Abstract
A gunshot wound to the mandible frequently creates a comminuted fracture that can be debilitating for the patient and challenging for the surgeon. In some instances, immediate open reduction and rigid fixation is not possible, and closed reduction with intermaxillary fixation is employed. This may lead to non-union or mal-union of the segments. This case report describes the management of mal-union of bilateral comminuted mandibular angle fractures secondary to a gunshot wound injury. The mandibular fractures were repaired using virtually planned patient specific reconstruction plates that included a specially designed crib cage to contain a bone graft. A cellular bone allograft—Vivigen (DePuy Synthes, Warsaw, IN)—was chosen as the bone grafting material. The patient was followed up for 7 months with normal functional status and mouth opening and without pain or signs of infection. This report demonstrates that using a virtually planned crib cage plate with cellular bone allograft can optimize surgical repair and bony healing of comminuted mandible fractures.
Keywords
Introduction
Virtual surgical planning (VSP) allows surgeons to visualize intra-operative steps and predicted post-operative results and to design customized hardware that can be used in the surgery. 1 Such level of planning is beneficial in taking care of patients with a gunshot wound (GSW) to the face due to distortion of local anatomy and elevated risk of complications.
A GSW to the mandible can result in a severely comminuted fracture due to its high kinetic energy and the projectile’s ability to fragment upon bony impact. 2,3 This often leads to avulsion of soft tissue and loss of continuity of hard tissue causing a significant functional deficiency for the patient. 4 The projectile devitalizes muscle and pulls skin, clothing, and bacteria into the tissue, facilitating infection, and the bony fragments created upon impact are also pulled along the projectile’s path. 3 Some complications commonly associated with GSW to the mandible include mal-union, non-union, devitalization of the bone, and infection. 5
When treating a mandibular non-union with a continuity defect, the use of bone grafts should be considered. Autografts are the gold standard as they can provide all 3 aspects of bone formation—osteoconduction, osteoinduction and osteogenicity. 6 In contrast, bone allografts typically lose osteogenicity as they undergo decellularization processes, such as irradiation, sonication and chemical treatment to reduce its immunogenicity. 7,8 Cellular bone allograft (CBA), however, is a new alternative to traditional bone allograft in that it retains mesenchymal stem cells (MSC) which have the potential to differentiate into bone, cartilage or fat cells. However, cartilage and fat cells are not wanted for bony fusion. Vivigen® (DePuy Synthes, Warsaw, IN) is a new type of CBA which contains bone-lineage committed cells instead of MSC, so its cells will transform into only bone cells.
