Abstract
Camurati-Engelmann Disease is a rare congenital sclerosing bone dysplasia condition. Affected patients manifest bony abnormalities including thickening of the skull base and orbital bones. The resulting orbital volume reduction associated with this condition can cause exophthalmos, distorting the facial profile. The authors report a 33-year-old man with a diagnosis of Camurati-Engelmann Disease exhibiting exophthalmos who was successfully treated with the insertion of bilateral lateral orbital wall patient specific PEEK implants via a bi-coronal flap approach. This case highlights the novel application of modern cutting-edge technology in the treatment of proptosis in Camurati-Engelmann Disease.
Introduction
Camurati-Engelmann Disease (CED) is a congenital sclerosing bone dysplasia caused by mutations in the gene encoding transforming growth factor beta 1 (TGF-β1). 1 The condition is rare, with just over 300 reported cases. 2 In those affected, bone formation and turnover is altered causing hyperostosis of long bones and diffuse thickening of the skull base. Orbital bones can be affected, resulting in shallow orbits with reduced orbital volume. 3 The resulting clinical exopthalmous is a well-described feature of the condition. 4 We describe a rare case of CED which was successfully treated with bilateral polyetheretherketone (PEEK) implants to restore the orbital volume and resolve exophthalmos. This research adhered to the tenets of the Declaration of Helsinki. Informed consent to publish the photographs was signed by the patient.
Case Report
A 33-year-old man with Camurati-Engelmann Disease was referred to the joint orbital clinic with cosmetic concerns regarding exophthalmos and secondary bilateral epiphora. Previous management had included bilateral lacrimal gland Botulinum toxin injections (5 IU), bilateral lower lid canthoplexy and bilateral lower eyelid dermal filler injections to improve epiphora and the lower eyelid protrusion, without success.
The patient’s disease presented in childhood with lower limb pain, decreased muscle mass and weakness resulting in gait disturbance. By his mid-20s the patient required a wheelchair for mobilization, regular physiotherapy and opioid analgesics for the management of severe pain affecting his lower limbs. The patient was under regular review by the metabolic bone team and treated with long term Prednisolone.
