Abstract
Sport-related mandibular fracture is a common injury in the field of maxillofacial surgery. However, the treatment of mandibular condylar fractures in professional soccer goalkeepers is rarely reported. A 32-year-old male professional soccer goalkeeper was referred for malocclusion after collision with an opponent player during a game. The patient’s mandible was displaced between the left lower lateral incisor and left lower canine. Computed tomography showed right condylar base fracture with medial displacement and left para-symphysis fracture. Internal fixation using retromandibular anterior trans-parotid approach via 25-mm skin incision immediately below the earlobe and intraoral vestibular approach were performed under general anesthesia 2 days after the injury. The patient was discharged without complications 3 days after surgery, with mandibular protrusion and diduction exercises with limitation of mouth opening. Soft diet and limitation of mouth opening was performed for 4 weeks after surgery. To achieve early return-to-play, rehabilitation based on Fowell and Earls’ return-to-play guidelines following facial fractures was started, with moderate exercise 5 days after surgery, and progressively full exercise without contact 8 days after surgery. He started normal team training with individualized jaw-guard 4 weeks after surgery. His body weight decreased by 2.2 Kg 1 week after surgery, gradually recovered, and became normal 4 weeks after surgery. The patient returned to a game 2 months after surgery. This case report can be a reference case in condylar fractures of professional soccer players, as the available scientific literature is limited with regard to return-to-play after maxillofacial fracture in professional athletes.
Keywords
Introduction
Sport-related mandibular fracture is one of the most common injuries in the field of the maxillofacial surgery. 1 –5 However, the scientific evidence is lacking with regard to return-to-play after maxillofacial fracture in professional athletes, 6,7 with the management of the mandibular fracture in professional soccer goalkeeper rarely being reported. 8,9 In this case report, mandibular condylar fracture in a professional soccer goalkeeper caused by impact with an opponent player was reported. The management for early return-to-play and face-guard for condylar fracture were discussed.
Case Report
A 32-year-old male professional soccer goalkeeper was transferred to Tokyo Women’s Medical University due to malocclusion after a collision with an opponent player during a night game in professional soccer J. League YBC Levain Cup. The patient’s mandible was displaced between the left lower lateral incisor and left lower canine. The patient crashed with an opponent player while running to clear the ball out during the game (Highlights of FC Tokyo vs Vegalta Sendai. 2019 J League YBC Levain Cup GS Section 5. https://youtu.be/PaXnpRReyeI.). Panoramic radiograph and computed tomography (CT) showed right condylar base fracture with medial displacement and left para-symphysis fracture (Figure 1). Simple tooth ligation with a wire was performed between the left lower central incisor and the first premolar for left para-symphysis fracture (Figure 2). The patient was admitted to the hospital, and an internal fixation using Innsbruck style retromandibular anterior trans-parotid approach with a 25-mm skin incision immediately below the earlobe 10,11 and intraoral mandibular vestibular approach were performed under general anesthesia 2 days after injury. Eight internal maxillomandibular fixation (IMF) screws were placed on the bilateral maxilla and mandible to perform temporary IMF during osteosynthesis, and the fracture of condyle and symphysis were fixed by using 2 four-hole mini-plates and screws on the ideal lines of the osteosynthesis (Figures 3 to 6). After the osteosynthesis, all IMF screws were removed. No postoperative IMF was performed. The patient showed no postoperative facial palsy. Soft diet and limitation of the mouth opening was instituted for 4 weeks after surgery. The patient took 600 kcal 3-4 times a day (1800-2400 kcal in total) for 4 weeks after surgery (e.g. soft food, 250 kcal; Ensure liquid dietary supplement [Abbott, Japan], 250 kcal; smoothie, 90 kcal; and protein, 80 kcal). The patient started mandibular protrusion and diduction exercises with limited mouth opening 3 days after surgery; each exercise was held for 6 seconds followed by a 6-second relaxation period. Each exercise was repeated 10 times at least 3 times a day. 12 The patient was discharged without complications 3 days after surgery. To achieve early return-to-play, the authors started rehabilitation based on Fowell and Earls’ return-to-play guidelines following facial fractures (Table 1). 13 The patient started moderate exercises such as stationary bike and core training 5 days after surgery, and then progressively full exercises without contact including jogging, running, strength training, and basic training 8 days after surgery. The patient started normal team training with a personalized jaw-guard 4 weeks after surgery. Mouth opening exercises and progressively normal diet were also started 4 weeks after surgery, with additional mouth opening exercises repeated for 5 min at least 3 times a day. His body weight decreased by 2.2 kg 1 week after surgery, gradually recovered, and finally became normal again 4 weeks after surgery.
