Abstract
Study Design
Case report
Objective
To present an alternative method to traditional iodoform gauze packing for the management of soft tissue defects. Hydrogel dressings are modern packing materials that can be used to hold negative space, provide moisture to the wound, and absorb wound exudates.
Methods
This report describes the case of a 28-year-old patient who suffered facial gunshot injuries, including an approximately 3-centimeter diameter avulsion of soft tissue at the posterior right cheek. After wound debridement and irrigation, Intrasite™ hydrogel was used as a wound dressing to fill the soft tissue defect. The injectable and slowly resorbable material was added as needed by the patient for eight weeks until wound healing.
Results
Wound healing by secondary intention was achieved with acceptable esthetic outcomes while avoiding traditional dressing changes.
Conclusions
Facial gunshot wounds present a multitude of challenges particularly when complex soft tissue avulsions are involved. The surgeon must adequately debride these wounds and manage soft tissue healing to prevent infection and ensure satisfactory aesthetic and functional outcomes. Long-term patient compliance is equally important; however, dressing changes are often difficult and uncomfortable for the patient. The use of an injectable hydrogel dressing facilitated soft tissue healing while affording greater comfort to the patient compared with traditional dressing changes, thus likely improving compliance during the crucial healing period.
Background
The management of facial gunshot wounds with complex soft tissue avulsion has traditionally involved packing a strip of gauze into the wound with daily dressing changes using sequentially shorter lengths of gauze.1-4 For more than one hundred years, this method has been used to promote healing by secondary intention and prevent infection, but it is technique sensitive and relies on patient compliance after patient discharge. Newer dressing materials and alternative techniques such as negative pressure wound therapy may provide advantages in wound care and healing that traditional gauze does not offer.3-8 However, treatment with more modern packing materials is often overlooked in oral and maxillofacial surgery and there is a lack of research involving these materials for the management of facial wounds.
This case report presents the use of Intrasite™ hydrogel wound dressing (Smith+Nephew, Andover, MA) for the treatment of avulsed soft tissues following a facial gunshot wound. Intrasite™ is a non-adherent amorphous cross-linked hydrogel dressing containing propylene glycol that provides hydration and support to the injured tissues and absorbs wound exudates.
9
Intrasite™ hydrogel is indicated for the treatment of superficial burns, abrasions, and lacerations, as well as deeper defects such as pressure and venous ulcers. The product is injectable using a disposable application cartridge that is available in various volumes (Figure 1). Compared to the traditional gauze approach, viscous hydrogel dressings may promote an environment more conducive to wound healing by secondary intention because it provides moisture, holds negative space, and stimulates the formation of microvasculature in the injured tissues.7,8,10,11 Additionally, because Intrasite™ is resorbable and can be easily reapplied, it offers many advantages for patient satisfaction and compliance during the post-operative care period. Intrasite™ hydrogel application cartridge.
Report of Case
A 28-year-old male patient presented to the emergency department with a gunshot wound to the right midface resulting in an open comminuted fracture of the right zygomaticomaxillary complex (ZMC) and associated complex avulsed soft tissue injuries. The patient also suffered gunshot wounds to the right temporal and occipital scalp, base of posterior neck, and left posterior shoulder. The type of weapon and caliber of the projectiles used is unknown. Clinical examination showed an approximately 5-centimeter stellate laceration at the bullet entry wound in the right infraorbital region involving the lower eyelid and an approximately 3-centimeter diameter avulsion of soft tissue at the exit wound in the posterior right cheek. There was a significant decrease in facial width due to loss of malar projection. Hypoglobus and enophthalmos of the right eye were noted, consistent with injury to the orbital floor. The right pupil was not reactive to light, but the globe and lens appeared undamaged and extraocular movements were intact. The ophthalmology service was consulted due to an injury of the right lower eyelid involving the canalicular system.