Several authors have described using CBA for spine and other orthopedic surgeries, but reports on CBA use for mandibular reconstruction appear to be sparse. This article depicts a case of using VSP, patient specific implants and CBA to treat a patient with non-union of bilateral mandibular fractures from a GSW to the face after an initial closed reduction with maxillomandibular fixation (CR-MMF) failed to address the fracture.
Case Presentation
A 72-year-old male presented to the emergency department (ED) after 3 self-inflicted gunshot wounds to his face. The patient was intubated for airway protection en-route to the ED. Upon arrival, the trauma team stabilized and performed initial workup for the patient. Computed tomography (CT) of the face revealed comminuted bilateral mandibular fractures along with bilateral comminuted maxillary sinus fractures, maxillary alveolar fracture, and bilateral orbital floor fractures. (Figure 1(A) to (C)).
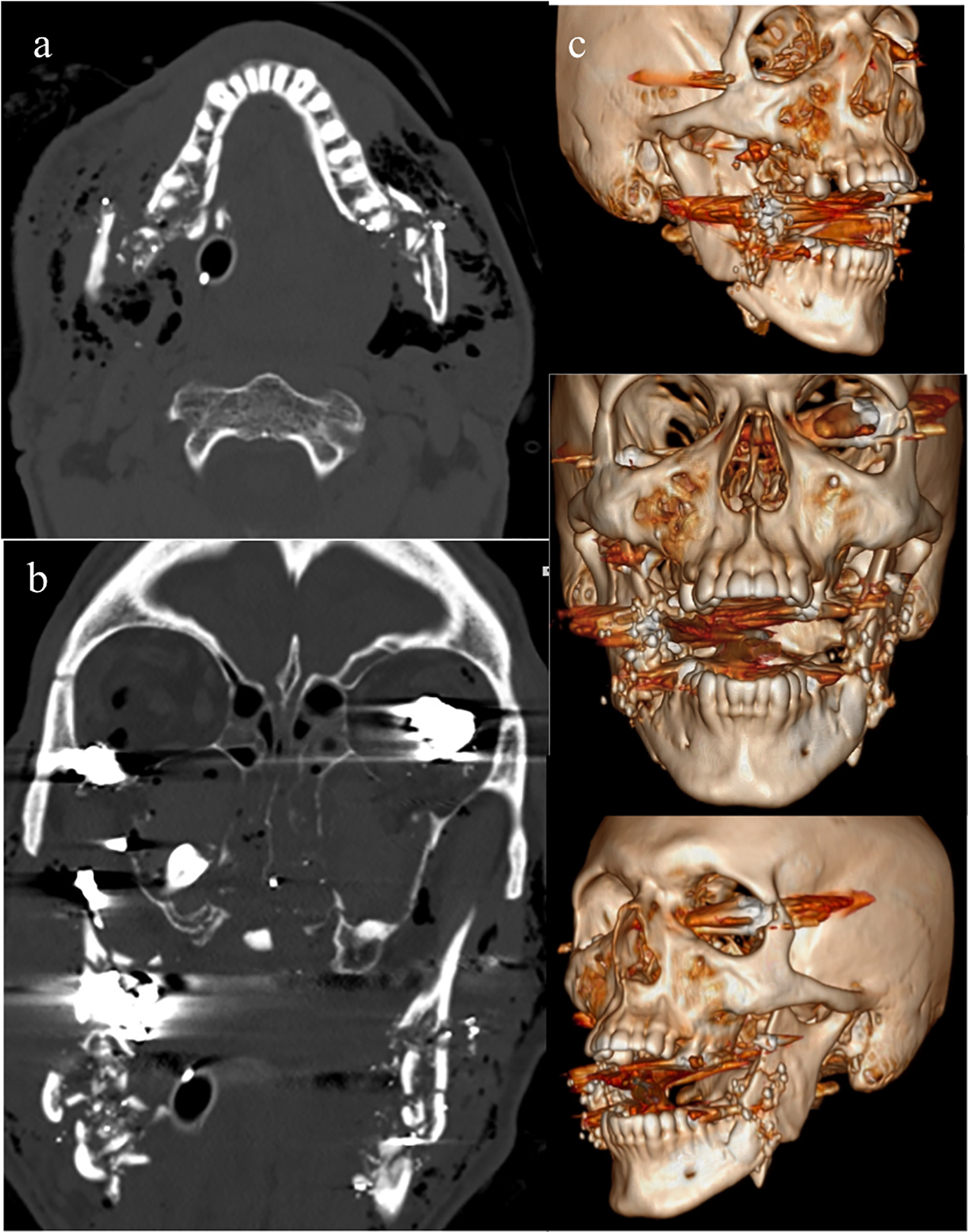
Initial CT (A) axial view showing comminuted bilateral mandibular fractures. (B) Coronal view showing bilateral mandibular angle fractures. (C) 3D reconstruction showing the mandibular fractures.
The patient’s physical exam revealed 2 entry wounds in the right submandibular area and left cheek without exit wounds, a bilateral mandibular deformity with multiple step-offs, partial tongue and left buccal mucosa avulsion with controlled hemostasis, and a stable maxilla. While he sustained multiple facial injuries, this report will focus on the management of his mandible fractures.
The Oral & Maxillofacial Surgery team performed CR-MMF for the mandible fractures as the initial management. The patient was followed up in the clinic 7 weeks later. MMF was released and a non-union of the bilateral mandibular angle fractures was noted with mobile segments. No signs of infection were present. At this point, it was determined that the patient would require an open reduction and internal fixation (ORIF) of the mandible with a bone graft for bony defect. The MMF was reapplied, and a 1 mm thin-sliced CT of the face was obtained to perform Virtual Surgical Planning (Figure 2).
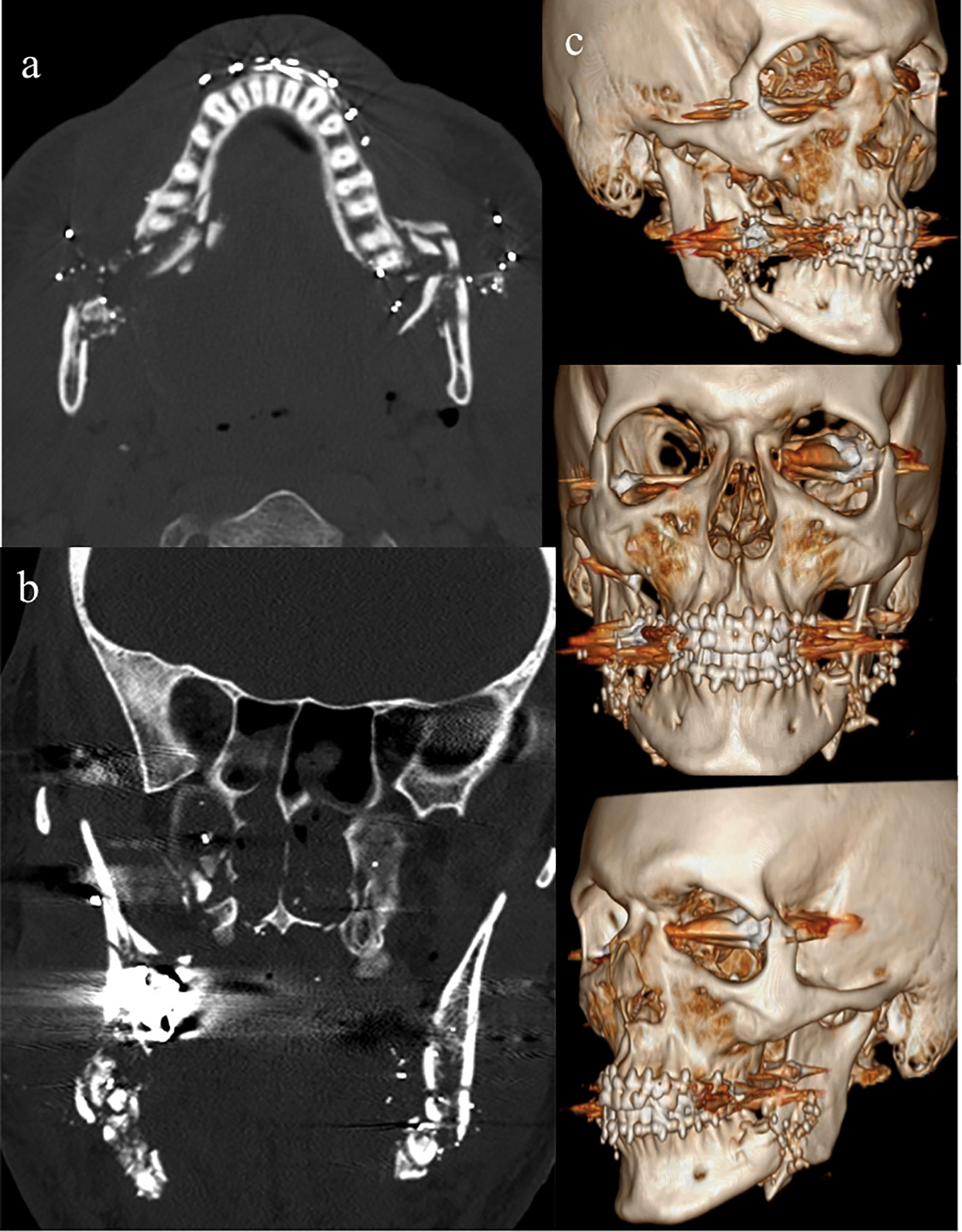
CT of the face with MMF for VSP (A) axial view showing comminuted mandibular fractures with arch bars. (B) Coronal view showing mandibular fractures. (C) 3D reconstruction with arch bars and patient in MMF.