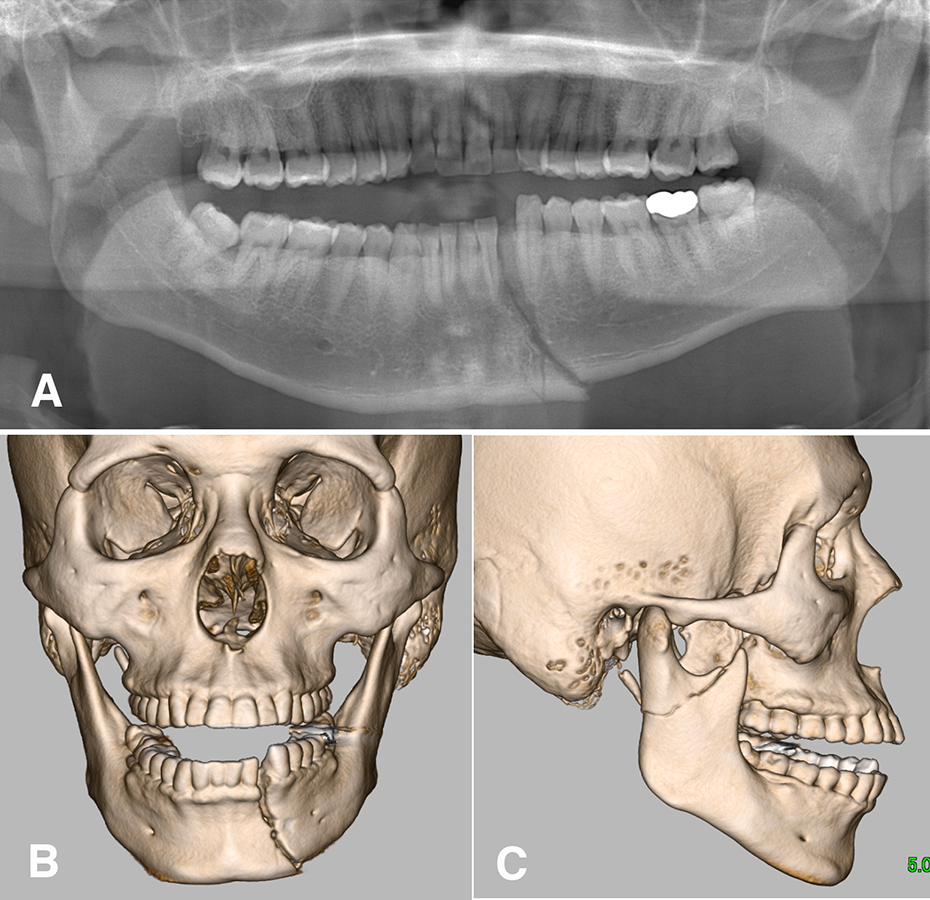
Mandibular fracture in a 32-year-old professional soccer goalkeeper. (A) Panoramic radiograph, (B) frontal and (C) lateral view of the 3-dimensional computed tomography (3D-CT) findings of the right mandibular condylar base and left para-symphysis fracture.
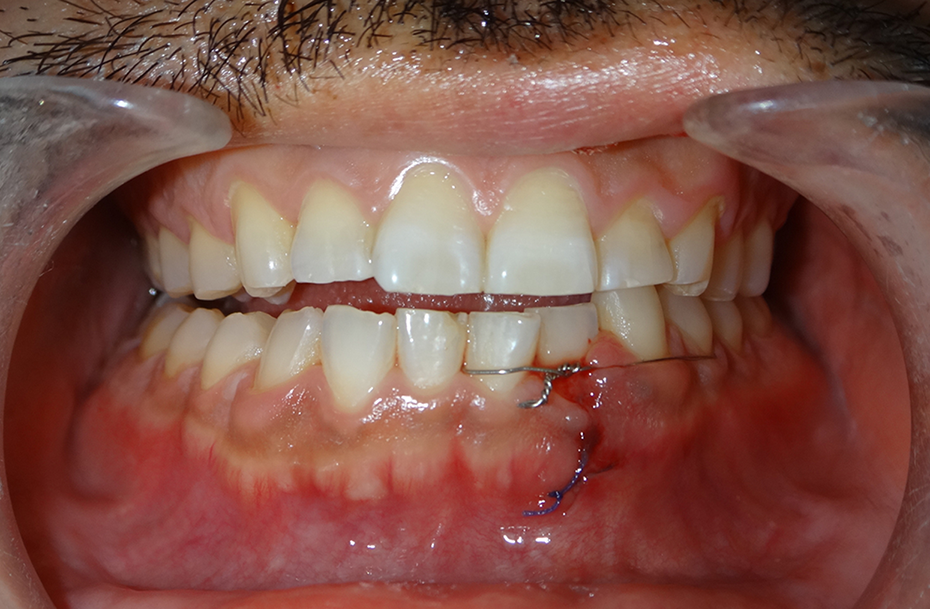
Intraoral photographs in the fracture of the left para-symphysis and the right condylar base before surgery. A malocclusion was noted on the right side. Left para-symphysis fracture was fixed via simple tooth ligation with a wire between the left lower central incisor and the first premolar upon admission.
