Abstract
Background
Routine removal of titanium miniplates in the maxillofacial region is still controversial. This current study hopes to share our experience with the different reasons for maxillofacial plates and screws removal following miniplate osteosynthesis.
Methods
This was a retrospective study of plates and screws removal following Open Reduction and Internal Fixation (ORIF) of maxillofacial fractures at King Khalid Hospital, Kingdom of Saudi Arabia, from 2005-2019. Information collected includes demographics, etiology and pattern of maxillofacial fractures, treatment modalities as well as reasons for plates and screws removal. Data was stored and analyzed using IBM SPSS Statistics for windows Version 25 (Armonk, NY: IBM Corp).
Results
A total of 985 patients with maxillofacial bone fractures had ORIF during the study period out of which 149 had miniplates and screws removed, giving a prevalence rate of 15.1%. There were 141 (94.6%) males and 8 (5.4%) females, with a M:F of 17.6:1. Their ages ranged from 4-65 years with mean (SD) at 24.6 (12.2) years. The age group from 16-30 years had the most cases of plates removal with statistical significance (P = .000). Young age (43 (28.8%)) constituted the majority of reasons responsible for plate removal. The angle of the mandible is the site with the largest number of plate removal with 34 (22.8%) cases followed by the parasymphyseal site with 21 (14.1%) cases.
Conclusion
With removal rate of 15.1%, this study concluded that there is no evidence to support routine removal of asymptomatic plates and screws in maxillofacial region.
Introduction
The use of miniplates and screws osteosynthesis has revolutionized the management of maxillofacial bone fractures and additionally, following orthognathic surgery.1,2 Since its introduction by Champy et al. 3 in the maxillofacial region, the materials for this hardware have also transformed from the bulky, less biocompatible stainless-steel or chrome-cobalt plates and screws to more thin, flexible, and biocompatible titanium and its alloy plates and screws. 1 Despite the fact that its use has been popularized, it is associated with complications such as metal toxicity and allergy, stress shielding, metallosis, migration, palpability, and thermal sensitivity. 4 Champy et al. 3 have recommended the removal of this hardware following the healing of the fractures; however no specific reason was given.
Controversy still exists among maxillofacial surgeons on the need for routine removal of asymptomatic plates and screws. 5 While some clinicians have recommended their routine removal following fracture healing, 6 others have opposed it unless they are associated with clinical symptoms.1,7
Based on the above, this current study hopes to share our experience on the different reasons for the removal of titanium plates and screws following maxillofacial bone fractures osteosynthesis in Najran region, southwestern province of the Kingdom of Saudi Arabia as no such study existed previously.
Materials and Methods
This was a retrospective study of plates and screws removal following open reduction and fixation (ORIF) of maxillofacial fractures in King Khalid Hospital, the main tertiary referral hospital in Najran Region, Kingdom of Saudi Arabia from 2005-2019.
Information collected includes demographics such as age and gender of patients, etiology and pattern of maxillofacial fracture, treatment modalities as well as reasons for plates and screws removal. All miniplates were 1.5 and 2 mm titanium plates.
Ethical clearance for the study was obtained from the Ethics and Research Committee of the Hospital with IRB number H-11-N-081. Inclusion criteria are cases of maxillofacial fractures treated with ORIF and those that had plates and screws removal. Exclusion criteria are such cases with incomplete records.
Data was stored and analyzed using IBM SPSS Statistics for windows Version 25 (Armonk, NY: IBM Corp). Results were presented as simple frequencies and descriptive statistics. Pearson Chi-square was used to compare variables. Statistical significance was set at P ≤ .05.
Results
Distribution of Reasons for Plate Removal According to Gender of Patients.
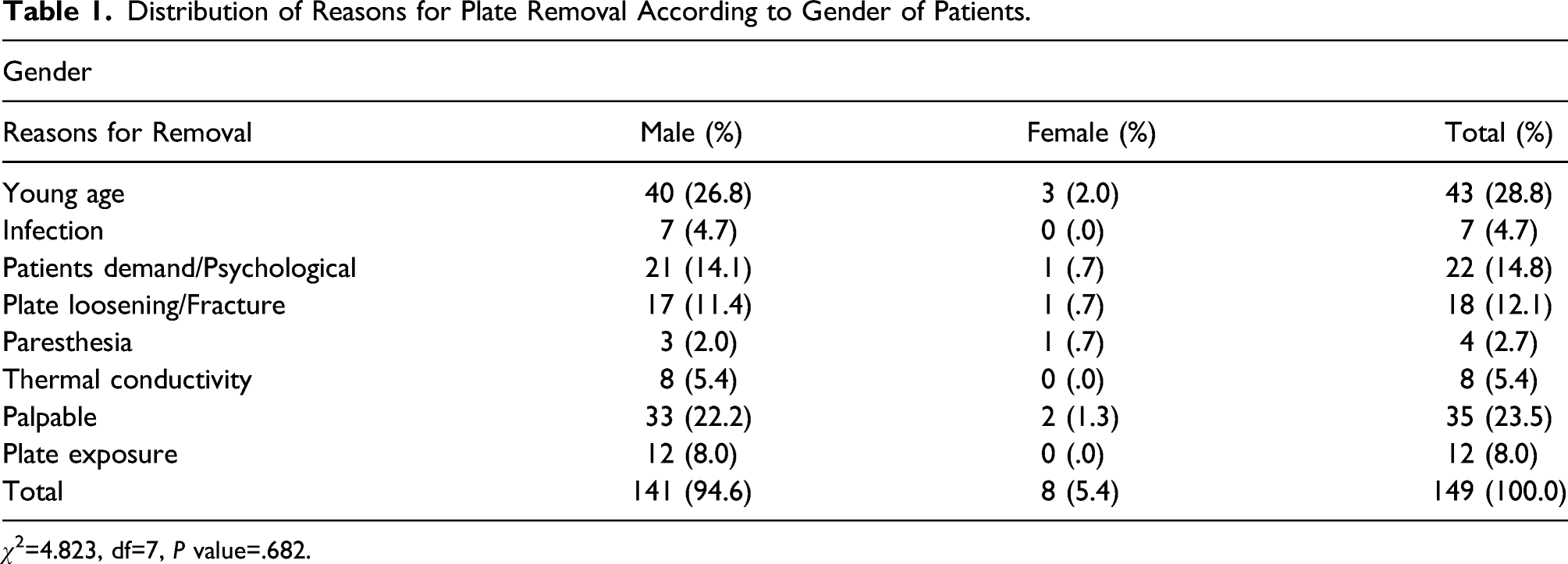
χ 2 =4.823, df=7, P value=.682.