The patient was in a good occlusion, which assisted in positioning the distal segment. Proximal segments (ramus) were rotated to the correct position, and debris from comminuted pieces was virtually removed, establishing a gap between the repositioned segments (Figure 3). A mirror image of the intact left ramus was used to virtually reduce the fracture on the right ramus and create a custom plate that would stabilize the anterior segment of the right ramus that contains the coronoid process to the posterior segment (Figure 4). Then, reconstruction plates for the bilateral mandibular angles were planned using a combined feature of crib cages to hold the bone graft (Figure 5). Sites for screws to fixate the plates were virtually determined. Based on this position, drilling guides were designed to anatomically fit the fracture segments (Figure 6). These patient specific guides and plates were then printed with a 3D-printer using pure titanium dust.
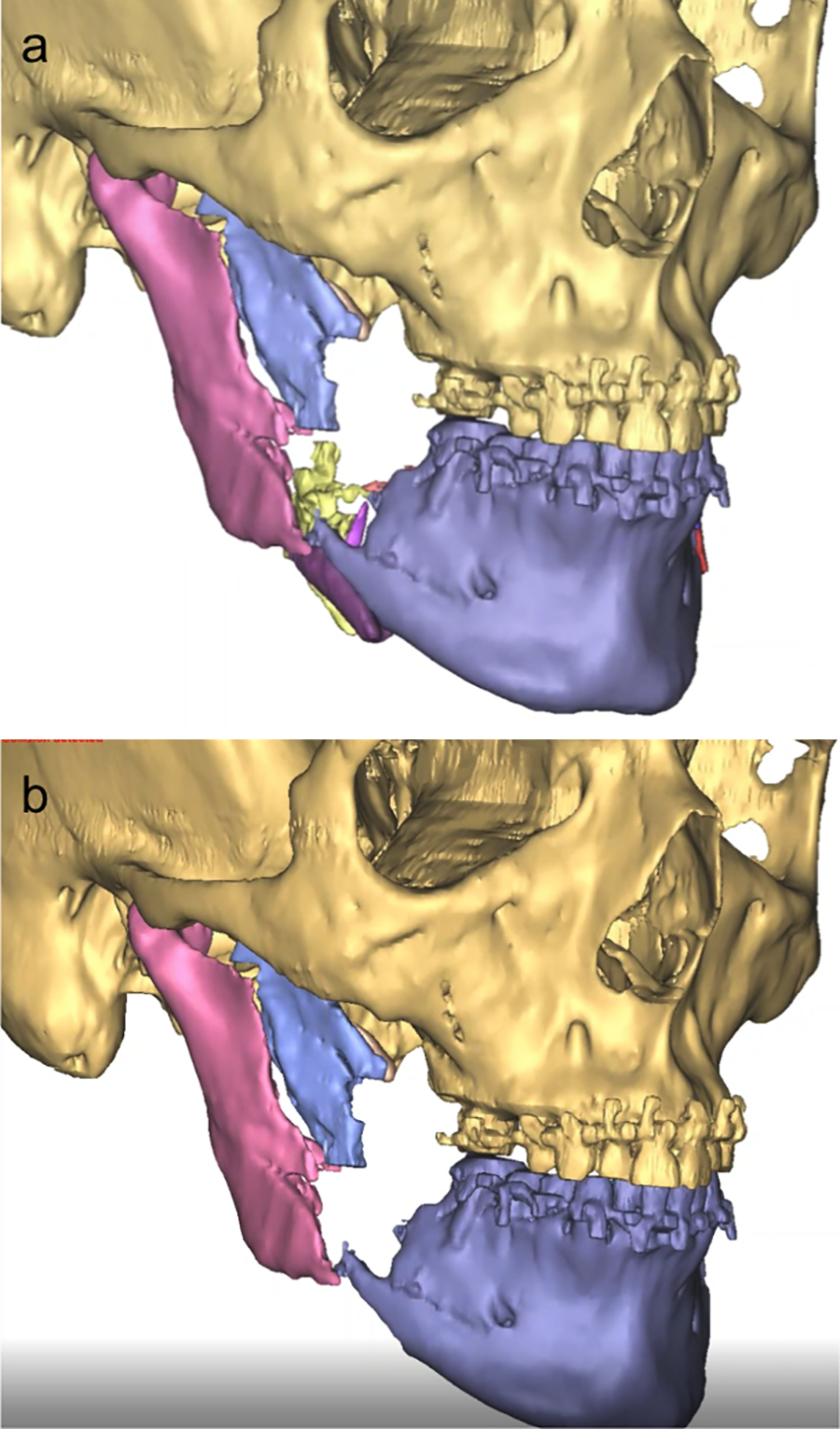
VSP session (A) right mandible with bone debris (B) right mandible with bone debris virtually removed.
