Abstract
The treatment of mandibular condylar fractures is a controversial topic in maxillofacial surgery. Open surgery with anatomic reduction and internal rigid fixation is well established in the literature and appears to be the most common approach. Nonsurgical therapies are indicated to intracapsular fractures, medial condylar displacement, and pediatric trauma. The high capacity of tissue remodeling and articular adaptation are important factors to support nonsurgical treatment in pediatric patients. The purpose of this article is to present a case of a pediatric mandibular bilateral condylar fracture treated with closed reduction with 10 years of follow-up and a discussion based on the literature.
Introduction
The treatment of pediatric fractures is related to the etiology, location, type of injury, among other factors. Correct diagnosis is essential when deciding on the most convenient approach. 1,2 The multicenter study of Boffano et al. 3 analyzed 114 pediatric fractures for 1 year. The mandible was the most common fracture (36%), with the condyle the most affected area, followed by orbital (17%), nose (16%), and zygomatic complex (15%).
Cruz et al. analyzed 454 cases of facial trauma in childhood between 1973 and 2011, the most common fracture was the mandible with the condyle being the most affected region. In only 20% of these condylar fractures, the location was bilateral. 2 With the advent of computed tomography (CT) and its wide use in dentistry, the diagnosis has become faster and more accurate. 4
The aim of this article is to report a case with 10 years of follow-up of a bilateral pediatric mandibular fracture that was treated conservatively.