A computed tomography (CT) scan demonstrated an underlying acute nondisplaced transverse fracture of the right temporal bone and an acute comminuted ZMC fracture with infraorbital nerve involvement (Figure 2). Retained bullet fragments and bone spicules were noted in the right ZMC, periorbital and extraconal soft tissues, right maxillary sinus, right posterior nasal cavity, and along the right nasal choana. Moderate extraconal orbital emphysema was noted. No retrobulbar hematoma or intraconal retained hyperdense foreign body were noted. The right inferior rectus was displaced inferiorly towards the right orbital floor defect. Three-dimensional reconstruction of the computed tomography scan showing an acute comminuted fracture of the right zygomaticomaxillary complex with retained bullet fragments and bone spicules embedded in the soft tissues.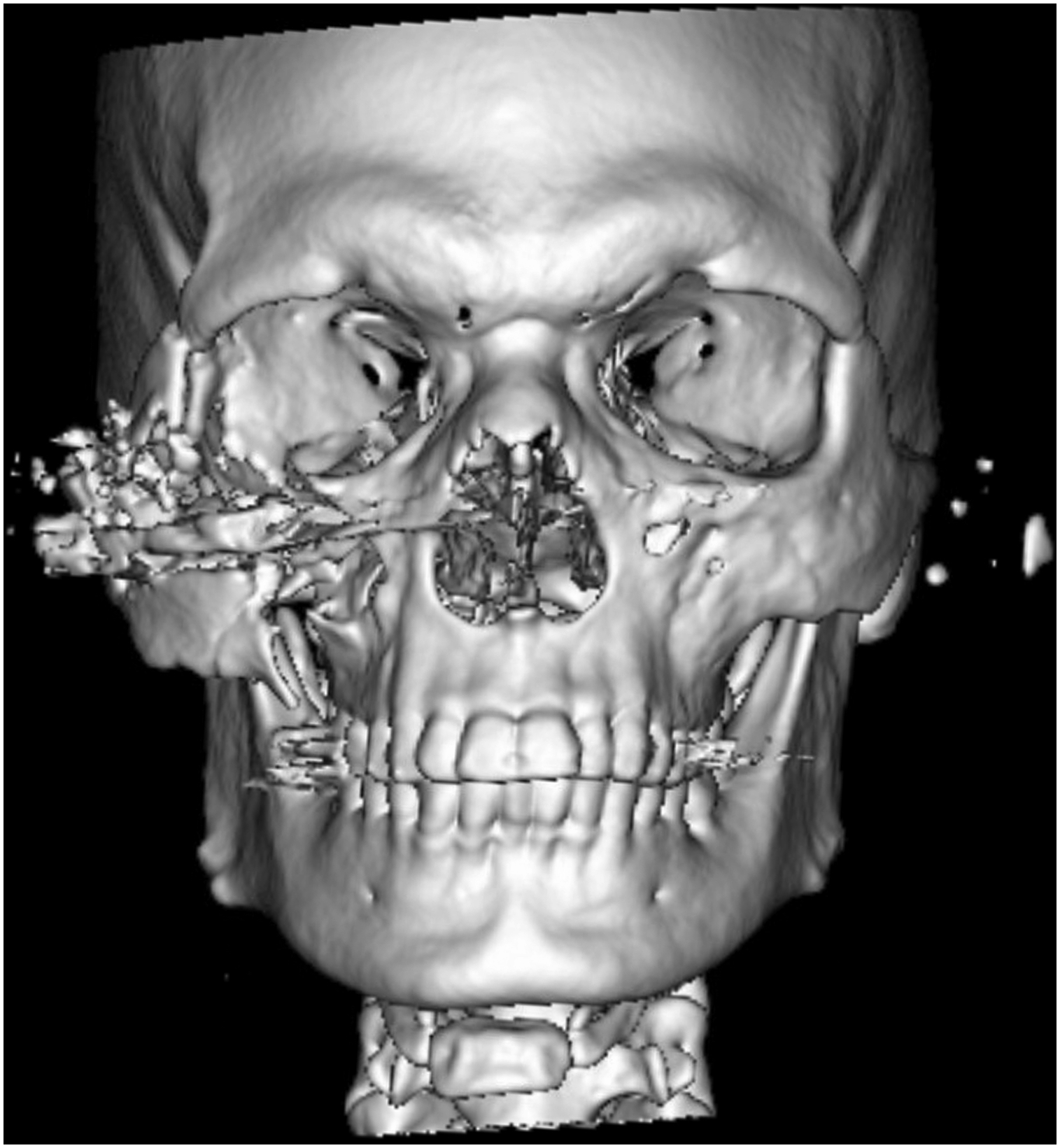
Immediate management in the emergency department involved removal of superficial bullet fragments, wound irrigation with sterile saline, and packing of the posterior wound with iodoform gauze. The patient was admitted and scheduled for formal wound washout and debridement in the operating room. The ophthalmology service performed closure of the full thickness right lower eyelid laceration and repair of the canalicular system. Two days after the injury, the patient was taken to the operating room for irrigation and debridement under general anesthesia. Multiple small bone and bullet fragments were removed from the wound, which was again copiously irrigated with saline solution containing bacitracin. The wound was noted to be hemostatic, and 1% silver sulfadiazine cream was applied to the wound margins. Intrasite™ amorphous hydrogel was injected into the wound to fill the entire cavity until flush with the skin, and a wound dressing was applied. The patient was discharged from hospital the following day. Daily wound care instructions were to remove the outer protective dressing to evaluate the wound, gently rinse the wound with sterile saline, apply antibiotic cream to the wound periphery, inject Intrasite™ hydrogel dressing as needed to keep it flush with the surrounding skin, and to apply a clean wound dressing. Additionally, the patient was instructed to always keep the wound dry.