The joint orbital clinic is run by an orbital surgeon and a maxillofacial surgeon experienced in the management of complex congenital deformities. Assessment revealed posteriorly set lateral orbital rims causing bilateral globe prominence. There was associated inferior scleral show and the stretched lower lid was positioned below the globe (belt-under-belly effect), leading to reduced tear clearance and epiphora. CT imaging identified sclerosis and thickening of the skull base with the middle cranial fossa most severely involved. No significant maxillary or mandibular abnormality was noted. Significant orbital bone thickening was demonstrated, with shortening of the lateral orbital wall causing shallow orbits (Figure 1).
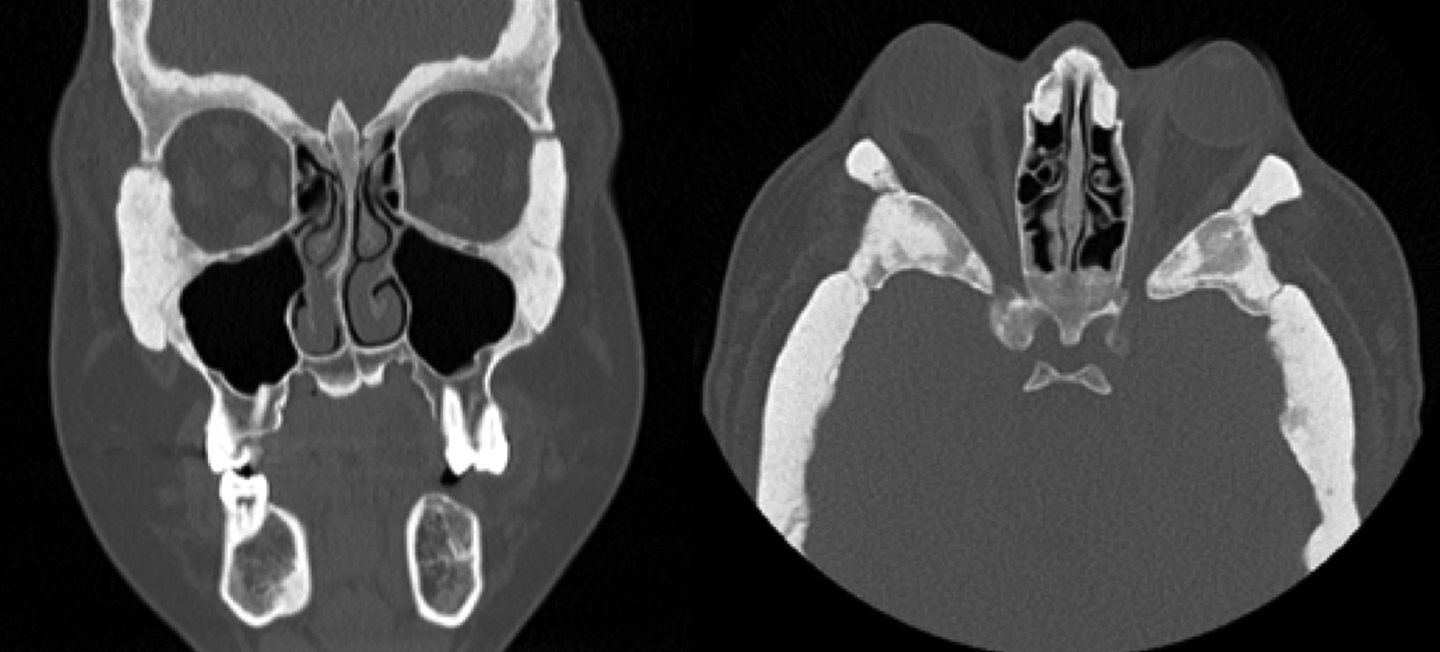
Preoperative CT images of coronal (left) and axial (right) views.
After multi-disciplinary team discussion, bilateral placement of PEEK implants to augment the lateral walls of the orbits was planned. The computer-aided design of the implants was assisted by a clinical engineer and then milled by the manufacturer (DePuy Synthes, Oberdorf, Switzerland). The implants were devised to sit over the lateral rims to improve lateral orbital wall profile and fit comfortably within soft tissue envelope extending the lateral orbital walls by 3.6 mm on the left and by 4.6 mm on the right (Figure 2). The right orbital wall required a greater correction due to an asymmetrically reduced lateral wall projection compared to the left side. Pre and post-operative Hertel exopthalmometer readings are provided in Table 1. Surgical access was performed by raising of a bi-coronal flap, chosen to ensure adequate access for implant placement and avoidance of visible scaring. The implants were seated as planned and anchored with the mid-face plating system (Synthes). At the end of surgery, a double armed 5.0 Vicryl suture was passed from the upper and lower limbs of the lateral canthal tendon onto the periosteum overlying the Whitnall’s tubercle so as to tighten and reposition the lateral canthus in its correct anatomical position 1 mm higher than the medial canthal tendon. The post-operative period was uneventful. The patient retained full facial nerve function, unaltered sensation to the forehead and no post-operative infections or complications. Fundoscopy and ocular motility assessments were normal pre and post-surgery. Orbital volume calculations pre and post-surgery identified an increase of 559 mm2 (left eye) and 592 mm2 (right eye).
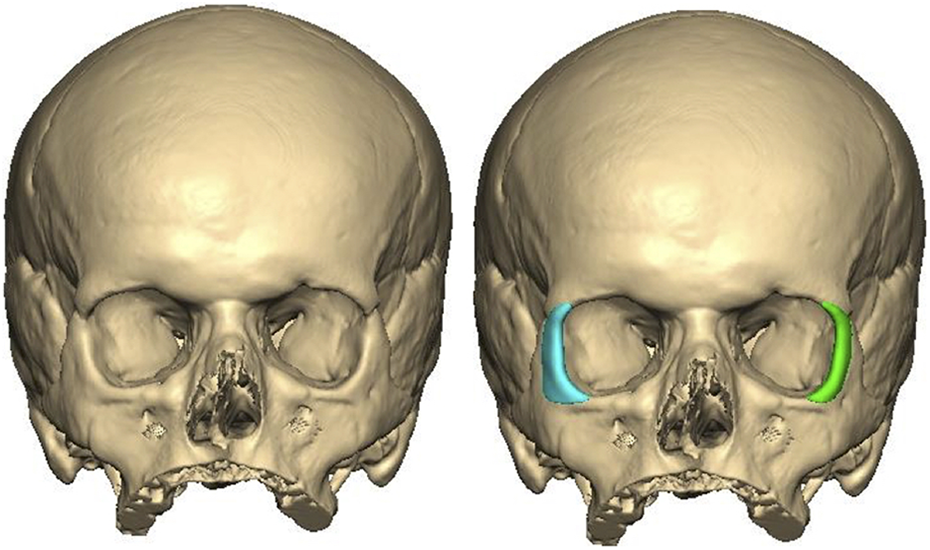
Coronal view CT 3D reconstruction of facial bone profile. Left image shows shallow orbital profile with a relative posterior position of the lateral orbital wall. Right image shows position of patient-specific PEEK implants extending the lateral walls.