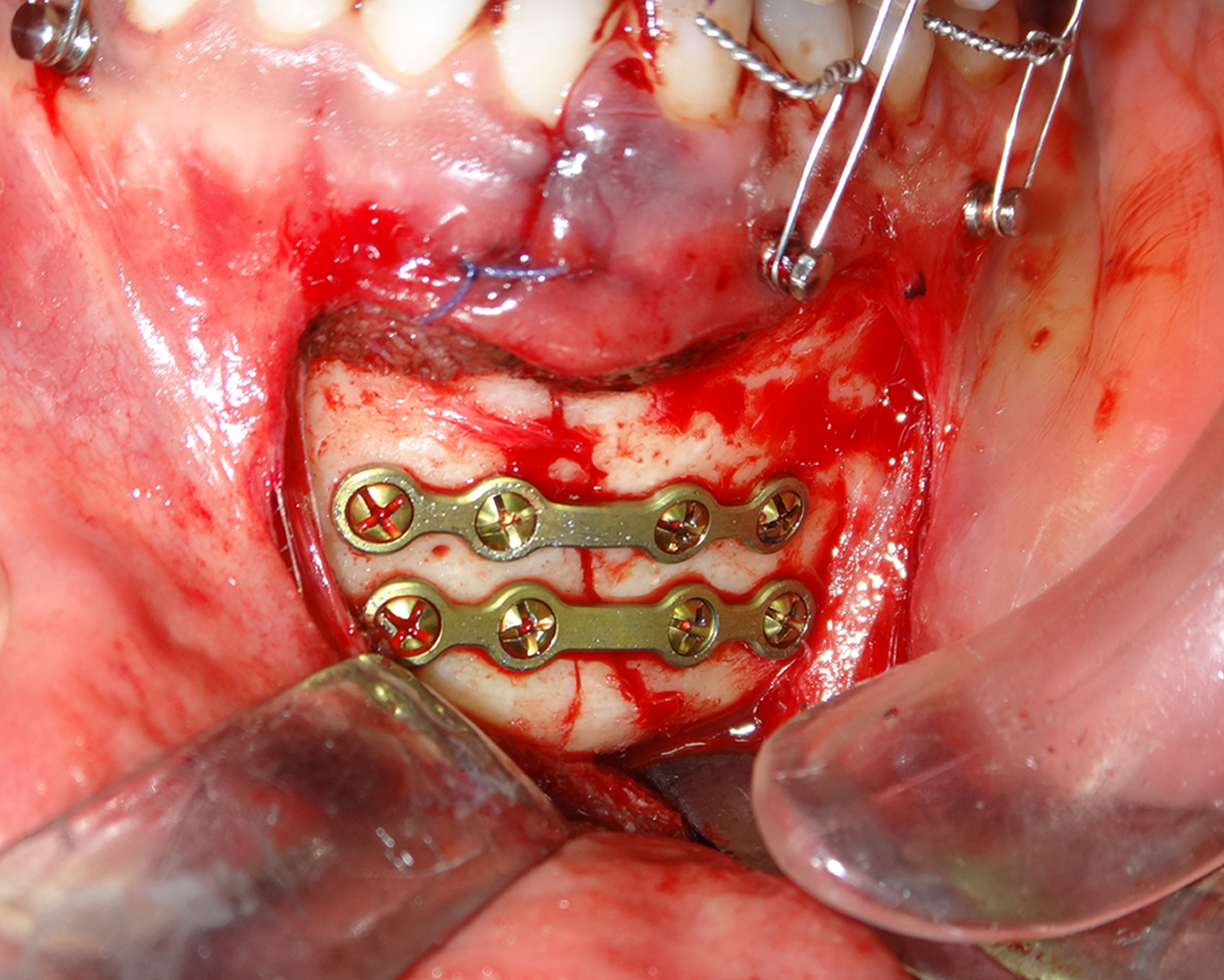
Intraoperative photographs of the internal fixation of the para-symphysis fracture using intraoral vestibular approach. The fracture of para-symphysis was fixed using 2-mini-plates and screws on the ideal lines of the osteosynthesis.
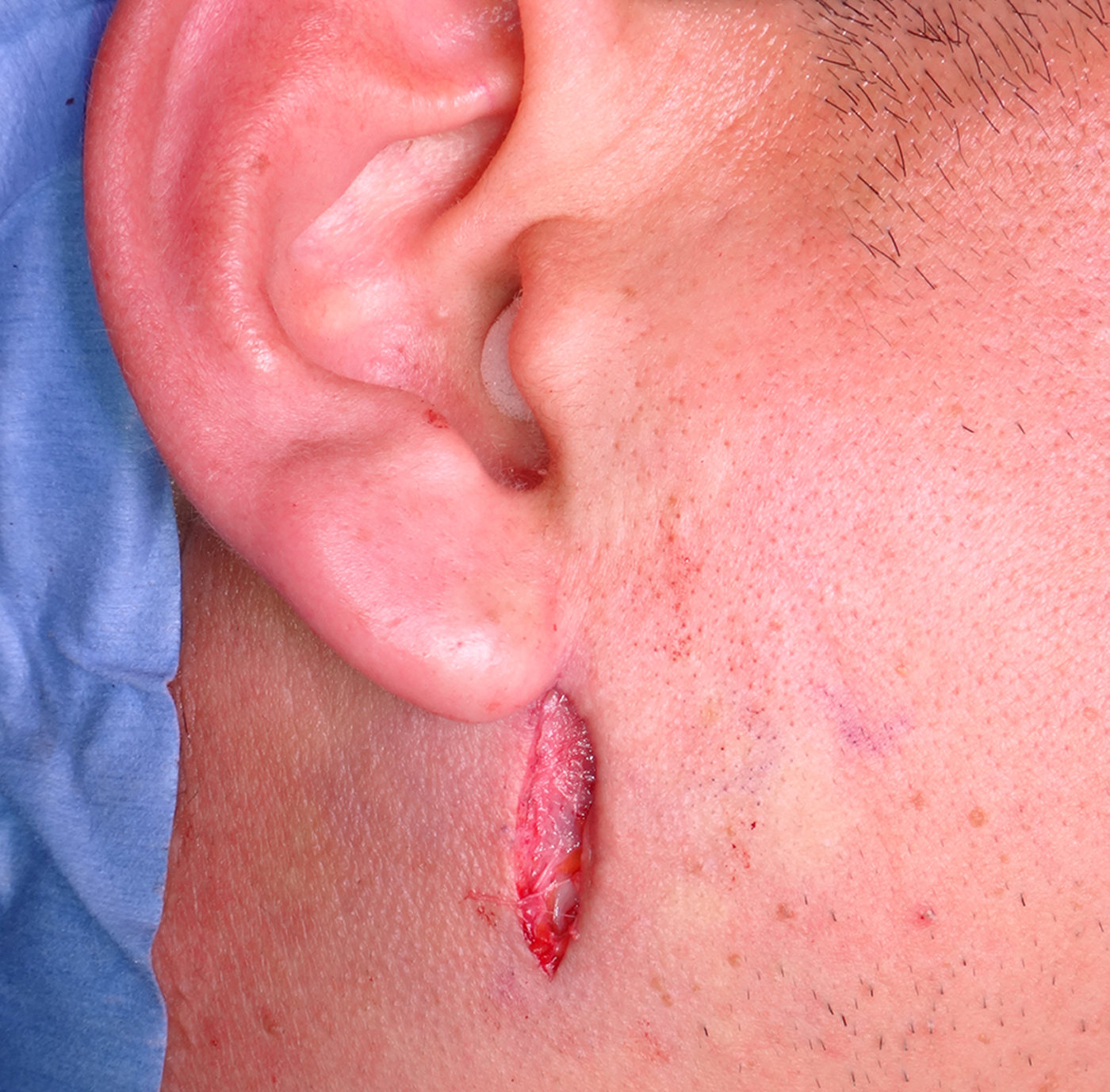
Intraoperative photographs of the internal fixation of the condylar base fracture using the Innsbruck-style retromandibular anterior trans-parotid