Abstract
Study Design:
Systematic review.
Objective:
Vastus lateralis is used to reconstruct defects in the head and neck. While the advantages are documented, donor-site morbidity requires further investigation. Before an investigation can commence, a review of the literature is required. The aim of this study was to review the existing evidence regarding the use of the vastus lateralis flap and donor-site morbidity. The results from this study will assist to determine further research and need for preventative and post-operative options to improve patient care and health outcomes.
Methods:
Electronic databases were searched (in January-February 2020). Peer-reviewed, English language articles were included if they investigated the association between the vastus lateralis flap and donor-site related health outcome. Two reviewers independently screened and assessed the articles. The risk of bias of each individual study was assessed using the Cochrane risk of bias assessment for observational and intervention studies.
Results:
Five articles representing 97 participants from 4 countries were included. The vastus lateralis flap (head and neck reconstruction) was shown to have a neutral association with donor-site leg strength, ability to climb stairs, walking and activities of daily living. Minor negative associations was found for changes in sensation and bruising.
Conclusion:
Current research reports a neutral effect between the use of the vastus lateralis and donor-site morbidity. Further research is required using a more rigorous investigative approach using a wider range of objective measures and larger sample sizes to confirm these findings to inform holistic post-operative care options.
Introduction
Head and neck reconstruction requires a careful balance between aesthetic and functional outcomes associated with donor-site morbidity. There are multiple considerations when choosing the appropriate reconstructive approach, including the size and type of defect, recipient vessel options, patient expectations and donor-site morbidity. Muscle flaps such as the Vastus Lateralis (VL) are used in various situations in the head and neck in circumstances where extra bulk is required, to fill cavities such as the orbit, vascular cover, for large defects combined with a skin graft, or for dynamic reanimation as a neurotised flap. 1,2
The VL muscle flap is reported to be a versatile and valuable reconstructive tool. 3,4 Its long pedicle is based on the descending branch of the lateral circumflex femoral artery and venae commitantes. The flap may be raised as either a simple muscle flap, a neurotised muscle flap or as a chimeric flap with components including skin and potentially even bone. Depending on the defect, up to 20 × 10 cm of muscle may be harvested. Despite these advantages, there are limited data available regarding VL flap donor-site morbidities. The vastus lateralis is 1 of at least 4 extensors of the knee and allows actions such as walking, running, sit to stand and climbing stairs. As the vastus lateralis is attached to the tibial tuberosity, it works alongside the vastus medialis muscle to maintain the position of the patella. Muscle strength changes in either the vastus lateralis or vastus medialis may lead to knee pain, which in this circumstance, is known as patellofemoral pain syndrome. 5 Changes in vastus lateralis musculature has also been implicated in patella tendinopathy 6 and gait abnormalities. 7,8
Identifying potential complications from this type of surgery may assist in the prevention of various conditions such as patellofemoral pain syndrome and decreased functional mobility. If significant donor-site morbidity is found and documented, patients may be able to be prescribed an early intervention or offered various post-operative care options to prevent or treat any lower limb functional impairments. Careful review of the literature is required to inform further investigation or prescription of preventative programs to improve patient outcomes. The aim of this systematic review is to comprehensively investigate the existing evidence regarding donor-site morbidity after harvest of a VL flap to reconstruct a defect of the head and neck.
Methods
Registration
This project was registered with PROSPERO, the international prospective register of systematic reviews (http://www.crd.york.ac.uk/prospero) and was reported in accordance with the Preferred Reporting Items for Systematic review and Meta-Analysis (PRISMA) statement. 9
Search Strategy
Computerized searches were completed in January and February 2020 using MEDLINE, PubMed, Web of Science and Scopus. The search was limited to titles/abstracts/keywords containing English, human and peer-reviewed articles using the search terms: “Head OR neck” AND “vastus lateralis” AND “surgery OR surgeries” AND “morbidi* OR function* OR lower limb OR musculoskeletal* OR mobility* OR balance OR strength OR pain OR nerve.” The output of the search strategy was screened manually using EndNote software program and duplicates were removed using this same program. The titles and abstracts were independently reviewed by 2 researchers to determine if they met the criteria for inclusion. Full-text articles were then reviewed to ensure eligibility. The reviewers discussed any differences and mutually came to a consensus regarding inclusion. Reference lists of included studies were also screened for possible studies. To capture any registered clinical trials, 2 trial registries (https://clinicaltrials.gov/andhttp://www.who.int/ictrp/en/) were searched in January 2020 using the search term “vastus lateralis.”
