Abstract
Study design:
Application of Damage Control Surgery (DCS) in Oral and maxillofacial surgery is still evolving, therefore, the current study hopes to share our experience in the management of bomb blast patients.
Objectives:
The objectives of the current study is to share our experience in the management of maxillofacial bomb blast injuries emphasizing on DCS.
Methods:
This was a retrospective study of combatant Yemeni war patients who were transported across the border from Yemen and treated in Najran, Kingdom of Saudi Arabia from December 2015 to December 2019. Information such as etiology of injury, age, zone of injury and mechanisms of bomb blast associated injuries, treatment protocol and complications. The treatment protocols adopted include; DCS in which exploration to control soft tissue bleeding was done and when bone bleeding could not be controlled, immediate reduction and osteosynthesis of bone fractures was carried out. Early Definitive Surgery (EDS) was done in patients that were hemodynamically stable with open reduction and internal fixation (ORIF) of all facial bone fractures. Closed reduction and fixation were done with the use of arch bars while in conservative approach, patients were placed only on soft diet. Data was stored and analyzed using IBM SPSS Statistics for IOS Version 25 (Armonk, NY: IBM Corp).
Results:
A total of 235 (57.6%) patients sustained bomb blast injuries from the 408 war casualties. Other patients (42.4%) sustained other types of injuries. All the patients were males. Their ages ranged from 21 to 53 years with mean (SD) at 27.3 (5.6) years. DCS was carried out in a large proportion of the patients totaling 78 (33.2%) patients, while EDS was carried out in 58 (24.7%) hemodynamically stable patients. ORIF was the main treatment modality for the fractures in 136 (57.9%) of the patients.
Conclusion:
The result of the study showed a large proportion of the patients were managed with DCS. DCS should be seen as a strategy in stabilizing the patients before definitive surgery is performed.
Introduction
Blast injuries result from explosions that have the capability to cause multisystem, life-threatening injuries in single or multiple patients simultaneously. 1 These types of events present complex triage, diagnostic, and management challenges for the health care provider. 1 Maxillofacial trauma in these scenarios exposed the patients, most importantly, to airway compromise and hypovolemic shock. 2 Hypovolemic shock is strongly associated with the “lethal triad” of hypothermia, acidosis and Trauma-Induced Coagulopathy (TIC) which further worsens the prognosis of the acutely injured patient. 3
It is now recognized that severely injured trauma patients, who are still alive at the point of medical intervention, are more likely to die from the metabolic consequences of the injury rather than the completeness of the immediate surgical repair to their damaged organs and tissues. 4,5 In this regard, Damage Control Surgery (DCS) has been adopted in the management of trauma patients who are too ill to undergo immediate comprehensive surgery. This DCS is to improve the survival of major trauma patients. The concept of DCS, a term that was originally coined by Rotondo and co-workers in 1993, has been embraced by surgeons of various specialities as a paradigm to manage these patients. 4,5
More recently, Damage Control Resuscitation (DCR) has been introduced which further improves greatly the chances of patient survival as well as increases the duration of surgery in the critically injured patient. 3,6 This DCR-DCS strategy focuses on the stabilization of the victims physiologically and hemodynamically before the start of all-inclusive anatomical and functional overhaul of all injuries. DCS, which involves immediate hemorrhage control, reduction of contamination, temporary fixation of fracture fragments and temporary wound closure, should be initiated simultaneously with the involvement of all medical personnel in trauma management. 7,8 Studies have shown the benefit of DCS in the management of maxillofacial and neck trauma. 9,10
We hope to share our experience with the application of DCS as an evolving principle in the management of some maxillofacial bomb blast patients.
Materials and Methods
This is a retrospective study of 408 war patients with maxillofacial injuries who were transported across the border from Yemen and treated in King Khalid Hospital, Najran in the Kingdom of Saudi Arabia, between December, 2015 and December, 2019. Ethical approval was obtained from the hospital research and ethics committee (IRB) with protocol number H-II-N-081. Information such as etiology of injury, age and sex were retrieved from the daily data of the Accident & Emergency (A & E) and Maxillofacial Surgery departments. Bomb blast injuries involving the maxillofacial region will also extend to the neck region, thus, classification was based on Monson classification
11
where Zone 1 extends from clavicles to cricoid, zone II from cricoid to angle of mandible, and zone III from angle of mandible to the skull base. The mechanisms of bomb blast injuries namely; landmines, landmine-induced Motor Vehicular Accidents (MVA) and Improvised Explosive Device’s (IED’s
Data was stored and analyzed using IBM SPSS Statistics for Windows Version 25 (Armonk, NY: IBM Corp). Results were presented as simple frequencies and descriptive statistics. Pearson Chi-square statistics was used to compare categorical variables. Statistical significance was set at p ≤ 0.05.
Results
A total of 235 (57.6%) patients sustained bomb blast injuries out of the 408 war casualties. Other patients (42.4%) sustained different types of injuries that were not the study focus in the current appraisal. All the patients were males. Their ages ranged from 21 to 53 years with mean (SD) at 27.3 (5.6) years. Table 1 illustrates distribution of patients’ age group by the mechanism of injury. The majority of the patients, numbering 214 (91.1%), were between the ages of 21 and 35 years with the age group from 21 to 25 years constituting the highest proportion (121 (51.5%)). Land mine explosions were the main mechanism of the blast injuries with 118 (50.2%) patients. MVA resulting from landmines, accounted for the blast injuries in 46 (19.6%) patients, while blast injuries in 71 (30.2%) patients were caused by Improvised Explosive Devices (IED’s) (Table 1).
Distribution of Mechanisms of Blast Injury According to Age Group of the Patients.