approach. A 25-mm skin incision was made immediately below the earlobe.
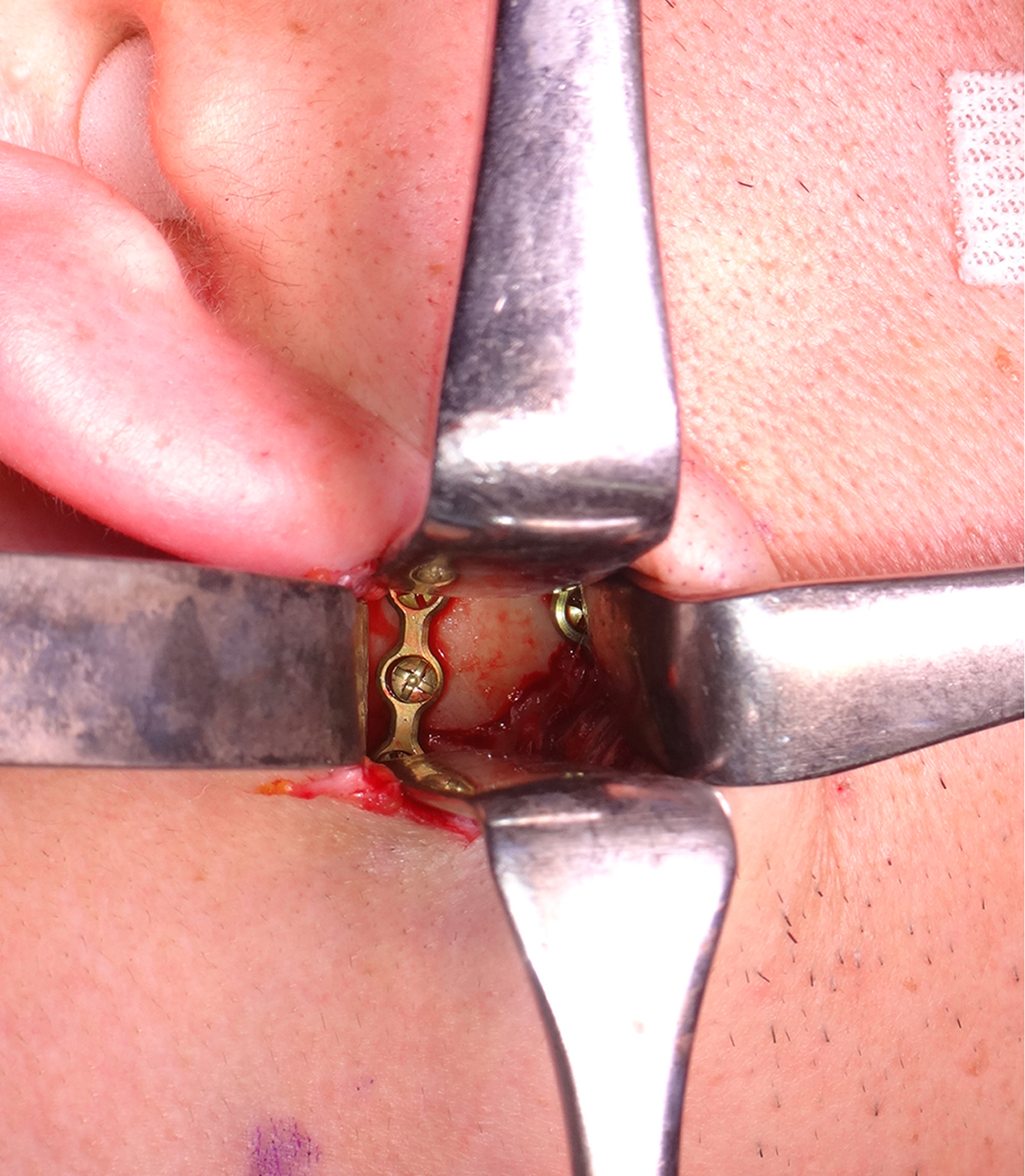
Intraoperative photographs of the internal fixation of condylar base fracture using the Innsbruck-style retromandibular anterior trans-parotid approach. The fracture of condylar base was fixed using 2-mini-plates and screws on the ideal lines of the osteosynthesis. The proximal segment of the condyle was placed totally four 7-mm screws.
