Abstract
Le Fort fractures in pediatric patients are rare, and their management has increased complexity due to the development of the maxillofacial musculoskeletal complex and dentition. The authors present a case using historic circum-zygomatic wiring with 21st century surgical planning in a 18 month old, who sustained complex Le Fort II and III fractures. Treatment involved surgical planning with dental and stereolithographic models, and the fabrication of a retention modified, occlusal splint. Closed reduction with circum-zygomatic wiring retained by the occlusal splint, for a 3 week period, prior to removal. At 12 month review, the patient had good facial symmetry, cosmesis, profile, and function. The use of circum-zygomatic wiring provided a conservative operative approach, achieving excellent functional and cosmetic results without the potential morbidity of more invasive surgery.
Introduction
Complex facial fractures in the pediatric population, from 0 to 2 years, are rare, with an overall incidence of 0.87-1%, of which the majority occur in boys (91%). 1,2 Parental supervision along with retruded facial skeleton, elastic cancellous bone, increased adiposity, undeveloped paranasal sinuses and tooth germs, all reduce the incidence of pediatric facial fractures. 2 In contrast to facial fractures in adults, pediatric fractures present less predictability, with oblique and Greenstick fractures being more common, increasing their difficulty of diagnosis and management. 3,4 In patients less than 5 years of age, the most common mechanisms of facial fractures are falls (44%), motor vehicles incidents (25%) and interpersonal violence (25%), with variation due to social, cultural and environmental factors. 3,5
