Abstract
Refracture of the mandible following stable internal fixation would be rare. A 28-years-old male patient was transferred to our emergency center due to fall caused by epilepsy seizure. Computed tomography (CT) showed left condylar base fracture with medial displacement and dislocation, and symphysis fracture. The fracture of condyle and symphysis were performed osteosynthesis with 2 mini-plates on ideal lines of osteosynthesis. The proximal segment of the condyle was placed totally three 7-mm-screws and 2 mini-plates. Six days after surgery, the patient transferred to our emergency center again due to fall by epileptic seizure. The patient drunk a lot of alcohol on the day before. CT indicated that left side fracture of condylar neck with medial displacement above the fixation plates, and no fracture of symphysis. The fracture line run on upper screw of posterior plate. The proximal segment of condyle could not be repositioned in the secondary surgery. The epilepsy patient following mandibular fracture might cause further epilepsy seizures. The risk factors of recurrence seizures should be evaluated including alcohol intake, less sleep and a history of noncompliance to anti-epileptic drugs.
Introduction
Refracture of the mandible following stable internal fixation with mini-plate would be rare. 1 In this study, refracture of the condyle 6 days after stable internal fixation was reported in epilepsy seizure.
Case Report
A 28-years-old patient was transferred to our emergency center due to fall caused by epilepsy seizure. He was an international student and stopped taking medicine of epilepsy after leaving the country 3 months ago. The patient showed laceration in mental region, crown fractures of the bilateral upper central incisors, and the mandible was displaced between bilateral lower central incisors. The patient suffered from epilepsy since 13-year-old. Epilepsy seizure was cured at 21-year-old, but epilepsy seizure was recurred at 25-year-old, and it was treated again in his country. Epilepsy seizure occurred once a year in recent year. Computed tomography (CT) showed left condylar base fracture with medial displacement and dislocation, and symphysis fracture. The step of fracture line between inner cortex and outer was noted in condylar fracture (Figure 1). Levetiracetam, second-generation anti-epileptic drug was started by intravenous administration for epilepsy. An internal fixation using retromandibular anterior trans-parotid approach
2