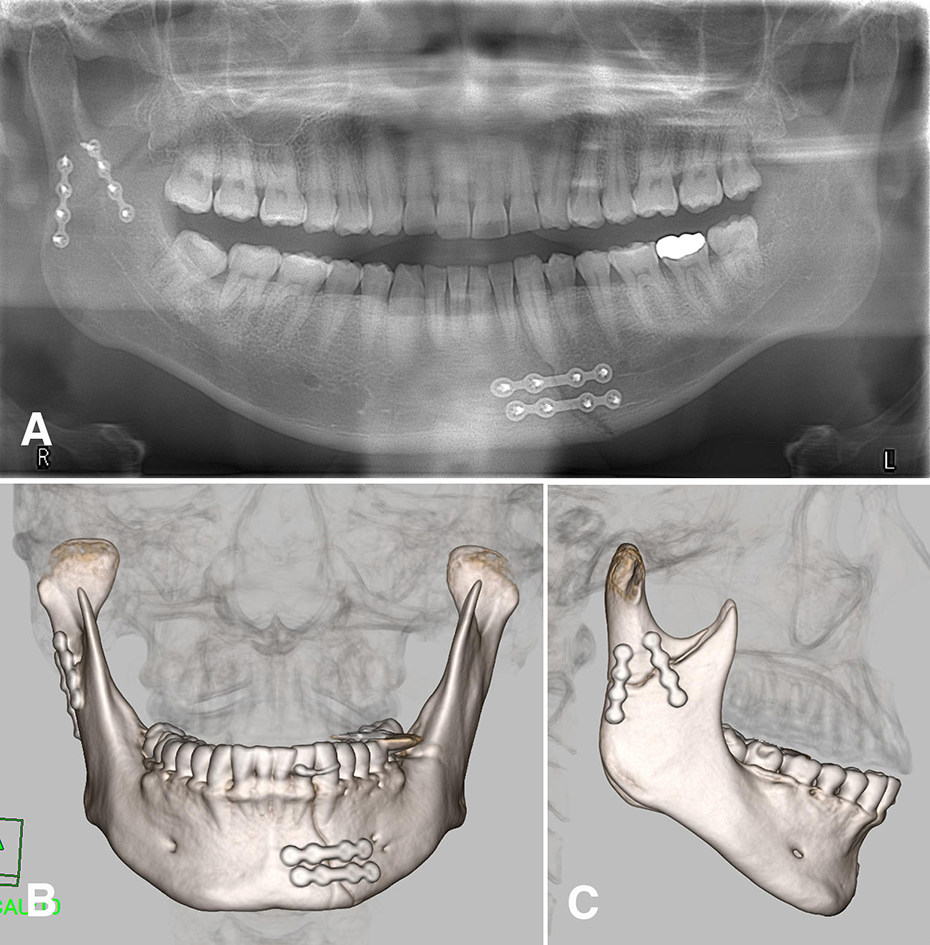
Postoperative panoramic radiograph and 3-dimensional computed tomography (3D-CT) findings. (A) Panoramic radiograph, (B) frontal view and (C) lateral view of 3D-CT.