Case Report
Female patient, 9 years old, their parents reporting a facial trauma after a bicycle accident, presenting chin laceration and malocclusion with anterior open bite. First, a panoramic X-ray was performed to confirm the diagnosis of a bilateral condylar fracture. Second, CT scan with 3D was indicated to specify the correct location of the fractures and the type of displacement (Figure 1). A neck fracture of both condyles with medial displacement and loss of ramus height was concluded justifying the anterior open bite.
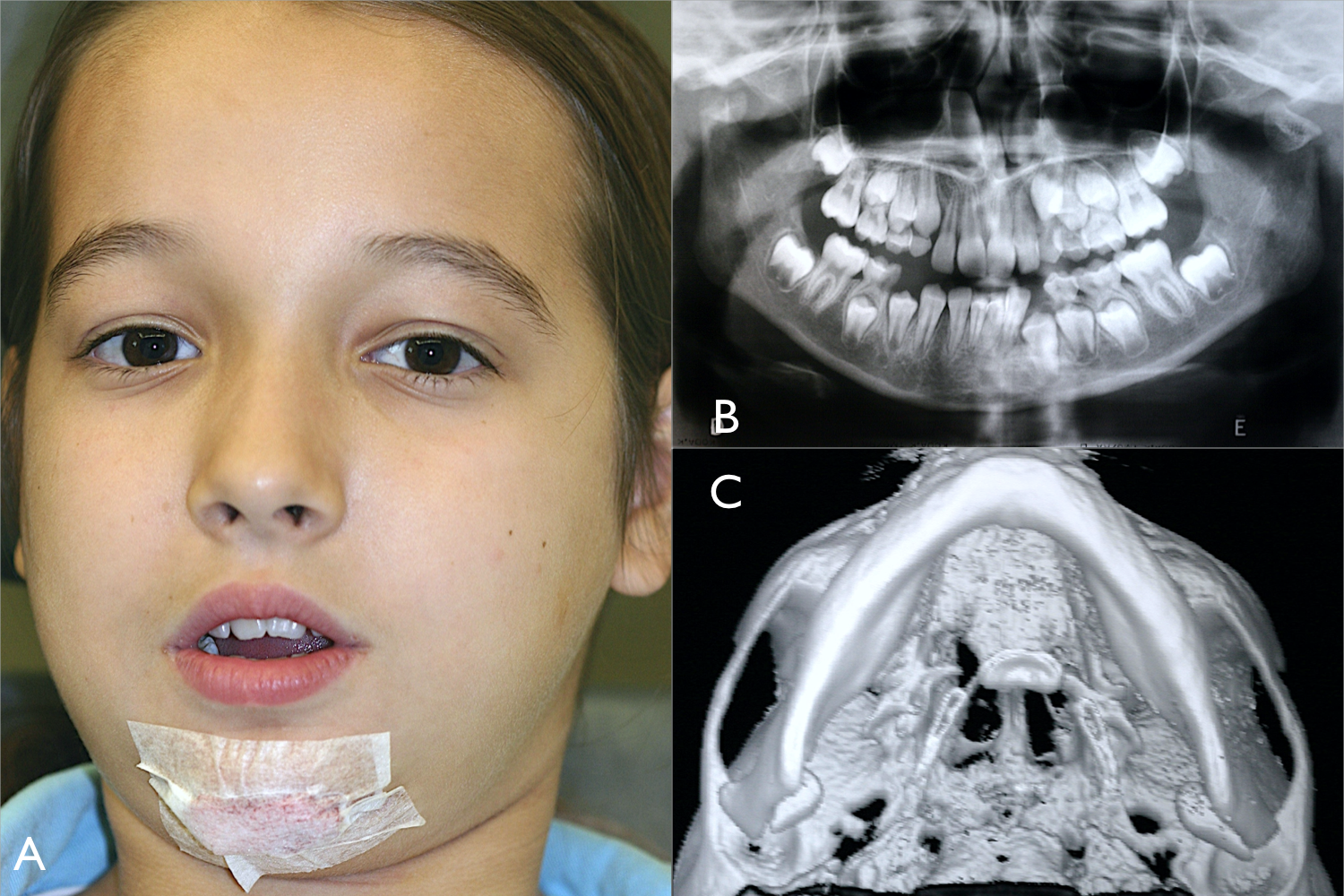
(A) Facial aspect after trauma with an open bite malocclusion. (B) Panoramic X-ray confirming bilateral condylar fracture. (C) 3D reconstruction after CT scan showing medial displacement of both condyles. CT indicates computed tomography.
After 2 days of the trauma, the patient was treated with intermaxillary fixation (IMF) using for 2 weeks. It was not possible to use teeth for anchorage because of the deciduous dentition, so the IMF was done using 4 conventional 2.0 mm screws (Figure 2). The procedure was performed under local anesthesia.
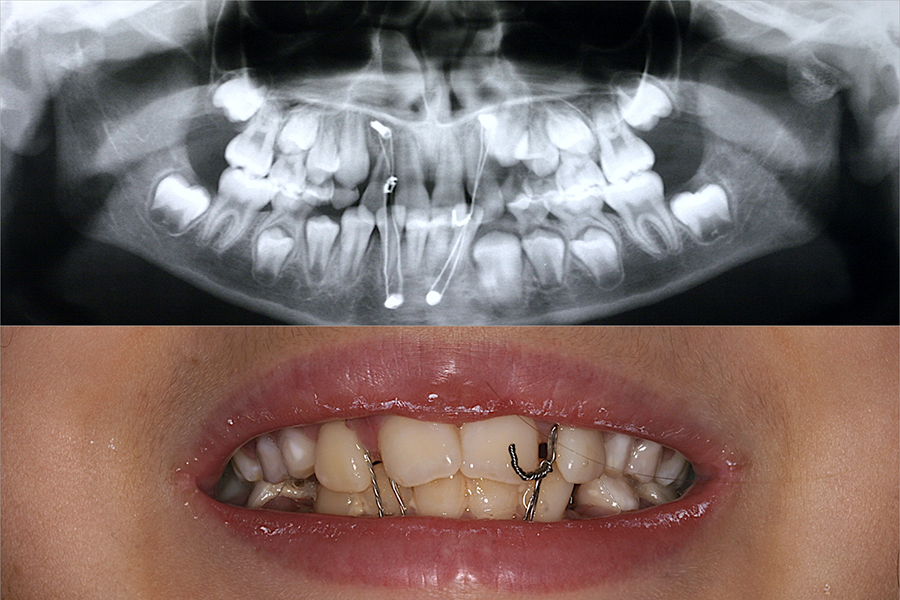
(A) Panoramic X-ray after IMF showing the position of screws in maxilla and mandible. (B) Clinical view showing IMF period. IMF indicates intermaxillary fixation.
After 2 weeks of rigid IMF, the wires were replaced for elastic with immediate physiotherapy treatment. After 45 days, orthodontic braces were installed with strong recommendations to keep physiotherapy for 3 months (Figure 3).
