Abstract
Additive manufacturing or 3-dimensional (3D) printing technology has an incredulous ability to create complex constructs with high exactitude. Surgical guides printed using this technology allows the transfer of the virtual surgical plan to the operating table, optimizing aesthetic outcomes, and functional rehabilitation. A vast variety of materials are currently being used in medical 3D printing, including metals, ceramics, polymers, and composites. The guides fabricated with titanium have high strength, excellent biocompatibility, and are sterilizable but take time to print and are expensive. We have thus followed a hybrid approach to fabricate an inexpensive surgical guide using metal where the advantage of 3D printing technology has been combined with the routinely followed investment casting procedure to fabricate guides using nickel–chromium, which has all the advantages of a metal and is cost-effective.
Keywords
Additive manufacturing (AM) or 3-dimensional (3D) printing is gaining more and more attention, especially in the head and neck surgical specialties. This technology has an incredulous ability to create complex constructs with high exactitude. Maxillofacial surgical procedures benefit immensely as it improves the esthetic and functional outcomes along with the predictability of the procedure. 1 Surgical guides allow the transfer of the virtual surgical plan to the operating table.
The ideal guide design should be such that it is not too bulky to block the surgical field and interfere with the surgical procedure or not too thin that it is likely to break and lacks strength to withstand the procedure. It should be biocompatible and should not leave traces of the material at the surgical site. Surgical guides are generally designed and printed using biocompatible resin. This is designed following a specific computer-aided design and computer-aided manufacturing protocol. Although stereolithography materials have the property of high stiffness along with its fine detailing quality, it may be expensive and not easily available in all centers. 2 It also becomes brittle when exposed to ultraviolet curing light. Guides fabricated with titanium have high strength, low density, resistance to corrosion, and excellent mechanical properties. 3 Additionally, they have good biocompatibility and are sterilizable, which makes it ideally suited for medical prostheses, dental implants, and surgical guides. Despite all these benefits, the main drawback is that they take time to print and are expensive. 3 To overcome these, we developed a hybrid approach to fabricate an inexpensive surgical guide using investment metal casting, utilizing 3D printing technology. These guides were used in a patient with right temporomandibular joint ankylosis presenting with reduced mouth opening and facial asymmetry. A single surgical procedure was done to release the ankylosis and to correct the facial deformity using extended lateral sliding genioplasty.
Methods
Simplified Digital Workflow
A preoperative computed tomography (CT) scan of the patient was taken (Ingenuity core 128 – Phillips multislice CT) and imported in Digital Imaging and Communication in Medicine format. A virtual 3D volumetric reconstruction was created in 3D Slicer 4.11.0 4 and exported in stereolithography tessellation language format. Virtual surgical planning of the osteotomy cuts in the ankylosis region and genial segment was performed, and osteotomy guides were designed (Meshmixer 3.3.15, Autodesk). The genioplasty guide was designed to avoid the mental nerves bilaterally and to protect the root apices. On the other hand, the ankylosis release guide was designed to get the accurate direction of the osteotomy plane and prevent injury to the mandibular foramen.
The guide designs were exported to a 3D resin printer (ProJet MJP 2500 W) and printed using castable resin (GC Corp.; Figures 1 and 2), which were invested in silica (Bellasun, Bego & Co.) and placed in a furnace similar to the procedure followed for casting dental crowns. It was initially heated to 150 °C to melt the resin and create a mold. The temperature was then raised to 930 °C to burn out any residual wax. The nickel–chromium (Ni-Cr)-based dental alloy (Scheftner) was filled into the mold using a vacuum casting technique to ensure complete filling of the dye created. No further post-processing was required. The guides were checked on a polylactic acid (PLA) 3D printed model for proper fit, and a mock surgery was performed. The guides were autoclaved in a steam sterilizer at the temperature of 121°C and pressure of 15 psi for 15 minutes prior to surgery.
