Abstract
Facial injury as a result of an industrial accident from a stationary saw is rather uncommon; however, such an injury can result in significant damage to vital structures in the maxillofacial region and can even be life-threatening. Expeditious and prompt treatment at the time of such penetrating facial injury results in a favorable outcome. Appropriate care and proper treatment of a patient with penetrating facial injury includes immediate clinical assessment, diagnostic imaging, early wound exploration, removal of the foreign body, wound debridement, repair of hard and soft tissue, and adjunctive antimicrobial therapy.
Keywords
Introduction
Penetrating facial injury can be life-threatening and often necessitates emergency management. Table saws are popular industrial tools that are frequently used at home or at work to cut wood. Many of the injuries related to stationary saws involve hands and fingers. Although facial injury as a result of table saws is rare, on occasion, a wooden object can kickback out of the saw causing a projectile and can result in significant damage to the maxillofacial structures of the operator. 1
Management of maxillofacial injuries as it relates to battlefield trauma from high-velocity/high-energy projectiles has been examined extensively in the literature; however, less attention has been given to injuries secondary to lower velocity projectiles in the civilian industrial setting. 2 –4 Initial management of a patient with a penetrating facial injury can lead to challenging problems and requires a comprehensive and multidisciplinary approach. 5 When faced with a large foreign body in the maxillofacial region lifesaving and resuscitative efforts must immediately commence. The airway and breathing must be immediately stabilized. 6 It is also critical to leave the impacted object in place, while controlling ongoing hemorrhage by application of direct pressure and packing of the wound. 7,8 Many times extraneous objects tamponade vascular structures and should be removed in the controlled setting of an operating room.
Maxillofacial impalement can be life-threatening and may be associated with other significant bodily injuries. Due to the presence of vital structures in the maxillofacial region, penetrating trauma can result in neurological, ophthalmic, vascular, oropharyngeal, and skeletal complications. 8,9 Prompt implementation of Advanced Trauma Life Support (ATLS) protocol, stabilization of the patient, appropriate imaging, and early intervention can significantly reduce morbidity and mortality. 6,8,10
The head and neck contains numerous vital structures and managing a penetrating injury to this region requires a selective trauma management protocol with examination and inquiry based on the patient’s symptoms. 11 Modern-day management of penetrating maxillofacial injury has evolved from delayed operative repair to an early, more aggressive operative management. In management of penetrating maxillofacial injury, early wound exploration, removal of the foreign object, proper debridement, anatomic fixation of bone segments and repair of soft tissue, and appropriate antimicrobial coverage will result in a more favorable clinical outcome. 12
Report of a Case
A 49-year-old male with history of hyperlipidemia, diverticulitis, and allergic rhinitis was working as a carpenter when a large plank of wood was ejected from a stationary saw and pierced his left cheek. After stabilization in the field by Emergency Medical Services, the patient was brought to the Emergency Department at the Elmhurst Hospital Center. Clinical examination revealed a large plank of wood emerging from the left cheek area resulting in a complex facial laceration (Figure 1A and B). There was no evidence of active hemorrhage. The patient was alert and oriented to person, place, and time with stable laboratory results and vital signs (Glasgow Coma Scale 15). The patient had not experienced loss of consciousness, however, he had noted copious hemorrhage from his nose and mouth at the time of injury. The patient also had anesthesia along the maxillary division of left trigeminal nerve (V2) distribution.
