Abstract
Myositis Ossificans Traumatica (MOT) is a rare condition that affects soft tissues after a trauma and hardly affects the mastication muscles. The occurrence in the temporal muscle is uncommon, and trismus is the most prevalent symptom. The diagnosis of the pathology is sufficiently obtained through the collection of clinical history, physical and imaging exams. Differential diagnosis is important mainly to rule out more aggressive diseases, such as osteosarcoma. Treatment becomes more invasive as the ossification matures, and resection of structures adjacent to the tumor, such as coronoidectomy, is well indicated for promoting good results on the mouth opening amplitude. However, to maintain this amplitude, aggressive myofunctional therapy is required. Nevertheless, the literature has no well-defined protocol for this physiotherapy. Therefore, this article reports a rare case of MOT in the temporal muscle that was treated conservatively, with bilateral coronoidectomy and mouth opening physiotherapy, and obtained a satisfactory result. Consequently, it also presents a suggestion of a postoperative physiotherapy protocol.
Keywords
Introduction
Myositis Ossificans is a rare disease that affects muscles or soft tissues. It is divided into Progressive Ossifying Myositis (MOP) and Myositis Ossificans Traumatica (MOT). 1 MOP is also known as Fibrodysplasia Ossificans Progressiva, a dominant autosomal hereditary disease that occurs in childhood. 2 This disorder affects several body muscles, which prognosis is generally poor due to pulmonary complications caused by restricted movement of respiratory muscles. 2 MOT also known as Myositis Ossificans Circumscripta, is a benign and non-neoplastic condition that usually causes mouth opening limitation. 3,4 It is characterized by the heterotopic formation of mature lamellar bone in muscles or other soft tissues after a trauma, 1,5,6 which can vary from a simple mandibular nerve block to a more severe trauma involving bone fracture. 7 –9
Although MOT in the craniofacial skeleton is relatively rare, 6,8,10 its cases have increased in recent years. 11 According to a recent literature review, from August 1984 to April 2019, only 53 cases of MOT were reported in English. 8 The masseter and medial pterygoid muscles were more involved, and only 12 cases involving the temporal muscle were reported. 8 The differential diagnosis for this pathology includes malignant and benign tumors, such as osteosarcoma and osteoma. 8,9 The treatment depends on the disease’s maturation stage and associated symptoms. In early injury stages, symptoms may or may not exist, and ossification is not evident. In these cases, treatment options are physiotherapy and use of medications, such as bisphosphonates and anti-inflammatory drugs. 4,10
Surgical intervention is indicated when ossification is mature, causing worsening of symptoms. In this situation, tumor resection and removal of adjacent structures, such as the coronoid process, can be employed. 8 –10 In addition, the use of immediate postoperative physiotherapy is considered essential for obtaining a satisfactory permanent result. 3,6,7 However, the literature has no consensus or detailed description about an exact protocol, which makes decision-making by surgeon difficult. Therefore this article aims to present a rare case report of Myositis Ossificans Traumatica involving the temporal muscle, which was treated with bilateral coronoidectomy with aggressive postoperative physiotherapy and obtained a satisfactory result. In addition, it also presents a suggestion of a postoperative physiotherapy protocol.
Case Report
A 45-year-old male patient was referred to the Oral and Maxillofacial Surgery team complaining of trismus of unknown origin. He reported that he would undergo an Endoscopic Retrograde Cholangiopancreatography (ERCP) exam, which would require general anesthesia. However, during the anesthesia process, even when the muscle relaxant was administered, there was no gain in mouth opening, which made intubation impossible. Therefore, the surgery was canceled, and he was referred for investigation of the trismus origin. During the anamnesis, the patient described that he suffered a severe trauma 13 years ago, that required a prolonged hospital stay. The trauma resulted in a fracture of the left zygomaticomaxillary complex that required a bone reduction and fixation surgery. Since then, he had a progressive decrease in the mouth opening.