Pediatric patients diagnosed with facial fractures exhibit a higher injury severity, with midface fractures being associated with a depressed Glasgow Coma Score (GCS), intracranial hemorrhage, cervical spine injuries, longer length of hospitalization, longer time spent in an intensive care setting and commonly have concomitant injuries (58% of patients). 6,7 The most common concomitant injuries include dentoalveolar (47%), traumatic brain injury (11%) and lower and upper limb fractures (13% and 11%, respectively). 7
Operative management of pediatric facial fractures presents surgeons with challenges and increased risks including scarring, growth disturbance, facial asymmetry and iatrogenic injury. 8 For this reason, most maxillofacial departments have a high threshold to operate on such patients and the majority of patients (∼70%) are managed conservatively, however operative management increases with age, severity of fracture (Le Fort fractures, 81% surgically managed) and violence. 5,9 –12
Case Report
A healthy 18 month old female was struck by a reversing vehicle at low speed. Clinical examination and computer tomography identified injuries isolated to the maxillofacial complex, consisting of bilateral Le Fort II fracture, a right sided Le Fort III fracture, and palatal fracture (Figure 1, 2).
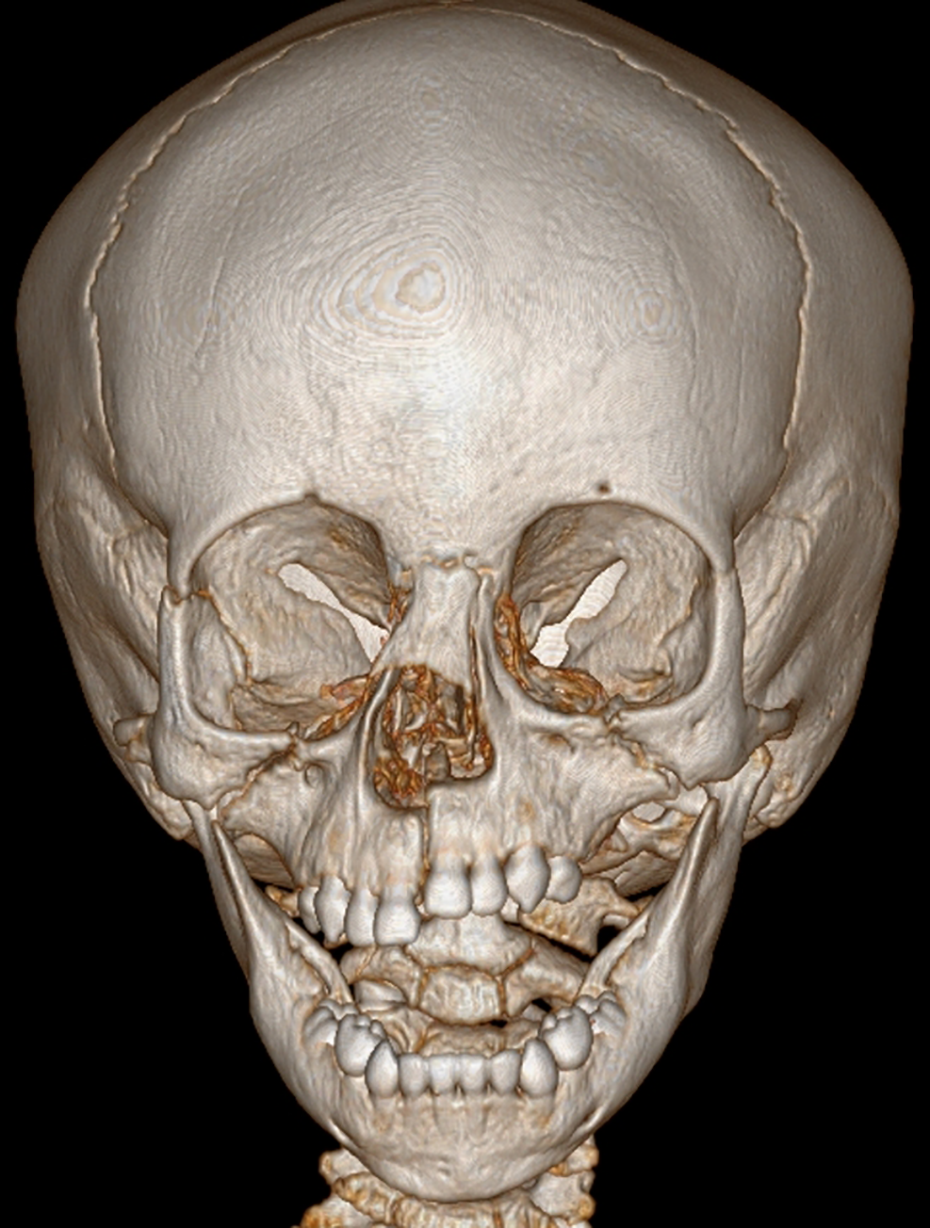
Pre-operative 3-dimensional reconstruction computer tomography imaging.
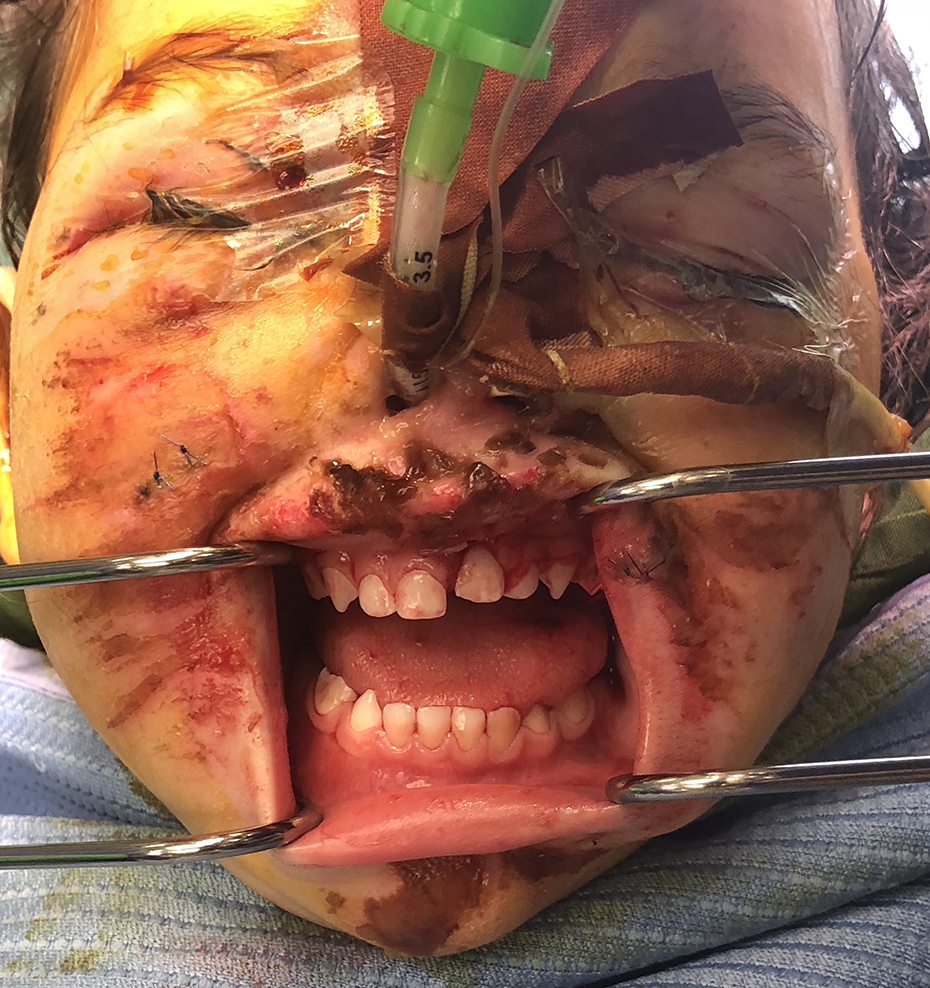
Perioperative clinical photograph complex mid-face fractures.
