Abstract
Study Design
Case Report
Objective:
A severe condylar resorption following internal fixation of the mandibular condylar fracture is rarely reported.
Methods
A 35-year-old female caused bilateral condylar base fracture due to fall. She had no connective tissue autoimmune disease, no temporomandibular joint (TMJ) problems, and no history of the orthodontic treatment. Each fractures of condyles were fixed by 2 none-locking titanium miniplates on ideal lines of the osteosynthesis.
Results:
6 months after surgery, although patient showed no malocclusion and no TMJ pain, panoramic X-ray showed left side condylar head resorption. Twelve months after surgery, bilateral plate removal was performed. Twenty-six months after internal fixation, panoramic X-ray showed bone formation at the left side of the condylar head. Magnetic resonance imaging of the TMJ showed left TMJ disc displacement without reduction and severe deformity of the left condylar head.
Conclusions
The condylar resorption might be caused by increasing functional loading due to new position of the condyle following osteosynthesis. Possible contributors for condylar resorption following osteosynthesis were: (1) internal fixation in bilateral condylar fracture, (2) disc displacement without reduction, and (3) female patient (hormonally-mediated theory, eg estrogen). However, the mechanize of condylar resorption was unclear and the further studies were necessary.
Keywords
Introduction
A severe condylar resorption following internal fixation of the mandibular condylar fracture is rare. A systematic review indicates that condylar resorption following internal fixation is .09% in condylar fractures. 1 Whereas, Iizuka et al has been reported that condylar resorption is radiologically noted in all cases following internal fixation of the condylar fractures with dislocation. 2 Condylar resorption has been associated with rheumatoid arthritis, temporomandibular joint (TMJ) internal derangement, trauma, steroid use, systematic lupus erythematosus, scleroderma, other vascular collagen diseases, orthodontic treatment, and orthognathic surgery.3,4 In this study, severe condylar resorption after internal fixation in bilateral condylar fracture was reported.