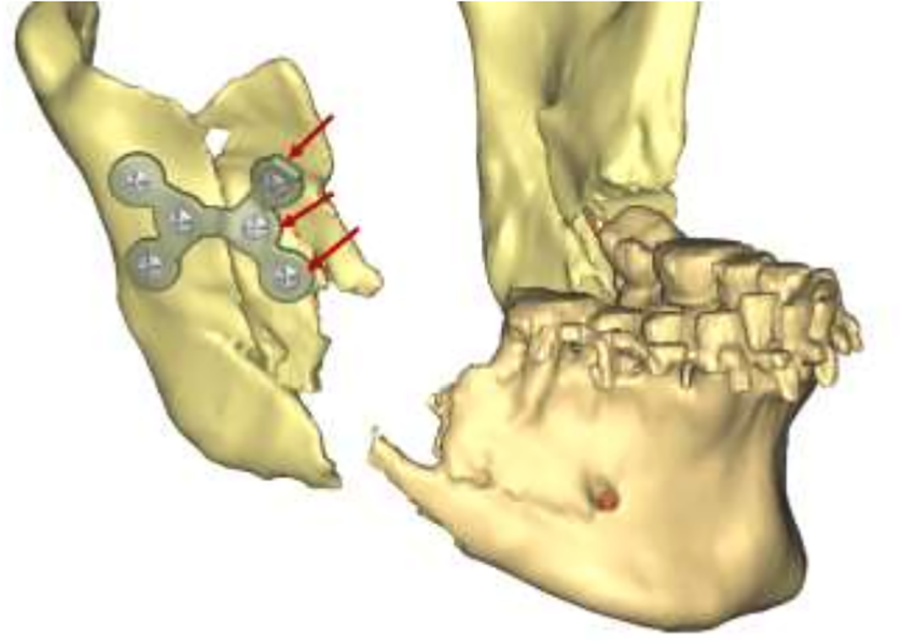
Plate to fixate the right ascending ramus.
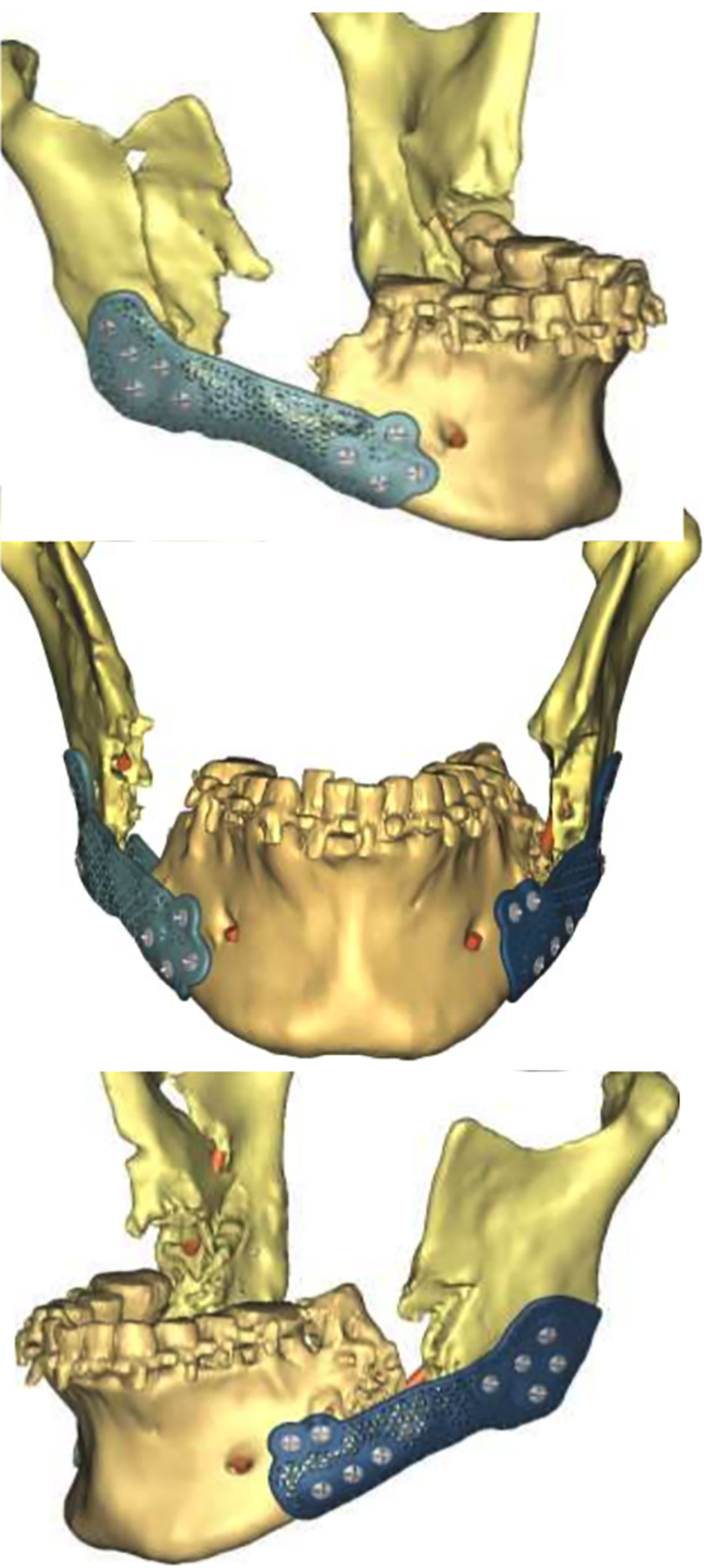
VSP workup. Right-frontal-left views of mandibular crib cage plates.