Inclusion and Exclusion Criteria
To be included in this review, the article was required to be published in a peer-reviewed journal, written in English, and meet the predetermined inclusion criteria. The review was based on the population, intervention/exposure, comparator/control, and outcome (PICO) study criteria 10 from the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) framework. 11,12 Conference abstracts, book chapters, and dissertations were excluded.
Population, Intervention, Comparator and Outcome
The population chosen to review were patients who had undergone reconstructive surgery of head and neck using the VL flap (any part of the muscle). To ensure all studies were captured, and to maximize the generalizability of findings, experimental studies were required to have a minimum sample size of 5 participants in at least 1 intervention group. In addition, observational studies were required to have a minimum sample size of 10 participants. Studies were excluded if they reported data only on patients receiving reconstructive surgery for a deficit of the head and neck using a different flap type (e.g. anterolateral thigh free flap, radial forearm free flap, fibula free flap) or if the VL flap was used to reconstruct an area of the body that was not in the head or neck.
The intervention/exposure was VL free flap reconstruction surgery to reconstruct deficits of the head and neck. Studies that investigated donor-site morbidity after using the VL flap combined with another flap (e.g. anterolateral flap) were excluded.
The comparators were objective or subjective normative measures from a non-surgical population or from the affected or unaffected limb of a patient who had undergone VL flap surgery from an observational or experimental study.
The outcomes were any health outcome that could be related to donor-site morbidity. For example: Function (lower limb mobility, activities of daily living, personal care, gait abnormalities); Muscle changes (lower limb muscle strength, lower limb muscle length, muscle wasting); Knee conditions (knee pain, patella tendinitis, patellofemoral pain syndrome); Nerve damage; Quality of life; Physical activity level; Obesity (body mass index) and risks/harm (injury, infection, death).
Data Extraction
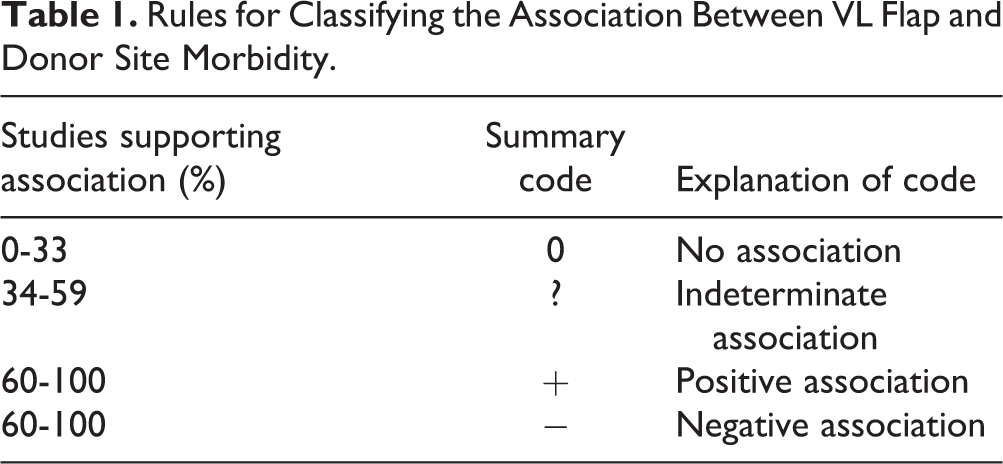
Data extracted included; authors name, publication year, country, study design, sample size, characteristics of participants, head or neck condition requiring a VL flap, characteristics of VL flap, health outcome measure, association of VL flap with the health outcome and the risk of bias. A finding was deemed to be statistically significant if P < 0.05. Two reviewers completed the data extraction for each included article and compared their findings to ensure consistency. The rules for classifying the effect of VL flap on donor-site morbidity are reported in Table 1. This method has been used in previous research. 13,14
Rules for Classifying the Association Between VL Flap and Donor Site Morbidity.
Quality Assessment
The risk of bias of each individual study was assessed using the Cochrane risk of bias assessment for observational and intervention studies. 15 Selection bias, performance bias, selective reporting bias, detection bias, attrition bias, and other biases (e.g. confounding factors) were assessed. 16 The risk of bias was assessed separately by the reviewers and then discussed to confirm the final assessment of the study.