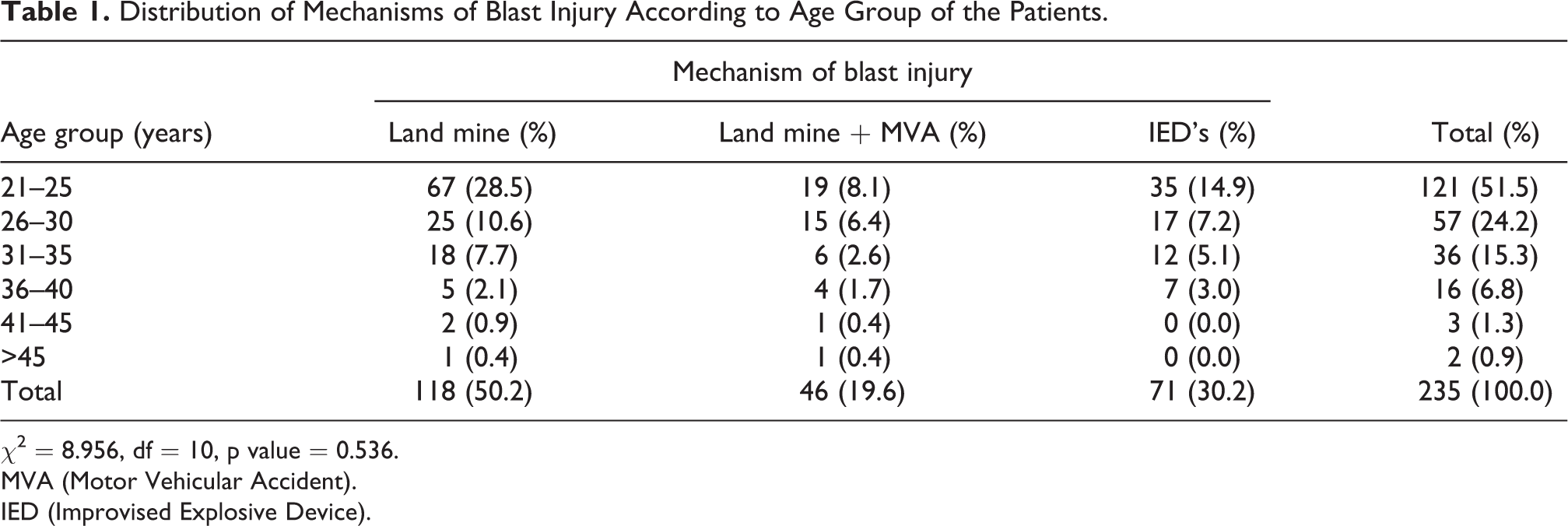
χ2 = 8.956, df = 10, p value = 0.536.
MVA (Motor Vehicular Accident).
IED (Improvised Explosive Device).
Regarding the type of injury, the combination of penetrating, perforating and avulsive injuries had the highest frequency as seen in 190 (80.8%) of the patients. A statistically significant majority of the patients, 226 (96.1%) had combination (penetrating (when the energized fragments puncture the body surface and lodges within the tissues), perforating ((when the energized fragments puncture the body surface and exits the body) and Avulsive (when there is tissue loss)) injuries to Zones 2 and 3 (χ2 = 33.436, df = 6, p value = 0.000*) when the injury zone was analyzed with injury type (Table 2). The mandible (90 (38.3%)), maxilla (40 (17.0%)) and orbit (27 (11.5%)) were the most fractured maxillofacial bones. Other maxillofacial bones fractures were as shown in Table 2.
Distribution of Blast Injury Zone According to Injury Type and Maxillofacial Bones Affected.
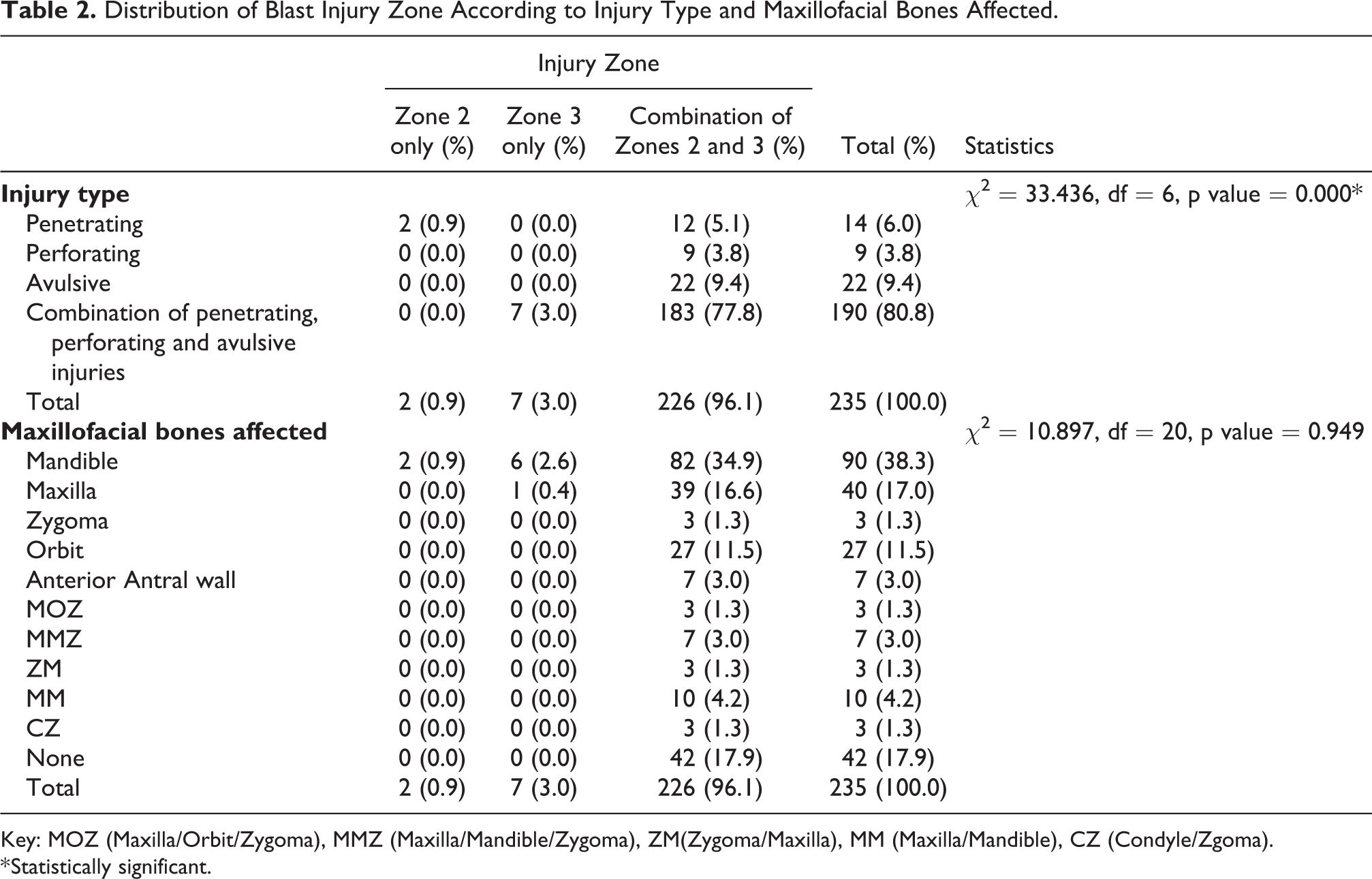
Key: MOZ (Maxilla/Orbit/Zygoma), MMZ (Maxilla/Mandible/Zygoma), ZM(Zygoma/Maxilla), MM (Maxilla/Mandible), CZ (Condyle/Zgoma).