Distribution of Age-Group of Patients According to Reasons for Plate Removal.
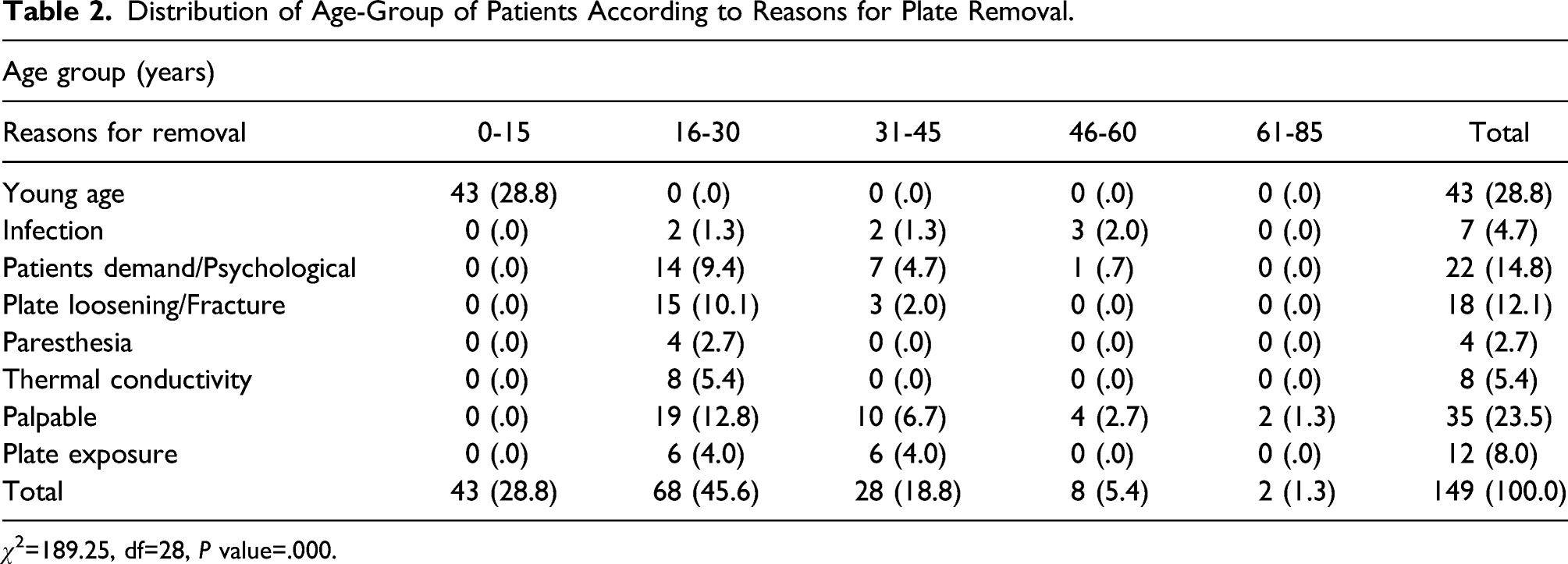
χ 2 =189.25, df=28, P value=.000.
Distribution of the Etiologies of Maxillofacial Bone Fracture.