Physical examination revealed a limited mouth opening (13 mm interincisal distance) and a mandible deviation to the left (Figure 1). A multislice computed tomography was requested, showing a hyperdense ectopic mass arising from the temporal bone with characteristics of cortical and medullary mature bone tissue (Figure 2). Supported by the clinical history, clinical examination, and imaging exams, the most accepted diagnostic hypothesis was Myositis Ossificans Traumatica and Osteoma. As the treatment aims to restore the movement of the jaw, surgical coronoidectomy has been proposed.
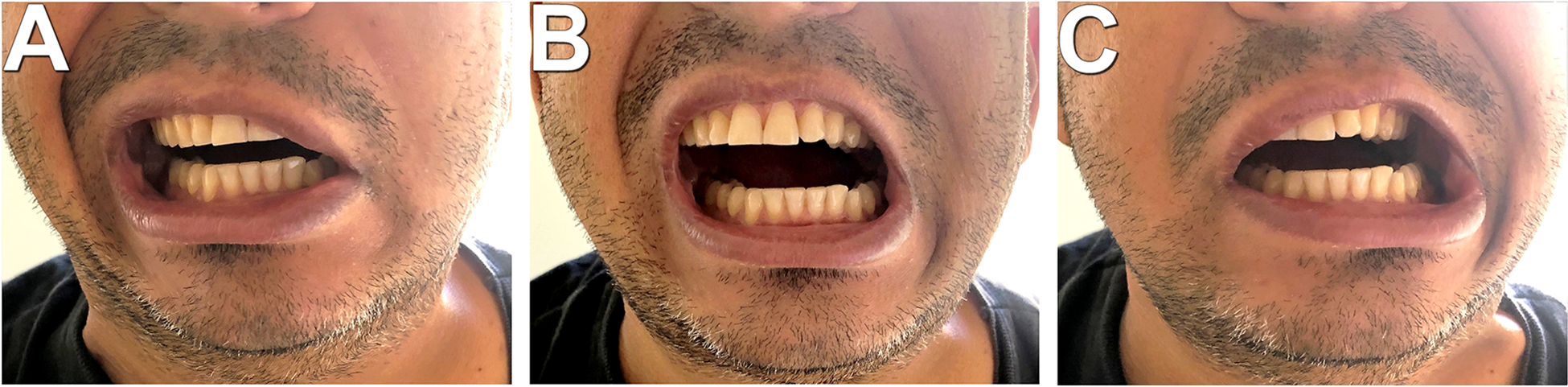
Initial clinical images. (A) Frontal photograph of the patient performing mandibular laterality movement to the right; (B) front photograph of the patient in maximum mouth opening, with a mandibular deviation to the left side; (C) frontal photograph of the patient performing mandibular laterality movement to the left.
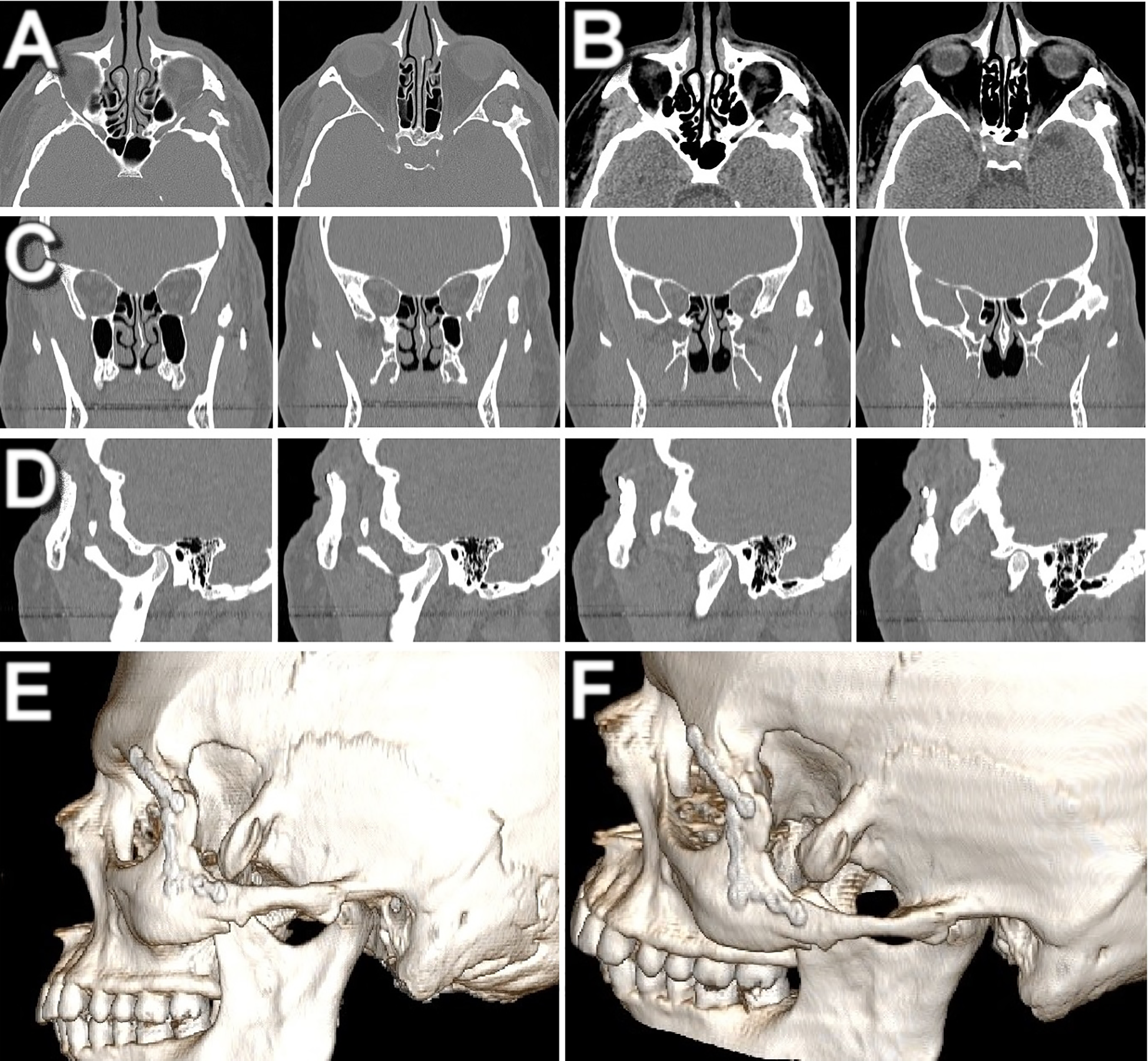
Initial helical computed tomography. (A) Sequence of axial sections showing hyperdense lesion in the left temporal region; (B) sequence of axial slices with soft tissue window; (C) sequence of coronal sections; (D) sequence of sagittal cuts; (E) lateral image of three-dimensional reconstruction; (F) tilted image of three-dimensional reconstruction showing proximity of the temporal lesion to the left coronoid process.
As a mechanical impediment was causing the trismus, conventional intubation would be more difficult and riskier, so fiber-optic-assisted nasotracheal intubation was adopted. This technique is made under conscious sedation, safe, and well used in difficult airway situations. 12 After intubation, the mouth opening was 12 mm (Figure 3A). With an intraoral approach, local anesthesia was performed and an incision of about 3.5 cm was made in the right ascending ramus on the oblique line. Then, a full-thickness mucoperiosteal flap was elevated and the external oblique ridge and base of the coronoid process were visualized.