* Statistically significant.
DCS was carried out in 78 (33.2%) patients, while EDS was carried out in 58 (24.7%) hemodynamically stable patients. In patients who had DCS, temporary osteosynthesis was performed to achieve bone fragment stabilization pending definitive surgery, while in EDS cases, ORIF was carried out to completely achieve anatomical bone fixation (Table 3). The majority of the patients had no complications as seen in 144 (61.3%) cases. Some of the recorded complications include wound dehiscence (35 (14.9%)), plate exposure (19 (8.1%)) and surgical/injury site infection (30 (12.8%)). Other complications were shown in Figure 1. Figure 2A and B showed associated injuries that were observed in these patients.
Distribution of Treatment Type According to Surgical Procedure.
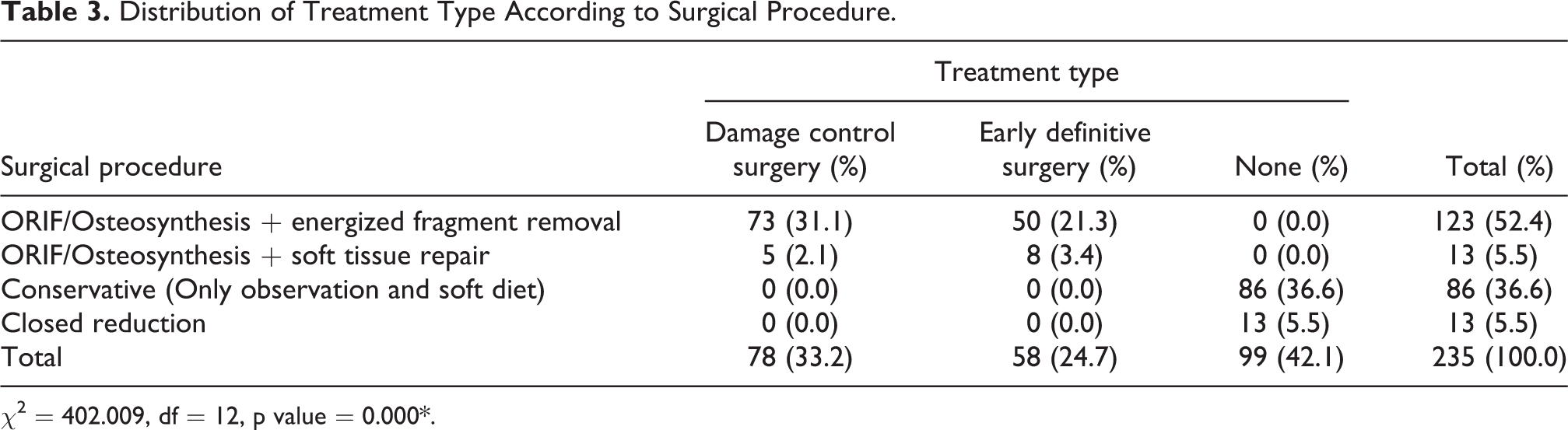
χ2 = 402.009, df = 12, p value = 0.000*.