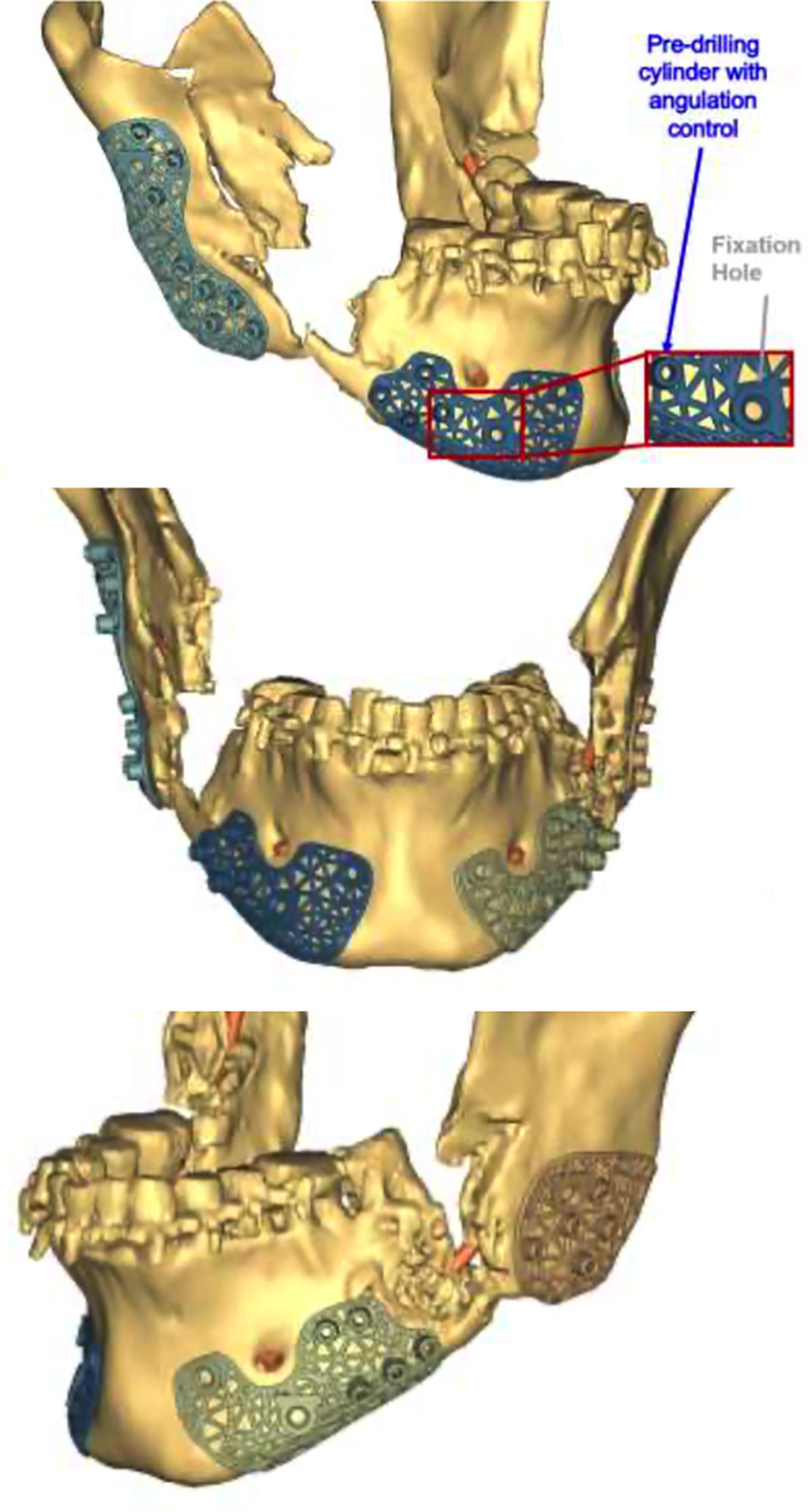
VSP workup. Right-frontal-left views of mandibular drilling guides.
Operative Management
In the operating room, a bilateral submandibular approach was employed to gain access to the mandible. Both sides were debrided, removing small bony spicules and obtaining healthy bleeding bones on both sides of the bony discontinuity. The patient had no intraoral communication from the surgical site. Proximal and distal segments of the bilateral mandible were drilled using the drilling guide as per the VSP (Figure 7). Vivigen was packed into the crib cage (Figure 8). Then, the crib cage plates were applied, and both proximal and distal segments of bilateral mandible fit precisely into the plates, allowing for a predictable reduction of the fractures with the bone graft inside the crib cages (Figure 9). The incisions were then closed in layers. The patient was then discharged after 2 nights of observation at the hospital with chlorhexidine mouth rinse and 7-day course of augmentin.