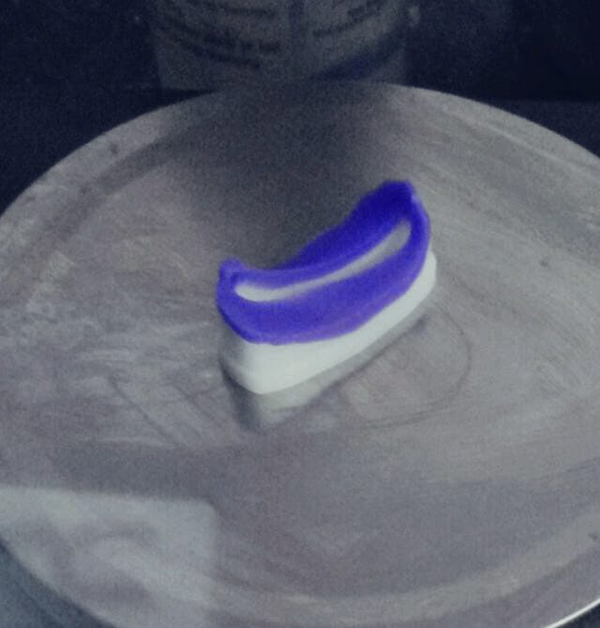
Wax pattern design for the TMJ ankylosis release guide. TMJ indicates temporomandibular joint.

Wax pattern design for genioplasty guide.
Surgical Procedure
The ankylotic mass was exposed using an Al Khayat and Bramley incision. The ankylosis release guide was placed as planned, which fit snugly into the surgical site, and the ankylosis was released with a guide in place (Figure 3). A temporalis interpositional arthroplasty was done, and the site was sutured. The genial segment was exposed intraorally, and bilateral mental nerves were identified. The genial osteotomy (genioplasty) guide was placed in position, and osteotomy was performed (Figure 4). The guide helped achieve a symmetrical cut while protecting the vital structures. After rotation and advancement of the genial segment, the preadapted plates were fixed. Postoperatively, the patient achieved satisfactory results with adequate mouth opening, range of motion, and obtained a functional outcome of the surgery (Figures 5 and 6).
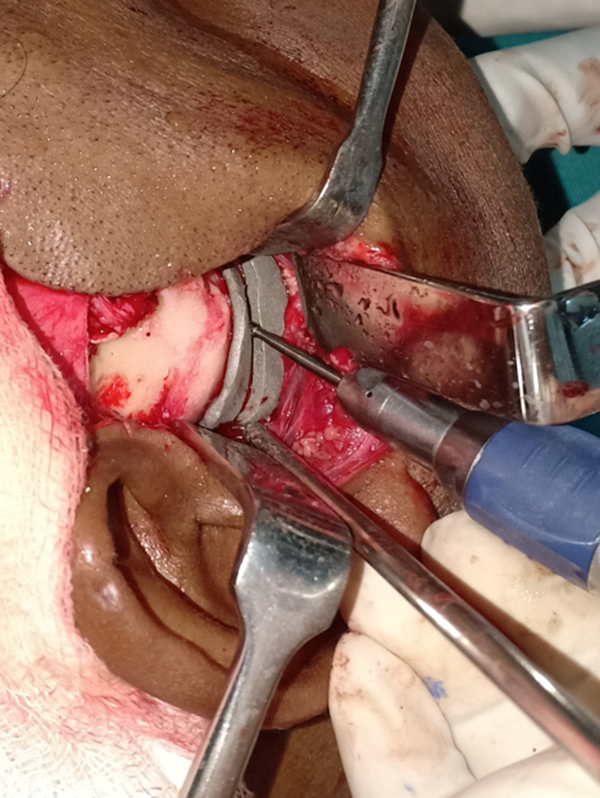
TMJ ankylosis cast metal guide in position intraoperatively. TMJ indicates temporomandibular joint.
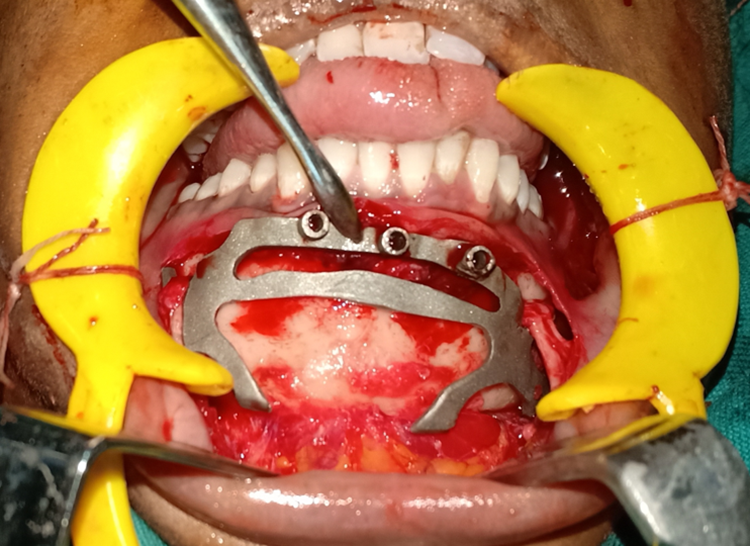
Genioplasty cast metal guide in position intraoperatively.