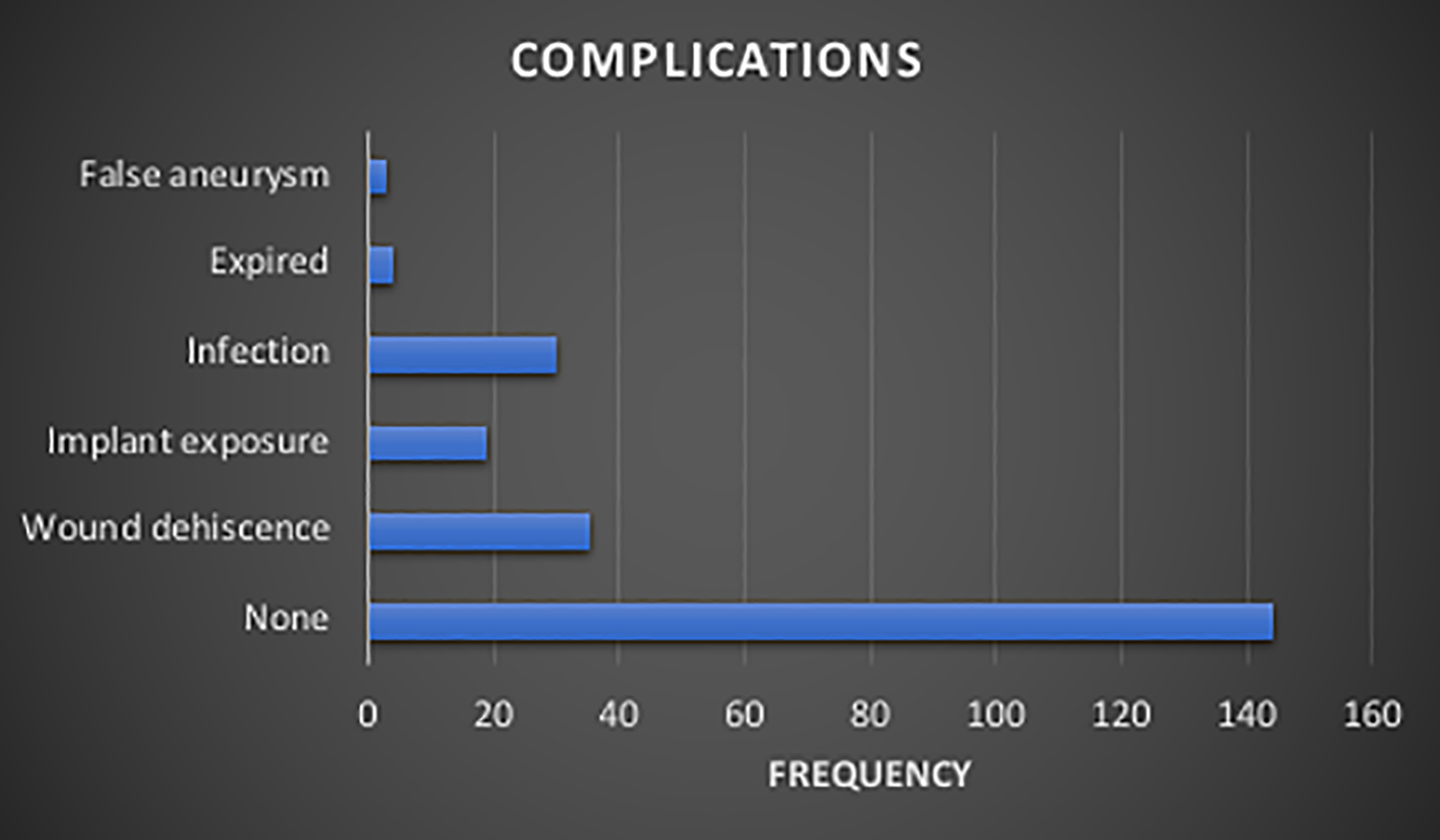
Bar chart showing the distribution of complications associated with the bomb blast patients.
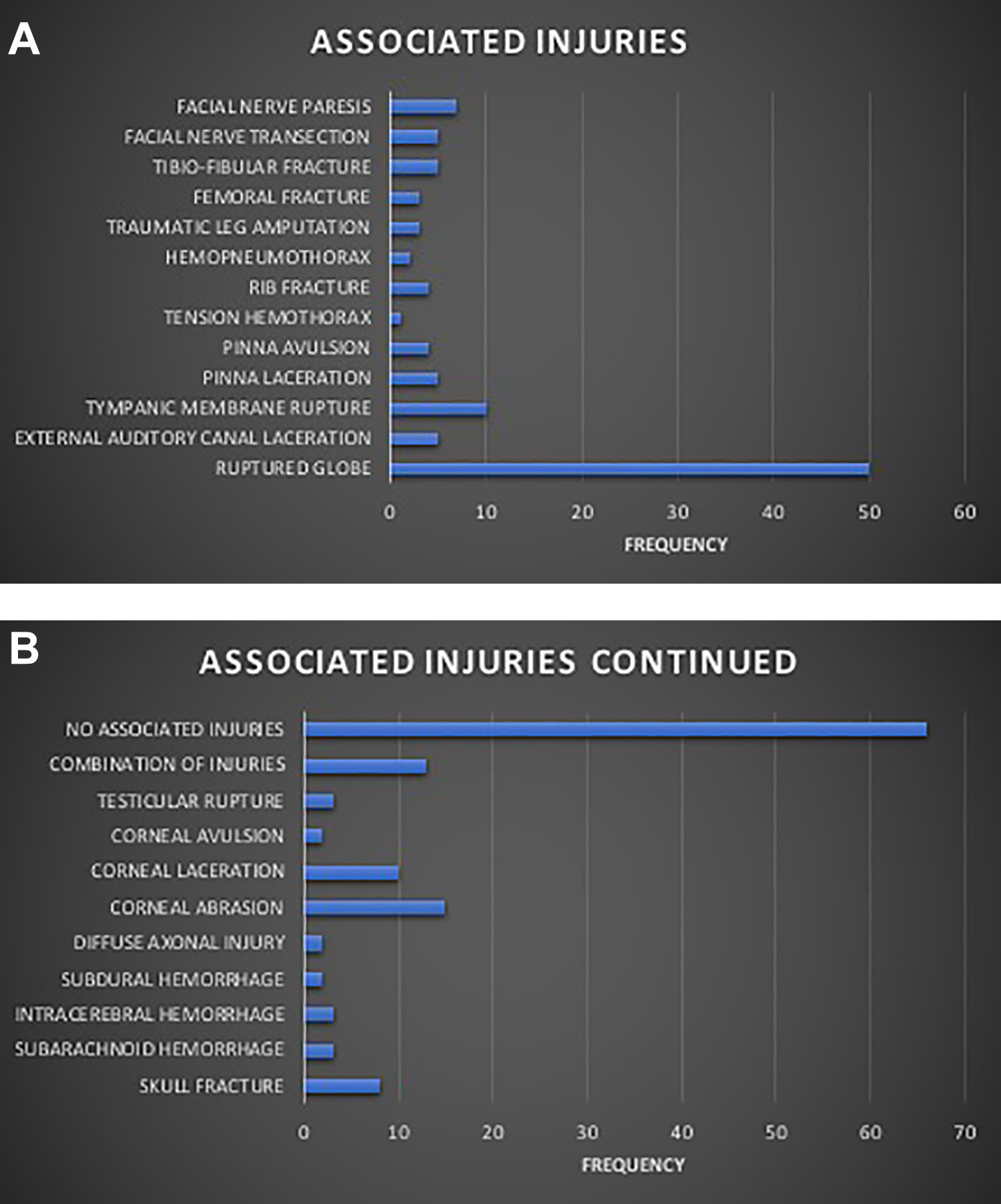
A and B, Bar charts showing the distribution of associated injuries with the bomb blast patients.