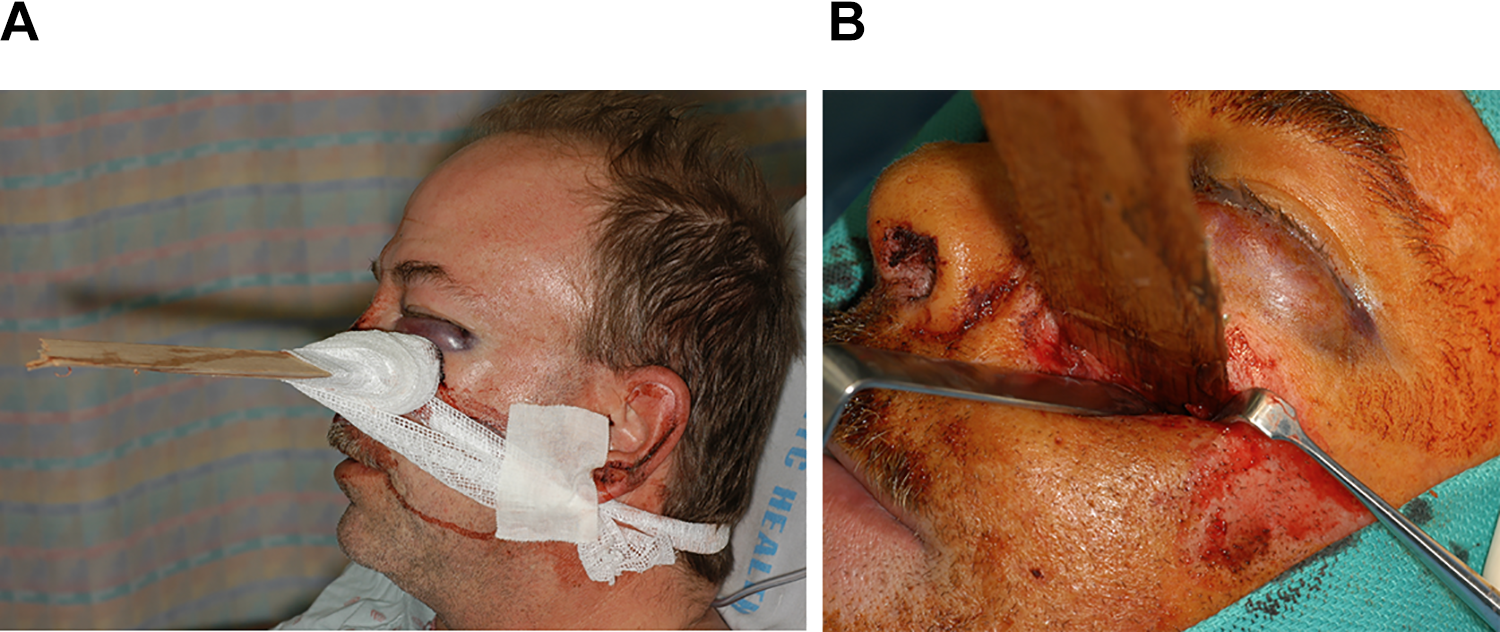
A and B, Left cheek foreign body and wound.
The patient was stabilized by implementing ATLS guidelines and following traditional sequence of trauma protocol. A computed tomography (CT) scan of the head and neck was performed to further evaluate the extent of the injury to adjacent maxillofacial structures (Figure 2A to D). CT demonstrated that the patient had zygomatic, maxillary, inferior orbital rim and septal bone fractures. There was no evidence of orbital or cranial penetration. CT angiogram was also obtained and did not demonstrate any contrast extravasation suggestive of vascular injury.
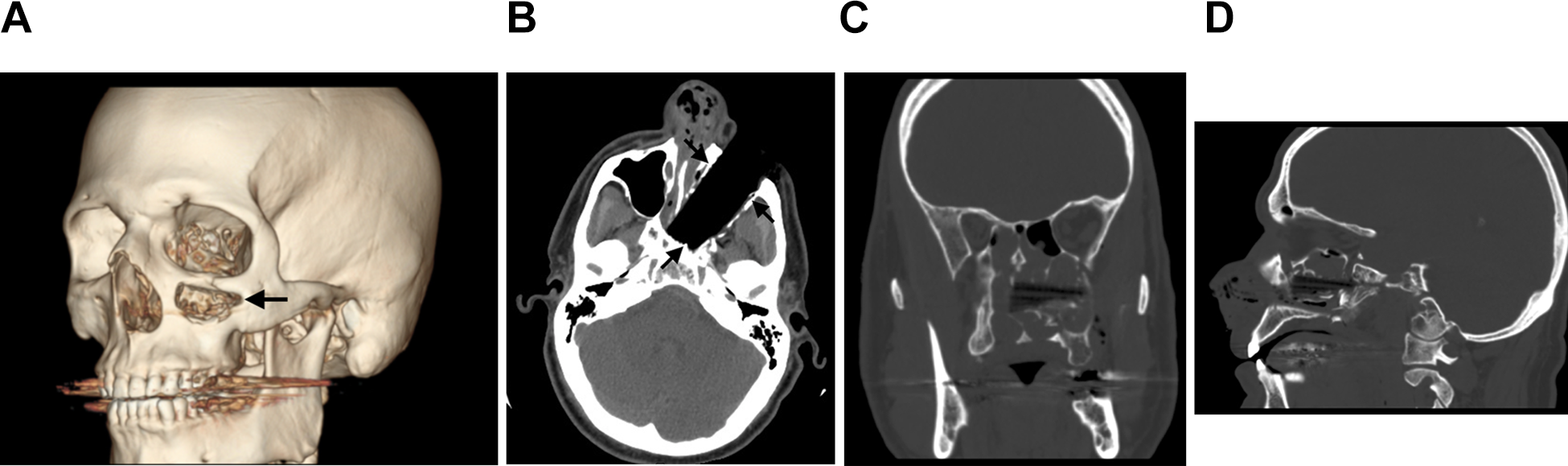
A to D, Computerized axial tomography scan showing the extent of the maxillofacial injury along with position and depth of the foreign body penetration (black arrows).