Results
Description of Studies
After duplicates were removed (n = 99), 805 titles and abstracts were reviewed and 59 full-text articles were screened (Figure 1). A total of 5 articles met the inclusion criteria. Reasons for excluding articles are summarized in Figure 1. The 5 articles involved 97 participants from 4 different countries. The year of publication ranged from 1995 to 2017. There were no experimental or longitudinal study designs, all were observational cross-sectional studies. Donor-site morbidity was measured subjectively in 4 articles as part of the surgeon’s post-operative assessment 3,17 –19 and objectively in 1 article using objective stress testing. 20 The overall quality of the included studies was low. All studies had high selection bias due to the use of convenience undiversified groups of participants (with small sample sizes) in each of the studies. Further information regarding the included studies are reported in Table 2.
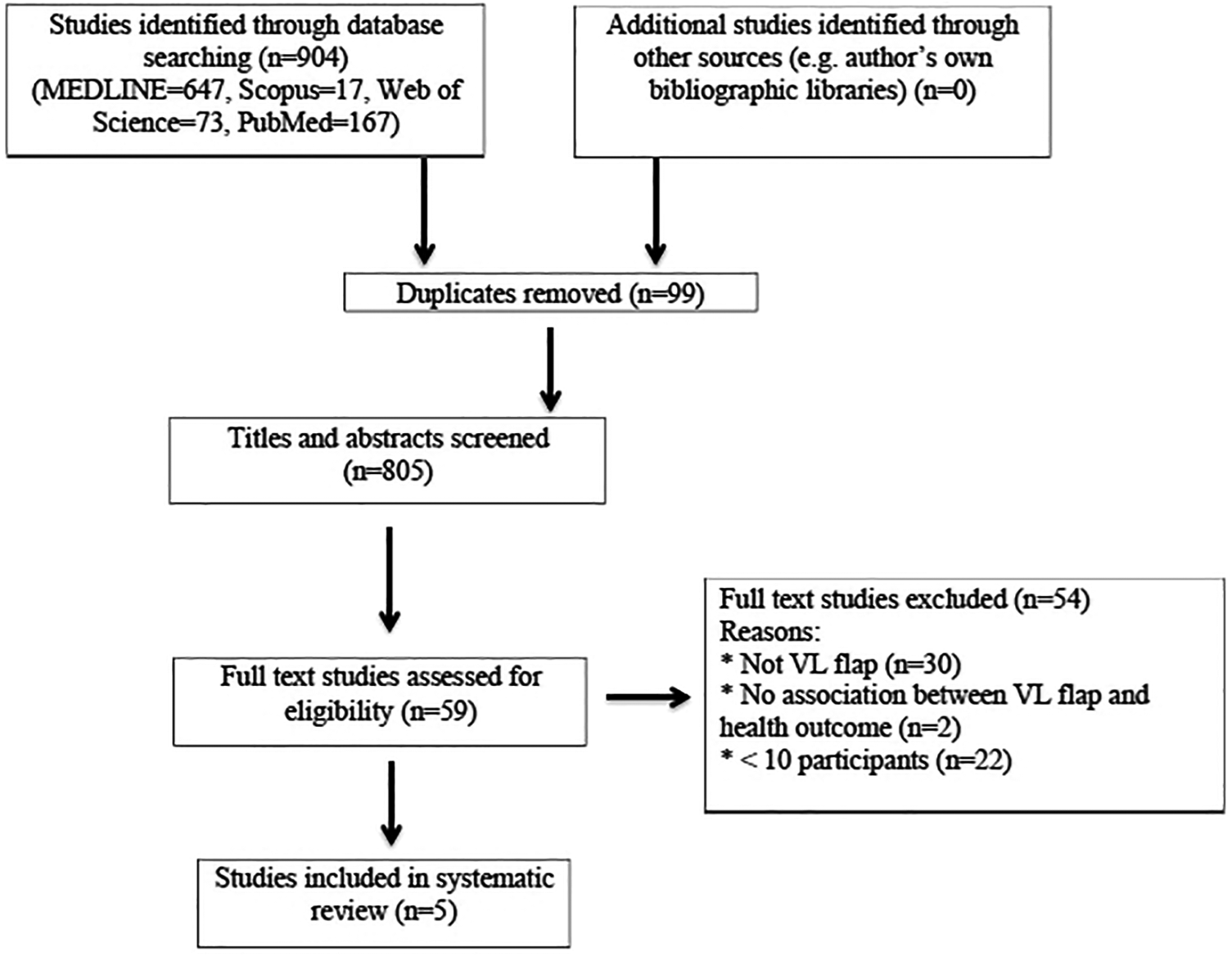
Flowchart of included and excluded studies.