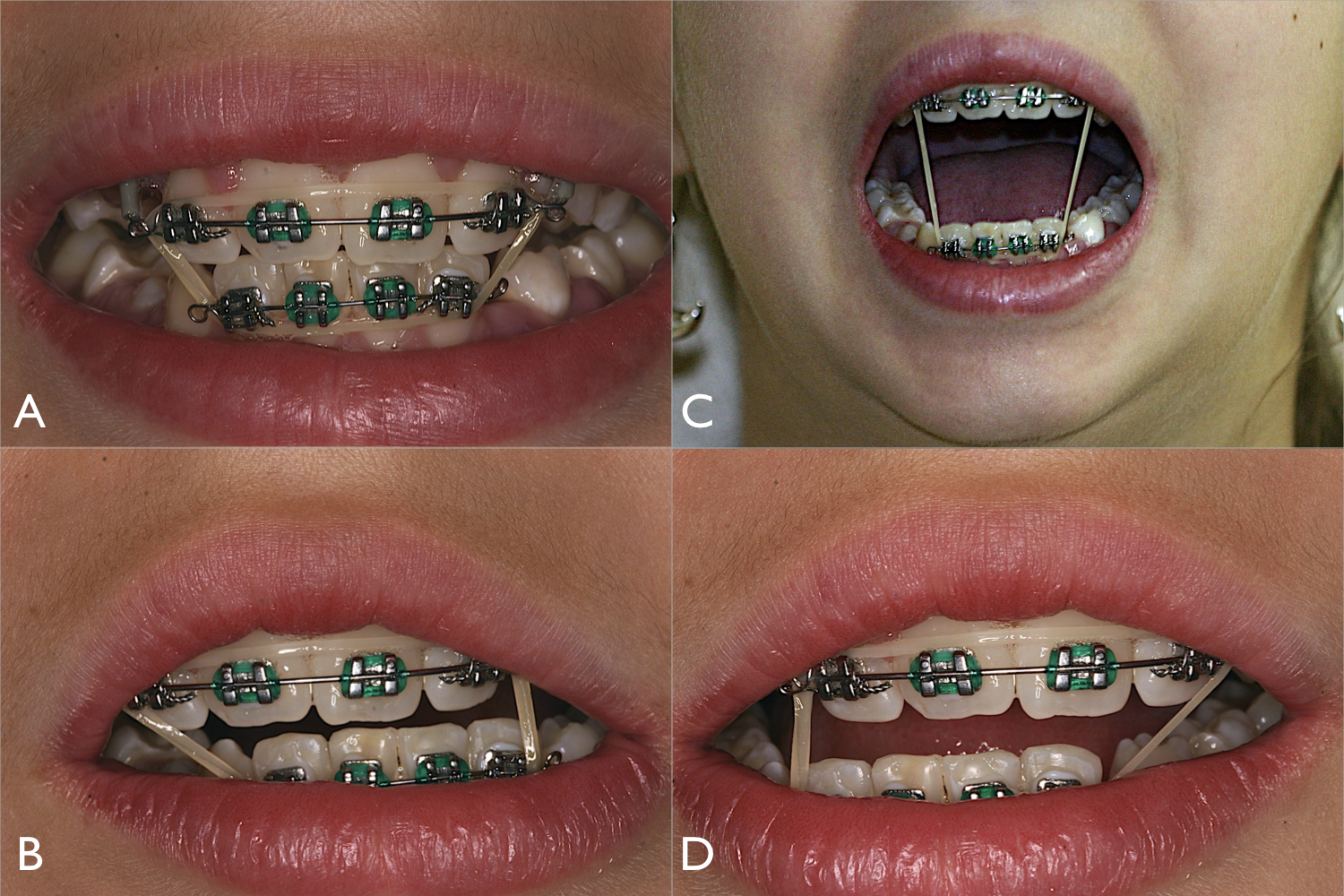
(A-D) Clinical view, orthodontic and physiotherapy, showing normal occlusion and excursive movements.
After 9 months of follow-up, the patient already had a satisfactory mouth opening of approximately 45 mm, adequate excursive movements, with clinically full recovery signs. One-year post-op X-ray showed a very satisfied condylar remodeling. After 2 years of follow-up, a new CT scan revealed an impressive bone remodeling of both condyles (Figure 4) and the patient was discharged from the Maxillofacial Department.
