Abstract
Background:
Trigeminal trophic syndrome is a rare complication of peripheral or central damage to the trigeminal nerve characterized by anesthesia, paresthesia and a secondary persistent facial ulceration.
Methods:
We describe the case of a 40-year-old woman with previous history of Le Fort I osteotomy for a class III malocclusion who developed trigeminal trophic syndrome. Atypically, the cutaneous symptoms appeared bilaterally and 8 years after surgery.
Results:
Differential diagnosis was based on clinical history, tissue biopsy and serologic evaluation. Atypical findings could be linked to the surgical burdens of Le Fort I osteotomy, a procedure characterized by a bilateral incision on the maxillofacial bones with a reasonable probability of causing a bilateral injury of the peripheral branches of the trigeminal nerve.
Conclusion:
Although the long delay between trigeminal trophic syndrome onset and surgery and the absence of adequate medical evidence cannot confirm a link with previous surgery in this case, the increasing number of maxillofacial surgery cases suggests that this complication may be more frequent in the next decades, and thus, involved specialists should be aware of this condition as a possible complication of maxillofacial surgery procedures.
Keywords
Introduction
The trigeminal trophic syndrome (TTS) is a rare clinical entity described for the first time in 1901 by Wallenberg. 1 TTS develops cutaneous painless and disfiguring ulcerations within the trigeminal dermatomes and may be caused by central or peripheral injuries of the trigeminal nerve. 2 To date, about 100 cases have been described and reported in the literature. 3
The causes of this condition remain unclear; TTS has been reported as a complication of trigeminal nerve ablation following surgery, stroke with posterior inferior cerebellar artery occlusion (Wallenberg’s lateral medullary syndrome), psychiatric disorder, local infection or cancer.4–8 The time between the primary causative condition and the onset of the first symptoms ranges from 2 weeks to 30 years. 8 Similar lesions have also been reported in different body areas as a complication of similar insults in other nervous traits. 9
TTS is typically localized in the facial areas reached by the branches of the trigeminal nerve, and its classical clinical triad is composed of the following: (1) trigeminal anesthesia, (2) facial paresthesia and (3) crescent lateral ala nasi ulceration.10–12 It is important to clarify that the term “trophic” can be misleading since the ulcerations appear to be self-inflicted by the patient as an attempt to relieve itching and pain; such behavior has also been reported during the sleep. 13
Case presentation
A 40-year-old woman came to our attention for assistance in legal proceedings involving compensation for her compromised health condition. Her clinical history was significant for migraine, celiac disease, cephalosporin intolerance and nickel allergy. In 1996, she underwent Le Fort I osteotomy and bilateral positioning of two metal “L” plates and wires for maxillofacial malformation and malocclusion. There were no complications during surgery and follow-up. During the following years, the patient reported a significant increase in the pre-existing migraine with aura, photophobia and dizziness.
In 2004, the patient noticed the appearance of a skin rash located in the right regions of the forehead, nose, upper and lower jaw associated with trigeminal paresthesia. Ulcerations were painless but pruriginous. The right side of the face was severely disfigured; the left side had similar, but less severe, lesions. The tip of the nose was completely spared.
Dermatological examination diagnosed an allergy to nickel, a material found in the metal plates positioned during surgery 8 years before (Figure 1); plates and wires were therefore removed in 2005. Instrumental tests, including skin biopsy, were negative for human herpes virus, autoimmune vascular and connective diseases, leprosy, granulomatosis and skin cancer. No clinically evident neurologic deficits were reported during neurological examination. In 2008, a psychiatrist also diagnosed a severe reactive chronic depressive syndrome caused by the social difficulties following the disfiguring effects of the disease. In 2010, the ulceration of the right ala nasi caused the collapse of the nasal septum (Figures 2 and 3).