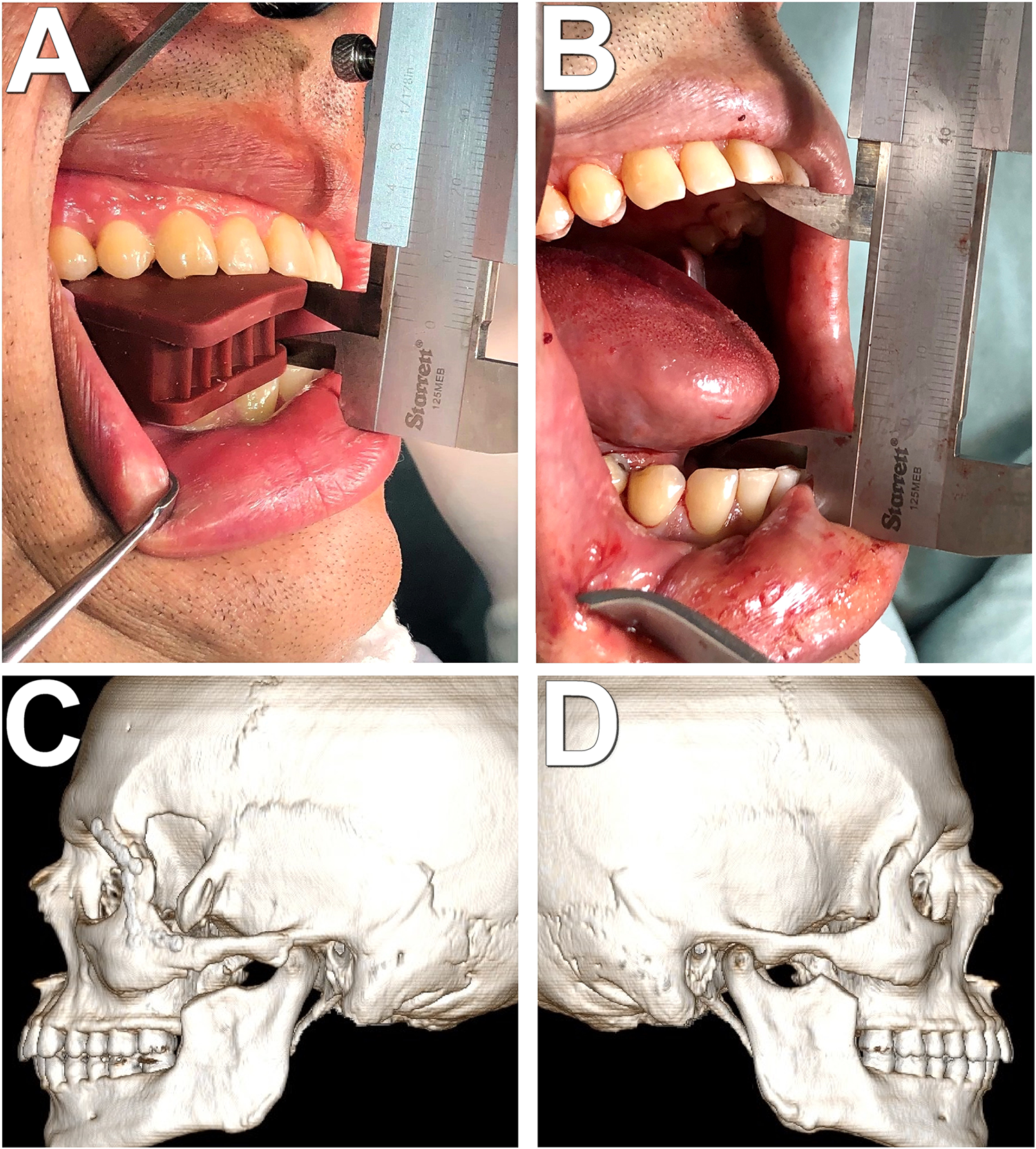
Trans-surgical images and immediate postoperative exams. (A) Maximum mouth opening of 12 mm after intubation; (B) maximum mouth opening of 41.5 mm after removal of bilateral coronoid processes; (C) three-dimensional reconstruction of computed tomography—left side; (D) three-dimensional reconstruction of computed tomography—right side.
As expected, the musculature on this side showed more adherence and stiffness than normal, so detaching the soft tissues over the coronoid processes was difficult. During the procedure, it is important to hold the coronoid process with some forceps, as the muscles tend to have a whip behavior pulling up the fragment if it is not well attached. After its detachment, the coronoid process was removed from its base using a reciprocating saw, and then the mouth opening was measured again (25 mm). However, sufficient mouth opening could not be obtained, so the same process was performed on the opposite side, and the release movement of mouth opening was immediately observed (Figure 3B). Due to a 29.5 mm gain compared to the initial mouth opening, it was decided not to remove the bone pedicle from the temporal muscle (Figure 3C and 3D).