The patient was taken to the operating room for removal of the foreign object and repair of broken facial bones. Under general anesthesia, the margins of the laceration were retracted and the foreign body was visualized in all directions. While maintaining head and neck stabilization, the foreign body was manually luxated. With deliberate and controlled force the foreign body was removed from the left cheek area (Figure 3). After removal of the foreign body, the extent of the injury was visible (Figure 4). There were multiple fractured bone segments and wood splinters in the wound as a result of the sustained trauma. There was significant comminution of the left lateral maxillary sinus wall, medial maxillary sinus wall, associated zygomatic bone, and inferior orbital rim on the left side. The nasal septum was also fractured. All the loose fractured bone fragments and visible wood splinters were removed from the left cheek wound and maxillary sinus region. There was no herniation of orbital contents into the maxillary sinus. The bony fragments were repositioned anatomically and were fixated using plates and screws (Figure 5A and B). The left infraorbital nerve (ION) was found to be transected at the infraorbital rim area (Figure 6). After reduction and fixation of the fractured segments, epineurial repair of the left ION was performed. The main stump of the left ION was carefully prepared using a surgical blade. The labial and lateral nasal branches were also identified from the caudal aspect of the soft tissue flap and prepared using a surgical blade. The transected nerve endings were coapted. Tension-free neurorrhaphy of the ION was performed utilizing a 7-0 Prolene suture in an interrupted fashion (Figure 7). Due to significant comminution of the maxillary bone, there was still a notable defect in the left lateral sinus wall. The remaining anterior maxillary wall defect was covered with a titanium mesh to provide further support for the soft and hard tissue in this area of defect (Figure 8). Care was taken to prevent compression of the repaired nerve stumps. Following completion of the reconstruction of the bony elements, attention was given toward repair of the soft tissue defect. The laceration measured approximately 4 cm in length and had a hockey-stick configuration. The wound was copiously irrigated and debrided and necrotic wound edges were resected. The muscular aponeurotic layer of the left cheek area was first resuspended utilizing multiple 4-0 Vicryl sutures in interrupted fashion. Layered closure of the wound was accomplished. Following closure of the skin, attention was directed to reduction of the nasal septum. A Goldman elevator was gently inserted into the nose and the fractured septum was medialized over the nasal crest of the maxilla bilaterally. The patency of the airway was confirmed by the passive introduction of the Goldman elevator on each side of the nasal airway. Following completion of the reduction of nasal septum, 2 Merocel packings soaked in Bacitracin were inserted into the nasal cavities in order to prevent hematoma formation. Surgical site hemostasis was confirmed (Figure 9). The patient had a satisfactory emergence from anesthesia.

Retained wooden projectile which had resulted in facial laceration and maxillary bone comminution.
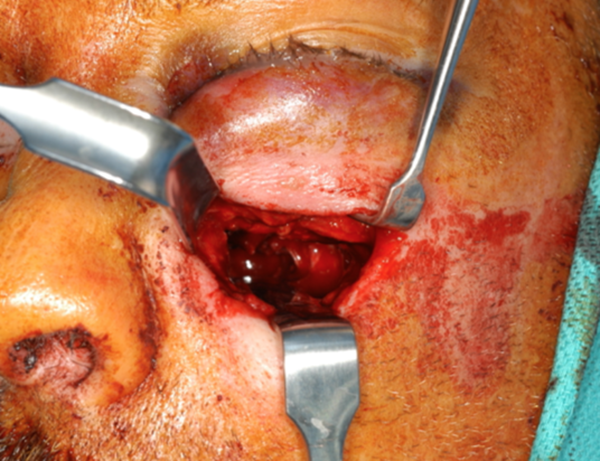
Following removal of the foreign body the extent of the injury was visible.