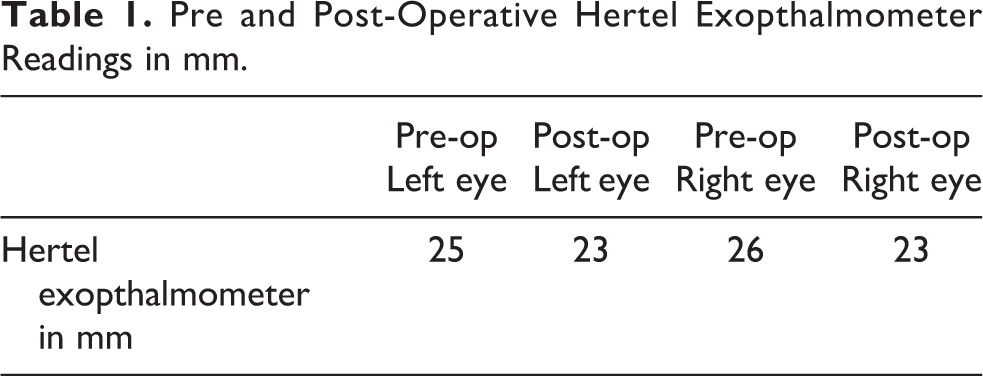
Pre and Post-Operative Hertel Exopthalmometer Readings in mm.

The patient was delighted with the significant improvement to the facial appearance, with reduced proptosis and decreased scleral show (Figure 3 & 4). The epiphora improved, although did not completely resolve, probably associated with nasolacrimal duct stenosis due to his underlying disease. He remains satisfied 1-year post-surgery.
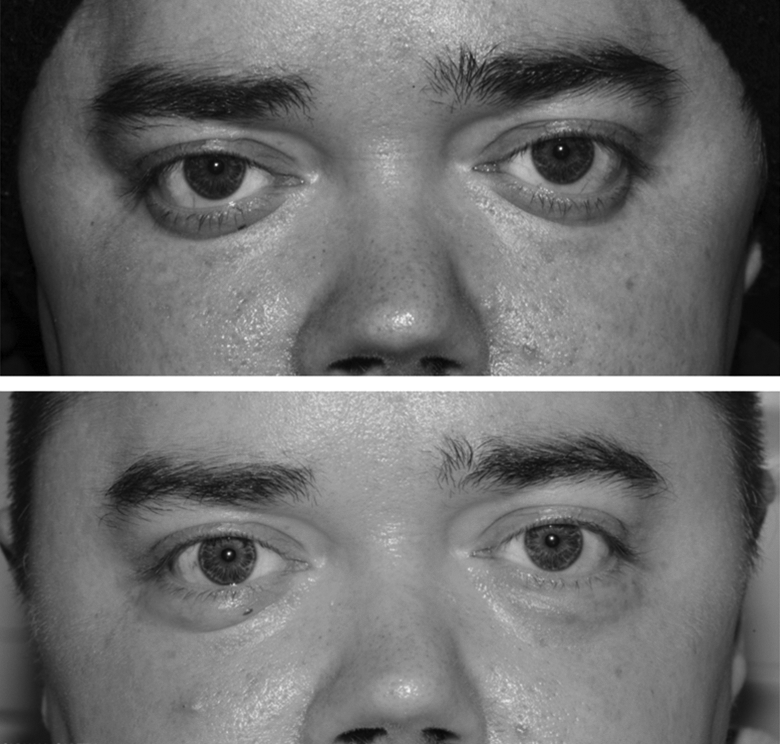
Clinical photographs of the patient (front view). Top image taken pre-surgery. Bottom image taken post-surgery.