Case Report
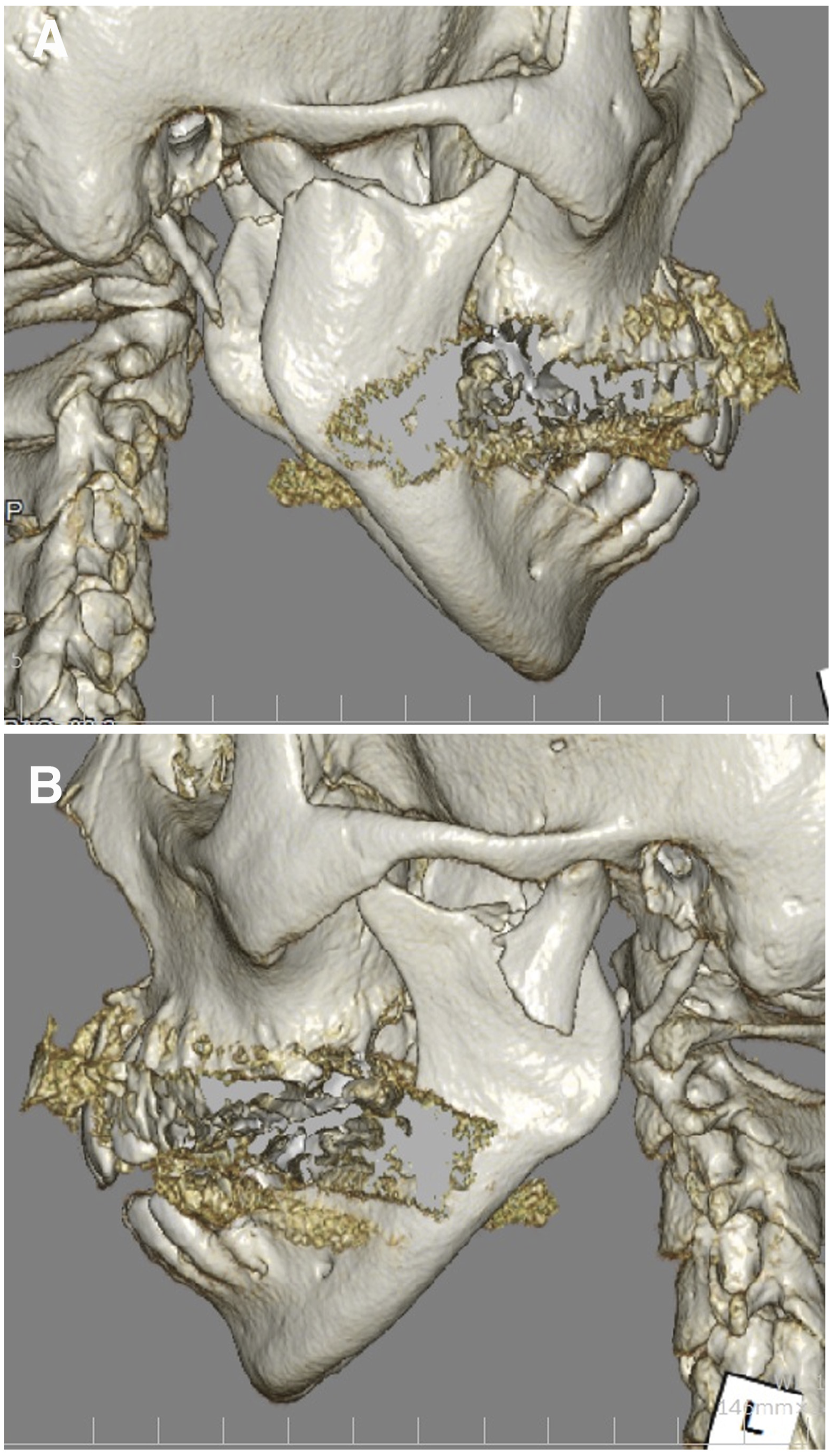
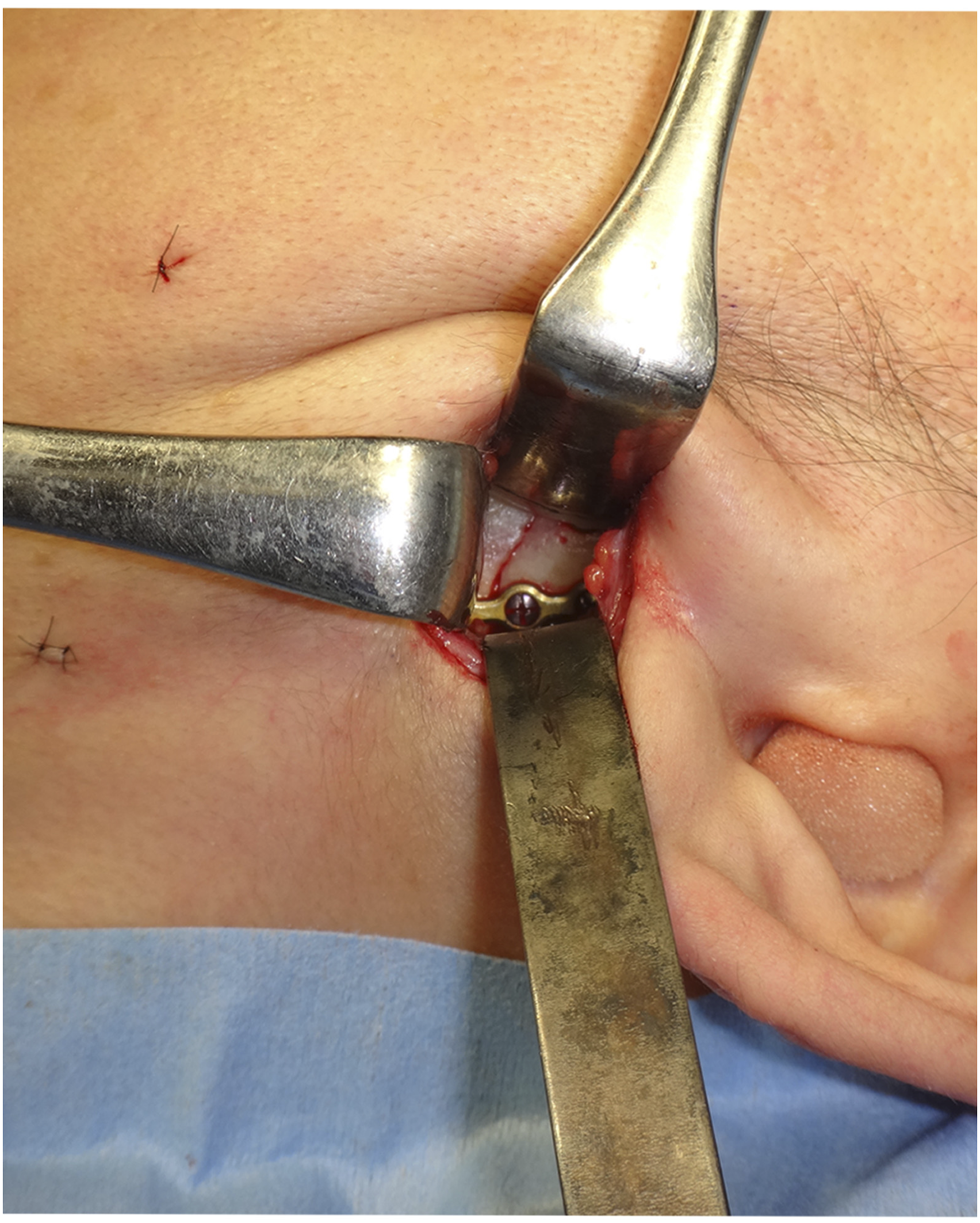
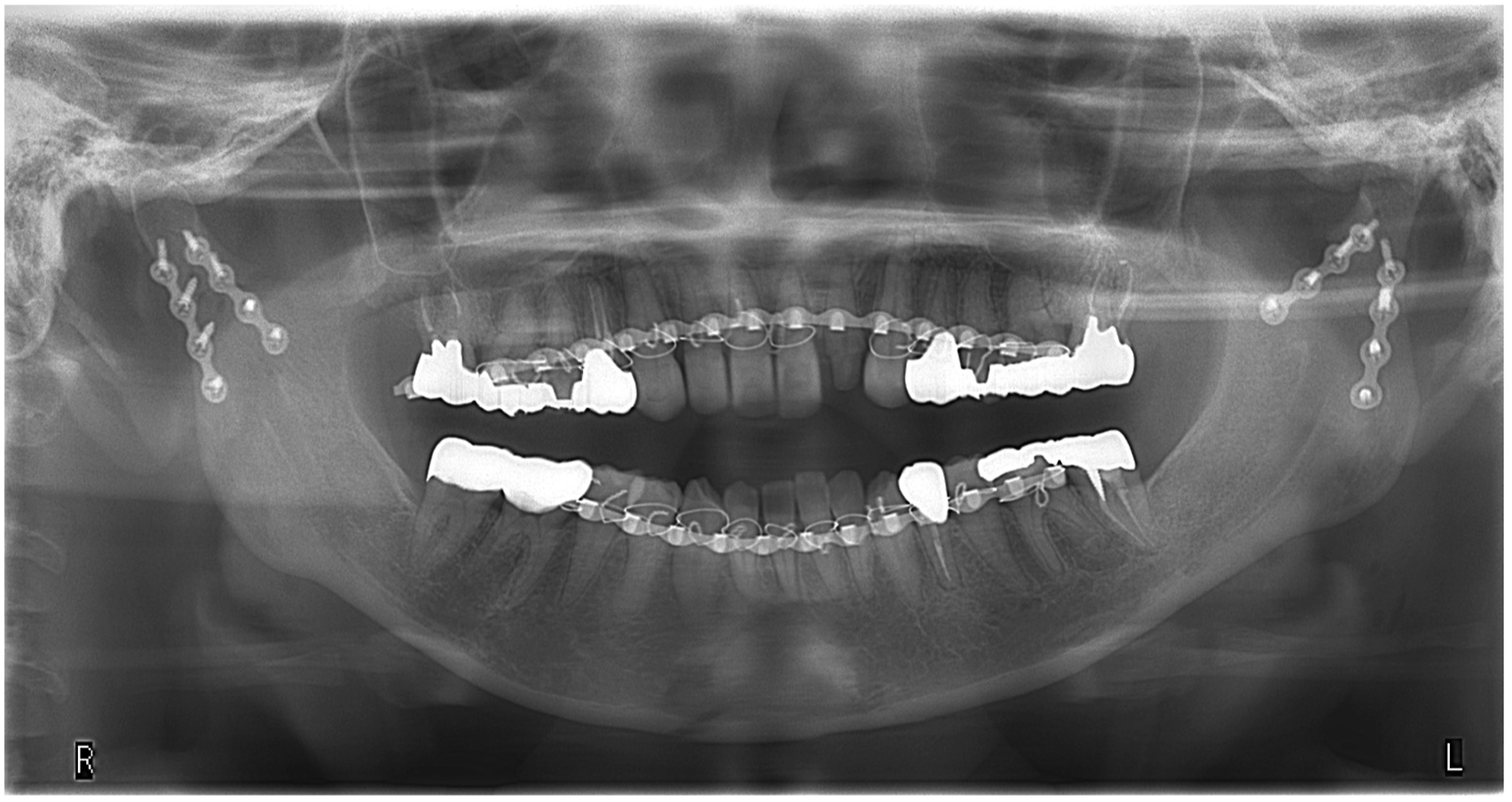
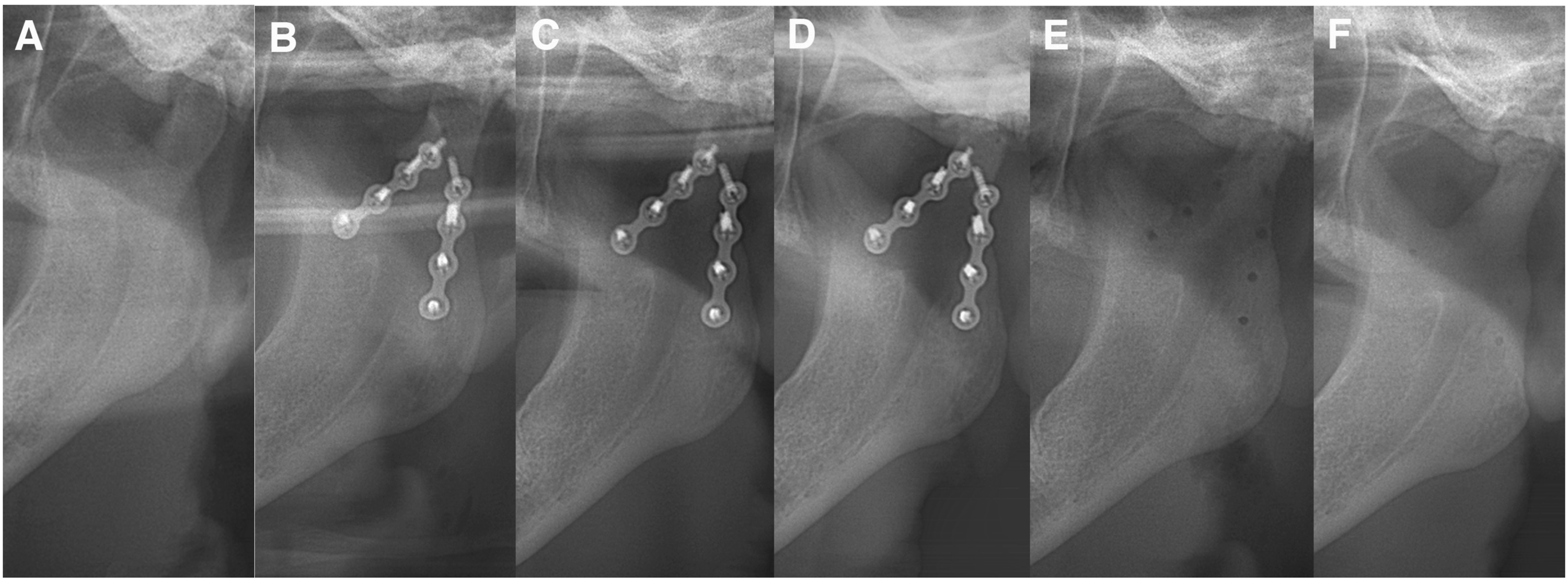
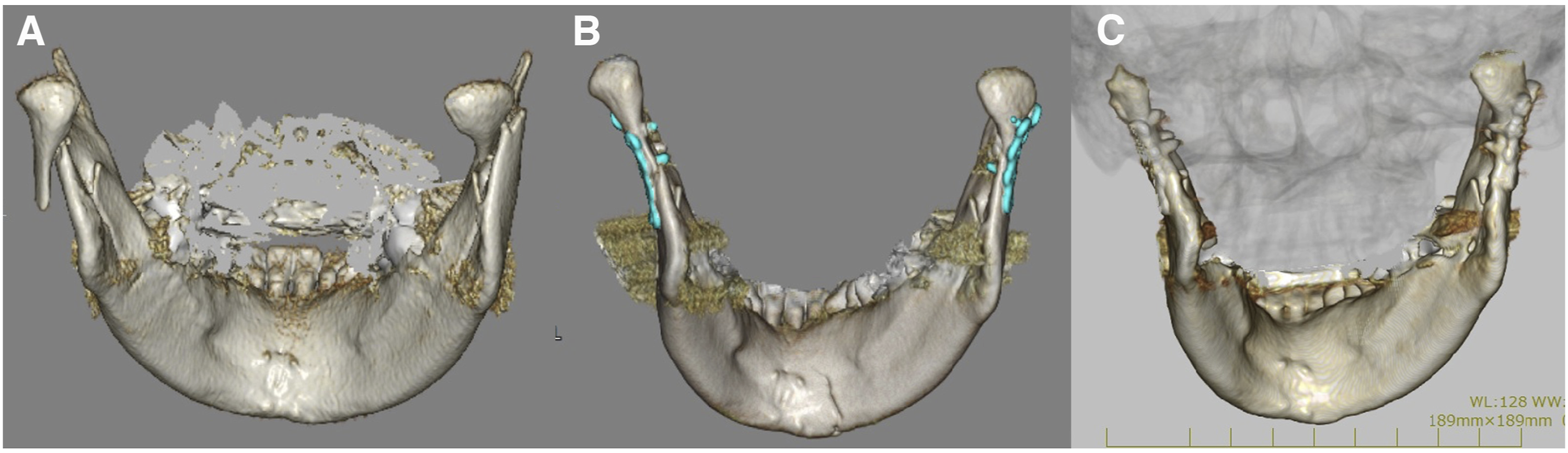
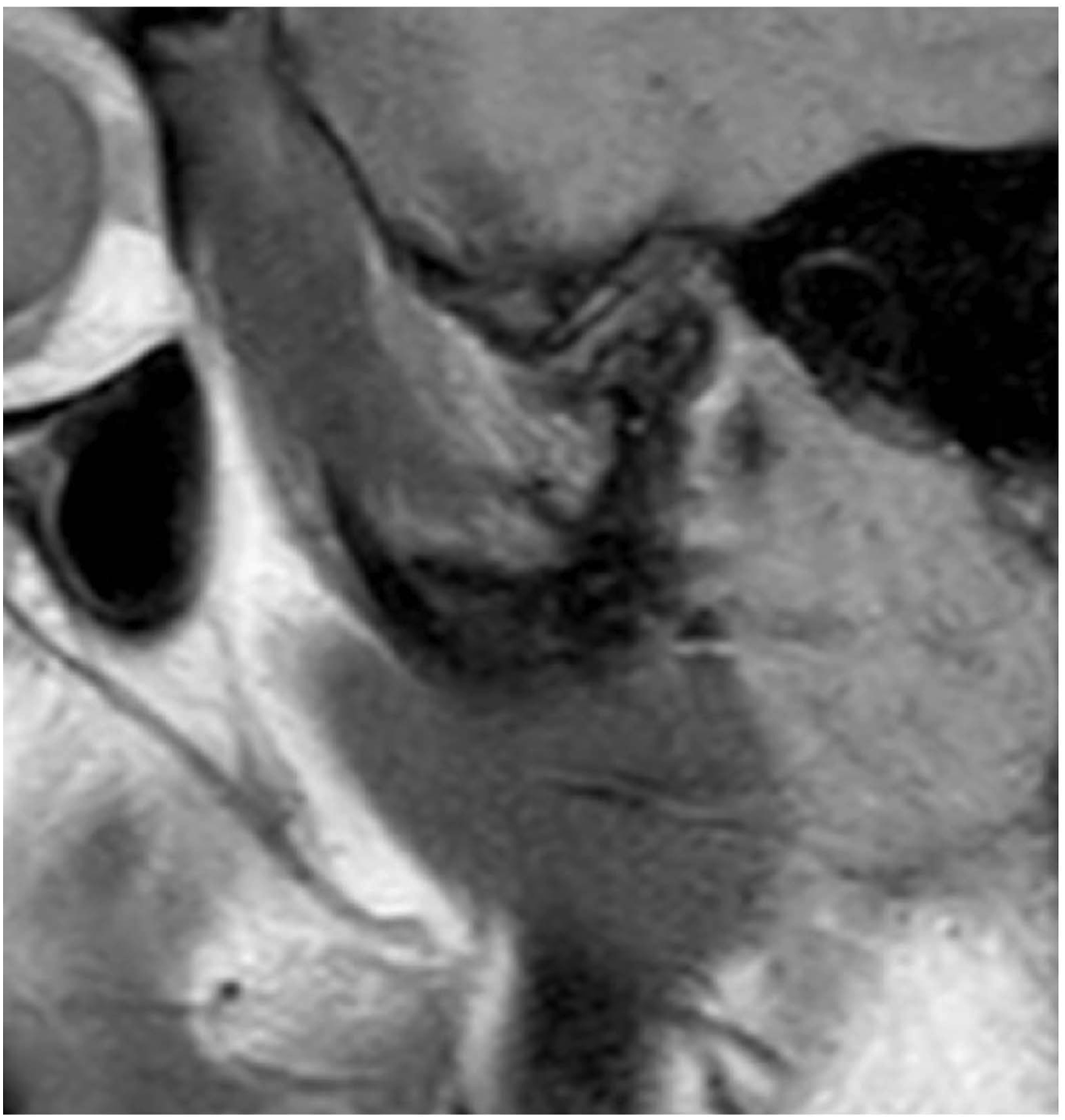
A 35-year-old female was referred to our department due to condylar fracture caused by fall. The patient showed malocclusion, trismus, luxation of the maxillary incisors and lacerations of the lower lip and chin. Panoramic X-ray and computed tomography (CT) showed bilateral condylar base fracture with lateral displacement at the left, and medial displacement at the right condyle (Figures 1, 2, 5(a), 6(a)). She had anemia and no autoimmune disease such as rheumatoid arthritis, Sjogren’s syndrome and systemic lupus erythematosus, and she had no medication use. She never showed TMJ problems, including dysfunction, pain and sound of the joint, and