Indications for surgical management included unstable, displaced Le Fort fractures with facial asymmetry, and malocclusion. Management involved 3 general anesthetic procedures, over a 1 month period. Upon presentation, acute examination and treatment under general anesthesia enabled management of facial abrasions and lacerations, and allowed for treatment planning with dental impressions. Printed stereolithographic 3-dimensional biomodels, along with dental models allowed for the fabrication of a retention modified, occlusal splint.
On the following day circum-zygomatic closed reduction was achieved via an incision at the maxillary sulcus of the first deciduous molar with a Kohler Obwegser Awl, guiding a 0.5 g stainless steel wire medial to the zygomaticomaxillary buttress with perforation transcutaenously posteriorly and laterally to the lateral canthus. The Awl was then re-inserted within the first exit point, and guided circum-zygomatically laterally to the zygomatic buttress/ arch and out into the oral cavity. The operator must ensure the awl is re-inserted transcutaneously within the first exit point to prevent soft tissue entrapment. The wire placement was completed bilaterally, and used to provide retention to the modified occlusal splint for 3 weeks, prior to removal (Figure 3, 4). The occlusal splint retained by circum-zygomatic wiring provided stable vertical, transverse and sagittal correction of facial symmetry and function with minimal manipulation and surgical access. Furthermore it did not further inhibit the patients nutrition or their airway, and allowed for oral hygiene to be conducted. At 12 month review the patient had good facial symmetry, cosmesis, profile, and function (Figure 5). Postoperative radiography was not taken to reduce the patient’s radiation exposure.