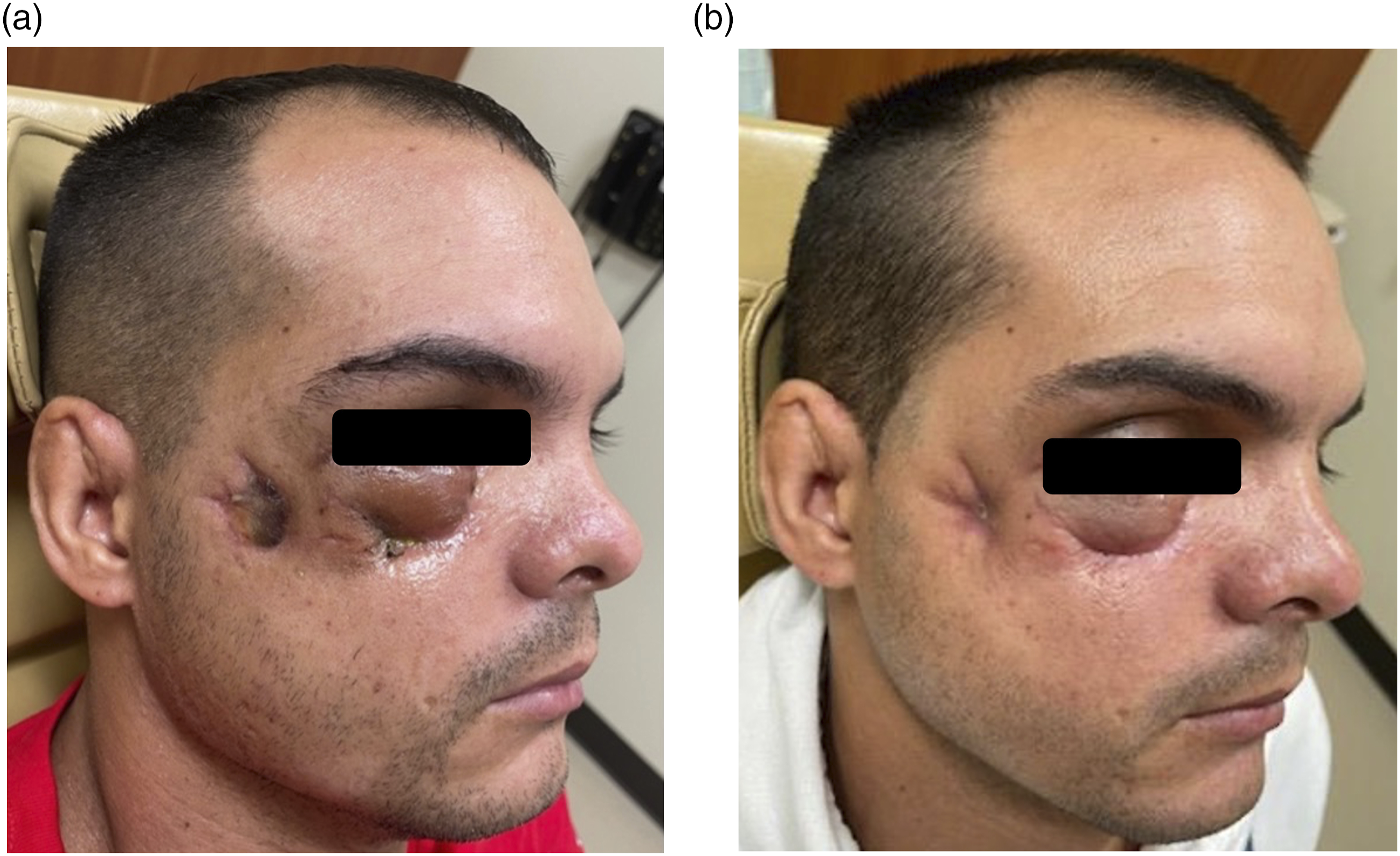
The patient was followed weekly in clinic for one month, then monthly for three months. During this period, he reported full compliance with discharge instructions and daily wound care and noted a gradual return of sensation in the distribution of the right infraorbital nerve. Clinical examinations revealed progressive healing by secondary intention and continued absence of infection. Intrasite™ hydrogel dressing was reapplied as needed per the above protocol (Figure 3). Upon completion of the Intrasite™ hydrogel therapy eight weeks postoperatively, the soft tissue defect was healed via secondary intention (Figure 4). Clinical photographs during the 1-week follow-up appointment (A) prior to reapplication of Intrasite™ hydrogel, showing the soft tissue avulsion defect of the posterior right cheek, the repaired stellate laceration of the right lower eyelid, and right periorbital edema and ecchymosis; (B) application of Intrasite™ hydrogel into the soft tissue avulsion defect of the posterior right cheek; (C) completed application of Intrasite™ hydrogel within the soft tissue avulsion defect of the posterior right cheek until flush with the surrounding skin and application of 1% silver sulfadiazine cream to the wound periphery. Clinical photographs during the (A) 3-week follow-up appointment and (B) 8-week follow-up appointment on completion of Intrasite™ hydrogel therapy, showing progressive healing by secondary intention of the soft tissue avulsion defect of the posterior right cheek.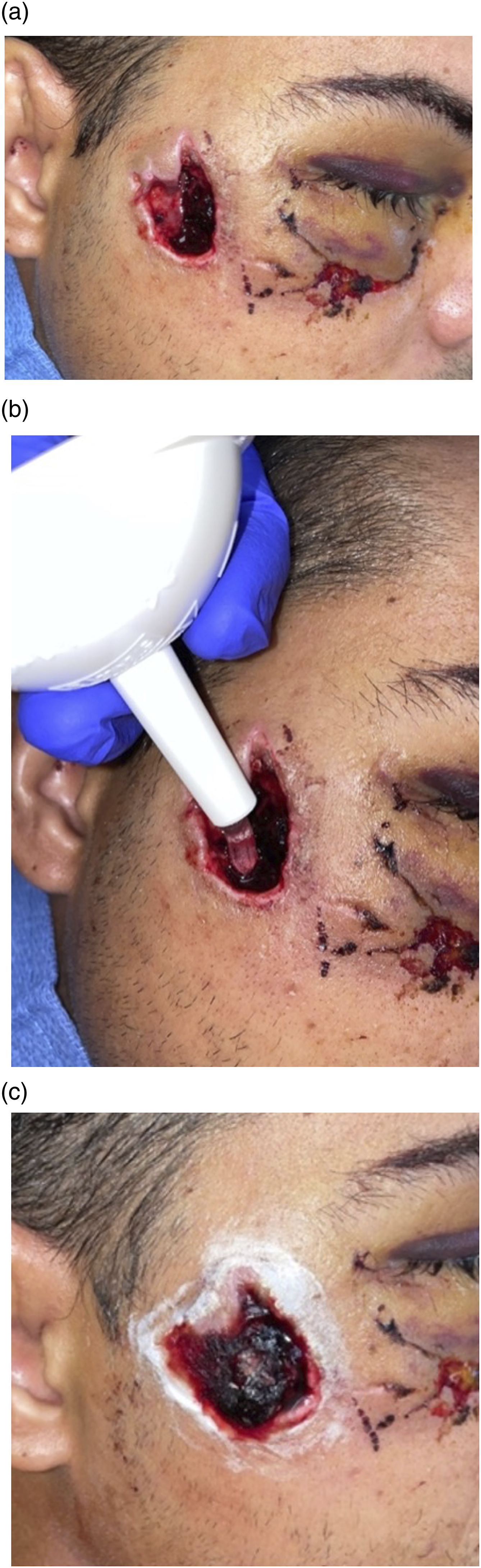
Six months after the injury, the patient underwent hard tissue reconstruction of the right ZMC and orbital floor with custom hardware to address the loss of malar projection and hypoglobus and enophthalmos of the right eye (Figure 5). Clinical photograph taken seven months after the injury and three weeks after reconstruction of the right ZMC and orbital floor with custom hardware, showing healing of the soft tissue avulsion injury and improvement to the contour of the midface.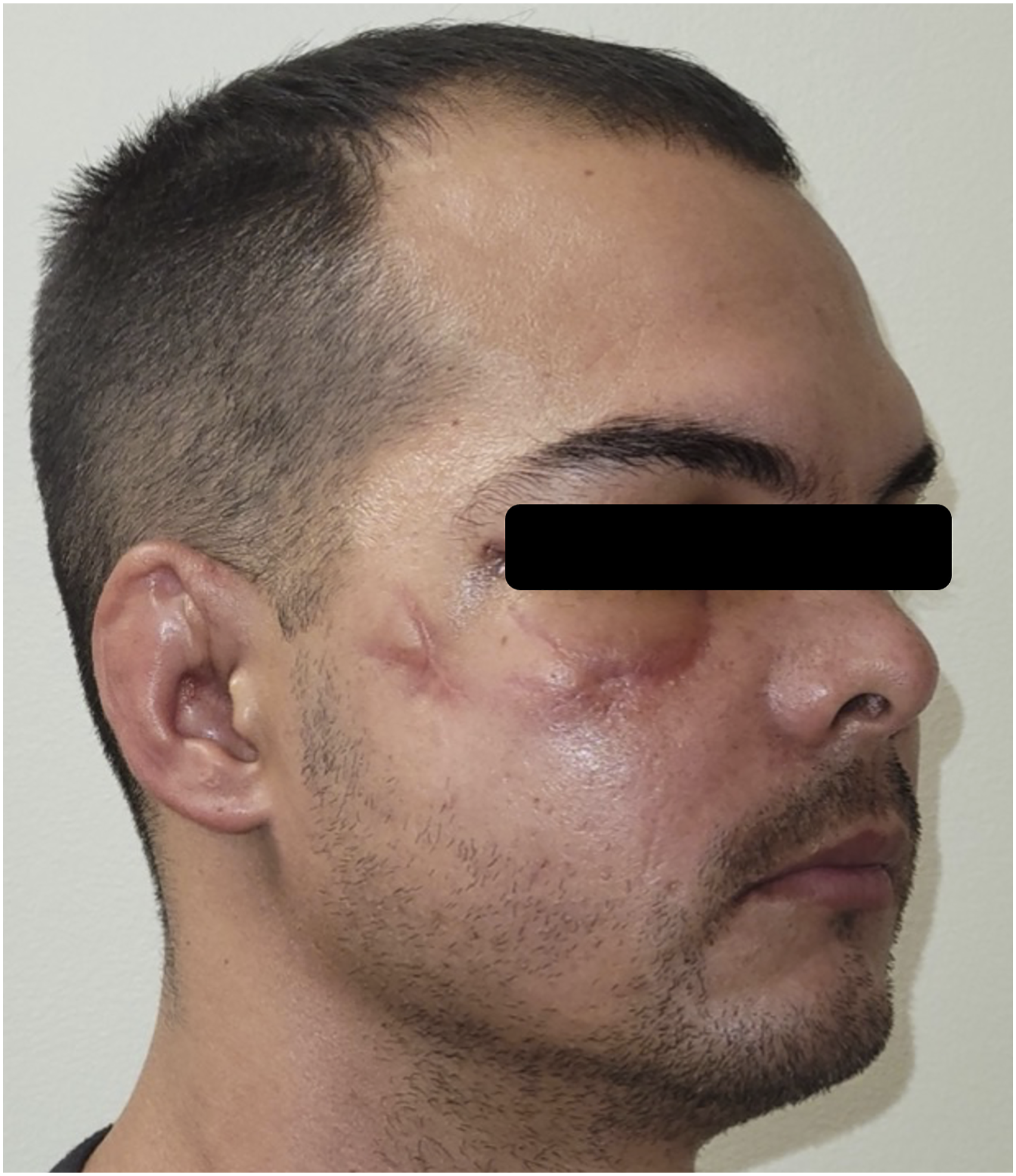