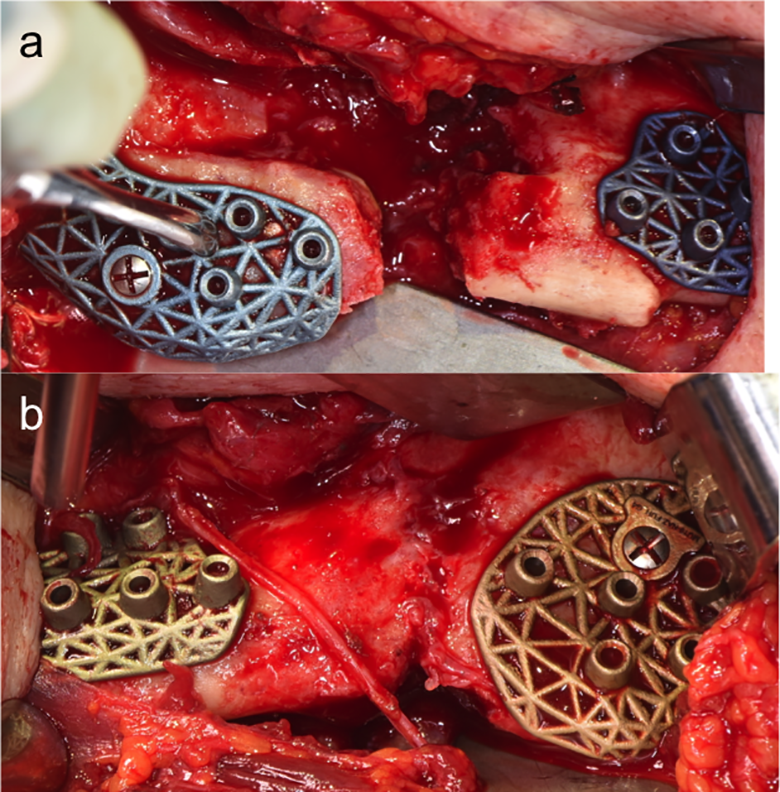
(A) Drilling guides on the right mandible. (B) Drilling guides on the left mandible.
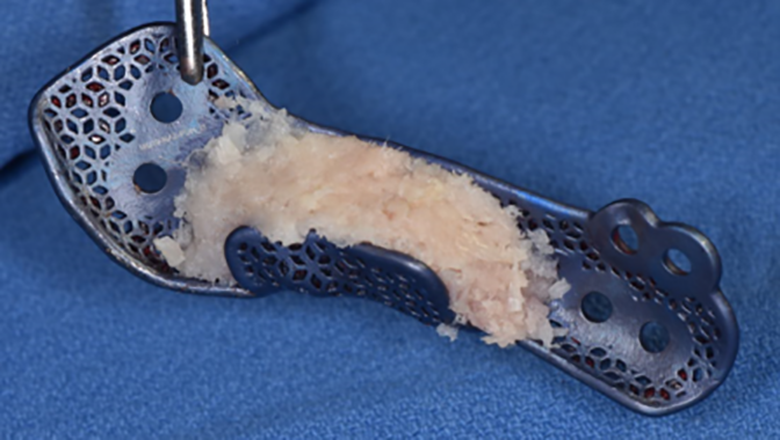
Vivigen packed in left mandibular reconstruction plate prior to adapting the plate.
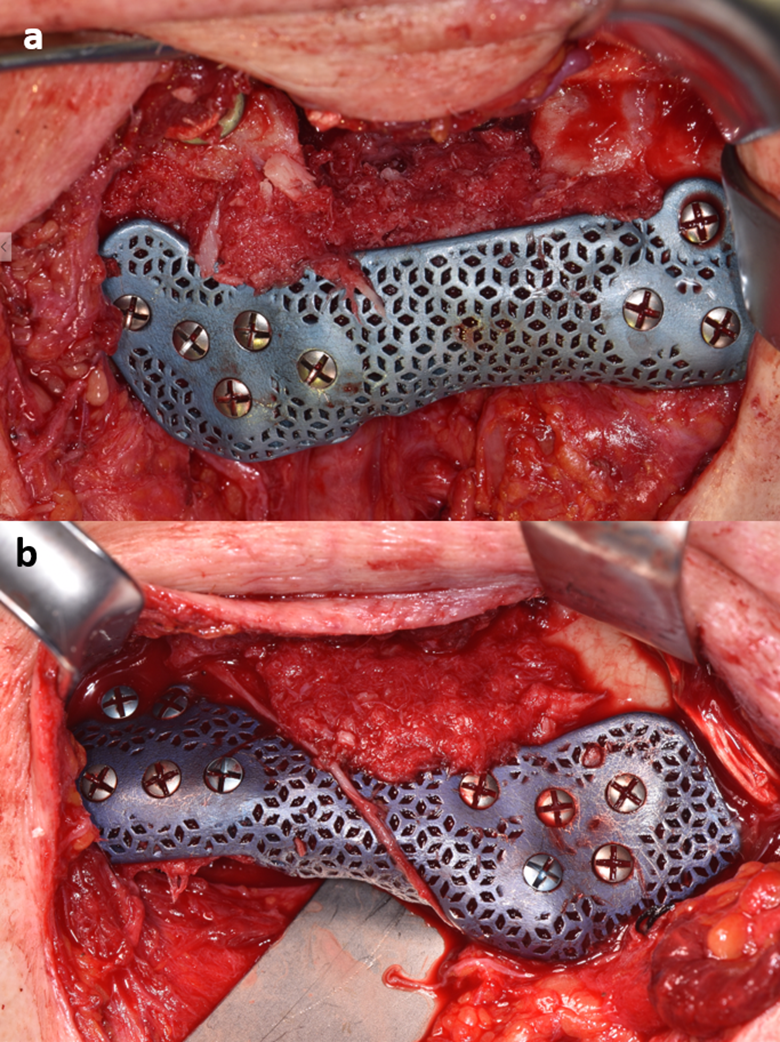
(A) Right mandibular reconstruction plate in situ. (B) Left mandibular reconstruction plate in situ.