Descriptive Information and Risk of Bias of Included Studies (Ordered Alphabetically).
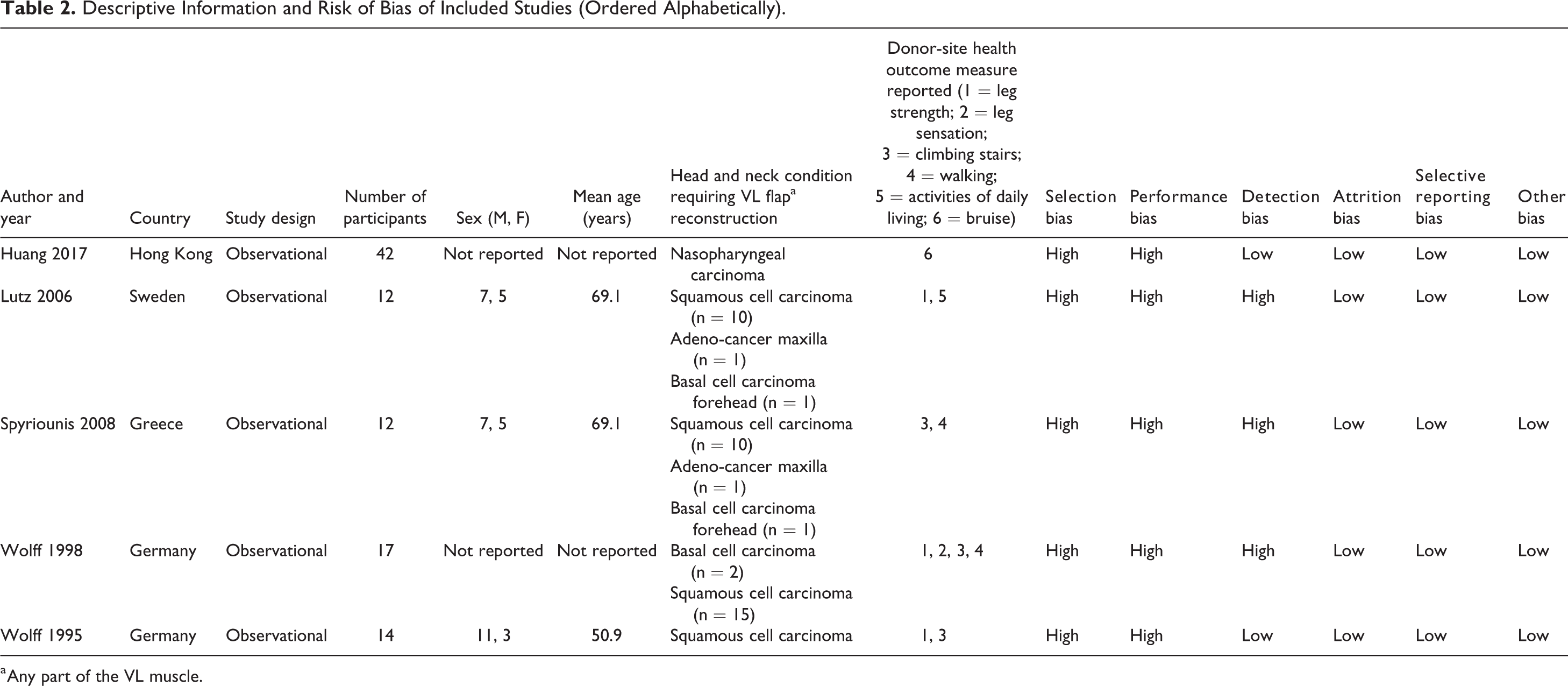
a Any part of the VL muscle.
Association With Donor-Site Morbidity
All outcomes that had a positive, neutral or negative association with the use of VL flap (any part of the muscle) to reconstruct defects of the head and neck are reported in Tables 2 and 3. Six outcomes relating to the donor-site were examined overall. These were leg strength, leg sensation, ability to climb stairs, walking, activities of daily living and the presence of a hematoma.