any other body joint issues. She had no history of the orthodontic treatment. An internal fixation using retromandibular anterior trans-parotid approach5–7 were performed under general anesthesia at 12 days after injury. Each fractures of condyles were fixed by 2 four-hole-miniplates (none-locking 2.0 mm titanium miniplate and 5 mm or 7 mm screws) on ideal lines of the osteosynthesis (Figure 3). No bilateral lateral pterygoid muscles were detached during surgery. No postoperative internal maxillomandibular fixation was performed after surgery. The patient showed no postoperative facial palsy. The postoperative X-rays showed good reduction and fixation (Figures 4 and 5(b)). Whereas, the postoperative CT showed acceptable reduction and good fixation (Figure 6(b) Panoramic radiograph findings of the bilateral mandibular condylar fracture in a 35-year-old female. Three-dimensional computed tomography (3D-CT) findings in the bilateral condylar fracture. (a) Right condylar base fracture with medial displacement. (b) Left condylar base fracture with lateral displacement. Intraoperative photograph of the internal fixation of left condylar base fracture using the Innsbruck-style retromandibular anterior trans-parotid approach. The fracture of condylar base was fixed using 2 non-locking-miniplates and screws on the ideal lines of the osteosynthesis. The proximal segment of the condyle was placed totally 4 screws. Panoramic radiograph findings of the bilateral mandibular condylar fracture immediate after internal fixation. Panoramic radiograph finding of the left condyle (a) before, (b) immediate, (c) 6 months, (d) 9 months, (e) 12 months (immediate post plate removal), (f) 26 months after internal fixation. Three-dimensional computed tomography findings (back view) (a) before, (b) immediate, (c) 12 months after internal fixation. Magnetic resonance imaging finding of left temporomandibular joint at mouth opening at 26 months after internal fixation (14 months after plate removal). TMJ disc displacement without reduction and severe deformity of the left condylar head were noted. The disc was displaced anteriorly and had degenerative changes.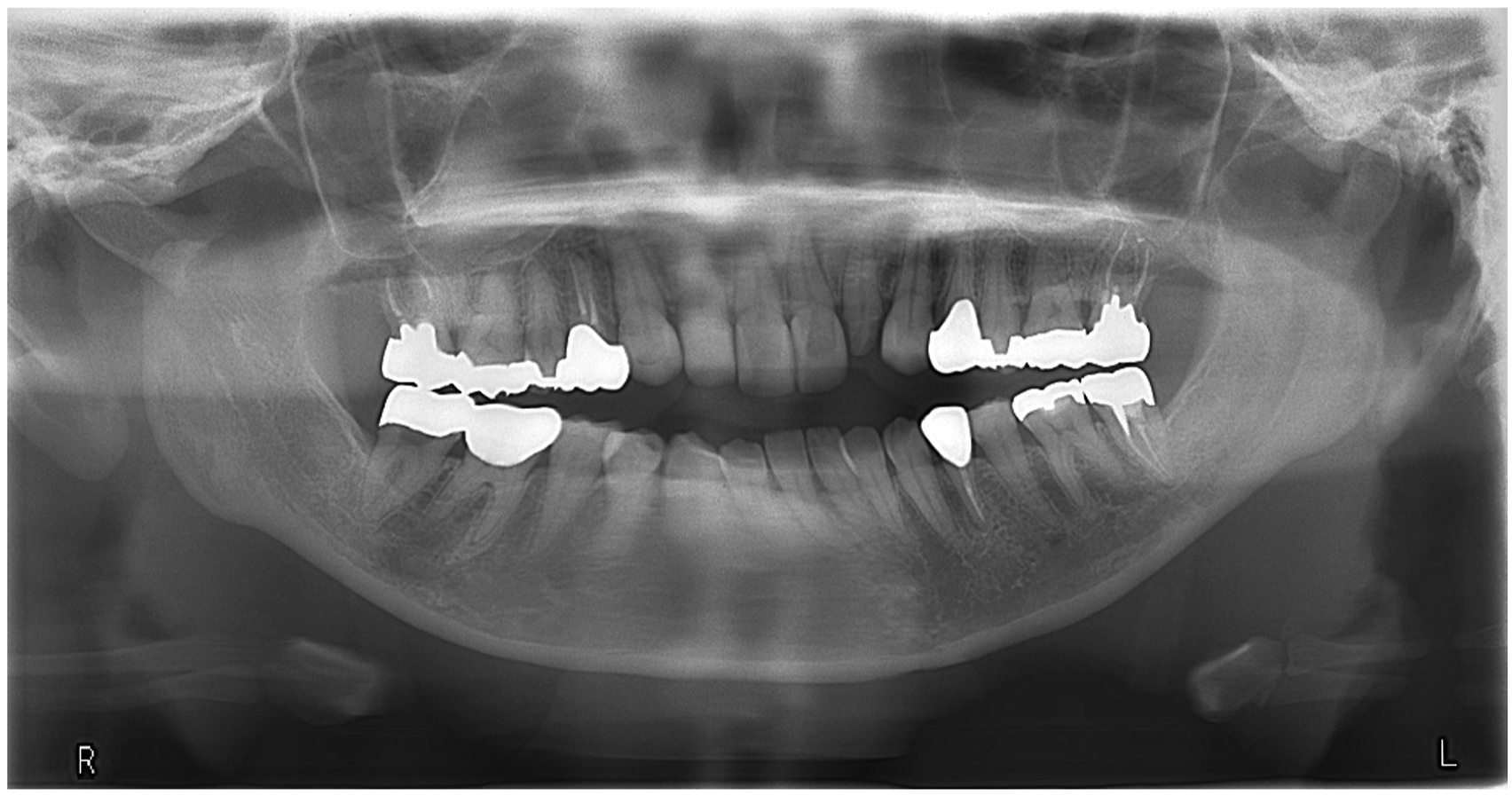