Post-operative Follow-up
Post-operative imaging showed well-adapted bilateral reconstruction plates containing Vivigen (Figure 10A to C). At 2-week follow-up, the patient had a maximum incisal opening (MIO) of 15 mm, but denied having any pain nor difficulty eating regular food. The operated sites were not mobile to palpation, and without step-offs along the inferior borders. At 2-month follow-up, the patient’s MIO was increased to 28 mm with normal, pain-free functioning. Physiotherapy with tongue blades and local heat were applied. The patient no longer wished to physically come in for an appointment due to concerns for the coronavirus pandemic but agreed to intermittent virtual follow-ups. The patient was virtually followed up 7 months later, and he reported having no pain and tolerating a regular diet without issues.
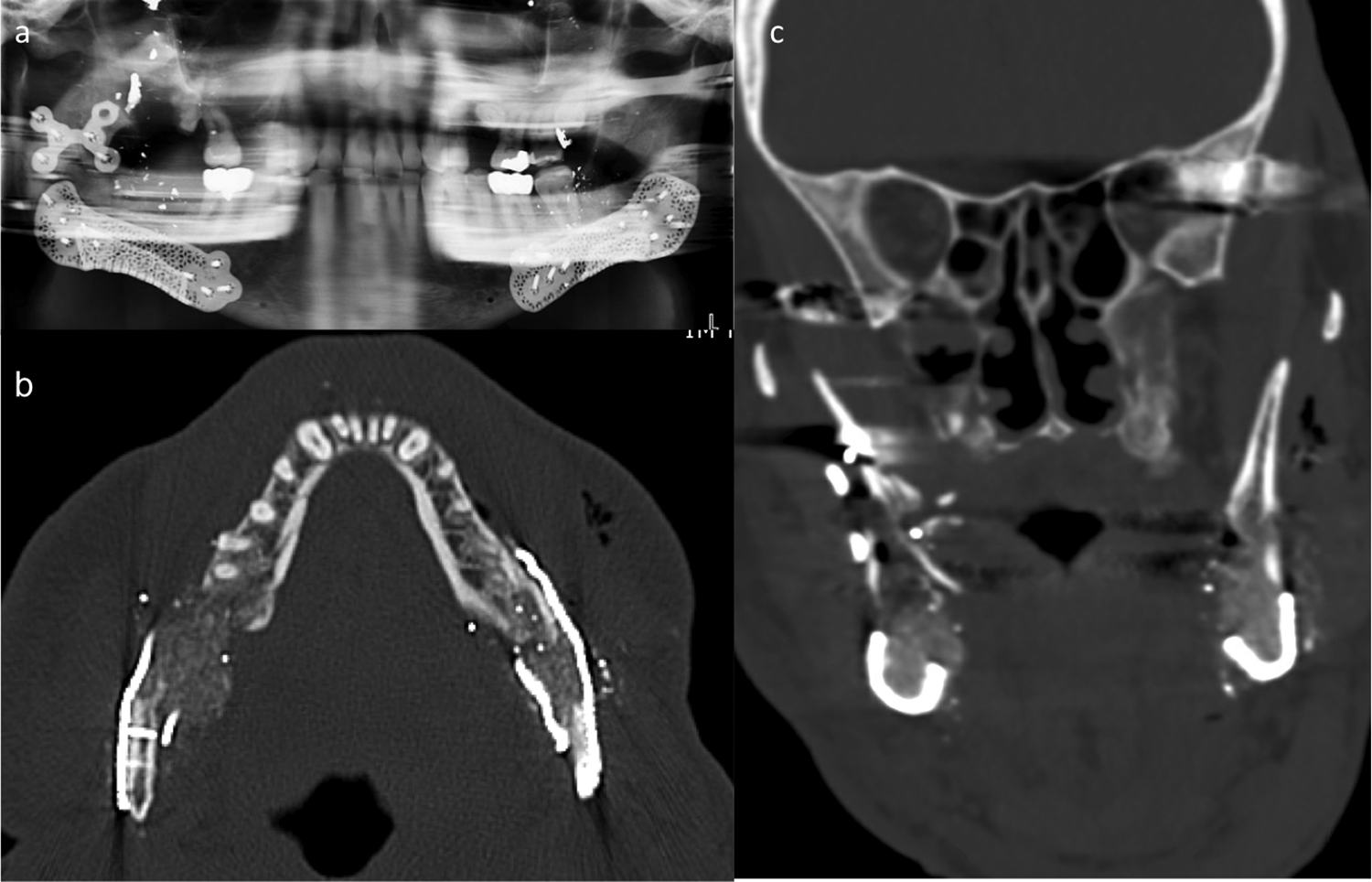
(A) Post-operative orthopantomogram. (B) Axial view of CT of the face with reconstruction plates and bone graft material; (C) Coronal view of CT of the face with crib cage containing bone graft material.