Discussion
Studies have shown that ballistic injuries account for 2% to 6% of maxillofacial fractures seen in the civilian population 13 with 6% to 81% of them reported to be suicidal attempts globally. 14 However, battlefield maxillofacial injuries involving US soldiers during the Middle Eastern conflicts were reported to represent about 26% of all the injuries. 15 As reported in the literature, majority of the combatant patients are usually young adults between the ages of 20 and 35 years and mostly males. 13 This has been corroborated by our study where 241 (91.1%) of the patients were within this reported age bracket and all were males.
Recently, with more advances in bomb weapon systems that can cause more extensive damage than guns, the incidence of blast injuries is on the increase 16 similar to results from the current study. Conversely, other studies have reported a higher incidence of gunshot injuries. 17,18
In the current study, most of the injuries were seen in the Zones II and III, which is contrary to a previous study that reported Zone II injuries to be more common. 19 Injuries involving the Zone I region were managed primarily by the ENT surgeons as the hospital protocol demands.
The mandible was the most commonly fractured bone, accounting for 90 (38.3%) cases, which is consistent with previous reports in the literature. 20 The mandible is the only movable bone in the craniofacial region and the most prominent after the zygoma, therefore, more prone to direct forces and injuries. 21 As common with firearms injuries, comminution of hard tissues and avulsion of both hard and soft tissues (Figure 3A–D) were also observed in this group of patients. Regarding the mid-face, the maxilla 40 (17.0%) and orbit 27 (11.5), were the second and third most fractured bones after the mandible (Figure 4A–D). This finding is also consistent with reports in the literature. 22
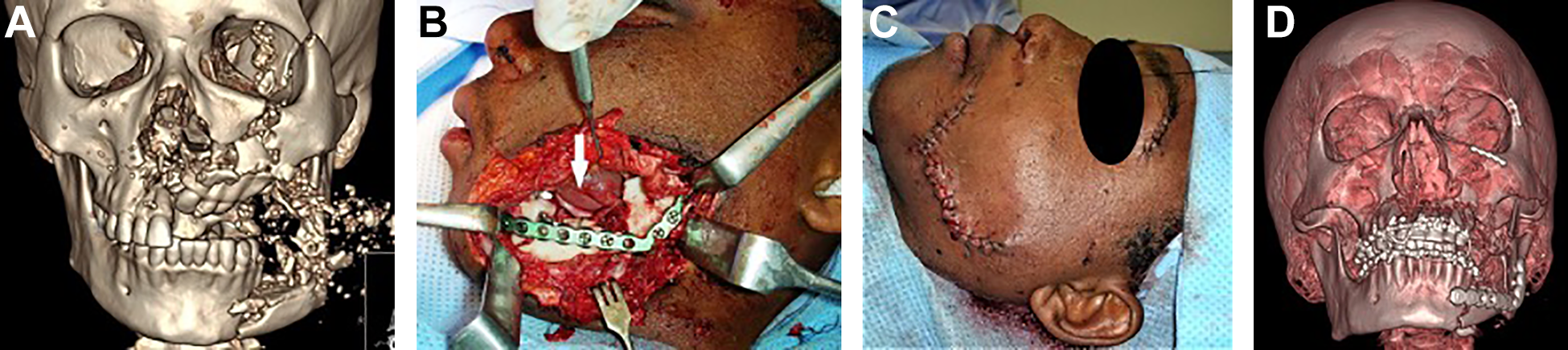
A, Anteroposterior view of 3-D CT scan of a bomb victim showing comminuted fractures of left body, angle and coronoid process of mandible, left maxilla and left zygoma. B, Intraoperative photograph showing a large defect in the left cheek used as an access for ORIF of left mandibular fracture. The white arrow points the tongue which is visible through the wound. C, Intraoperative photograph showing closure of the defect in the left cheek. D, Anteroposterior view of postoperative 3-D CT scan showing ORIF of the comminuted fractures.
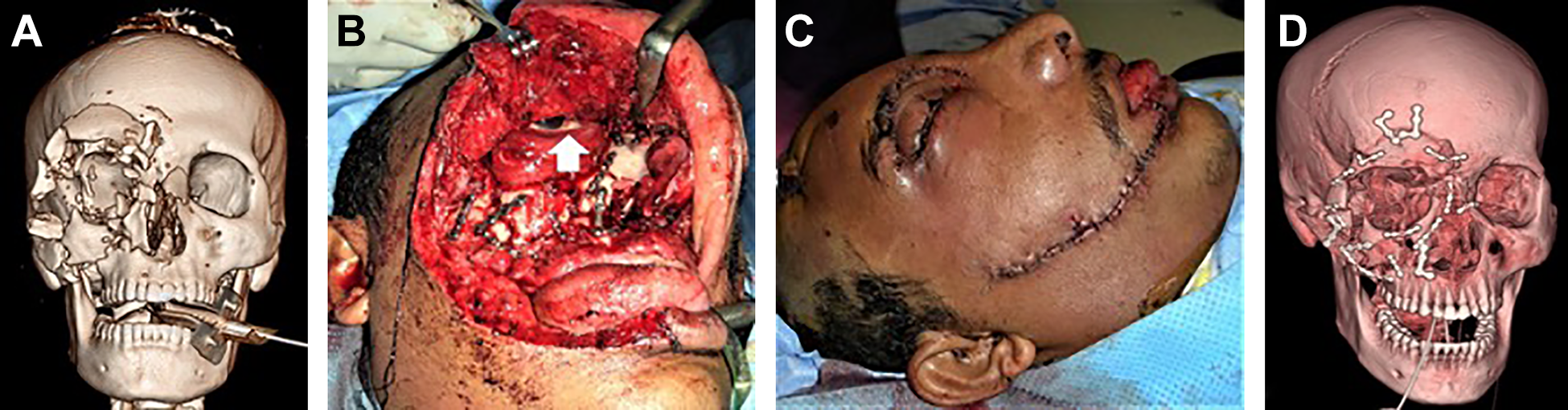
A, Anteroposterior view of 3-D CT scan of a bomb blast patient showing comminuted fractures of right maxilla, zygomatic complex, frontal bone and nose and debris embedded in the scalp. B, Intraoperative photograph showing ORIF of comminuted fractures of right maxilla, zygomatic complex and nose with access gained through degloving wound on the right side of face. The white arrow shows exposure of the right eye through the wound. C, Postoperative photograph showing repair of the degloving lacerations. D, Lateral view of postoperative 3-D CT scan showing ORIF the comminuted fractures.
