Abstract
We report a case of orbital Rosai–Dorfman disease in a 45-year-old man who presented with exophthalmos as the first symptom for 6 months. He did not have any itching, photophobia, tears, headache, dizziness, nausea, vomiting, or other symptoms of discomfort. A soft tissue mass was found in the left orbital by a magnetic resonance imaging scan, and we were able to diagnose lymphoma before the operation. Rosai–Dorfman disease was finally diagnosed by surgical biopsy. The patient received radiotherapy. At a 1-year follow-up, there was no sign of a residual tumor. Rosai–Dorfman disease is easily misdiagnosed and accurate diagnosis of this condition is important for choosing the best treatment plan.
Introduction
Rosai–Dorfman disease (RDD) is a rare, idiopathic, non-Langerhans cell histiocytosis of unknown etiology. RDD is characterized by fever, painless lymphadenopathy, cervical lymph nodes as the best site of occurrence, and often bilateral involvement at the same time. Approximately 43% of cases of RDD are extranodal, including the nasal cavity and paranasal sinuses, respiratory tract, skin, and central nervous system.1–5 A total of 10% of RDD cases involve the orbit, but orbital involvement alone is rare.6–8 RDD is similar to lymphoma, histiocytosis, and lacrimal gland tumors.1,9–12
Accurate diagnosis of RDD is helpful for choosing a treatment plan. At present, a variety of treatments have been proposed for RDD, including steroid therapy, chemotherapy, radiotherapy, surgery, and a combination of these treatments. However, the best treatment for RDD has not yet been established. We report a case of orbital RDD in a 42-year-old man who was initially misdiagnosed.
Case report
This study was approved by the Second Xiangya Hospital of Central South University Medical Ethics Committee review board. Informed written consent was obtained from the patient for publication of this case report and accompanying images.
A 45-year-old man was admitted to hospital with discovery of a left orbital mass for 6 months. He experienced swelling of the left eye without obvious inducement and left proptosis for 6 months. There was no itching, photophobia, tears, headache, dizziness, nausea, vomiting, or other symptoms of discomfort. An ophthalmological examination showed left infraorbital and interorbital soft masses, with slight tenderness. Ocular pressure was 17 mmHg in the right eye and 22 mmHg in the left eye. Measurement of exophthalmos was 15 mm in the left eye, internal rotation was −1°, and the bulbar conjunctiva was mixed with hyperemia. Magnetic resonance imaging (MRI) showed that the left orbital soft tissue mass, which extended to the nasal cavity, measured 3.4 × 2.4 × 3.7 cm. The mass was isointense on T1- and T2-weighted images, and it had obvious and homogenous enhancement (Figure 1a–d). These findings suggested the diagnosis of lymphoma or inflammatory pseudotumor. Under local anesthesia, the left orbital mass was partly removed and biopsied. A yellow mass in the lower orbit was found during the operation. The edge of the mass was unclear and lobulated, the texture was medium, and approximately a 2.0 × 2.0-cm2 mass was removed for pathological examination. A histopathological examination showed patchy staining of tissue cells, which stretched into lymphocytes and plasma cells. The cytoplasm was rich and transparent, with a large nucleus (Figure 1e, f). Immunohistochemistry showed that large histiocytes reacted strongly and positively to S-100 protein and CD68, weakly and positively to CD4, and negatively to CD1α.
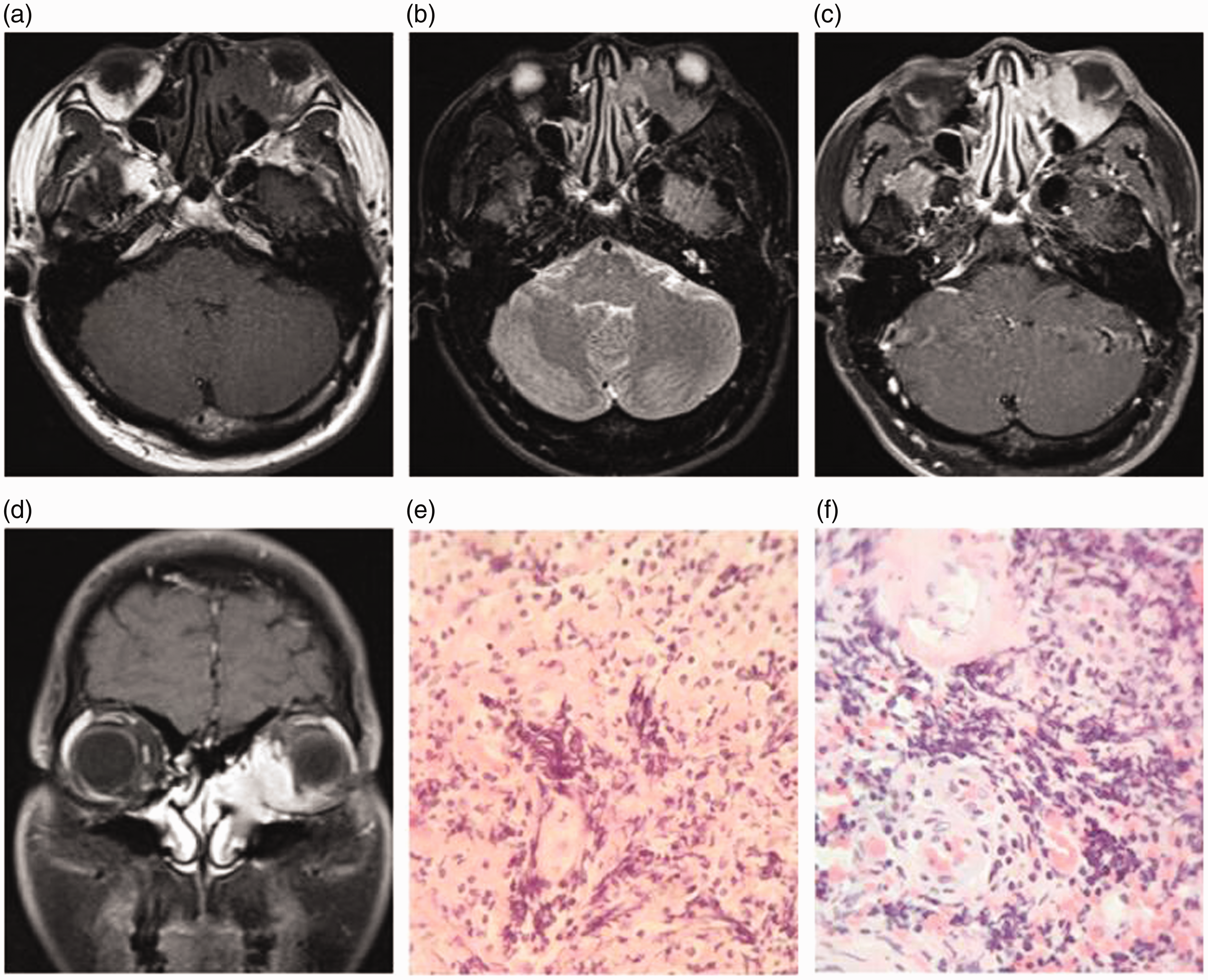