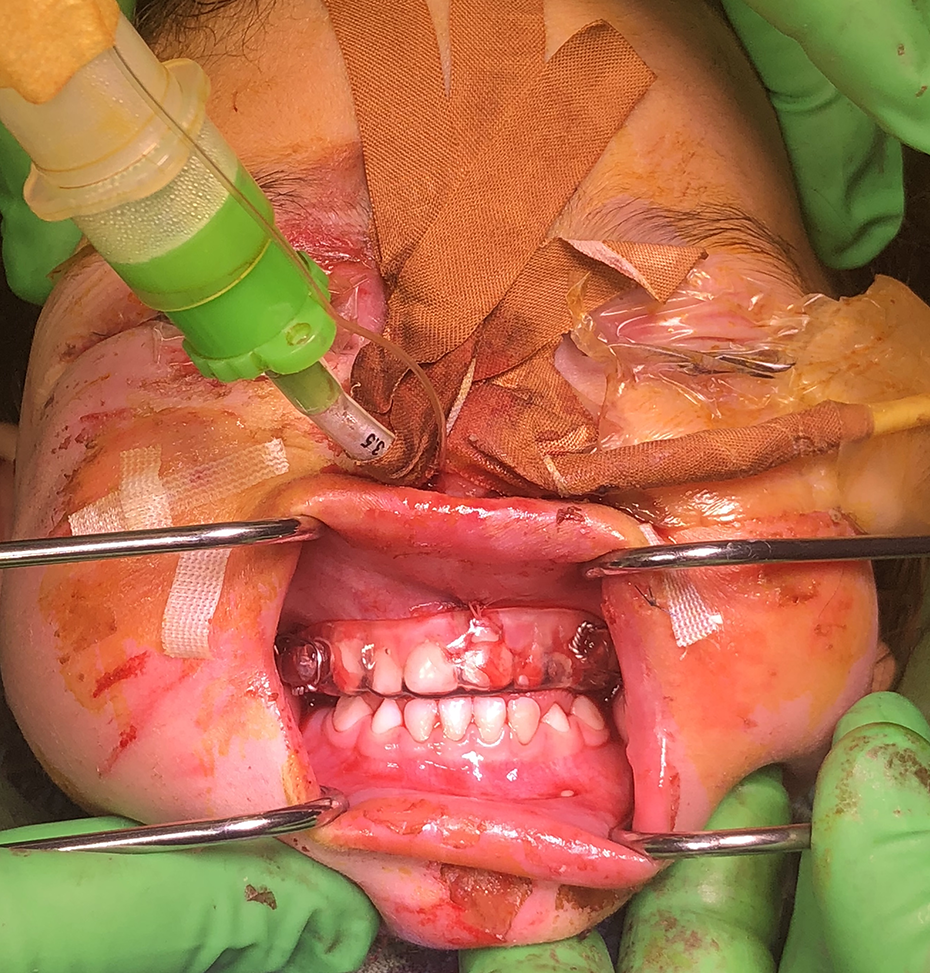
Perioperative clinical photograph trans maxillo-zygomatic buttress wiring retained by retention modified occlusal splint.