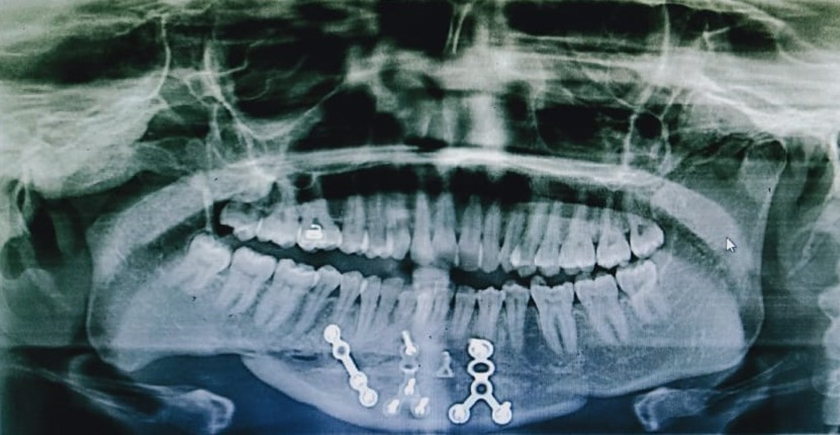
Postoperative orthopantogram.
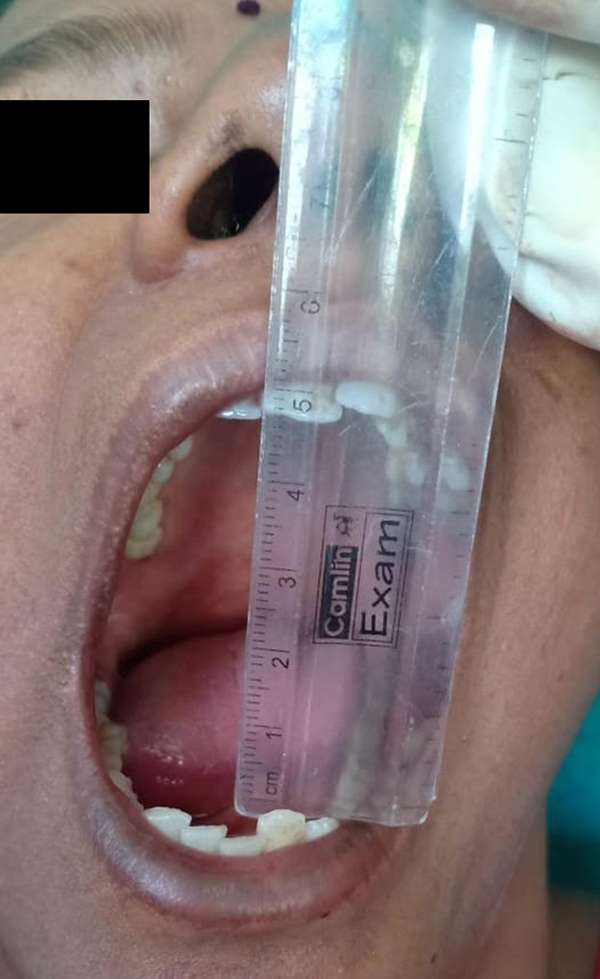
Mouth opening at 6-month follow-up period.
Discussion
Ankylosis of the TMJ is a challenging problem for both the patient and the surgeon. Meticulous preoperative virtual surgical planning is becoming more common in several clinical settings. However, precise virtual surgery planning is of no value if it cannot be transferred to the operating room. To ensure this, 3D printed photopolymeric resin surgical guides, and laser-melted titanium cutting guides have been developed. 1 However, there is a cost associated with the time, effort, and materials needed to design and manufacture these surgical guides.
To mitigate the concerns, we report an inexpensive, hybrid manufacturing approach to fabricate ankylotic and genioplasty surgical guides in biocompatible dental alloy material, combining 3D printing and investment casting technologies. The surgical guides were fabricated in Ni-Cr-based dental alloy material.