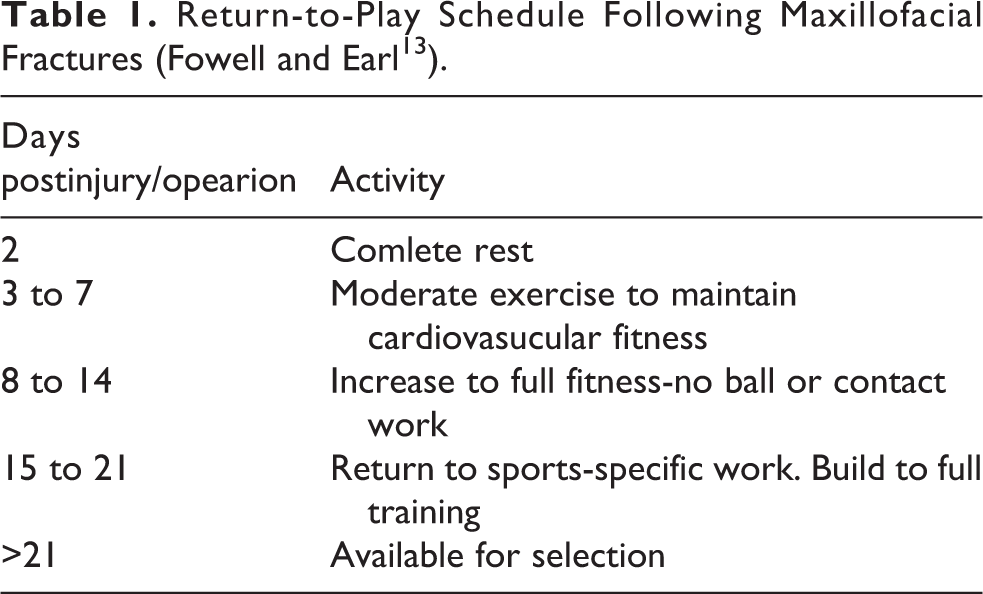
Return-to-Play Schedule Following Maxillofacial Fractures (Fowell and Earl13).
To make a jaw-guard for early return-to-play, a plaster wrap casting of the face was obtained with plaster bandage (Prusrungips, Alcare, Tokyo), by an orthotist 2 weeks after surgery. The jaw-guard was configured with 3 layers, composed of a hard outer surface, an inner cushion, and bandage; (1) the outer surface was made with 3-mm-thick high density polyethylene (HDPE) (breaking strength: 37 MPa/cm2, KI restra sheet, Keiai orthopedic appliance, Tokyo), (2) the inner cushion was a closed-cell-foam type polyethylene foam made of low density polyethylene and ethylene-vinyl acetate (Sunpelca, Sanwa kako, Kyoto), and (3) bandage was made of vneoprene. The jaw-guard covered the area from the left mandibular angle to the right ear, including the right condyle region. To improve breathability and hearing, the jaw-guard portion around the ear was perforated with 7 small holes. The bandage could be separated and washed (Figures 7 and 8).
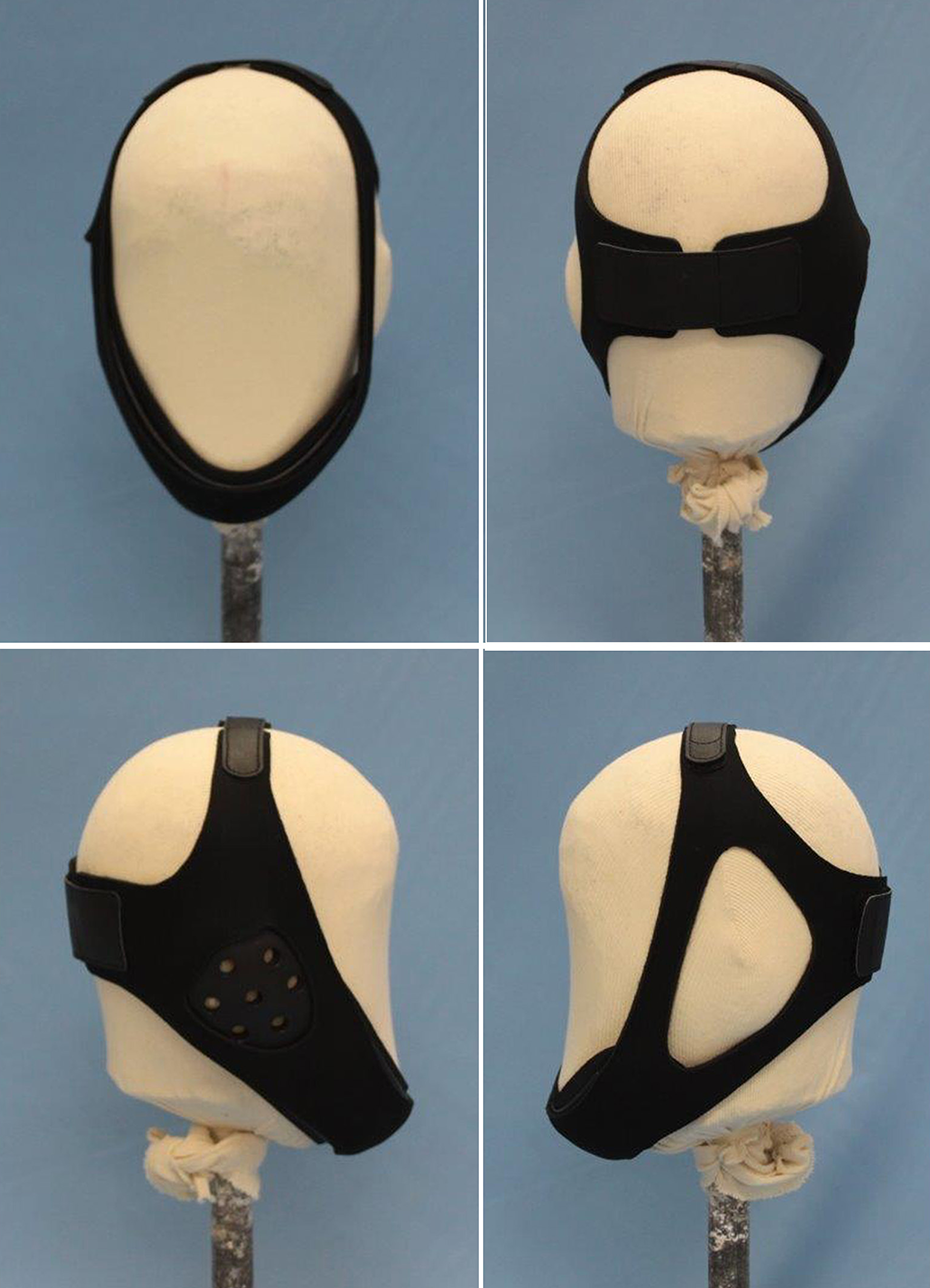
Photographs of the frontal, back, and lateral view of the patient specific jaw guard. The jaw guard is composed of 3 layers, including a hard outer surface, inner cushion, and bandage; the outer surface is made of high density polyethylene (HDPE), the inner cushion is made of closed-cell-foam type polyethylene foam made of low density polyethylene (LDPE) and ethylene-vinyl acetate (EVA), and the bandage is made of neoprene.