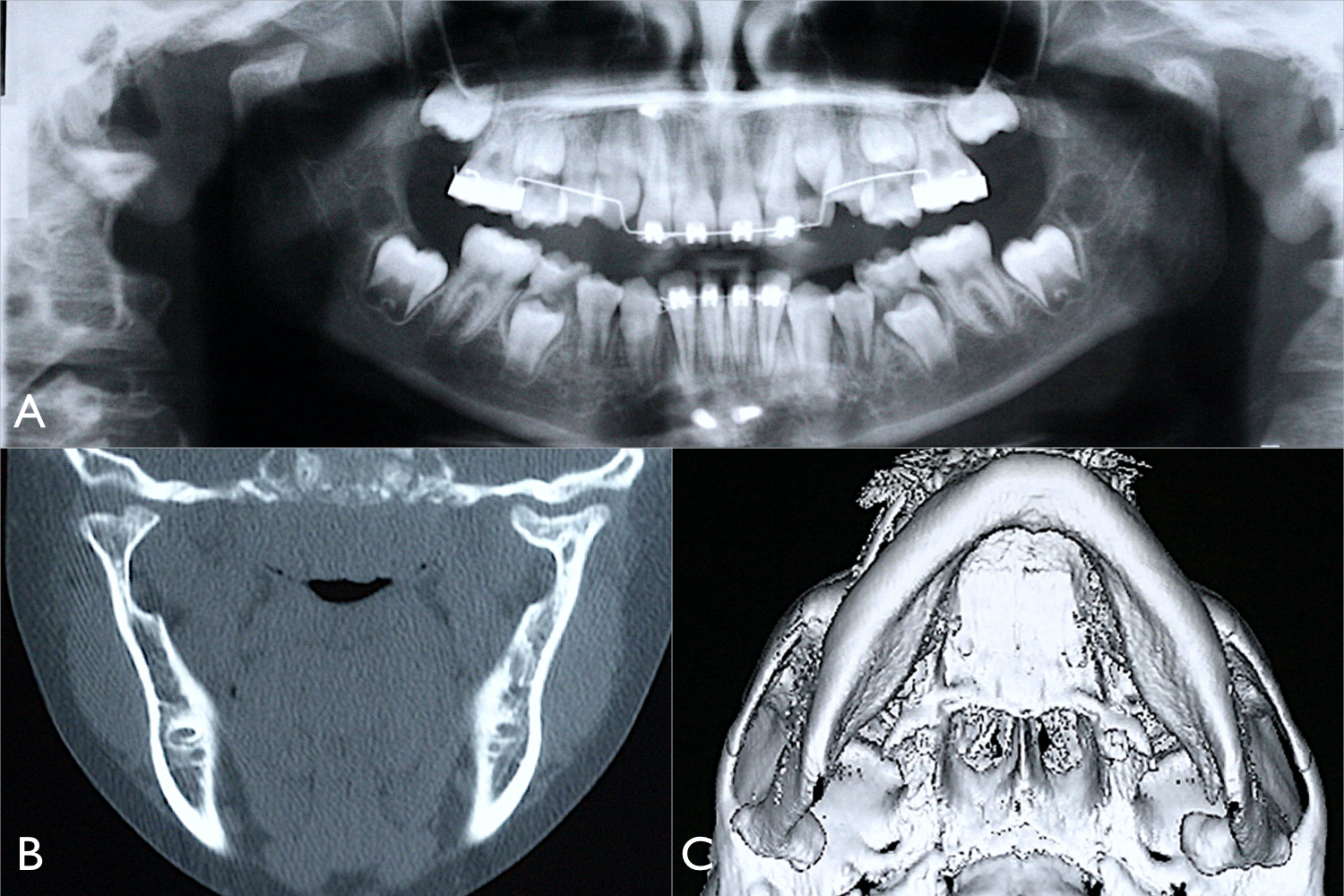
(A) Panoramic X-ray 1 year after treatment. (B) Coronal view from CT scan showing a lot of bone formation and remodeling process with functional articular space. (C) 3D reconstruction showing normal ramus height. CT indicates computed tomography.
Eight years later, 10 years after trauma, she searched for the former resident looking for wisdom teeth removal, with panoramic X-ray. The image showed a full remodeling in the fracture region with the anatomy very similar to a normal temporomandibular joint (TMJ). Clinically, the patient presented normal joints, with clinically adequate mouth opening, lateral movements and occlusion (Figure 5).