Ni-Cr-based dental casting alloys are widely used in dentistry, especially in contact with oral tissues for many years for the fabrication of crowns, bridges, and implant prostheses. These alloys have also been used in the field of orthopedics as surgical instruments. 5 Like titanium, Ni-Cr-based biocompatible alloy exhibits a high corrosion resistance, fatigue strength, and good biocompatibility properties. 6 Er and Unsaldi investigated the in vivo cytotoxicity and biocompatibility properties of Ni-Cr-based bone implant and concluded that a dental alloy with an open pore structure could also be used as a biocompatible hard tissue implant material for orthopedics. 7 But it is well-known that Ni contact can result in an allergic response and is the most common sensitizer among all metals. 8
Moreover, as Ni sensitivity has been reported with its long-term use inside the body, the European Union (EU) has accordingly decreed a directive stating that all metallic parts that are inserted into the human body must not have a Ni release rate higher than 0.2 µg/cm2/week. Besides, in certain countries such as Sweden and Denmark, Ni-Cr alloys are subjected to more stringent regulations and even banned due to the presence of Ni. 8 In such scenarios, te option to use cobalt (Co)-Cr-based alloy materials can serve as an alternative to fabricate guides with investment casting, conforming to the medical device regulations in these countries. Despite the restrictions imposed by these countries, the usage of Ni-Cr dental alloys is on the increase, especially in developing countries due to economic concerns and its mechanical stability properties. Taken together, the authors would like to state that the use of Ni-Cr/Co-Cr-based alloy material as a surgical guide (an alternative to titanium guides) for short transient duration (and not as implants) during the surgical procedure can potentially pave the way for safer and economical utilization in underdeveloped and developing countries with less strict regulations. However, specific quality management and regulatory aspects should be followed per the guidelines from the respective country. 9
Besides operational and regulatory aspects, there are a few technical points that should be considered when utilizing this technique. The present report used material jetting 3D printing technology to print the casting wax pattern. This method enables printing with a smooth surface at an accuracy of 29–32 µm. 10 However, as the material used is cured by ultraviolet light, distortion due to sunlight-related degradation is possible. To avoid this effect, the present casting pattern was rapidly invested after printing. Therefore, there should be no time lag between the printing and the casting procedure, as this may cause distortion or shrinkage and affect the final adaptation of the guide in the surgical site. Diwan et al 11 reported the accuracy of fit of the dental cast framework based on wax pattern storage time. They concluded that the storage time of the wax pattern has a significant effect on the accuracy of the fit of the connectors, and the investing procedure should be possibly completed, preferably within 1 hour or less. Considering that, it may be more helpful to have a laboratory set up where 3D printing and the casting procedures are executed in the same place, as transportation of the printed pattern is also challenging due to the possibility of distortion. The guides in the present report were fabricated conforming to the ISO 9001 Indian guidelines, which are standard requirements for a quality management system, similar to ISO 13485, for the development, production, and servicing of medical devices.
The fabrication accuracy of the guide was assessed subjectively by simulating a conventional mock surgery. The guide provided a perfect adaptation to the 3D printed PLA anatomical model, requiring no adjustments. Additionally, the pre-bent plates on the models had an ideal fit during the surgical procedure. The manual adjustment of the osteosynthesis plates during surgery can be time-consuming and can affect the accuracy of the operation. Intraoperatively, the success of the guide was assessed by the fit in the surgical sites requiring no adjustments, and the ease of performing the osteotomy cuts exhibiting no movement of the surgical guides.
Additionally, no metal debris was noticed during the drilling procedure, due to excellent Vickers hardness properties of the casting alloy material. However, we did see some disadvantages during the surgical procedure. Although the guides had a perfect fit, the thickness of the fabricated guides could have been further decreased, considering its high mechanical strength properties. Secondly, as the guide material had a strong corrosion resistance and hardness properties, the drilling/cutting burs might require a frequent change.
Within the limitations of this report, the authors would like to state that further analysis related to the fabrication accuracy along with a comparative study with titanium surgical guides are required.
Conclusion
The improvised fabrication technique of metal guides with investment metal casting using AM offers ease of production and cost-effectiveness 5 compared to titanium guides making it a copacetic alternative that can be used in various areas in the maxillofacial region. This simple technique of printing cast metal surgical guides is beneficial in many developing countries where 3D printing is expensive and gives better functional and esthetic outcomes of the procedure.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval/Patient Consent
As per the guidelines of the representative country, ethical approval was not applicable. The patient consent was obtained.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