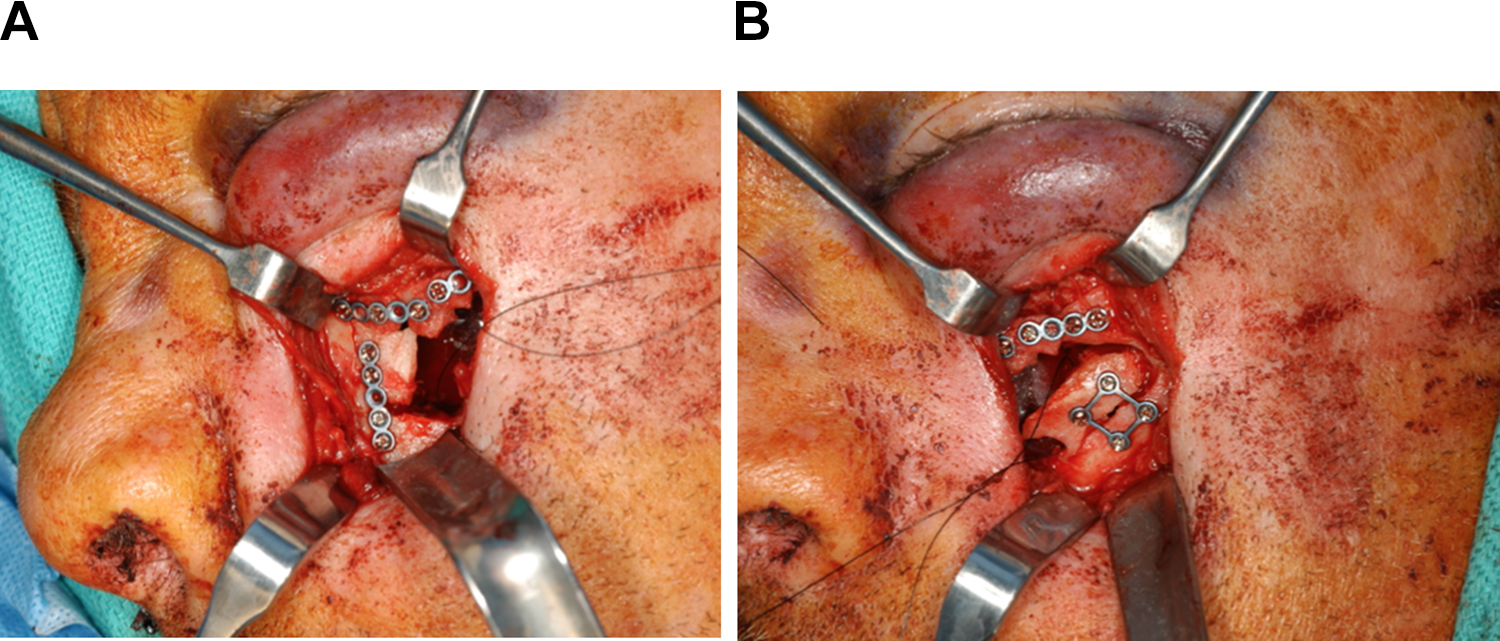
A and B, The fracture repair of comminuted maxillary and orbital bone.
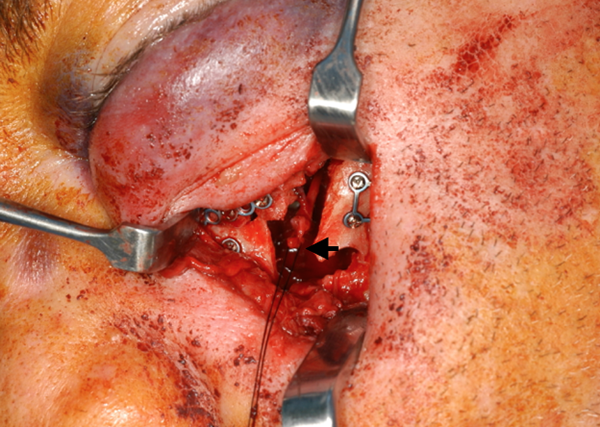
The transected end of the main trunk of ION (black arrow) was identified. ION indicates infraorbital nerve.