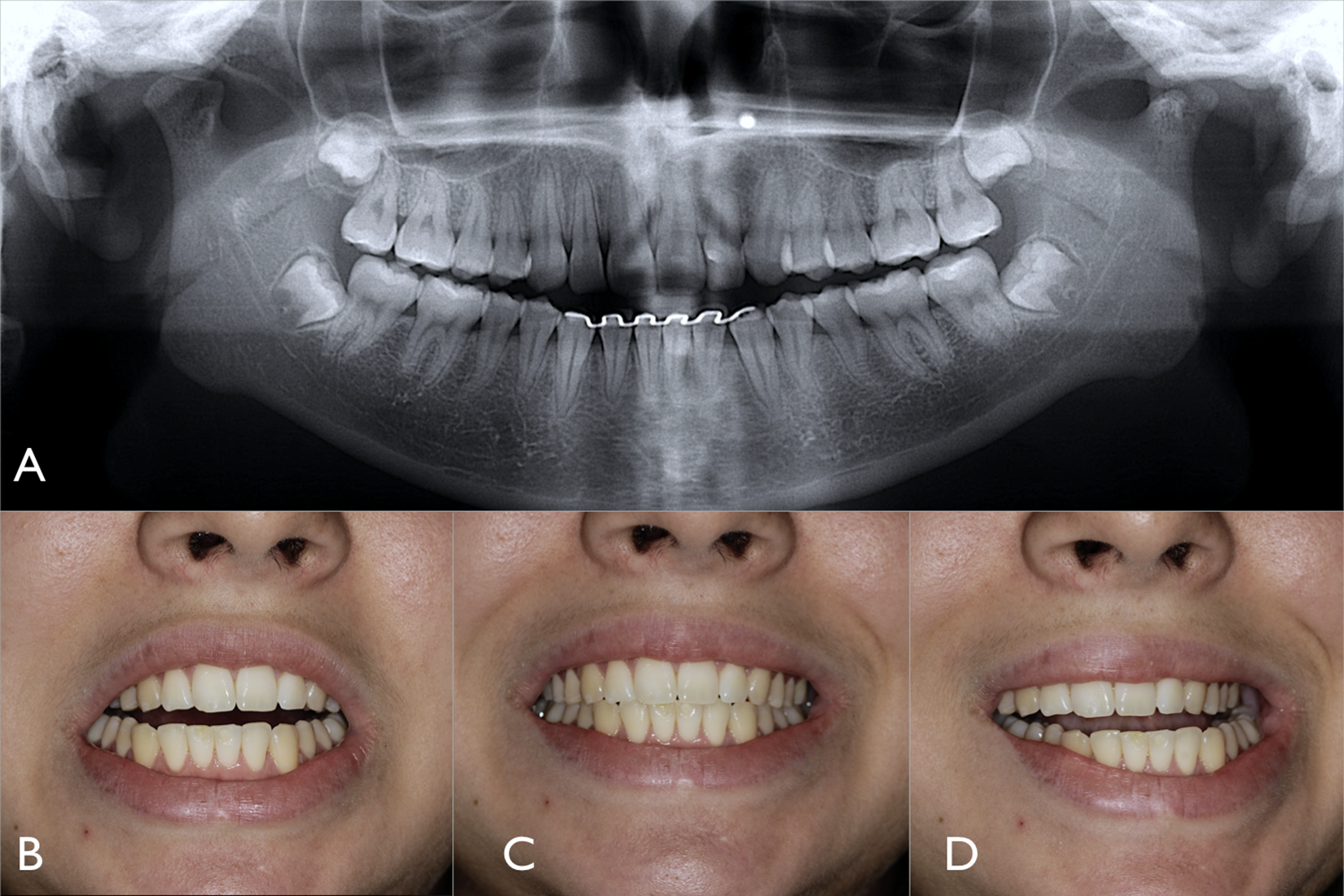
(A) Panoramic X-ray with 10 years of follow-up showing both condyles with a very satisfactory anatomy and appropriate condylar space. (B to D) Clinical views showing normal occlusion and excursive movements.
Discussion
The treatment goal of pediatric condylar fractures is to reestablish function and prevent future complications. Fractures where there are no signs of malocclusion, bone displacement, or comminuted fracture are indicative for conservative nonsurgical therapies. 1,5
Conservative treatment is based on a liquid diet, clinical follow-up, elastic therapy, and/or IMF. 1,4 Many maxillofacial surgeons choose for conservative treatment because of the adaptation process in growing patients and the risks related to open surgery. A poor diagnosis can lead to occlusal changes, skeletal deformities, ankylosis, among others, which makes new interventions necessary including orthognathic procedures. 3 –5
Boffano et al. analyzed 14 patients with displaced condylar fractures between 6 and 13 years old treated conservatively. After 1 of year follow-up, there was no case of malocclusion, pain, or trismus, only 1 patient related click on TMJ. Complete healing of condylar process was found in panoramic X-rays in 13 patients. In the remaining patients, although the condylar process didn’t show a normal shape, it presented normal functional with no restrictions or symptoms. 6
Treatment should be chosen according to each patient, type of fracture, location, and related injuries. The pediatric patients are recommended to evaluate factors such as the stage of mandibular and dental development. Both conservative and surgical treatment are described and can be performed according to each case. This isolated report highlights the possibility of full recovery, functional and esthetic, for pediatric patients with bilateral condylar displaced fractures treated with conservative nonsurgical therapy.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