and mandibular vestibular approach were performed under general anesthesia. The fracture of condyle and symphysis were fixed by 2 mini-plates on ideal lines of the osteosynthesis, and a lag screw was added to close approximately 1.0 mm gap of the fracture line on the inferior of the fixed mini-plates in symphysis fracture. The proximal segment of the condyle was placed totally three 7-mm-screws; 1 screw of anterior 3-hole-mini-plate and 2 screws of posterior 4-hole-mini-plate on the proximal segment of the condyle (Figure 2)*. The proximal segment of the condyle was reduced by joystick method. At first, 1 screw on the top 1 hole of 3-hole-anterior mini-plate and 2 screws on the top 2 holes of 4-hole-posterior mini-plate were placed on the proximal segment of the condyle. And then, 2 fixed mini-plates were pulled to the distal segment, and each bottom 2 holes were fixed loosely by each 2 screws. Finally, temporally internal maxillomandibular fixation (IMF) was performed, and the screws were tightened. The postoperative X-rays showed good reduction and fixation (Figure 3). The patient showed no postoperative facial palsy. He discharged without IMF and complications 3 days after surgery. Oral administration of levetiracetam was continued. Six days after surgery, the patient transferred to our emergency center again due to fall by recurrence seizure. The patient drunk a lot of alcohol and slept the medicine again on the day before. The patient showed laceration in mental region. No displacement plates were observed from the laceration. A panoramic radiograph showed fracture of condylar neck above the fixation plates and no fracture of symphysis (Figure 4A). CT indicated that left side fracture of condylar neck with medial displacement above the fixation plates, and no fracture of symphysis. There was no fracture of glenoid fossa (Figure 4B and C). The authors tried to perform reduction and internal fixation again under general anesthesia. The fracture line run on upper screw of posterior plate (Figure 4D). Although the authors tried to perform fixation, the proximal segment of condyle could not be returned. Finally, the plates and screws were removed, and IMF was performed for 2 weeks
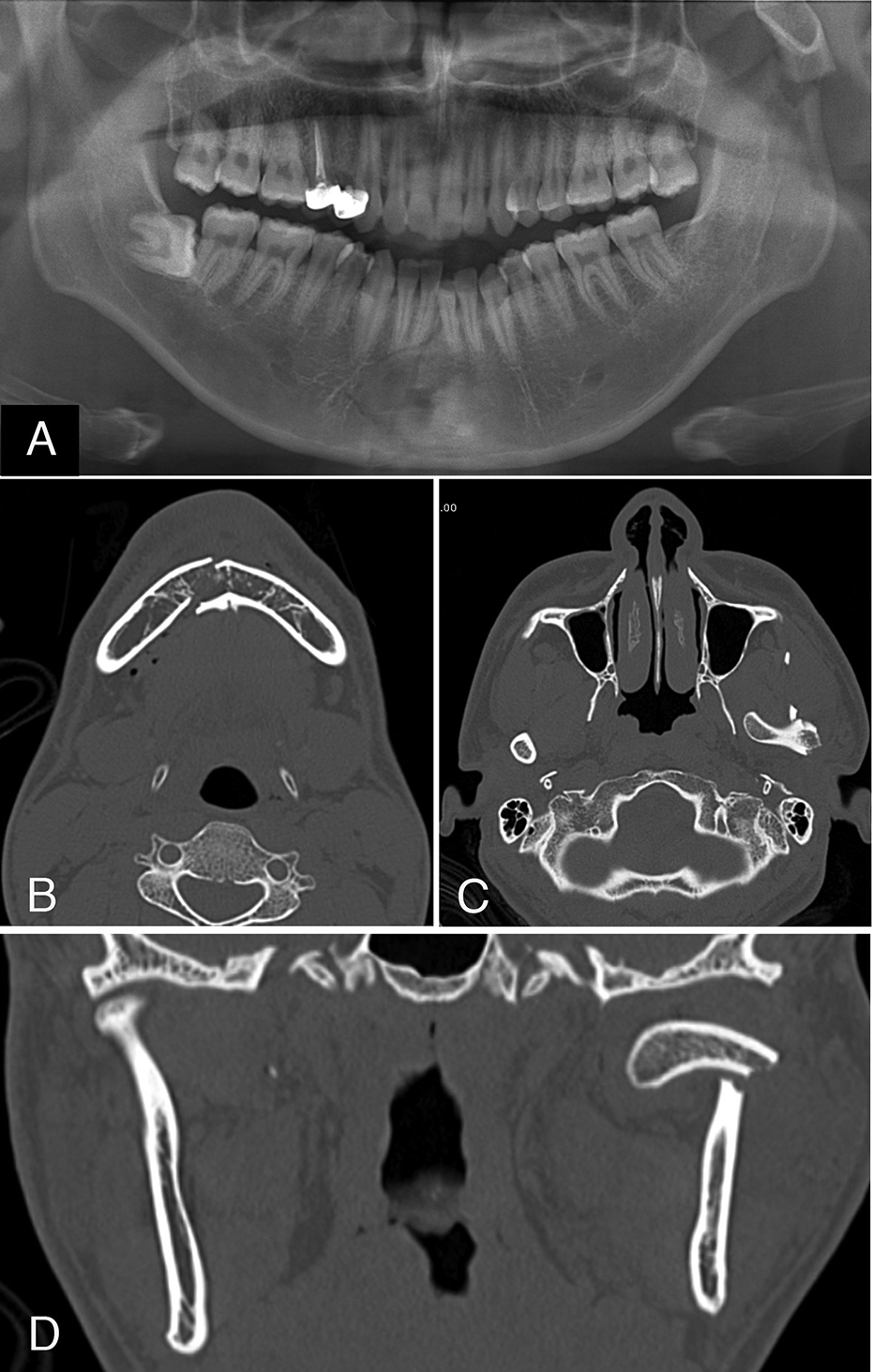
(A) Panoramic radiograph, (B and C) axial computed tomography (CT) and (D) coronal CT findings of the mandibular condyle and symphysis fracture in 28-years-old epilepsy patient. Axial and coronal CT showed mandibular condylar base fracture with medial displacement and dislocation.