After surgery, a mouth opener was inserted in the patient’s molar teeth (Figure 4A), which was kept in continuous use for uninterrupted 24 hours. During the next 7 days, the patient used this device continuously, removing it only for eating and oral care (approximately 3 hours a day). From this moment on, the use of the mouth opener was gradually decreased. In the second postoperative week, the patient did not use it for approximately 4 hours, and in the third postoperative week, this period was increased to 6 hours per day. Device removal occurred at intervals during the day (when the patient was eating). From the fourth postoperative week on, the patient did not use the mouth opener for 8 hours a day, removing it during sleep. From the 30th postoperative day, the patient did not use the device for approximately 12 hours a day (interspersed). At 45 days postoperatively, the mouth opener was used for approximately 6 hours a day (2 hours in the morning, 2 hours in the afternoon, and 2 hours in the evening). After 60 days of follow-up, the patient had a 35 mm mouth opening (Figure 4B). This last frequency of use was maintained until mouth opening amplitude was stable, which could vary between 4 to 6 months of total physiotherapy. Thus, after 4 months of follow-up, the mouth opening amplitude was stable and increased to 40 mm. In addition, the patient had no pain complaints or mandibular deviations (Figure 4C), and he continues with regular follow-ups.
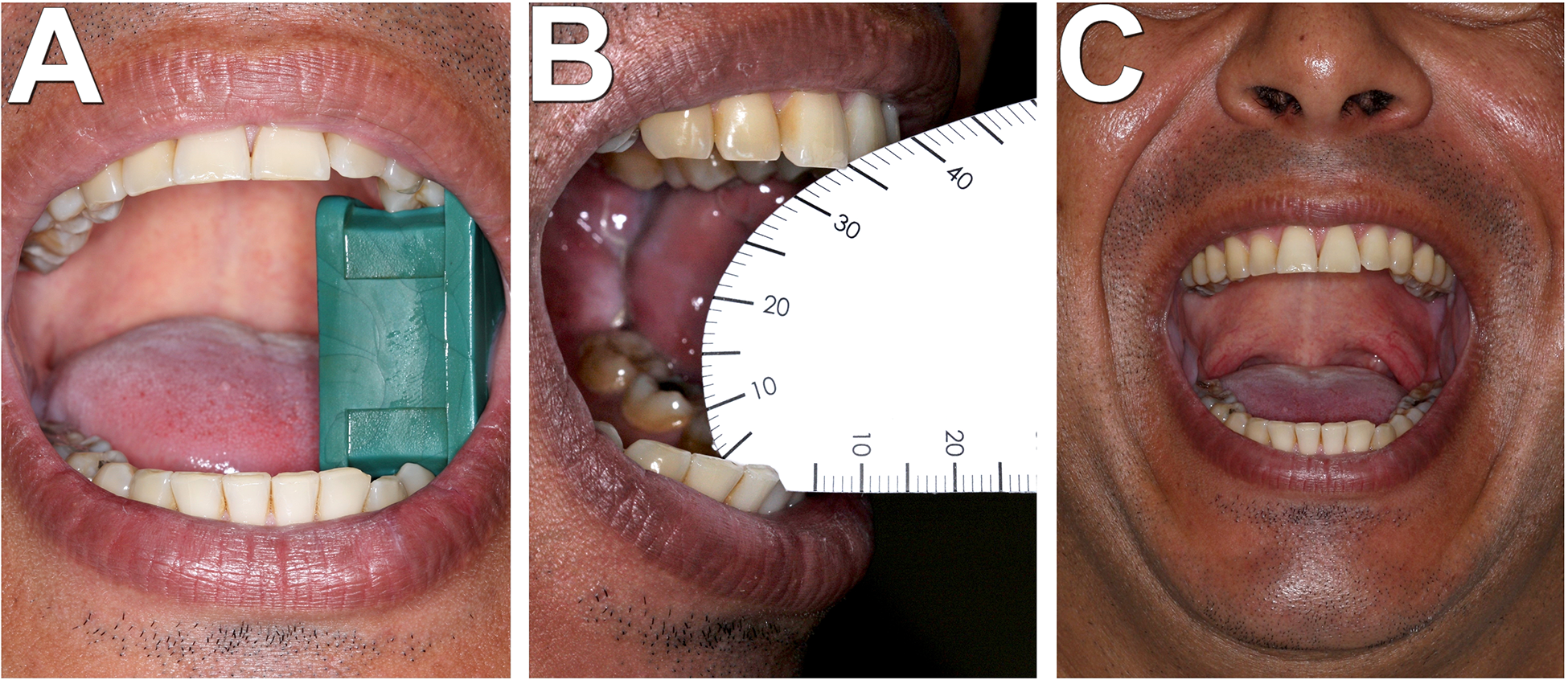
Clinical images of postoperative follow-up. (A) Front photograph of the patient using the mouth opener; (B) 60-day postoperative period with a maximum mouth opening of 35 mm; (C) 4-month postoperative period with a maximum mouth opening of 40 mm, and mandibular symmetry, without deviations.