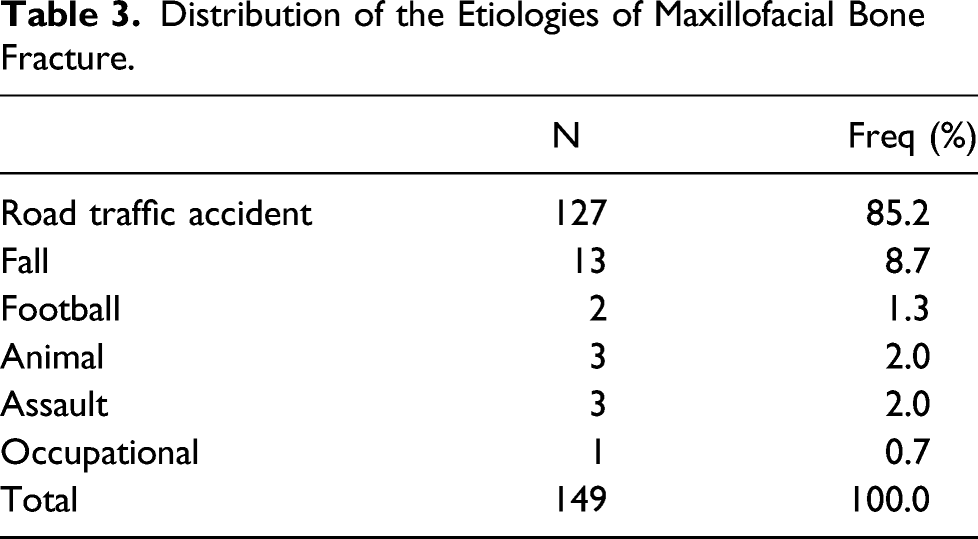
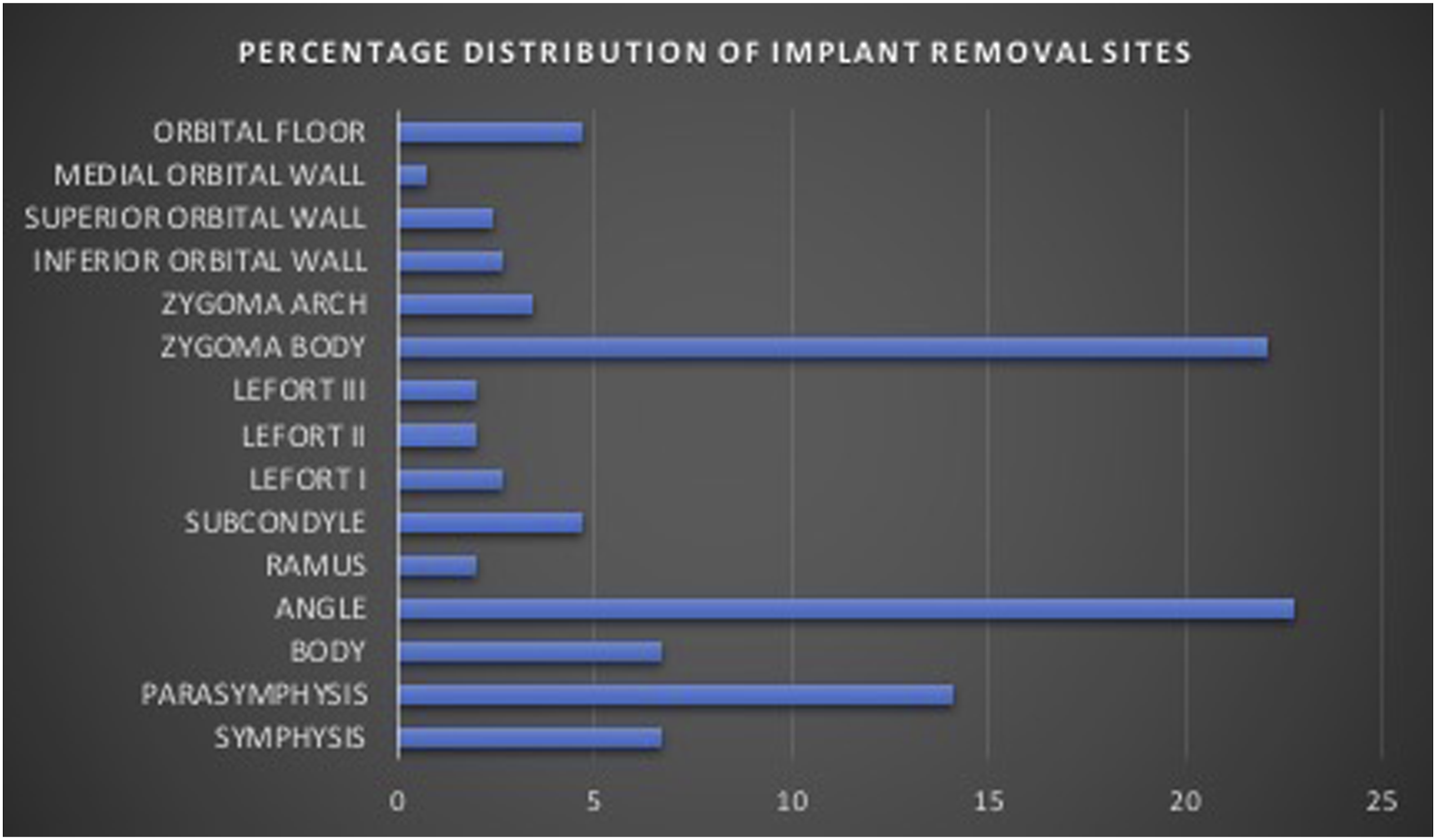
Out of 505 patients who had ORIF in the mandible, 85 (16.8%) had plates removed while in the zygoma, 38 (16.5%) out of 230 patients with ORIF had plates removed. Other distributions were as shown in Figure 1. The angle of the mandible constituted the site with the largest number of plate removal comprising of 34 (22.8%) cases followed by the parasymphyseal site with 21 (14.1%) plates removal. In the mid-face, zygomatic body and arch (zygomatic complex) had the highest rate of plate removal with 38 (25.5%) cases. In the orbit, inferior orbital rim had the highest rate of removal with 7 (4.7%) cases. Other distributions of plate removal according to site are as shown in Figure 2. Bar chart showing distributions of number of plates inserted and removed from maxillofacial bones. Bar chart showing distributions of plates removal sites from different maxillofacial bones.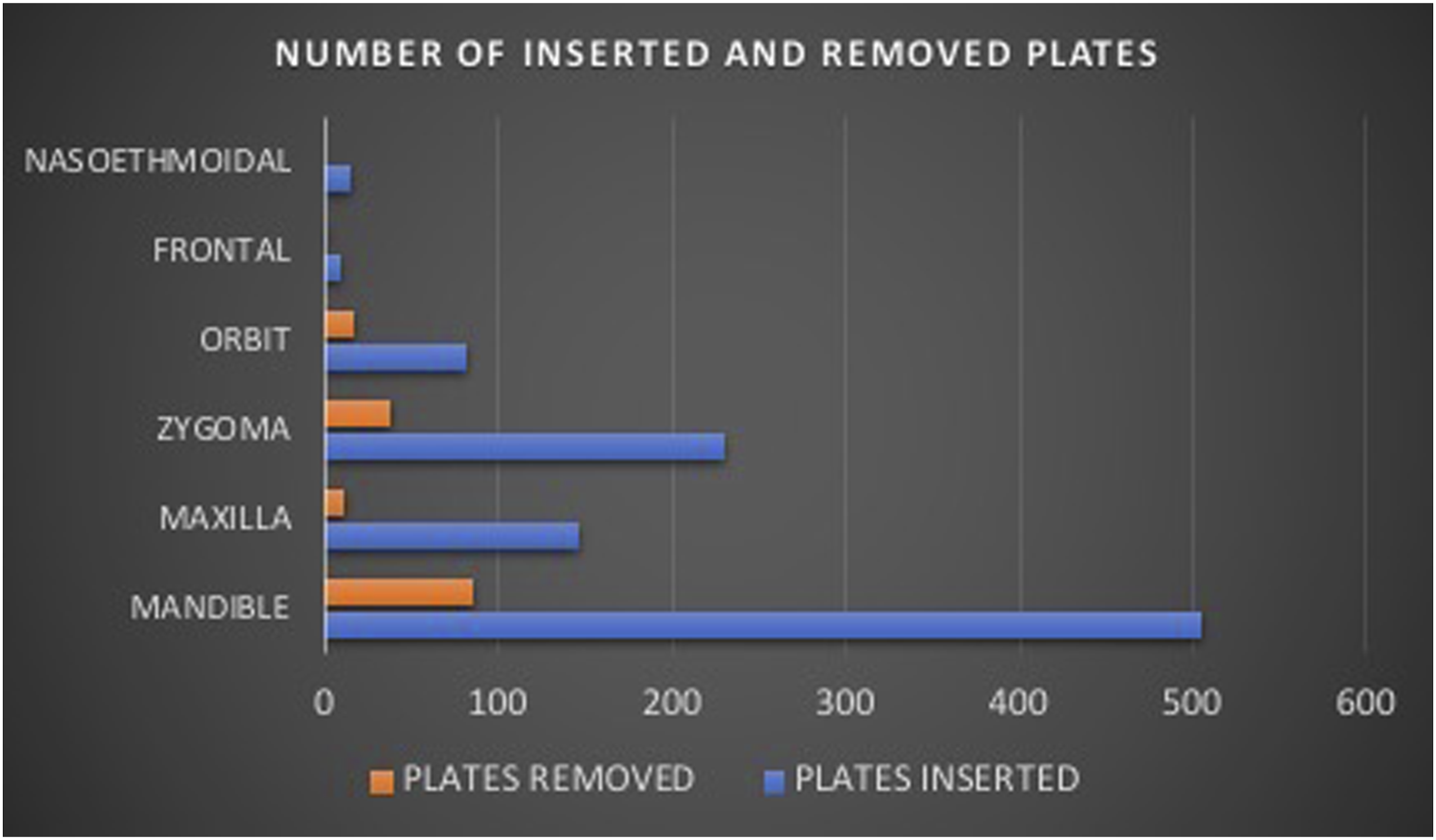
Discussion
This retrospective study reports the prevalence and motives for maxillofacial miniplates removal in 985 patients who sustained maxillofacial trauma and were treated with ORIF. During the 15-year period, 149 of the patients had plates removed, giving a prevalence rate of 15.1%. This is consistent with other documented studies in which 10-17% plate removal rate was reported.8-11.However, in a recent Korean study, a higher prevalence rate of 22.6% was reported. 4
Many recent studies have reported lack of evidence to support the routine removal of plates and screws after osteosynthesis in the maxillofacial region.4,8-11 However, older studies have recommended its routine removal because most of the plates used then were less bio-compatible.1,7 The current study have added to the literature on the lack of evidence to support routine removal of plates and screws following osteosynthesis in the maxillofacial region as no plate was removed routinely.