Summary of Reported Association of VL Flapa Use (To Reconstruct a Head and Neck Defect) With a Donor-Site Health Outcome.
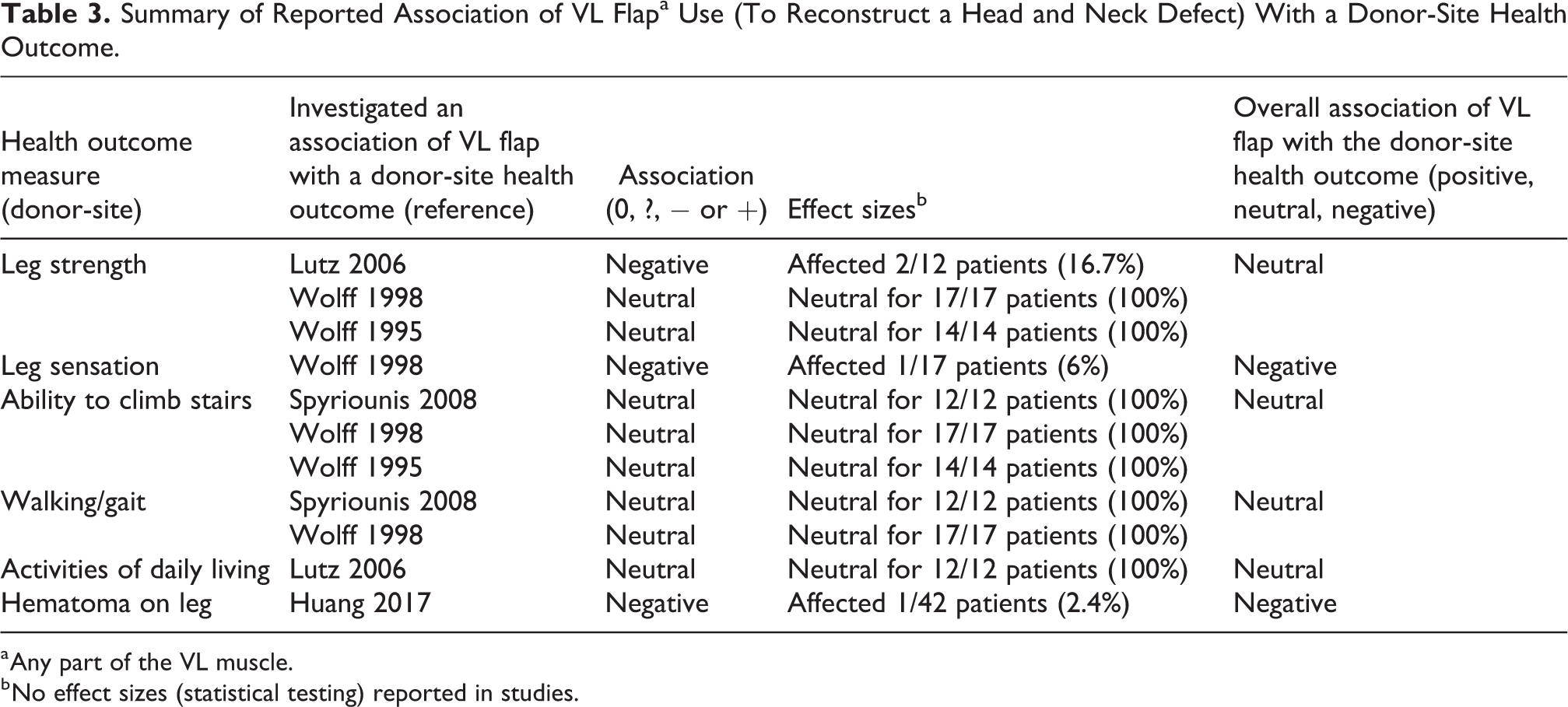
a Any part of the VL muscle.
b No effect sizes (statistical testing) reported in studies.
Leg strength
Three studies reported an association between VL flap use and leg strength. 18 –20 For one study VL flap use was associated with complaints regarding weakness in the donor leg when kicking a ball or when riding a bicycle. However, this was confined to patients where the whole or a large portion of VL flap was required to reconstruct a deficit following a basal cell carcinoma (forehead) and squamous cell carcinoma (scalp). 18 The other 2 studies reported no weakness in the legs and no complaints of a loss of strength from the post-operative assessment completed by the surgeon 19 and objective stress testing. 20
Leg sensation
One study reported a negative association between VL flap use and disturbed sensation from the innervation area of the lateral cutaneous femoral nerve. 19 They also report this loss of sensation then resolved after 6-9 months post-surgery.