A contrast-enhanced magnetic resonance imaging scan of a 45-year-old male patient shows an irregular mass located in the left orbital (a–d). Magnetic resonance imaging shows a low signal on T-weighted imaging and isointensity on T2-weighted imaging (a, b), and shows a homogenous mass in the left orbit extending to the nasal cavity. A pathological examination (e, f) shows infiltrates composed of histiocytes, lymphocytes, and plasma cells (×400).
After definite diagnosis by biopsy, our patient received adjuvant radiotherapy. The target area included left nasal cavity lesions and left orbital lesions, and the radiation dose was 2 Gy in a fraction, 5 fractions a week. The total dose reached 20 Gy in 10 fractions. The left eyeball and lens were limited by the normal dose of radiation. After radiotherapy, a few symptoms appeared, such as photophobia and tears, and these disappeared after treatment. An ophthalmological examination showed left interorbital soft masses less than 1 cm, with slight exophthalmos. There was no considerable increase in the masses during a 1-year follow-up.
Discussion
RDD, also called sinus histiocytosis with massive lymphadenopathy, was first reported in 1965. In 1969. 13 Rosai and Dorfman 13 described the clinical and pathological features of this disease in detail and called it RDD. At present, the exact pathogenesis of RDD is unclear. Some studies have shown that RDD may be related to human herpesvirus 6 and Epstein–Barr virus infection. 14 RDD can be divided into lymph node, extranodal, and mixed types according to the location of the lesion, among which the extranodal type and mixed type are rare.15,16
Orbital involvement in RDD has rarely been reported alone, and it is usually unilateral and rarely can be bilateral,6–8,16 but its imaging features have been poorly described. Xu et al. 15 reported a case of RDD with lacrimal gland involvement. In this previous case, MRI showed a mass with intermediate signal intensity on T1- and T2-weighted images and intense homogeneous enhancement, which is similar to our case. Other cases in Xu et al.’s report, 15 such as cervical, nasal cavity, or paranasal sinus involvement, showed some different intensity in T2-weighted imaging, while all of them showed homogeneous enhancement. Therefore, homogeneous enhancement might be a feature of RDD. Xu et al. 15 showed that the orbital mass of the patient was confirmed as RDD, and it was the extranodal type. The imaging features of RDD were mostly equal or slightly high-density soft tissue masses on a plain scan, most of them had a clear boundary, and absorption and thinning were observed in the adjacent bone. Localized bone destruction was observed in a few cases, with homogeneous enhancement. Orbital RDD needs to be differentiated from inflammatory pseudotumor, Langerhans histiocytosis, and lymphoma. 17
The diagnosis of RDD mainly depends on the pathology. Pathologically, RDD is characterized by proliferation of different forms of histiocytes, infiltration of a large number of mature plasma cells and lymphocytes, and typical phagocytic lymphocytes in the cytoplasm. Immunohistochemical staining of S-100 protein and CD68 is important for diagnosis, but CD1α, which is often present in Langerhans’ cell histiocytosis, should be negative.
Our patient was a male adult, who was initially diagnosed with lymphoma or inflammatory pseudotumor by an MRI scan. A biopsy should be considered when orbital masses cannot be diagnosed. Bijlsma et al. 18 demonstrated that a biopsy is safe in not delaying diagnosis of malignancies and efficient in providing a rapid diagnosis. Extranodal RDD has a good prognosis and mostly presents as a benign process. Surgical resection is the main choice for RDD, and should be supplemented by steroids, radiotherapy, or chemotherapy. After definite diagnosis by biopsy, our patient received adjuvant radiotherapy. After radiotherapy, a few symptoms appeared, but these disappeared after treatment.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