Management of ballistic missile injuries has continued to generate controversies among surgeons and researchers. Basically, there are 2 groups of management strategies: The older group of “delayed surgical repair” and the more recent group of “early surgical repair.” Advocates of “delayed surgical repair” argue that since ballistic wounds are contaminated, delayed repair will ensure clean and segregated wound bed. 23
Because blast injuries result from explosions that have the capability to cause multisystem, life-threatening injuries in single or multiple patients simultaneously, EDS may be impracticable. Recently, DCS has been advocated in the management of these patients. 3,6 The concept of DCS may operate as an intermediate approach between the 2 previous management strategies of “delayed” and “EDS.” Essentially, it is an operative strategy that sacrifices the completeness of the EDS in order to address the physiological consequences of the combined trauma of the injury and surgery. 5 Initially used mainly for abdominal injuries, DCS application has been extended to include the management of wounds, head injuries, maxillofacial trauma and fractures. 5,9,10
There are 5 stages of DCS as recommended by Fries and Midwinter
5
namely: Stage 1: Patient selection and decision-making. This should occur rapidly either immediately preoperatively or within minutes of the start of surgery. Physiological measures suggested to determine when a DCS approach should be adopted for trauma victims include; injury severity score of more than 25, systolic blood pressure less than 70 mmHg, core temperature less than 34 °C and a pH of less than 7.1.
4
Stage 2: Intraoperative stage. Priorities are hemorrhage control by ligation, suture or packing, limiting contamination and temporary closure. Limited operation time is essential and temporary closure is established to allow the patient to be moved to a critical care environment. Stage 3: Critical care stage. In the critical care environment such as the ICU, continued attempts at correcting the physiological consequences of the injury and metabolic failure are pursued by correction of hypothermia, acidosis and coagulopathy. Stage 4: Return to the operating theater. This is dictated by the improvement in the patient’s physiological status. Appropriate surgical team must be put in place to ensure that the optimum repairs of the injuries are performed in the optimum surgical environment. Stage 5: Formal closure. If is not possible to close the wounds at stage 4 as there may still be significant edema or clinical risk of developing other complications such as a compartment syndrome.
In the current study, DCS was carried out in 78 (33.2%) very critically injured patients and EDS was carried out in 58 (24.7%) hemodynamically stable patients. With our experience, when patients were hemodynamically stable, EDS of fractures with ORIF and soft tissue repair was our treatment option. This approach is consistent with the current trend of treatment by early surgical intervention of maxillofacial ballistic injuries. 24 In our emergency unit, efficient protocol have been instituted to promptly provide optimal surgical care for war patients referred from the field health facility. Before arrival of these patients, the trauma team is informed ahead and all resources (both human and material) including laboratory are already on ground before arrival of the victims. Detailed injury situations are also relayed ahead to the hospital with most of the patients intubated before arrival. This arrangement has continued to increase the survival rate of patients and minimize morbidity. Most of the times, patients were taken from the transferring ambulance and directly into the operation room with critical care facilities to reverse the lethal triad associated with severe acute injuries. Hypovolemic shock is strongly associated with the “lethal triad” of hypothermia, acidosis and Trauma-Induced Coagulopathy (TIC), which further worsens the prognosis of the acutely injured patient. 3
Recent evidences have shown that in the maxillofacial region, many ballistic injuries may be treated early to achieve re-establishment of the integrity of the facial bones, lower morbidity, faster return to function, shorter hospital stay, and the possibility of fewer operations for the patients. 24 –27
In a systematic review of DCS in combat-related maxillofacial and cervical injuries by Tong and Breeze, 28 2 papers were identified that shared their experiences with the concept of Damage Control Surgery (DCS). 29,30 These studies were conducted by the UK military oral and maxillofacial surgeons during the Afghanistan war from 2006 to 2009. 28,29 In their review, both papers reported the use of DCS for the maxillofacial injuries. In another review article, Krausz et al, 8 reported that some maxillofacial injuries may require immediate attention at the resuscitation period. He defined these injuries as “maxillofacial medical emergencies” which include unstoppable hemorrhage from maxillofacial bone fractures that requires immediate reduction and osteosynthesis. 8 In our study, those patients whom we applied the DCS to, had exploration to control soft tissue bleeding and when bone bleeding could not be controlled by bone stabilization, we carried out immediate reduction and osteosynthesis of bone fractures by picking viable bone pieces and aligning them with the use of wires, microplates and/or flexible 2.0 miniplates during the Stage 2 as suggested by Fries and Midwinter 5 and then reinforcing the realigned segments with rigid 2.0-mm miniplates, 2.4-mm plate or 3-mm reconstruction plates as required during the Stage 4 (Figure 5A–F). In one of our patients with very severe multiple injuries including orthopedic, ophthalmic, urological and abdominal injuries as well as extensive facial soft tissue loss, reconstruction of soft tissue defect involving the lower lip and chin was done with pectoralis major flap to cover exposed anterior mandible at Stage 5 of DCS (Figure 6A–F). With the recent development of Damage Control Resuscitation (DCR), a change in approach is required to integrate resuscitation and surgical phases more closely. In order to achieve the goal of optimizing outcome, DCR and DCS should be considered a single concept. 4 The combined DCR-DCS addresses both the resuscitation and surgical issues concurrently (Stages 1 and 2 of the classical DCS as described by Fries and Midwinter 5 ) and need to occur together from the outset 5 and requires a fully integrated cross-disciplinary trauma team with joint training and understanding in this approach. 4 DCR-DCS also increases the surgical time which would otherwise not be possible if DCS was applied alone and allows extended operating time (with median of about 4.5 hours). In this particular patient in Figure 6A to J, the application of the combined DCR-DCS approach allowed for a longer operation time for combined surgeries by orthopedic, maxillofacial and plastic surgeons.
