Having that in mind, in pediatric patients with ankylosis, the growth has come to an end and thereafter alloplastic TJR may be advised. 15 Alloplastic TJR will not experience over or undergrowth or graft fracture. 12 It should also be considered that there is a physical and psychosocial benefit having a single rather than multiple operations. 12
Treatment of temporomandibular joint ankylosis with custom-made total joint prosthesis is a recommended treatment method in both children and adults with TMJ ankylosis unresponsive to other modalities of treatment, such as recurrent bony ankylosis, TMJ arthritis or failed tissue grafts. 16
Our patient showed normalization of mouth opening, increased quality of life and reduction in pain after surgery, this fact supports the evidence found in the literature that alloplastic TMJ reconstruction is an effective and safe, long-lasting management of patients with severe TMJ end-stage disease such as ankylosis.17,18
Conclusion
Ankylosis of the TMJ in young and adult population presents unique challenges given the need to account for growth of the mandible and anatomical variations. This report supports the use of total joint reconstruction for end-stage TMJ disease.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
IRB Statement
The Ethical Committee exempted the approval for this article, because it is a case series and the patients had signed the informed consent for the publication of their data.
Informed Consent
Written consent was obtained from the patient whose identifiable images were included in this study. Verbal consent was obtained from patients for the use of their deidentified case information.