Climbing stairs
Three studies reported a neutral association between VL flap use and the ability to climb stairs after VL flap surgery. 3,19,20 Two studies completed an assessment of the patient’s ability to climb stairs within 7-10 days post surgery and reported that all patients were able to achieve this task. 19,20 The remaining study reported the follow up range to be between 3 and 48 months post surgery. 3
Walking
Two studies reported a neutral association between gait and VL flap use. 3,19 Patients were found to have no functional impairment when walking. Both studies used the post-operative surgeon assessment to determine this finding. Details are not given regarding the specific functional tests that were used.
Activities of daily living
One study reported there was no association between VL flap use and the patient’s perception regarding any problems that may occur in their daily activities. 18 All patients in this study reported no complaints with activities of daily living with some of these patients residing alone.
Hematoma
One study reported a negative association between VL flap use and the presence of a hematoma on the donor-site thigh. 17 However, this was present in only 2.4% of participants in this study. Time taken to resolve and the impact on function was not reported.
Discussion
This systematic review explored the donor-site morbidity associated with using the VL flap to reconstruct defects of the head and neck. This study reports a neutral association between VL flap use and donor-site morbidity. To our knowledge, the need for further investigation into donor-site morbidity post this type of surgery was currently unknown. This study confirms that further research is required to post-operatively review the functional outcomes (donor-site) following this surgery using more rigorous design methods.
Recent studies have investigated donor-site morbidity of patients undergoing anterolateral thigh flap reconstruction of the head and neck. 21 Seventy percent of patients 21 receiving this type of flap demonstrated a significant decrease in isokinetic knee extensor and flexor strength of the donor leg (P < 0.01), a compensatory significant increase in muscle strength of the unaffected leg (P < 0.05), and decreased sensation in the distribution of the lateral femoral cutaneous nerve. Given that the nerve to vastus lateralis is frequently partially or completely sacrificed during anterolateral thigh flap harvest, it is likely that the VL flap would demonstrate similar functional impairment if more comprehensively assessed. Although the donor site morbidity of the VL flap is reported to be relatively low, it is recognized that there are other thigh muscle flaps commonly used in head and neck reconstruction, such as the gracilis, which have exceedingly low donor site morbidity. 22,23 However, the VL flap is able to reconstruct much larger defects and has a longer pedicle, making it a more versatile option in the head and neck.
Further investigating the donor-site morbidity of VL flap use will serve as a useful comparison and assist head and neck surgeons with their decision-making processes and advice given to patients. As such, further investigation into the effect of VL flap use and donor-site morbidity is justified to inform the need for alternative surgical or rehabilitative options for head and neck patients. Identifying potential complications may assist in the rehabilitation of patients following head and neck surgery through early intervention programs to ensure donor-site morbidity has minimal impact on the health of the patient.
The limitations of this review are the small number of studies available to analyze. There were 7 additional studies that were excluded due to having a sample size of between 5 and 10 participants. 24 –30 However, these studies also reported donor-site morbidity to be low or negligible. All studies in this review were observational in design and lack the rigor of objective testing and advanced statistical analysis thus confirming the need for further investigation.
Conclusion
The literature were systematically reviewed to investigate the association between VL flap use for the reconstruction of head and neck defects and donor-site morbidity. Overall, there was minimal donor-site morbidity reported as a neutral association was found for donor-site leg strength, ability to climb stairs, walking, and activities of daily living. Studies designed with validated objective measures, larger sample sizes and the assessment of a wide range of health outcomes are recommended to further inform appropriate preventative and follow up care options for this group of head and neck patients.
Highlights
Vastus lateralis flap—no effect on leg strength, stair climb, walking, activities
Vastus lateralis flap—minor negative effect on leg sensation and bruising
Further investigation (vastus lateralis flap and donor-site morbidity) justified
Comprehensive assessment required using objective measures and larger sample sizes
The need for additional preventative or follow up care options yet to be determined
Footnotes
Acknowledgment
The authors would like to thank Rachael Blackbourn, Librarian, Wollongong Hospital, Illawarra Shoalhaven Local Health District for her assistance and time given to this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Publication of this article was supported financially from the Illawarra Shoalhaven Local Health District.