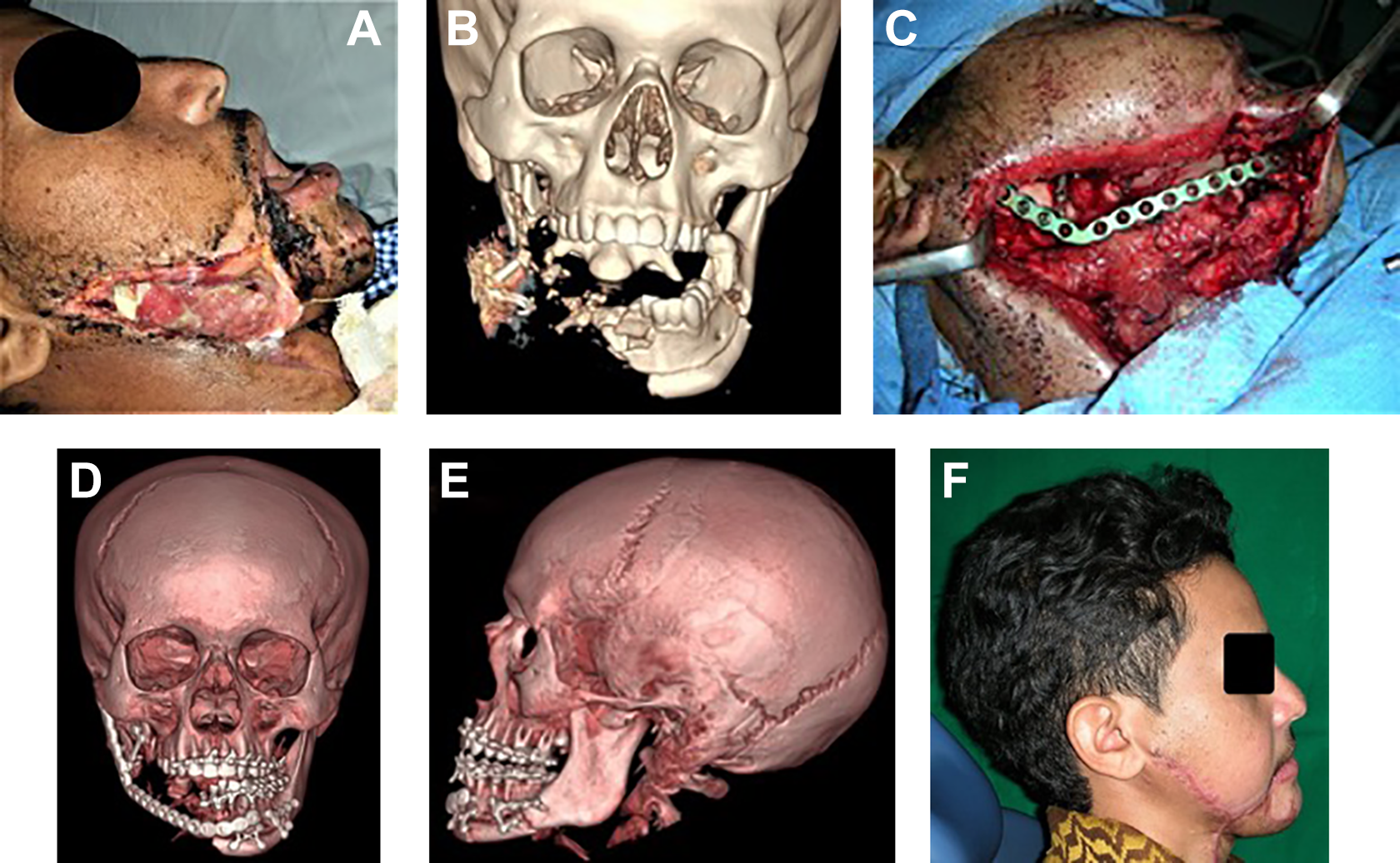
A, Preoperative photograph of bomb blast patient showing an infected deep and large wound in the right cheek and neck with some tissue loss. The right side of mandible was avulsed with only the proximal stump showing at the upper end of the wound. B, Anteroposterior view of 3-D CT scan of the bomb victim showing fractured left mandible and avulsed right side of mandible. C, Intraoperative photograph showing replacement of missing right mandible with 3 mm reconstruction plate using an access through the defect in the right cheek. D, Anteroposterior view of postoperative 3-D CT scan showing ORIF of comminuted fracture of left mandible and replacement of avulsed right mandible with reconstruction plates. E, Left lateral view of postoperative 3-D CT scan showing ORIF the comminuted fractures of symphysis and body of mandible. F, Postoperative photograph of the patient with avulsed right mandible and comminuted left side of mandible.