The postoperative timing for plate removal is controversial in the literature. Some studies have reported that plates should be removed within 6 months of insertion8,12 while others have favored removal within 1 year.1,13 In the current study, majority of the plate removal was carried out within the first year of osteosynthesis. Attempt at removal after 1 year may be difficult especially in adolescents where the plates would have been covered by bone.4,11
It is not surprising that most of the cases of plate removal occurred in the males and road traffic accident (RTA) remain the main etiological factor of the maxillofacial injuries. In our center, Daniels et al.14,15 have reported male predominance among the victims of maxillofacial injuries and RTA as the main etiology of these injuries because of the cultural background and socio-economic activities in Najran region of the Kingdom of Saudi Arabia.
Regarding age distribution, most of the patients who sustained facial bone fractures necessitating osteosynthesis were within the age range of 16-30 years and highest rate of removal was among patients aged 30 years or younger. This compares favorably with the study of Park et al,
4
however it differs from that of Rosenberg et al.
16
which reported higher rate of miniplates removal among patients in this age group. Concerning pediatric patients, researchers have recommended removal of miniplates within 2-3 months after fracture healing as a result of possible growth restriction.
12
In view of this, researchers have recommended the use resorbable plates and screws in the management of facial fractures in children.
5
However, insufficient stabilization has been reported with the use of resorbable plates especially at fractures sites involving the infraorbital rim and the zygomaticomaxillary crest/anterior sinus wall.