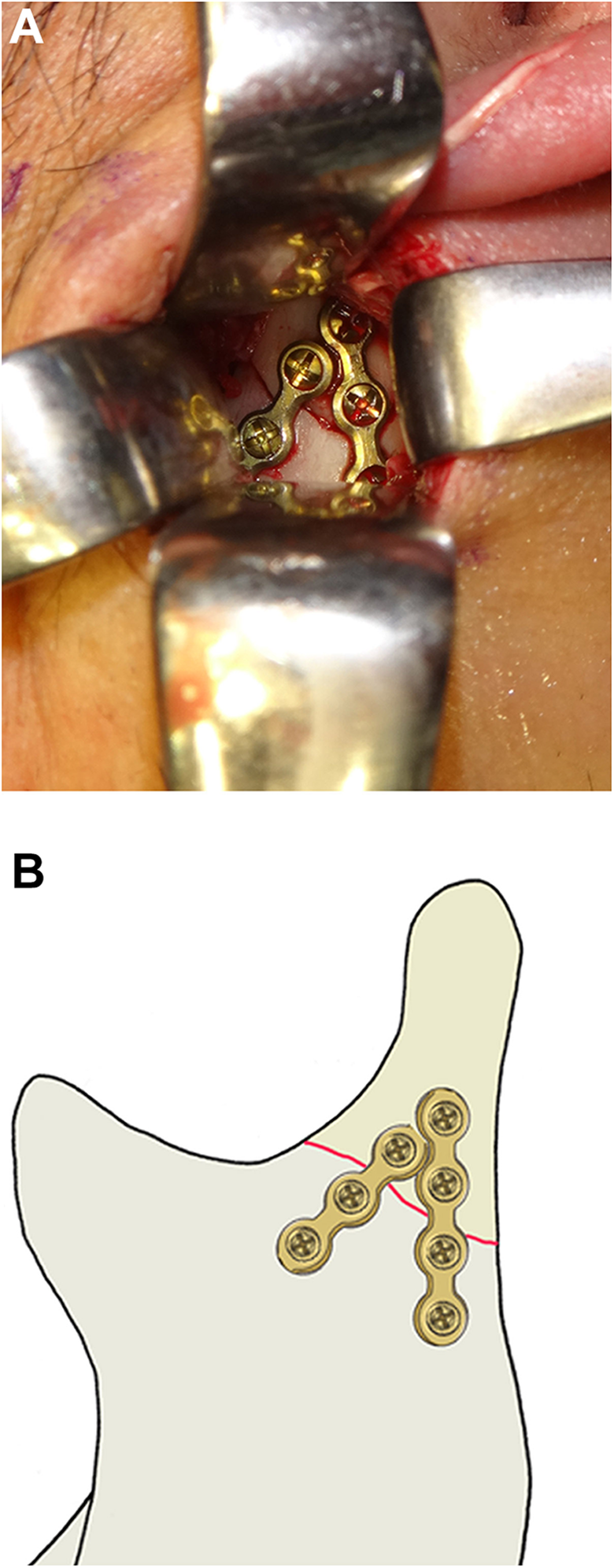
(A) Intraoperative photograph of the internal fixation of the condylar base fracture. (B) Schematic diagram of the internal fixation of the condylar base fracture. The proximal segment of the condyle was placed totally three 7-mm-screws.*