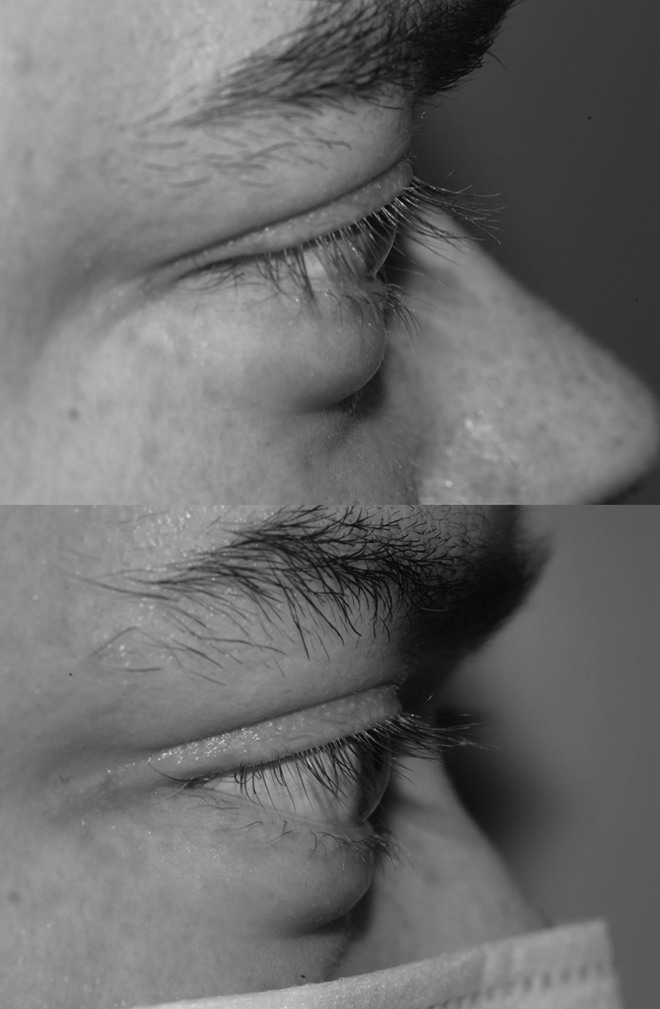
Clinical photographs of the patient (lateral view). Top image taken pre-surgery. Bottom image taken post-surgery.
Discussion
Camurati-Engelmann Disease was first reported in the 1920s. It is a rare congenital sclerosing bone dysplasia caused by mutations in the gene that encodes transforming growth factor-1 (TGF-β1). The gene is located on chromosome 19q13.2, with mutations identified affecting the region between amino acids 218 and 225. 1 There have been just over 300 cases reported, with an estimated frequency of 1:1,000,000. 5 TGF-β1 is an important regulator of the bone remodeling process. Its upregulation in CED affects osteoclast binding and osteoblast stimulation in the bones formed by intra-membranous ossification, including long bone diaphysis and the bones of the skull base. 2 Detailed radiological assessment is essential to diagnosis. Characteristic features include uneven cortical thickening and increased diameter of one or more of the long bones sparing the spine, often symmetrically, and diffuse sclerosis of the base of skull. 6 Presentation is variable, with phenotypical divergence even between family members with the same TGF-β1 mutation. Signs and symptoms may change in affected individuals throughout life. The most common symptom described in over 90% of patients is limb pain, which is often persistent and difficult to control with analgesics. Proximal muscle weakness with accompanying decreased muscle mass can cause a waddling gait. Other associated musculoskeletal problems include kyphosis, scoliosis, flat feet and genua valga. 7
Around 55% of patients demonstrate skull base hyperostosis on imaging. Carlson et al reviewed the prevalence of skull base manifestations among 306 published cases. They found hearing loss (19.0%), headache (10.4%), exophthalmos (8.2%), and frontal bossing (7.2%) to be the most common. 3 Facial nerve palsies and numbness have been described occurring in the fourth to fifth decade caused by bone encroachment and stenosis of associated foramen. 2 Frontal bossing may be present in 7% of cases, caused by hyperostosis of the cranial vault. While dental eruption is usually normal, the mandible can become sclerotic in 25% of patients and palatal exostosis is a common finding. 7 Mandibular and maxillary enlargement is described as a late feature. The mandible is more frequently involved, with the condyle and coronoid process becoming hyperostotic, resulting in reduced mobility and trismus. 8 A combination of raised intracranial pressure, orbital bone overgrowth, and optic canal stenosis can cause vision changes in up to 5.6% of patients with CED, with papilledema demonstrated in 4.6%. 3,9 A single case report exists documenting angioid streaks identified on fundoscopy in a patient with CED. It is likely that this is a coincidental finding rather than related to CED. 10
With regards to orbital involvement, thickening and sclerosis of the orbital bone cause a relative reduction in orbital volume resulting in shallowing of the orbits. 8 Exophthalmos is a commonly reported complication of this condition, as seen in our case. In some instances, progressive proptosis may be the initial presenting manifestation. 4 Although the majority of patients with globe protrusion are asymptomatic, associated eye pain and diplopia secondary to restricted eye movements and a single case of globe subluxation have been reported. 3 In our case, proptosis became more prominent into adulthood. As far as we are aware, this the first time epiphora has been reported in association with this disease.