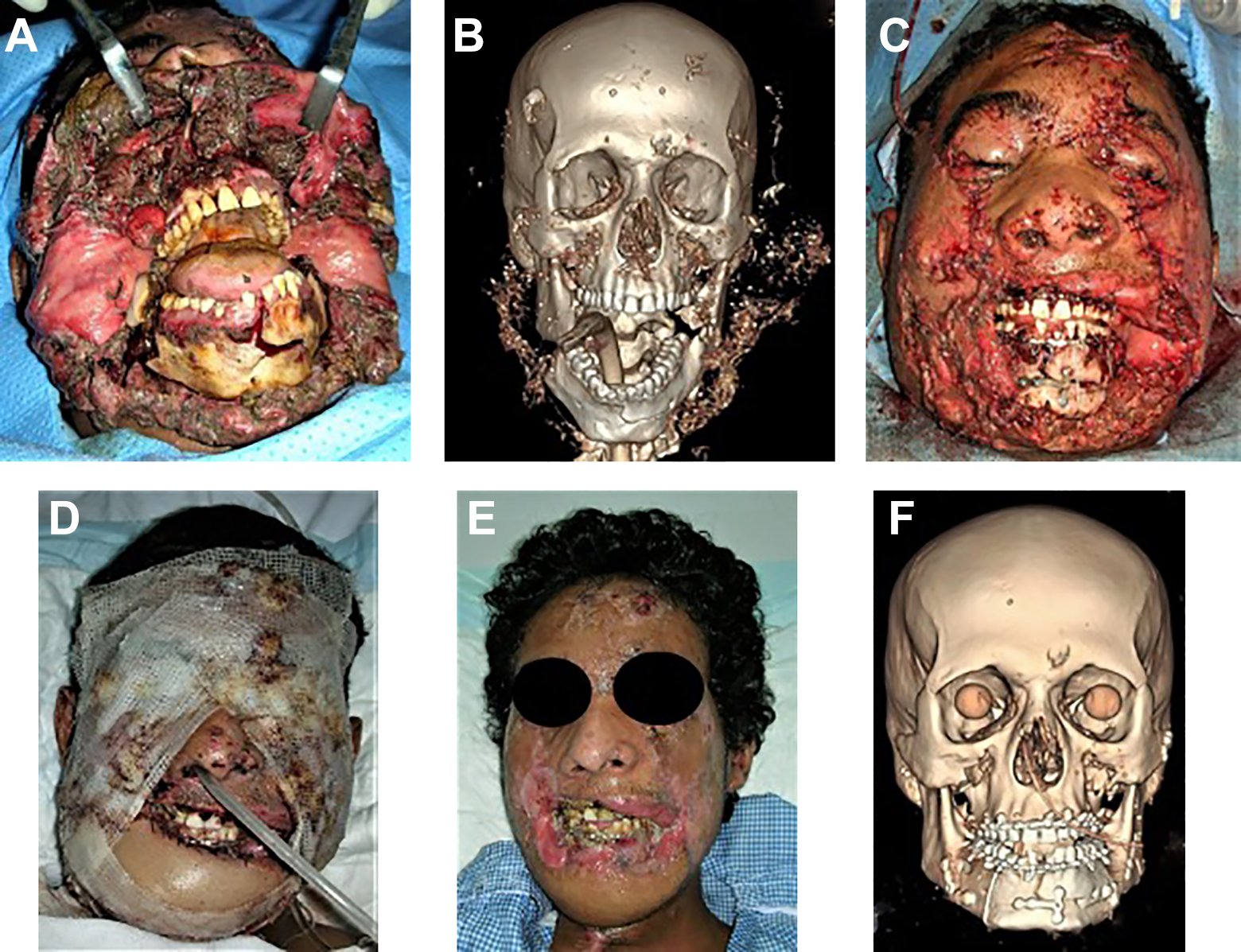
A, Photograph of patient showing intraoral degloving lacerations of upper lip and cheeks, comminuted fractures of mandible exposed by loss of lower lip and soft tissue covering the mental region. Note the tracheostomy done to protect the airway. B, Anteroposterior view of 3-D CT scan of the patient showing multiple fractures involving right and left angles as well as symphysis of mandible and a lot of debris embedded in the soft tissues. C, Intraoperative photograph after debridement of facial wounds, ORIF of mandibular fractures and repair of lacerations. Note the exposed anterior mandible due to avulsion of entire lower lip and the rest of soft tissue covering the chin. D, Postoperative photograph showing reconstruction of the lower lip and the rest of soft tissues with pectoralis major flap. E, Photograph of the patient taken 3 weeks after reconstruction of lower lip. F, Anteroposterior view of postoperative 3-D CT scan showing ORIF of comminuted fractures of mandible and prostheses inserted bilaterally to replace ruptured globes.
Closed reduction was done with the use of arch bars and intermaxillary fixation in 13 (5.5%) patients who had no fracture displacement. This presentation was observed mainly in the group with Land mine + MVA as the etiology of the injury in which the primary presentation in such group were injuries related to MVA without any chemical burns or loss of tissues.
Wound dehiscence and local infections were complications observed in our series and were treated with local measures and medications. Patients that had plate exposure as complication had them removed. Three (1.3%) patients developed false aneurysms in which vascular embolization of the relevant feeding branches of the external carotid artery were carried out in 2 patients by interventional radiologists and surgical evacuation done in 1 victim by vascular surgeons. Most of the patients (61.3%) recovered uneventfully and returned home. Two patients passed away because of severe head and thoracic injuries and not primarily from the maxillofacial injuries. Although, the patients survived from the battlefield up to the hospital, they later succumbed to the injuries despite all efforts by the trauma team after 24 hours of intensive care.
Because of the high turnover rate of patients for emergency surgery during the conflict, some of these elective procedures were deferred. Appropriate and comprehensive medical report, detailing the treatment given and any recommendations for further treatment were provided to all patients returning to their country for adequate follow-up.
Conclusion
Our experience as oral and maxillofacial surgeons in the management of bomb blast injuries showed that large proportion (78 (33.2%)) of the patients were managed with DCS by repairing soft tissue injuries to achieve hemostasis and utilizing reduction and temporary osteosynthesis of bone fragments when bony hemorrhage could not be controlled. The DCS approach adopted for those with severe injuries, should not be confused with older view of “wait and see” option, however, it should be seen as an intermediate treatment between it and newer view of “early definitive surgical intervention.” Multi-specialty approach and follow-up should be employed in the management of this group of patients.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