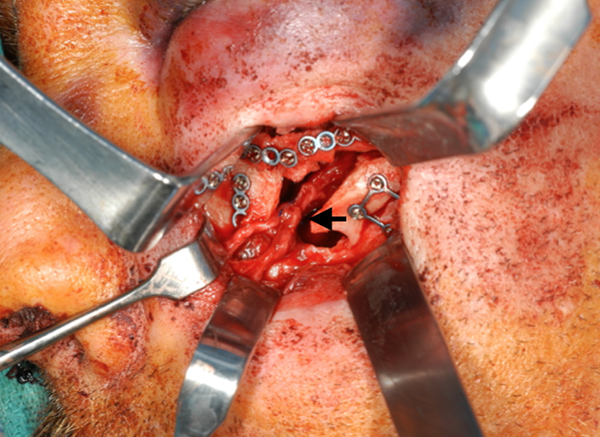
Tension-free neurorrhaphy of the ION (black arrow) with 7-0 Prolene sutures. ION indicates infraorbital nerve.
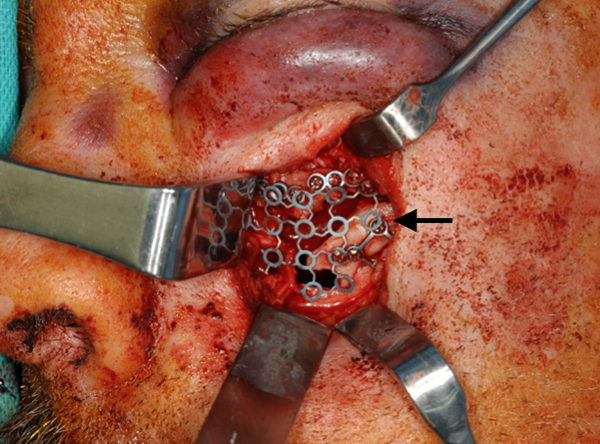
The maxillary wall defect was covered with a titanium mesh (black arrow) to provide further support for the soft and hard tissue.
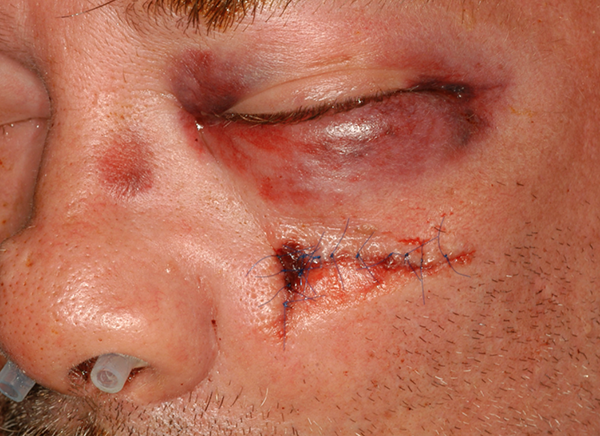
Final repair of facial laceration with nasal packings in place.
On follow-up exams, the patient had significant improvement in neurosensory function along the left ION distribution. However, the patient had decreased sensation along the left upper lip region. Otherwise, the patient’s postoperative course was uneventful and the facial wound healed well without objectionable scarring or deformity (Figures 10 and 11).
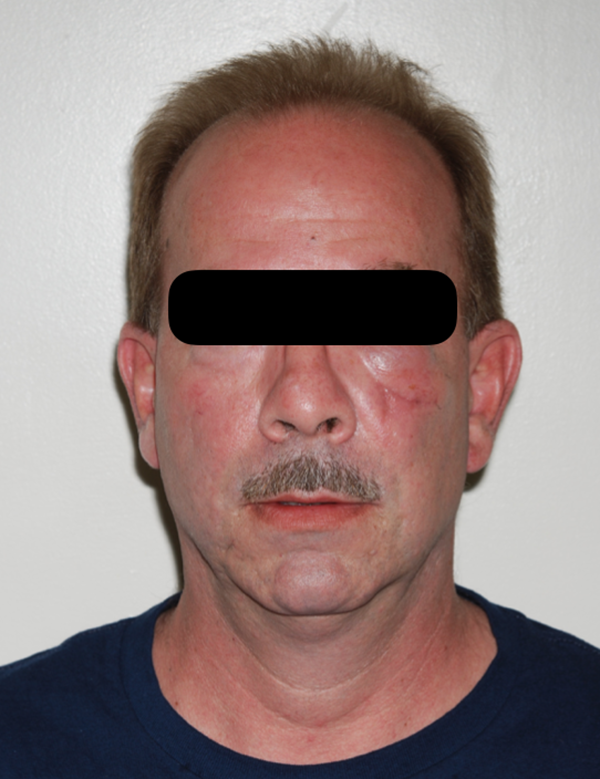
Postoperative photo at 12 weeks showing a well-healed laceration.