Discussion
A GSW to the mandible can create comminuted fractures that are prone to complications. 9 VSP can facilitate reconstruction of complex comminuted defects with virtual manipulation of injured sites prior to surgery. 10 –13 For instance, a dislocated condyle can be virtually brought back to the correct position, a mandible with widened width can be manipulated to its proper width, and a fracture with a continuity defect or with a displaced segment can be realigned with a flush inferior border. 11 Additionally, VSP can allow the creation of a mirror image of the uninjured side for planning purposes. In the case above, VSP was used with this method to reconstruct the patient’s fractured right ramus. It was also used to prefabricate individualized mandibular reconstruction places with crib cage plates with which CBA was used to unite the bilateral proximal and distal mandibular segments into an anatomically ideal position. This precise fit allowed the surgical team to reconstruct the gap in the mandible in a more predictable manner.
The benefits of using VSP are clear. The VSP allows the surgeon to visualize the anatomy pre-operatively in 3-dimensional view and reduce intra-operative errors. 14 The same data gathered for VSP can also be used to create stereolithographic models for additional visualization, pre-operative plate bending and determination of the patient’s projection. 12
El-Gengehi et al found that post-operative imaging of mandibular fractures repaired using VSP accurately matched forecasted outcomes. 15 In addition, with the availability of pre-fabricated, pre-bent implants, OR time can be decreased, reducing the duration of general anesthesia for the patients. 10 Geriatric patients, like our patient in this report, tend to have impaired cardiac, respiratory, gastrointestinal and endocrine systems that affect their peri-operative outcome. 16 As such, it is preferable to reduce the surgical time to reduce the peri-anesthetic complications. 17
Using VSP also has some disadvantages. While the cost of VSP varies widely, it often adds thousands of dollars to the patient’s care. 13,18 The decrease in cost due to the decrease in OR time often does not offset the cost of VSP itself. 13 Use of VSP is frequently not an option for time-sensitive cases as virtual planning and delivering pre-fabricated plates can take up to 14 days in some cases. 14 Additionally, VSP is a multi-step process including acquiring data, communicating with the software engineer, and pre-fabricating hardware. Any inaccuracy incurred at any of these steps may lead to less than ideal surgical outcome. 14
In the case above, the mandibular defects were approximately 1.9 cm on the right and 1.5 cm in length on the left. As the defect sizes were smaller than 6 cm, we decided to use non-vascularized bone graft. 19 In our case, VSP allowed us to create accurate plates with crib cages to hold the CBA. Efforts had been made previously to contain particulate graft in mandibular reconstruction. Dacron-urethane tray, a malleable stock tray that is manufactured in the shape of a mandible that can be bent and cut to fit the mandible, and titanium mesh tray, another form of a stock tray with mesh bed that can harbor particulate bone graft and can be manipulated to fit the mandibular defect, had been used previously. 20 –23 These trays required manipulation intra-operatively that could be cumbersome at times and might lead to lack of rigidity needed to bear the mandibular load. Customized rigid titanium crib cages, however, combined the features of patient specific reconstruction plates and bone graft bed that enabled us to pack CBA right in the bony discontinuity with ease while reconstructing the mandibular continuity defect simultaneously.
Carlock et al show that iliac crest bone graft is equally effective in elderly and non-elderly patients in treating fracture non-union. 24 However, iliac crest bone graft may cause donor site morbidities, such as impaired gait, potential fracture, pelvic instability, and paresthesia in up to 30% of patients and also lead to increased operative time and blood loss that we wanted to avoid in our elderly patient. 25,26 Considering the patient’s mechanism of self-injury and underlying depression, we also wanted to make the patient as comfortable as possible after surgery, so we decided to use bone allograft instead of autograft.
Unlike traditional bone allograft which does not have osteogenic potential, CBA, with its retained MSC, has osteogenic capability. 25 Gonshor et al looked into the maxillary sinus augmentation using CBA and conventional allografts and showed that the sinus augmentation done using CBA had a statistically significant increase in vital bone content (32.5% ± 6.8%) compared to the one done with conventional allograft (18.3% ± 10.6%). 27 However, Myerson et al compared the radiographic evidence of bony fusion of subtalar arthrodesis completed with CBA and autograft, and concluded that the autograft group showed higher rate of radiographic fusion than the one completed with CBA. Of note, both groups had favorable clinical outcomes. 28
MSC have the potential to differentiate into bone, cartilage, or fat cells, the latter 2 of which are unwanted when trying to achieve bony fusion. 29 Osteogenic potential of Vivigen had been improved from conventional CBA in that it retains bone-lineage committed cells instead of MSC so that the cells in Vivigen will become bone cells, not cartilage or fat cells. 25 Shahrdar et al looked at bone formation after Vivigen use in hip arthroplasty and noted that Vivigen use led to rapid bone formation that exceeded the rate of usual new bone formation and did not elicit an immune response. 6
Conclusions
Through this case, we hope to illustrate how the combination of VSP (Virtual Surgical Planning), PSI (patient specific implants) and Cellular bone allograft (CBA) can facilitate surgical reconstruction of comminuted mandibular fracture and bone graft placement. By combining features of reconstruction plates and crib cage for bone graft placement with VSP, reconstruction becomes more predictable, and the time spent in the operating room can be reduced. Also, this case demonstrates that Vivigen, with its bone-lineage committed cells as opposed to traditional CBA with MSC, can be a helpful tool for reconstruction of mandibular non-union or for the patients at risk for non-union. To the best of our knowledge, there has been no published article of Vivigen use in mandibular reconstruction nor one comparing Vivigen to an autograft. This could be an area of research in the future.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