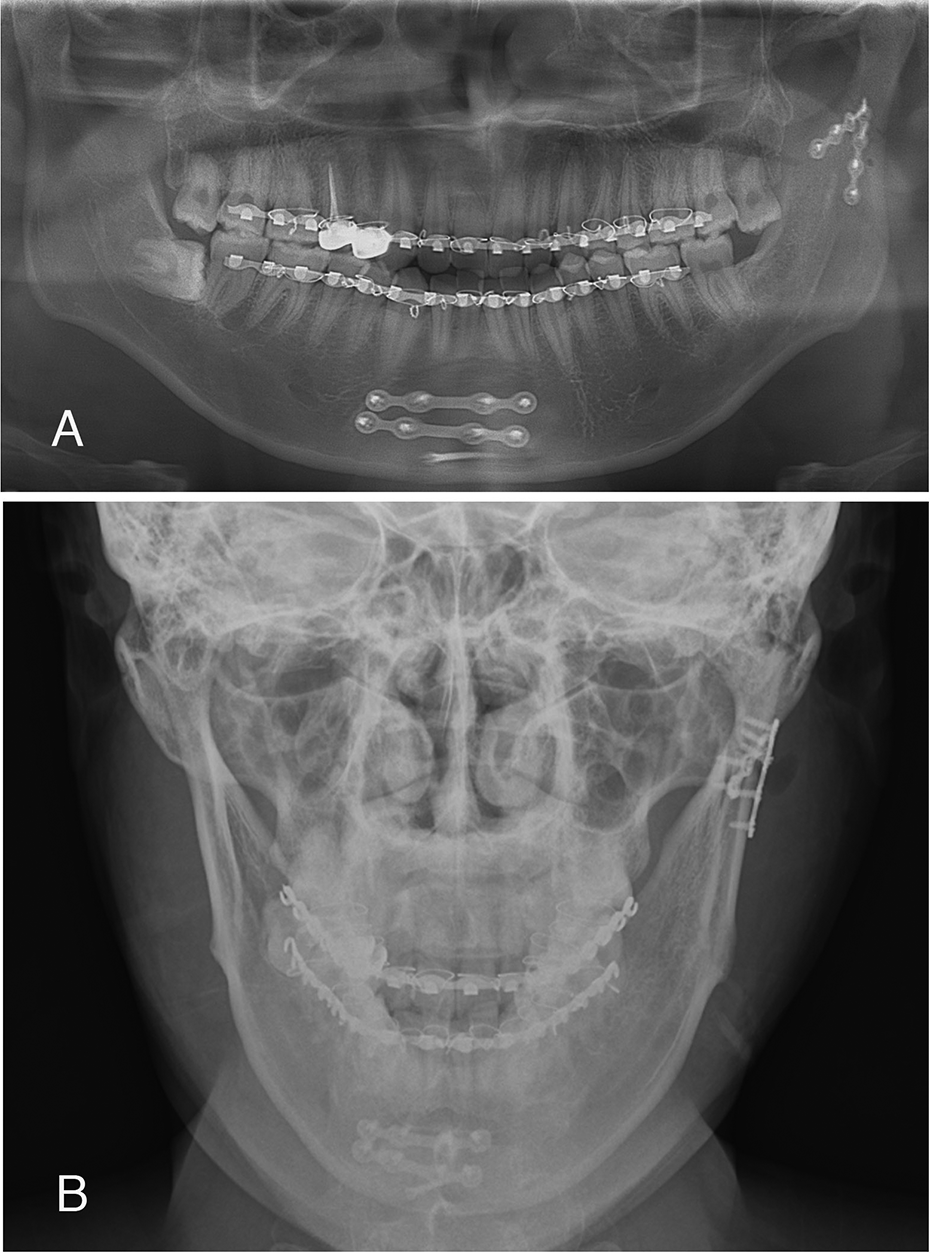
(A) Postoperative panoramic radiograph and (B) posterior-anterior radiograph of the skull immediate after stable internal fixation.
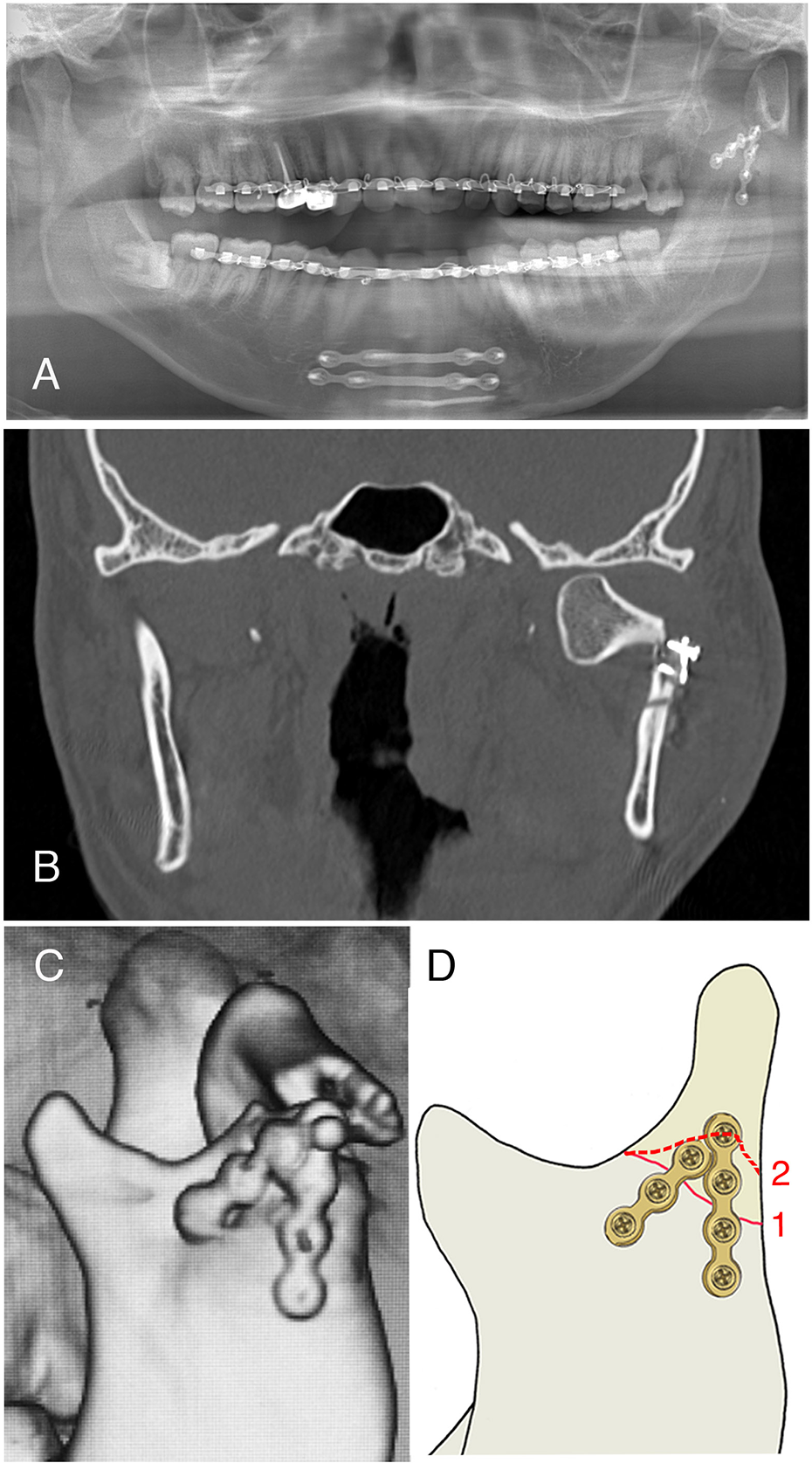
Refracture 6 days after surgery. (A) Panoramic radiograph, (B) coronal