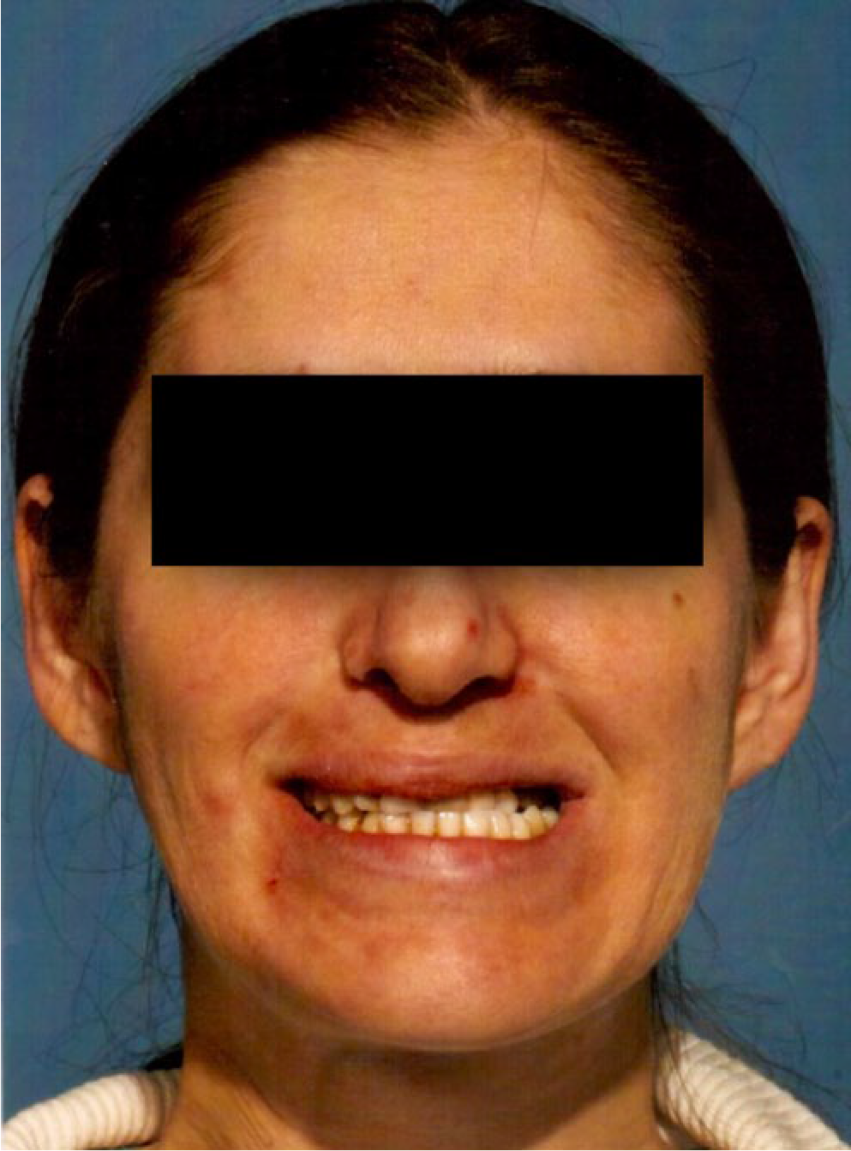
Picture showing patient’s malocclusion and the first ulcerations.

Right side view of the face of the patient; ulcerations and collapse of the ala nasi are clearly visible.

Detail of the left side of the patient’s face; ulcerations are clearly visible.
The diagnosis of TTS was based on the instrumental test results, clinical history and the exclusion of other possible causes of the painless, non-healing ulcerations present in the patient.
Discussion
TTS diagnosis can be made on the basis of observation and clinical history; the patient described in this report was examined by various specialists and underwent several instrumental tests due to the rare nature of the disease.
The atypical element of this case is the bilateral injury of the trigeminal nerve branches; other elements reported in this case are typical for TTS: (1) the ulcerations were distributed in the trigeminal nerve dermatomes, (2) the tip of the nose was spared, (3) the patient reported paresthesia of the trigeminal nerve, (4) numbness, (5) itch similar to ghost limb sensation and (6) the ulcerations did not respond to medical treatment.
Differential diagnosis was conducted with instrumental and clinical tests. The skin biopsy excluded other diseases such as herpes simplex, herpes zoster, leprosy, syphilis, diphtheria, leishmaniasis, mucomycosis, granulomatosis, vasculitis, lymphomas and skin cancer. Osteomyelitis was excluded by total body scan and computer-assisted tomography. Blood tests were within normal range.
A possible explanation for the atypical finding of bilateral injury of the trigeminal nerve branches could be linked to the surgical burdens of Le Fort I osteotomy, characterized by a bilateral incision on the maxillofacial bones with a reasonable probability of causing a bilateral injury of the peripheral branches of the trigeminal nerve.
In legal medicine terms, it is important to note that this case regards a very rare syndrome with about 100 cases reported in the literature, and hence, the professional opinion inherent compensation or professional responsibility may only be given on a probabilistic base. In this patient, the long delay between TTS occurrence and surgery and the absence of adequate medical evidence do not allow to confirm the hypothesis of a link between TTS and previous maxillofacial surgery. Although just a speculation, the necessity to remove plates for the allergy to nickel may have contributed to TTS development. Furthermore, many clinical and etiopathological mechanisms of TTS are still unknown, as this condition may present in different forms: there may be central or peripheral lesions of the trigeminal nerve, the involvement of multiple areas of the trigeminal dermatomes, the appearance of skin ulcerations at different times from the initial cause of the nerve injury, the presence of similar nerve injuries in different body parts and the appearance, as in this case report, of bilateral lesions.
Although in this case it was not possible to find a clear link between TTS and surgery, such link may exist especially when TTS follows surgery in a short time frame (e.g. within 1 year from surgery). In light of this, the increasing number of maxillofacial and dental surgery procedures 14 suggests that there may be an increase in TTS in the next decades; besides the clinical awareness that will necessarily need to include TTS as a possible complication, 15 also healthcare specialists involved in legal medicine procedures should familiarize with this syndrome for a better evaluation of its outcomes.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