Discussion
The pathogenesis of MOT is still controversial, and several theories have been proposed over the years to hypothesize it. Apparently, after a trauma, blood extravasation and myonecrosis facilitate the development of osseous metaplasia released from native bone. 5,6,13,14 However, it was also hypothesized by Arima et al, who state that the autolysis of bone fragments releases BMP, which induces the differentiation of perivascular mesenchymal cells into the muscular tissue, resulting in a relatively homogenous bone mass. 15 The present paper reported a case of myositis ossificans caused by a mechanical and structural disorder, such as a zygomatic fracture affecting the temporal muscle. In other cases, isolated or repeated trauma (including blows, traffic accidents, violence, work-related accidents, gunshots), alveolar nerve block, dental extractions, and infections are among the possible causes mentioned. 1,5,8,10,11,16 But in some cases, there is no history of trauma. 3,7,16,17
The vast majority of ossifying myositis occurs in lower muscles due to their lower location and their repetitive motion during mastication, making them more vulnerable to trauma. 7,8,13,16 The medial pterygoid muscle is the most affected, followed by the masseter. 7,8 Though temporalis muscle is vulnerable to trauma like the masseter, less cases of MOT are observed in this group and the reason for this is still unknown. 3 In this case report, only the temporalis muscle was involved, but in some cases, more than 1 chewing muscle may be involved. 3,9,10,16 There is also a higher incidence in men due to their more active lifestyle and probably that is the reason why they suffer more traumas. 8,13
Differential diagnoses of MOT include several diseases involving ossification and calcification processes like thrombosis, phlebolites, osteomyelitis, osteomas, osteochondromas, hemangiomas, nodular fasciitis, and neoplasms such as synovial sarcoma, soft tissue sarcoma, osteochondroma, osteosarcoma, rhabdomyosarcoma, and metastatic disease. 7,18 Malignant tumors of the temporal bone are rare, with an estimated incidence of about 0.8 to 1 per million inhabitants per year. 18,19 Temporal bone tumors are manifested by non-specific symptoms, such as otorrhea, otalgia, or hearing loss, which are often attributed to inflammatory otological diseases. 19,20 Our patient did not report any of these symptoms and other related symptoms, such as trismus, are uncommon and indicative of advanced disease. 21,22
The biggest difficulty in differentiating MOT from a malignant tumor is in its initial stage when ossification is not yet mature. 7,18,21 As the lesions mature, the imaging characteristics are better observed. Malignant tumors often cause destruction or invasion of adjacent structures or tissues, and the calcification begins at the center and progresses toward the periphery. 3,8 In MOT cases, the calcification begins at the periphery and progresses toward the center, which may or may not be attached to the adjacent bone, depending on the maturity of MOT. 1,7,11,17 This characteristic is considered pathognomonic by some authors. 14 The diagnosis of MOT is based on a trauma history, usually with a blunt injury. Although, the trauma is reported in only 70% of the cases with supportive clinical, radiographic, and microscopic features. 3 Malignant transformation of traumatic myositis ossificans has not been reported yet. 22 In the present case, there was nothing suggestive of malignancy.