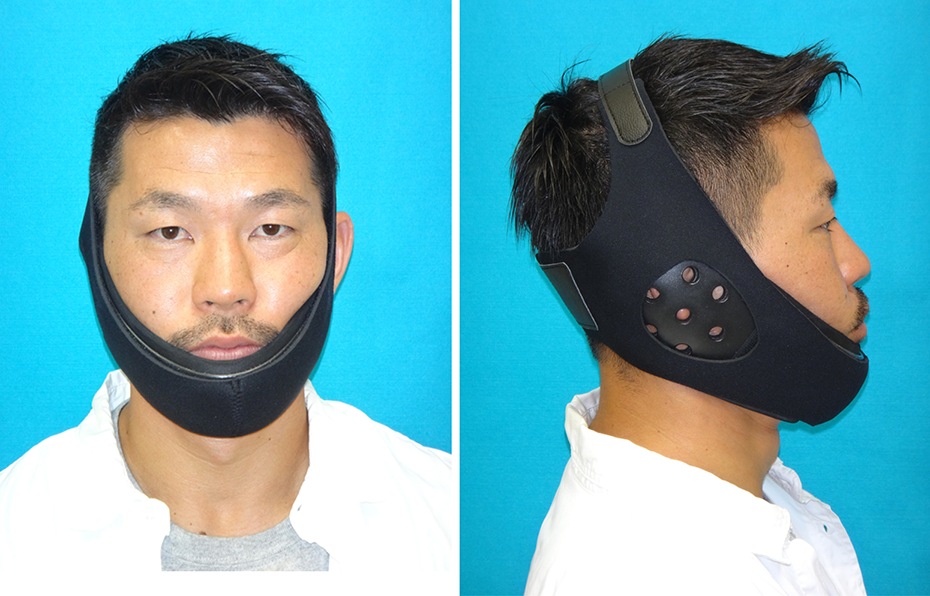
Photograph of the frontal and lateral view of the patient with the patient specific jaw guard.
The patient returned to play a game 2 months after surgery (Figure 9). The jaw-guard was used from 4 weeks after surgery until 3 months after surgery.

The patient wearing the jaw guard in a soccer game 2 months after surgery.
Discussion
Soccer is one of the most common sport-related cause of maxillofacial fractures. 2,3,5 Cerulli et al reported that zygomatic fractures (44%) and nasal bone fractures (29%) are prevalent among soccer-related maxillofacial fractures, followed by mandibular fractures (15%) and blow-out fractures (12%). These fractures are provoked by direct contact between players, including elbow impact, head impact, and a kick from a goalkeeper. The mandibular fractures occur more frequently in the angle (60%) than in the condylar region (40%). 2
Roccia et al reported 138 sport-related maxillofacial fractures in a retrospective study. They suggested that in the protocol for the follow-up of the maxillofacial fractures, following surgical intervention/injury, patients are advised to take 20 days of complete rest. Patients were encouraged to start light aerobic exercises 21-30 days after surgery/injury. Noncontact training drills are feasible 31-40 days after surgery/injury, and noncombat sporting activities may be restarted 41 days after surgery/injury. Combat sporting activities may be restarted 90 days after surgery/injury. 3 A systematic review conducted in 2019 regarding early return-to-play following maxillofacial fractures in professional athletes found that there are only 17 papers, including 1 prospective study (level 3) and 2 large retrospective studies (level 4). 3,5,7,13 Nowadays, the scientific evidence is still limited with regard to return-to-play after maxillofacial fractures in professional athletes. 6,7 A survey in the United Kingdom indicated that most consultant maxillofacial surgeons advise zygomatic fracture patients to refrain from contact sports for an average of 6 weeks after treatment, based on traditional practice and common sense. 14 Although non-professional athletes might accept long-term rest (e.g., for 3 months) as common sense, maxillofacial surgeons have to seek early return-to-play clearance for professional and semi-professional athletes, as long-term rest might jeopardize their patients’ professional careers. Fowell and Earl reported in a prospective study, which included 19 professional and semi-professional athletes who sustained 20 fracture cases in a football and rugby union, that return-to-play 3 weeks after surgery is possible following facial fractures. Following surgical intervention, patients are recommended to take 2 days of complete rest. For the first week after surgery/injury, patients are restricted to a moderate cardiovascular fitness regimen in order to maintain baseline fitness. This regimen is modified in the second week to rehabilitate patients back to full fitness. After 2 weeks, patients are allowed to resume sport-specific training, progressing to availability for selection at 3 weeks (Table 1). 13 The authors started rehabilitation based on Fowell and Earls’ return-to-play guidelines to achieve early return-to-play.