17
Because of this shortcoming, titanium plates have been recommended in these regions in the pediatric victims.
18
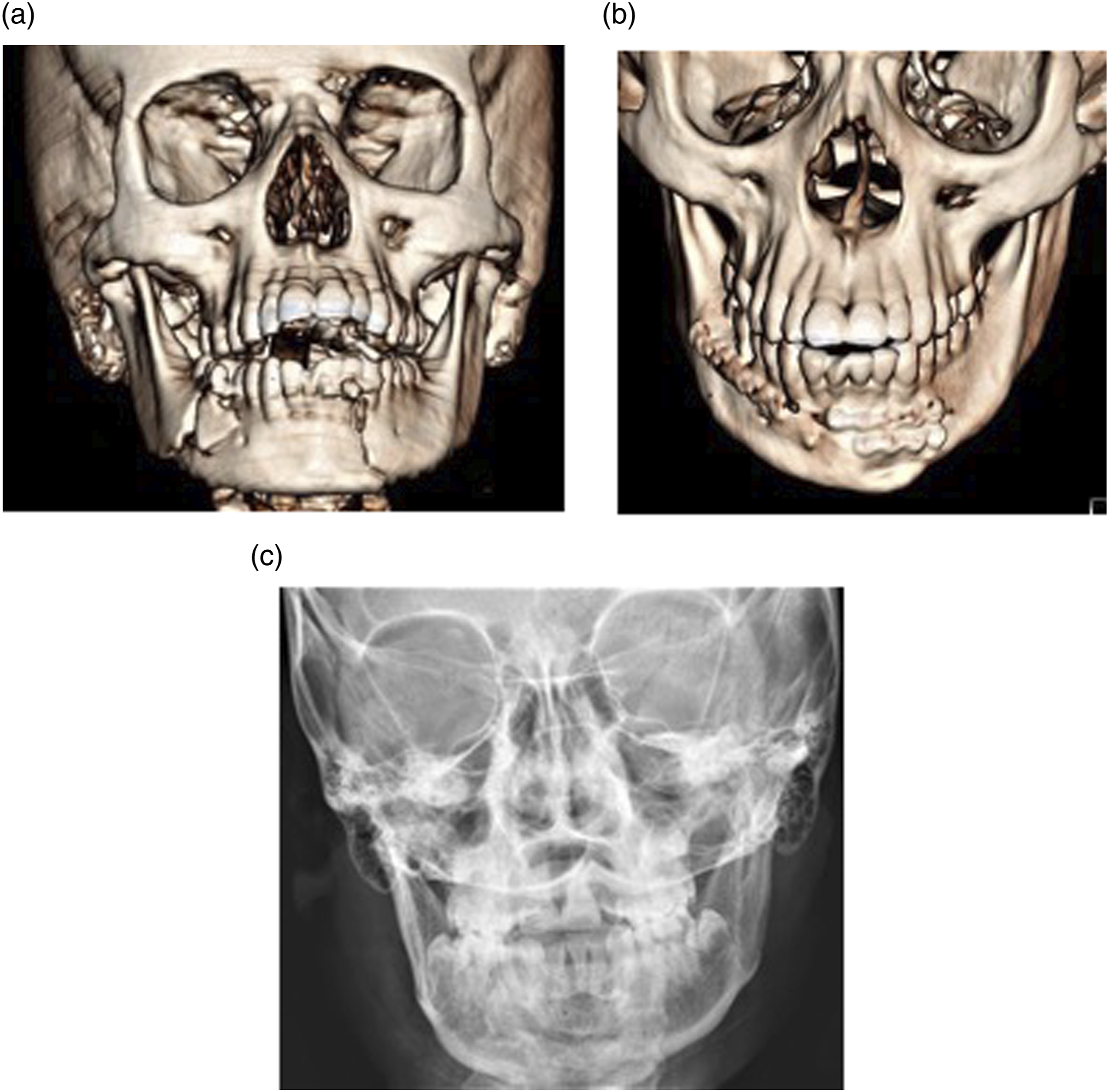
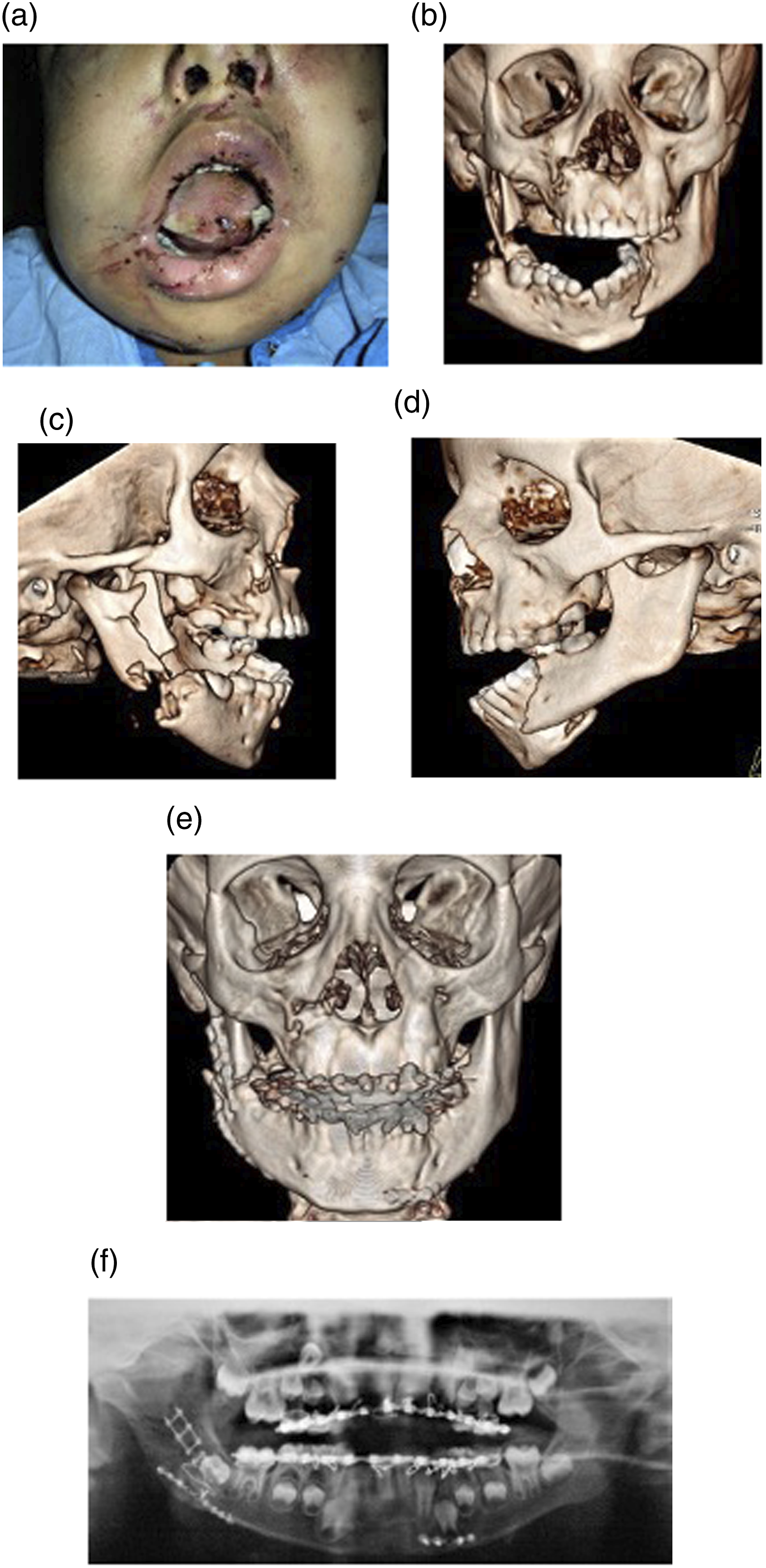
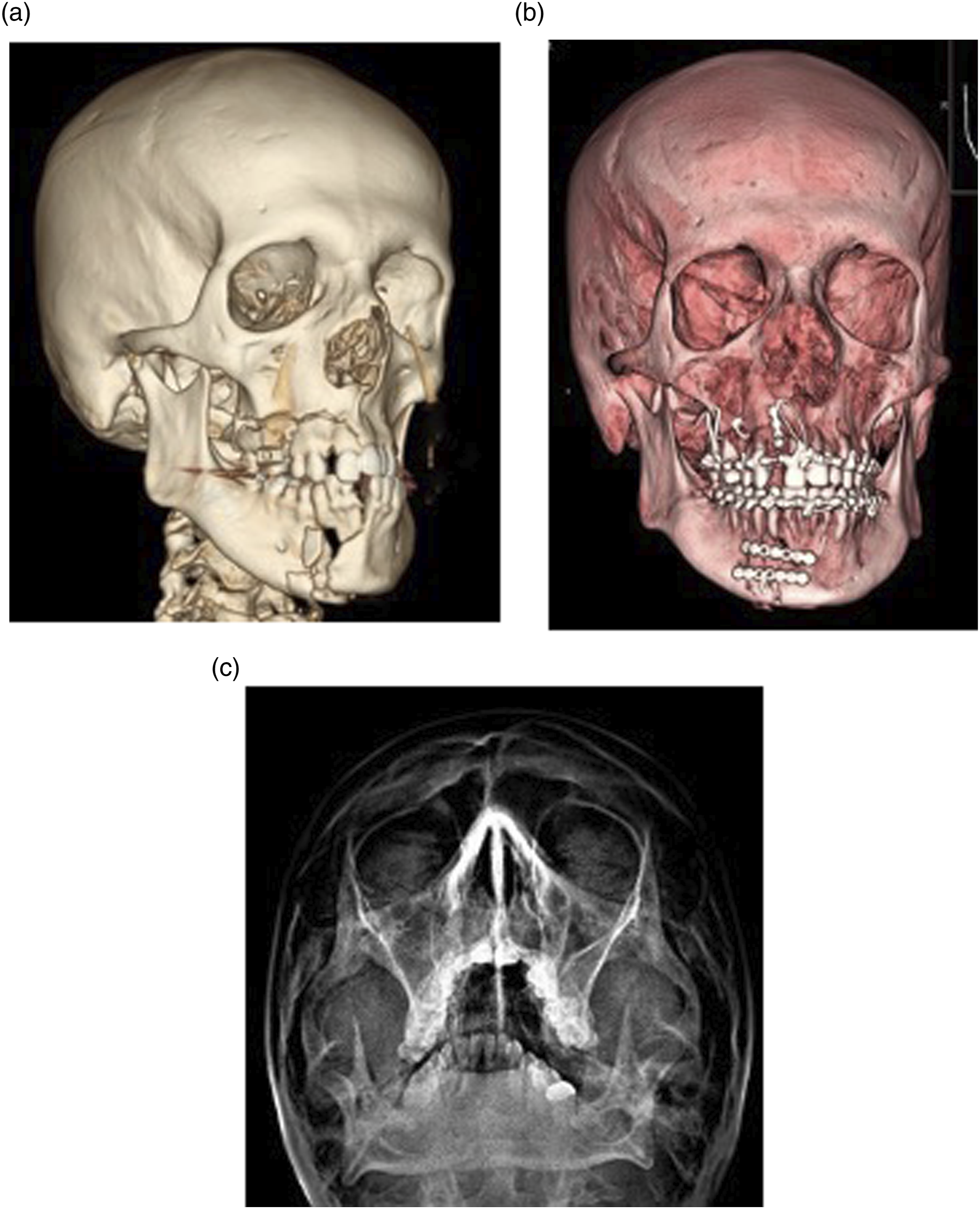
In our series, no resorbable plates and screws were used. Consequently, all our pediatric cases had removal of the titanium miniplates (Figures 3A-3C) and (Figures. 