computed tomography (CT), (C) 3-dimentional CT and (D) schematic diagram of the first and secondary fracture line.
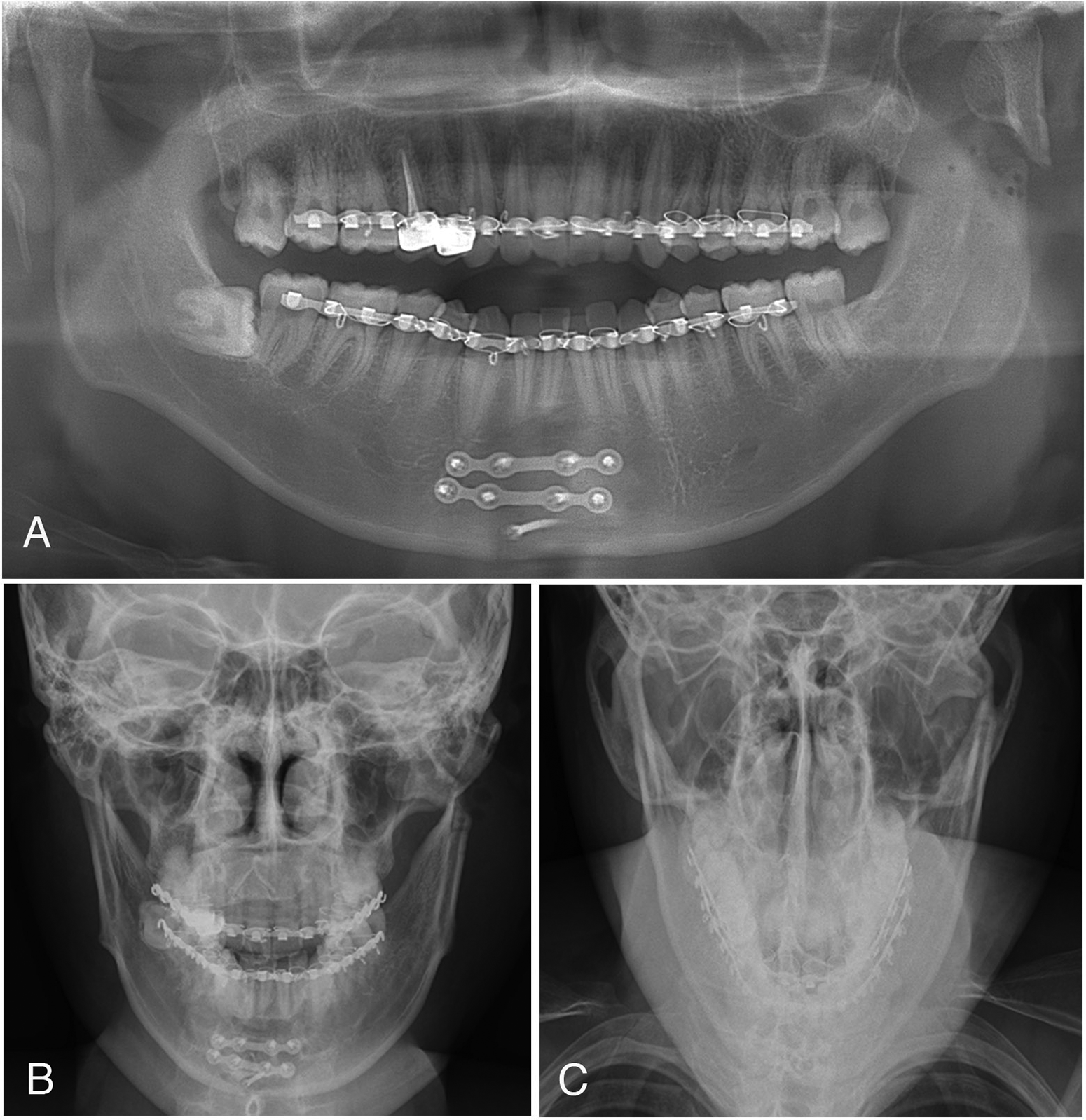
(A) Postoperative panoramic radiograph, (B) posterior-anterior radiograph of the skull and (C) Town’s view after secondary surgery.