Discussion
Complex facial gunshot wounds commonly present with significant soft tissue defects of both aesthetic and functional concern. 2 With the many challenges that arise with facial gunshot wounds, it is important to optimize the sequence of surgical interventions, appropriate soft tissue management, and long-term patient compliance in wound care. 12 Because ballistic injuries resulting in soft tissue defects often present with tissue necrosis and a high susceptibility to infection, these injuries require thorough debridement and careful packing to optimize tissue healing.2,5,12,13 Tissue avulsion injuries must often be allowed to heal by secondary intention, where the maintenance of tissue moisture and support become imperative.5,12
The traditional approach to the repair of avulsed facial soft tissue wounds is iodoform gauze packing, which has been used since at least the First World War. Newer packing materials and approaches are often overlooked in favor of traditional gauze, despite research demonstrating that traditional gauze has been associated with prolonged nursing time and patient dissatisfaction due to pain and difficulty during dressing changes.5,6 There is also a lack of evidence to show that traditional gauze packing is more conducive to wound healing. Traditional gauze has the advantages of being readily available and low in cost, though one study found hydrogels to be more cost effective overall when considering time required to change dressings and to perform wound debridement, and the amount of material needed. 5
A relatively new technique for wound management is negative pressure wound therapy, which involves mechanical tension applied by a vacuum over polyurethane or polyvinyl wound dressings. While there is support for this method for the treatment open wound, a recent review found no clear difference between negative pressure wound therapy and other treatment modalities in duration of treatment, risk of infection, pain, and other adverse events. 14 Another study cautions the use of negative pressure wound therapy in wounds with poor or compromised vascularity, 15 and this type of treatment may also be associated with painful dressing changes and skin irritation. 16
There are many different types of dressings, each with its indications, advantages, and disadvantages.3-8,17 In general, superficial wounds are typically managed with traditional woven gauze, which can be medicated or impregnated with various substances, or covered with semi-permeable dressings in the form of a film or containing foam or hydrocolloid materials. Deeper wounds with soft tissue defects can be packed with traditional gauze, alginate, or hydrogel dressings, and the above-mentioned negative pressure wound therapy can also be used. Since most of these dressing types must be changed daily to maintain tissue moisture and prevent infection, patient compliance is crucial in attaining good aesthetic and functional outcomes. A Cochrane review concluded that traditional gauze was associated with greater pain and discomfort for the patient but could not identify improved treatment outcomes with the more advanced dressing types. 15
Hydrogel dressings have recently gained support in general surgery for the treatment of chronic wounds with soft tissue defects, such as pressure ulcers. These biocompatible materials provide constant moisture to the wound and its edges and can absorb wound exudates. The amorphous and porous nature of hydrogel materials allows oxygen diffusion and provides a suitable environment for