4A-4C). This constituted the highest reason of plate removal in our series. One pediatric patient who relocated to another country, had the plates removed after contacting our center on the brands of the plates and screws used (Figures 5A-5F).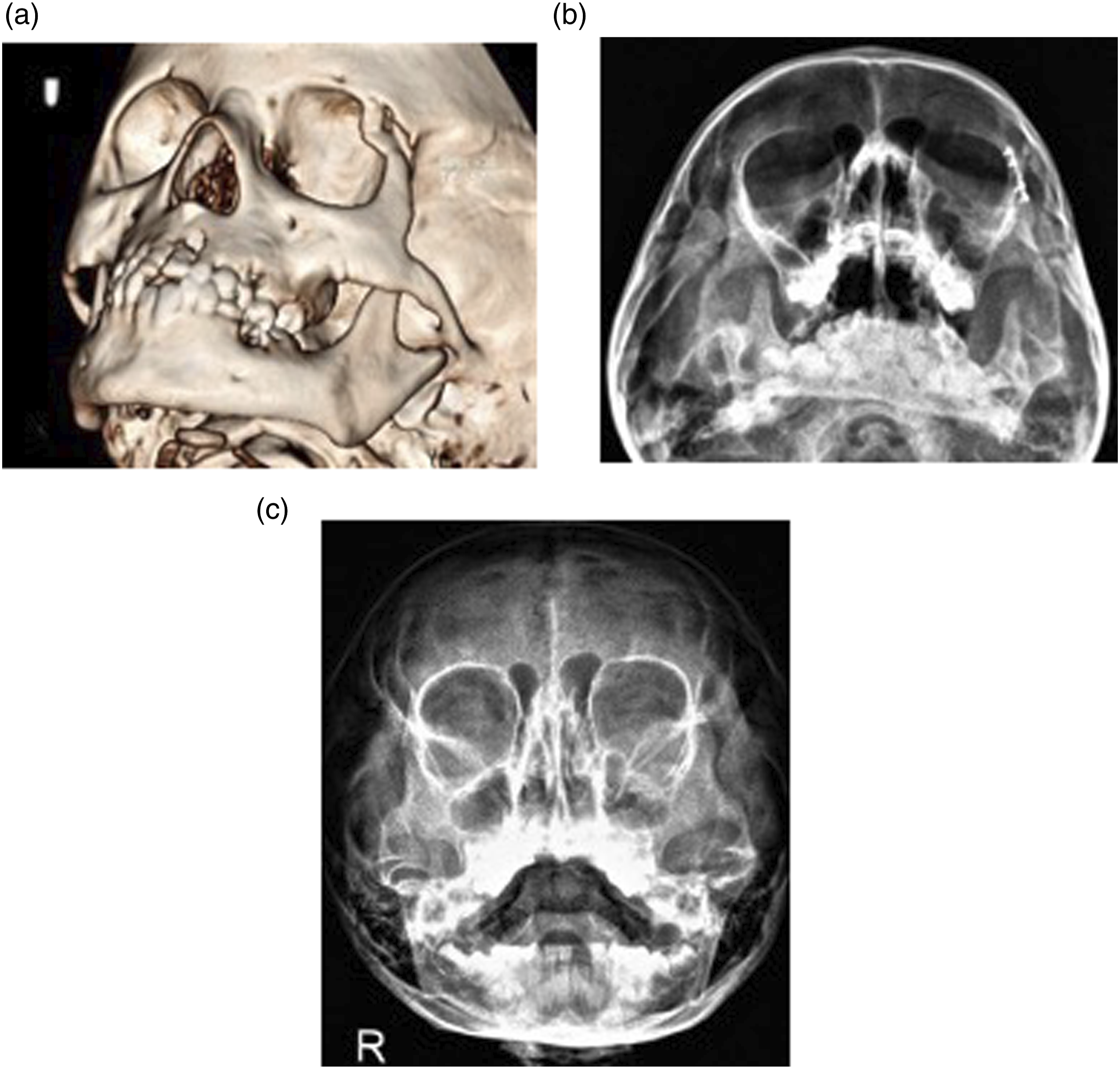
The second most common reasons for plate removal in the current study were palpable plates followed by patients’ request (Figures 6A-6C.) This agrees favorably with the study of Rallis et al.
11
Psychological factors may be responsible for this as palpable plates become a source of concern for the patients.
11
Infection, as reason for plate removal, was very low in our series with 7 (4.7%) cases as compared with other studies in which infection was the main reasons for their removal.1,8,11 Chronic smoking has been suggested as a risk factor for the development of superficial infections following ORIF of fractures.