Discussion
The risk of fractures among epilepsy patients is approximately 2-fold higher compared with general population patients without epilepsy in the population-based study. 3 Approximately 40% epilepsy patients experience dental and oral injuries. Most injuries are crown fracture, followed by mandibular fracture and tooth avulsion. 4 In this case, the patient discharged without complications 3 days after stable internal fixation. He drunk a lot of alcohol, skipped the medicine and slept only 3 hours at 5 days after surgery. And he occurred epilepsy seizure at 6 days after surgery. Several studies indicated that small to modest alcohol intake does not increase seizure frequency or significantly alter blood levels of anti-epileptic drugs. However, exceptions may include (1) patients with a history of noncompliance to anti-epileptic drugs, (2) prior history of alcohol or other substance abuse, (3) those with alcohol-related seizures, (4) young adults who have difficulty limiting their alcohol intake. Drinking moderate or heavy amounts of alcohol increase risk of seizures, with the greatest risk occurring 7 to 48 hours after the last drink. 5 Moreover, lack of sleep and higher stress and anxiety are associated with seizure occurrence. 6 In this case, recurrence epileptic seizure would be induced by (1) heavy amounts of alcohol, (2) skip of anti-epileptic drugs, and (3) less sleep. The rate of dentoalveolar and maxillofacial injuries increase in patients with poorly controlled epileptic seizures. 4 In this case, the patient was international student who could not speak Japanese and English. His Japanese school teachers supported him and they translated our informed consent to the patient. However, the authors could not predict the patient drunk a lot of alcohol after discharge. It is indicated that whether the patient had another risk factor of the recurrence seizures should be evaluated in the management of the epilepsy patient.
Refracture of the condyle after internal fixation using mini-plates would be a rare. 1 Although biomechanical force was changed by internal fixation with mini-plates and screws in condyle after first surgery, secondary injury caused no fracture of glenoid fossa. Barron, et al. reported no case of fracture of glenoid fossa following internal fixation of the condylar fracture in the review of the 33 cases of middle cranial fossa injuries caused by condylar dislocations. 7 In this case, the authors found that (1) secondary fall after the treatment caused no refracture of symphysis by direct external force, but caused fracture of condyle by indirect force, (2) it caused no plate fracture in condyle and (3) no fracture of the glenoid fossa caused by dislocation of the condyle, (4) fracture line of the condyle run on upper screw of posterior plate instead of the first fracture line, and (5) it caused impossible repositioning. Kulahci et al. reported a similar case: a 36-year-old male presented left condylar base fracture caused by epilepsy seizures due to discontinue of the medicine 10 months ago. He is performed internal fixation and discharged uneventfully 10 days after surgery. Four months after surgery the patient stop the medicine 1 month ago himself. The patient cause recurrence seizures and show refracture of the left condylar base and a new fracture on the right condylar base. 8
To conclude, the epilepsy patient following mandibular fracture might cause further epilepsy seizures. The risk factors of recurrence seizures should be evaluate including (1) alcohol intake, (2) less sleep and (3) a history of noncompliance to anti-epileptic drugs. 5,6 Strict patient education following surgery was recommended.
Footnotes
*
Figure 2 A & B have been updated since the article was initially published. They has been rotated at 90 degree angle.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