microvascular ingrowth and cell proliferation, but consequently results in low mechanical strength and the need for a secondary dressing.10,11,17 Additionally, because hydrogel dressings lack antimicrobial properties, an antibiotic ointment or cream such as 1% silver sulfadiazine must be applied to the wound periphery. Hydrogel dressings are therefore not indicated for wounds with large amounts of exudate or in the presence of infection. 5 Furthermore, multiple reviews have failed to identify studies demonstrating superior wound healing with the use of hydrogel dressings in diabetic foot ulcers and pressure ulcers.18,19
There are many forms of hydrogel dressings and skin replacement materials. This case report demonstrates the use of Intrasite™, an amorphous gel that can be injected into a soft tissue defect to protect and facilitate wound closure via secondary intention. 9 Intrasite™ hydrogel can be added as needed as it slowly resorbs, making it a convenient treatment option because it eliminates the need for daily replacement of packing when using traditional packing strips. The patient is instructed to gently rinse the wound with sterile saline, apply antibiotic cream to the wound periphery, add enough Intrasite™ hydrogel to keep the dressing flush with the skin surrounding the wound, then cover with a wound dressing for protection. Wound care with hydrogel dressing therefore offers greater efficiency and improved comfort for the patient compared with traditional gauze packing.
Intrasite™ hydrogel dressing could be an attractive option during the acute treatment of complex facial gunshot wounds with tissue avulsion. Its physical and chemical properties allow for the efficient addition of hydrogel packing and may provide a better environment for wound healing when compared with traditional gauze packing.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