PEEK is a polyaromatic semi crystalline thermoplastic polymer with chemical formula (–C6H4–O–C6H4–O–C6H4–CO–) first proposed as a material for biomedical application in 1998. 11 Its use in maxillofacial surgery has become widespread in recent years owing to its advantageous properties in the accurate reconstruction of complex craniofacial anatomy. Utilizing computer-aided design (CAD) and computer-aided manufacturing (CAM), PEEK can produce precise patient-specific implants, superior to alternative biomaterials. Studies have shown excellent postoperative stability, cosmetic results, fewer alterations at implantation and reduced donor site morbidity. 12 Additionally, PEEK has proven biocompatibility with innate antioxidant properties, promoting active wound healing. 13
Alternative biomaterials include autologous bone, titanium and high-density polyethylene (Medpour), which are all well-established orbital floor reconstruction materials. Autologous bone grafting is considered the reference standard and has excellent biocompatibility and low infection rates. 14 However, lacking digital precision contorting, high latent resorption risk and potential for donor site morbidity represent major disadvantages. Titanium implants have excellent biocompatibility and high osseointegration. Although patient-specific implants can be fabricated, adjustment at the time of surgery is very difficult. Other disadvantages include thermal sensitivity and higher infection rates. 15 Medpour is non-resorbable and easy to handle and adjust. However, it demonstrates radiolucency on imaging, risks of infection and rates of orbital implant exposure in the region of 4.5%. 16
There exist no randomized control trials of treatments and no consensus management guidelines for CED. Treatment with non-steroidal anti-inflammatory drugs and corticosteroids have been reported to provide effective symptomatic relief of bone pain. There is however no clear evidence to suggest that steroids are effective at reducing bone formation or reverse sclerosis. 1 Long-term use of corticosteroids is not advisable. Although the angiotensin-II receptor antagonist Losartan has been proposed as an alternative to steroids due to downregulation of TGFβ1, there is conflicting evidence for its effectiveness at controlling symptoms. 5 Treatment with bisphosphonates remains disputed. Some studies have demonstrated reduced biochemical markers of bone turnover and improved symptoms, with other studies demonstrating no effect. 17,18
Surgical options for correction of raised intercranial pressure and papilledema include cranial volume expansion with craniectomy and titanium mesh cranioplasty. 19 Symptomatic skull base involvement may require cranial nerve decompression surgery. This surgery is challenging due to the loss of landmarks and post-surgical relapse remains problematic. 3
Our case is the first time in the literature that PEEK patient-specific lateral orbital wall implants have been used to correct exophthalmos associated with CED. In our case, augmentation of the orbits successfully improved the facial profile, correcting the relative eye protrusion and reduced scleral show without requiring bone removal. Although the epiphora was not completely resolved, the patient noted significant cosmetic benefit, improving his quality of life.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