Discussion
Systematic review regarding the complications of the condylar fractures treated by surgical or conservative treatment indicates that condylar resorption following internal fixation and closed treatment are .09% and 0%, respectively. 1 Whereas, Oezmen et al has been reported 80% condylar fracture treated conservatively show condylar head deformation. In comparison, none of the patients from the surgically treated condylar fracture show any deformation of the condylar head on MRI examination. 8 Iizuka et al has been reported that 13 condylar fractures with dislocation from the glenoid fossa. They are treated by internal fixation with miniplates, and condylar resorption is radiologically noted in all cases on average 18 months follow up. However, no correlation between the clinical results and the changes detected radiologically are noted. 5 It is indicated that condylar resorption following internal fixation might be not rare. The condylar resorption might just not be noticed, because (1) panoramic X-ray might be difficult to detect the minor change of the condylar head, and (2) it might show no symptoms of TMJ and no malocclusion. Moreover, they reported that detachment of the condyle during surgery also has no correlation between the rate and degree of resorption. And then, condylar resorption are markedly more severe than cases treated by none-rigid fixation with the trans-osseous wiring and subsequent IMF for 3 to 7 weeks. 2 They considered that nutritional disturbance to the condyle is not the main cause of the condylar resorption, and the condylar resorption is caused by increasing functional loading due to new position of the condyle following osteosynthesis. 2 In this case, although the patient showed good clinical results after surgery, unilateral condylar resorption was noted at 6 months after surgery, and interestingly bone formation of the condylar head was noted at 26 months after internal fixation (14 months after plate removal).