5
Literature is silent on the association between rate of plate removal in healthy and immunocompromised patients. One study has eliminated this group of patients in order to remove confounding factors. 19 Majority of patients with facial trauma requiring osteosynthesis are young healthy folks, hence the possibility of the scarce literature on relationship between plates removal in the healthy and the immunocompromised. In the current study, none of our patients were immunocompromised necessitating plate removal. Two (1.3%) older patients in our study required plate removal because the plates and screws were palpable. Further studies regarding immunocompromised status and plate removal is essential.
Studies have shown that over 50% of plates inserted following maxillofacial bone fractures are placed in the mandible.
5
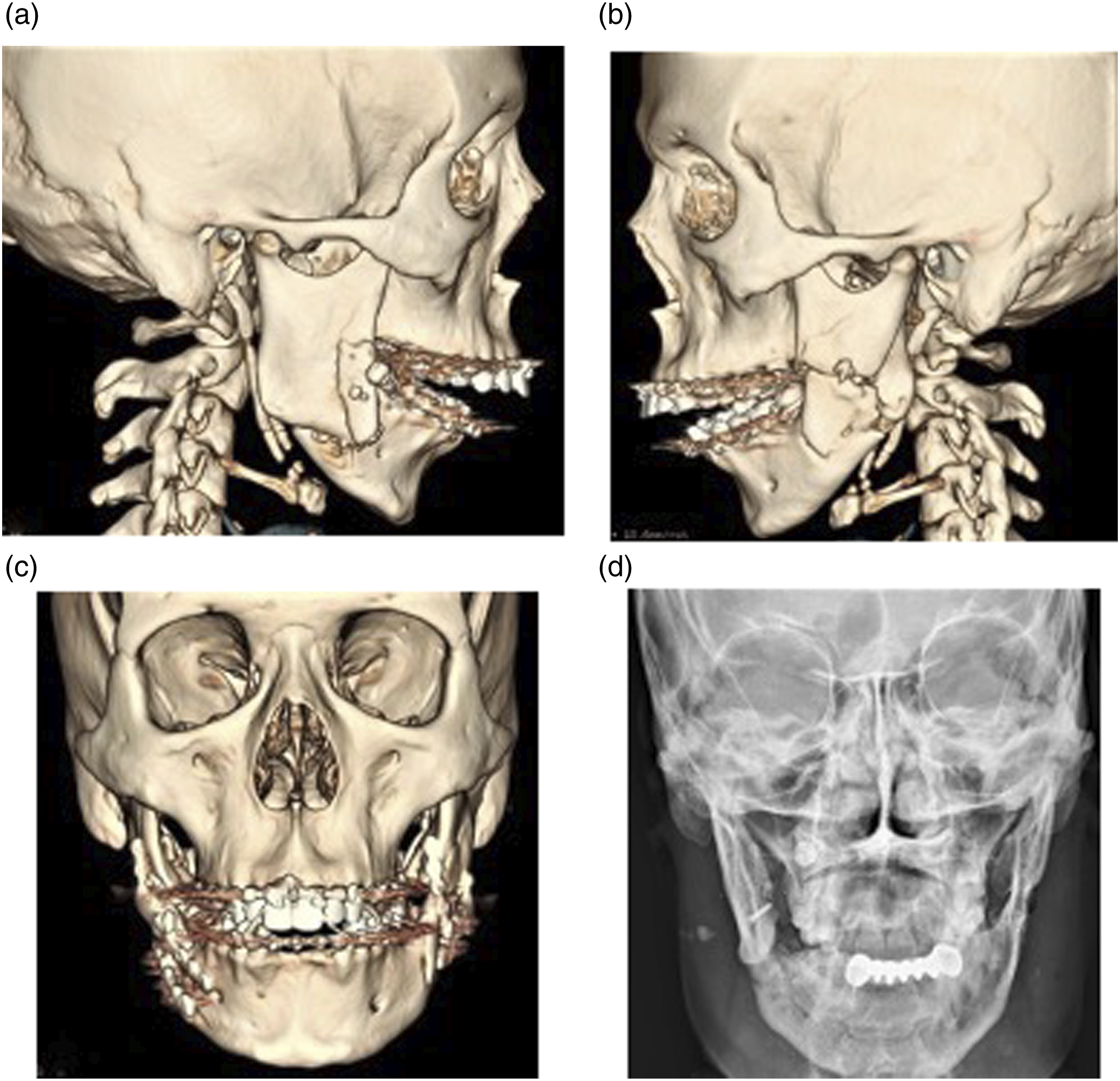
Therefore it is not surprising that in this study, 85 (57.1%) (n = 149) of plates removed were from the mandible with 34 (40%) (n =85) of these plates removed from the angle (Figures 7A-7D). Gabrielli et al.
20
have reported similar findings with most removal of plates from the angle of the mandible. During mastication, the biomechanical forces that occur at the angle region may have been responsible for higher incidence of complications.5,21 Yamamoto et al.
22
have recommended routine removal of plates and screws in the angle region because of this reason especially with presence of an impacted third molar. On the contrary, other studies reported that most cases of plate removal were from the parasymphyseal region.1,8 In this series, the frontal and NOE site did not record any plate removal while the maxilla has very low rate of plate removal. This observation has also been reported by Rallis et al.
11
Conclusion
As the controversy of whether to leave a non-functioning and asymptomatic plates in-situ persists, this retrospective study has reported a 15.1% removal rate over a period of 15 years. No asymptomatic plates and screws were removed routinely in the current study. Young age constitutes the main reason responsible for plate removal because of growth concern. The angle of the mandible is the site with the largest number of plate removal, while the maxilla, frontal, and NOE are of low risk for plates removal. This study concludes that there is no evidence to support routine removal of asymptomatic plates and screws in maxillofacial region.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