To achieve early return-to-play after maxillofacial fractures, patient-specific face guards have been recommended for professional soccer players, 4,8 although scientific evidence of the effectiveness of face guards following maxillofacial fractures in professional athletes is currently limited. 4 The face guard is required to fulfill the following 3 requirements: (1) protect the player from re-injury, (2) not hurt other players, and (3) not narrow the player’s field of vision. 15,16 The face guard is mainly composed of 2 layers of hard thermoplastic material and soft cushioning material to provide shock absorption properties. 4,8,15,16 The inner layer reduces the impact force and spreads it over a wider area. 4 Polymethyl methacrylate, polytrimethyl hexamethylene terephthalamide, Kevlar, and carbon fiber (Torayca, Toray, Tokyo) are used for the outer surface of face guards for professional soccer players. 4,8 There are also face guards for midfacial fractures, including nasal and zygomatic fractures. 4 Face guards for mandibular fractures in professional soccer players are rarely reported. 8 Moreover, little is known about face guards for condylar fractures. It is well known that condylar fractures are caused by direct and indirect forces, and as protection from both of these forces, head protection such as American football or hockey helmets would be effective, essentially protecting the player from condylar fractures. However, none of these helmets are permitted in soccer games. Koloskie and Orr reported a basketball player with mandibular symphysis and condyle fracture who used a hockey helmet during practice and an orthoplast nasal mask (Johnson & Johnson) during games. 17 In this case, the jaw guard was composed of 3 layers, including a hard outer surface, inner cushion, and bandage. The outer surface was made of HDPE. HDPE is lightweight, with high stiffness and strength properties, and ease of forming. It is used for hard corset in vertebral fractures. The jaw guard covers the areas from the left mandibular angle to the right ear, including the right condyle region, to reduce the impact force. This type of jaw guard might protect the wearer from condylar fractures caused by direct impact forces; however, it is unknown whether this jaw guard is enough to protect the condyle from indirect forces. Jaw guards for condylar fractures need further study with regard to its ability to prevent both direct and indirect fractures.
Rigid internal fixation is necessary for condylar fracture patients to achieve early return-to-play. Although various surgical approach to the condylar base fractures have been reported, 18 the authors performed the Innsbruck-style retromandibular anterior trans-parotid approach and a triangular-positioned double mini-plate osteosynthesis technique reported by Torre et al in this particular case. 10,11 Early recovery is possible with this approach as it is minimally invasive. This technique provides direct visualization of the condyle with a small incision (approximately 25 mm) and has lower incidence of facial palsy. No postoperative IMF is necessary. They reported the mean maximal interincisal distance as ranging from 38 mm after 1 week, to 45 mm after 6 months. Temporary facial palsy was reported in 3.9% patients, with an average recovery time of 3 months after surgery. No patient had occlusal disturbances or complications regarding the parotid gland or the osteosynthesis 6 months postoperatively. 10
In conclusion, to achieve early return-to-play, the authors managed mandibular condylar fracture of a professional goal keeper based on Fowell and Earls’ return-to-play guidelines following facial fractures. 13 The patient was able to return to normal team training with normal weight 4 weeks after surgery. It was faster than the average recovery time of 6-8 weeks. Using the Innsbruck-style retromandibular anterior trans-parotid approach with a 25-mm skin incision for condylar fracture would contribute to early recover due to its minimally invasive nature. 10 Further research is necessary regarding mechanical effects and morphology of the jaw guard for mandibular condylar fractures in athletes. This case report can be a reference case in condylar fractures of professional soccer players, as the available scientific is was limited with regard to return-to-play after maxillofacial fracture in professional athletes. 6,7
Footnotes
Acknowledgements
The authors thank Mr. Keisuke Niiyama, Mr. Tomonori Tada, and all the staff at Vegalta Sendai for their kind support and assistance. The authors also thank Mr. Kenichi Suzuki (Nippon Artificial Limbs Manufacturing) for fabrication of the patient-specific jaw guard; Dr. Masahiro Kumagai, Dr. Yuta Yanagisawa, and Dr. Tsuyoshi Kurobane (Tohoku Kosai Hospital) for their kind support and follow-up of the patient; and Prof. Tomohiro Ando for his valuable comments.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient Consent
Patient consent was obtained to publish the study.