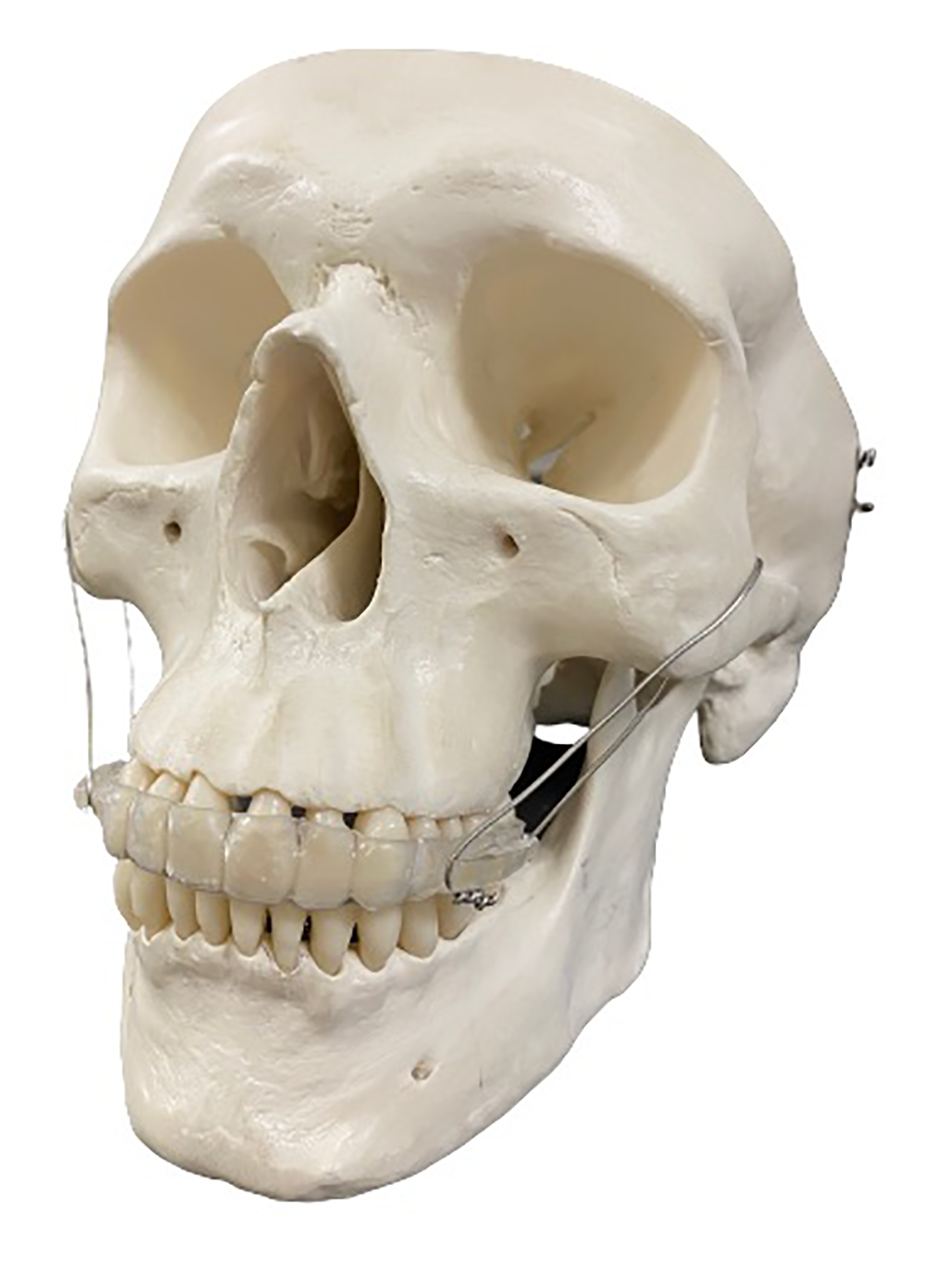
Circum-zygomatic wiring model.
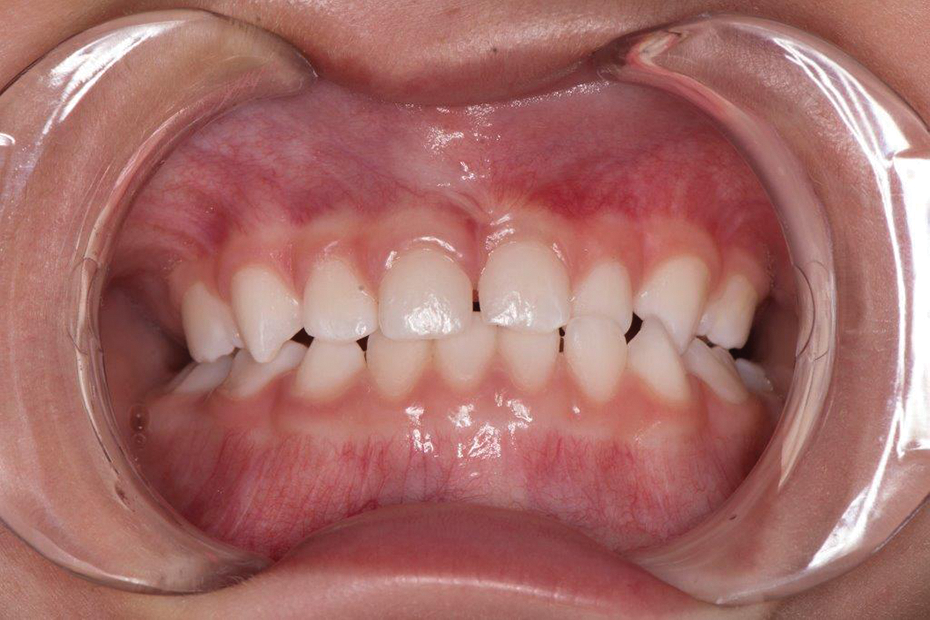
Clinical photograph 6 month post treatment.