The interval between trauma and the first detection of calcified mass is variable, and it can start immediately or show its first symptoms after 20 years. 8,10 These signs and symptoms may usually include trismus, firm/solid persistent edema, and single or multiple calcifications seen on imaging exams. 8,10 In our case, some of the disease signs and symptoms were mistaken with those from the postoperative period after facial fracture. For this reason, it was difficult to investigate another cause of this limitation, which was discovered 13 years later by chance. As mouth opening was limited, intubation with the aid of a fiber-optic bronchoscopy was used, as in other cases in the literature. 7,13 This technique is considered a gold standard of difficult airway management, when a conventional technique is not successful. 12
Knowing that this patient’s biggest problem was caused by stiffening of the masticatory muscles, also observed by other authors, 23 and mechanical interference due to contact between the coronoid process and the ectopic mass in the mouth opening, surgical coronoidectomy is the treatment of choice. 3,5 –9,11,13,16,23 However, as the patient remained with limited mandibular movement for many years, it is natural to have a stiffening of the contralateral musculature either, 23 so the 40 mm mouth opening was only possible after coronoidectomy on both sides, and the jaw became more passive, avoiding the removal of ectopic calcification.
The volume and extent of the heterotopic bone in relation to the skull bases bear a considerable risk during radical excision, contraindicating its removal at first. Therefore, its removal is indicated only in case of little or no gain in mouth opening. In addition, the preauricular approach with temporal extension involves a series of nerves and blood vessels, such as auricular, superficial temporal arteries, and the temporal branch of the facial nerve that could be affected causing praxis, paresthesia, and hemorrhage. 15 As the MOT was not removed, we did not obtain material to perform a biopsy. Although some authors recommend a biopsy for a complete diagnosis of the lesion, in most cases the clinical and imaging tests are sufficient to define a treatment plan. 5,6,10,13
Surgery is most appropriate when there is a mature bone formation, as any surgical trauma in the region at an early stage could cause an increase in ectopic calcification. 9 Complete excision and coronoidectomy are the most common treatment for MOT in the temporal muscle and it is frequently associated with postoperative physiotherapy, that should happen as soon as possible. 3,6,7,11,13,16,21 In the present case, the patient remained with the rubber mouth opener to maintain a satisfactory opening range. This method was also used by Mevio et al 6 in 2001, emphasizing the idea of aggressive physiotherapy, especially when the patient is not collaborative, because, when using a rubber opener of predetermined size, the patient is forced to open his mouth enough to fit the mouth opener among the molar teeth, which provides tissue healing without contraction of the muscles and recurrence of limited mouth opening.
Since the literature has no well-defined protocol on how to use the mouth opener as physiotherapy, we suggest a physiotherapy protocol that was applied to a patient and presented good results. We know that a single case report does not have sufficient scientific basis to institute protocols, and this is not the objective of our paper. We suggest a treatment protocol that was appropriate for our case. This therapy consisted of aggressive physiotherapy with a gradual reduction in the use of the mouth opener, which can be used for up to 4 to 6 months, if necessary. The patient started with continuous use for 24 hours uninterrupted, decreasing each week, respectively: 3 hours/4 hours/6 hours/8 hours/12 hours/18 hours a day without using the mouth opener.
Conclusion
Myositis ossificans remains an uncommon clinical entity especially when it involves the temporal muscle. Coronoidectomy is still one of the most widely implemented surgical modalities when it comes to temporal muscle MOT. Aggressive physiotherapy is essential in the postoperative period to maintain an adequate mouth opening. Our work suggests a protocol that has shown good results, however, further studies are necessary to properly institute a protocol.
The present case shows a patient who discovered that he had MOT just because he needed an exam with general anesthesia, so all healthcare professionals must know this condition because it must be considered from a differential diagnosis of trismus to a tumor in the temporal region.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