Condylar resorption has been associated with rheumatoid arthritis, TMJ internal derangement, trauma, steroid use, systematic lupus erythematosus, scleroderma, other vascular collagen diseases, orthodontic treatment, and orthognathic surgery.3,4 Progressive condylar resorption (PCR) following eg orthognathic surgery is well documented, but the mechanize of resorption is still unclear. Review of literature regarding PCR indicates that there are 3 main aetiological theories: (1) sex hormone-induced necrosis, (2) avascular necrosis caused by pathological compression of the condyle, and (3) resorption caused by loss of the capacity to remodel. 9 It is well known that PCR following orthognathic surgery is mainly caused in young female.3,4,9,10 There are no laboratory tests specific for PCR. 4 Disc displacement without reduction has also been associated with the development of PCR. 10
In this case, connective tissue autoimmune diseases, direct trauma to the condylar head (indirect fracture via chin was suspected), TMJ internal derangement and orthodontic treatment were ruled-out as a factor. TMJ disc displacement without reduction was found at the resorption side of the condyle but not contralateral side. The left condylar base fracture was laterally displaced indicating likely rupture of the lateral ligaments of the joint, whereas on the right side, the condylar segment was medially displaced which likely would have had little to no impact on the lateral ligaments. This would be expected as displacement of the articular disc could initiate a cascade of events that lead to condylar resorption. MRI findings at 26 months after internal fixation showed the degenerative changes of the disc (Figure 7). This suggested that the disc displacement might be a result of the injury, because the patient had no TMJ dysfunction and sound before injury. Wang et al indicate that disc displacements in condylar fractures with dislocation and without dislocation are 97% and 30%, respectively on MRI evaluation. 11 Takaku et al has been reported that all discs were displaced in an anteromedial direction along with the fractured condylar fragments in ten patients with condylar and subcondylar fractures at 2 to 12 days after injury. 12 Cho et al reveals that 4 (20%) of the 20 cases show the disc displacement without reduction on MRI evaluation after internal fixation of the condylar fractures. Three of the 4 cases had a high condylar neck fracture with dislocation and 1 had a high condylar neck fracture with displacement. It is indicated that repositioning the dislocated condyle did not always lead to anatomical restoration of the joint structures. 13 Oezmen et al has been reported that disc displacement is noted in 30% cases in conservative therapy group and in 10% case in the surgery group. In each group two, 10% case have disc displacement at the nonfractured side on MRI evaluation. 8
In conclusion, the condylar resorption might be caused by increasing functional loading due to new position of the condyle following osteosynthesis in this case. 2 Possible contributors for condylar resorption following osteosynthesis were: (1) internal fixation in bilateral condylar fracture (it might be changed condylar head position following internal fixation more than unilateral condylar fracture, it increased functional loading to the condylar head), (2) disc displacement without reduction, and (3) female patient (hormonally-mediated theory in PCR, eg estrogen). 9 However, the mechanize of condylar resorption was unclear and the further studies were necessary.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was given by the Ethics Committee of the Tokyo Women’s Medical University (reference number 4610-R3).
Informed Consent
Written patient consent was obtained.