Discussion
Pediatric craniofacial structures and fractures, along with their management, are different to adults, due to their differences in the topography of the craniofacial skeleton, osteogenic potential and growth. 5 In adults, complex displaced facial fractures are commonly managed by performing open reduction, internal fixation with or without intermaxillary fixation. 13 In pediatric patients open reduction, internal fixation risks traumatic periosteal elevation, iatrogenic injury to dental elements and developing tooth buds, growth disturbances, scarring, plate migration or exposure and revision procedures. 8 However resorbable plating systems have been developed to provide temporary stabilization of the bony fracture without the need for a second surgery for plate removal. 5 Intermaxillary fixation, to control the dental occlusion and associated fractures, is poorly tolerated in the primary or mixed dentition, as it has the potential for tooth avulsion, inadequate retention due to conical shaped teeth and dental spacing, and a non-reproducible occlusion due to less or partially erupted teeth. 14 Circum-zygomatic closed reduction provides a conservative alternative to traditional surgical management reducing the potential perioperative issues, with adequate patient tolerance and compliance. 14
Unlike in adults, early anatomical reduction with short periods of fixation is not always required in pediatric patients with facial fractures, due to their osteogenic potential. 14 Children’s more prominent periosteum provides increased vasculature, oxygenation and nutrition to osteochondroprogenitor cells, increasing bony union and remodeling potential. 15 Increased remodeling may correct for anatomic and functional discrepancies in closed reduction of midface fracture along with growth and development, and tooth exfoliation. 2 Due to the greater osteogenic potential and remodeling, pediatric patients are less likely to develop malunion, non-union, malocclusion, or postoperative infections. 16 However, in cases where complex fractures are displaced and grossly mobile with malocclusion and orbital dystopia, a non-operative approach is not possible. In such cases, a minimally invasive approach allows reduction and stabilization of fractures while utilizing the osteogenic potential to optimize healing.
Long term follow up of pediatric patients with facial fractures is imperative to ensure adequate aesthetics and functional outcomes. Davidson et al 10 demonstrated that severe midfacial trauma in pediatric patients results in clinically significant discrepancies in growth in 86%. Trauma to sutures, synchondrosis and interruption of apposition-resorption in pediatric patient can disrupt midface development. 17 Patients with facial fractures in their first decade of life, involving multiple buttresses or with bone loss, and those with more extensive and numerous surgical interventions have the most severe growth disruption. Furthermore pediatric patients with Le Fort pattern fractures have a higher frequency of post-traumatic complications (60%) including enophthalmos, vertical dystopia, telecanthus, midface hypoplasia and malocclusion. 11
Conclusion
Management of complex midface fractures in pediatric patients has multiple considerations. Comprehensive knowledge of growth and development is required for diagnosis and management of pediatric facial fractures. Circum-zygomatic closed reduction with retention modified occlusal splinting allows osteosynthesis and can provide anatomical reduction of facial fractures, restore facial symmetry, cosmesis, and function. This technique should be considered as an alternative to open reduction internal fixation of displaced complex midface fractures in the pediatric population.
Footnotes
Authors’ Note
Mr Angus Colquhoun, Oral and Maxillofacial Surgeon, Waikato District Health Board as the operating surgeon. Michael Williams & Mustafa Mustafa Oral and Maxillofacial Technician’s, Waikato District Health Board for preparation of 3D stereolithic models, primary casts, and fabrication of retention modified acrylic splint.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval/Patient Consent
Ethics approval was not required. Written informed consent was obtained and is available upon request. No identifying information is within the report.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