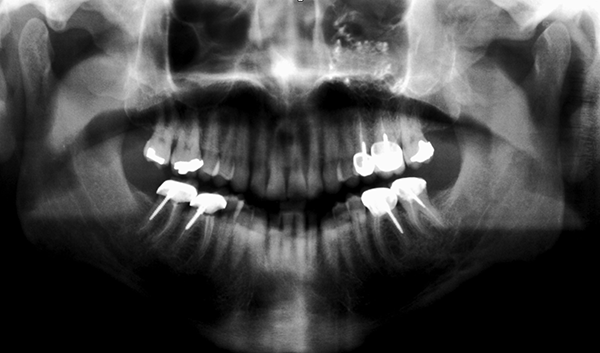
Postoperative radiograph showing fixation of fractured bone segments.
Discussion
Penetrating maxillofacial injury as a result of industrial accidents can be life-threatening and disfiguring. Initial management of any facial trauma patient begins with primary survey of ATLS, followed by secondary and tertiary surveys after patient is initially stabilized. Each of these surveys are conducted as a part of a concise algorithm designed to diagnose and manage injuries sequentially in order to mitigate morbidity and mortality. 6,10
Practitioners’ chief concern at the time of any penetrating maxillofacial injury is securing the airway followed by control of life-threatening bleeding. Diagnosis of injury to the craniomaxillofacial structures involving a projectile requires prompt CT imaging to identify the position and depth of the foreign body. This will also allow the practitioner to rule out vascular injury or endocranial penetration. Systemic and multidisciplinary approach to diagnosis and management of all facial injuries is necessary. 8,13,14 A shooting projectile such as the aforementioned case can penetrate the posterior maxillary wall and result in severe injury to the muscles, bones, the branches of external carotid especially the internal maxillary artery and its associated branches, pterygoid venous plexus, and surrounding cranial nerves. It is not inconceivable that such injury can result in acute hemorrhage from the site of trauma. The presence of rich collateral blood supply and venous tributaries can make management of bleeding following facial trauma a challenging task. At times, the protective soft tissue envelope and bony cavities such as the pterygopalatine fossa or even the sheer volume of blood make identifying or gaining proper access to the source of bleeding impossible. 7,14,15 Management of acute bleeding from those vessels may necessitate application of pressure packing or compressive bandages. If bleeding continues, direct compression of the bleeding may be achieved with packing the maxillary sinus or with application of anterior and posterior nasal packing. If severe maxillofacial hemorrhage is not amenable to direct ligation of the bleeding vessel or cannot be controlled by local conservative means, selective angiography with embolization is the treatment of choice. 15,16 However, if angiography remains unsuccessful, surgical reexploration and ligation of the bleeding vessel and ultimately ligation of external carotid artery and its major branches are effective options for management of acute maxillofacial hemorrhage. It is noteworthy that continued blood loss could still occur due to the presence of rich arterial collaterals or venous tributaries. 9,15
When it comes to injuries associated with stationary saws, focusing on prevention is significantly more critical as ATLS would only address the initial part of any trauma care after patient has already sustained the injuries. Resultant injuries from table saws can often be severe and the injured patient could require multiple operations. The victim may still suffer significant disfigurement and disability. Use of workplace safety protocols as well as personal protective equipment including head and eye protection, hand/foot protection, and other equipment accessories, such as blade guards, can minimize exposure to injuries at the workplace. 17,18
When faced with maxillofacial impalement as a result of an industrial accident, the retained object must only be removed after thorough clinical and radiological assessment. The patient must be first adequately resuscitated and medically stabilized. The airway must be secured and the bleeding should be diligently controlled. Only then, should the removal of the retained object be performed following the original direction of the injury. The affected wound should be cleared of debris such as bone particles, teeth, non-vital mucosa and any other foreign body fragments. The site of injury must be copiously irrigated with sterile normal saline and necrotic tissue removed from the wound. Anatomic reduction and reconstruction of fractured bone segments with internal rigid/semi-rigid fixation should take place. If required, immediate bone grafting should be performed. Finally, the overlying soft tissue is repaired by layered closure of deep and superficial layers. 12,18,19
In conclusion, early management of penetrating maxillofacial trauma in an injured patient as a result of an industrial accident begins with standard and accepted protocols of ATLS. Timely intervention, which includes early wound exploration and debridement, anatomic fixation and repair of fractured bone fragments, early definitive management of soft tissue, and appropriate antimicrobial coverage including tetanus prophylaxis, is critical in achieving favorable outcomes with penetrating maxillofacial injury as a result of an industrial accident.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
